Introduction
The Department of Loreto is located in the Amazon Basin, covering 368 851.95 km2, or 28.7% of the total geographical area of Peru (G Meza Sánchez, oral presentation, 2005). The department is home to approximately 891 700 people, 66.3% of whom live below the poverty line1. Approximately 50% of Loretans live in smaller cities or rural villages distributed along the system of rivers that feed into the Amazon River. The largest city in Loreto is Iquitos, with a population of approximately 323 990. Iquitos is located on the Amazon River and is reachable only by boat or plane.
Loreto faces its own unique medical situations and obstacles to healthcare delivery because of its geography and large rural area. The population is extremely dispersed, with an average of less than 10 inhabitants per km2, compared with Lima at 186-5774 inhabitants/km22. This low population density results in significant distances between healthcare facilities and patients; it requires that either physicians travel to reach few patients, or that patients travel long distances to reach medical care. As a result, patients sometimes delay seeking medical care, preferring to consult local healers first or simply suffering illness until symptoms are so severe that medical care cannot be avoided. Weather conditions and the expense of boat travel further contribute to patients' delayed arrival to healthcare facilities.
While working in various medical environments in Loreto, the authors have repeatedly encountered concerns regarding a lack of adequate healthcare personnel, particularly specialized physicians ('specialists'). This study was conceived to examine this concern, with particular focus on the obstacles faced by locally trained GPs in pursuing specialization training.
Medical education in Peru can be completed at both public and private universities. There are 34 faculties of medicine, eight of which are located in the capital Lima. Students apply to a faculty of medicine directly after finishing high school, generally at approximately age sixteen. They are accepted to medical school pending their performance on a traditionally very challenging entrance exam. Medical school consists of 6 years of undergraduate education, followed by a seventh year of rotating internship. At the end of the internship, graduates receive their medical degree, and are obligated to complete 1 year of rural service. On completion of their rural service, graduates are considered to be medicos generales, or GPs, and are fully qualified to pursue medical practice. Specialization is considered optional in Peru. Admission to residency programs, which are only available in selected cities, is highly competitive and is contingent on performance on the national entrance exam. Preference is sometimes given to applicants who have completed rural service in certain regions3.
Loreto has one medical school, the Facultad de Medicina Humana at the public Universidad Nacional de la Amazonía Peruana (UNAP) in Iquitos. Graduates of the medical school complete their internship at either the Hospital Apoyo Iquitos or the Hospital Regional de Loreto. Currently there are no residency programs in Loreto; those physicians who choose to specialize must leave the region in order to do so. Historically, only 10% of graduates from Iquitos apply to residency programs, and their performance on the entrance exam is inferior to the national average (GM Sánchez, Loreto Proyecto Salud; pers.comm., 2009). Loreto has struggled to reclaim its graduates who have left the region in order to specialize. Recruiting specialists from other regions of Peru has proven equally challenging, because 90% of Peruvian physicians are unwilling to commit to a long-term career in the rural sector4. As a result Loreto does not have enough specialists to staff even its tertiary care hospital with appropriately qualified physicians.
The Peruvian College of Physicians reported an overall surplus of physicians in 2007. According to its analysis, there are approximately 38 000 physicians in all of Peru4, yielding a physician to patient ratio of 13:10 000. This actually exceeds the ratio of 10:10 000 recommended by the Pan American Health Organization (PAHO) for achieving basic healthcare coverage4. In addition, the number of students matriculating and graduating from Peruvian medical schools has increased since 19994. Despite this reported oversupply of physicians, a discrepancy remains between supply and demand of doctors in Loreto. This is due in large part to geographic distribution: 57.9% of GPs are concentrated in the Department of Lima (vs 1.2% in Loreto; Peruvian College of Physicians 'Consejo Regional de Iquitos', equivalent and subsequently referred to as the Department of Loreto); similarly, 69.4% of specialists are in the Department of Lima (vs 0.7% in Loreto)4. This distribution of physicians is disproportionate to the population differences between the two areas (30.8% of Peruvians live in Lima, 3.3% in Loreto)5, resulting in a relative lack of both primary care and specialized physicians in one of the most impoverished regions of the country.
Not surprisingly, Loreto has yet to achieve the PAHO recommended physician to patient ratio. According to the Peruvian College of Physicians analysis, Loreto (2005 population 884 144) has 416 general physicians (4.7:10,000), and 132 specialists (1.5:10,000)4. The realities of geography and population distribution in the Peruvian Amazon, and Loreto in particular, are such that even if this recommended ratio were met, it would be unlikely to guarantee adequate healthcare delivery or access to care. Considering that rural physicians in Loreto may travel great distances along the rivers in order to reach their patients, it could be argued that Loreto would benefit from even more than the officially recommended 10 physicians per 10 000 inhabitants.
While the vast majority of health problems in Peru can and should be managed at the primary care level, ideally some of the physicians staffing this level would have completed residency6. The reality, however, is that the majority of practicing Peruvian physicians have not pursued specialty training; 65% of all doctors who graduated before 2006 are GPs, compared with 35% who are specialists. Further, doctors working in primary and secondary care centers tend to be younger, less experienced, and not specialized4. It is the recent medical graduates who run rural health posts during their required year of rural service. Working alone in remote villages, the young doctors are faced with limited resources and the inability to consult with more experienced physicians about their cases.
Ultimately, Loreto needs more physicians, particularly more specialists. The Peruvian College of Physicians recognizes this problem and recommends enhancing residency opportunities in the 'basic specialties': internal medicine, pediatrics, surgery, and obstetrics/gynecology4. According to the Peruvian Ministry of Health in 2004, Loreto needs an estimated 32 internists, 82 pediatricians, 30 general surgeons, and 46 obstetrician-gynecologists6. Most general physicians working in Loreto would like to specialize; however, it is proposed that they are limited by at least one of the following factors:
- location
- finances: cost of relocating to Lima, as well as loss of income while applying for and completing training
- academics: discrepancy between training level at UNAP and the academic level required to be accepted to residency in Lima
- personal or family reasons
Because the physicians most likely to stay in Loreto are those who are native to the area, Loreto needs to find a way to attract and retain its own medical graduates, in addition to attracting doctors from more urban areas. The Loreto Ministry of Health is therefore currently considering building residency programs in the four basic specialties (GM Sánchez, Loreto Proyecto Salud; pers. comm., 2009). This study was intended to provide baseline information to the Ministry of Health, characterizing the population of practicing GPs in two locations: Iquitos and Requena (located 157 km up-river from Iquitos, population 26 969). This research was conducted in the authors' final year of medical school while on a two-month clerkship in international health and medicine, working in the Iquitos Regional Hospital and later at the Requena Health Center.
Goals and objectives
The goals and objectives of this study were to:
- Characterize the population of currently practicing GPs in Iquitos and Requena in terms of demographics, current medical practice, and educational goals.
- Determine the obstacles faced by general physicians in Loreto, Peru in pursuing residency training.
- Provide baseline information to be used by medical academic institutions, particularly UNAP, to develop specialization programs in Loreto.
Methods
A 55 question survey was created with questions about demographics, current medical practice, education, training, and professional goals. With the help of officials at the Dirección Regional de Salud de Loreto, who track all of its 416 GPs, all 50 of the GPs in Iquitos, and all 5 in Requena were identified. For practical reasons, the research was limited to Iquitos and Requena, because reaching other Loreto communities required river travel of up to several days each way. Surveys were administered at hospitals, clinics, and during meetings at which multiple GPs gathered; consent was given verbally. The survey was written in Spanish, and it was self-administered. Survey responses were translated into English, entered data in EpiData, and analyzed data using SPSS software (SPSS Inc; Chicago, IL, USA).
Results
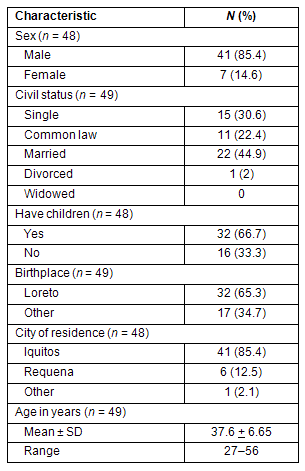
The study was conducted from 17 January to 13 March 2009. A total of 49 surveys were completed by GPs encountered in Iquitos and Requena. Of the respondents, 84% were male, the majority were either married or in common-law relationships, with at least one child. The average age was 37.6 years. Sixty-five percent were born in Loreto and most currently lived in Iquitos (Table 1).
Table 1: Characteristics of survey population
Current medical practice
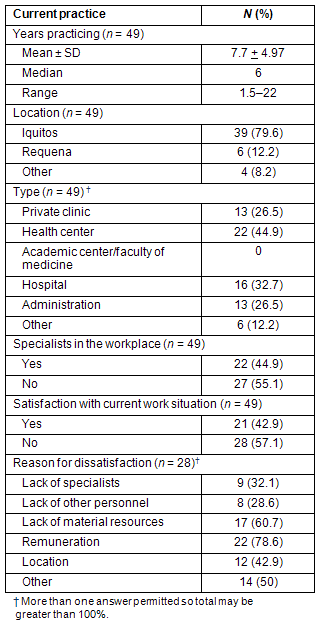
The surveyed physicians had been practicing medicine for an average of 7.7 years (Table 2). The majority practiced medicine in Iquitos and worked in a public health center (Centro or Puesto de Salud), hospital, administration or private clinic. Forty percent of the respondents worked in multiple clinical settings. On average, they had been working in their current primary work locations for 2.7 years; 45% worked with medical specialists on the same site. Only 43% expressed satisfaction with their current work situation. Of those who were dissatisfied, the most prominent reasons for their dissatisfaction were remuneration and lack of material resources. Other reasons noted included location, lack of specialists, lack of other personnel, lack of or need for further training opportunities, and problems with infrastructure and bureaucracy.
Table 2: Current medical practice
Training and specialization
Seventy-one percent of the surveyed GPs completed their medical studies at UNAP (Table 3). They took on average 9.69 years to complete the 7 year course. The majority completed internship in Iquitos, at either the Hospital Regional de Loreto or the Hospital Apoyo Iquitos.
Of the survey respondents, 92% reported that at the initiation of their medical studies they intended to pursue residency training. Only four reported intending to remain as GPs at that time and not pursuing any residency. Of this four, none intended to remain a GPs at the completion of their internships. Two other physicians reported their intent to remain a GPs at the end of their internship. In general, overall interest in the four basic specialties remained at the same level across the period of medical education - 61% versus 63% among those respondents who indicated only one intended specialty.
When asked to compare their desired work locations (rural, urban, Lima or other country) at the onset of medical education and at the completion of internship, there were notable shifts over the period of study (Fig1). Interest in working either in a rural setting or in another country increased, while interest in urban settings and Lima decreased (Table 3).
Table 3: Goals according to education stage
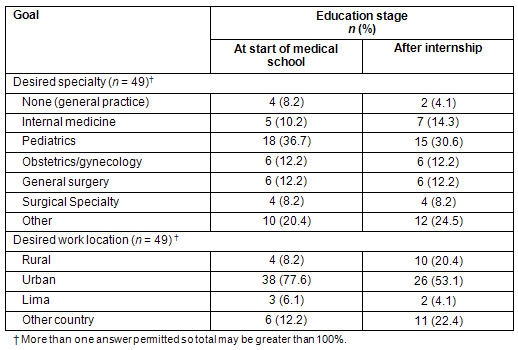
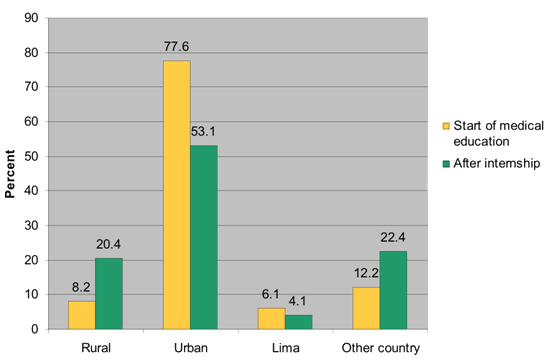
Figure 1: Desired work location
Of the respondents, two-thirds have pursued some sort of further medical training since completing their rural service and beginning to work as GPs (Table 4). The majority had participated in continuing education courses, some had completed diploma courses or apprenticeships, and 26% had pursued master's degrees. Two enrolled in residency but failed to complete the training, and two were participating in a special training arrangement, residencia no escolarizada, in which a GP who has been working in one specific specialty for many years can supplement his/her clinical work with distance learning courses and eventually obtain certification as if he/she had completed residency in that field3. Overall, these physicians had completed an average of an additional 1.25 years of training.
Nearly all the respondents reported that they intended to pursue further training; the majority (59%) intended to pursue residency. Of those intending to complete a residency in the future, 40% specified a desired specialty among the basic four, 22% a more specialized residency, and 37% did not specify (Fig2). The second most popular type of further training indicated was a master's degree, which can be attained in Iquitos.
Table 4: Participants' training
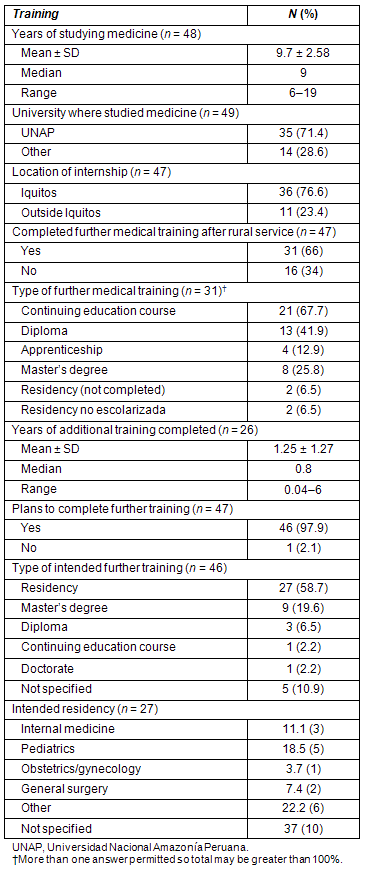
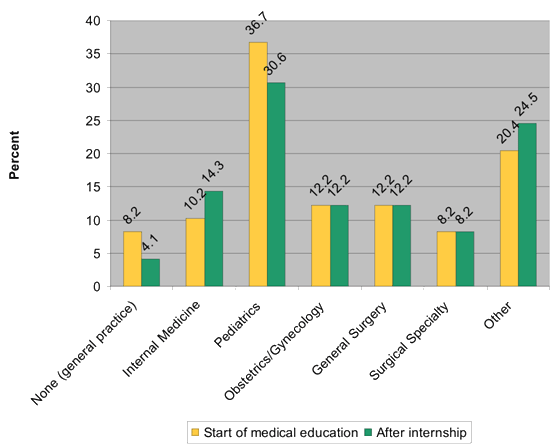
Figure 2: Participants' desired specialty
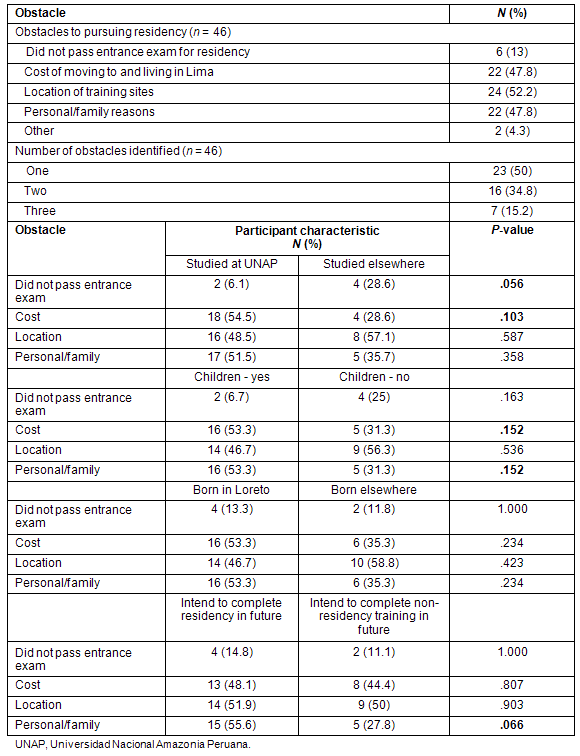
The location of training sites, cost of moving to and living in Lima, and/or personal or family reasons were each identified by approximately 50% of respondents as obstacles to their pursuit of residency. Less common but still notable were not passing the entrance exam, lack of job stability, and not knowing English. Fifty percent of the respondents only identified one obstacle, while 35% identified two and 15% identified three.
Some specific characteristics of the responding physicians were selected and compared with their indicated obstacles, in an attempt to determine if certain demographic or educational factors were associated with particular obstacles (Table 5). Sex, having children, region of birth, city of residence, study at UNAP, having specialists in the primary work setting, having already completed further medical training, and current intent to pursue residency in the future were all cross-tabulated with the four main obstacles. Generally, the sample size was too small to show statistically significant associations or correlations; despite this, statistical tests suggest some trends. Those who studied at UNAP were slightly more likely to cite cost as a limiting factor than those who studied elsewhere (p = 0.103); those with children were slightly more likely to cite both cost and personal/family reasons as obstacles (p = 0.152 for both); and people who currently intended to pursue residency were more likely to cite personal/family reasons than people who intended to pursue non-residency training (p = 0.066). Studying at a university other than UNAP was correlated with not passing the entrance exam (p = 0.056).
Table 5: Participants' obstacles to pursuing residency
Discussion
Over the course of data collection, it was learned (often from the same physicians who were participating in the study) that there were additional barriers to residency that did not appear in completed surveys. In order to even apply for residency in Peru, a physician must leave his/her current job to travel to Lima to take the entrance exam. Those physicians who live and work in the Peruvian coastal regions have access to preparation courses for the entrance exam; however, these same preparatory resources are not available to physicians in Loreto, thereby decreasing the likelihood that they will pass the exam. If residency training were to be offered in Loreto, local candidates would still compete against those from urban centers, although perhaps there would be a set quota for Loretan applicants. Finally, the numbers of residency positions are limited; in 2004, there were 844 residency positions across all specialties and only approximately 30% of those who applied succeeded in securing positions7. In a scenario where an individual must relinquish his/her employment in order to even begin the process to apply for a position he/she is unlikely to get, it is not surprising that so few of the physicians in Loreto pursue residency. Despite these numerous obstacles, GPs in Loreto are a motivated and enterprising group: the majority of doctors surveyed have pursued further training such as master's degrees, apprenticeships, and diploma courses.
It was a surprise to discover the lack of knowledge GPs had about family medicine; many did not recognize the specialty as a field distinctly different from their own. While there is a projected need of 31 family doctors in Loreto6, currently there is only one family physician in the whole Department, and he is not in clinical practice. The authors also became aware of Loreto's acute need for pediatricians and obstetricians/gynecologists, due to the region's high fecundity(C Carey Angeles, oral presentation, 2009). In 2000, 43.4% of all hospitalizations in Peru were attributed to pregnancy, delivery and postpartum care8.
There were several limitations to this study. While 89% (49/55) of the targeted population were surveyed, the sample size of GPs remains small and not randomized; for these reasons the characteristics of this physician population cannot be expected to be representative of the entire population of GPs in Loreto. Although the proportion of males in the surveyed population was similar to the proportion of male physicians in all of Loreto (83.7% vs 84.3%7), the age distribution of the surveyed population is skewed toward younger physicians when compared with the age distribution of physicians in Peru7. The small sample size also limits the strength of statistical correlation, making it difficult to pinpoint associations between personal characteristics and specific obstacles to pursuing residency. Time limitations in the authors' two-month clerkship did not allow them to pilot the survey, which would have identified and allowed the reworking of some problematic questions. Surveying GPs proved quite time-consuming; it involved arriving at a clinic or hospital, often unannounced, presenting the study, and waiting for a physician to find time to complete the questionnaire by hand. Additionally, a researcher-administered, rather than self-administered survey, could have prevented some problematic responses. Reporter bias may also be a source of error, particularly in the case of the question regarding passing the national entrance exam. Finally, some typographical errors in the Tables section of the Peruvian College of Physicians analysis were noted and adjustments were made to the present study data.
Despite these limitations, the data collected in this study do allow us to describe, in general terms, the population of GPs in Iquitos and Requena, and their perceived obstacles to pursuit of residency. Clearly, cost and location were the most significant factors preventing physicians from pursuing residency; overall, 83% of the physicians surveyed identified one or both of these as a factor that prevented them from pursuing residency. Despite the fact that nearly all of the surveyed physicians intended to complete residency training when they finished their internship, they are all currently working as general physicians. Although it has been suggested that the quality of medical education at UNAP is below the standard set by the rest of the country, the present small sample suggests that having studied at UNAP is not associated with higher rates of failure on the entrance exam. Overall, this study suggests that there may be an interested and capable applicant pool for future residency programs established in Loreto.
This study focused exclusively on physicians; however, it goes without saying that good health care is delivered by a team of people working together. The Joint Learning Initiative, launched by the Rockefeller Foundation, took into account physicians, nurses, and midwives when it reported that, on average, countries with fewer than 25 healthcare professionals per 10 000 people failed to achieve an 80% coverage rate for deliveries or for measles immunization9. It is suggested, therefore, that this research be viewed as a pilot study; future studies on healthcare human resources in Loreto should address the issues of distribution and training of allied health personnel, such as nurses, midwives, and technicians in the entire department. While this study focused on the poorest region of Peru, physician recruitment and retention in rural and remote areas is a universal challenge. It is hoped that this research will help both developing and developed countries approach this problem.
Another area for future research is investigation into the population of specialists who work in Loreto. Understanding who these physicians are and what brought them to Loreto after having completed their residencies may help focus efforts to attract more specialists to the region.
Acknowledgements
The authors thank all the GPs in Loreto who completed the survey. In addition, the following people were a tremendous help in administering the surveys: Oswaldo Videira Paredes, MD; Maria Huilca Chambi, MD; Mario Pereyra Rimachi. The authors are also grateful to Cristiam Carey Angeles, MD, MPH for his data, and to Dahlia Weitzman, PhD, for her statistical expertise. Finally, they thank Graciela Meza Sánchez MD, MPH, an invaluable resource, advisor and friend.
References
1. Instituto Nacional de Estadística e Informatica [National Statistics and Information Institute]. Nota de Prensa No. 135 Julio 2007 [Press Release n135, July 2007]. Available: http://www.inei.gob.pe (Accessed 29 March 2009).
2. Instituto Nacional de Estadística e Informática [National Statistics and Information Institute]. Perú: Densidad Poblacional, Por Departamento, 1993 y 2007 [Peru: Population Density, By Department, 1993 and 2007]. (Online) 2007. Available: http://www.inei.gob.pe (Accessed 29 March 2009).
3. Garmendia LF. El Residentado Médico en Perú: Analisis Crítico del Residentado en el Perú. Academia Nacional de Medicina - Anales 2005 [Medical Residency in Peru: Critical Analysis of Residency in Peru]. Annals of the National Academy of Medicine 2005; September: 73-77.
4. Carrasco Cortez V, Lozano Salazar E, Velásquez Pancca, E. Current and prospective analysis of physician supply and demand in Peru for years 2005-2011. Acta Medica 2008; 25(1): 22-29.
5. Instituto Nacional de Estadística e Informatic [National Statistics and Information Institute]. Primeros Resultados Perú: Crecimiento y Distribución de la población, 2007 [First Results Peru: Population Growth and Distribution, 2007]. (Online) 2007. Available: http://www.inei.gob.pe (Accessed 29 March 2009).
6. Carrión Arrunátegui, Rómulo; Instituto de Desarrollo de Recursos Humanos [Institute of Human Resources Development]. Formación de especialistas en el Perú [Formation of specialists in Peru]. Lima: Instituto de Desarrollo de Recursos Humanos, 2009.
7. Carrasco Cortez V, Lozano Salazar E, Velásquez Pancca E. Análisis actual y perspectivas de la oferta, demanda y necesidad de médicos en el Perú, 2005-2011 [Current and prospective analysis of physician supply and demand in Peru for years 2005-2011]. Lima: Colegio Médico del Perú, 2007.
8. Alarcón Villaverde J. Perú. El Perfil epidemiológico en un contexto de demanda reprimida de servicios de salud . [Epidemiological profile in the context of confined demand of health services]. Informe Técnico No. 025S. Bethesda, MD: Socios para la reforma del sector salud. Proyecto PHR plus Abt Associate, 2003; 33.
9. WHO. World Health Report 2006: working together for health . (Online) 2006. Available: http://www.who.int/whr/2006/whr06_en.pdf (Accessed 4 April 2009).
______________________________
Appendix I: Survey instrument



