Introduction
The rates of smoking in the US are now at their lowest levels since World War II1,2. In addition to a drop in the percentage of adults who currently smoke, the percentage of high school students who reported smoking in the past month decreased from 35% in 1999 to 23% in 20053. Despite the reduction in tobacco use among American youth, smoking remains well above the goal of 16% set by Healthy People 2010 (HP 2010)2. Understanding the epidemiology of active cigarette smoking as a type of tobacco use is important in order to establish targets and develop strategies to achieve them. The data used by HP 2010 incorporated race and ethnicity, parents' education level, gender, sexual orientation2, and other associations linked to patterns of overall tobacco use in youth. However, rural residence or, more broadly, place of residence was not among the factors considered in developing HP 2010 objectives regarding youth tobacco use. Because rural residency is associated with higher smoking prevalence estimates among US adults4, it may also be a risk factor among the adolescent population.
Among the many studies examining youth cigarette smoking as tobacco use4-6, most studies that stratified adolescent smoking by rural, suburban, and urban residence were conducted outside the United States of America7-16. These international studies often yielded conflicting findings. For instance, a study of seventh grade Chinese students found no significant differences between rural and urban adolescent smoking rates8, while in Sweden researchers found significantly increased smoking in rural eighth grade students compared with students living in urban areas14. In contrast, the results of a cross-sectional study conducted in Scotland demonstrated higher rates of lung cancer among urban residents due to a higher probability of active tobacco smoking in the USA10,11.
Most US studies on youth smoking that included rurality in the analysis used either regional or otherwise limited data sets4-6. Although these studies have suggested an overall higher prevalence of smoking among rural adolescents6,12, the limitations of these smaller studies leave unanswered the question about whether rurality is a risk factor for youth tobacco use.
Tobacco studies also use different variables, such as experimenter, current social smoker, daily smoker or former smoker, to define tobacco use17-23. For the adolescent smoker, the evolution from experimenter to daily user is a critically important shift. A recent study17 found that the variables that predict a shift from experimental to regular smoking differ from those that predict smoking onset. Likewise, another study18 comparing regular smokers with social smokers also identified variables that differed between the two groups. Neither of these studies included rurality or place of residence in their analyses, leaving a gap in the literature on the impact of residence on the risk of an adolescent becoming a regular or daily smoker.
Using a national data base, this study investigated the question of rurality and its impact on being a daily or regular smoker. Specifically, we explored the question of whether rural residency was an independent risk factor for being a regular/daily smoker among adolescents aged 12 to 18 years. In addition, we sought to characterize rural adolescents who became regular/daily cigarette smokers. Finally, we also explored the issue of how tobacco use in adolescents changed over the study period, and whether this change differed according to place of residence.
Methods
Analyses were conducted on national weighted data from the 1997-2003 Youth Risk Behavior Surveillance System (YRBSS) data to examine factors associated with adolescents who became regular/daily smokers as well as the 7 year trend for becoming a regular/daily smoker. The YRBSS is a school-based survey administered every 2 years under the aegis of the Center for Disease Control and Prevention (CDC) to 9th thru to 12th grade students nationwide to monitor their health risk behaviors. The age of respondents generally ranges between 12 and 18 years. Overall, the survey attempts to collect data on a myriad of behaviors related to six core foci: violence and unintentional injuries; tobacco use; alcohol and other drug use; sexual behaviors; unhealthy dietary behaviors; and physical inactivity, all believed to impact on morbidity and mortality.
Developed in 1990, the purpose of the YRBSS is to determine the prevalence of health-risk behaviors among high-school students in order to assess whether these behaviors increase, decrease, or stay the same over time, and to examine the co-occurrence of health-risk behaviors. It is also used to provide comparable national, state, and local data as well as comparable data among sub-populations of youth.
The survey, developed by an expert panel of scientists, physicians and epidemiologists was constructed so that it could be completed in one 45 min class period. The surveys are administered by using standardized procedures and, since inception, the survey has undergone a number of revisions. A more detailed discussion of YRBSS sampling strategies and data collection methodologies can be found elsewhere24.
The data made available in the weighted national YRBSS datasets minimally have a 60% response rate from the state of collection. For this analysis we merged the relevant 4 years of survey data (collected once every 2 years) into a single dataset, and re-coded a number of the factors of the original variables. Multiple years of the dataset were merged in order to ensure a sufficient number of observations of rural adolescents. The re-coding was assisted analytical ease, and also standardized the responses across the multiple years of survey data examined in this study. Originally our intent was to include more years of survey data than the 1997 to 2003 range; however, specific variables of interest for this study, such as geographic place of residence (urban, suburban and rural), were not included in the datasets outside this range. The specific survey questions and re-coded categories are presented (Table 1). In addition, CDC provides a weighting variable for analysis. We used this weighting variable in the analyses conducted here to ensure the results represented the youth population of the USA.
Table 1: Variables, original survey questions, and re-coded factors used in analysis - 1997-2003 Youth Risk Behavior Survey

For our analysis we used the geographic designations provided by the CDC in their publicly available datasets. We did not re-code these distinctions. To create the rurality variable, the sampling strategy for the 1997-2003 YRBSS expressly took into account the metropolitan statistical area in order to allow for analyses of data stratified by urbanicity (urban, suburban or rural residency). For the YRBSS, the first-stage sampling frame included primary sampling units (PSU) that consisted of large-sized counties or groups of smaller, adjacent counties. The PSU were selected from 16 strata categorized according to the metropolitan statistical area (MSA) status as well as the percentages of African American and Hispanic students in the PSU. The PSU were classified as urban if they were in one of the 54 largest MSA in the USA; otherwise, they were considered rural. A suburban category was created from sub-units of PSU based on proximity to the large MSA24 In the national YRBSS data, students are classified as 'urban', 'suburban', or 'rural', based on the location of the school they attended. Schools defined as urban were located inside an MSA and inside the central city. Schools defined as suburban were located inside an MSA, but outside the central city. Schools defined as rural were located outside an MSA.
Univariate, bivariate and multivariate analytical techniques were employed to examine the study hypotheses. Alpha was set at .05 for all tests of statistical significance. For this analysis we identified seven independent variables that were examined using bivariate contingency tables for their relationship to 'ever being a regular smoker'. Smoking regularly was defined as smoking at least one cigarette a day for 30 days. The independent variables included in the analysis were: age, sex, race/ethnicity, rurality, age when first smoked a whole cigarette, smoking on school property in last 30 days, and use of smokeless tobacco. Based on the results of this bivariate analysis, we developed and tested a multivariate logistic regression model that included all of the independent variables and used smoking status (regular smoker vs never smoked regularly) as the dependent variable. Only youths reporting that they had tried cigarette smoking at least once were included in the multivariate regression analysis. The results of the first multivariate model tested led us to perform a second multivariate analysis using the same dependent variable (daily cigarette smoking) but limiting the population to rural youths who reported trying cigarette smoking at least once. The Statistical Package for Social Scientists (SPSS) v15.0 (SPSS Inc; Chicago, IL, USA; http://www.spss.com/ was used to perform all analyses in this study. This statistical software package allows for the analysis of data collected using a complex sampling design25 and is one of the software packages CDC acknowledges as capable of performing analysis on this database26. This study was approved by the University of Illinois-Chicago College of Medicine at Rockford's Institutional Review Board.
Results
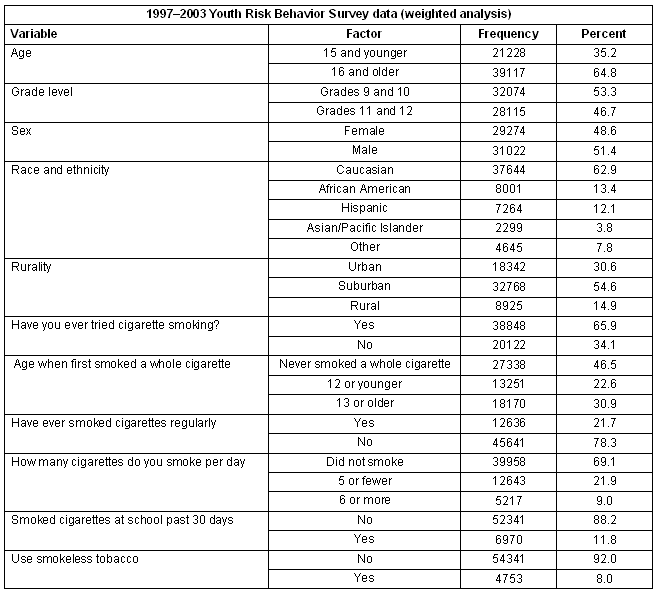
From the merged dataset 60 296 research subjects were included in the analysis. A full description of the population is presented (Table 2). This univariate analysis indicated that 48.6% were female, 35.2% were aged 15 years or younger and 64.8% were aged between 16 and 18 years. Caucasians constituted 62.9% of the population, African Americans 13.4%, and Hispanics 12.1%. Fifty-three percent of the sample was in grades 9 and 10, and 46.7% was in grades 11 and 12. The majority of the surveyed students lived in suburban areas (54.6%), while the smallest proportion lived in rural areas (14.9%). Sixty-six percent of the respondents reported having tried cigarette smoking at least once in their lifetime, with 21.7% reporting that they now or at some time were regular cigarette smokers. Slightly less than 23% of the respondents reported that they had tried smoking cigarettes by age 12 years, and 8% percent of the respondents reported using a smokeless tobacco product in the past 30 days.
Table 2: Univariate description of US population 12-18 years - 1997-2003 Youth Risk Behavior Survey data (weighted analysis)
Overall an examination of the 7 year trend lines indicated that the percentages of youths who reported being regular or habitual cigarette smokers declined from 1997 to 2003 (Fig1), and that this trend held regardless of locale (eg urban, suburban and rural). Between 2001 and 2003 this decline was slightly more pronounced for rural, rather than either urban or suburban, youth although a higher proportion of rural adolescents still reported becoming regular cigarette smokers (p<.05) (Fig1).
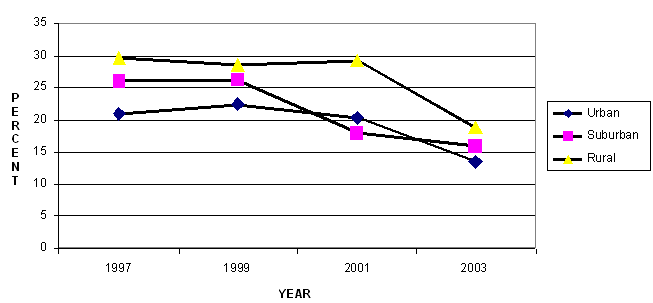
Figure 1: Adolescent 7 year smoking trend, percent regular smoker by locale - 1997-2003 Youth Risk Behavior Survey data.
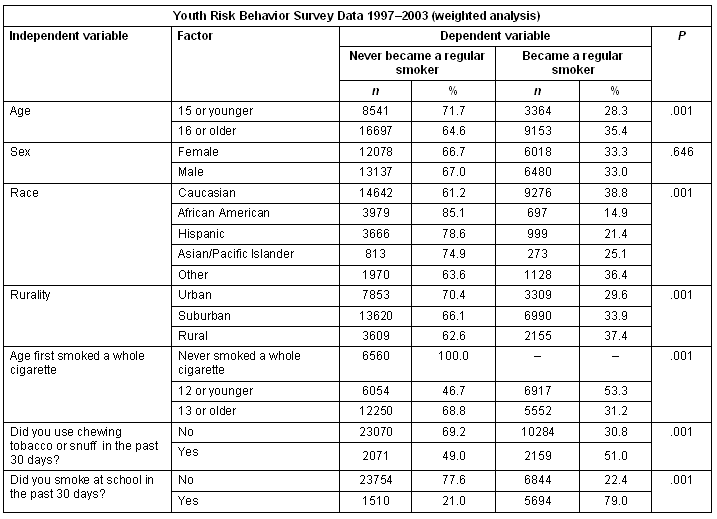
Bivariate analysis using a χ2 test revealed statistically significant relationships between the dependent variable (smoking status) and all of the independent variables, except for sex (Table 3). Only youths reporting that they had tried smoking cigarettes at least once were included in the bivariate analysis. This bivariate analysis revealed a statistically significant (p<.001) relationship between regular smoking among adolescents and place of residence (rurality) with higher rates of regular smoking among rural adolescents (37.4%) when compared with either suburban (33.9%) or urban (29.6%) adolescents. In addition, a higher proportion of youths who first smoked a whole cigarette when they were 12 years old or younger reported becoming regular smokers at some time (53.3%), compared with the proportion of youths who first smoked a whole cigarette when they were 13 years old or older (31.2%). Furthermore, a higher proportion of adolescents reporting that they had used chewing tobacco or snuff in the past 30 days also reported becoming regular smokers at some time (51.0%), compared with the proportion who did not use chewing tobacco or snuff (30.8%).
Table 3: Bivariate analysis of youths aged 12-18 years having tried cigarette smoking, independent variables by smoking status - 1997-2003 Youth Risk Behavior Survey data (weighted analysis)
To explore further the relationship between place of residence and tobacco use a bivariate analysis was completed examining place of residency by use of smokeless tobacco products. This analysis revealed that higher proportions of rural youths who had tried smoking had also tried or used smokeless tobacco products (15.8%) when compared with their urban (8.3%) and suburban (11.5%) counterparts. These differences were statistically significant (p<.05) by χ2 test (not shown).
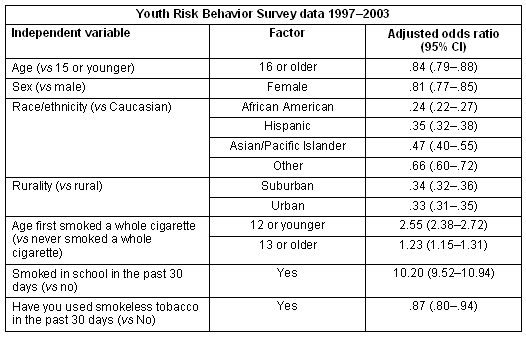
Multivariate logistic regression analysis was performed using daily smoking as the dependent variable and age, sex, race/ethnicity, rurality, age when first tried cigarette smoking, smoking at school in the past 30 days, and using smokeless tobacco as the independent co-variates (Table 4). This analysis revealed that adolescents who became daily smokers were more likely to have first smoked a whole cigarette when they were 12 years or younger (OR=2.55, CI=2.38, 2.72), and to have smoked at school in the past 30 days (OR=10.20, CI=9.52, 10.94). They were less likely to be female (OR=.811, CI=.77, .85) and less likely to be African American (OR=.24, CI=.22, .27), Hispanic (OR=.35, CI=.32, .39), Asian/Pacific Islander (OR=.47, CI=.40, .55) or other race/ethnicity (OR=.66, CI=.60, .72) than Caucasian. In addition, adolescents who lived either in suburban (OR=.34, CI=.32, .36) or urban (OR=.33, CI=.31, .35) locales were less likely to become daily smokers than adolescents living in rural locales.
Table 4: Multivariate regression analysis of youths ages 12-18 years who have tried cigarette smoking, dependent variable: daily smoker - 1997-2003 Youth Risk Behavior Survey data
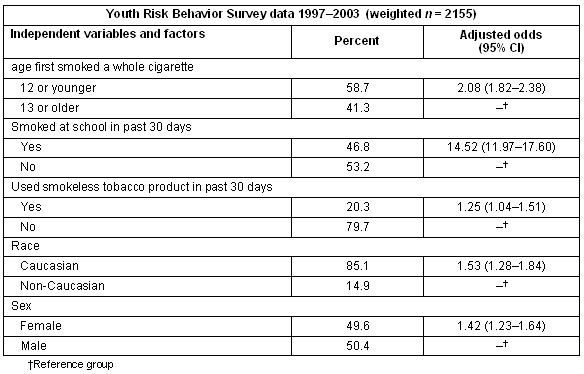
Based on the finding that rural adolescents were more likely to become daily smokers, a second multivariate model was tested using rural youth who had tried cigarette smoking at least once (Table 5). Regular/daily smokers were the dependent variable. For this analysis, race was recoded into a bifurcated variable with the categorical values of Caucasian and non-Caucasian, and smoked at school in the past 30 days was recoded into a variable with the categories of yes/no. The analysis revealed that rural youths who became daily smokers were more likely to: have used smokeless tobacco products in the past 12 months (OR=1.25, CI=1.04,1.51); be female (OR=1.42, CI= 1.23, 1.64); be Caucasian (OR=1.53, CI=1.28, 1.84); have first smoked a whole cigarette when they were 12 years or younger (OR=2.08, CI=1.82, 2.38); and have smoked at school in the past 30 days (OR=14.52, CI=11.97, 17.60).
Table 5: Characteristics of and multivariate regression analysis of rural youths ages 12-18 years who have tried cigarette smoking, dependent variable: daily smoker - 1997-2003 Youth Risk Behavior Survey data, (weighted n = 2155)
Discussion
This study used YRBSS data sets from 1997 to 2003 to compare the tobacco use behaviors of rural youths with their non-rural counterparts. The results indicated that rural high school students were significantly more likely than metropolitan and suburban youths to both try tobacco products and to become regular smokers. This was not surprising because it confirmed the findings of other smaller, regional studies that rural residence was a risk factor for tobacco use in younger individuals12 and that rural adults are more likely to smoke than their non-rural counterparts. An encouraging finding was that, over the study period, smoking prevalence declined in all locales (urban, suburban, and rural). Since 2001 the rate of rural youth smoking declined slightly more than in the other locales. The overall decline in tobacco use seen during the study period may be due in part to the 1998 tobacco settlement. The settlement fostered national anti-smoking campaigns that combined with other changes in public policy, such as increased excise taxes and public smoking bans may have contributed to the downward trend. Although a direct correlation cannot be made, the parallel timing of changes in public policy and the study period at least provides some indirect evidence of the effectiveness of public policy interventions that promote the cessation of tobacco use.
Some but not all of the increased prevalence for rural tobacco use may be attributed to demographics, such as sex and race. However, it seems likely that various characteristics of rural regions contribute to increased rates of tobacco use. For example, rural youth may have experienced less exposure to anti-tobacco advertising campaigns that can create an environment in which tobacco use is considered less acceptable. A study on Indiana youth found that adolescents residing in urban and suburban areas were twice as likely as those from rural areas to be aware of media messages about the dangers of tobacco use4. There may also be easier access and availability of tobacco products for rural youth, especially in tobacco growing regions27, and fewer regulatory restrictions on smoking in public places. Replicating the smoking bans in public places and businesses that are taking hold in metropolitan areas28,29 may make smoking less socially acceptable in rural communities. Even though the mechanisms of how social context influences teen smoking are not well understood30, exposure to smokers in an adolescent's environment is a significant risk factor for tobacco use31,32. The increased likelihood of exposure to smoking peers and adults most likely contributed to an environmental milieu conducive for young individuals to first try, and then maintain, tobacco use in rural settings.
Regardless of the underlying cause, addressing the risk for the more than 3 million adolescents who smoke32 is critical. Adolescents face immediate health consequences, such as more shortness of breath, poorer levels of fitness, and increased phlegm production33. Tobacco use is also commonly referred to as a gateway for other substance abuse34,35. For adults, smoking remains the greatest single cause of preventable death in the USA36 and, of those adolescents who smoke, one-third are expected to die prematurely as a consequence of smoking37. Targeting teens is particularly important because only 10% of adult smokers start after the age of 18 years. Our findings suggest that the anti-tobacco actions that have decreased tobacco use nationally should incorporate strategies aimed at addressing tobacco use in rural settings. For example, our findings demonstrated a correlation between the recent use of smokeless tobacco products and youths reporting being regular smokers. Because the rate of smokeless tobacco use was also found to be higher in rural areas, customizing anti-tobacco campaigns for rural youths to address the use of smokeless tobacco products may result in a larger decrease in the overall smoking rate in this population.
Limitations
This study has several limitations. First, the definition of rural used in this analysis was the one used by CDC, the agency designing the survey and the sampling methodology as well as collecting the data. Their single definition of rural may not be the best one available. It is difficult to assess what bias, if any, this definition introduced. Second, the data are self-reported and subject to error. Any bias in this case is likely be to in underreporting the rate of tobacco use, suggesting that the prevalence of tobacco use is actually higher in the high school population. Third, the population of this study included only youths who attended high school and were present to complete the survey. This suggests the possibility of a subpopulation of adolescent truants and drop-outs who were not represented using YRBSS data. Fourth, although several confounding variables associated with tobacco use were accounted for, it is possible that other unidentified factors accounted for the increase risk of tobacco use, other than rural residence. For instance, parental education levels, which were not included in the questionnaire, may have impacted smoking rates.
Despite these limitations, YRBSS is a primary data source on the health-risk behaviors of US youth, and its reliability and validity has been demonstrated repeatedly38. Presently, YRBSS data has been chosen as the source to monitor 16 national health objectives for 2010, and three of the 10 leading health indicators38.
Overall, our study revealed a favorable trend in youth smoking behavior in the USA during the past decade. All communities have seen a decrease in smoking prevalence; however, rural communities continue to experience a higher youth smoking rate compared with urban and suburban communities. Identifying rural residency as a potential risk factor for tobacco use is only a starting point, but one that suggests the need to develop interventions that target children in this setting. This analysis should be helpful in guiding the same combination of initiatives credited with reducing smoking levels nationally, including anti-tobacco educational efforts and messages, increasing tobacco prices, and implementing school programs and public policy for rural youth.
Acknowledgement
The authors acknowledge the helpful comments made by Eric Henley, MD, MPH on earlier drafts of this manuscript.
References
1. Cokkinides V, Bandi P, Ward E, Jemal A, Thun M. Progress and opportunities in tobacco control. CA: A Cancer Journal for Clinicians 2006; 56: 135-142.
2. US Department of Health and Human Services. Healthy People 2010: Understanding and improving health, 2nd edn. Washington, DC: U.S. Government Printing Office, November 2000.
3. National Center for Chronic Disease Prevention and Health Promotion, Division of Adolescent and School Health. Youth online: comprehensive results. (Online) 2008. Available: http://www.cdc.gov/HealthyYouth/yrbs/ (Accessed 11 January 2008).
4. Doescher MP, Jackson JE, Jerant A, Hart LG. Prevalence and trends in smoking: a national rural study. Journal of Rural Health 2006; 22: 112-118.
5. Zollinger TW, Saywell RM, Overgaard AD, Przbylski MJ, Dutta-Bergman M. Antitobacco media awareness of rural youth compared to suburban and urban youth in Indiana. Journal of Rural Health 2006; 22: 119-123.
6. Unger JB, Shakib S, Cruz TB, Hoffman BR, Pitney BH, Rohrback LA. Smoking behavior among urban and rural native American adolescents in California. American Journal of Preventive Medicine 2003; 25: 251-254.
7. Chen X, Stanton B, Fang X, Li X, Lin D, Zhang J et al. Perceived smoking norms, socio-environmental factors, personal attitudes and adolescent smoking in China: a mediation analysis with longitudinal data. Journal of Adolescent Health 2006; 38: 359-368.
8. Shakib S, Zheng H, Johnson CA, Chen X, Sun P, Palmer PH et al. Family characteristics and smoking among urban and rural adolescents living in China. Preventive Medicine 2005; 40: 83-91.
9. Barnett R, Pearce J, Moon G. Does social inequality matter? Changing ethnic socio-economic disparities and Maori smoking in New Zealand. Social Science and Medicine 2005; 60: 1515-1526.
10. Pearce J, Boyle P. Is the urban excess in lung cancer in Scotland explained by patterns of smoking? Social Science and Medicine 2005; 60: 2833-2843.
11. Iversen L, Hannaford PC, Price DB, Godden DJ. Is living in a rural area good for your respiratory health? Chest 2005; 128: 2059-2067.
12. Cronk CE, Sarvela PD. Alcohol, tobacco, and other drug use among rural/small town and urban youth: a secondary analysis of the monitoring the future data set. American Journal of Public Health 1997; 87: 760-4.
13. Volzke H, Neuhauser H, Moebus S, Baumert J, Berger K, Stang A et al. Urban-rural disparities in smoking behavior in Germany. BMC Public Health 2006: 6: 146.
14. von Bothmer MIK, Mattsson B, Fridlund B. Influences on adolescent smoking behaviour: siblings' smoking and norms in the social environment do matter. Health and Social Care in the Community 2002; 10: 213-220.
15. Barnett R, Moon G, Kearns R. Social inequality and ethnic differences in smoking in New Zealand. Social Science Medicine 2004; 59: 129-143.
16. Reitsma AH, Manske S. Smoking in Ontario schools: does policy make a difference? Canadian Journal of Public Health 2004; 95: 214-218.
17. Robinson LA, Murray DM, Alfano CM, Zbikowski SM, Blitstein JL, Klesges RC. Ethnic differences in predictors of adolescent smoking onset and escalation: a longitudinal study from 7th to 12th grade. Nicotine Tobacco Research 2006; 8: 297-307.
18. Ellison J, Mansell C, Hoika L, MacDougall W, Gansky S, Walsh M. Characteristics of adolescent smoking in high school students in California. Journal of Dental Hygiene 2006; 80: 1-16.
19. Leatherdale ST. Predictors of different cigarette access behaviours among occasional and regular smoking youth. Canadian Journal of Public Health 2005; 96: 348-352.
20. Murnaghan DA, Sihvonen M, Leatherdale ST, Kekki P. The relationship between school-based smoking policies and prevention programs on smoking behavior among grade 12 students in Prince Edward Island: a multilevel analysis. Preventive Medicine 2007; 44: 317-322.
21. Leatherdale ST, Manske S, Kroeker C. Sex differences in how older students influence younger student smoking behaviour. Addictive Behaviors 2006; 31: 1308-1318.
22. O'Connor RJ, Kozlowski LT, Vandenbergh DJ, Strasser AA, Grant MD, Vogler GP. An examination of early smoking experiences and smoking status in a national cross-sectional sample. Addiction 2005; 100: 1352-1357.
23. Wiltshire S, Amosa A, Hawb S, McNeillc A. Image, context and transition: smoking in mid-to-late adolescence. Journal of Adolescence 2005; 28: 603-617.
24. Brener ND, Kann L, Kinchen SA, Grunbaum JA, Whalen L, Eaton D et al. Methodology of the Youth Risk Behavior Surveillance System. Morbidity and Mortality Weekly Report 2004; 53: 1-13.
25. SPSS Inc. Tech tips. (Online) 2008. Available: http://www.spss.com/corpinfo/newsletter/december_tip1.htm (Accessed 11 January 2008).
26. National Center for Chronic Disease Prevention and Health Promotion, Division of Adolescent and School Health. Healthy youth! YRBSS. Frequently asked questions. Uses of youth risk behavior surveillance system (YRBSS). Results. (Online) 2006. Available: http://www.cdc.gov/HealthyYouth/yrbs/faq.htm (Accessed 11 January 2008).
27. Smith TM, Tingen MS, Waller JL. The influence of self-concept and locus of control on rural preadolescent tobacco use. Southern Online Journal of Nursing Research 2005; 6: 1-19.
28. Crawford MA, Balch GI, Mermelstein R. The Tobacco Control Network Writing Group. Responses to tobacco control policies among youth. Tobacco Control 2002; 11: 14-19.
29. Crawford MA, Tobacco Control Network Writing Group. Cigarette smoking and adolescents: messages they see and hear. Public Health Report 2001; 116: 203-15.
30. Wahl SK, Turner LR, Mermelstein RJ, Flay BR. Adolescents' smoking expectancies: psychometric properties and prediction of behavior change. Nicotine Tobacco Research 2005; 7: 613-623.
31. Biglan A, Duncan TE, Ary DV, Smolkowski K. Peer and parental influences on adolescent tobacco use. Journal of Behavioral Medicine 1995; 18: 315-330.
32. Schepis TS, Rao U. Epidemiology and etiology of adolescent smoking. Current Opinion In Pediatrics 2005; 17: 607-612.
33. Stone SL, Kristeller JL. Attitudes of adolescents toward smoking cessation. American Journal of Preventive Medicine 1992; 8: 221-225.
34. Haddock CK, Weg MV, DeBon M, Klesges RC, Talcott GW, Lando H et al. Evidence that smokeless tobacco use is a gateway for smoking initiation in young adult males. Preventive Medicine 2001; 32: 262-267.
35. Botvin GJ, Griffin KW, Diaz T, Scheier LM, Williams C, Epstein JA. Preventing illicit drug use in adolescents: long-term follow-up data from a randomized control trial of a school population. Addictive Behavior 2000; 25: 769-774.
36. Fagerstrom K. The epidemiology of smoking: health consequences and benefits of cessation. Drugs 2002; 62(Suppl2): 1-9.
37. CDC, Office on Smoking and Health, Division of Adolescent and School Health, National Center for Chronic Disease Prevention and Health Promotion. Cigarette Use Among High School Students --- United States 1991-2005. Morbidity and Mortality Weekly Report 2006; 55: 724-726.
38. Kann L. The youth risk behavior surveillance system: measuring health-risk behaviors. American Journal of Health Behavior 2001; 25: 272.
Abstract
Introduction: Daily cigarette smoking among US adolescents remains a significant public health problem. Understanding risk is important in order to develop strategies to reduce this type of tobacco use. Purpose: The primary objective of this research was to examine whether rural residency is an independent risk factor for being a daily smoker among adolescents ages 12 to 18 years.
Methods: This is a cross-sectional study where univariate, bivariate, and multivariate analyses were performed on a merged 1997-2003 Youth Risk Behavior Surveillance System dataset to determine whether rural residence was a significant risk factor for daily cigarette smoking, after adjusting for demographic factors.
Results: Using daily smoking as the dependent variable, initial multivariate analyses revealed that adolescents who lived either in suburban (OR=.34, CI=.32, .36) or urban (OR=.33, CI=.31, .35) locales were less likely to become daily smokers than adolescents living in rural locales. Subsequent logistic regression analysis yielded that rural youths who became daily smokers were more likely to: have used smokeless tobacco products in the past 12 months (OR=1.25, CI=1.04,1.51); be female (OR=1.42, CI=1.23, 1.64); be Caucasian (OR=1.53, CI=1.28, 1.84); have first smoked a whole cigarette when they were 12 years of age or younger (OR=2.08, CI=1.82, 2.38); and have smoked at school in the past 30 days (OR=14.52, CI=11.97, 17.60).
Conclusions: The results indicate that rural residency is a risk factor for tobacco use among US youth.
Key words: adolescent tobacco use, rural youth tobacco use, Youth Risk Behavior Surveillance System.
You might also be interested in:
2016 - Access to chlamydia testing in remote and rural Scotland
2010 - Postgraduate training at the ends of the earth - a way to retain physicians?
2009 - Reducing the risk of pandemic influenza in Aboriginal communities







