Introduction
Health care in rural Australia is strained due to poor funding1-3, a lack of medical staff4,5 and the size of the geographical catchments for rural hospitals5. This extends to the acute-care setting, directly affecting emergency departments (EDs). In rural areas a small number of people live in a vast area and patients with emergency medical needs may need to travel long distances for treatment6. Furthermore, the demographics of those who live in rural areas are different from the urban population, and this is reflected by a shift in age and cultural background among patients presenting to EDs3,7,8.
Understanding the demographics of these ED patients provides a way for rural hospitals to tailor their emergency services. However, there are few published studies that provide this information.
The present study aimed to establish patient numbers and demographics for those presenting to the ED of Cobram District Hospital (CDH), a rural hospital in the Australian state of Victoria. Daily and seasonal variations were also assessed, as was the catchment area and triage status of individual patients.
Cobram background information
The town of Cobram is on the Victoria-New South Wales (NSW) state border. Cobram's twin town in NSW, Barooga, is the only town in NSW that shares a Victorian postcode. According to the 2006 census, 5531 people reside in Cobram9 and 16549 in Barooga. The population of Cobram is mainly non-Indigenous Australian (84%)10,11; however, there is an increasing number of immigrants from Italy, Britain, Iraq and The Netherlands10,11. Like most rural areas, Cobram has a higher proportion of ageing residents than the average population of Victoria13, with 11.9% of the town's residents aged between 60 and 84 years, compared with 9.3% of the Victoria average11,12.
Background information on Cobram District Hospital and the emergency department
The CDH is solely funded by the Victorian government13. Despite this, CDH provides medical services to residents in Cobram and the surrounding areas on both sides of the Victorian-NSW border. Hospital facilities include a 17 bed ward for medical, surgical and palliative in-patient care. The CDH also has non-government funded X-ray, ultrasound and pathology services as well as an on-site GP clinic. The ED does not qualify for government funding because it does not see the requisite 5000 patients each year. Therefore, the patients are seen and billed privately by each attending physician.
The ED has a total of 3 non-publicly funded beds. Registered nurses are diverted from the inpatient units as needed to attend to patients presenting to the ED. Patients are triaged by the nurse who also administers basic and some advanced treatments, as per hospital protocols and specific training. If the nurse is able to provide the appropriate treatment required, he or she can discharge the patient without immediate review by a doctor. At the nurse's discretion, an on-call visiting medical officer GP is requested to attend the ED to review the patient for a decision about further treatment, admission or discharge.
The CDH physicians (VMOs) have multiple roles, including ward duty in the morning, GP clinics throughout the day and on-call for the ED.
Methods
All ED data from the 3 financial years July 2005 to June 2008 were collected retrospectively from medical records and analysed by two investigators not employed by or affiliated with CDH. Two separate datasets were compiled: patients presenting to the ED; and patients admitted as inpatients to CDH via the ED.
Parameters recorded included:
- the number of patients presenting to the ED
- the number of patients admitted to CDH as inpatients via the ED
- the date and time of presentations
- patients' Australasian Triage Scale (ATS) category (according ATS guidelines, Appendix I)
- patient details of sex, age group, postcode and state of residence.
The data were entered into MS Excel spreadsheets and tables and figures generated. From postcode data, maps were created in GoogleMaps and with graphic imaging software (Adobe Photoshop; Adobe Systems Inc; http://www.adobe.com).
Results
Patients by year
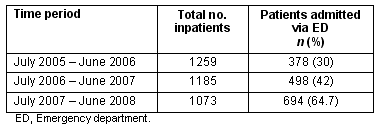
The number of presentations per year to ED remained under 5000 (Table 1); however, the number and percent of inpatients admitted from the ED increased during the 3 year period (Table 2). During this time the total number of CDH inpatients per year decreased from 1259 to 1073.
Table 1: Number of presentations to the emergency department, according to time period
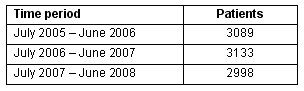
Table 2: Number of patients admitted via the emergency department, according to time period
Patient presentations by month
The greatest number of emergency presentations occurred in December (n = 320), with another small increase in March. The lowest number of presentations were in June (n = 214) (Fig1).
Patient presentations by time of day
The number of patient presentations rose steadily 06.00 to approximately 19.00. During this period there were 3 obvious peaks at 08.00, 14.00 and 19.00 (Fig2). Patient numbers dropped sharply after 19.00 and remained low until 06.00 the following day. In all, 40% of patients presented between 18.00 and 24.00, with 70% between 12.00 and 24.00.
Patients by age group
The age distribution of this patient population consisted predominantly of patients above 60 years, with a mean age of 70.3 years (Fig3). There were relatively few paediatric or young adult patients presenting to the ED.
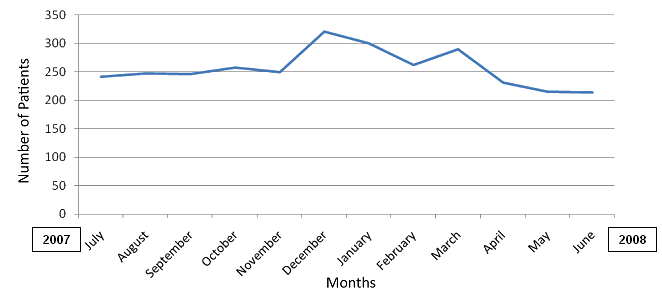
Figure 1: Number of emergency department patients per month, July 2007 to June 2008.
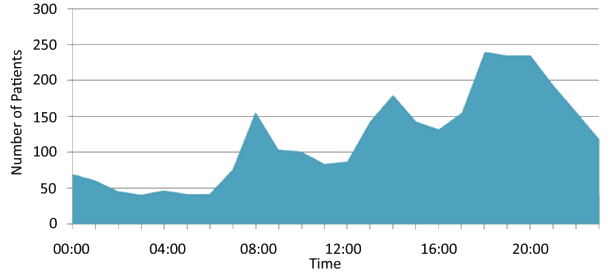
Figure 2: Average number of patients presenting to the emergency department by time, July 2007 to June 2008.
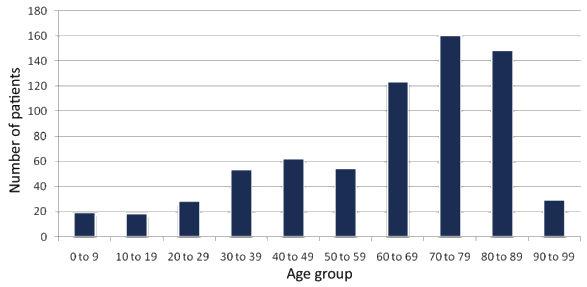
Figure 3: Age profile of patients presenting to the emergency department, July 2007 to June 2008.
Patients by location of residence
The majority of patients (2589/2998, 86%) presenting to the CDH ED came from the postcode 3644, which represents the sister towns of Cobram and Barooga (Table 3). However a significant number (409/2998, 14%) came from NSW. The postcode distribution demonstrates the catchment area of ED patients, compared with the predicted catchment area according to the CDH annual report13 (Fig4).
Patients by Australasian Triage Scale category
Almost 50% of ED patients were classified as ATS category 4, with 73% being either category 4 or 5; category 1 or 2 presentations were infrequent (Table 4).
Table 3: Number of patients by postcode and location admitted as inpatients via the emergency department, July 2007 to June 2008
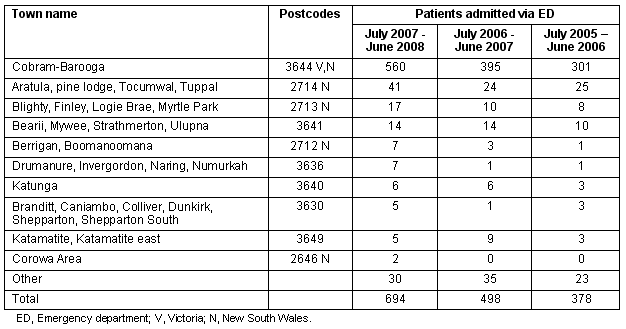
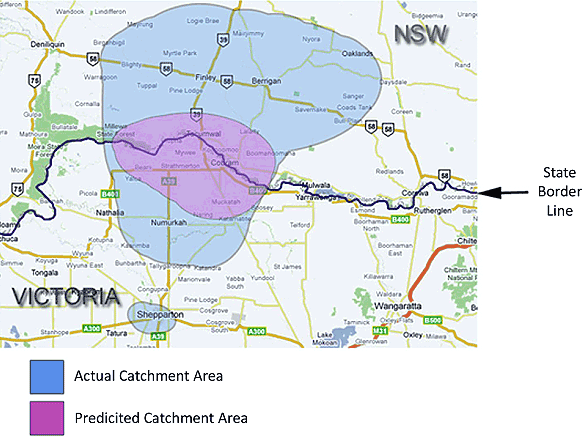
Figure 4: Catchment Area of Cobram District Hospital: predicted versus actual.
Table 4: Number and percentage of ED patients according to Australasian Triage Scale triage categories, July 2007 - June 2008

Discussion
The number of patients presenting to the CDH ED has remained stable over the past 3 years, reflecting the steady population of the area9,10; however, the admission rate via the ED has increased from approximately 11% to 22% of presentations. This suggests that sicker patients are being seen in the ED. Although the number of admissions to the hospital reduced, the number of admissions from the ED increased dramatically. This may have been due to changes doctors' discretion, changes to internal policy regarding criteria for admission, or a change in the types of presenting complaints. A recent decline in general practice physicians in Cobram13 could mean that patients are being diverted from GP clinics to the ED.
The increase in patient numbers in the warmer months, especially in December, coincides with an influx of tourists during the Christmas holidays and fruit pickers who work seasonally in local orchards. Outdoor activities among residents also rise during the warmer months; however, the admission data is heavily skewed to older age groups, among whom social and non-medical issues strongly influence the admission decision, and this is common among rural hospitals.
The number and time distribution of presentations suggests one ED patient presents every night. The on-call roster is shared between 3 to 4 doctors, and providing after-hours care may therefore be burdensome.
Our data identified 3 patient presentation time peaks and a steady baseline increase from 06.00 to approximately 19.00. This information, combined with data about after-hours presentations, will assist the ED staff to prepare for patients fluctuations.
The CDH sees relatively few paediatric and young adult patients, in common with most Australian hospitals14,15. The majority of patients are ≥60 years, with many over 70 and 80 years, which confirms the trend in rural health for older patients with a growing burden of disease and complications that require hospitalisation7.
It is not surprising that the majority (84%) of patients were from postcode 3644, which represents Cobram and its twin town Barooga. However, a significant proportion (16%) of patients came from NSW and, as Barooga is a NSW town with a Victorian postcode many of these patients are treated as Victorian. This cross-border health service delivery is problematic for CDH in terms of funding. Current state government policies about funding and access to health services require state governments only to provide medical funding for residents living in their respective states. Therefore the Victorian-based CDH currently provides ED facilities for many NSW residents without government financial support.
This situation may be alleviated by a nationalised hospital funding and healthcare system, which would eliminate cross-state access boundaries. Alternatively, CDH could apply for additional funding to cover patients from NSW. Similar problems have been identified in other towns, indicating this is a widespread issue in Australia16.
The catchment area of CDH appears significantly larger than predicated, which places an additional burden on the resources of CDH, for example in increase travel times and distances for the ambulance. Patients who live more than 2 hours away by road may suffer worse outcomes in an emergency situation. However, the postcode of residence data should be interpreted with caution. It is possible that some patients with a distant postcode may have been temporarily living in or travelling close to CDH at the time of their emergency.
Problems and limitations with data
Several problems have been identified concerning the recorded dataset, which was drawn directly from records maintained at CDH at the time of collection. That the data relate to a single centre is a major limitation to the study. In addition, the ED data were not computerised prior to 2005, so long-term trends cannot be established.
The data manager at CDH only works on-site once a month, which significantly delays data entry and access. While the funding of a dedicated data manager may not be possible for a small rural hospital, the data management tasks could be shared among administration and nursing staff.
In addition, the ED data were divided among multiple computer and handwritten databases, which prevented prompt access. The data were also incomplete or contained errors. Record-keeping must be improved and this may be achieved by educating nurses in data entry, or compiling data centrally (eg by an on-site manager).
The postcodes of patients were only recorded if they were admitted to the medical ward. Therefore analysis was restricted to the population of patients admitted via the ED. However, these data can be extrapolated to represent the full population presenting to the ED, assuming that the decision to admit a patient was not biased to the origin of residence.
Residents of Barooga share the same postcode (3644) as Cobram and this may have caused an underestimation of the number of NSW residents treated at CDH. To clarify this the records of patients from postcode of 3644 should clearly show their state of origin.
The difficulty of rural emergency healthcare for physicians
The Cobram rural physicians face similar everyday challenges to other Australian rural doctors. These are a combination of medical, social and geographical challenges. For example, the hospital and on-call arrangements may be unfavourable for many GPs and access to continuing medical education is not readily available. Moving to a rural location such as Cobram can place a strain on the family, with fewer employment opportunities for the partner and fewer educational options for their children. The geographical isolation of the town may mean living away from close family and friends. However remuneration, lifestyle and more affordable housing are all positive factors17.
In the past 3 years the number of GPs in Cobram dropped from 11 to 4. The four remaining doctors have been working increasingly longer hours, especially in their private clinics. The hospital works entirely on an on-call system. The doctors perform a swift ward round in the early morning and attend patients at their private clinic for the rest of the day, while one doctor remains on-call for the ED for after office hours. The burden on the remaining doctors is becoming increasingly heavy, especially with the steady number of patients presenting to the ED and an increase of in-patient admissions.
One of the difficulties of rural practice is the low number of category 1 patients (only 11 in 3 years). Given that the number of doctors has reduced, it is likely that any doctor would only see patient requiring resuscitation each year. It is difficult to maintain critical care skills without regular onsite experience.
Conclusion
The ED of CDH sees approximately 3000 patients per year. The majority of patients are over 60 years of age and there is a significant number of patients presenting from NSW. Twice as many patients present to CDH ED during the warmer months, compared with winter. Furthermore, the majority of patients present during the afternoon, night and outside business hours. Only 2% of all emergency patients are ATS categories 1 and 2, while 73% are categories 4 and 5. Incorrect record keeping presented difficulties when analysing the data but the introduction of simple protocols could minimise this. This demographic data has implications for health policy and should be of concern to administrators and policy-makers planning future resource allocation.
Acknowledgements
The authors thank all the staff at CDH for their support and assistance, in particular: Nick Bush (CEO) for kindly providing us with the support of the hospital; Chelsea Dove (nurse unit manager) for the wonderful clinical support; Jo Duffy (data manager) for assistance with data collection; Gabrielle Ransley (clinical nurse educator) for reviewing the study; and Dr John Best (medical director) for his supportive words.
References
1. Fatovich DM, Jacobs IG. The relationship between remoteness and trauma deaths in Western Australia. Journal of Trauma 2009; 67(5): 910-914.
2. Ruston SA. Extended scope practitioners and clinical specialists: a place in rural health? Australian Journal of Rural Health 2008; 16(3): 120-123.
3. Dunbar J, Reddy P. Integration and coordination of care. Australian Journal of Rural Health 2009; 17(1): 27-33.
4. Henry JA, Edwards BJ, Crotty B. Why do medical graduates choose rural careers? Rural and Remote Health 9: 1083. (Online) 2009. Available: www.rrh.org.au (Accessed 21 January 2010).
. Pond BR, Dalton LG, Disher GJ, Cousins MJ. Helping medical specialists working in rural and remote Australia deal with professional isolation: the Support Scheme for Rural Specialists. Medical Journal of Australia 2009; 190(1): 24-27.
6. Muir J, Lucas L. Tele-dermatology in Australia. Student Health Technology Information 2008; 131: 245-253.
7. Davis S, Bartlett H. Healthy ageing in rural Australia: issues and challenges. Australasian Journal of Ageing 2008; 27(2): 56-60.
8. Schofield DJ, Earnest A. Demographic change and the future demand for public hospital care in Australia, 2005 to 2050. Australian Health Review 2006; 30(4): 507-515.
9. Australian Bureau of Statistics. 2006 Census. Canberra, ACT: Australian Bureau of Statistics, 2006.
10. Australian Bureau of Statistics. Census of Population and housing - 2001 census articles. Canberra, ACT: Australian Bureau of Statistics, 2001.
11. Moira Shire Council. Key Statistics (2006), Moira Shire Council Community Profile. (Online) 2006. Available http://www.moira.vic.gov.au (Accessed 21 January 2010).
12. Australian Institute of Health and Welfare. Rural and remote populations. In: Australia's Health 1998: the sixth Biennial Health Report of the AIHW, cat. no. AUS 10. Canberra, ACT: AIHW, 1998.
13. Cobram District Hospital. Annual Report June 2007-July 2008. Cobram, VIC: Cobram District Hospital, 2008.
14. Committee for Economic Development of Australia. Australia's ageing population: meeting the challenge. Canberra, ACT: Committee for Economic Development of Australia, 2004.
15. Australian Government Department of Health and Ageing. The state of our public hospitals. (Online) 2007. Available: http://www.health.gov.au/ahca (Accessed 21 January 2010).
1. O'Meara PF, Kendall , Kendal L. Working together for a sustainable urgent care system: a care study from south eastern Australia. Rural and Remote Health 4: 312. (Online) 2004. Available: www.rrh.org.au (Accessed 21 January 2010).
17. Meek R, Doherty S, Deans A. Factors influencing rural versus metropolitan work choices for emergency physicians. Emergency Medicine Australia 2009; 21(4): 323-328.
18. Australasian College for Emergency Medicine. Policy on Australian Triage Scale. (Online) 2006. Available: http://www.acem.org.au/media/policies_and_guidelines/P06_Aust_Triage_Scale_-_Nov_2000.pdf (Accessed 21 January 2010).
______________
Appendix I: Australasian Triage Scale guidelines, reproduced with the permission of the Australasian College for Emergency Medicine18

