Access to quality health care is a significant challenge in many parts of sub-Saharan Africa where the density of trained healthcare providers is the lowest in the world1. Despite trends towards urbanization, much of Sub-Saharan Africa is heavily rural with limited access to hospitals and clinics in urban centres2. Many studies document barriers to care for people living in rural settings worldwide, including the poor availability of trained staff, barriers to information, basic equipment and materials for care, and physical distance to care3-6 . A number of studies have evaluated strategies for improving healthcare access in rural Sub-Saharan Africa, including the use of community health workers and participation in health insurance7-9 . However, few have looked at employers' willingness to pay for health insurance as a strategy to improving healthcare access.
Namibia, in particular, has the second lowest population density in the world, with many of its people living in rural settings and working in the agricultural sector10. There are 13 political regions in Namibia and commercial farming takes place in 8 of these, with the remaining regions having communal land11. Providing access to health care for the largely dispersed population presents a serious challenge. While Namibia is significantly improving its healthcare financing and delivery system due to exceptionally high government expenditure on health (7.6% of GDP12), and an extensive coverage of people on anti-retroviral therapy (ART) for HIV/AIDS13, there is a lack of trained health professionals serving in the public sector. In 2008, 72% of doctors (n=774) and 46% of registered nurses (n=2,989) in Namibia were in private practice, serving less than 20% of the population14. On average, the private sector employs 8.8 health workers per 1000 people, compared with 2 health workers per 1000 people in the public sector14.
A potential partner in the provision of better health services is the commercial agricultural sector, the largest private employer in Namibia. As a significant contributor to the economic development of Namibia, this sector has already been engaged in addressing the HIV/AIDS epidemic, which still represents a significant health burden in the country11,15-17 . For example, in 2005 the Agricultural Employers' Association (AEA), a membership-based organization representing employers in the commercial agricultural sector, and the Namibia Farm Workers Union (NAFWU) signed an HIV/AIDS policy in 2005 to manage and mitigate the impact on the commercial agricultural sector11. However, there is no current system in place to provide basic primary care to those employed in agriculture in Namibia14.
Besides an increase in health professionals working in the public sector, another potential opportunity for improving access to care for those in rural settings is the introduction of health insurance and cost-sharing approaches7. Health insurance can be an important mechanism to avoid catastrophic individual and household healthcare expenditure18. While a number of innovated insurance schemes targeted at Namibians who could not afford private health insurance have been developed, at the last report only 12.5% of the population was covered by health insurance, and this represented people with middle to high incomes19-22 . Given the small number of Namibians covered by health insurance, engaging employers could provide a way to expand that coverage and reduce high healthcare costs to individuals. Understanding the patterns of utilization among those employed in the agriculture sector, barriers of access to care, and the willingness of employers to pay for insurance schemes could help improve access to basic care for many Namibians.
In 2007, at the request of the AEA, the PharmAccess Foundation in Namibia conducted a survey of AEA member commercial farm employers to describe utilization of health services by employers and employees and associated costs; describe employer knowledge, attitudes, and practices regarding the provision of health services and support to employees; assess the status of accessible medical service delivery; and assess employer willingness to pay for health insurance schemes, including cost-sharing and reducing out-of-pocket expenditures. The survey was designed to inform the implementation plan of the AEA workplace policy. Although AEA members comprise only one-third of the estimated number of commercial farms, their farms are geographically representative of the greater farming sector in Namibia.
Survey design and target population
In 2007, the PharmAccess Foundation in Namibia conducted a cross-sectional survey of members of the AEA to assess utilization and provision of health services on farms (in particular HIV/AIDS services) and possibilities for the development of employer-provided insurance schemes. The survey was piloted with 10 AEA-member commercial farming employers and, following this, the questions were amended to better assess the primary goals of the survey. In addition, a list of frequently asked questions was compiled. Once finalized, the survey was carried out using a structured questionnaire with telephone interviews. Any AEA-member commercial farm was eligible for inclusion and all were contacted regarding participation. Of the 1708 members invited to participate, 1402 employers (82.1%) agreed to the telephone survey and were included in this study. The employers represented 1414 farms throughout 8 regions of Namibia.
The survey gathered data on:
- general characteristics of the farm and number of employees and dependants
- use of medical facilities and health expenditure by all people working or living on farms
- local available medical expertise and services on site
- availability of first aid and provision of medicines on farms
- general knowledge of HIV/AIDS as specified in AEA policy, including prevention
- willingness to pay for health insurance.
Personal identifiable information was not collected in order to respect the privacy of respondents and eliminate any risk of breach of confidentiality. The telephone interviews were conducted by 20 peer enumerators selected from AEA members in each region and lasted approximately 30 min each. Prior to the survey, enumerators received a one-day training covering the content of the questionnaire, interviewing skills, and responses to frequently asked questions. Employers were asked to provide information about their farms regarding employee and employee-dependants' healthcare-seeking behaviour. After the survey, the peer enumerator answered questions for respondents from among the frequently asked questions collected from the pilot of the survey, or relayed questions which the enumerator could not answer to the AEA leadership for follow up.
Statistical analyses
Data collected were entered into a database using MS Access 2007. Statistical analysis was performed using R v2.10.0 (http://cran.r-project.org/bin/windows/base/) statistical software. Bivariate analyses of categorical variables were assessed using Pearson's X2, continuous variables were assessed using Welch's t-test, and an alpha of 0.05 was considered statistically significant.
General characteristics
Of the 1708 members invited, 1402 employers (82.1%) representing 1414 farms agreed to participate in the telephone survey; the farms were located throughout 8 geographical regions of Namibia (Fig1). Surveys were administered on a 'per-farm' basis, so that employers who managed more than one farm responded more than once to the survey. Therefore, in the results when referring to employers it is implied that they are representing a unique farm. In total, 87.1% of employers (95%CI: 85.4, 88.9) resided permanently on a commercial farm. They reported a total of 8721 permanent employees, 5728 temporary employees, and 14 754 employee dependants on all farms over the 12 months leading up to the survey date. The mean number of employees per farm was 10.2 (range 0-342; 95% CI: 9.5, 10.9).
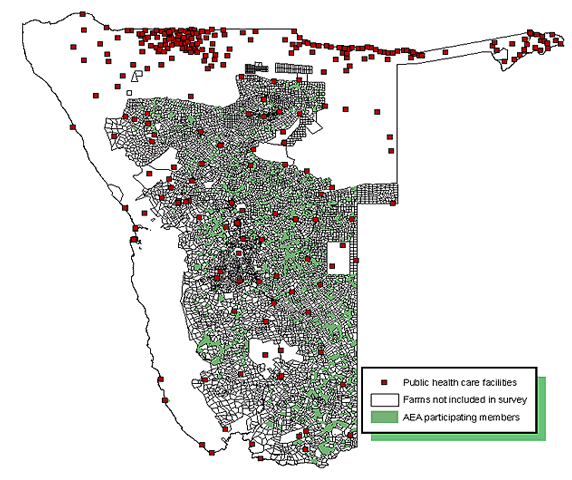
Figure 1: Location of employers in relation to other commercial farms and public health facilities in Namibia.
Utilization, access and expenditures
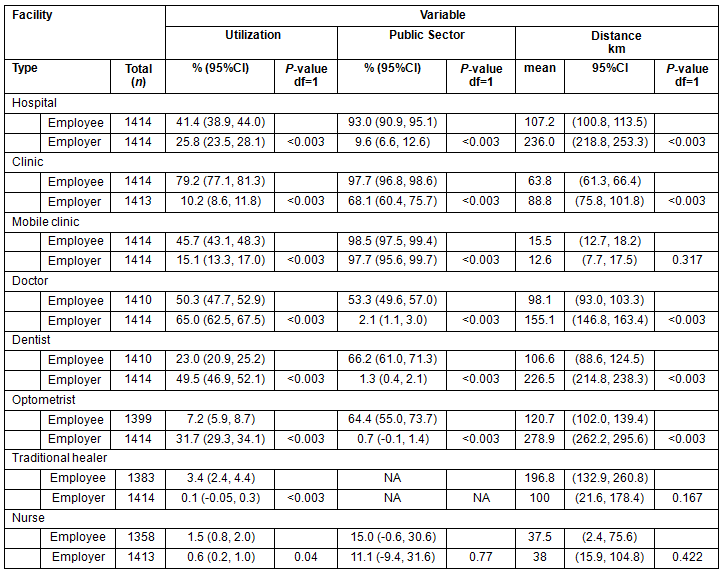
Employers (n=1414) were asked to report on the healthcare-seeking behaviour of themselves and their employees in the 12 months prior to the survey (Table 1). A great majority of employers (94.7%; 95%CI: 93.6, 95.9) reported that employees had visited at least one medical facility and most frequently used clinics (79.2%, 95%CI: 77.1, 81.3), followed by doctors (50.1%; 95%CI: 47.5, 52.7) and mobile clinics (45.7%; 95%CI: 43.1, 48.3). The vast majority of health utilization by employees was from public sources. From all types of health facilities, employees used health services significantly more than employers and used significantly more public facilities than private (Table 1).
The great majority of farm employers (90.7%; 95%CI: 89.2, 92.2) reported they had visited at least one medical facility over the previous 12 months. However, employers mostly visited doctors (65.0%; 95%CI: 62.5, 67.5), dentists (49.5%; 95%CI: 46.9, 52.1) and optometrists (31.7%; 95%CI: 29.3, 34.1), and used primarily private facilities. Except for the use of mobile clinics, traditional healers, and nurses, employers reported travelling significantly longer distances to access health facilities than their employees (Table 1). The location of all commercial farms in Namibia and AEA members who participated in the survey in relation to health facilities is shown (Fig1). In general, health facilities are located at considerable distances from the widely dispersed farms.
Table 1: Employer-reported utilization of and access to health facilities on farms
Costs of care
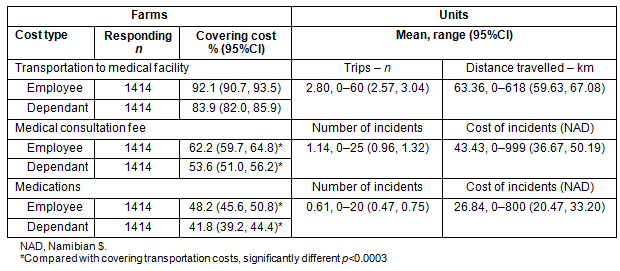
The health-related costs assessed in this survey included the costs of a consultation, medications and transportation to and from the health facility. Employers were significantly more likely to pay for employees' transportation costs (mean=2.8; 95%CI: 2.57, 3.04; χ2=303.5, df=1, p<0.0003) than the costs associated with medical consultations (mean=1.1; 95%CI: 0.96, 1.32; p<0.0003) or medications (mean=0.61; 95%CI: 0.47, 0.75; χ2=538.1, df=1, p<0.0003) (Table 2). The situation was similar for employee dependants. Although the average costs of transportation were not collected, the average cost of a medical consultation (NA$43.43; 95%CI: 36.67, 50.19) was almost double that of medications (NA$26.84; 95%CI: 20.47, 33.20). The average one-way distance travelled to a consultation was 63.36 km (95%CI: 59.63, 67.08), which could result in several hours of employees' work lost.
Table 2: Employer-reported coverage of costs for utilization by employees and their dependants
Provision of health care and medications
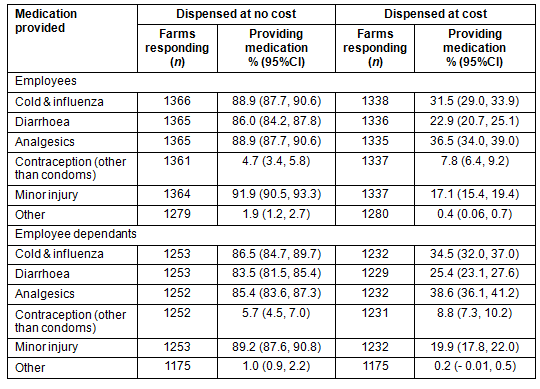
Because of the long travel distances often needed to reach basic care, a great majority of farms reported providing care for minor illnesses for employees (95.9%; 95%CI: 94.9, 97.0) and their dependants (87.9%; 95%CI: 86.2, 89.6) on site. The details of how this care was provided were not captured by this survey; however, employers were asked whether any person living on the farm had some form of professional medical training. The study found that more than 10% of farms (10.47%; 95%CI: 8.9, 12.2) had at least one person in residence who had received professional medical training (Table 3); however, this does not include the most common form of training: basic first aid certification (16.8%; 95%CI: 14.8, 18.7). The details of why these professionals were on site or of their primary role was not collected in this survey. However, their presence represents an opportunity for farm worker to avoid the costs of and travel time for health care otherwise necessary. In addition, employers reported providing different types of basic medications to employees and their dependants on site (Table 4). The most provided medication was for minor injuries, but medications for colds and influenza, diarrhoea, and analgesics were also commonly available on farms at no cost to employees. Some employers reported selling medications to employees but free medications were most common.
Table 3: Employer-reported on-site presence of trained health professional
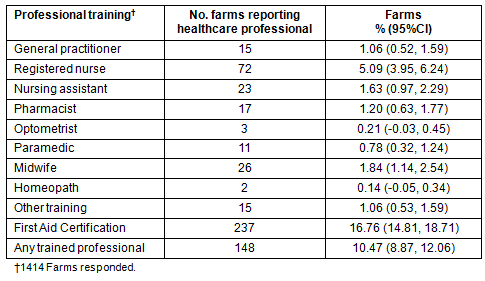
Table 4: Employer-reported provision of medications and care on-site in farms
HIV/AIDS
As requested by the AEA, questions regarding an employer's knowledge, attitudes and practices for HIV/AIDS were also collected. Employers on 44 farms (3.1%; 95%CI: 2.2, 4.0) reported they knew of employees receiving ART for HIV/AIDS. Employers on only 8 farms (18.1%; 95%CI: 6.7, 29.4) covered the costs associated with the publicly funded ART program for employees with HIV/AIDS; on 19 farms (43.1%; 95%CI: 29.3, 58.7) the employees paid for these costs themselves. The publicly funded ART program costs NA$8 per consultation; medications are covered by the state. Access to HIV prevention measures on farms was also limited. Employers on 203 farms (14.3%; 95%CI: 12.2, 15.8) reported that they were aware of 1130 employees or their dependants who had gone for HIV testing in the 12 months prior to the survey. However, this may not reflect the actual number of employees or their dependants being tested, especially regarding the associated sensitivity and stigma. In addition, the following HIV-related services were being provided to employees on some farms: condoms (14.6%; 95%CI: 12.7, 16.4), HIV-specific education (11.3%; 95%CI: 9.7, 13.0), training on condom use (13.1%; 95%CI: 11.25, 14.75), and peer education (1.8%; 95%CI: 1.1, 2.5).
While relatively few services were provided to employees on farms, knowledge regarding HIV by employers was comparatively strong. Employers on 89.8% farms (95%CI: 88.2, 91.4) were able to correctly identify two possible routes of HIV infection, and reject at least three common misconceptions about HIV transmission. The most widespread misconception was that HIV can be transmitted by mosquito bites (12.8%; 95%CI: 11.1, 14.5). Also, 20% of employers (95%CI: 17.9, 22.1) did not know that mother-to-child HIV transmission can be prevented.
Insurance availability and prospects for future investment
The survey assessed the health insurance coverage reported by employers for themselves, employees, and their dependants. Just over half the employers reported their farms provided health insurance, covering both in- and outpatient services, for themselves (57.5%; 95%CI: 54.9, 60.1) and their own dependants (53.7%; 95%CI: 51.1, 56.3). Conversely, almost no employers reported health insurance coverage on farms for employees (0.85%; 95%CI: 0.37, 1.33) and their dependants (0.50%; 95%CI: 0.13, 0.86). Farms provided significantly more insurance to employers and their dependants than for employees and employee dependants (χ2=1098, df=1, p<0.0003).
Employers were asked about their willingness to pay for private health insurance for employees that would cover only out-patient care through a mobile clinic. The hypothetical monthly cost of this scheme was calculated to be a NA$100 premium (approximately US$14.30) per person. This premium is significantly cheaper than any existing health insurance product on the Namibian market because it does not include in-patient care. While few employers were willing to pay the full monthly premium for their employees (16.0%; 95%CI: 14.1, 17.9) or employee dependants (3.7%; 95%CI: 2.7, 4.7), among those who would not pay the full premium, willingness to share the cost (co-payment) was much higher (employees: 77.1%; 95%CI: 74.6, 79.4; employee dependants: 38.7%; 95%CI: 36.1, 41.3). Employers were willing to co-pay on average NA$44 (approximately US$6.30) per employee and NA$39 (approximately US$5.60) per dependant per month. Employers also indicated they were prepared to co-pay for an average of 2.8 dependants per employee. Employers on farms that provided free medicines to employees and their dependants, and those who reported paying for transportation to medical care were significantly more likely to be willing to co-pay insurance (χ2=5.70, df=1, p=0.01; χ2=8.84, df=1, p=0.002, respectively).
Discussion
Access to health care in rural settings is notoriously limited in Sub-Saharan Africa, where populations are often highly dispersed5. The low population density means that many rural Namibians suffer from this lack of access to care. Commercial farms are one of the largest employers in Namibia representing 65 000 employees and employee dependants who often live permanently on the farms. Partnerships with the agricultural sector organisations, such as the AEA, provide an opportunity to improve access to care for a large number of people.
Currently, the provision of health care, including health insurance, for people living on AEA farms is at the discretion of the employer and not a standard policy. From the survey results, employees are making use of a variety of health services, mostly in the less expensive public sector, and travelling long distances to do so, bearing most of the cost themselves. Employers, by contrast, are consistently using more private services and travelling even longer distances. It is possible that employers use private services due to a perceived increase in quality of more expensive care. More employers benefit from health insurance coverage than employees. The cost of full private health insurance is prohibitive for the average farm worker who often must also provide for his or her family who also live on the farm. While this study found a very small number of employers who provide health insurance for employees, there is a strong willingness to share insurance costs with employees, which offers an opportunity to improve access to care.
Another opportunity identified in this study was that some farm employers supported costs for employees and their dependants, providing free basic medications and often covering the cost of travel or health consultations. These employers were more likely to be willing to co-pay for health insurance for employees than employers who did not provide this type of support. It may be that these employers saw value in investing in the health of their employees to avoid costs related to absenteeism. Some farms also housed a number of trained health professionals, presumably to provide care for farm residents. Although the employment status of these health professionals was not clear from the study, their presence represents a resource that could be engaged and strengthened to provide basic care on remote farms.
In Sub-Saharan Africa there is an increasing lack of healthcare workers16, a persistent burden of HIV/AIDS and an emerging epidemic of chronic disease23. Task shifting, or delegating tasks from more- to less-specialized health workers, has been proposed as a potential solution to this problem24,25. The resident, trained health professionals identified in this study could potentially be motivated or re-trained to provide healthcare to employees on a cache of nearby farms. Building the capacity of these professionals to provide care by giving training on relevant public health topics and providing basic diagnostic and treatment tools would greatly improve access to health care in these remote regions, as has been shown in previous studies24.
Given the cost of current private Namibian health insurance packages, novel approaches must be taken to make cost-sharing by employers an affordable and attractive option. Engaging in public-private partnerships, as in other developing countries, could also be utilized in Namibia26. With the adoption of health insurance, the use of the private health sector could increase and significantly alleviate the burden on the public health sector19,27. Health insurance could also lead to gains from a healthier workforce with greater productivity, a reduced need for worker replacement, and direct financial gains for the commercial farming sector28-30 . Currently uninsured employers and their families (43% of the participants in this survey) could also benefit from such an insurance scheme.
Other novel approaches to improving access to care, such as the strengthening of mobile clinics and the introduction of remote-care communications such as telehealth have been shown to work in other rural settings and could be applied in Namibia31-33 . A recent meta-analysis found that home-based telehealth has a positive effect on clinical outcomes33. While telemedicine has not yet been implemented in Namibia, the geography of the country suggests a potentially important role for this technology32. In addition, affordable fingerprint technology, which has been used in other developing countries with success, could be used for identification and medical monitoring33.
This study also identified a significant gap in the provision of basic services for HIV/AIDS prevention, education and management. Very few farms supported ART for their employees and there was no evidence of an established structure for voluntary counselling and testing for HIV. The burden of HIV/AIDS is significant in Namibia13 and all sectors, especially where employees live with their families in the workplace, must be engaged to curb the epidemic. Although the study showed that employers had good knowledge of the transmission of HIV/AIDS, some misconceptions were identified and systematic support or education was not being provided for those living and working on their farms. The introduction of health insurance for employees could lower the threshold for seeking HIV-testing; however, this would need to be supported by the employers or the insurance scheme.
Limitations and biases
All information collected was from employers only who were asked to respond on behalf of employees and employee dependants. This is the greatest limitation to the findings as it presents a risk for information bias, recall bias, and reporting bias. Ideally, employees and their dependants would have been questioned directly in order to limit this bias. However, that was outside the scope of this study. Questions were designed to limit speculation by employers on employee behaviour and instead provide evidence or counts of events. To avoid recall bias, employers were asked to report on only the 12 months prior to the administration of the survey.
In addition, there was a risk of reporting bias if employers gave inaccurate information, either regarding the provision of health services or the health status of their employees, leading to a possible inflation of the numbers. Because the AEA has no specific policy requiring employers to provide health services to employees - and thus there are no repercussions for not providing services - this risk was considered to be low.
While conducting interviews by telephone was deemed to be the most feasible way of reaching the largest number of participants, this may have had an impact on willingness to participate, leading to a selection bias. Ideally, a random sample of employers would have been used to avoid a systematic selection of any particular kind of respondent. In addition, having AEA-member moderators conduct the survey may have had an impact on employer responses. Again, this approach was taken because it was the most feasible and could provide the largest number of responses. It was also potentially beneficial to have employers speaking with colleagues rather than with an 'outsider'.
The study results underscore the limited access to health care for people living in rural communities in Sub-Saharan Africa, particularly in lower income groups. However, as this study demonstrates, the commercial farming sector in Namibia is a potential partner for improving access through cost-sharing insurance schemes and leveraging the existing health services on many farms. The introduction of affordable private health insurance, including HIV/AIDS coverage, for commercial farm workers is feasible. This study did not assess the costs associated with health insurance; however, such information would be valuable in strengthening the case for greater coverage, and future studies would be useful to identify the most cost-effective solution. Innovative interventions such as mobile clinics, telehealth and the involvement of medical professionals in task shifting to competent lay people residing on farms would also increase access and greatly benefit resident workers.
Acknowledgements
The authors acknowledge the help and support of the members of the AEA and commercial farmers in Namibia without which this work would not have been possible. In addition, they thank visiting scientist Huub Gelderblom for his valued assistance and input, by contributing to the concepts and critically reading the manuscript.
References
1. Dal Poz MR, Kinfu Y, Drager S, Kunjumen T. Counting health workers: definitions, data, methods and global results. Geneva. WHO: Department of Human Resources for Health Evidence and Information for Policy, 2006.
2. United Nations. World Population Prospects: the 2008 Revision. Geneva: United Nations Population Division, 2008.
3. Mueller KJ, Ortega ST, Parker K, Patil K, Askenazi A. health status and access to care among rural minorities. Journal of Health Care of the Poor and Underserved; 10(2): 230-249.
4. Raso G, Utzinger J, Silué KD, Ouattara M, Yapi A et al. Disparities in parasitic infections, perceived ill health and access to health care among poorer and less poor schoolchildren of rural Côte d'Ivoire. Tropical Medicine and International Health 2005; 10(1): 42-57.
5. Tanser F, Gijsbertsen B, Kobus H. Modelling and understanding primary health care accessibility and utilization in rural South Africa: An exploration using a geographical information system. Social Science and Medicine 2006; 63(3): 691-705.
6. Martínez A, Villarroel V, Seoane J, del Pozo F. Analysis of information and communication needs in rural primary health care in developing countries. IEEE Trans Inf Technol Biomed 2005; 9(1): 66-72.
7. Jutting JP. Do Community-based health insurance schemes improve poor people's access to health care? Evidence from rural Senegal? World Development 2004; 32(2): 273-288.
8. Wilkinson D, Gouws E, Sach M, Karim SS. Effect of removing user fees on attendance for curative and preventive primary health care services in rural South Africa. Bulletin of the World Health Organisation 2001; 79(7): 665-71.
9. Asenso-Okyere WK, Osei-Akoto I, Anum A, Appiah EN. Willingness to pay for health insurance in a developing economy. A pilot study of the informal sector of Ghana using contingent valuation. Health Policy 1997; 42(3): 223-237.
10. United Nations Population Division. Population Database. (Online) 2008. Available: http://esa.un.org/ (Accessed 5 May 2010).
11. The Agricultural Employer's Association. Policy on managing HIV/AIDS within the commercial agricultural sector. Windhoek, Namibia: The Agricultural Employer's Association, 2006.
12. The World Bank. Health expenditure, total (% of GDP). (Online) 2007. Available: http://data.worldbank.org/indicator/SH.XPD.TOTL.ZS (Accessed 23 May 2010).
13. WHO. HIV/AIDS: Dispatch from Namibia. (Online) 2009. Available: http://www.who.int/hiv/mediacentre/namibia/en/index.html (Accessed 23 May 2010).
14. Namibia Ministry of Health and Social Services. Health and Social Services System Review. Windhoek, Namibia: Namibia Ministry of Health and Social Services, 2008.
15. UNAIDS and WHO. Sub-Saharan Africa: AIDS epidemic update regional summary. Geneva: WHO, 2007.
16. Cohen J. The great funding surge. HIV/AIDS 2008; 321(5888): 512-519.
17. WHO/UNAIDS/UNICEF. Towards Universal Access: scaling up priority HIV/AIDS interventions in the health sector. Geneva: WH0, 2008.
18. Ranson MK. Reduction of catastrophic health care expenditures by community-based health insurance scheme in Gujarat, India. Bulletin of the World Health Organisation 2002; 80(8): 613-621.
19. Sekhri N, Sayedoff W. Private health insurance: implications for developing countries. Bulletin of the World Health Organisation 2005; 83(2): 127-134.
20. Feeley F, de Beer I, Rinke de Wit T, vander Gaag J. The health insurance industry in Namibia: Baseline Report. Namibia: Windhoek, 2006.
21. Hohman S. Options and scenarios for HIV/AIDS risk cover for low income employees within NABCOA member companies in Namibia. Namibia, Windhoek: 2004.
22. Schellekens O, de Beer I, Lindner ME, van Vugt M, Schellekens P, Rinke de Wit T. Innovation in Namibia: preserving private health insurance and HIV/AIDS treatment. Health Affairs 2010; 28(6): 1799-1806.
23. Abegunde D, Mathers C, Adam T, Ortegon M, Strong K. The burden and costs of chronic diseases in low-income and middle-income countries. Lancet 2004; 370(9603): 1929-1938.
24. Morris M, Chapula B, Chi B, Mwango A, Chi H, Mwanza J et al. Use of task-shifting to rapidly scale-up HIV treatment services: experiences from Lusaka, Zambia. BMC Health Services Research 2007; 9(5): no pp.
25. Samb B, Celletti F, Holloway J, Van Damme W, De Cock K, Dybul M. Rapid expansion of the health workforce in response to the HIV epidemic. New England Journal of Medicine 2007; 357(24): 2510-2514.
26. Widdus R. Public-private partnerships for health: their main targets, their diversity, and their future directions. Bulletin of the World Health Organisation 2001; 79(8): 713-720.
27. Feeley F, Connelly P, Rosen S. Private sector provision and financing of AIDS treatment in Africa: current developments. Current HIV/AIDS reports 2007; 4(4): 192-200.
28. Piot P, Greener R, Russell S. Squaring the circle: AIDS, poverty, and human development. PLos Medicine 2007; 4(10): 1571-1575.
29. Larson B, Fox M, Rosen S, Bii M, Sigei C, Shaffer D et al. Early effects of antiretroviral therapy on work performance: preliminary results from a cohort study of Kenyan agricultural workers. AIDS 2008; 22(3): 421-425.
30. Fox M, Rosen S, MacLeod W, Bii M, Foglia G, Simon J. The impact of HIV/AIDS on labour productivity in Kenya. Tropical Medicine and International Health 2004; 9(3): 318-324.
31. Bagayoko C, Muller H, Geissbuhler A. Assessment of Internet-based telemedicine in Africa (the RAFT project). Computed and Medical Imaging Graphics 2006; 30(6-7): 407-416.
32. Wootton R. Telemedicine support for the developing world. Journal of Telemedicine and Telecare 2008; 14(3): 109-114.
33. Ozuah P, Reznik M. The role of telemedicine in the care of children in under-served communities. Journal of Telemedicine and Telecare 2004; 10(Suppl 1): 78-80.





