Introduction
Videoconferencing technology first appeared in the early 1980s when interactive video systems based on analogue television were used by clinicians to broadcast live telemedicine demonstrations, also known as telelectures, to remote lecture theatres1-2. As digital technology has rapidly developed, the use of videoconferencing in health care has become more affordable and readily accessible within both educational and clinical facilities2.
The advantageous aspects of videoconferencing, such as enabling live interaction among geographically dispersed professionals1,3, has highlighted the potential of such technology in the development of learning communities4,5. The purpose of this article was to present the findings from a survey of a videoconference community of professional development.
Videoconferencing and professional development
Healthcare professionals in rural and remote areas of Australia are faced with challenges in their access to professional development. Geographical isolation often influences the ability for healthcare professionals to interact with colleagues, and greatly reduces opportunities to participate in educational activities. It is believed that such factors are influential in attracting and retraining healthcare professionals in rural and remote areas6.
Videoconferencing is therefore becoming a valued method for delivering continuing education opportunities to healthcare practitioners in rural and remote communities. Despite a paucity in the literature regarding the use of videoconferencing in healthcare professional development, the use of this technology is estimated to be increasing rapidly in conjunction with increased availability of and access to digital and audio technology. In Australia, for example, the use of videoconferencing to promote multidisciplinary interactive discussions between healthcare members of child development services in Queensland and Northern New South Wales (NSW) increased from two sessions per year in 2001 to 49 sessions in 20047.
Reported evaluations of the use of videoconferencing in the delivery of education and professional development for healthcare professionals in Australia have similarly illustrated high participant satisfaction and reduced professional isolation6,8,9. In Western Australia, a videoconferencing training initiative provided educational opportunities for those working with at-risk young people in rural areas8. Over 70% of the 18 participants gave overall high satisfaction ratings and consultation between agencies was enhanced with all participants agreeing that the training had influenced their initiative to seek consultative support. A Queensland survey of 166 clinicians (83% of attendees) who attended educational clinical forums provided by mobile videoconferencing units indicated very high satisfaction ratings for both content and transmission quality9. Eighty-eight percent of participants agreed that the sessions were relevant, 90% agreed that new content was provided, and 91% indicated that the video quality was acceptable. In addition, the mobility aspect of the videoconferencing units enabled sessions to be conducted in hospital wards, facilitating high attendance of clinicians. More recently, the evaluation of a series of national interactive videoconference seminars for the continuing professional development for rural psychiatrists throughout Australia highlighted the seminars' effect on reducing feelings of professional isolation6. Other positive feedback in this evaluation included 90% of respondents agreeing that the seminars permitted interaction between presenter and audience. The interactive component of videoconferencing was also rated highly in a Canadian study of 593 rural practitioners participating in professional development delivered by videoconferencing technology10.
International studies evaluating the use of videoconferencing in the delivery of continuing education to healthcare professionals have, in addition to highlighting participant satisfaction, detailed less desirable aspects to the use of the technology. Allen et al11 for example, conducted a study in Canada with the aim of evaluating the feasibility, acceptability, effectiveness, and cost of conducting practice-based continuing education using videoconferencing technology. While the videoconferencing format was well accepted by participants, the facilitator found that discussions were hindered by technical aspects such as poor audio and visual quality and audio lag. Layout and seating positions of participants were also identified as problematic, when in some sessions participants could not been seen by the facilitator. Technical problems resulted in delayed start times and the difficulty with connection at one site resulted in a missed module. The authors concluded that while videoconferencing may be efficacious under study conditions (because post-tests revealed evidence of knowledge gain), its effectiveness in practice is unknown. Similar technical hindrances have been highlighted in studies evaluating the use of videoconferencing in nursing education12-14.
The advantageous aspects of videoconferencing technology delivery of education and professional development has influenced the use of technology in the development of learning communities. The concept of 'learning communities' is educational, and has been described as a 'powerful means of creating and sharing new knowledge'5. A learning community is a group of individuals with a common interest, whose learning needs are addressed in trusting collaborative relationships; group values and new knowledge are constructed through social interaction5. Using videoconferencing technology, a learning community has the potential to include professionals from both isolated and metropolitan areas, whose live interaction with colleagues is collaborative and educational. The aim of this article was to present the findings of a survey of a videoconference community in NSW, Australia in 2008.
Setting
The videoconferencing symposium aimed to build a learning community among leading academics, researchers and clinicians in a more accessible way than by attendance at traditional conferences. The symposium involved four sites in NSW. Three sites were within North Sydney Central Coast Area Health Service (NSCCAHS; at Macquarie Hospital, Wyong Hospital, and Gosford Hospital), and one site was within Greater Western Area Health Service (GWAHS; at Broken Hill Hospital).
The Macquarie Hospital had had a regular program of symposia for more than 3 years. In 2007/2008 discussions between NSCCAHS senior nursing staff and GWAHS (responsible for local and regional educational programs) identified an opportunity to share resources among sites. The difficulties health professionals in rural and remote communities experience in accessing continuing education has long been recognised15, and attempts to video-conference the Macquarie symposia had met with limited success. It was recognised that improving linkages required more extensive preparation.
Further, Birden and Page16 stated the importance of etiquette, teaching methods and technological testing and back-up to enable quality educational opportunities. To foster interactivity the continuing education was delivered from different sites with Macquarie Hospital and Broken Hill Hospital each delivering sections of the symposium. Technical preparation was led by NSCCAHS conferencing and media staff, identifying and liaising with counterparts at the other sites. Technological equipment defined the potential number of participating sites. Site facilitators were identified and briefed. Speakers were provided with guidelines on etiquette and teaching methods. Technical rehearsals were held prior to the event.
Method
All attendees were given a survey to complete and return to a site facilitator at the end of the day. The survey was based on Salmon's principals of building online communities. Salmon17 began studying and practising the art of online teaching, also known as 'e-moderating', in the late 1980s when information and communication technology was primitive. Salmon was inspired to create a model for training and development from action research that investigated the use of computer mediated communication. Salmon's five-stage model, in addition to providing insight into what happens in online communities, forms a scaffolding for individual development using a constructivist approach17.
The first stage relates to access and motivation. This involves the prerequisites for conference participation, individual access and participation ability. Stage 2 concerns online socialisation and involves the establishment of individual identities and interaction with others. Stage 3 is concerned with information exchange, where there is a focus on the giving and receiving of information. During the first three stages co-operation between participants is required where each person is supported. Stage 4 relates to knowledge construction. It is at this stage that interaction becomes more collaborative. This stage reflects communication among group members that is based on common understandings. The fifth and final stage relates to development. Participants reflect on the learning process and seek personal achievement of goals. Participants reach this stage when they are using a constructivist approach to learning.
In the present research, questions were categorised into four stages identified and adapted from Salmon's model17: (i) access and motivation; (ii) socialisation; (iii) information exchange; and (iv) knowledge construction. Salmon's fifth stage (development) was not included as it was considered beyond the scope of the symposium. Participants rated statements using a four-point Likert scale: disagree, partly disagree, partly agree and agree. The results were entered into Microsoft Excel to generate descriptive statistics and their visual representations.
Ethical considerations
Participant completion of the survey was deemed to imply consent, therefore ethical approval was not sought. Participation in the event was not contingent on willingness to complete the survey.
Results
Sample
The participating site with the largest attendance was Macquarie Hospital based at North Ryde in NSCCAHS. This site had a total of 46 individuals at the videoconference, and 27 completed a survey (response rate 58.7%). The site's respondents comprised 48.2% of all respondents. A 100% response rate was achieved at the remaining three sites. The site with the lowest number of respondents was Gosford Hospital with three attendees (5.4%). Wyong Hospital had 15 attendees (26.8%), and Broken Hill Hospital 11 attendees (19.6%). The total response rate was 55%.
Demographic data
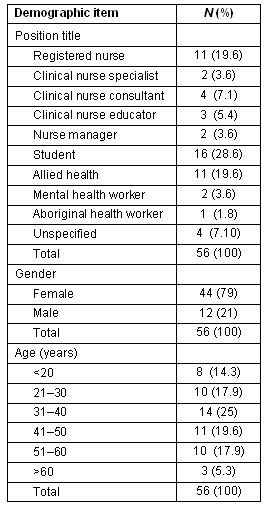
Table 1 outlines respondents' position titles, gender and ages. The majority were nurses or pre-registration nursing students (67.9%, n = 38), of which 79% (n = 44) were female. The most frequent age range was 31-40 years (n = 14, 25%).
Table 1: Demographic data of survey respondents
Survey results
The majority of respondents (n = 34, 60.7%) had attended less than 2 video presentations previously; 19.6% (n = 11) had attended 3-4 video presentations; 5.4% (n = 3) had attended 5-7 presentations; while 14.3% (n = 8) had attended more than 7 video presentations.
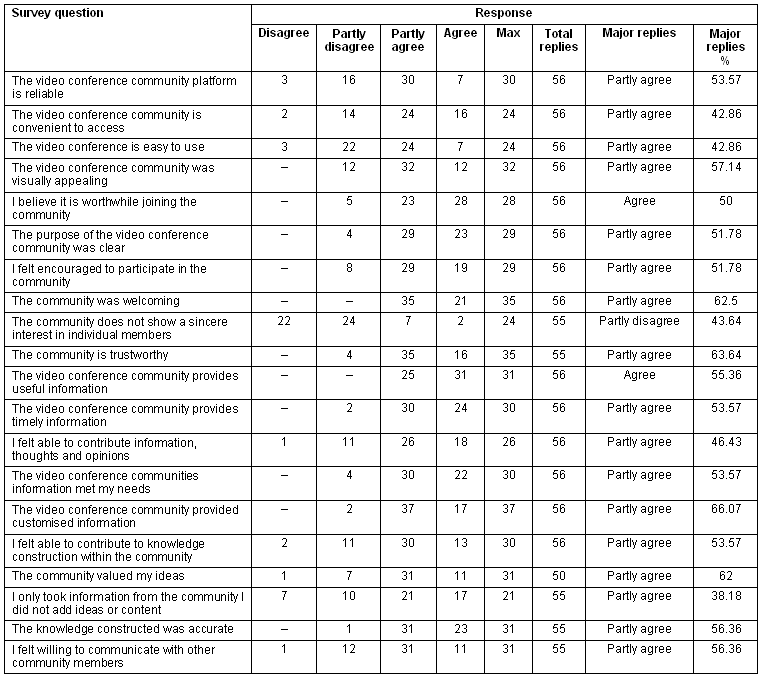
The survey was categorised into four stages; access and motivation, socialisation, information exchange, and knowledge construction. Survey questions and responses are detailed (Table 2).
Table 2: Survey questions and responses
Access and motivation
The majority of respondents agreed or partly agreed that the video conference community platform was reliable (n = 37, 66.1%), that the community was visually appealing (n = 44, 78.6%) and that the video conference community was convenient to access (n = 40, 71.4%). While the majority of respondents agreed or partly agreed that the video conference was easy to use (n = 31, 55.4%), a notable group disagreed or partly disagreed with this statement (n = 25, 44.6%). Almost all respondents (n = 51, 91%) agreed or partly agreed that joining the community was worthwhile.
Socialisation
Respondents reported that they agreed or partly agreed that the purpose of the videoconference community was clear (n = 52, 92.9%), that they were encouraged to participate (n = 48, 85.7%), and that the community was trustworthy (n = 51, 92.7%). The majority of respondents partly disagreed or disagreed that the community did not show a sincere interest in members (n = 46, 83.6%) and 100% of respondents (n = 56) agreed or partly agreed that the community was welcoming.
Information exchange
All 56 respondents agreed or partly agreed that the videoconference community provided useful information. The majority of respondents (n = 54, 96.4%) agreed or partly agreed that the videoconference community provided both timely and customised information. A large number of respondents (n = 52, 92.9%) agreed or partly agreed that their needs were met and that they felt able to contribute information thoughts and opinions (n = 44, 78.6%).
Knowledge construction
While 98.2% (n = 54) of the respondents agreed or partly agreed that the information was accurate and 76.4% (n = 42) agreed or partly agreed that they felt willing to communicate with other community members, a large number of respondents (n = 38, 69.1%) agreed or partly agreed that they only took information and did not add ideas or content. The majority of respondents (n = 43, 76.8%) agreed or partly agreed that they felt able to contribute to knowledge construction within the community and 84% (n = 42) agreed or partly agreed that the community valued their ideas.
Discussion
Despite intensive preparation, on the actual day a range of technological difficulties occurred. These included a temporary loss of the visual link with Broken Hill and Wyong, which impacted on the timing of the symposium. Additionally, there were limitations to the ability for those on screen to see the full audience at the larger site (Macquarie Hospital). The large audience at this site also meant that questions from the audience had to be restated by the speaker or site convener in order for all community members to hear. These limitations have been experienced previously11-14, and the present survey responses indicated a small number of participants were dissatisfied in relation to access issues.
Other features impacted on the spontaneous interaction of the learning community. For instance, the site technological co-ordinator at Macquarie Hospital unexpectedly took on the role of directing question opportunities among sites. Anecdotally this is a not an uncommon convention in video-conferencing, but it curtails spontaneity and provides an additional barrier to direct interaction in the learning community.
The videoconference had a number of successes. All respondents were partially or fully in agreement that the videoconference community was welcoming and that useful information was provided, as has been experienced elsewhere11.
The videoconference community aimed for the construction of new ideas through discussion stimulated by the presenters. However 69.1% of respondents indicated that they only consumed information and did not add new ideas or content, even though 76.8% reported feeling able to contribute to knowledge construction. This suggests that despite the attempt at creating an interactive approach to the development of knowledge, a significant proportion of respondents only passively received knowledge from the environment. This outcome is similar to the findings of Allen et al11.
Limitations
The convenience nature of the sample and a response rate of 55% must be factored into the interpretation of survey results.
Conclusion
Videoconferencing technology has the potential to enable rural and remote healthcare professionals to participate in a community for professional development. Common limitations to the technology cited in the literature relate to technical problems and difficulty in achieving a fully interactive environment. While both these elements were identified in the present survey, the inevitable technical difficulties were minimised by thorough preparation, rehearsals and the presence of technicians. The videoconference was an overall success, with respondents indicating generally positive results across the four areas of the survey. However the attempted move towards knowledge construction was not successfully achieved, despite the encouragement of an interactive environment. Further research is required to fully understand this phenomenon; however, a more naturalistic approach to communication that avoids a mediator at each site repeating questions and channelling information may be productive.
References
1. Cannavina G, Stokes CW, Cannavina C. Evaluation of video-conferencing as a means to facilitate outreach and work based learning. Work Based Learning in Primary Care 2004; 2: 136-47.
2. Sackett K, Campbell-Heider N, Blyth JB. The evolution and evaluation of videoconferencing technology for graduate nursing education. Computers, Informatics, Nursing 2004; 22: 101-106.
3. Kaufman DM, Brock H. Enhancing interaction using videoconferencing in continuing health education. Journal of Continuing Education in the Health Professions 1998; 18: 81-85.
4. Daley LK, Spalla TL, Arndt MJ, Warnes A. Videoconferencing and web-based conferencing to enhance learning communities. Journal of Nursing Education 2008; 47: 78-81.
5. Kilpatrick S, Barrett M, Jones T. Defining learning communities. (Online) 2003. Available: http://www.aare.edu.au/03pap/jon03441.pdf (Accessed 25 February 2009).
6. Greenwood J, Williams R. Continuing professional development for Australian rural psychiatrists by videoconference. Australasian Psychiatry 2008; 16: 273-276.
7. Bailey MA, Smith AC, Fitzgerald A, Taylor E. Delivery of child development services by videoconferencing: a review of four years' experience in Queensland. Journal of Telemedicine and Telecare 2005; 11: S2:1-3.
8. Haythornthwaite S. Videoconferencing training for those working with at-risk young people in rural areas of Western Australia. Journal of Telemedicine and Telecare 2002; 8(Suppl3): 29-33.
9. Harris V, Smith AC, Armfield NR. Education for regional health professionals using mobile videoconferencing. Journal of Telemedicine and Telecare 2007; 13(Suppl3): 44-47.
10. Klein D, Davis P, Hickey L. Videoconferences for rural physicians' continuing health education. Journal of Telemedicine and Telecare 2005; 11(Suppl1): 97-99.
11. Allen M, Sargeant J, Mann K, Fleming M, Premi J. Videoconferencing for practice-based small-group continuing medical education: feasibility, acceptability, effectiveness, and cost. The Journal of Continuing Education in the Health Professions 2003; 23: 38-47.
12. Chandler G, Hanrahan P. Teaching using interactive video: creating connections. Journal of Nursing Education 2000; 39: 73-80.
13. Martin P, Klotz L. Implementing a nursing program via live interactive video. Nurse Educator 2001; 26: 187-190.
14. MacIntosh J. Learner concerns and teaching strategies for videoconferencing. Journal of Continuing Education in Nursing2001; 32: 260-265.
15. Curran V, Fleet L, Kirby F. Factors influencing rural health care professionals' access to continuing professional education. Australian Journal of Rural Health 2006; 14: 51-55.
16. Birden H, Page S. Teaching by videoconference: a commentary on best practice for rural education in health professions. Rural and Remote Health 5: 356. (Online) 2005. Available: www.rrh.org.au (Accessed 6 April 2009).
17. Salmon G. Moderating - the key to teaching & learning online, 2nd edn. London: Taylor & Francis, 2003.
