Introduction
Population aging is the most important demographic change worldwide, with an increase in not only the absolute number of older adults, but also a higher proportion of older adults in the overall population. This was originally a phenomenon of the developed world; however, recently developing countries have shown the highest rates of increase1,2. An important consequence of the increase in the number of the elderly in a population is that these individuals are more likely to have illnesses and/or chronic conditions that require a higher level of medical and social services.
Arterial hypertension is one of the most frequent chronic health conditions in Western countries. According to the National Health and Nutrition Examination Survey (NHANES) approximately 65% of people older than 65 years have hypertension3. Despite strong evidence that high blood pressure (BP) is an important and curable risk factor for cardiovascular disease and mortality in the elderly4-6, few population-based studies have focused exclusively on this age group7-11. Likewise, fewer still and none in a Greek population, have studied the factors associated with the awareness and treatment of hypertension among older adults (≥ 65 years). The aim of the present study was to estimate the prevalence, awareness, treatment and control of hypertension in the total elderly population of a Greek village, and to detect the factors associated with awareness of hypertension.
Methods
Study area and population
The study used a cross-sectional survey in the village Paliouri in northern Greece, located in Cassandra, Chalkidiki, 120 km from Thessaloniki. Paliouri is a typical coastal Greek village with 826 residents. The study was conducted in collaboration with the Primary Health Care Center of Kassandra and the Second Propedeutic Department of Internal Medicine, Aristotle University of Thessaloniki, Greece. All adults who were ≥65 years (a total of 191 in the local registry database) were contacted by telephone and invited to participate. Reminders were sent to non-responders, also by telephone, at least twice during the study period.
Subject evaluation
A well-trained medical doctor evaluated all participants in a GP's office over two visits. The survey was conducted from March to June 2006 and 95% of the subjects were evaluated during the spring. The initial visit involved a 15 to 20 min interview to obtain socio-demographic data (age, sex, marital and educational status, and monthly family income), information on habits (smoking and alcohol consumption), medical history (hereditary and personal), and details of drug treatment for hypertension or other diseases. More specific information was collected about the frequency and location (clinic or home) of BP monitoring before the study, and the number and type of devices used for home BP monitoring.
All anthropometric measurements (weight, height and waist circumference) were performed without shoes and in light clothing. Waist circumference was measured in centimetres at the narrowest part of the torso. Body mass index (BMI) was calculated as weight (kg) divided by standing height (m2). All participants were invited to attend a second visit 7 to 14 days later to have their BP re-measured.
The study was conducted in accordance with the principles of the Helsinki Declaration12. All subjects gave informed consent and the procedures followed were in accordance with institutional guidelines and approved by the review board of the collaborating university hospital.
Blood pressure measurements
Blood pressure was measured according to international guidelines13,14. Measurements were taken using a standard mercury sphygmomanometer with bladder size 12 x 35 cm, or another appropriate sized cuff if required. The subject remained at rest in the sitting position for at least 5 min before the BP was measured in both arms at the level of the heart. If there was a difference between arms, the measurements were taken in the arm with the highest BP. First (appearance) and the fifth (disappearance) Korotkoff sounds were recorded as indicative of the systolic blood pressure (SBP) and diastolic blood pressure (DBP) respectively. Blood pressure was evaluated on two occasions with a 7 to 14 day interval between them. At every visit, three BP measurements were taken with at least 1 min interval between them. In the analysis, only the average BP of the second clinic visit was used. Subjects who were only examined on the initial visit were excluded from the analysis. Consumption of caffeine and smoking was prohibited for at least 30 min before the measurements.
Definitions
Hypertension was defined according to the guidelines of European Society of Hypertension13 and the Joint National Committee (JNC) VII14 as SBP ≥140 mmHg and/or DBP ≥90 mmHg, and/or current treatment with antihypertensive drugs. Awareness of hypertension was described as any prior diagnosis of hypertension according to a health professional or the patient's health record10. Treatment for hypertension was defined as current use of antihypertensive drugs; and hypertension control was defined as treated hypertension with SBP <140 and DBP <90 mmHg10. In order to avoid the misclassification of non-hypertensive individuals taking cardiovascular medication for other indications a diagnosis of 'treated hypertension' was made only if the subject reported a prior diagnosis of hypertension and was using antihypertensive agents.
Participants were classified in 3 groups according to BMI values: normal (BMI <25), overweight (BMI 25≥ to <30) and obese (BMI ≥30). Abdominal obesity was defined as waist circumference ≥88 cm for females and ≥102 cm for males15.
Statistical analysis
Analysis was performed using the Statistical Package for Social Sciences v16 for Windows (SPSS Inc; www.spps.com). Results are expressed for continuous variables as mean ± standard deviation (M±SD) and for qualitative variables as frequencies. To determine whether each variable had a normal distribution, the Kolomogorov-Smirnov algorithm was used when the sample was ≥50, and Shapiro-Wilk when the sample was <50. Student's t- test or the Mann-Whitney U- test was used to estimate differences between mean values. Comparison of frequencies was performed by Pearson's χ2 with Yates' correction where appropriate (continuity correction was used to improve the fit to exact probability) and Kendall's tau b test or the Kruskal-Wallis test for variables with more than 2 groups. A probability value of p <0.05 was considered statistically significant. In addition, 95% confidence intervals (95% CI) were given where relevant, estimated using confidence interval analysis (CIA)16. The Wilson test was used for solitary percentages and the Newcombe test to estimate differences in paired proportions.
Results
Of the target population of 191 aged ≥65 years identified from the local registry, 171 agreed to participate (89.5%). Of these participants, four who were bedridden and unable to participate were excluded. Six subjects with only one visit for measurement of BP as well as seven normotensive patients who were taking antihypertensive drugs for another cardiovascular disease and who had no history of hypertension were also excluded. The working sample, therefore, was 154 people (80.6%). There were no statistically significant differences between participants included and excluded from the study in terms of mean age (74.2±5.8 versus 74.9±6.2, p = 0.498) and sex ratio (males' participation 97/104, 93.3% versus females' participation 74/87, 85.1%, CI 95% -6, 17.8).
Study sample characteristics
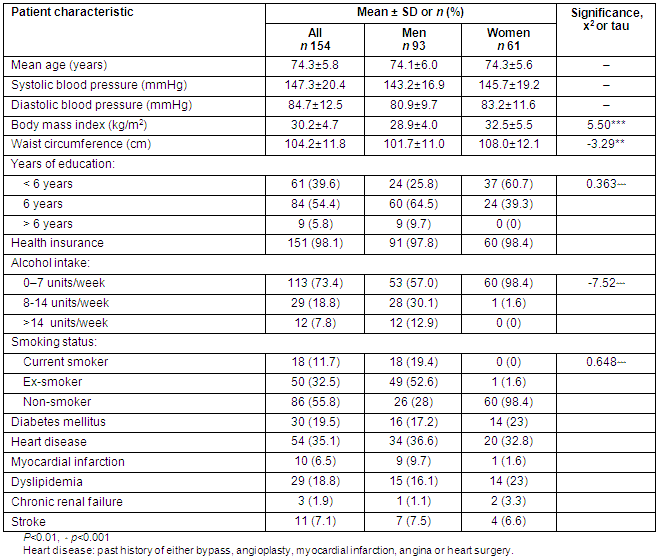
Paliouri represents a typical Greek rural village. The characteristics of the studied population are presented (Table 1). Among the 154 subjects who were included in the analysis, 93 were men (60.4%) and 61 women (39.6%). The mean age was 74.2±5.8 years (range 65-94 years). According to BMI 14% were normal, 35% were overweight and 51% were obese; according to waist circumference cut-off points 71.1% (CI 95% -51.5,-31.3) had abdominal obesity. The BMI and waist circumference were significantly higher in women than men (32.50±5.46 vs 28.94±4.04, p <0.001; and 108±12.08 vs 101.7±11.02, p <0.01) and in the younger elderly (<75 years) than the older (≥75 years) (31.03±4.6 vs 29.20±4.63, p <0.01; and 106.8±11.01 vs 101.1±12.04, p <0.01).
Table 1: Characteristics of the studied population
Prevalence, awareness, treatment and control of hypertension
The prevalence of hypertension was extremely high 89% (88.2% in men vs 90.2% in women, CI 95%: -0.117 - 0.092); with mean SBP and DBP levels 145.7±19.16 and 83.15±11.59 mmHg, respectively. There were no significant differences in SBP and DBP between men (147.3±20.4 / 84.7±12.5) and women (143.2±16.9 / 80.9±9.7), p = 0.082 for SBP and p = 0.108 for DBP, but SBP was significantly higher in participants ≥75 years (149.4±19.5 / 81.8±12.1) than participants <75 years (142.5±18.4 / 83.9±10.3), p = 0.028 for SBP and p = 0.257 for DBP.
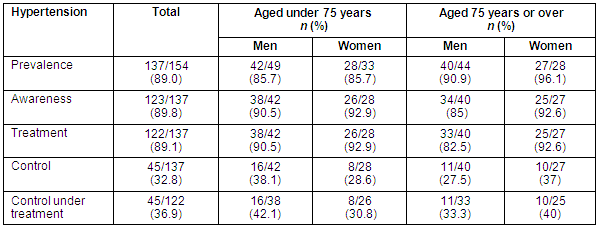
The levels of awareness, treatment and control of hypertension are presented (Table 2). Of the 137 hypertensive patients, 89.8% were aware of their condition. Mean SBP was significantly lower in those who were aware of their disease, compared with those who were not (146.7±18.73 vs 158.7±19.46, z = -2.065, p = 0.039); DBP was not significantly different (83.36±11.21 versus 88.1±16.31, t = -1.565).
Table 2: Prevalence, awareness, treatment and control of hypertension by age and sex
Awareness of hypertension was associated with a high frequency of BP measurement (p = 0.007), history of coronary (p = 0.006) or other chronic disease (p = 0.001), lower education (p = 0.032), and living with a spouse (p = 0.036).
Only one of the 123 individuals (0.8%) who were aware of their condition was not being treated for hypertension; of all the hypertensives only 45 (32.8%) had their hypertension controlled. Among treated hypertensives, SBP control was achieved in 41% and DBP control in 74.6%. Levels of awareness (CI 95%-0.128 - 0.064), treatment (CI 95% - 0.162-0.054) and control (CI 95% -0.159 - 0.155) were not significantly different between men and women.
Severity of hypertension
Classification of hypertension according to Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure14 showed that among the patients receiving treatment, 36.9% (CI95% 28.8-45.7%) were controlled, 37.7% (CI95% 29.6-46.6) had hypertension stage 1 and 25.4% had hypertension stage 2. Patients with uncontrolled hypertension were more likely and statistical significantly (CI 95% 3.7- 34.0) to have stage 1 hypertension (59.7%, CI 95% 48.6-70.0) than stage 2, (40.3%, CI 95% 30.0-51.4).
Drug treatment of hypertension
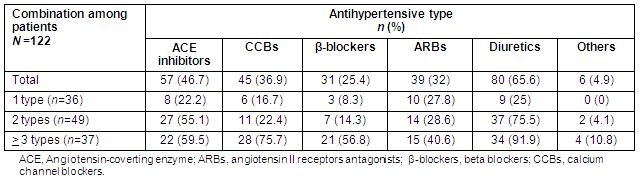
Study participants were followed up by various GPs. The number and types of antihypertensive medication received are presented (Table 3). In all, 29% of the patients receiving antihypertensive drugs were taking only one, 40.2% two and 30.3% at least 3 drugs. Among the patients receiving 2 drugs, the most common two combinations were a diuretic with an angiotensin-converting enzyme inhibitor (42.9%), and a diuretic with an angiotensin II receptor antagonist (22.2%).
Table 3: Types and combinations of antihypertensive medications used
Type of blood pressure monitoring
All participants reported that they had measured their BP at least once in the previous 2 years, and 89% once in the past 3 months. Of the 154 participants, 8.2% were measuring their BP once each year and 12.3% only if they had symptoms (headache or dizziness). Although 63.6% of the total population had a personal manometer, only 40.1% could measure their BP independently. Of the type of devices used for home BP monitoring, 65.5% owned a manual sphygmomanometer and 34.5% an electronic device. Regarding sex-related frequency of BP measurement, men were measuring their BP more often than women (at least once a month, 75% vs 51.7% (CI 95% 7.4 - 38.1). Women reported measuring their BP more often when they had symptoms (headache or dizziness) (8% men vs 19% women, CI 95% -23.6 - 0)
Discussion
This study showed the prevalence of hypertension in this elderly rural population to be extremely high (89%). However, despite the levels of awareness and treatment of hypertension being similarly high (approximately 89%), BP was poorly controlled at only 32%. The proportion of those taking combined therapies in our study was also relatively high (70%).
At the present time, 8 epidemiological studies7,17-23 have been conducted in Greece, with only 4 of them reporting data specific to the elderly: two local studies (Didima18 and Nemea7 study), the EPIC study21 and the only national study, Hypertenshell17, which reported only on the prevalence of hypertension among the elderly. The findings according to prevalence, awareness, treatment and control of hypertension in previous Greek studies are presented (Fig1).
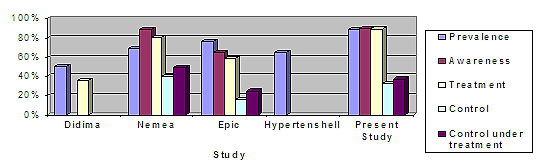
Figure 1: Comparison of present study with other Greek studies according to prevalence, awareness, treatment, control and control-under-treatment of hypertension in the elderly in Greece7,17,18,21.
Prevalence of hypertension
Our results are similar to Nemea, a study that also focused on an elderly, rural Greek population. The higher prevalence of hypertension in our study, the most recent one, may be explained by the fact that the prevalence of hypertension tends to increase with the passage of time24-26.
The prevalence of hypertension in the elderly (>60 or >65 years) according to studies in America3,24,27 and Europe8-11,25,28-30, varies from 64.8% in Italy (the results of a local study conducted exclusively in the elderly in 1992 in 3 Italian villages8) to 80.5% in England (the results of a national study carried out in 2001 that exclusively studied the elderly11). Therefore, although our study's prevalence seems very high, it is not significantly different from the studies of European countries (England 80.5%11, Portugal 78.9%29, France 78.2%10).
Awareness of hypertension
In studies conducted in the developed world, the frequency of awareness of hypertension ranged from 56.5% in England25 to 89% in Nemea, Greece7. The awareness of hypertension in our study was extremely high at 89.8% and this is similar to awareness found in the Nemea survey7.The high rate of awareness in our study could be attributed to Greece's free public health system and the easy access of the rural population to health services. In rural, in contrast to urban regions of Greece31, primary health care is well established and there is a doctor responsible for a specific population. Finally, awareness of hypertension was associated with a high frequency of BP measurement, a history of coronary or other chronic disease, lower education, and living with a spouse.
Treatment of hypertension
Similar to awareness, the rate of hypertension treatment was very high (89.1%), partially reflecting the implementation of guidelines for the treatment of hypertension. It is noteworthy that aware hypertensives were more likely to receive drug treatment than their counterparts in the surveys of other countries. Treatment rates in the elderly in other developed countries vary from 30.6% in Canada to 62.7% in the USA3,7-9,11,24,25,27-29. Most of the Mediterranean countries have treatment proportions of approximately 55%9,10,25,28-30, while in Greece this varies from 35.6% in the Didima study18 to 80.9% in the Nemea study7. It must be noted that in the present study, drug treatment was recorded according the health record, contrary to other studies which depended on patient-provided information24,32. The extremely low proportion of untreated aware patients (0.8%) in contrast to 5.3%-29% in the rest of the developed regions3,7-9,24,25,27-30, indicates an aggressive attitude among Greek doctors, who seem to prefer earlier drug treatment. This attitude has also been reported in the previous Greek studies (Didima and Nemea)7,18.
Control of hypertension
Only one out of three hypertensives had successfully controlled BP. In accordance with previous reports9-11,18, 5,27-30, even in the USA (control 27.4%)24, our study (control 32.8%) and the Nemea study (control 39.8%) suggest relatively high worldwide control rates among the elderly. This may partly be due to the perceived high rates of awareness in both of the studies. The proportions of combined therapy were also relatively high in our study, with only 29% of the pharmacologically treated hypertensive patients receiving only one drug. This is lower than has been reported in the elderly in Italy (72%)8 and Germany (53%)33. The high prevalence of combination therapy in our study may be responsible, at least in part, for the better control in Paliouri (32.8%), compared with these other studies (Italy 17.6%8 and Germany 22%33). Reports from large clinical trials suggest that the majority of hypertensive patients require two or more antihypertensive agents to reach the target BP14.
Strengths and limitations
Our study has some unique characteristics. First, all inhabitants were contacted, and an especially high response rate was achieved, among the highest in similar studies. Second, our study focused exclusively on the elderly, adding information about a group that is under-researched. Third, we provide data about factors associated with hypertension awareness, an issue of scarce and limited information. Finally, the vast majority of subjects (95%) was evaluated in spring, thus avoiding seasonal BP variations that could affect the results.
The interpretation of our findings is limited by the small size of our study population (the elderly of a small village). Our study also has the inherent limitation of studies into the elderly (over the age of 65) - that those with cardiovascular disease have already died and those still living are survivors. Likewise, because the overall number of unaware hypertensives was relatively small, any subgroup analysis should be interpreted with caution.
Conclusion
In conclusion, this study provides data that suggests hypertension is an important public health issue among the Greek elderly population. Despite high rates of awareness and treatment, control rates are disappointingly low. To manage this important problem the local health system must be more oriented to the prevention and control of high BP. Systematic prevention, together with greater efforts towards regular and strict surveillance and management in already diagnosed hypertensives may lead to better BP control and a subsequent reduction of cardiovascular events in this high risk population.
References
1. Lloyd-Sherlock P. Population ageing in developed and developing regions: implications for health policy. Social Science and Medicine 2000; 51(6): 887-895.
2. Eurostat. EU25 population aged 65 and over expected to double between 1995 and 2050. (Online) 2006. Available: http://epp.eurostat.ec.europa.eu (Accessed 4 March 2009).
3. Centers for Disease Control and Prevention. NHANES 1999-2000 public data release file documentation. (Online) 2000. Available: http://www.cdc.gov (Accessed 23 October 2000).
4. National High Blood Pressure Education Program Working Group. Report on hypertension in the elderly. Hypertension 1994; 23(3): 275-285
5. O'Donnell CJ, Kannel WB. Cardiovascular risks of hypertension: lessons from observational studies. Journal of Hypertension Supplement 1998; 16(6): S3-S7.
6. He J, Whelton PK. Elevated systolic blood pressure and risk of cardiovascular and renal disease: overview of evidence from observational epidemiologic studies and randomized controlled trials. American Heart Journal 1999; 138(3/2): 211-219.
7. Skliros EA, Papaioannou I, Sotiropoulos A, Giannakaki G, Milingou M, Lionis C. A high level of awareness but a poor control of hypertension among elderly Greeks. The Nemea primary care study. Journal of Human Hypertension 2002; 16(4): 285-287.
8. Prencipe M, Casini AR, Santini M, Ferretti C, Scaldaferri N, Culasso F. Prevalence, awareness, treatment and control of hypertension in the elderly: results from a population survey. Journal of Human Hypertension 2000; 14(12): 825-830.
9. Banegas JR, Rodriguez-Artalejo F, Ruilope LM, Graciani A, Luque M, de la Cruz-Troca JJ et al. Hypertension magnitude and management in the elderly population of Spain. Journal of Hypertension 2002; 20(11): 2157-2164.
10. Brindel P, Hanon O, Dartigues JF, Ritchie K, Lacombe JM, Ducimetière P et al. Prevalence, awareness, treatment, and control of hypertension in the elderly: the Three City study. Journal of Hypertension 2006; 24(1): 51-58.
11. Primatesta P, Poulter NR. Hypertension management and control among English adults aged 65 years and older in 2000 and 2001. Journal of Hypertension 2004; 22(6): 1093-1098.
12. Goodyear MD, Krleza-Jeric K, Lemmens T. The Declaration of Helsinki. BMJ 2007; 335(7621): 624-625.
13. Mancia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, Germano G et al. 2007 ESH-ESC Practice Guidelines for the Management of Arterial Hypertension: ESH-ESC Task Force on the Management of Arterial Hypertension. Journal of Hypertension 2007; 25(9): 1751-1762.
14. Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr. et al. Seventh report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure. Hypertension 2003; 42(6): 1206-1252.
15. Anon. VA/DoD clinical practice guideline for screening and management of overweight and obesity. Washington, DC: US Department of Veterans Affairs, 2006; 117. Available: http://www.guideline.gov
16. Altman DG, Malhin D, Bryant TN, Gardner MJ. Statistics with confidence: confidencee intervals and statisticall guidelines, 2nd edn. London: BMJ, 2000.
17. Efstratopoulos AD, Voyaki SM, Baltas AA, Vratsistas FA, Kirlas DE, Kontoyannis JT et al. Prevalence, awareness, treatment and control of hypertension in Hellas, Greece: the Hypertension Study in General Practice in Hellas (HYPERTENSHELL) national study. American Journal of Hypertension 2006; 19(1): 53-60.
18. Stergiou GS, Thomopoulou GC, Skeva II, Mountokalakis TD. Prevalence, awareness, treatment, and control of hypertension in Greece: the Didima study. American Journal of Hypertension 1999; 12(10/1): 959-965.
19. Moulopoulos SD, Adamopoulos PN, Diamantopoulos EI, Nanas SN, Anthopoulos LN, Iliadi-Alexandrou M. Coronary heart disease risk factors in a random sample of Athenian adults. The Athens Study. American Journal of Epidemiology 1987; 126(5): 882-892.
20. Panagiotakos DB, Pitsavos CH, Chrysohoou C, Skoumas J, Papadimitriou L, Stefanadis C et al. Status and management of hypertension in Greece: role of the adoption of a Mediterranean diet: the Attica study. Journal of Hypertension 2003; 21(8): 1483-1489.
21. Psaltopoulou T, Orfanos P, Naska A, Lenas D, Trichopoulos D, Trichopoulou A. Prevalence, awareness, treatment and control of hypertension in a general population sample of 26,913 adults in the Greek EPIC study. International Journal of Epidemiology 2004; 33(6): 1345-1352.
22. Sarafidis PA, Lasaridis A, Gousopoulos S, Zebekakis P, Nikolaidis P, Tziolas I et al. Prevalence, awareness, treatment and control of hypertension in employees of factories of Northern Greece: the Naoussa study. Journal of Human Hypertension 2004; 18(9): 623-629.
23. Rudenco I, Sotirakopoulos N, Tsitsios T, Peiou M, Kalogiannidou I, Mavromatidis K. Epidemiological features and treatment of arterial hypertension in patients of an insular area. Arterial Hypertension 2003; 12(1-3): 79 - 86.
24. Hajjar I, Kotchen TA. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988-2000. JAMA 2003; 290(2): 199-206.
25. Primatesta P, Poulter NR. Improvement in hypertension management in England: results from the Health Survey for England 2003. Journal of Hypertension 2006; 24(6): 1187-1192.
26. Hajjar I, Kotchen JM, Kotchen TA. Hypertension: trends in prevalence, incidence, and control. Annual Review of Public Health 2006; 27: 465-490.
27. Joffres MR, Ghadirian P, Fodor JG, Petrasovits A, Chockalingam A, Hamet P. Awareness, treatment, and control of hypertension in Canada. American Journal of Hypertension 1997; 10(10/1): 1097-1102.
28. Puras A, Sanchis C, Artigao LM, Divison JA. Prevalence, awareness, treatment, and control of hypertension in a Spanish population. European Journal of Epidemiology 1998; 14(1): 31-36.
29. Macedo ME, Lima MJ, Silva AO, Alcantara P, Ramalhinho V, Carmona J. Prevalence, awareness, treatment and control of hypertension in Portugal: the PAP study. Journal of Hypertension 2005; 23(9): 1661-1666.
30. Primatesta P, Brookes M, Poulter NR. Improved hypertension management and control: results from the health survey for England 1998. Hypertension 2001; 38(4): 827-832.
31. Yfantopoulos NG. Planning of health care in Greece. Economic and social dimensions. Athens: National Center social research, 1988; 64-66
32. De Backer G, Myny K, De Henauw S, Doyen Z, Van Oyen H, Tafforeau J et al. Prevalence, awareness, treatment and control of arterial hypertension in an elderly population in Belgium. Journal of Human Hypertension 1998; 12(10): 701-706.
33. Trenkwalder P, Ruland D, Stender M, Gebhard J, Trenkwalder C, Lydtin H et al. Prevalence, awareness, treatment and control of hypertension in a population over the age of 65 years: results from the Starnberg Study on Epidemiology of Parkinsonism and Hypertension in the Elderly (STEPHY). Journal of Hypertension 1994; 12(6): 709-716.
Abstract
Introduction: Hypertension is a major public health problem and its prevalence increases with age. Despite an aging population, only a limited number of population-based studies, and fewer Greek studies, have focused exclusively on the elderly. The objective of this study was to investigate the prevalence, awareness, treatment and control of hypertension in the rural residents of Paliouri village in Greece who were aged 65 years and older.
Methods: In total there were 171 participants (response rate 89.5%). Six blood pressure (BP) measurements were obtained in two visits and hypertension was defined as a mean systolic BP ≥140 mmHg and/or mean diastolic BP ≥90 mmHg, and/or current use of an antihypertensive medication.
Results: The prevalence of hypertension was 89%. Of the 137 hypertensive patients, 89.8% were aware of their disease, 89.1% were receiving treatment, and the hypertension of 32.8% was controlled. Awareness of hypertension was significantly higher among those with a high frequency of BP measurements, a history of coronary or other chronic disease, lower education, and those living with a spouse.
Conclusion: The findings indicate that hypertension is highly prevalent in this Greek elderly population. Similarly high is the awareness and treatment of hypertension. However, the control rates were relatively low, suggesting that the local health system requires a greater orientation to the prevention and control of hypertension.
Key words: cross sectional study, elderly, epidemiology, Greece, hypertension.
You might also be interested in:
2015 - Effect of rural practice observation on the anxiety of medical students
