Introduction
Of the estimated 314 million people who are visually impaired, more than 90% live in developing countries. Approximately one-fifth of these live in Africa1. More than three-quarters of visual impairment could be prevented or treated by an appropriately trained healthcare workforce with the relevant infrastructure to support them. However, Africa has insufficient healthcare providers. For example, it is estimated that 1 million extra health workers would have to be trained by 2010 to meet the targets of the UN Millennium Development Goals2. To help overcome this, the efficiency of the current healthcare workforce could be increased if human resources, materials, and financial management systems were well managed3,4. Well trained non-clinical managers could support the delivery of efficient and effective health care that is accessible to as many people possible. This would allow clinicians to concentrate on providing much needed health care4. In Sub-Saharan Africa, many eye care managers progress through clinical career-pathways and are ophthalmologists, ophthalmic clinical officers or optometrists. Many assume management roles in eye care programs without any formal management training.
Training courses should adequately prepare graduates for the tasks they need to undertake. Although the generic principles of management courses offered on different continents are similar, the context and setting are vastly different between, for example, India and Africa. Therefore, the direct appropriation of an Indian course for African eye care program managers would likely be inappropriate. Also, experience has shown that courses frequently do not permit adequate time for participants to learn and apply all that is required by the course and their employment. This is particularly so for 'short courses', but is not limited to these. The result is that despite attending formal training, as with public sector hospital managers in South Africa5, many feel unprepared for the responsibilities of their job. Also, many program management courses do not result in a formally recognized qualification. This frequently leaves graduates without the prospect of career progression or the authority to implement plans6.
In response to the need for personnel with skills to manage eye care programs in Africa, and a desire for recognition of their training, a Postgraduate Diploma in Community Eye Health course (PGDCEH) was proposed at the University of Cape Town (UCT).
To avoid inappropriate and/or ineffective training, a competency-based approach for the PGDCEH course was adopted. Many other courses, including ophthalmology, have adopted this approach7,8. Using this approach, the learning content reflects the actual skills required after graduation, both faculty and students have clarity on learning outcomes expected, and student assessment can be based on and be appropriate to these learning outcomes. Consequently, the focus becomes the outcome of the education, rather than the education process (ie how knowledge, skills and attitudes are applied, rather than how knowledge is gained)8,9. In addition, concentrating on competencies helps differentiate the role of the eye care manager from those of other members of the eye care team, and provides a framework for the performance evaluation of graduates when they return to their workplace. The result is accountability in education and, ultimately, to the public10.
This article reports on the assessment of the requirements for a human resource capacity development strategy, specific to Sub-Saharan Africa: the role and tasks expected of eye care managers in this region, competencies from related fields, and the corresponding competencies that would form the basis of a postgraduate education course. Comment is made about the curriculum development process, its outcome, and the next steps to ensuring the resultant course has a favorable impact on eye health. The objective of this undertaking was to develop a competency-based curriculum that could guide the course towards the application of knowledge and skills, with the expectation that this would enhance the workplace performance of the graduates. During the course, competencies, expressed as measurable behaviour, could also be used to evaluate competence independent of the performance of other learners. After the course, these competencies could be used for ongoing evaluation of the graduates' performance. Furthermore, documented competencies serve to communicate the expected outcomes of the course to learners and other interested parties.
Methods
A widely consultative process was used to gather information to guide the curriculum development. Clinicians, eye care managers, heads of eye care programs and public health professionals from eye care training institutions were consulted. A core team consisting of community eye health clinicians, managers and faculty from UCT initiated the curriculum development process. Two of the present co-authors formed part of this core team. The first draft of the curriculum was distributed for review and comment to ophthalmic and public health professionals at several institutions that provide eye care management training.
In February 2008, a training curriculum review meeting was held to evaluate the existing training programs available to eye care programs in Sub-Saharan Africa. Heads of eye care programs, non-government organization representatives, national blindness prevention coordinators, and faculty and directors of training institutions participated in this structured three-day curriculum planning meeting. The meeting included a workshop component to encourage interaction. A highly regarded academic with international expertise in eye health development, especially in Sub-Saharan African programs, facilitated the discussions. The UCT team presented the proposed draft curriculum, and the different groups negotiated the merits of including or excluding certain components from the course. The meeting reached consensus on job descriptions and the knowledge that eye care managers would require. This information formed the basis of the PGDCEH curriculum. A faculty member from an external training institution (the first author) collected information from focus group discussions about the perceived role and tasks of eye care managers from ophthalmologists and eye care managers from the same geographical area and also from the literature. The minutes of curriculum planning meetings and the PGDCEH curriculum were examined to identify content areas and the required knowledge for associated practical application.
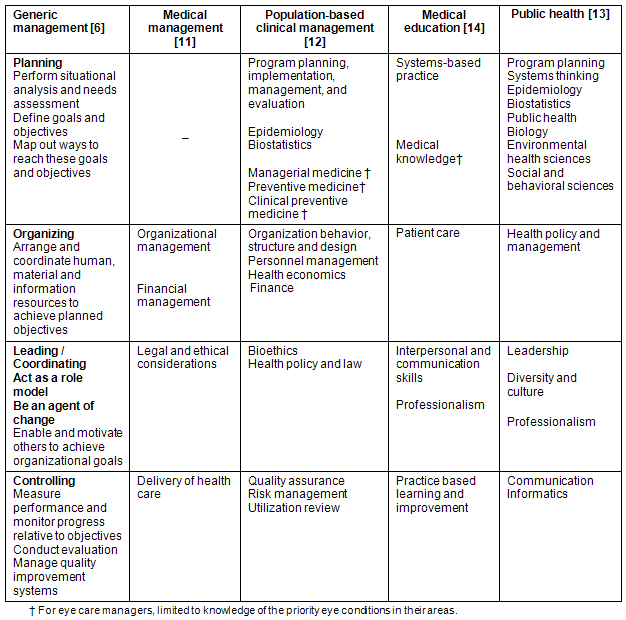
For the purposes of this article, competencies have been defined as the 'knowledge, skills, attitudes and personal qualities that an individual needs to effectively fulfill a particular set of functions, occurring across disparate job descriptions and employment situations'9. The generic competencies and skills required by managers6 as well as the documented competencies for hospital-based managers6, medical managers11, population-based clinical managers12, public health13, and medical education14 were explored. Fayol's classical management function framework (planning, organizing, leading/coordinating [implementing] and controlling [monitoring, evaluation and learning]) was used to organize these data15.
Albanese's five theory-based criteria were used to guide the development of competencies for this course9. Consequently the competencies are expressed as measurable behaviours, focusing on the expected performance of the graduates, to ensure the course content is aligned to the application of knowledge and skills. Furthermore, because the standards used for assessing competence are independent of the performance of other learners, this facilitates criterion-based assessment for this course. These also serve to inform learners and others about the outcomes expected after the course.
Results
There was considerable overlap and agreement between the perceptions of ophthalmologists and eye care program managers as to the role and tasks of the managers. However, there was difference in emphasis. The heads of eye care programs (non-government organization representatives and national blindness prevention coordinators) focused on the knowledge and understanding that an eye care manager should possess (Tables 1,2). The key differences in emphasis are indicated in the tables in italicized font.
The core expectations of what is required of eye care managers (Tables 1,2) were in keeping with what are regarded as generic management competencies and skills (Table 3)6. However, there was an expectation (Tables 1,2) of a wide range of additional competencies (eg population/public health, including eye health promotion; clinical/medical eye care) because these would be necessary in the provision of comprehensive eye care services. These were commensurate with the competencies specified for medical and population-based clinical management, medical education and public health (Table 3)6. Research focused, and more analytical skills such as epidemiology and biostatistics were considered less relevant to the tasks of an eye care manager and were therefore excluded. Public health biology and environmental health sciences were also excluded.
Program heads, eye care managers and ophthalmologists made little reference (Tables 1,2) to the broader aspects of eye care (eg patient-based care or considering care from a patient point of view; how eye care interacts with the larger health context; system and ethical/legal aspects of eye care provision). However, the consultation process that involved ophthalmic, population public health and education expertise ensured that a consensus of broader competencies was ultimately incorporated into the PGDCEH (Fig1; Appendix I).
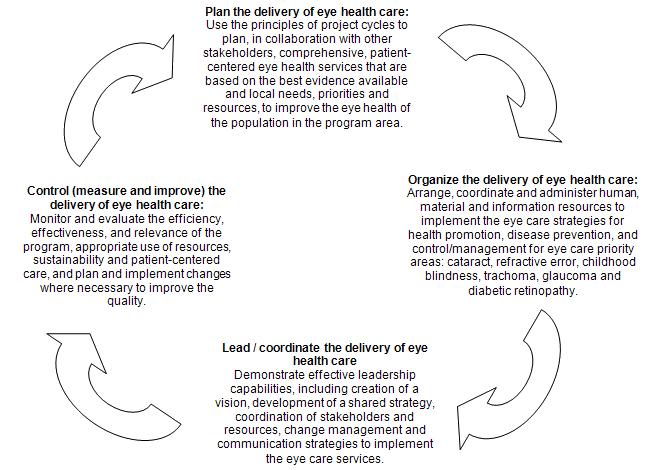
Figure 1: Competency areas for eye care managers as presented in the University of Cape Town Postgraduate Diploma in Community Eye Health curriculum.
Table 1: Definitions of the role of a Sub-Saharan eye care manager
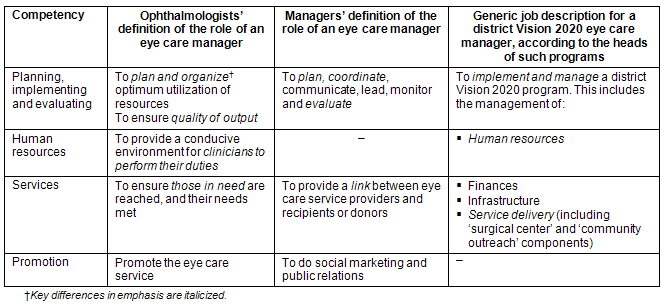
Table 2: Definitions of tasks/ 'generic competencies' of a Sub-Saharan eye care manager
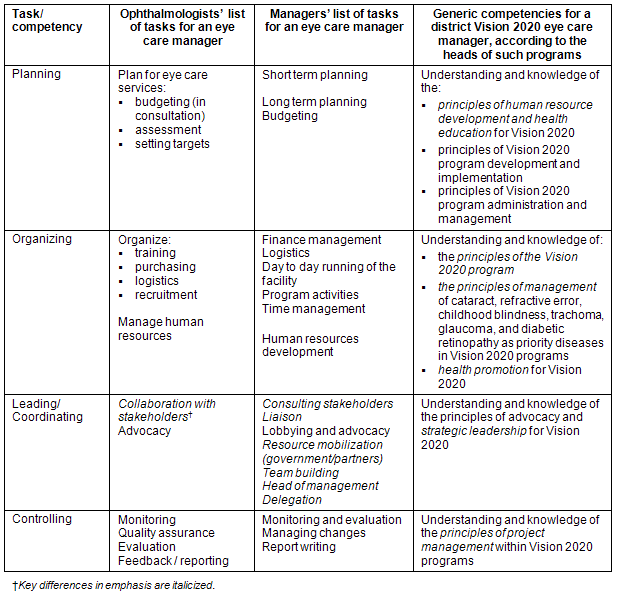
Table 3: Competency areas for generic, medical and population-based clinical management, and medical education and public health6,11-14
The curriculum is composed of a combination of on-campus and remote study blocks to optimize the opportunities for knowledge assimilation and experiential learning in the workplace. Much deliberation was required to finalize the logistics and feasibility of these components. Once these components were finalized, the curriculum was submitted to the stringent approval processes of the Higher Education Qualifications Authority of South Africa (HEQA). Guided by the rules and standards of HEQA, the UCT-based faculty modified the curriculum content and structure, and as requested. In particular, HEQA required more details about the activities and outcomes envisaged for the remote component of the course curriculum. After submission of the revised curriculum, the program was accepted and entered into the University's academic program for implementation in 2009.
Conclusions
A systematic process, informed by best available evidence from the literature and stakeholders from a wide experience base, was used to develop a competency-based curriculum (Appendix I) anchored in the realities of providing eye care in Sub-Saharan Africa. This ensured that the curriculum was in concordance with the expected combination of generic competencies and skills required by eye care managers and those needed for medical and population-based clinical management, medical education and public health (Table 3). It is anticipated that this curriculum will enhance the effectiveness of training eye care program managers and the resultant management-related performance after training.
The process of developing competencies to be taught in the PGDCEH was participatory. In the first instance, a range of workers in the field (clinicians, program directors and eye care managers) were used to define the role, tasks and generic competencies required of an eye care manager. Each group gave emphasis to different functions and skills, depending on their own work experience and perspective. This enriched the quality of the raw material on which the final competencies were based. Also importantly, this process garnered ownership and buy-in by those who in the future may be recommending or selecting candidates to attend this course.
The process was further strengthened by the use of a multidisciplinary group of experts who, with a wider public health and education perspective, finalized the competencies. This ensured that essential aspects such as the provision of patient-centered care, ethical/legal issues and systems thinking, which had been ignored by the primary informants, were included. These are necessary for the provision of good quality comprehensive eye care services, integrated with general health care, and to ensure continued utilization of services and service sustainability.
However, the pursuit of a quality education experience delivering competent graduates able to implement workplace activities and produce favorable impact on eye health does not conclude here. Teaching faculty require information, training and support to facilitate the implementation of this competency-based curriculum. It is this information and the emphases placed within it that will further differentiate an African course from those from other parts of the world. Also, appropriate assessment of student learning must be organized7,16,17.
This assessment of required eye care manager competencies further provides the basis for future evaluation of the appropriateness of the curriculum, and the impact of the eye care managers' training program on eye care service delivery in Sub-Saharan Africa. A widely available, but indirect measure of the effectiveness of the course is assessing the cataract surgical rates of the districts with formally trained eye care managers. However other more direct indictors and qualitative information will be collected for ongoing evaluation and modification of the course to enhance the learning experience and increase its effectiveness. In a continuing process of refinement, the competencies will be evaluated for relevance and relative importance to the everyday work of eye care managers. Existing eye care managers, graduates of the course, employers and other stakeholders will be asked to rate these and provide an assessment of their perception of the proficiency required for each. This information may then be used to modify the competencies, improve course teaching (including appropriation of increased time to competencies deemed more important or difficult to acquire) and assessment, and/or plan continuing or refresher education18,19.
References
1. Resnikoff S, Pascolini D, Etya'ale D, Kocur I, Pararajasegaram R, Pokharel GP, et al. Global data on visual impairment in the year 2002. Bulletin of the World Health Organisation 2004; 82(11): 844-851.
2. World Health Organization. High level forum on the health MDGs. Addressing Africa's health workforce crisis: an avenue for action. (Online) 2004. Available: www.hlfhealthmdgs.org/Documents/AfricasWorkforce-Final.pdf (Accessed 1 July 2009).
3. Rowe AK, de Savigny D, Lanata CF, Victora CG. How can we achieve and maintain high-quality performance of health workers in low-resource settings? Lancet 2005; 366(9490): 1026-1035.
4. Lewallen S, Kello A. The need for management capacity to achieve VISION 2020 in Sub-Saharan Africa. PLoS Medicine 2009; 6: e1000184.
5. O'Neil ML. Human resource leadership: the key to improved results in health. Human Resources in Health 2008; 6: 10.
6. Pillay R. Managerial competencies of hospital managers in South Africa: a survey of managers in the public and private sectors. Human Resources in Health 2008; 6: 4.
7. Golnik KC, Lee AG, Wilson MC. A national program director survey of the shift to competency-based education in ophthalmology. Ophthalmology 2008; 115(8): 1426-1430.
8. Gukas ID. Global paradigm shift in medical education: issues of concern for Africa. Medical Teacher 2007; 29(9): 887-892.
9. Albanese MA, Mejicano G, Mullan P, Kokotailo P, Gruppen L. Defining characteristics of educational competencies. Medical Education 2008; 42(3): 248-255.
10. Knebel E, Puttkammer N, Demes A, Devirois R, Prismy M. Developing a competency-based curriculum in HIV for nursing schools in Haiti. Human Resources in Health 2008; 6: 17.
11. Halbert RJ, Bokor A, Castrence-Nazareno R, Parkinson MD, Lewis CE. Competencies for population-based clinical managers. A survey of managed care medical directors. American Journal of Preventive Medicine 1998; 15(1): 65-70.
12. Lane DS, Ross V. Defining competencies and performance indicators for physicians in medical management. American Journal of Preventive Medicine 1998; 14(3): 229-236.
13. Calhoun JG, Ramiah K, Weist EM, Shortell SM. Development of a core competency model for the master of public health degree. American Journal of Public Health 2008; 98(9): 1598-1607.
14. Swing SR. The ACGME outcome project: retrospective and prospective. Medical Teacher 2007; 29(7): 648-654.
15. Fells MJ. Fayol stands the test of time. Journal of Management History 2000; 6(8): 345.
16. Frank JR, Danoff D. The CanMEDS initiative: implementing an outcomes-based framework of physician competencies. Medical Teacher 2007; 29(7): 642-647.
17. Burdick W. Challenges and issues in health professions education in Africa. Medical Teacher 2007; 29(9): 882-886.
18. Axworthy S, MacKinnon NJ. Perceived importance and self-assessment of the skills of Canada's health-system pharmacy managers. American Journal of Health System Pharmacy 2002; 59(11): 1090-1097.
19. Rademakers JJ, de Rooy N, Ten Cate OT. Senior medical students' appraisal of CanMEDS competencies. Medical Education 2007; 41(10): 990-994.
___________________________
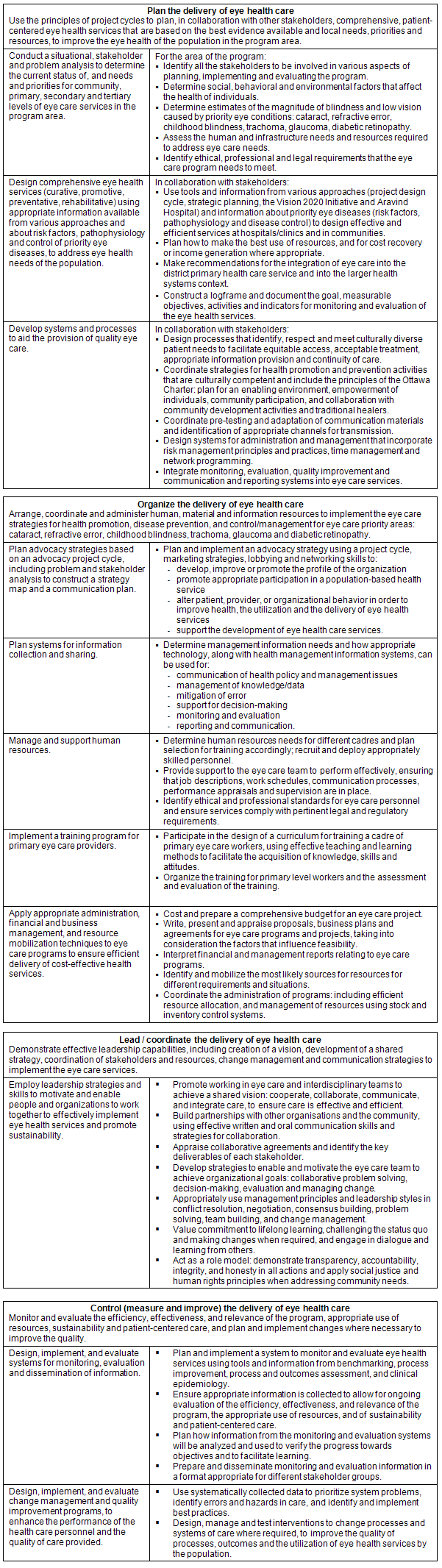
Appendix I: Competencies for eye care managers: University of Cape Town Postgraduate Diploma in Community Eye Health