Introduction
Internationally, the prevalence of long-term health conditions is at epidemic proportions, placing considerable emphasis and responsibility on health systems and on the broader community for prevention, management and treatment of the effects and impacts of this disease burden1. Nationally, more than 80% of premature mortality, morbidity, disability, injury and health care expenditure is due to chronic disease and injury1, a burden that has already exceeded previous predictions to 20202. Addressing the increasing burden of chronic disease has been prioritised on the Australian national agenda since 20043, with specific strategies to encourage collaborative, multidisciplinary and multi-agency approaches to the identification and management of long-term conditions3,4, including recent, targeted efforts in the primary health sector5.
International literature6 suggests significant health and other system changes are required for the care of people with long-term health conditions, including promoting active consumer involvement and self-management. Evidence7 for the latter is strong in reducing unplanned hospital admissions and/or length of stay in hospital, more efficient use of health professionals' time and improved self-care capacity and skills8. Evidence for positive health outcomes is controversial. While many studies, including randomized control trials, demonstrate benefits, some systematic reviews have concluded that positive health outcomes have only been demonstrated for people with diabetes and hypertension, and not for those with arthritis9,10. However, these reviews have been selective in their outcomes of interest11 examining biomedical outcomes only, deliberately excluding outcomes such as quality of life, self-efficacy and activity participation.
In Australia, policy2 and priority action funding responses12 have reflected this evidence, although implementing changes poses significant challenges11. The purpose of this article is to report both the processes of implementation and patient outcomes following the introduction of the Stanford Chronic Disease Self-Management Program (CDSMP) into an existing service in a rural setting.
Description and implementation of the Chronic Disease Self-Management Program
During the period 2005 to 2007 a series of innovative service approaches to the management of long-term conditions, including a pilot Stanford Chronic Disease Self Management Program13 was implemented by the South West Area Health Service (WACHS-SW) in the south west of Western Australia (during 2006 the South West Area Health Service became part of the WA Country Health Service [WACHS], to become WACHS-SW. The term WACHS-SW is used in this article).
A total of seven health professionals and three lay (peer) leaders were trained in the CDSMP, and 3 courses were offered between November 2005 and February 2007. The first 2 courses were jointly lead by a health professional and a peer leader. The last was lead by two health professionals because the lay leader was unavailable.
Three main recruitment strategies were used to promote the program in the catchment area:
- General practitioners: by briefing sessions, 2 direct mail-outs including a referral template, and fortnightly information faxes.
- Community: by 2 newspaper articles, 8 community presentations and 4 information stands at 3 shopping centres, all of which provided access to a template for self-referral. (Medical confirmation of a chronic condition following self-referral was not required. Condition inclusion criteria were not specified, although type 2 diabetes and congestive heart failure were highlighted as priorities in all recruitment communications).
- WACHS-SW staff: by 2 staff briefings, numerous meetings with site management, informal conversations and information on the health service intranet.
Exact enrolment rates (ie the number of people who participated in courses compared with the number who expressed interest) cannot be calculated due to the wide range of formal and informal strategies utilised. However, it was estimated that of the 100 potential participants spoken to, 33 enrolled and 21 attended the 3 courses. No referrals came from GPs.
Methods
Evaluation of the Chronic Disease Self-Management Program
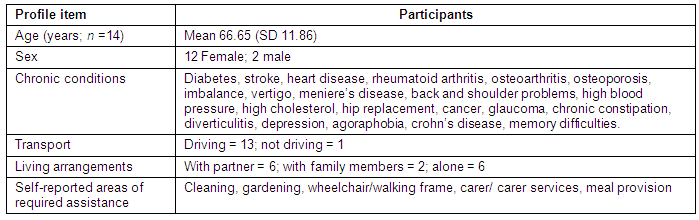
Participants: The Centre for Research into Disability and Society at Curtin University was contracted to conduct the evaluation of implementation processes and selected participant outcomes. All aspects of the evaluation were conducted independently of WACHS-SW management. Ethics approval was granted by the Curtin University Human Research Ethics Committee. Thirteen managers and health professionals and 21 CDSMP course participants received letters of invitation to participate in the evaluation from the research group. One manager/health professional declined; the other 12 were interviewed. Fourteen course participants took part (two by telephone interview but not the self-report outcome measurement), six declined to be interviewed and one was deceased. A profile of the 12 female and 2 male CDSMP course participants is provided (Table 1). Collectively, the 14 participants self-reported a total of 21 conditions with six of 14 participants individually reporting 3 or more conditions.
Table 1: Profile of Chronic Disease Self-Management Program course participants
Research design/ evaluation tools
Implementation processes were evaluated using semi-structured interviews with consistent verbal prompts, conducted with managers, lay and health professional course leaders and participants about positive and negative aspects of providing a CDSMP in WACHS-SW. Interviews were audio-recorded and transcribed.
Participant outcomes were evaluated using a modified pre-test, post-test design to evaluate changes in activity participation and self-management knowledge and skills. Because the evaluation began post-implementation, tools that provide a pseudo pre-test score were required. Activity participation was evaluated using the Activity Card Sort - Australia Recovery Version (ACS-Aus14). The ACS-Aus yields scores for previous, current and percentage of retained activity levels. 'Previous activity level' is defined as any activity performed as an adult, 'current activity level' is defined as any activity in which participants still engage. Knowledge and skills were evaluated with the Health Education Impact Questionnaire v2 (heiQ - RETRO)15. This version provides both a current and a previous score, thus allowing a comparison of 2 points in time.
Data analyses
Data were thematically analysed to identify emergent themes as well as positive and negative perceptions of the program.
Descriptive statistics were first calculated for participant outcomes. Scores on the ACS-Aus were calculated using procedures defined in the ACS protocols, and then compared with data available for community dwelling older adults without a chronic condition. The heiQ-RETRO was scored according to standard protocols to obtain the 2 scores needed for comparisons. Due to the small sample size (n = 12) the non-parametric Wilcoxon signed-ranks test was used for all comparisons.
Results
Implementation process and evaluation
Managers and course leaders identified both negative and positive aspects of providing a CDSMP in WACHS-SW. These were represented by 2 key themes: (i) program content and quality; and (ii) logistics of delivery (Table 2).
Chronic Disease Self-Management Program course participants identified positive and negative aspects in 3 main areas (Table 3): (i) health benefits; (ii) program content and quality; and (iii) logistics of delivery.
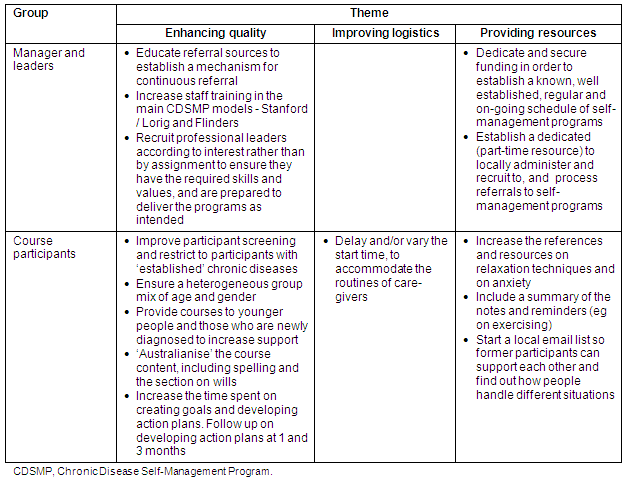
Throughout the interviews, managers and leaders, and course participants offered recommendations for setting up a CDSMP, and these have been thematically grouped into 3 categories: (i) enhancing quality; (ii) improving the logistics; and (iii) providing resources. These recommendations have been summarised (Table 4).
Table 2: Managers and leaders - positive and negative aspects of the Chronic Disease Self-Management Program courses
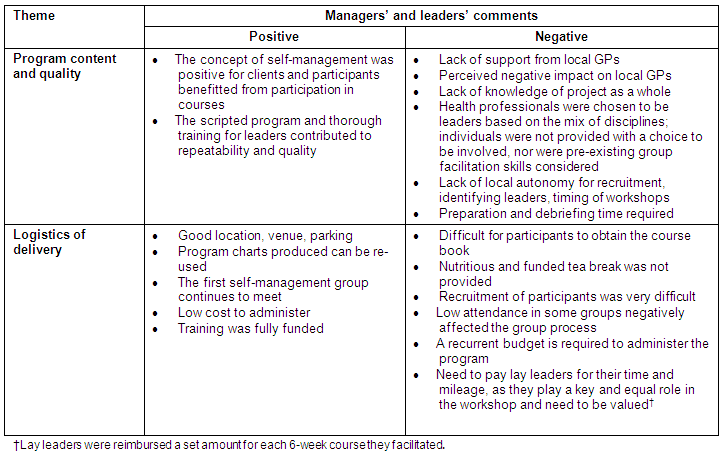
Table 3: Course participants - positive and negative aspects of the Chronic Disease Self-Management Program courses
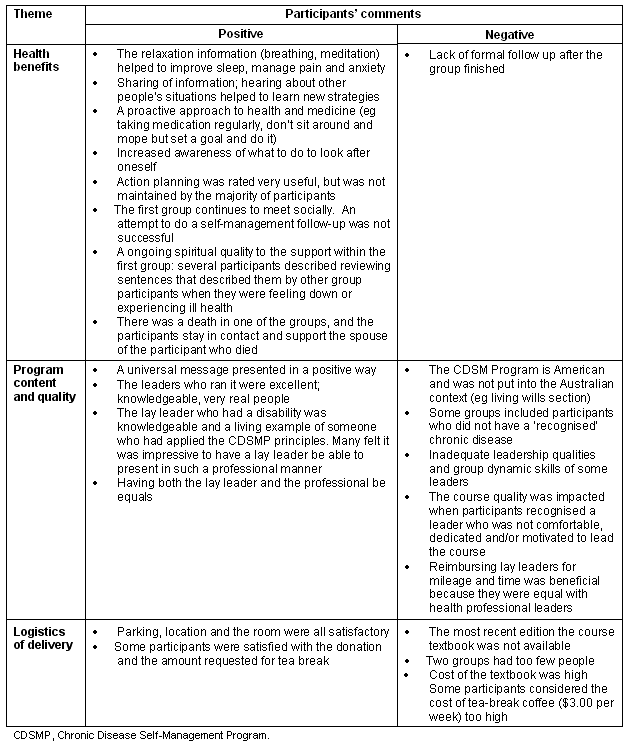
Table 4: Thematic grouping of recommendations from managers, leaders and course participants
Participant outcomes
The ACS-Aus scores are reported (Table 5) and also displayed graphically (Fig1), as are data for 2 comparison groups of adult Western Australians without long-term health conditions. Comparison group 1 consisted of 48 community-dwelling adults aged 75 years or under; comparison group 2 consisted of 45 community-dwelling adults aged over 75 years.
In lieu of pre-test and post-test data the 'previous activity' and 'current activity' levels were compared to determine changing activity patterns of program participants (Table 5). The results indicated a significant drop in activity level in this group over time (Wilcoxon signed ranks test Z = - 2.91; p = 0.004). Because previous activity is defined as 'activities performed as an adult' the comparison must be interpreted with caution. Data from comparison groups is provided to further examine participation levels. Comparisons group 1 had a mean age of 67.94 years, making them similar in age to the WACHS-SW group (Table 5). Visual inspection indicates that all 3 groups had similar previous activity scores. However, while the mean age of the WACHS-SW group was similar to comparison group 1, their current and retained activity scores were more similar in pattern to the older subjects in comparison group 2 than to their age-matched peer group.
The Wilcoxon signed ranks test results of the heiQ - RETRO demonstrated statistically better scores at post-test on 2 of the 8 domains (self-monitoring and insight, and health service navigation) with a trend toward significance on 3 other domains (positive and active engagement in life, skill and technique acquisition, and constructive attitudes and approaches) (Table 6, Fig 2).
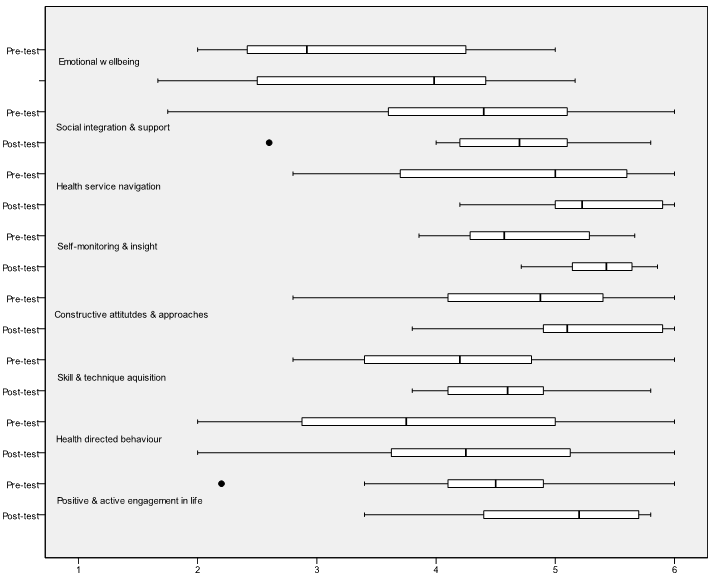
Figure 1: Box plots of the activity card sort for Western Australian Country Health Service - South West participants and 2 comparison groups.
Table 5: Activity card sort scores of the Western Australian Country Health Service - South West participants compared with two other groups of Western Australians
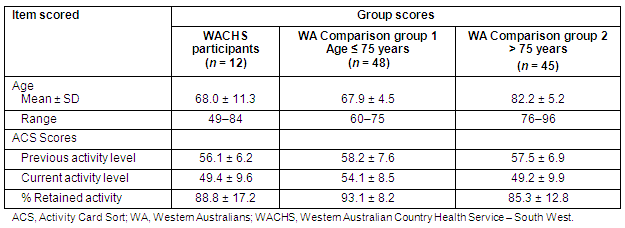
Table 6: Results of the Health Education Impact Questionnaire
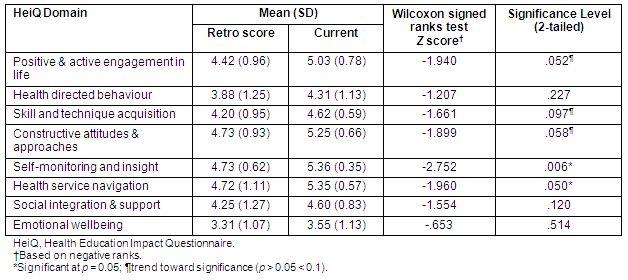
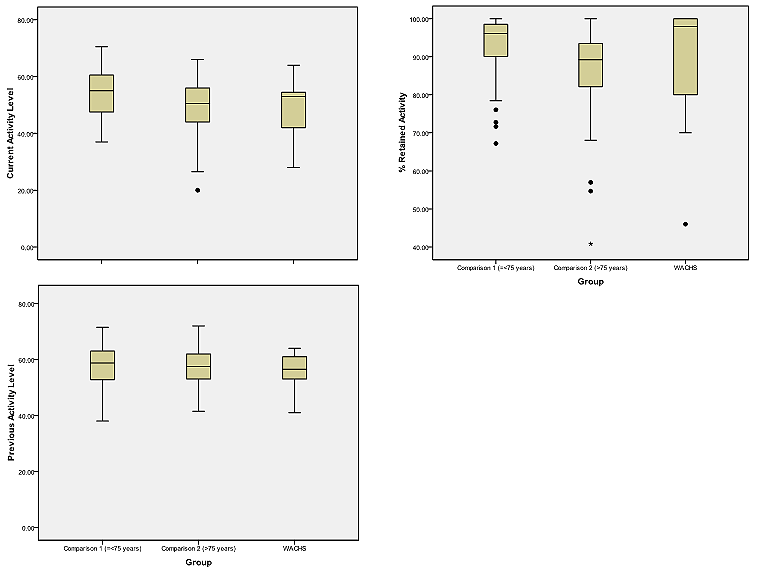
Figure 2: Box plots of the Health Education Impact Questionnaire for Western Australian Country Health Service - South West participants.
Discussion
This evaluation sought to describe patient and process outcomes following introduction of the CDSMP into an existing service in a rural setting. Given the small sample size and pilot nature of the project, participant outcomes were measured to provide early information regarding effectiveness and to guide future research. The evaluation process was considered a useful tool for identifying possible barriers and enablers to program implementation throughout rural and urban Australia16. Participant outcomes are first discussed, followed by a discussion of the evaluation recommendations in the context of relevant literature on CDSMP implementation and, where available, within Australian rural practice.
Participant outcomes
The participation levels of participants were measured with the ACS-Aus which provides 3 scores. The previous activity level is defined as 'activities performed as an adult'. In this study, participants had significantly lower participation levels compared with their previous activity levels at some time during their adult life. Because the time span does not correspond with participation in the CDSMP program, no conclusions can be drawn regarding the impact of the program on participation. However, on comparison with healthy older adults living in the community, the WACHS-SW group and older adults in comparisons group 2 both demonstrated a reduction in current activity levels from that of their earlier adult life, and a lower percentage of retained activities than their peers. Hence it can be concluded that the WACHS-SW program targeted a population in need. Future research should use more rigorous pre- and post-test design to increase understanding of the impact on participation.
The heiQ testing allowed a more precise measure of the impact of the CDSMP on participants, rating their abilities just prior to and just after participation. Even with the small sample size significant improvements were found on the domains of self-monitoring, insight and health-service navigation. Trends toward significance were found on 3 additional domains. As the heiQ was specifically developed to measure improvements in self-management skills, this is an indicator that the CDSMP is relevant and effective in rural communities.
Establishing regular cycles of Chronic Disease Self-Management Program courses with recurrent funding
This series of pilot courses demonstrated improved self-management outcomes for participants. However, a need was identified to allocate recurrent funding in order to establish a regular cycle of CDSMP courses, so that they become part of 'usual care'. International attempts to fully fund and sustainably embed CDSMPs into core practice have experienced varied success within disease-specific, state-wide program coordination planning and funding17, national healthcare18, and via a health insurance model19. While there is little evidence in Australia of factors that will facilitate the uptake and sustainability of CDSPMP courses20, a lack of full integration into primary care supported by devolved funding models is considered a barrier to full implementation13.
Integrating Chronic Disease Self-Management Program into everyday practice
A whole-of-system approach18,19 that includes system redesign to focus on continuity of care among service providers21 and practitioners20 may assist with integrating the self-management philosophy and principles into everyday practice. This evaluation suggests that, based on demographic and disease-burden profiles within a community, consideration be given to the place of CDSMPs in the local healthcare 'mix' of interventions, that priority costs and processes be identified, and the appropriate resource allocation be provided to maximise program sustainability, an issue of particular importance in rural communities22,23.
Establishing and maintaining group leadership skills and responsibilities
Self-management is characterised by a genuine partnership between clients and clinicians21, a paradigm shift that is not well understood or embraced by all health professionals13,24,25. Supporting clients in their attempts to self manage requires healthcare professionals who have a particular interest and belief in the philosophy of self-management and client-centred practice, and whose role to deliver programs is legitimised25. Of particular value are general skills in group dynamics and a belief in the behaviour change potential of self-efficacy26. Thus, establishing the capacity to deliver courses may be enhanced by identifying a core group of health professional and lay leaders to take full responsibility for program implementation. This would include preparing, scheduling and leading courses; and recruiting, registering and following up participants. Maintaining ongoing capacity, especially in rural areas, requires planned and structured professional development opportunities, including the possibility of at least one person becoming a 'master trainer' to ensure a sustainable resource training base21.
In line with overseas findings19, this evaluation found that lay leaders were well received, and that they need to be included in, and valued within the group of course leaders. To assist with the challenge of retention, they also require specific supports and incentives, with a minimum of a reimbursement for mileage and possibly an ongoing 'retainer' salary, which carries with it additional responsibilities such as assisting with course promotion and wider community education of the goals of self-management programs and the expected benefits to clients. This strategy may help facilitate local ownership of programs13 and address local needs, especially those of sub-groups21, all of which contribute to longer-term sustainability.
Group implementation strategies
Recruiting, screening, and reducing cancellations: Recruitment to the 3 locally-run courses appears to have reached those in need of self-management intervention. Levels of retained activity were lower in WACHS-SW participants than in a similar aged peer group without disabilities. This finding supports those from an earlier study in rural Australia, and warrants further investigation, in particular to identify if activity loss is more pronounced in rural than urban communities22. However, in the present evaluation, these findings contrasted with interview data indicating that not all participants had what would be generally considered a 'chronic condition'. This could be overcome by using a standardised screening tool designed to identify eligibility27, including health conditions, and informing care by a multidisciplinary team28. Engaging GPs in the recruitment process may also assist in confirming condition status, and in supporting appropriate referral to programs in the longer term20,22 via standardised referral pathways21.
General practitioners can also assist program sustainability through personalised and targeted recruitment strategies, such as a signed letter sent to patients by direct mail, recommending a CDSMP to meet a patient's identified needs. Using uncomplicated language may help in reaching those who have lower literacy levels, which can be a limiting factor in rural program delivery22. Cancellation rates following course registration can be reduced by simple and cost-effective strategies, such as a reminder phone call following a direct mail out21. Together, these strategies may all be complemented by the use of media and community partnerships to improve coordination and access, and to broaden the reach of community-based programs13.
Contextualise the Chronic Disease Self-Management Program: While exact enrolment rates were not able to be calculated due to the wide range of formal and informal strategies used, approximately one-fifth of all potential participants spoken to attended CDSMP courses, and no referrals came from GPs. Recruiting participants was difficult, with some not recognising the course as a Chronic Disease Self-Management Program. This finding is consistent with the generally low profile, and 'newness' of CDSMPs in Australia11. A variety of mechanisms is required to convey messages and to encourage clients to consider alternative ways to manage their health29. As such, future implementation could consider conducting research into appropriate and localised marketing strategies, taking into account the local context, population demographic (including long-term condition profile) and self-care needs, specific descriptions of what is being offered and the benefits of attending CDSM courses30.
Implementation of follow up for participants: Course participants cited lack of post-course follow up as a gap that reduced overall program quality. Access to follow up and review are deemed standard best practice management of long-term conditions and should be included in all program structures6. Course participants found scheduled face-to-face meetings with each other and with course leaders to be helpful after courses had finished. Other forms of follow up can be less formal, and may include online meetings and hard-copy and email newsletters via distribution lists.
Limitations
Research design: There are several limitations to the evaluation process and research design reported in this article:
- Because the evaluation was undertaken after the CDSMP was completed, true pre-test values were not available, nor was there a control group for comparison.
- Measurement tools were chosen to account for this limitation, and for their capacity to identify any measure of relative change between pre- and post-test, and to describe the participants in the CDSMP relative to a population without chronic conditions.
- Small numbers of participants attended the CDSMP and took part in this evaluation. Even with this small sample size and associated low power, significantly improved self-management behaviours were demonstrated in 2 of 8 domains with a trend to significance in 3 others. Further research using a larger sample to guard against type II error, and more rigorous testing are warranted to further understand effect on health outcomes and participation in activities following courses.
Conclusions
The evaluation findings reported in this article revealed that participants demonstrated fewer retained activities than their peers without long-term conditions. Despite this apparent loss, trends toward significant improvements were found on 2 heiQ-RETRO domains, along with significant improvements on 3 domains. These are powerful finding given the limitations imposed by the nature of the intervention in practice, the small participant numbers and the compromised research design.
Future implementation of CDSMPs within the WACHS will be encouraged by these patient outcomes, and informed by the qualitative findings from managers, leaders and course participants. Together, these findings may have application for implementation of CDSMPs in other rural and regional areas of Australia.
Acknowledgements
This research was made possible by a grant provided to the Centre for Research into Disability and Society at Curtin University from the WA Country Health Service. The authors also acknowledge Ms Jillian Swaine (Lecturer School of Occupational Therapy Curtin University of Technology), project officer and co-author of evaluation report; Ms Setareh Ghahari (Senior Research Fellow Centre for Research into Disability and Society Curtin University of Technology) for data analyses and technical assistance; Ms Silvia Clearwater and Ms Shelley Paterson (WACHS-SW Population Health Unit) for client recruitment to CDSMP courses; and the management and staff of the Busselton Community Health Centre for CDSMP course implementation.
References
1. Australian Institute of Health and Welfare. Indicators for chronic diseases and their determinants. Sydney, NSW: AIHW, 2008.
2. National Health Priority Action Council, Australian Government Department of Health and Ageing. National Chronic Disease Strategy. (Online) 2006. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/pq-ncds-strat (Accessed 2 August 2008).
3. Australian Government Department of Health and Ageing. Australian Primary Care Collaboratives Program (APCCP). (Online) 2004. Available: http://www.health.gov.au/internet/main/publishing.nsf/Content/health-pcd-programs-apccp-index.htm (Accessed 2 August 2008).
4. Australian Government Department of Health and Ageing. Primary Health Strategy. (Online) 2008. Available: http://www.yourhealth.gov.au/internet/yourhealth/publishing.nsf/content/NPHCS (Accessed 28 August 2008).
5. Western Australian General Practice Network. Australian Better Health Initiative - Primary Care Integration Program. (Online) 2008. Available: http://www.wagpnetwork.com.au/site/content./ (Accessed 28 August 2008).
6. Wagner EH. Chronic disease management: what will it take to improve care for chronic illness? Effective Clinical Practice 1998; 1(1) : 2-4.
7. Birmingham and the Black Country Strategic Health Authority. Reducing unplanned hospital admissions. What does the literature tell us? (Online) 2006. Available: http://www.hsmc.bham.ac.uk/publications/pdfs/How_to_reduce.pdf (Accessed 6 June 2008).
8. Lorig KR, Sobel DS, Stewart AL, Brown BW, Bandura A, Ritter P et al. Evidence suggesting that a chronic disease management program can improve health status while reducing hospitalisation: a randomised trial. Medical Care 1999; 37: 5-14.
9. Warsi A, Wang P, LaValley M, Avorn J, Solomon D. Self-management education programs in chronic disease: a systematic review and methodological critique of the literature. Archives of Internal Medicine 2004; 164(15): 1641-1649.
10. Chodosh J, Morton SC, Mojica W, Maglione M, Suttorp MJ, Hilton L et al. Meta-analysis: chronic disease self-management programs for older adults. Annals of Internal Medicine 2005; 143(6): 427-438.
11. Jordan JE, Osborne RH. Chronic disease self-management education programs: challenges ahead. Medical Journal of Australia 2007; 186(2): 84-87.
12. Council of Australian Governments (COAG). Australian Better Health Initiative (ABHI). (Online) 2006. Available: http://www.healthnetworks.health.wa.gov.au/abhi/home/ (Accessed 6 June 2008).
13. Lorig KR, Ritter P, Stewart AL, Sobel DS, Brown BW, Bandura A et al. Chronic disease self management program: 2 year health status and health care utilisation outcomes. Medical Care 2001; 39(11): 1217-1223.
14. Doney R, Packer TL. Measuring changes in activity participation of older Australians: validation of the Activity Card Sort - Australia. Australasian Journal on Ageing 2008; 21(1): 33-37.
15. Osborne RH, Elsworth GR, Whitfield K. The health education impact questionnaire (HEIQ): an outcomes and evaluation measure for patient education and self management interventions for people with chronic conditions. Patient Education and Counseling 2007; 66(2): 192-201.
16. Feyer AM, Francis C, Quigley R, Jessop R, Walsh J. The Sharing Health Care Initiative: issues in design of the evaluation of a national program of demonstration projects for self management of chronic conditions. Australian Journal of Primary Health 2003; 9(2&3): 208-216.
17. Lorig KR, Holman HR. Self management education: history, definition, outcomes, and mechanisms. Annals of behavioural Medicine 2003; 26: 1-7.
18. The EPP Evaluation Team. Process evaluation of the EPP - Report 11: Examination of the implementation of the Expert patient programme within the structures and locality of the NHS in England. Manchester: University of Manchester: National Primary Care Research and Development Centre, 2005.
19. Lorig KR, Hurwisc ML, Sobel DS, Hobbs M, Ritter PL. A national dissemination of an evidence-based self management program: a process evaluation study. Patient Education and Counseling 2005; 59: 69-79.
20. Francis CF, Feyer AM, Smith BJ. Implementing chronic disease self management in community settings: lessons from demonstration projects. Australian Health Review 2007; 31(4):499-509.
21. Kennedy A, Rogers A, Bower P. Support for self care for patients with chronic disease. BMJ 2007; 335: 968-970.
22. Bell E, Orpin P. Self management of chronic conditions: implications for rural physicians of a demonstration project Down Under. Canadian Journal of Rural Medicine 2006; 11(1): 33-40.
23. Williams A, Harris M, Daffurn K, Powell Davies G, Pascoe S, Zwar N. Sustaining chronic disease management in primary care: lessons from a demonstration project. Australian Journal of Primary Health 2007; 13(2): 121-128.
24. Skills for Care Skills for Health. Common core principles to support self care: a guide to support implementation. (Online) 2008. Available: http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_084505 (Accessed 4 September 2008).
25. Weeks A, McAvoy B, Peterson C, Furler J, Walker C, Swerrissen H et al. Negotiating ownership of chronic illness: an appropriate role for health professionals in chronic illness self-management programs. Australian Journal of Primary Health 2003; 19(2&3): 25-33.
26. Santurri LE. Patient empowerment: improving the outcomes of chronic diseases through self management education. The MPHP 439 online text Book. (Online) 2006. Available: http://www.cwru.edu/med/epidbio/mphp439/Patient_Empowerment.htm (Accessed 3 March 2009).
27. Foster M, Kendall E, Dickson P, Chaboyer W, Huner B. Participation and chronic disease self-management: are we risking inequitable resource allocation? Australian Journal of Primary Health 2003; 19(2&3): 132-140.
28. Orchard M, Green E, Sullivan T, Greenberg A, Mai V. Chronic disease prevention and management: implications for health human resources in 2020. Healthcare Quarterly 2008; 11(1): 38-43.
29. California Healthcare Foundation. Motivating change - Innovative approaches to patient self management. (Online) 2007. Available: www.chcf.org (Accessed 4 September 2008).
30. National Health Service. Research evidence on the effectiveness of self care support. (Online) 2007. Available: http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_081251.pdf (Accessed 20 January 2010).

