Population health scholars have noted that a demographic challenge to population health is the unequal distribution of access to health care. Likewise, health scholars and policy makers have been concerned about increasing physician shortages in the USA for several decades, an issue that has been particularly challenging in Mississippi1,2. While measures of access to care include more than the availability of physicians, physician shortages hinder residents from obtaining routine care easily, which potentially magnifies health disparities as individuals may postpone care until encountering severe health problems. A shortage of primary care physicians is not only detrimental to individual health, but also harmful to the economic and social structures of the communities involved.
Another detriment to individual and community wellbeing is physicians exiting practice, particularly in shortage areas. Prior research has focused on the links between physician workforce exit and physician, practice, and patient characteristics associated with physician career satisfaction3-12. Physicians who are dissatisfied with their career are more likely to exit practice5. Primary reasons for leaving a practice location include poor fit, financial reasons, and lack of a work-life balance11,13, although the strength of the association varies based on physician and practice characteristics4-10,12.
Despite extensive research on physician career satisfaction and its association to remaining in practice, little research has focused on the number of years that physicians practice. This study focuses on the physician workforce of Mississippi, a state plagued by extreme health disparities and high poverty rates. Physicians in Mississippi report higher levels of career dissatisfaction6. Using data from licensure applications, this study assessed the expected career duration of Mississippi's physician population active in patient care. This study also estimated the expected number of years in active patient care for physician specialty, gender, race, urban-rural practice location, and health professional shortage area location. The following hypotheses were tested:
- The career life expectancy of primary care physicians is longer than that of specialists.
- Men physicians will have longer career life expectancy than women physicians.
- The career life expectancy of white physicians is longer than that of minority physicians.
- Physicians in rural counties will have a longer career life expectancy than that of physicians in urban counties.
- Physicians practicing in health professional shortage counties will have a shorter career life expectancy than that of physicians practicing in non-shortage counties.
The study also hypothesized that the difference in career expectancy between each physician population subgroup would be statistically significant. Findings of this study may contribute to the development of recruitment and retention strategies of physicians in Mississippi and other areas that struggle with physician shortages.
Data
Data on the Mississippi physician population were obtained from the Mississippi State Board of Medical Licensure's applications for the years 2007-2011. These applications provide information on individual physicians such as primary practice location, practice specialty, hours worked per week at primary practice location, race, gender, and date of original licensure in Mississippi. An advantage of this data is that it is in real time and avoids the issue of reporting lags found in the American Medical Association Masterfile14.
Measures
Physician population (N=5418) is defined as the number of physicians who applied for licensure or renewed their medical license, who identified a primary practice location in Mississippi, and who were involved in at least 20 hours per week of active patient care during the 5-year period of 2007-2011. The study also examined physician career life expectancy for five physician population subgroups: practice specialty, gender, race, rural/urban location, and health professional shortage area. Practice specialty was categorized as either primary care or specialist. Physicians who identified a primary specialty of family medicine, general medicine, internal medicine, obstetrics/gynecology, or pediatrics on their licensure application were categorized as primary care physicians (PCP). All other physicians were categorized as specialists. Physician gender was categorized as men or women. Physician race was categorized as white or minority. Due to the underrepresentation of minority physicians in Mississippi, further delineation of racial groups was not possible.
The 2003 Rural-Urban Continuum Codes (RUCC) were used to categorize physicians' primary practice county as either rural or urban. These codes are based on population size, the level of urbanization, and the adjacency of non-metropolitan counties to a metropolitan area15. In this study, rural counties refer to non-metropolitan counties per the RUCC (codes 4-9); urban counties are those identified as metropolitan counties according to the RUCC (codes 1-3). It is important to examine the differences in career life expectancy for Mississippi physicians by the rural or urban characteristic as half of Mississippians reside in a rural county16, a rate considerably greater than the national average.
Primary Medical Care Health Professional Shortage Area (HPSA) designations, as determined by the Health Resources and Services Administration17, were used to determine if a physician's primary practice location was in a shortage area. Physicians' primary practice county was categorized as either HPSA or non-HPSA. Mississippi counties that were designated as a single-county HPSA were coded as a HPSA county; all other counties were coded as a non-HPSA county. It is essential to observe variations in expected career life for Mississippi physicians based on HPSA designation as more than half of Mississippians reside in a primary care HPSA, the highest estimate of a state's medically underserved population in the USA. But primary care HPSAs are not limited to individual counties. While many shortage areas are based on access to medical care within a geographic area, such as county, other shortage areas may be found within a county based on population demographics, such as low income. A limitation of this research is the use of primary practice county to identify the number of physicians entering and exiting practice in primary care HPSAs. While some HPSA physicians may have been undercounted in the study analysis, roughly 60% of Mississippi's 82 counties are designated as a single-county HPSA, so any bias in the results is likely minimal.
Statistical analysis
To determine how long physicians practice in Mississippi, separate abridged period career life tables were constructed for the physician population and for 10 physician subgroups based on practice specialty, gender, race, urban/rural practice, and HPSA/non-HPSA practice. The abridged table consisted of career age groups at 5-year intervals to compare career expectancy from career entry (<1 year) to older career age (≥45 years). To determine the physician population at each career age interval, a measure of physician career age was calculated using the date medical licensure was obtained in Mississippi and the midpoint of the years 2007-2011. The number of physicians who exited practice at any point during the period studied was also calculated. Physicians were considered to have exited practice if they had not renewed their medical licensure with the Mississippi Board of Medical Licensure, no longer claimed a primary practice location in Mississippi or had not engaged in active patient care for at least 20 hours per week. Gehan's generalized Wilcoxon test was used to determine if the odds of remaining in practice were statistically different between the two categories for each of the five subgroup populations.
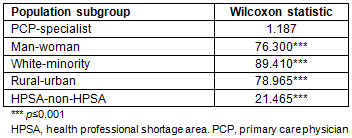
Descriptive statistics for the active physician population in Mississippi are presented in Table 1. The average age of Mississippi's physician population was 50.24 years, which is comparable to the national physician mean age of 50 years in 20102. On average, physicians active in patient care had been licensed to practice medicine in Mississippi for about 17.5 years. Primary care physicians accounted for 42.28% of the population; 57.72% of Mississippi's physician population self-identified as specialists. Men physicians represented 80.27% of the physician population in Mississippi, indicating that women were underrepresented at 19.73% of Mississippi's physician population. Nationally, women physicians accounted for about 30% of the physician population2. White physicians represented 80.55% of the population; minority physicians in Mississippi were also underrepresented, accounting for 19.45% of the physician population. These statistics do not reflect Mississippi's racial distribution, where non-Hispanic whites were estimated to be 58.25% of the population in 2007-201118. Physicians practicing in rural counties accounted for 39.15% of Mississippi physicians, while 60.85% of Mississippi physicians practiced in an urban county. Physicians practicing in a HPSA county represented 13.65% of the population; 86.35% of the physician population primarily practiced in a non-HPSA county.
Table 2 presents the expected career life of active Mississippi physicians. Career expectancy at career entry (<1 year) was 14.4 years for all active physicians. Essentially, physicians in Mississippi would practice an average of 14.4 years if, throughout their career, they were to experience the age-specific career exit rates for the 2007-2011 period. Career expectancy for all physicians remained similar at the 1-4 years career age interval. Mississippi physicians who continued to actively practice at the career age interval of 5 -9 years could expect to practice another 22.2 years, suggesting that the first 5 years of practice in Mississippi are critical to physician retention. The Mississippi physician population with a career age of 30-34 years would expect to practice an average of 16.8 more years. Considering this physician group is most likely in their early 60s in terms of biological age, this finding suggests many Mississippi physicians do not conform to the expected retirement age of 65 and continue to practice medicine into their 70s.
Primary care physicians have longer career expectancies than do specialists at all career age intervals. They can expect to practice for 15.6 years upon licensure in Mississippi, and specialists can expect to practice 14.0 years at career entry. As with all physicians, career expectancy increased at the 5-9 years interval for both PCPs and specialists, again suggesting that the first 5 years of practice in Mississippi are crucial to retention. The difference in career expectancy between PCPs and specialists was widest at the 35-39 years interval, where PCPs have a career expectancy of 18.1 years compared to 13.3 years for specialists. At this career age interval, many physicians are in their 60s and are likely considering retirement. The widening gap between PCPs and specialists at this interval may indicate that specialists enter retirement earlier than PCPs.
Career expectancy for men physicians was greater than that for women physicians at all career age intervals. Upon licensure in Mississippi, men physicians could expect to practice 15.1 years, and women physicians could expect to practice 12.8 years. At the 5-9 years interval, the career expectancy of men was 23.5 years and 18.8 years for women, suggesting that the first 5 years of practice in Mississippi are essential for physician retention. The difference in career expectancy between men and women physicians is wider than that of the other subgroups at most career age intervals. Compared to other subgroups, women physicians experienced the lowest career expectancy at all intervals, indicating that they were more likely to exit practice than any other characteristic examined.
White physicians experienced shorter career expectancy at licensure than did minority physicians. White physicians in Mississippi would practice for an average of 14.6 years if they were to experience the age-specific career exit rates for the 2007-2011 period throughout their careers. Minority physicians could expect to practice for 15.8 years. At the 5-9 years interval, career expectancy increased to 22.8 years for white physicians and 24.4 years for minority physicians. These increases from the career expectancy at career entry likely imply that the emphasis on retention efforts should occur within the first 5 years of practice in the state. Minority physicians experienced longer career expectancies at all career age intervals compared to white physicians, indicating that minority physicians remained in active practice longer than their white peers. The greatest difference between white and minority physicians occurred at the 35-39 years interval, where the career expectancy for white physicians was 15.3 years and 23.7 years for minority physicians. This difference likely implies that minority physicians retire or exit practice at older ages than white physicians.
Physicians practicing primarily in rural counties had a career expectancy at career entry of 16.3 years, the highest of all groups examined. Physicians in urban counties had a career expectancy at career entry of 13.5 years, one of the lowest among all groups in the study. Career expectancy increased at the 5-9 years interval to 23.9 years for rural physicians and 21.1 years for urban physicians, indicating that the first 5 years of practice are important in physician retention. Rural physicians had longer career expectancy than did urban physicians at all career ages. The difference between the two narrowed at the 10-14 years interval and remained narrow until the 40-45 years interval, which is the widest difference in career expectancy between rural and urban physicians. The widening at the 40-45 years interval likely indicates that physicians practicing in urban counties exited the workforce earlier than their rural colleagues.
The expected career life at career entry of Mississippi physicians practicing primarily in HPSA counties was 16.1 years, one of the longest in the study. Physicians practicing in non-HPSA counties had a shorter career expectancy at career entry, 14.2 years, than their peers in HPSA counties. At the 5-9 years interval, the career expectancy of HPSA physicians increased to 22.1 years and to 22.0 years for non-HPSA physicians, again suggesting that the first 5 years of practice are vital to physician retention. The difference in career expectancy between HPSA and non-HPSA physicians was minimal, at least until the 20-24 years interval where it widened substantially. However, the difference between the two groups was widest at the 40-44 years interval, implying that HPSA physicians are more likely to remain in practice at older ages and to potentially delay full retirement.
Results of the Wilcoxon test statistic to determine if the survival difference between each of the subgroups is statistically significant are shown in Table 3. The risk of exiting active physician practice in Mississippi was significantly different for men and women physicians, white and minority physicians, rural and urban physicians, and HPSA and non-HPSA physicians, but not for primary care and specialist physicians.
Table 1: Descriptive statistics, Mississippi physicians active in patient care, 2007-2011 (N=5418)
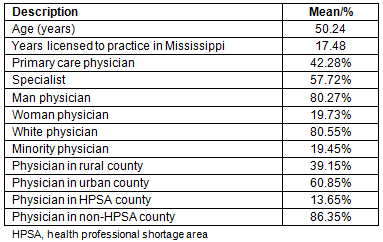
Table 2: Expected career life of Mississippi physicians, total active population and physician population subgroups
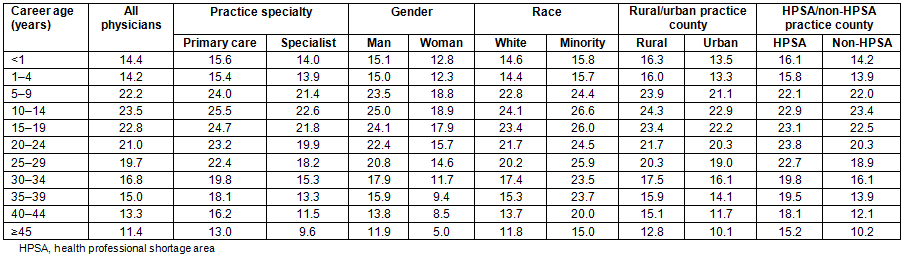
Table 3: Subgroup differences in risk of exiting practice (Gehan's generalized Wilcoxon test)
Discussion
The primary objective of this research was to estimate how many years physicians actively practice in Mississippi. Upon entry into practice in Mississippi, physicians could expect to practice for 14.4 years. Career life expectancy increases substantially in the 5-9 years category, suggesting that physicians are more likely to exit practice in the state of Mississippi within their first 5 years of practice. This finding supports prior research that found young physicians are more likely to change practices in their first 5 years13. Three of the five hypotheses concerning expected subgroup differences in the career life expectancy of Mississippi physicians were supported. As hypothesized, PCPs did experience a greater career life expectancy upon entry into practice in Mississippi than did specialists. However, the risk of exiting practice was not significantly different for these two subgroups. Little is known about the differences in career life expectancy of physicians based on practice specialization, but prior research has found that PCPs were generally more likely to report being dissatisfied with their careers7. Thus the expected and actual finding seem contradictory. However, there were two reasons for the expectation that PCPs would have longer career expectancy. First, the incomes of specialists tend to be higher than PCP incomes19, and these higher incomes may allow specialist physicians to exit practice earlier than their primary care peers. Second, PCPs in Mississippi may be more likely to be self-employed. Although the data did not provide clear indicators of employment status, the assumption was based on the fact that PCPs accounted for the greatest share of solo practices20 and were more likely to be self-employed physicians13. Additionally, the physicians in most Mississippi communities were PCPs working in solo or small group practices, and the financial investment to be a self-employed physician likely reduces the odds of relocating practice. Compared to employee physicians, self-employed physicians are less likely to exit practice and more likely to report greater work autonomy13.Work autonomy is one of the strongest indicators of physician satisfaction11, and physicians who are satisfied are more likely to practice longer5 or to remain in their current practice location10.
The findings also support the hypothesis that the career life expectancy of men physicians would be greater than that of women physicians, and the findings also revealed that the risk of exiting practicing was significantly different for men and women physicians. Female physicians in Mississippi seemed to struggle with career duration, and this shorter career expectancy of women physicians may be tied to socially assigned gender roles. Women are more likely to exit the workforce, even if temporarily, due to family reasons. Prior studies have found that women physicians encounter conflict between work and family roles more so than their male peers3,8,21,22. Unlike most men physicians, women physicians are more likely to be part of a dual-career couple3,13,21. Thus, women physicians may need to practice in areas that provide employment opportunities for their romantic partners, as their partner's career may take precedence over their own. Consequently, being part of a dual-career couple may limit the practice location choices of women physicians. Because women are more likely to take on the role of caregiver within the family, women physicians with young children may also need more flexible work schedules than men physicians. This need for flexibility may deter women physicians from self-employed practice and encourage them to seek employee positions. Female physicians tend to have lower incomes8 and are more likely to experience workplace discrimination22 and patient conflicts12. Because each of these factors is strongly related to career satisfaction, women physicians may exit practice in Mississippi for underlying reasons that are different from those of men physicians. Understanding more about the reasons women physicians exit practice, as well as that women physicians may be practicing fewer hours or returning to the workforce in later years, could be the first steps in designing recruitment strategies and improving the retention rates of women physicians in Mississippi.
As hypothesized, Mississippi physicians who primarily practiced in a rural county enjoyed longer careers upon receiving their medical licensure than their urban counterparts. The risk of exiting practice was also significantly different for rural and urban physicians. Although there is a strong association between work demands and physician career satisfaction11 and a consistent finding that urban physicians report greater satisfaction than their rural counterparts23, support for this hypothesis was expected because of the association of employment status to career satisfaction. Because rural counties tend to have fewer physicians, self-employed physicians may be more common. However, differences in the career expectancy of physicians in rural and urban counties may merely be highlighting variations in the spatial distribution of physician specialties, as specialists tend to be concentrated in population centers and exhibit shorter career expectancy. These urban-rural differences may also be highlighting gender differences in the distribution of physicians as women physicians are also more likely to practice in urban areas24 and have shorter practice lives than men.
The finding that physicians practicing in HPSA counties experienced greater career expectancy than do physicians in non-HPSA counties was not expected. By definition, HPSA counties are medically underserved with too few physicians, so the hypothesis was based on the assumption that HPSA physicians would burn out faster and experience greater career dissatisfaction due to demanding work schedules based on patient and community characteristics. However, one study found perceived quality of care to be a crucial indicator of career satisfaction9, so HPSA physicians may be experiencing greater career expectancy if they feel that they are providing a high quality of care by working in areas where the physician supply is not sufficient to meet the needs of a community. The risk of exiting practice was statistically different for HPSA and non-HPSA physicians.
Another unsupported hypothesis was that white physicians would experience a greater career expectancy than minority physicians. This hypothesis was based on the notion that minority physicians, relative to their white counterparts, would face difficulties in finding a cultural fit in predominantly white practices or communities, experience discrimination12, and have greater career dissatisfaction4. However, the analysis revealed that minority physicians experienced longer career expectancy at all career age intervals than white physicians. This finding may be indicative of prior research that suggests that some minority physicians, primarily black physicians, experience greater job satisfaction if the majority of their patient base is of the same race4. Likewise, minority patients have shown a preference for physicians of the same race25. Given that the population of Mississippi is disproportionately black, attracting and retaining black physicians in Mississippi may be one possible step to reducing health disparities in the state. Additionally, the risk of exiting practice was statistically different for white and minority physicians. Differences in the career expectancy at all career ages of white and minority physicians suggest that more needs to be understood about the push and pull factors appealing to minority physicians in order to increase the share of minority physicians practicing in the state.
This research is not without its limitations and highlights the need for additional measures of physician subpopulations that could shape career expectancy. First, employee physicians and self-employed physicians may have different career longevity trajectories as self-employed physicians tend to be less likely to relocate their practice, while employee physicians may be more mobile due to weaker ties to the communities in which they practice13. Second, information on the location of training seems vital to the validity of differences in career longevity as in-state versus out-of-state and international medical graduates and domestic medical graduates likely have different work and retirement patterns. Physicians who start practice in the state where they attended medical school are more likely to remain in that initial practice location13. International medical graduates are more likely than domestic medical graduates to experience discrimination by patients12, which likely directly affects their career satisfaction and indirectly affects their career longevity in a single location. Third, increases in osteopathic physicians nationally and the opening of an osteopathic school within Mississippi may result in a need to distinguish differences in career longevity between osteopathic and allopathic physicians. Finally, Mississippi recently reduced practice constraints of advanced practice registered nurses, potentially alleviating workloads for PCPs in shortage areas, particularly since the projected growth in the number of these nurses is more substantial than that of physicians26. Thus, understanding the career expectancy of primary care providers may be essential to the recruitment and retention practices and individual and community wellbeing.
Another limitation of this research is the lack of patient characteristics and how they may shape differences in physician career expectancy. Future research could focus on patient characteristics, such as socioeconomic status, insurance status, and health status. However, it may be difficult to obtain this information for each practicing physician. Instead, future research could assess physician career life expectancy differences based on county-level measures, such as the percentage of the population in poverty or receiving Medicaid. Such research is still problematic because many patients cross county and state borders to receive medical care, but it may be a starting point for considering how patient or community characteristics influence physician career longevity.
A final limitation of this research is that the results lack local and national comparability as it is not possible to determine if or how the career expectancy of Mississippi physicians is markedly different from that of prior years or from that of physicians practicing elsewhere. Some degree of turnover is normal, but the bigger question becomes what is normal and how can medical schools, policy makers, and employers minimize turnover and improve retention for newly licensed physicians. Minimizing physician turnover is particularly critical in a state like Mississippi, which has a physician shortage and a population that is unhealthy. Examining changes in career expectancy of Mississippi physicians over time may be particularly important as the Mississippi physician workforce ages and diversifies. The physician and practice characteristics examined in this study do not operate independently, thus physician career expectancy is more complex. Identifying the career expectancy of physicians nationally based on practice specialty, gender, race, and location of practice and how these characteristics intersect may also be important to reduce physician shortages.
Physician, practice, and patient characteristics undoubtedly shape the career life of Mississippi physicians. Differences in career expectancy for the various physician subgroups may have serious implications for population health, unintentionally maintaining health disparities in areas with a large proportion of vulnerable populations and negating efforts of population health scholars and policies to reduce health disparities by improving access to care. An assessment of current recruitment and retention policies is needed to identify and build on the successful programs in order to expand the career life expectancy of physicians who are specialists, women, white, practicing in urban counties, or practicing in non-HPSA counties and to grow the share of physicians who are PCPs, minorities, and practicing in rural or HPSA counties. More importantly, understanding the push and pull factors linked to practice medicine in Mississippi can guide the development of policies and programs aimed at recruitment and retention, particularly among newly licensed physicians. In many areas of Mississippi, the loss of just a single physician could dramatically affect patient workloads for remaining physicians, creating additional barriers to care as residents may be forced to seek healthcare outside of their county of residence. Traveling to other communities for healthcare may not be an option for many residents, particularly poorer ones. However, increasing physician career expectancy in Mississippi alone is unlikely to improve population health substantially, as improvements in social and economic equity are key determinants of population health.
References
1. Association of American Medical Colleges. 2013 state physician workforce data book. Washington, DC: Association of American Medical Colleges, Center for Workforce Studies, 2014.
2. Young A, Chaudhry HJ, Thomas JV, Dugan M. A census of actively licensed physicians in the United States, 2012. Journal of Medical Regulation 2013; 99(2): 11-24.
3. Dyrbye LN, Shanafelt TD, Balch CM, Satele D, Sloan J, Freischlag J. Relationship between work-home conflicts and burnout among American surgeons: a comparison by sex. Archives of Surgery 2011; 146(2): 211-217.
4. Glymour MM, Saha S, Bigby J. Physician race and ethnicity, professional satisfaction, and work-related stress: results from the Physician Worklife Study. Journal of the National Medical Association 2004; 96(10): 1283-1294.
5. Landon BE, Reschovsky JD, Pham HH, Blumenthal D. Leaving medicine: the consequences of physician dissatisfaction. Medical Care 2006; 44(3): 234-242.
6. Leigh J, Kravitz RL, Schembri M, Samuels SJ, Mobley S. Physician career satisfaction across specialties. Archives of Internal Medicine 2002; 162(14): 1577-1584.
7. Leigh JP, Tancredi DJ, Kravitz RL. Physician career satisfaction within specialties. BMC Health Services Research 2009; 9: 166.
8. McMurray JE, Linzer M, Konrad TR, Douglas J, Shugerman R, Nelson K, et al. The work lives of women physicians. Journal of General Internal Medicine 2000; 15(6): 372-380.
9. Pratt WR. Physician career satisfaction: examining perspectives of the working environment. Hospital Topics 2010; 88(2): 43-52.
10. Rittenhouse DR, Mertz E, Keane D, Grumbach K. No exit: an evaluation of measures of physician attrition. Health Services Research 2004; 39(5): 1571-1588.
11. Scheurer D, McKean S, Miller J, Wetterneck T. U.S. physician satisfaction: a systematic review. Journal of Hospital Medicine 2009; 4(9): 560-568.
12. Yoon JD, Rasinski KA, Curlin FA. Conflict and emotional exhaustion in obstetrician-gynaecologists: a national survey. Journal of Medical Ethics 2010; 36(12): 731-735.
13. Willke RJ. Practice mobility among young physicians. Medical Care 1991; 29(10): 977-988.
14. Kletke PR. Physician workforce data: when the best is not good enough. Health Services Research 2004; 39(5): 1251-1256.
15. United States Department of Agriculture (USDA). Measuring rurality: rural-urban continuum codes. (Internet) 2004 Available: http://www.ers.usda.gov/Briefing/Rurality/RuralUrbCon/ (Accessed 11 June 2013).
16. United States Census Bureau. 2007-2011 American Community Survey 5-year estimates, Table B03002: Hispanic or Latino origin by race. Washington, D.C.: US Census Bureau, 2012.
17. Health Resources and Services Administration. Designated primary care health professional shortage areas. Washington, D.C.: United States Department of Health and Human Services, 2012.
18. United States Census Bureau. 2006-2010 American Community Survey 5-year estimates, Table B02001: Race, total population. Washington, D.C.: U.S. Census Bureau, 2011.
19. Bodenheimer T, Berenson RA, Rudolf P. The primary care-specialty income gap: why it matters. Annals of Internal Medicine 2007; 146(4): 301-306.
20. Bodenheimer T, Pham HH. Primary care: current problems and proposed solutions. Health Affairs 2010; 29(5): 799-805.
21. Spenny ML, Ellsbury KE. Perceptions of practice among rural family physicians - is there a gender difference? The Journal of the American Board of Family Practice 2000; 13(3): 183-187.
22. Spickard A, Gabbe SG, Christensen JF. Mid-career burnout in generalist and specialist physicians. Journal of the American Medical Association 2002; 288(12): 1447-1450.
23. Cutchin MP. Physician retention in rural communities: the perspective of experiential place integration Health & Place 1997; 3(1): 25-41.
24. Levinson W, Lurie N. When most doctors are women: what lies ahead? Annals of Internal Medicine 2004; 141(6): 471-474.
25. Saha S, Taggart SH, Komaromy M, Bindman AB. Do patients choose physicians of their own race? Health Affairs 2000; 19(4): 76-83.
26. United States Bureau of Labor Statistics (BLS). Occupational outlook handbook, 2014-2015 edition: nurse anesthetists, nurse midwives, and nurse practitioners. Washington, D.C.: U.S. Department of Labor, 2014.

