Introduction
Hearing health in farming communities has been identified as a major issue of concern by Farmsafe Australia and has formed one of their 4 priority health goals and targets1. The levels of occupational hearing loss in agriculture are significant with approximately 60-70% of Australian farmers having measurable hearing loss2, compared with 22-27% of the general Australian community3. This damage is not only restricted to older farmers but has also been identified in younger farming cohorts aged 15-24 years4.
Occupational Health and Safety (OHS) legislation in Australia stipulates that exposure to noise levels above 85 A-weighted decibels (dBA) over an 8 hour period or its sound energy exposure equivalent, poses an unacceptable risk. In the agricultural sector typical sources of noise exceeding this limit include tractors, chainsaws, workshop tools and firearms5.
There are approximately 313 000 people directly employed in the Australian farm sector. While this has retracted considerably due to the on-going drought, it still accounts for approximately 3% of the national workforce6. These individuals are employed on Australia's 155 000 farms, 98.5% of which are family owned and operated7. Hence farmers, farm-workers, bystanders and farm families, including children who may be assisting with farm tasks, are all potentially at risk of noise injury.
Because hearing loss is not traumatic nor visibly apparent, the disabling consequences on the individual, their families and work colleagues are often overlooked and underestimated. For example, there is strong emerging evidence that hearing loss has a significant negative impact on mental health and overall quality of life, in part due to increased social isolation8,9. Furthermore, the impact is widespread and not restricted to noise injury, with individuals with a hearing loss having higher rates of injury in agricultural and other occupational settings10-12. However, the fact remains that hearing loss due to excessive noise exposure is the result of a preventable physical injury to the hearing mechanism.
To investigate methods of addressing noise injury in the agricultural sector using a community-based approach, the Australian Department of Health and Ageing supported a 12 month demonstration intervention. The Better Hearing for Farming Families Project sought to implement local demonstration projects in 3 communities, with specific objectives to improve:
- Awareness of priority noise injury prevention and hearing health practices.
- Access to services providing hearing health advice, screening, assessment and management/devices for those in the farming community with a hearing loss.
- Networking of services in local communities, to sustain the ongoing hearing health needs of farming families.
This article reports on the interventions and its findings, with the long-term aim being to provide insight into ways to reduce the impact of noise injury on farm family members throughout Australia.
Methods
The 3 communities were purposively selected based on geographical considerations, population size, the nature of agricultural production and the level of locally available support. The communities were nominally defined as the Far West, North Coast and New England regions of the state of New South Wales (NSW). Based on Statistical Local Area data13, this selection entailed the involvement of a major regional centre (New England - population 42 000), a rural township (North Coast - population 21 000) and a remote area (Far West - population 32 000), encompassing approximately 25% of the area of NSW (200 000km).
Project management
To oversee the operation of the project, a reference group was convened consisting of relevant stakeholders representing the Australian College of Audiology, NSW Farmers, NSW Health, National Acoustic Laboratories and the Commonwealth Department of Health. In addition, in each of the 3 project communities, small local advisory groups were convened to provide guidance on local factors to be considered in developing and implementing interventions. To assess progress against the project objectives, process measures were defined noting: (i) the coverage of local social marketing initiatives; (ii) service utilization data, where available; and (iii) network linkages and relevant training in hearing health and noise injury prevention. At the conclusion of the project the local advisory groups were each consulted and a formal reference group meeting conducted to elaborate on findings relating to these 3 process measures, examine policy and clinical implications and to define approaches to enhance sustainability.
Hearing information networks
Using social network analysis (SNA) an assessment of the local farm and hearing health networks was undertaken in the New England and North Coast communities to determine the existing information links and referral pathways for farming families. A full description of the SNA process and results are available elsewhere14; however, details assessed included: agency roles in relation to prevention, screening and provision of other hearing services; links over recent times with stakeholders related to the exchange of information; and client referrals. These results were then used to assist in developing interventions in consultation with the local advisory groups.
Increasing awareness
Local social marketing programs were designed for the intervention periods in the New England and North Coast. Strategies were based on feedback from the SNA and on the principles of the Health Belief Model15. Three core messages were included:
- Prevent hearing loss by adopting the hierarchy of health and safety controls: eliminate the hazard; substitute for a less noisy piece of equipment, engineering and design options that limit noise (such as a cabined tractor); use safer work practices by standing away from noisy equipment; and use personal protective equipment such as ear plugs and muffs.
- Maintain existing hearing.
- Improve quality of life by accessing/using hearing services and devices.
An initial phase focused on general awareness-raising using the local media and distributing existing noise injury resources by targeted mechanisms to farmers (eg direct mail-outs from agricultural suppliers, the New South Wales Farmers Association and agricultural show societies). These existing resources included fact sheets specifically developed for farmers relating to noise injury, its impact and how to minimize injury. As the project progressed, additional media promotions included a series of newspaper editorials, advertising for hearing services in local newspapers and the distribution of new hearing health resources.
Noise injury prevention training
Training sessions for stakeholders identified as important information links in their respective areas (as part of the SNA) was undertaken. These sessions covered basic information pertaining to the extent of the problem in rural Australia, how noise injury can be prevented, how farmers can maintain the hearing they have, and the type of local services available if farmers want further assessment. Resources to assist with the transfer of information and uptake by the community were also provided to these stakeholders for their use and dissemination.
Hearing services and information
Service utilization data in the North Coast and New England communities were monitored and reported by Community Health Centres and private providers. In New England, data from 2007 were compared with a matched period in 2008. This was not feasible for the North Coast because the service had only recently commenced. However, to assist in identifying the impact of local advertising and promotion, all new clients were asked why they had come for an assessment.
Far West region
The SNA was not feasible within the vast catchment of the Far West region. However, the local reference committee suggested that audiometric screening be undertaken by visiting several remote agricultural properties (stations) and towns. This would include screening for farmers and those working in agricultural related services, such as professional kangaroo shooters. Given the geographic area covered (approximately 200 000km2), a fly-around service using a small plane (similar to the Royal Flying Doctor Service) was recommended. Acknowledging the socially isolating impact of hearing loss and possible links to mental health, a mental health staff member from NSW Health accompanied the team that included an audiologist and a farm safety specialist. To identify any potential trends, data were analysed comparing the hearing profiles of subjects in the Far West with those for the rest of the state over recent years.
Results
An improved awareness of priority noise injury prevention and hearing health practices, including specific issues that place farm families at greater risk of hearing loss, was demonstrated in several ways.
Awareness
Extensive local media coverage outlined core issues relating to noise injury and ensured wide coverage of information in the target group. Two phases of marketing were conducted incorporating two TV and radio segments at each site, plus the publication of print articles in local papers (8 in New England; 15 in North Coast) and supporting advertising for local hearing services (20 in New England; 12 in North Coast).
The New England advisory group identified a particular need for a new resource relating to hearing protection and shooting. The resource was developed in conjunction with the advisory group and the content validated by experts from the project reference committee. A total of 5000 'shooting' brochures were distributed throughout the 3 project areas by networks that were familiar to farmers and their families (ie agricultural retailers, agricultural show societies and NSW Farmers). Following the project in the latter half of 2008, a further 4500 brochures were distributed through farmer networks in other Australian states.
Complementing the hearing health awareness raising in these communities, information sessions were conducted that were designed specifically for key stakeholders. A major focus was on agricultural retailers (who sell farm equipment and safety resources), with local agricultural high school teachers and senior farming organization representatives also given prominence. In New England and North Coast, 22 and 15 representatives attended these sessions, respectively.
Access
In comparing data from 2007 with that of 2008 when the project operated, providers in New England reported an increase of 26% in service utilization by farmers, although the sample was small (29-39 farmers). Providers from the North Coast reported only one instance where a client had indicated that the local promotion had been central to attending for a hearing assessment. However, the local advisory group identified additional audiometric screening capacity as an important issue. This resulted in the procurement of a mobile screening unit for use at local agricultural field days, which commenced operation in June 2009.
In the Far West, 60 individuals from 7 stations/townships participated in the screening activities. Although the data are limited by the small sample size for this cohort and are not age-standardized, preliminary results for the 41 subjects (mean age 46 years) who use firearms, compared with NSW data (mean age 41.3 years) collected from 1994 to 200816, suggest that firearms usage has a significantly negative impact on hearing profiles in the region (Fig1).
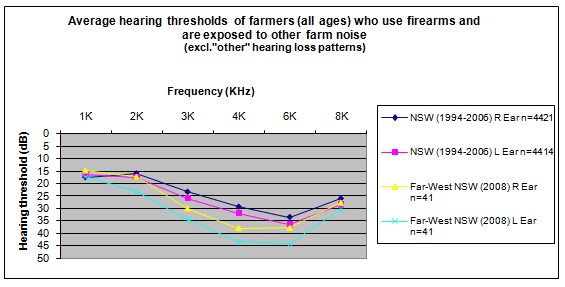
Figure 1: Comparison of audiometric results for farmers who reported using firearms in the Far West (2008) and New South Wales (1994-2006).
Network development
The project advisory groups suggested that greater involvement among agencies working with farmers (other than just audiometry and audiology services) was crucial to effective hearing health promotion. Integration of hearing health promotion within the activities of agencies, such as the Country Women's Association, LandCare and local health services (eg mental health) was strongly recommended.
The general practice divisions covering both communities were involved and were provided with hard copies of resource information for distribution through their clinics. They were also provided with electronic versions of the resources for use in one-on-one client situations and for uploading and on-going use on their respective web sites. In New England this was supplemented by an audiometric training session for practice nurses working with local GPs. In the Far West the Royal Flying Doctor Service also included the electronic resources in its portfolio of patient materials, enabling download at any location for provision to remote patients.
Discussion
This project has demonstrated positive impact on the way hearing health may be improved in farming communities. Although the results should be interpreted with caution, the evidence suggests enhanced community and key stakeholder awareness of hearing health issues, improved service utilization at least one location, and a strengthening/expansion of local networks with knowledge of and an interest in hearing health.
Enhancing the farming communities' awareness and knowledge of hearing as an important health issue is likely to be crucial in overcoming hesitance to reduce further damaging noise exposure and/or undertake a hearing assessment. Studies in occupational noise injury prevention have previously identified a range of barriers that seem equally applicable to the farming sector17. These include optimistic biases that noise injury will not occur personally and/or that the effects are minimal, the discomfort of using hearing protectors, the adequacy and relevance of information, and culture and management issues. This study has illustrated that a coordinated awareness program including direct mail-outs, the use of local media and training for key stakeholders in hearing health issues, and linkage with existing health providers to distribute information, results in improved access to preventive information and may enhance the uptake of treatment services. While distribution of information does not guarantee improved awareness or behavioural change, anecdotal feedback from the local advisory groups suggested the profile of hearing health was raised as a result of these actions.
As in other occupations, farmers frequently defer any action until significant damage and subsequent lifestyle deficits are present17. Consequently, as long as suitable prevention and treatment services are available in a given community, raising the perception of harm (in accordance with the Health Belief Model) may assist in heightening the sense of personal severity of and susceptibility to hearing loss, thereby increasing receptiveness to preventive and hearing screening messages. Presenting hearing damage as a physical injury to which farmers are well accustomed, such as 'bleeding from the ears', may be a useful and practical option in future interventions.
It has also been identified that medium to large businesses tend to have better knowledge and implementation of noise management strategies than small businesses18. Because the majority (approximately 98%) of farming enterprises are small family-based operations7, their self-efficacy for introducing and maintaining noise injury strategies will require ongoing information and support.
To engage farming families, the use of respected and known information sources for the dissemination of information was important. Although several sources were used in this project within each of the 3 communities, focusing on agricultural retailers as a conduit for information appeared particularly successful. Agricultural retailers proved to be adept at enhancing awareness of hearing health while simultaneously providing reliable advice about the suitable purchase and effective use of hearing protectors in a farmer-friendly environment and manner. This relationship could be enhanced at both national and local levels with presentations relating to hearing health at annual merchandising conferences for major agricultural retailers with national reach (eg Landmark, Elders and Wesfarmers in Australia).
The encouraging increase in service utilization in the New England community should be interpreted with caution. While direct cause and effect cannot be demonstrated, the results suggest a positive impact on the uptake of services. Access to hearing screening at convenient locations and times was defined as a major barrier to the use of services. Consequently, steps to alleviate disincentives through the provision of services at suitable locations (eg agricultural field days) is important. Assuming state-based health services may be amenable to supporting staff to complete relevant training and engage in community-based screening activities, there may be potential to work with local community service groups to find sponsorship for the provision of mobile audiometry booths.
The project demonstrated considerable hearing deficits in the Far West, illustrating the unmet need for adult hearing health information and screening in this remote area. The receptivity of participants to hearing health, in particular the preventative information relating to shooting and hearing protection, was very high. Steps to work more closely with remote health service providers nationally (eg Royal Flying Doctor Services) should be undertaken where possible.
There is significant work needed to enhance hearing health networks at a community level. Integrating hearing health with projects delivered by agencies already working with farmers may be a cost-effective form of promotion. The effective distribution of relevant information in Australia could be channelled through rural divisions of general practice, the Mental Health Drought Support Program, Older Farmers Program, General Practice Farmer Health Tool Kits, state farmer conferences, men's health forums, agricultural retailers, rural community groups and rural health gatherings. Such links and pathways must be developed and maintained so that hearing health has a broad network of agencies promoting messages about the prevention of hearing loss and access to hearing services.
Strengths and weaknesses
This is the first community based initiative conducted in Australia to specifically address hearing health in farming communities, and it appears to be the first report of such an intervention in the international literature. Importantly, the results suggest that hearing health program delivery may best be integrated with other issues and the work of existing agencies, rather than being delivered as a stand-alone program.
There were several limitations that impacted on the demonstration project, including the relatively short time-frame (effectively 10 months) and the prolonged drought through vast areas of NSW that made health issues such as hearing loss a low priority for farming families. An outbreak of equine influenza also negatively impacted on the conduct of several locally planned initiatives in New England and the North Coast, while major flooding in the North Coast later in the project further impeded activities. These are typical problems in farming communities where immediate physical difficulties tend to take precedence over longer-term health issues.
Methodologically, the impact of promotions on noise injury awareness and hearing screening utilization proved difficult to assess. Future service evaluations should consider the use of a reply-paid survey with all new clients.
Policy and clinical implications
From a policy perspective, there is potential for introducing incentives to farming families for noise reduction initiatives and screening through insurance companies. Similarly, simplifying the warning system relating to noise exposure/control for building work underway in the construction industry, and introducing the use of hearing protection by a colour coded system should be explored further by farmer agencies and workplace safety authorities.
In relation to providing accessible screening services, mobile hearing screening is not feasible across the expanse of rural Australia. Difficulties include the availability of suitably qualified staff willing to work outside conventional working hours (eg for weekend agricultural field days). Staff also require the support of employing agencies; however, hearing health is rarely viewed as a rural health priority.
Responsibility for the provision of publicly funded hearing screening in NSW rests predominantly with nurse audiometrists working for NSW Health. Throughout Australia there are different state-based arrangements for the integration of publicly funded hearing screening with the respective state/territory health agencies. As well as addressing this variation among states, the support, availability and role of nurse audiometrists within NSW Health (and relevant public providers in other states) as related to conducting hearing health initiatives for farming families, should be evaluated.
Finally, the recent development of the Telscreen self-check hearing assessment may complement the somewhat limited availability of mobile hearing screening services in rural and remote areas of Australia. Telscreen is an initiative of Australian Hearing and it provides a basic assessment of hearing function which can be conducted confidentially over the phone (call 1800 826 500).
Conclusion
For the first time in Australia a project has described how locally based hearing health initiatives for farming families can increase general awareness and strengthen local networks. Several of the project findings require continued action at a national level. However, the project also highlights a potential integration with existing local programs that would enhance hearing health.
Acknowledgements
The Better Hearing for Farming Families Project was funded by the Commonwealth Department of Health. The authors thank all participants and the local advisory groups for their input.
References
1. Farmsafe Australia. Farmsafe goals and targets. Farmsafe Australia Strategic Plan 2002-2007. Moree, NSW: Australian Centre for Agricultural Health and Safety, 2002.
2. Voaklander D, Franklin R, Depczynski J, Challinor K, Fragar L. Evaluation of the NSW Rural Hearing Conservation Program. Sydney: NSW Health, 2006.
3. Williams W, Forby-Atkinson L, Purdy S, Gartshore G. Hearing loss and the farming community. Journal of Occupational Health and Safety - Australia and New Zealand 2002; 18(2): 181-186.
4. Franklin R, Challinor K, Depczynki J, Fragar L. Noise exposure, hearing protection and noise injury in young adult farmers. Moree, NSW: Australian Centre for Agricultural Health and Safety Rural Industries Research and Development Corporation, 2002.
5. Depczynski J, Franklin R, Challinor K, Williams W, Fragar L. Farm noise emissions during common agricultural activities. Journal of Agricultural Safety and Health 2005; 11(3): 325-334.
6. Australian Bureau of Statistics. Australian labour market statistics, cat no. 6105.0. Canberra, ACT: ABS, 2008.
7. Australian Bureau of Agricultural and Resource Economics. Australian commodity statistics, 2007. Canberra, ACT: ABARE, 2007.
8. Chia E, Wang J, Rochtchina E, Cumming R, Newall P, Mitchell P. Hearing impairment and health-related quality of life: The Blue Mountains Hearing Study. Ear Hearing 2007; 28(2): 87-195.
9. Hogan A, O'Loughlin K, Miller P, Kendig H. The health impact of a hearing disability on older people in Australia. Journal of Aging Health 2009; 21(8): 1098-1111.
10. Choi S, Peek-Asa C, Sprince N, Rautiainen R, Donham K, Flamme G et al. Hearing loss as a risk factor for agricultural injuries. American Journal of Industrial Medicine 2005; 48 (4): 293-301.
11. Hwang S, Gomez M, Stark A, St John T, May J, Hallman E. Severe farm injuries among New York farmers. American Journal of Industrial Medicine 2001; 40(1): 32-41.
12. Palmer K, Harris E, Coggon D. Chronic health problems and risk of accidental injury in the workplace: a systematic literature review. Occupational Environmental Medicine 2008; 65(11): 757-764.
13. Australian Bureau of Statistics Census. 2006 Census of Population and Housing, cat. no. 2068.0. Canberra, ACT: ABS, 2008.
14. Lower T, Fragar L, Depczynksi J, Fuller J, Challinor K, Williams W. Social network analysis for farmers' hearing services in a rural community. Australian Journal Primary Health 2010; 16(1): 47-51.
15. Rosenstock I. Historical origins of the Health Belief Model. Health Education Monographs 1974; 2: 328-335.
16. Australian Centre for Agricultural Health and Safety. Rural Noise Injury Prevention Program. Moree, NSW: ACAHS, 2009.
17. Williams W, Purdy S. Factors in reducing occupational noise exposure. Journal of Occupational Health and Safety - Australia and New Zealand 2007; 23(2): 166-171.
18. Williams W, Kyaw-Myint S, Crea J, Hogan A. Occupational noise management: what's happening in industry? Journal of Occupational Health and Safety - Australia and New Zealand 2008; 24(4): 299-307.





