Introduction
Less than a century ago, rural populations living traditional lives had no problems related to high blood pressure (BP) and it has been erroneously assumed by many that the situation is unchanged. This is largely attributable to a lack of reliable data on BP levels in these settings. Recent reports have shown that high BP is no longer uncommon in rural settings in sub-Saharan African countries1. Cooper et al2 reported a high BP prevalence of 15.4% in rural Cameroon. A mean prevalence of approximately 16% has been reported in rural West African countries3. For those over 65 years, recent studies have shown a prevalence as high as between 30% and 40% in rural West Africa4.
There are limited data on BP profiles in Ghana, especially for the rural population. Studies undertaken in rural populations in the 1970s and 1980s generally reported a low prevalence of high blood pressure. In 1973, Pobee et al5 reported high BP prevalences of 2% to 5% for those in 20 rural Ghanaian villages. The study concluded that high BP was not a significant health problem in rural Ghanaians and that large scale programs for the control of high BP should therefore be limited to the urban populations. In the 1980s and 1990s, the prevalence of high BP in rural Ghanaian populations was reported as 4.1%5. However, in recent times a 2002 BP survey of two rural communities in the Volta Region of Ghana reported the prevalence of high BP to be 32.8%6; and a 2005 cross-sectional study of four rural communities in the Ga District of Ghana reported a high BP prevalence of 25.4%7.
The aims of this article were to measure BP levels, to determine the proportion of individuals with high blood pressure, to estimate the regression dilution factor in order to guide judgments about the likely distribution of usual blood pressures, and to assess associations with anthropometric and other variables putatively related to BP in a rural adult population in Northern Ghana.
Methods
Study area
The study was conducted in the Kassena-Nankana District (KND) of Northern Ghana. Ghana is a tropical country located on West Africa's Gulf of Guinea, a few degrees north of the Equator. Ghana borders Cote d'Ivoire to the west, Burkina Faso (formerly Upper Volta) to the north, Togo to the east and the Gulf of Guinea to the south, and has a total area of 238 540 km2. Of its estimated population of 19.7 million, almost one-third live in towns or cities. The literacy rate is 74.8%.
The KND is one of the eight districts in the northernmost part of Ghana with Navrongo as its commercial and political capital. It is a relatively flat area and covers 1675 km2. The rainy season extends from April to September and the prolonged and intensely hot dry season from October to March. Rainfall averages from 850 to 950 mm per year with the peak occurring in August. Daily mean temperatures range from 20ºC to 40ºC.
The mode of life is traditional with 90% of the inhabitants being small-scale subsistence farmers who depend mostly on the weather for their farming activities. In addition, women work at minor trading activities to supplement agricultural production. The population of the KND is largely dispersed but is also clustered in a few concentrated settlements. In 2006 the population was 143 742, approximately 40% of which was aged under 15 years and 4.9% was 65 years and over. Females constitute 53% of the population. The two main ethnic groups in the population are the Kassena (49%) and the Nankana (46%)8.
There is a district hospital located in Navrongo town and four health centres distributed regionally over the district. The mean minimum distance to a health facility is 4.6 km. In addition to the static health facilities, there are community-health nurses who have been retrained and deployed into some communities in the district to offer door-to-door health services to the people. Estimates of the prevalence of high BP are lacking and there is also generally lack of mortality and morbidity data on cardiovascular diseases and strokes. There are some hospital-based data but these are generally not reliable since death certification and causes of death are not consistently recorded.
Educational attainment in the district is low. About 66% of the population aged 15 years and above have never been to school and only 8% have attained senior secondary or higher levels of education8.
Study design and participants
Fieldwork was carried out in the KND from February to April 2007. A random sample of 600 participants was drawn from a population register, regularly updated by the Navrongo Demographic Surveillance System (NDSS), which is owned by the Navrongo Health Research Centre, a field station of the Health Research Unit of the Ghana Health Service. The NDSS is a continuous population registration system that assesses the demographic dynamics of the entire population of the KND. Every 90 days, all compounds in the district are visited to update vital events such as births, deaths, pregnancy, marriages and migration in and out. The sample size required (n = 531) was calculated according to an estimated prevalence of high BP of 5.9%9, with a precision of 2% and a confidence level of 95%. To this approximately 70 participants were added to compensate for refusals to participate, anticipated as approximately 10% to 15%.
The response rate was 95.7% with 207 males and 367 females completing the study protocol. The imbalance between the sexes in the random sample was due to females constituting the larger percentage of the population. The 26 non-respondents, all males, were either busy on their farms or not interested in participating. Participants with a previous diagnosis of high BP were not excluded from the study because they had either not been on any medication or had ceased taking their medication. Household salt consumption was also measured in 20 randomly selected households in the district.
Ethical approval was obtained from the local Institutional Review Board of the Navrongo Health Research Centre. The traditional chiefs, community leaders, political and opinion leaders were approached prior to commencement of the fieldwork and community meetings were held to explain the purpose of the study. Individual affirmations of informed consent were obtained from residents willing to participate using informed consent forms. The consent forms were signed by those who were literate and marked with the left thumbprint of those who were not.
Five field workers and a supervisor with prior experience and training in epidemiological surveys of this nature were recruited and retrained in all the techniques of questionnaire administration, anthropometric and BP measurements, according to standardized protocols. The study team were all local to the study area and were fluent in the local languages. Before commencing the fieldwork, each of the techniques and instruments was tested on a small sample of the population and was shown to be practicable, sufficiently reliable and valid.
Data were collected by interview using a simple structured questionnaire, and measurements were recorded on a standard form. For date of birth, an estimated date was assigned to those who were unable to give their exact dates of birth using the seasons, festivals and some historical indicators as guides. June 30th was allocated if the exact date and month could not be decided upon. All participants were visited in their homes by the field workers and subsequently invited on specific dates to attend the various health centres designated for data collection.
Weights were measured to the nearest kg in light clothing and without shoes using calibrated Salter scales (Salter Australia; Melbourne, VIC, Australia). Portable Leicester stadiometers (Invicta Plastics Ltd; Leicester, UK) were used to measure height to the nearest cm with the head in the Frankfurt position. Waist circumferences were taken with non-stretch tape measures and measured to the nearest 0.0 or 0.5 cm. Waist circumference was measured halfway between the lower border of the ribs and the anterior superior iliac spine. All the measurements were taken twice and the means used in the analyses.
Blood pressure measurements followed administration of questionnaire and anthropometric measurements. Blood pressure was measured in the right arm with participants in the sitting position. Reliable automatic BP devices (Omron MX3 Pus; Omron Healthcare; Kyoto, Japan) which are validated against the reference method of sphygmomanometry (ie has passed the validation recommendations of the International Protocol of the European Society of Hypertension10) were used by trained staff. Following the WHO MONICA methodology11, BP was measured twice and the mean of the two used in the analyses. The same trained staff made BP measurements in all locations.
As a result of within-person variability in BP values, baseline BP measurements do not often reliably indicate the long-term average or usual BP and this can underestimate its association with an end outcome such as cardiovascular disease. This is known as the regression dilution effect or bias. To correct for this regression dilution effect, repeat measurements of BP in a representative sample of the study participants can be used to obtain an estimate of the attenuation factor known as the regression dilution ratio (RDR). The RDR was determined using a non-parametric method as described by Clarke et al12. Repeat measurement data was collected for 89 of the study participants 2 weeks after taking the baseline measurements. After an open invitation was extended to all study participants to attend for re-measurement after 2 weeks, 89 participants presented. These subjects were placed into four quartiles on the basis of their first measurement. The mean systolic BP (SBP) was then calculated for each of these quartiles at baseline and on repetition. The means of the repeat measurements provide unbiased estimates of the usual levels of BP in each quartile. The ratio of the gap between the mean SBP of quartile 1 and quartile 4 on repeat measurement to that at baseline represents the RDR - the factor by which the standard deviation (SD) of the casual SBP measurements needs to be multiplied to determine the usual SBP distribution.
Salt consumption was also estimated in 20 single family households randomly selected from the survey area. Each family shared the same meals, ate the two or three main meals prepared and rarely bought ready-prepared meals. These were also mainly adult households; only three households contained children and these were aged over 10 years so they were counted as adults. A preliminary survey showed that most households bought just a small bag of salt, which was usually used within 5 to 7 days. Salt consumption over 4 days was measured by household inventories. The results, therefore, represented the usual salt consumption more adequately than a single 24 hour food record. Standardized weighing scales of 5 kg (accurate to 0.01 kg) were used to weigh household stocks, including their containers. The survey started with measuring opening stocks of salt before breakfast on the first day of surveillance. Closing stocks were measured on the fourth day before breakfast. Total consumption of each household was calculated as (inventory + new purchase) - remainder. The average salt consumption per day for each household was calculated by dividing the total consumption per each household by 3 days. The average salt consumption per individual per day was then calculated using the number of people in each household. A sample of the rock salt was sent to the Dunn Nutrition Unit (Diet & Cancer Group) of the Medical Research Council, Cambridge, UK to determine the Sodium (Na) concentration. Assays were conducted on 10 samples of 0.5g/100 ml solutions of the rock salt sample (after grinding in a coffee grinder) for Na concentration and the mean was then calculated. The Na concentration in the rock salt was measured using the technique of flame photometry13.
Definitions
Casual high BP was defined as an SBP ≥140 mmHg and/or diastolic BP (DBP) ≥ 90 mmHg measured on a single occasion. The BMI was calculated as weight (kg) divided by height (m2). Weight categories were defined based on the calculated BMI (kg/m2) according to the World Health Organization14. Underweight is defined as BMI ≤18.5; normal weight BMI = 18.5-24.99; overweight BMI = 25.0-29.99; obese BMI ≥30.0.
Statistical analysis
The data were coded and entered into a database using Statistical Package for Social Sciences Software v 15.0 (SPSS Inc: Chicago, IL, USA) for Windows and checked for range and internal consistency before analysis using the same package. The mean SBP and DBP were determined for both age and sex categories. Multiple linear regression analysis enabled age-adjusted comparisons of SBP and DBP levels to be made between males and females. Bivariate regression analyses were performed to assess associations with SBP. Multiple regression analyses were performed separately for males and females to assess the independent associations of predictor variables (waist circumference, BMI, age and time of BP measurement) with SBP and DBP. P-values <0.05 (two-sided) were considered statistically significant. All results were given as mean (standard deviation) unless indicated otherwise.
Results
Descriptive statistics
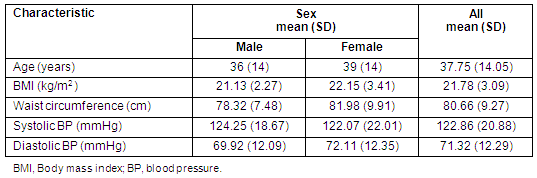
Table 1 shows the characteristics of the study population, anthropometrics and BP levels. In all, 75% of study participants were from the Kassim ethnic group; 72.0% were married and almost half (45.3%) had no formal education.
Mean BMI was 21.78 (3.09) kg/m2; 21.13 (2.27) and 22.15 (3.41) kg/m2 for males and females, respectively. Mean BMIs did not vary significantly with age. Of all participants, 75.4% were in the normal weight category.
Table 1: Summary characteristics of the population, anthropometrics and mean blood pressures by sex
Blood pressure levels
Overall prevalence of casual high BP was 19.3%. Table 2 shows age-specific mean (standard deviation) blood pressures for each sex. The SBP and DBP increased with age in both males and females. Tables 3 and 4 show age-specific mean SBP levels from reports of studies in various sub-Saharan African rural adult populations for comparison.
Table 2: Age and sex specific systolic and diastolic blood pressures
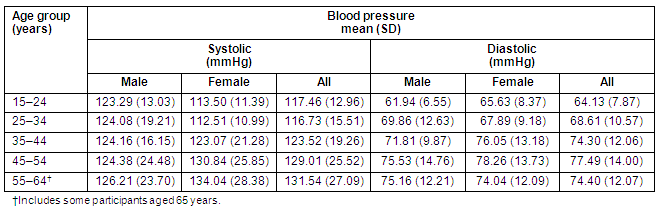
Table 3: Mean blood pressures in other studies of sub-Saharan rural adult African populations
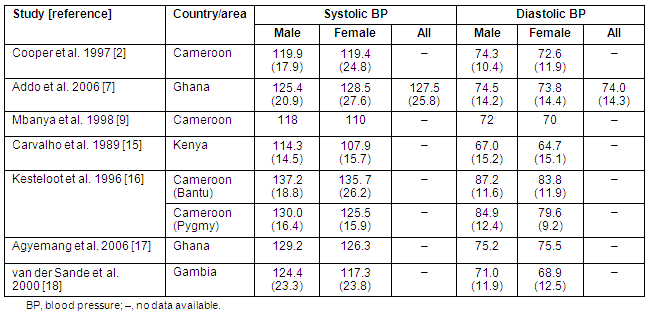
Table 4: Age-specific mean systolic blood pressures (SD) in sub-Saharan rural African populations in published studies

Univariate and multivariate associations with blood pressure
To assess factors associated with SBP, bivariate and multivariate regression models were developed. Linear regression analyses showed that SBP increased with increasing BMI, age and waist circumference. Systolic and diastolic BPs increased by 4.0 and 3.0 mmHg per decade, respectively. All regression coefficients were statistically significant (p <0.000).
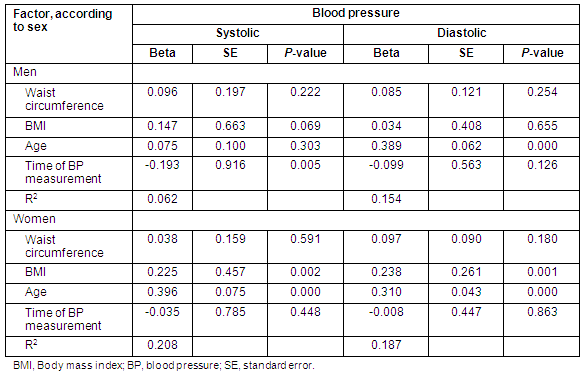
Table 5 shows independent contributions of factors associated with SBP and DBP. Both age and BMI were positively and independently associated with SBP and DBP in females, while age was positively and independently associated with DBP in males. Time of BP measurement made a negative independent contribution to SBP in males.
Table 5: Multiple regression analysis of factors associated with systolic and diastolic blood pressure, according to sex
Distribution of usual blood pressures and the regression dilution ratio
The overall mean SBP and DBP for the 89 participants changed from 125.66 (22.57) and 72.20 (12.35) mmHg, respectively, at baseline to 121.54 (19.55) and 70.53 (11.91) mmHg 2 weeks later. Apart from these changes, there were marked differences observed in the mean values of the repeat measurements after 2 weeks of the baseline-defined quartiles.
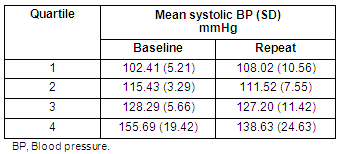
The mean SBP of participants who were in the top category of the four quartiles declined from 155.69 mmHg at baseline to 138.63 mmHg after 2 weeks. The mean for those in the bottom quartile increased from 102.41 mmHg to 108.02 mmHg after 2 weeks. The range for the mean baseline SBP values was 53.28 mmHg and 2 weeks later 30.61 mmHg yielding an RDR of 0.57 for SBP in this rural population. Table 6 shows the results of the analysis:
Table 6: Mean systolic blood pressure of 89 individuals measured on two occasions, arranged by quartiles on the basis of measured level on the first occasion
Salt consumption
The average amount of impure rock salt used per day per household was 46.53 g and the average household number was 3.92. The average amount of impure rock salt used per person per day therefore amounted to 13.07 g. The mean Na concentration for 0.5g/100 mL solution of rock salt sample was found to be 81.7 mmol/L. The average Na concentration being used per day per person came up to approximately 5.2 g which was equivalent to 12.5 g/day of (pure) salt.
Discussion
Blood pressure levels
The findings of BP levels and a high prevalence of high BP in rural Northern Ghana are broadly consistent with reports from other sub-Saharan rural populations2,3,7,9,15-18, although direct comparison is difficult because of a variation in techniques and the type of BP monitors used. A similar study conducted in 2006 in four rural communities in Ghana7 reported a mean SBP of 125 (25.8) mmHg and DBP of 74.0 (14.3) mmHg, which is comparable to the findings of the present study. The sex specific mean pressures are consistent with the results from rural populations in Ghana: Addo et al7 reported a mean SBP of 125.4 (20.9) and 128.46 (27.6) mmHg for males and females, respectively, and a mean DBP of 74.5 (14.2) and 73.8 (14.4) mmHg for males and females, respectively. Agyemang et al17 also reported 129.2, 126.3, 75.2 and 75.5 mmHg in the same order as above.
The age-specific mean BP levels in this study were also consistent with the findings of other studies19,20. There was an increase in SBP with age.
Predictor variables for BP evaluated
Several factors were identified as related to BP in this rural population. These included age, BMI and waist circumference. Blood pressure increased with age, BMI and waist circumference. Determinants for increasing BP in a similar study among a rural population in the Ashanti region of Ghana included increasing age and BMI1. Addo et al's7 study of four rural communities reported increasing BMI and age to be related to increasing BP.
The increase in BP with age is consistent with reports from other studies conducted in other Ghanaian populations1,19. Gone are the days when rural populations showed very little or no increase in BP with increasing age21.
The low mean BMIs for this rural population are consistent with the results of other studies conducted in sub-Saharan African rural populations2,7,9,15-18. Mean BMIs for females in other rural African populations ranged between 19.8 (3.0) and 23.9 (5.4) kg/m2, while that for males was between 19.8 (2.5) and 23.5 (3.1) kg/m2, which is also consistent with the finding in this study that mean BMI levels of males and females were not significantly different.
Regression dilution ratio
There were marked differences observed in the mean values at repeat measurements of participants sub-divided into quartiles on the basis of their baseline measurements. As expected, the baseline BP values had a wider distribution than the repeat BP measurements.
The RDR for SBP estimated was 0.57 which is comparable to the results of other studies22. The value of the RDR for SBP in this study indicates high within-person variability in SBP, which emphasizes the need to always take repeat measurements of BP after baseline in such population-based studies to correct appropriately for regression dilution.
Salt (Na) intake
The estimated amount of Na used per adult per day was 5.2 g, which is equivalent to 12.5 g of (pure) salt per day (on the assumption that all Na came from salt). This far exceeds current international recommendations of <5g salt per day23,24. Our estimates for salt consumption were subject to biases from the exclusion of stock cubes and salt-containing condiments for meal preparation, and failure to account for salt discarded in cooking water.
Salt intake has been associated with higher levels of BP and with more marked increases in BP with age25-27. In some developed countries, 80% of salt intake has been found to come from processed foods such as bread, pies, ready meals and takeaways28. As urbanization continues in sub-Saharan Africa, it is probable that salt consumption will increase due to increased patronage of processed foods. This rural populace still relies on a predominantly traditional 'healthy' diet but their use of salt in cooking, at the table and to preserve fish and meat is common.
There is reliable evidence that a reduction in salt intake reduces BP and that people of black African origin respond well to this strategy. Two short-term clinical trials conducted in Nigeria and Jamaica recently showed the effectiveness of a reduction in salt in lowering BP levels23,29. A community program conducted by Cappuccio et al19 in the Ashanti region of Ghana showed that a reduction in average salt intake led to a small but worthwhile reduction in BP. Current recommendations on salt intake for the prevention of cardiovascular disease is <5 g per day (<2 g/day of Na) or, for persons with high BP, African Americans and middle-aged or older adults, <3.6 g of salt per day23,24.
Study limitations
Our study was subject to multiple potential biases. The use of the automated BP device (Omron MX3 Plus) as opposed to the random-zero sphygmomanometer recommended by the WHO MONICA protocol11 may have introduced measurement biases. However the Omron MX3 Plus used has been validated against the reference method of sphygmomanometry and has passed the validation recommendations of the International Protocol of the European Society of Hypertension, making it eligible for use in epidemiological surveys10. Validated automated electronic BP devices may actually improve reliability and reproducibility of BP measurements2. The measurements were also regularly standardised against mercury sphygmomanometers to check for any drifts.
While estimation of the waist : hip ratios would have been relevant for further understanding the epidemiology of BP in this population, this was not possible due to cultural and religious concerns. Only waist circumferences were therefore measured. The salt consumption survey was conducted on only 20 randomly selected households; a larger sample would have made the results more representative. Ideally 24 hour urine collections to measure Na excretion would have been the best way to accurately estimate salt (Na) consumption.
Issues in the descriptive epidemiology of blood pressure
'Casual' (or baseline) BP is BP measured on a single occasion, while 'usual' BP is estimated by averaging readings over several occasions. For groups and populations, mean 'casual' BPs are unbiased estimators of mean 'usual' BPs. An individual diagnosis of high BP cannot be made based on casual blood pressures; it can only be made after repeated measurements.
Previous WHO guidelines gave the cut-off level for high BP as a usual SBP ≥160 mmHg and/ or a usual DBP ≥95 mmHg. This was changed in 1998 to a usual SBP ≥140 mmHg and/ or usual DBP ≥90 mmHg. Evans and Rose30 proposed the seemingly pragmatic definition of high BP as the level of BP above which treatment does more good than harm. This definition, when applied to BP levels in isolation, also has its short-comings; the associated absolute risk is not taken into account. Though the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation and Treatment of High BP (JNC VII) still does not embrace an absolute risk approach in addition to the level of BP to guide treatment, compared with its previous version, the WHO and European guidelines now emphasise the importance of an absolute risk approach in cardiovascular disease interventions31,32.
There have been suggestions about the need to set different thresholds for different populations because risk factor levels and disease risk varies in different populations. Very little data exists on what constitutes an appropriate threshold in African populations. Law and Wald33 suggested that everyone at high risk of cardiovascular disease should be targeted instead of imposing risk-factor thresholds in cardiovascular disease intervention. They examined seven dose-response relations between physiological variables and risk of disease. It was realised that a given absolute change in a risk factor reduces the risk of disease by a constant proportion, irrespective of the starting level of the risk factor. The best predictors of risk of cardiovascular disease are the risk factors that cannot be changed, such as age and sex, and therefore interventions should be determined by a person's level of risk and not by the level of risk factors. Therefore BP lowering drugs should not only be limited to people with high BP because offering treatment only to those who have high values of the risk factors mean targeting a small percentage of the population destined to suffer a disease event. It has been suggested that there may be a lower threshold for target organ damage in African populations, implying that BP lowering medication should be initiated earlier34. This is a topic for continuing investigation.
Implications for the study
Major implications for studies of this kind include difficulties in interpreting the proportion of the population with high BP, which hampers the comparability of studies, especially with regard to prevalence of high BPs, because of different definitions used and a weakening of the association of BP with risk. Despite the various implications, such studies are still needed in order to provide an indication of the distribution of BPs in populations that were previously thought to be at no risk of cardiovascular diseases and related mortalities.
Conclusion
Findings from the Northern Ghana Blood Pressure Survey show that prevalence of high BP and mean BPs are consistent with the findings of similar studies conducted recently in rural communities in sub-Saharan Africa. This cross-sectional survey provides a baseline against which future changes can be compared, considering the paucity of data on BP levels and factors associated with increased BP in this West African rural population.
This study identifies a need to prevent increasing BP contributing to a major increase in associated health burdens. The problem of excessive salt consumption needs to be addressed. Because salt is added to food by the consumers themselves (they have little dependence on processed foods), health education programs are needed to specifically target reducing salt intake.
Acknowledgements
The authors are very grateful to Dr Patrick Ansah of the Navrongo Health Research Centre; the study would not have been possible without him. The authors are also grateful to Dr Abraham Hodgson and Rufina Asuru for their great assistance during data collection. Thanks are also extended to the field workers, their supervisor, the study participants and all who contributed to making the study possible.
References
1. Agyemang C, Bruijnzeels MA, Owusu-Dabo E. Factors associated with hypertension awareness, treatment, and control in Ghana. Journal of Human Hypertension 2006; 20: 67-71.
2. Cooper R, Rotimi C, Ataman S, McGee D, Osotimehin B, Kadri S et al. The prevalence of hypertension in seven populations of West African origin. American Journal of Public Health 1997; 87: 160-168.
3. Cooper R, Rotimi C. Hypertension in blacks. American Journal of Hypertension 1997; 10: 804-812.
4. Steyn K, Gaziano TA, Bradshaw D, Laubscher R, Fourie J. Hypertension in South African adults: results from the Demographic and Health Survey, 1998. Journal of Hypertension 2001; 19: 1717-1725.
5. Pobee JO, Larbi EB, Belcher DW, Wurapa FK, Dodu SR. Blood pressure distribution in a rural Ghanaian population. Transactions of the Royal Society of Tropical Medicine and Hygiene 1977; 71: 66-72.
6. Burket BA. Blood pressure in two communities in the Volta Region, Ghana, West Africa. Ethnicity & Disease 2006; 16(1): 292-294.
7. Addo J, Amoah AGB, Koram KA. The changing patterns of hypertension in Ghana: A study of four rural communities in the Ga District. Ethnicity & Disease 2006; 16(4): 894-899.
8. Navrongo Health Research Centre. Navrongo Health Demographic Surveillance Report 2006. Navrongo: NHRC, 2006.
9. Mbanya JC, Minkoulou EM, Salah JN, Balkau B. The prevalence of hypertension in rural and urban Cameroon. International Journal of Epidemiology 1998; 27: 181-185.
10. Coleman A, Freeman P, Steel S, Shennan A. Validation of the Omron MX3 Plus oscillometric blood pressure monitoring device according to the European Society of Hypertension International Protocol. Blood Pressure Monitoring 2005; 10(3): 165-168.
11. MONICA Manual. Part III: Population Survey. (Online) 1997. Available: http://www.ktl.fi/publications/monica/manual/part3/iii-1.htm (Accessed 15 February 2009).
12. Clarke R, Shipley M, Lewington S, Youngman L, Collins R, Marmot M et al. Underestimation of risk associations due to regression dilution in long-term follow-up of prospective studies. American Journal of Epidemiology 1999; 150: 341-353.
13. Harris DC. Quantitative Chemical Analysis. New York: WH Freeman and Company, 1995; 21.
14. Spencer C, Lip G. Epidemiology of hypertension and risks. Pharmaceutical Journal 1999; 263: 280-283.
15. Carvalho JJ, Baruzzi RG, Howard PF, Poulter N, Alpers MP, Franco LJ et al. Blood pressure in four remote populations in the Intersalt Study. Hypertension 1989; 14: 238-246 .
16. Kesteloot H, Ndjitoyap N, Sasaki S, Kowo M, Seghers V. A survey of blood pressure in Pygmy and Bantu populations in Cameroon. Hypertension 1996; 27: 108-113.
17. Agyemang C. Rural and urban differences in blood pressure and hypertension in Ghana, West Africa. Public Health 2006; 120: 525-533.
18. Van der Sande MA, Milligan PJ, Nyan OA, Rowley JT, Banya WA, Ceesay SM et al. Blood pressure patterns and cardiovascular risk factors in rural and urban Gambian communities. Journal of Human Hypertension 2000; 14: 489-496.
19. Capuccio FP, Micah FB, Emmett L, Kerry SM, Antwi S, Martin-Peprah R. Prevalence, detection, management, and control of hypertension in Ashanti, West Africa. Hypertension 2004; 43: 1017-1022.
20. Poulter NR, Khaw KT, Hopwood BEC, Mugambi M, Peart WS, Rose G. Blood pressure and associated factors in a rural Kenyan community. Hypertension 1984; 6: 810-813.
21. Shaper AG, Wright DH, Kyobe J. Blood pressure and body build in three nomadic tribes of northern Kenya. East African Medical Journal 1969; 46: 273-281
22. Lewington S, Thomsen T, Dacidsen M, Sherliker P, Clarke R. Regression dilution bias in blood total and high-density lipoprotein cholesterol and blood pressure in the Glostrup and Framingham prospective studies. Journal of Cardiovascular Risk 2003; 10(2): 143-148.
23. World Health Organization. Diet, nutrition and the prevention of chronic diseases. Report of a Joint WHO/FAO Expert Consultation. Geneva: World Health Organization; 2003.
24. World Health Organization. Reducing Salt intake in populations. Report of a WHO Forum and Technical Meeting. Geneva: World Health Organization; 2007.
25. Stamler J, Rose G, Elliot P, Dyer A, Marmot M, Kesteloot H. Findings of the international cooperative INTERSALT study. Hypertension 1991; 17(Suppl): I9-15.
26. Stamler J, Elliot P. Commentary: Evidence on salt and blood pressure is consistent and persuasive. International Journal of Epidemiology 2002; 31(2): 316-319.
27. Obarzanek E, Proschan MA, Vollmer WM, Moore TJ, Sacks FM, Appel LJ et al. Individual blood pressure responses to changes in salt intake: results from the DASH-Sodium Trial. Hypertension 2003; 42(4): 459-467.
28. World Health Organization. The World Health Report - Preventing Risks, Promoting Healthy life. (Online) 2002. Available: http://www.who.int/mediacentre/releases/pr83/en (Accessed 15 July 2007).
29. Forrester T, Adeyemo A, Soarres-Wynter S, Sargent L, Bennet F, Wilks R et al. A randomized trial on sodium reduction in two developing countries. Journal of Human Hypertension 2005; 19: 55-60.
30. Evans V, Rose GA. Hypertension. British Medical Bulletin 1971; 27: 32-42.
31. World Health Organization. International Society of Hypertension Guidelines for the Management of Hypertension. Journal of Hypertension 1999; 17: 151-183.
32. European Society of Hypertension. European Society of Cardiology Guidelines for the Management of Arterial Hypertension. Journal of Hypertension 2003; 21: 1011-1053.
33. Law MR, Wald NJ. Risk factor thresholds: their existence under scrutiny. BMJ 2002; 324: 1570-1576.
34. Chaturvedi N, McKeigue PM, Marmot MG. Resting and ambulatory blood pressure differences in Afro-Caribbeans and Europeans. Hypertension 1993; 22: 90-96.

