Introduction
It is well known that the rapid identification and treatment of patients with myocardial infarction, either by thrombolytic therapy or primary angioplasty, reduces mortality and morbidity and improves cardiac function1-3.
Most people experiencing an acute coronary event delay seeking medical assistance; as a result and some are ineligible for thrombolytic therapy4. Delay time has been reported to be affected by a number of variables, including age, sex, race, socioeconomic status, history of coronary artery disease (CAD) and interpretation of symptoms among others5-7. Several studies have examined the effect of these factors on the patient's decision to seek medical care, with conflicting results5-8.
Although patients from city, suburban and rural areas have been studied, most of the current research has been conducted in urban settings9-11. A direct comparison of the characteristics and associated delay time between rural and urban patients has not been conducted.
This study sought to investigate whether patients living in urban and rural areas differ in the decision time for seeking medical assistance (patient-related delay) and in the time it takes to reach hospital (pre-hospital delay) during myocardial infarction, and to determine the factors associated with these time delays.
Methods
Study population
The island of Crete has approximately 600 000 inhabitants and is divided into 4 prefectures. The prefecture of Heraklion is the largest and, according to the most recent census, has 292 489 inhabitants, of which 137 711 are residents of the major Heraklion city district area and 154 778 reside in rural areas. Apart from the two major metropolitan areas of Athens and Thessaloniki, residents' sociodemographic characteristics are similar to the general Greek population12. The regional and university hospitals are providers of secondary and tertiary care for patients with acute coronary syndromes; both are located in the city of Heraklion. The hospitals have 6 connected public health centres, serving mainly rural areas (and area was considered rural if it had a population of between 10 and 59.9 inhabitants/mile2 (1.6 km2).
The distance between the public health centres and Heraklion city ranges from 30 to 65 km, a travel time of approximately 30 min for two of the health centres, and 35 min; 50 min; 1 hour; and 1 hour and 10 min, respectively, for the other four.
The inclusion criteria were all patients with a confirmed diagnosis of acute myocardial infarction (by ECG and positive creatinephosphokinase-MB or troponin I), who were hospitalised in either hospital during a 16 month period and were available for interview. Patients with both ST segment and non-ST segment elevation myocardial infarction were included.
Questionnaire
A questionnaire was completed by each patient regarding the following characteristics:
- Medical history: presence of CAD (including previous myocardial infarction or previous revascularisation)
- Education (elementary or higher)
- Place where symptoms started
- How medical help was sought
- What symptoms the patient experienced
- Whether they recognized the symptoms as originating from the heart
- Whether they interpreted the symptoms as serious
- Whether concomitant symptoms such as dyspnoea, nausea or collapse were present
- The severity of their chest pain (0-10 scale, with 0 being 'no pain' and 10 'the worst imaginable pain')
- Their reasons for delaying seeking help (professional, financial, lack of trust in the medical system, waited until symptoms waned, didn't want to bother others).
All interviews were conducted between the second and fourth day after discharge from the coronary care unit. Two time intervals were recorded: (i) from symptom onset to when medical assistance was sought (patient-related delay); and (ii) from the time when such assistance was sought (which included from a health centre, private doctor or emergency response system) until arrival at hospital (pre-hospital delay). If primary care was bypassed, the pre-hospital phase was taken as the time from initiating travel to hospital to arriving at the hospital. If time intervals or questionnaire content were uncertain, confirmation was obtained from ambulance records, relatives or bystanders.
Three time periods (patient-related, pre-hospital and total delay) were compared in the two populations and characteristics related to delay periods were identified for the entire patient population. These characteristics included age, sex, history of CAD, diabetes, smoking, hyperlipidaemia, education, and the previously described reasons for delay.
Of the 362 patients who fulfilled the study criteria, 14 refused participation. Therefore, a total of 348 patients were included, 172 from an urban area and 176 a rural area. The characteristics of both groups are shown (Table 1).
All patients gave informed consent before participating in the study. The study was approved by the University Hospital ethics committee. The study protocol conformed to the Declaration of Helsinki's ethical guidelines.
Table 1: Characteristics of the study population
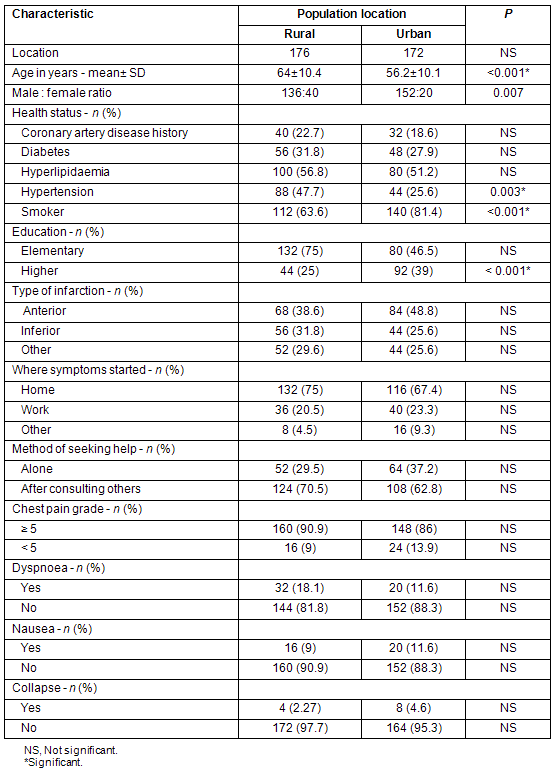
Statistics
Descriptive statistics for continuous variables are reported as median and mean standard deviation (SD). Comparisons of continuous parameters between the two groups were performed using t-tests or Mann-Whitney tests, as appropriate. Chi-squared or Fisher's exact tests were used to compare the distributions of various categorical variables between rural and urban areas.
Kaplan-Meier product limit estimate curves were constructed in order to compare the effect of various demographic and clinical parameters on patient related delay, pre-hospital delay and total delay time, using a log-rank test. Factors that were found to be significant in the univariate analysis were then entered in a stepwise Cox proportional hazards model in order to identify independent significant factors. The criteria for entry into and removal from the model were set at 5% and 10%, respectively. The level of significance for all statistical tests was set at 5%. The software SPSS v12 (SPSS Inc; Chicago, IL, USA; www.spss.com) was used for all statistical calculations.
Results
One hundred and thirty-four patients from a rural area (76%) had first contacted a health centre and were then transferred by ambulance, 23 (13%) had driven directly to a hospital, and 19 (11%) had first contacted a physician other that one from the health centre. Sixty-two patients (36%) from an urban area had been brought to hospital by car and 86 patients (50%) directly by ambulance, while 24 (14%) had come to hospital after contacting a physician.
Delay time
Only four patients arrived at a hospital within 1 hour, while 50% of the patients from a rural area and 55.8% from an urban area were delayed by more than 4 hours after symptom onset (not significant).
There were no differences in patient-related and total delay time between the two groups, although a trend to a shorter patient-related delay was noted for rural participants. The median time was 180 min (rural) versus 240 min (urban) (mean 559.8 vs 844.9 min; SD 893.1 vs 1197.9; p=0.058). Those living in a rural area had a longer delay in reaching hospital. The median time was 50 min vs 20 min (mean 75.9 vs 44.4 min; SD 68.5 vs 75.5; p<0.0001). The total (median) delay time was 255 min for rural and 285 min for urban patients; the difference was not significant (mean 635 vs 889.30 min; SD 895.2 vs 1206.1; p=0.9; Fig1)
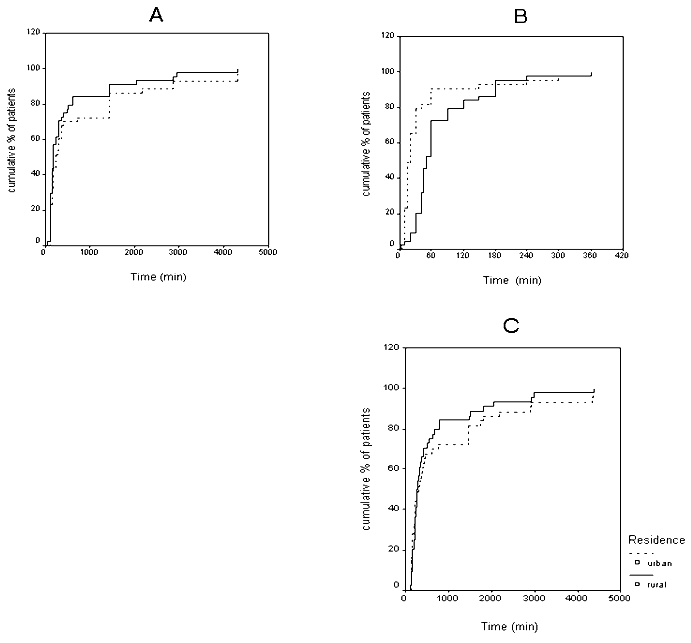
Figure 1: Kaplan-Meier curves showing: (A) patient-related delay; (B) pre-hospital delay; and (C) total delay for patients living in urban and rural areas.
Patient-related factors for delay
Regarding the reasons for not seeking earlier medical help, 84% of the patients from rural and 86% from urban areas said they had waited to see if their symptoms would subside; whereas 80% of patients from rural and 67% from urban areas did not recognise that their symptoms originated from the heart. Fifty-two percent of rural and 53% of urban patients considered their symptoms to be serious. Fifty-five percent of patients from rural and 62% from urban areas reported the delay was due to family or professional obligations, or financial considerations; while 13% of rural and 10% of urban patients did not trust the healthcare system. Fifty-two percent and 47% of the patients from rural and from urban areas, respectively, reported they did not want to bother other people. There was no significant difference in these results between rural and urban residents. However, multivariate Cox regression analysis showed that independent factors positively affecting patient-related delay were: (i) not considering symptoms to be serious (p<0.0001); and (ii) female sex (p=0.01); while the presence of CAD was negatively associated (p=0.043).
Pre-hospital delay was positively associated with rural residence (p<0.0001) and negatively associated with anterior (p=0.01) and non-Q (p=0.008) myocardial infarction. The total delay time was positively affected by female sex (p=0.003) and negatively affected by the presence of CAD (p=0.014) if the patients had considered the symptoms to be serious (p<0.0001) or had recognised them as originating from the heart (p=0.002).
Discussion
The rural and urban populations differed in certain ways: the rural participants were older, of lower educational and economic levels, and they had limited access to health-related information. Some of these characteristics have been associated with a greater delay in seeking treatment. Primary care in Greece's rural areas is provided mainly through local health centres; however, the management of emergency cases is only available at the two hospitals in Heraklion city. Therefore, the identification and quantification of pre-hospital time delays could have implications for the way the Greek National Health System is organized, particularly regarding emergency care in rural areas. Identifying factors that correlate with delay, regardless of residence (patient-related delay), can also provide clues to assist in shortening delays.
The first time interval studied concerned the patient and his/her decision to seek help exclusively, while the second interval was directly related to the healthcare system (health centres, ambulances, private doctor etc) in the majority of cases. The results of this study showed no significant time differences between rural and urban patients in their decision to seek medical help. This was despite rural patients being older and having a lower educational level, and the sample including a larger percentage of women (Table 1).
There is no satisfactory explanation for this but it should be borne in mind that the study was conducted in a region that is considered to have a low incidence of coronary events13,14. This could result in lower levels of awareness and greater denial among younger men and women regarding myocardial infarction, which is thought to affect more elderly men. This could result in a longer delay. The difference in age between the two groups may be related to a rising incidence of CAD among younger patients in the city and suburban areas of this region, the result of changes in diet (reduced Mediterranean diet, increased Western diet), a sedentary life style and an increased smoking prevalence (81% vs 63.6% in the rural areas).
The second time interval studied showed that rural patients take significantly longer (median time approximately 30 min more) than urban residents to reach hospital. This is not unexpected due to the distances involved but it may have significant consequences for patients' outcomes - a 30 min delay in the administration of thrombolysis reduces life expectancy by 1 year15.
Because rural patients cannot summon an ambulance directly but must go via an initial examination at the health centre, they present to hospital only if found to be suffering from acute coronary syndrome. The pre-hospital interval would be reduced if thrombolysis was administered at the health centre, but GPs in Greece are reluctant to administer thrombolytic therapy in patients with acute myocardial infarction. In fact, none of the present patients received thrombolytic therapy prior to arrival at hospital. This is in contrast to a recent study from Scotland, where 55% of rural GPs had administered thrombolysis at least once16. Due to the way the National Health System operates in Greece, efforts must be made to improve the expertise of health centre physicians, especially in remote areas, when dealing with coronary events and giving thrombolytics.
An alternative would be to change the system. In case of acute coronary syndrome patients could be permitted to bypass the health centre, but this presupposes a prompt diagnosis or high degree of suspicion, as well as an appropriate means of transportation and treatment in rural areas (ie a mobile heart unit with personnel trained in reperfusion therapy). Ambulances operate on a 24 hour basis in both rural and urban areas but none is equipped to support pre-hospital reperfusion therapy. It has been suggested that thrombolytic treatment should be initiated before the patient is transferred to hospital if the travelling time is more than 30 min17,18.
The longest interval was in patient-related delay for both groups (3 and 4 hours for the rural and urban populations, respectively) and this is of concern because the initial phase of an acute coronary event carries the greatest risk of sudden death. This delay was longer if the patient did not consider the symptoms serious, and total delay was shorter if symptoms were recognised as cardiac in origin. It seems, therefore, that the interpretation of symptoms by the patient19, as well as their severity, is of paramount importance in minimising delay. However only 20% of rural and 33% of urban patients considered their symptoms to be heart related, in contrast to a recently published Swedish study where three-quarters of the patients interpreted their symptoms as cardiac in origin11.
The total median delay (4.25 hours for rural and 4.75 hours for urban patients) was longer than in other northern European studies (range, 2.2-3.88 hours)20-23. Recent data also show marked geographic differences in the extent of pre-hospital delay in patients with ST-segment and non ST-segment elevation acute myocardial infarction24.
Whether a history of CAD is related to delay is controversial. Some investigators have reported that this does not affect delay25,26, while others have found it to be associated with shorter delay27. The latter was the case in the present study, where a history of CAD proved to be an independent factor for shortening both patient-related and total delay. Although previous studies have reported no relationship between sex and delay25-26, the findings of the present study regarding sex are consistent with others that have concluded women delay longer than men28. Ottesen et al22 reported that women had a longer pre-hospital interval, caused by prolonged physician and transportation delay. However, in another study29 the investigators reported that the most significant reasons for delay among women were atypical presentation of symptoms, severity of presenting symptoms, and incorrect attribution of symptoms.
It should be noted, however, that comparisons among studies may not be easy due to differences in the components of delay and the characteristics examined. In addition to cultural differences other factors, such as the overall incidence of CAD and the level of public awareness concerning acute myocardial infarction, may vary among countries. Continued improvements in the way emergency medical systems are organised (including the availability of on-site thrombolysis in health centres or in ambulances) are essential to improve patient care. However, if patient-related delay does not lessen significantly, the impact of such improvements on the overall care of patients with acute coronary syndromes will be less than optimal.
Educating the general public as well as patients at risk of CAD about the symptoms of acute coronary syndrome and the possibility of early treatment could be beneficial, although the impact of previous (mostly short-term) educational campaigns appears to be moderate30. It may be that long-term, low intensity campaigns (even starting in schools) that increase awareness of CAD in the community would be more effective.
Study limitations
The number of patients studied was not large, partly due to inclusion criteria that required participants to be confirmed as having had a myocardial infarction and to be hospitalized alive in either hospital during the period of the study. This may have limited the findings. Biased information from the patients cannot be excluded. Although many of the findings are consistent with studies from other countries, the study was limited to one region of Greece.
Conclusion
In conclusion, the study has a number of findings of note. Rural patients, despite being older and less educated than their urban counterparts, did not delay longer in seeking assistance, although they were delayed longer in reaching hospital once they obtained assistance.
The interpretation of symptoms as serious or heart-related shortened the delay for both groups but it is still unacceptably long for this region of southern Europe.
Finally, in addition to educational programs promoting early and correct recognition of cardiac symptoms, the National Health System in rural Greece needs to move towards a more effective system of dealing with emergencies such as myocardial infarction.
References
1. Gruppo Italiano per lo Studio della Streptochinasi nell'Infarto Miocardico (GISSI). Long-term effects of intravenous thrombolysis in acute myocardial infarction: final report of the GISSI study. Lancet 1987; 2(8564): 871-874.
2. The Gusto Investigators. An international randomised trial comparing four thrombolytic strategies for acute myocardial infarction. New England Journal of Medicine 1993; 329(10): 673-682.
3. Grines CL, Browne KF, Marco J. A comparison of immediate angioplasty with thrombolytic therapy for acute myocardial infarction. The Primary Angioplasty in Myocardial Infarction Study Group. New England Journal of Medicine 1993; 328(10): 673-679.
4. Dracup K, Moser DK, Eisenberg M, Meischke H, Alonzo AA, Braslow A. Causes of delay in seeking treatment for heart attack symptoms. Social Science and Medicine 1995; 4(3): 379-392.
5. Wielgosz AT, Nolan RP, Earp JA, Biro E, Wielgosz MB. Reasons for patients' delay in response to symptoms of acute myocardial infarction. Canadian Medical Association Journal 1988; 139(9): 853-857.
6. Turi ZG, Stone PH, Muller JE, Parker C, Rude RE, Raabe DE. Implications for acute intervention related to time of hospital arrival in acute myocardial infarction. American Journal of Cardiology 1986; 58(3): 203-209.
7. Schmidt SB, Borsch MA. The prehospital phase of acute myocardial infarction in the era of thrombolysis. American Journal of Cardiology 1990; 65(22): 1411-1415.
8. Moss AJ, Wynar B, Goldstein S. Delay in hospitalization during the acute coronary period American Journal of Cardiology 1969; 24: 659-665.
9. Rawles J, Sinclair C, Jennings K, Ritchie L, Waugh N. Call to needle times after acute myocardial infarction in urban and rural areas in northeast Scotland: prospective observational study. BMJ 1998; 317(7158): 576-578.
10. Murphy AW, McCafferty D, Dowling J, Bury G. One-year prospective study of cases of suspected myocardial infarction managed by urban and general practitioners. British Journal of General Practice 1996; 46(403): 73-76.
11. Thuresson M, Jarlov MB, Lindahl B, Svensson L, Zedigh C, Herlitz J. Thoughts, actions, and factors associated with prehospital delay in patients with acute coronary syndrome. Heart Lung 2007; 36(6): 398-409.
12. National Statistical Service of Greece. Demographic data, Vol II. Athens: National Statistical Service of Greece, 2001.
13. Aravanis C, Corcondilas A, Dontas AS. Coronary heart disease in seven countries. IX. The Greek islands of Crete and Corfu. Circulation 1970; 41(Suppl4): 88-100.
14. Menotti A, Lanti M, Puddu PE, Kromhout D. Coronary heart disease incidence in northern and southern European populations: a reanalysis of the seven countries study for a European coronary risk chart. Heart 2000; 84(3): 238-44.
15. Rawles JM. Quantification of the benefit of earlier thrombolytic therapy: five-year results of the Grampian Region Early Anistreplase Trial (GREAT). American Journal of Cardiology 1997; 30(5): 1181-1186.
16. Bloe C, Mair C, Call A, Fuller A, Menzies S, Leslie SJ. Identification of barriers to the implementation of evidence-based practice for pre-hospital thrombolysis. Rural Remote Health 9: 1100. (Online) 2009. Available: www.rrh.org.au (Accessed 29 April 20100).
17. Cobbe SM. Thrombolysis in myocardial infarction. BMJ 994; 308(6923): 216-217.
18. Rawles JM, Haites NE. Patient and general practitioners delays in acute myocardial infarction. BMJ 1988; 296(6626): 882-884.
19. Khraim FM, Carey MG. Predictors of pre-hospital delay among patients with acute myocardial infarction. Patient Education and Counselling 2009; 75(2): 155-61.
20. Horne R, James D, Petrie K, Weinman J, Vincent R. Patients' interpretation of symptoms as a cause of delay in reaching hospital during acute myocardial infarction. Heart 2000; 83(4): 388-393.
21. Broer J, Bleeker JK, Bouma J, de Jongste MJ, Erdman RA, Meyboom-de JB. Regional differences in prehospital time delay for patients with acute myocardial infarction; Rotterdam and Groningen, 1990-1995. Nederlands Tijdschrift voor Geneeskunde 2000; 144(2): 78-83.
22. Ottesen MM, Dixen U, Torp-Pedersen C, Køber L. Prehospital delay in acute coronary syndrome - an analysis of the components of delay. International Journal of Cardiology 2004; 96(1): 97-103.
23. Rasmussen CH, Munck A, Kragstrup J, Haghfelt T. Patient delay from onset of chest pain suggesting acute coronary syndrome to hospital admission. Scandinavian Cardiovascular Journal 2003; 37: 183-186.
24. Goldberg RJ, Spencer FA, Fox KA, Brieger D, Steg PG, Gurfinkel et al. Prehospital delay in patients with acute coronary syndromes (from Global Registry of Acute Coronary Events [GRACE]. American Journal of Cardiology 2009; 103(5): 598-603.
25. Maynard C, Althouse R, Olsufka M, Ritchie JL, Davis KB, Kennedy JW. Early versus late hospital arrival for acute myocardial infarction in the Western Washington thrombolytic therapy trials. American Journal of Cardiology 1989; 63(18): 1296-1300.
26. Schroeder JS, Lamb IH, Hu M. The prehospital course of patients with chest pain. Analysis of the prodromal, symptomatic, decision-making, transportation and emergency room periods. American Journal of Medicine 1978; 64: 742-748.
27. Ottesen MM, Køber L, Jørgensen S, Torp-Pedersen C. Determinants of delay between symptoms and hospital admission in 5978 patients with acute myocardial infarction. The TRACE Study Group. Trandolapril Cardiac Evaluation. European Heart Journal 1996; 17: 429-437.
28. Alonzo AA. The impact of the family and lay others on care-seeking during life-threatening episodes of suspected coronary artery disease. Social Science and Medicine 1986; 22(12): 1297-1311.
29. Lefler LL, Bonty KN. Women's delay in seeking treatment with myocardial infarction: a meta-synthesis. Journal of Cardiovascular Nursing 2004; 19: 251-268.
30. Blohm MB, Hartford M, Karlson BW, Luepker RV, Herlitz J. An evaluation of the results of media and educational campaigns designed to shorten the time taken by patients with acute myocardial infarction to decide to go to hospital. Heart 1996; 76: 430-434.
