Introduction
Rural social workers face significant challenges in the delivery of their services to rural and frontier residents. The National Association of Social Workers (NASW) reported that the number of new social workers providing services to older rural adults is decreasing, despite projected increases in the number of older adults who will need social work services1. The people served have the same basic needs as their urban counterparts; however, they are older than the national average and have higher rates of non-insurance, while their access to technology and technical expertise is more limited2.
The Idaho Health Care Association/Idaho Center for Assisted Living (IHCA/ICAL) found that education programs specific to nursing home social services were infrequent and were not convenient to those in rural areas. Furthermore, a comprehensive training curriculum was not available to employees statewide. This article explores one approach to addressing this inequity: the delivery of continuing education to health professionals in skilled nursing facilities (SNF) in rural Idaho in the form of Virtual Grand Rounds (VGR). This also represents one contribution to addressing the rural social worker shortage.
Literature review
The published literature indicates there are both positive and negative aspects to the application of technology to distance learning. Among the positive aspects are that distance education provides greater flexibility and student convenience, improved access/interaction with the instructor, better grades, and a more positive learning experience3. The negative aspects of distance education include a reduction in face-to-face interaction, concerns over technology and logistics, increased student workload, and increased costs to the student3.
However, distance education research has been conducted primarily in educational settings and very limited research has been conducted on adult work populations4. Existing workplace research suggests that learner needs, technology support and workplace constraints are different from those in education settings5,6. In addition, there is now industry acknowledgement of the critical importance of lifelong learning, and the focus of training has shifted from teaching specific skills to supporting organizational strategic goals7-10. The research from this project is unique because it provides a bridge between the educational institution and a workplace population.
Background
In August 2001, the Idaho State University Institute of Rural Health received funding to improve access to quality health care for people in rural and frontier Idaho, with a secondary purpose to establish a statewide telehealth resource center. To accomplish these goals, a project was devised with three objectives, to: (i) increase the workforce through new and expanded education; (ii) extend the reach of the existing workforce through telehealth; and (iii) preserve the existing workforce through professional support, thus increasing health professional quality of life and retention, and reducing the negative effects of care-giving.
In November 2001 a 'request for proposal' was publicized state-wide to solicit potential project partners. Among the responses, the proposal from IHCA/ICAL and the Idaho Chapter NASW (IDNASW) stood out because it was from two non-profit, state-wide organizations and was not from a hospital or clinic.
The purpose of their proposal was to address the shortage of qualified social workers in rural Idaho. As background, in 2001 every Idaho SNF (or long-term care facility, or nursing home) was required to have at least one employee who provided social services to residents. According to federal and state law, SNF employees are required to be either licensed social workers or non-licensed employees, and the director of social services in each facility must be a social worker if the facility is licensed for 120 beds or more. In facilities with 119 beds or less (more common in rural Idaho), the non-licensed employees are commonly known as resident care coordinators and generally do not have formal social work training.
Whether licensed or not, these employees provide important advocacy for long-term care residents and are part of the interdisciplinary care plan team. The documentation required is often of a technical nature. The social worker or residential care coordinator must also be able to provide admission and discharge guidance to residents, families and other healthcare professionals.
Facilities throughout the state have experienced difficulties in locating and recruiting qualified social workers to fill SNF positions in rural areas. In addition, few social work programs in Idaho provide adequate training in nursing home social services, so specific initial training was required for any social worker employed. In 2000 and 2001 the IDNASW sought to change the law requiring all facilities to employ a social worker as the director of social services. After 2 years in the legislature a compromise was reached between IHCA/ICAL and IDNASW, such that a residential care coordinator would not be referred to as 'social worker', and that they undergo a formal training program.
In 2001 and 2003 IHCA/ICAL and IDNASW worked together and developed a training curriculum for nursing home social workers and residential care coordinators, and this was taught at the annual IHCA/ICAL conference. The training was invaluable for employees hired prior to the conference and for those who were able to participate in the conference. For employees hired throughout the year or who worked in smaller, rural facilities (where a lack of replacement staff meant they were unable to be absent from work for the period of the conference) this was not satisfactory. To address this problem, IHCA/ICAL and IDNASW joined Telehealth Idaho to create the VGRs for resident care coordinator training.
Rurality and Idaho health professional shortages
For the purposes of this article, the adopted definition of 'rural' is that of the Health Resources and Services Administration (HRSA) Shortage Designation Branch. The HRSA Shortage Designation Branch determines whether a geographic area, population group or facility is a Health Professional Shortage Area (HPSA). Such shortages may be of primary medical care, dental or mental health providers in urban or rural areas, population groups or medical or other public facilities11. All 44 counties in Idaho are classified as HPSAs for mental health.
More than 50% of the non-metropolitan populations of Idaho live at least 66 miles (106 km; straight-line distance) from the nearest tertiary healthcare facility, while 25% live at least 95 miles (153 km) and 10% live 106 miles (171 km) away from such a facility (pers. comm., Dr Jaishree Beedasy, 16 December 2008). The actual road distance traveled is even higher, and other factors such as slope, type of road, number of junctions, and weather conditions increase the physical complexities of accessing care.
The virtual grand rounds design and implementation
The VGRs were created to address the need for continuing education and to provide professional support for rural health professionals by bringing current evidence-based practice to the rural professional in their community12. Essentially, VGRs are grand rounds delivered by statewide interactive videoconference. Two-way communication allows participants sufficient interaction to gain as much detail as a topic warrants. As in medical grand rounds, specialist presenters (often located outside of Idaho) are assembled to provide current information on a topic, allowing rural professionals access to experts in a variety of fields. Through the VGR process, the IHCA/ICAL provided training to its rural facilities.
Telehealth Idaho used existing videoconference resources across the state and VGRs were delivered using a network approach with Internet Protocol (IP) and Integrated Services Digital Network (ISDN) connectivity. Idaho State University's distance education network links to five of the state's largest communities and to eight rural counties in southeast Idaho. Additionally, it connects to the North Idaho Rural Health Consortium, which services five northern rural hospitals. Telehealth Idaho provided the technical infrastructure and support with scheduling, registration, publicity, and data collection. It funded the cost-of-line charges for interactive videoconferencing and staff time to arrange, coordinate, and collect data on each session.
Methods
Between July 2002 and December 2006, 740 person-hours (359 attendees x 2.06 hours) of continuing education were delivered to resident care coordinators and social workers in nine sessions of VGRs. The intervention was evaluated using a questionnaire that consisted of 10 questions, measuring participant satisfaction level with a five-point Likert scale, and a comments section. Volunteer proctors distributed and collected attendance, basic demographic, and program evaluation forms at each site for each session and returned the data to Telehealth Idaho for analysis.
This Telehealth Idaho continuing education evaluation form was approved by Idaho State University's Human Subject's Committee.
The curriculum delivered via video conferences and in lecture format, was chosen from the components shown (Table 1).
Table 1: Resident Care Coordinator Curriculum Components
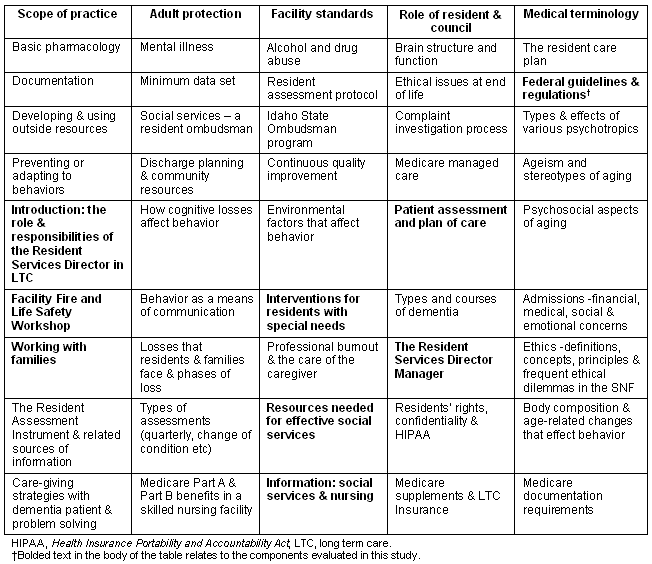
Results
In total, 283 evaluation forms (79% return rate) were collected on the quality of the presentation, the presenter's expertise and delivery, the relevance and value of the presentation to the attendee, and the quality of the technology. Programs and presenters consistently received very positive scores. Participants were pleased with the method of delivery. The overall participation satisfaction rating of the VGR was 4.1 (of a possible 5). When queried as to whether the information presented would lead to changes in practice, the participants responded positively with a score of 3.25.
For the first VGR on 23 July 2002, data were gathered differently from the remainder of the research. The summary statistics for 23 July 2002, and the remaining residential care coordinator VGR series from 25 October 2002 to 5 December 2006 are given in Tables 2 and 3.
Table 2: Class evaluation summary (30 of 60 students registered), 23 July 2002
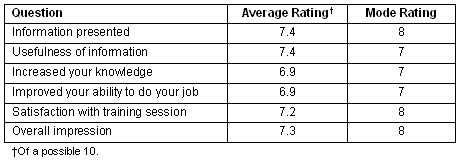
Table 3: Program evaluation - residential care coordinator VGR series, July 2002, and the remaining residential care coordinator VGR series from 25 October 2002 to 5 December 2006
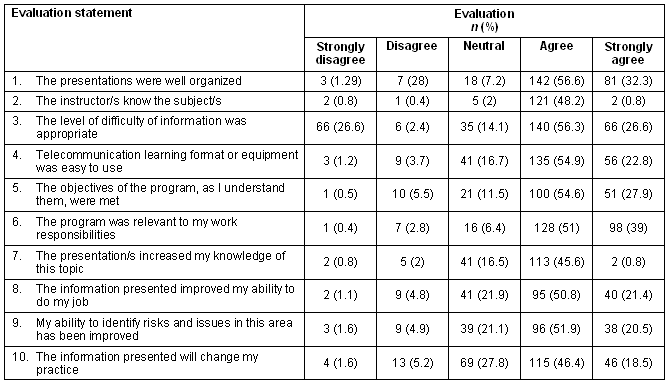
Discussion
Virtual Grand Rounds is a positive alternative to face-to-face traditional lecture-type learning, and it has the added bonus of reaching professionals at rural sites who are unable to travel to a centralized conference.
Although our results cannot show direct correlations between VGRs and benefits, the possible benefits include:
- More individuals trained, with an average of 90 participants per year
- Improvements in social services delivery
- Improved orientation and greater support for new social workers and residential care.
Because there are regional telehealth resource centers located throughout the USA, the VGR model of education and training could be adapted for and used in other states and regions. However, because technology develops rapidly, other distance learning technologies may have the potential to surpass the breath and depth of video conferencing in the foreseeable future.
Conclusion
The Telehealth Idaho program helped provide new rural healthcare employees with a more thorough training than they may otherwise have received. It also allowed IHCA/ICAL to deliver the training to existing rural healthcare employees who may not have been able to attend training at the annual conference. As a result SNF employees were no longer required to travel across this very large, rural state for training.
Because the training of social workers and residential care coordinators was so successful, the program was expanded to include other facility staff, and other VGR topics. As a result, an entirely new system and infrastructure of training was established for the benefit of long-term health care providers and patients in rural Idaho. At the very least, this represents one unique contribution to addressing the rural social worker shortage.
Acknowledgements
This project is supported by grant #1 D1B TM 00042-01 from the Department of Health and Human Services (DHHS) Health Resources and Services DHHS, Health Resources and Services Administration, Office for the Advancement of Telehealth. The contents of this article are the sole responsibility of the authors and do not necessarily represent the official views of DHHS.
References
1. Nadelhaft A. Landmark study warns of impending labor force shortages for social work profession: Services to Millions Threatened. (Online) 2006. Available: http://www.socialworkers.org/pressroom/2006/030806.asp (Accessed 16 December 2008).
2. University of Pittsburgh, Center for Rural Health Practice. Bridging the health divide: the rural public health research agenda (Online) 2004. Available: http://www.upb.pitt.edu/uploadedFiles/About/Sponsored_Programs/Center_for_Rural_Health_Practice/Bridging%20the%20Health%20Divide.pdf (Accessed 16 December 2008).
3. Valenta A, Therriault D, Dieter M, Mrtek R. Identifying student attitudes and learning styles in distance education. Journal of Asynchronous Learning Networks 2001; 5(2): 111-123.
4. Salas E, Kosarzycki C, Burke S, Fiore S, Stone D. Emerging themes in distance learning research and practice: some food for thought. International Journal of Management Reviews 2002; 4(2): 135-153.
5. Paulsson K, Sundin L. Learning at work a combination of experience-based learning and theoretical education. Behaviour and Information Technology 2000; 19(3): 181-188.
6. Stefanov K, Stoyanov S, Bujikiv R. Design issues of a distance learning course on business on the Internet. Journal of Computer Assisted Learning 1998; 14: 83-90.
7. Eamon DB. Distance education: has technology become a threat to the academy? Behavior Research Methods, Instruments, and Computers 1999; 31(2): 197-207.
8. Farber J. The third circle: on education and distance learning. Sociological Perspectives 1998; 41(4): 797-814.
9. Fulmer RM. The evolving paradigm of leadership development. Organizational Dynamics 1997; 25 (4): 59-72.
10. Salas E, Cannon-Bowers JA. The science of training: a decade of progress. Annual Review of Psychology 2001; 52: 471-499.
11. Health Resources and Services Administration. Shortage designation: HPSAs, MUAs & MUPs. (Online) 2008. Available: http://bhpr.hrsa.gov/shortage/index.htm (Accessed 16 December 2008).
12. Stamm BH, Rudolph JM. Changing frontiers of health care: Improving rural and remote practice through professional conferencing on the Internet. Journal of Rural Community Psychology 1999; E2 (1). Available: http://www.marshall.edu/jrcp/vole21/e21contents.htm (Accessed 16 December 2008).

