Introduction
Human resources have been described as 'the heart of the health system in any country', 'the most important aspect of health care systems', and 'a critical component in health policies'1,2. Despite the importance of rural health workers, and doctors in particular, to rural health systems, the lack of an adequate rural health workforce is a worldwide issue. Various policies to address this have been reported as decentralization of the location of training institutions, the introduction of recruitment quotas to ensure that the most peripheral areas are represented among medical students, and making rural field experience compulsory during medical training3-7.
Sub-Saharan Africa faces a human resources crisis in the health sector. The demand for improvement in health services is hampered by a scarcity of health workers, especially in rural areas8,9. The severely weakened and under-resourced health systems characteristic of these countries increase the difficulty of producing and recruiting skilled health professionals for underserved areas, and then retaining them10. In order to reduce the critical shortage of doctors in rural areas, it has been suggested that medical students should be provided with rural experience3,11. Rural-based training placements enable urban trainees to overcome the culture shock of relocation to a rural area12.
However, even if graduates are partially trained in a rural environment, the motivation to practice in a rural area comes from a complex interaction of personal, situational and environmental factors4,5,13-15. Understanding these factors and implementing strategies to support them may increase the recruitment and retention of health personnel in rural areas6.
Both educators and health administrators strive to identify factors associated with an acceptance of the rural working environment; however, most studies into these factors have concerned physicians. By enabling medical students to learn in rural communities for significant periods, universities can contribute to meeting the medical workforce needs of the communities they serve while also providing intrinsic educational advantages to their students11,16-18. The decision to practice in a rural area is facilitated by exposure to rural practice during training, having a clear understanding of rural needs and being exposed to rural role models; while knowledge of the rural context and work environment influence the decision to remain there7,15.
Despite plentiful Ugandan health professionals completing their training and a national policy that supports strengthening health care in all areas of the country, many rural and remote areas in Uganda have insufficient health professionals. This is partly due to a failure to recruit, deploy and/or retain health workers in these underserved areas. There is thus an urgent need for effective strategies to address this issue.
With this imperetive, the Makerere University Faculty of Medicine, Uganda, changed the traditional training of medicine and nursing students to a problem-based learning (PBL) curriculum in 2003. The first of the nursing and medicine PBL graduates completed their studies in 2007 and 2008, respectively. A comprehensive evaluation of the PBL curriculum aimed to assess the influence of graduates' training on their choice of workplace. The objective of the evaluation reported here was to assess the influence of training experience on the willingness, readiness and competence to work in rural health facilities. To this end 60 recent graduates of Makerere University Faculty of Medicine, who completed their studies during the transition from traditional to PBL curriculum, were assessed.
Methods
Setting
The assessment was part of the comprehensive Makerere University Faculty of Medicine PBL curriculum evaluation conducted from 19 to 31 October 2008 at Metropole Hotel, Kampala, Uganda.
Participants and curricula
The participants were 60 selected Makerere University graduates:
- 16 medicine or nursing graduates who completed their undergraduate training in 2003 (traditional curriculum, not influenced by PBL)
- 14 medicine graduates who completed training in 2007 (influenced by the PBL curriculum but trained in the traditional curriculum)
- 30 medicine or nursing graduates who completed in 2007 and 2008 and were trained in the PBL curriculum.
The participants were randomly selected to be generally representative of their group. They were listed alphabetically in MS Excel (2003), contacted and invited to participate in the curriculum evaluation. All participants gave written informed consent prior to participation and were assured of confidentiality.
Study design
Using a participatory approach, an open-ended questionnaire was first administered to participants to assess training experience factors that might influence their willingness, readiness and confidence in working in a rural health facility. The issues enquired about included what motivated them to choose a career in a medical field; whether they had ever worked in a rural area; what enhanced their confidence for rural practice; what would discourage them from working in a rural area; and the perceived skills required for successful rural practice. The participants were also asked if they had experiential training at a rural health facility during their undergraduate studies and, if so, which aspects of the community training experience were instrumental in future practice learning. Finally they were asked about factors that could enhance their willingness, confidence and competence to work in a rural health facility in the future.
After completing the questionnaires the participants were asked to record their answers to each question on small cards which were subsequently collected and displayed on notice boards. Participants in the traditional and PBL curricula were then requested to identify criteria for clustering and ranking from their own responses written on the cards. They were permitted to give explanations or clarifications in defense of these. The individual card responses were collected, after which participants were required to cluster the responses according to an agreed thematic area. They then developed and agreed on a theme title for the clustered responses, as well as a ranking system for the suggested responses, based on selected criteria. Some of the issues considered in ranking or prioritizing the responses were feasibility, time, cost-effectiveness, sustainability and social or economic impact.
The group then evaluated each response cluster for relevance (high, medium or low) relative to the others. These factors were compared for graduates trained in the traditional medical and nursing curriculum before and during the implementation of the PBL curriculum, and for graduates trained in the PBL curriculum. The initial questions were further explored during identification of clusters and themes. Throughout ensuing discussions, clarifications and reflections, the information on each card was justified and eventually agreed upon.
Analysis
The open-ended answers from the questionnaires were initially entered in a MS Excel spreadsheet, then reviewed, summarized into related thematic areas and post-coded. These data were analyzed using STATA v 9 (StataCorpLP). The clustered entries were summarized into frequencies. The participants' responses were compared according to training curriculum (PBL or traditional with or without PBL influence).
Ethical considerations
Each participant received an in-depth explanation of the evaluation. Written agreement to participate was requested. The evaluation was approved by Makerere University Faculty of Medicine Ethics Committee.
Results
Participants' age and sex
Of the 60 participants, 26 were female (43.3%) and the mean age was 26.5 ± 2.5 years. The proportion of females in the various curriculum categories were 8/16 (traditional); 9/14 (traditional with PBL influence); and 9/30 (PBL only).
Motivation to seek a career in a medical field
The majority of participants (39 graduates; 65%) reported the desire to save lives or help others as their primary motivation for seeking a career in a medical field (Table 1). The remaining 21 graduates nominated the scarcity of health workers and the many diseases for which there is no cure, as well as personal factors such as the prestige of the profession, family influence, having obtained good grades, a well paying job and job security.
Essential skills for rural practice
Graduates of the traditional and PBL curricula reported clinical, leadership, problem-solving and communication skills as essential to graduates succeeding professionally in rural practice (Table 2).
Table 1: Graduates' motivation for choosing a career in medicine or nursing, according to curriculum
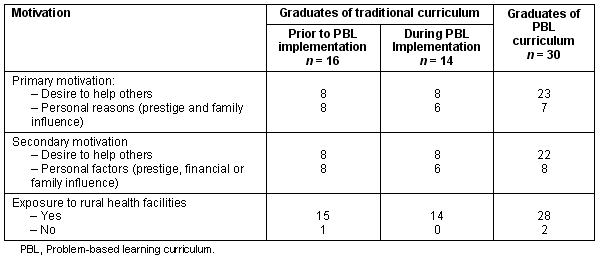
Table 2: Essential skills for graduates' successful rural practice, according to curriculum
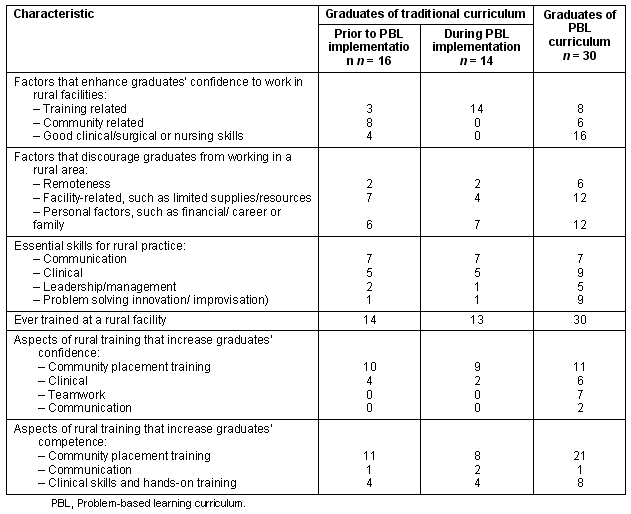
Perceived challenges faced by health workers in rural practice
The respondents identified the following among challenges faced by health workers in rural practice: inequitable and poor remuneration, overwork due to understaffing, having no time for holidays, and the overwhelming responsibilities of clinical care, planning and administration in the context of limited resources or prior experience. Among other discouraging factors (Table 3) were a work environment lacking stimulation and characterized by inadequate supplies, equipment and support supervision from the ministry of health or district officials, and low access to continued professional education. Another area mentioned was the limited opportunity for career progression, such as specialization or short-term courses for skills and competence updates, especially for long-term rural health workers. Also mentioned was the lack of transparency in recruitment and deployment (leading to some health workers feeling unfairly bypassed for opportunities), and discrimination in remuneration (with similarly qualified personnel with similar responsibilities being paid different salaries and allowances).
Table 3: Factors that discourage graduates from working in a rural area

Overall, there was no marked difference in responses among graduates of the different curricula. However, in the discussion, community based training was identified as the main factor shaping the values and attitudes of those who were in favor of rural practice, and were confident and willing to work in a rural area. Issues identified included the availability of social amenities and affordable cost of living; ease of communication (no language or cultural barriers); personal safety and security considerations; the opportunity for career advancement; and considerations about workload.
Coping strategies suggested by the doctors included looking for ways to earn extra income to support their families. These might include working in a rural area for a short period where the cost of living was perceived to be cheaper; having more than one job; running a small to medium business; and operating a private clinic. Noted as having influence on personal values were stage of life, characteristics of the rural work site, rural background, and the need to care for family members. These, in turn, impact on recruitment and retention.
The interaction of medical and nursing graduates with the community during the PBL curriculum's community based training appeared to prepare trainees for rural practice by changing their attitude to working in a rural area. Participants identified community, job and regional aspects when describing why they would competently and confidently work in a rural area. These included personal background, security and ease of communication.
Discussion
This study shows that community based training experience can play a significant role in influencing health workers to choose rural practice or to work in underserved areas in Uganda. Training experience in the community may motivate rural practice or increase the competence and confidence of health workers taking up rural employment, possibly by shaping ideals and values related to rural practice. Problem-solving skills acquired and experience in interaction with the community emerged as important.
The methods used in this study enabled participants to transform individual responses into ranked and discussed thematic areas. The study findings are in agreement with existing literature that suggests working conditions (including organizational arrangements, management support, high-risk work environments and the availability of equipment) are a major factor in determining whether health workers remain in remote areas1,19,20. Community based training experience prepares trainees for their future work environment because they have been exposed to the conditions and problems of the workplace.
Career advancement has a strong link with workforce retention. Evidence from a six-country study in Africa (Cameroon, Ghana, Senegal, South Africa, Uganda and Zimbabwe21), based on interviews with between 5% and 20% of skilled public-sector health personnel in each country, showed a strong correlation between career advancement opportunities and retention, a feature more common in Africa than in developed countries. Many health professionals value having access to further training. One of the main reasons for departure to a foreign destination among health workers in Ghana and Cameroon, for example, was the desire for further professional training21.
Sponsoring agencies and government are more likely to support postgraduate training for a university employee than for a health professional working in a non-educational institution21. This makes training institutions more attractive for health professionals who wish to obtain higher qualifications, at the expense of rural locations.
Other elements that attract staff include higher rates of remuneration, more satisfying working conditions and a safe working environment, as well as broader factors such as quality of life, freedom from political persecution, freedom of speech and educational opportunities for children22-26. The presence of social unrest and conflict has a major influence on where health workers seek employment, both within and outside their home countries21.
Also influential are the research projects of global health initiatives, which often offer attractive employment terms and benefits and draw health workers from the public sector. Many staff at central and district health facilities leave public sector postings for such projects, or for positions sponsored by foreign universities or nongovernmental organizations9. In this way, such initiatives can weaken the national health sector, rather than strengthen it, particularly if issues of sustainability have not been sufficiently addressed.
While providing training in rural areas may have a role in improving recruitment to rural areas24-29, other issues that dissuade health workers from rural practice must be addressed. Of the many other factors mentioned by the participants (eg communication issues and lack of social amenities such as schools and recreation facilities) the generally poor socioeconomic conditions for rural health workers is important, because most participants reported they would only work in a rural area if the financial situation of the health workers was improved. The current rural-urban, public-private salary disparities for health workers is a major consideration for graduates in their choice of practice location. Financial incentives from central or local governments would attract health workers to rural areas.
There are other issues that need to be addressed, such as poor rural health infrastructure, the lack of equipment or supplies in rural facilities and the understaffing that leads to ask shifting among available staff. Finally, political interference in the running of rural health units and ineffective leadership and management further discourage health graduates from seeking positions in rural areas.
Conclusion
Interaction with the community during community based training prepared these medical and nursing graduates for rural practice by changing their attitudes to working in a rural area and shaping their personal values. Health sciences programs designed to attract students who are likely to practice and remain in a rural area will succeed only if relevant retention factors are addressed.
Acknowledgements
The authors extend their thanks to all the healthcare professionals who participated in this study and to Cole Dodge and the Makerere University College of Health Sciences staff who were involved in the curriculum evaluation.
References
1. Dieleman M, Cuong PV, Anh LV, Martineau T. Identifying factors for job motivation of rural health workers in North Viet Nam. Human Resources in Health 2003; 1: 10.
2. Hongoro C, McPake B. How to bridge the gap in human resources for health. Lancet 2004; 364: 1451-1456.
3. Daniels ZM, Vanleit BJ, Skipper BJ, Sanders ML, Rhyne RL. Factors in recruiting and retaining health professionals for rural practice. Journal of Rural Health 2007; 23(1): 62-71.
4. Mathauer I, Imhoff I. Health worker motivation in Africa: the role of non-financial incentives and human resource management tools. Human Resources for Health 2006; 4: 24.
5. Fritzen SA Strategic management of the health workforce in developing countries: what have we learned? Human Resources for Health 2007; 5: 4.
6. Kotzee TJ, Couper ID. What interventions do South African doctors think will retain them in rural hospitals of the Limpopo Province of South Africa? Rural and Remote Health 6: 581. (Online) 2006. Available: www.rrh.org.au (Accessed 5 March 2009).
7. Stilwell B, Diallo K, Zurn P, Vujicic M, Adams O, Dal Poz M. Migration of health-care workers from developing countries: strategic approaches to its management. Bulletin of the World Health Organisation 2004; 82(8): 595-600.
8. Anyangwe SC, Mtonga C. Inequities in the global health workforce: the greatest impediment to health in sub-Saharan Africa. International Journal of Environmental Research and Public Health 2007; 4(2): 93-100.
9. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8: 19.
10. Muula AS, Maseko FC. How are health professionals earning their living in Malawi? BMC Health Services Research 2006; 9(6): 97
11. Worley PS, Prideaux DJ, Strasser RP, Silagy CA, Magarey JA. Why we should teach undergraduate medical students in rural communities. Medical Journal of Australia 2000; 172(12): 615-157.
12. Wyss K. An approach to classifying human resource constraints to attaining the Health related Millennium Development Goals. Human Resources and Health 2004; 2(1): 11.
13. White CD, Willet K, Mitchell C, Constantine S. Making a difference: education and training retains and supports rural and remote doctors in Queensland. Rural and Remote Health 7: 700. (Online) 2007. Available: www.rrh.org.au (Accessed 5 March 2009).
14. Martineau T, Decker K, Bundred P. Briefing note on international migration of health professionals: leveling the playing field for developing country health systems. Liverpool: Liverpool School of Tropical Medicine, 2002.
15. Couper ID, Hugo JF, Conradie H, Mfenyana K; Members of the Collaboration for Health Equity through Education and Research (CHEER). Influences on the choice of health professionals to practice in rural areas. South Africa Medical Journal 2007; 97(11): 1082-1086.
16. Tesson G, Curran V, Strasser R, Pong R, Chivot D Adapting medical education to meet the physician recruitment needs of rural and remote regions in Canada, the US and Australia. Cahiers de sociologie et de démographie médica 2005; 45(2-3): 229-253.
17. van Diepen K, MacRae M, Paterson M. Use of clinical placements as a means of recruiting health care professionals to underserviced areas in Southeastern Ontario: part 2 - community perspectives. Australian Journal of Rural Health 2007; 15(1): 29-34.
18. Dunbabin JS, McEwin K, Cameron I. Postgraduate medical placements in rural areas: their impact on the rural medical workforce. Rural and Remote Health 6: 481. (Online) 2006. Available: www.rrh.org.au (Accessed 5 March 2009).
19. Dieleman M, Toonen J, Toure H, Martineau T. The match between motivation and performance management of health sector workers in Mali. Human Resources in Health 2006; 4: 2.
20. Zurn P, Dal Poz MR, Stilwell B, Adams O. Imbalance in the health workforce. Human Resources in Health 2004; 2: 13.
21. Awases, A.Gbary, A.Nyoni, J. Chatora, R. Migration of health professionals in six countries: a synthesis report. Brazzaville, WHO; 2004.
22. Orpin P, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural and Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 5 March 2009).
23. Richards HM, Farmer J, Selvaraj S. Sustaining the rural primary healthcare workforce: survey of healthcare professionals in the Scottish Highlands. Rural and Remote Health 5: 365. (Online) 2005. Available: www.rrh.org.au (Accessed 5 March 2009).
24. Liaw ST, McGrath B, Jones G, Russell U, Bourke L, Hsu-Hage B. A compulsory experiential and inter-professional rural health subject for undergraduate students. Rural and Remote Health 5: 460. (Online) 2005. Available: www.rrh.org.au (Accessed 5 March 2009).
25. Magnus J, Tollan A. Rural doctor recruitment: does medical education in rural districts recruit doctors to rural areas? Journal of Medical Education 1993; 27: 250-253.
26. Chaytors RG, Spooner GR. Training for rural family medicine: a cooperative venture of government, university and community in Alberta. Academic Medicine 1998; 73: 739-742.
27. Easterbrook M, Godwin MA, Wison R. Rural background and clinical rotations during medical training: effect on practice location. Canada Medical Association Journal 1999; 160: 1159-1163.
28. Sen Gupta TK, Muray RB, McDonell A, Murphy B, Underhill AD. Rural internships for final year students: clinical experience, education and workforce. Rural and Remote Health 8: 827. (Online) 2008. Available: www.rrh.org.au (Accessed 5 March 2009).
29. Rosenblatt RA, Whitcomb ME, Cullen TJ, Lishner DM, Hart LG. Which students become rural physicians? JAMA 1992; 268: 1559-1565.


