Introduction
Chronic kidney disease (CKD), a condition frequently attributed to uncontrolled diabetes and hypertension, has become an economic and public health burden both globally and locally1-3. The prevalence of CKD, particularly the early stages, has grown 40% over the past decade, with the disease now affecting 13.8-15.8% of the general population3. Untreated or poorly managed CKD can lead to numerous health problems, particularly cardiovascular disease and kidney failure, also known as end-stage kidney disease (ESKD), requiring treatment with dialysis or a kidney transplant for survival. African-Americans are four times more likely to progress to ESKD than are their Caucasian counterparts and are more likely to develop kidney failure due to uncontrolled high blood pressure3.
Kidney disease is the tenth most common cause of death in North Carolina. National CKD incidence and prevalence rates have increased steadily between 1994 and 2005 and have been higher in North Carolina when compared with the national average. It has been estimated that over 26 million Americans and 900 000 North Carolinians are currently living with early CKD4.
Early identification of and treatment for CKD can be crucial to maintaining a person's quality of life and keeping health costs low. Late referrals have been shown to be associated with increased mortality and decreased access to renal transplantation, even among those who survive their first year on dialysis5-9. Early identification of and intervention for CKD can also lead to better management of diabetes and hypertension, the two main risk factors for CKD10. However, public awareness of CKD and its associated risk factors is low, in both the general population and in populations already diagnosed with the disease11-14.
Focus groups provide a mechanism to gather information from individuals in high risk communities with regard to CKD awareness, as well as general issues relating to access and barriers to health care. An understanding of these issues in a community is needed in order to design effective awareness and education programs. Individuals at high risk for kidney disease include African Americans and the elderly, particularly those in low income communities with limited education. Therefore, understanding these issues in the context of the social structure of each community is critical.
In 2005, the University of North Carolina (UNC) Kidney Center implemented the Kidney Education Outreach Program (KEOP), a comprehensive, community and evidence based initiative to raise at-risk North Carolinians' awareness about the primary risk factors for kidney disease and the importance of early diagnosis and intervention as strategies to stop CKD or slow its progression to ESKD. Using 3 principles derived from a compilation of work on the science of how people learn, the KEOP is designed to promote learning with understanding15.
The 3 principles and the associated KEOP program components are: (i) assess preconceptions with community-based focus groups to assess at-risk citizens' ideas about CKD and access to health care; (ii) deliver new information in formats that promote active learning by providing interactive information sessions that are augmented with a media campaign that uses local citizens as spokespersons; and (iii) provide opportunities for meta-cognition with free CKD screenings that include one-on-one conversations about findings and written summaries of test results with recommendations for subsequent action.
This article explores themes from conversations about kidney disease, health screenings, and barriers to care from 17 focus groups conducted across 5 rural, North Carolina counties with high rates of ESKD, through the UNC Kidney Center's KEOP.
Methods
Study sample
Seventeen focus groups with a total of 201 citizens were conducted in 5 North Carolina counties between March 2005 and October 2007. A summary of the counties and type, size and racial makeup of the focus groups is shown (Table 1). Twelve focus groups were conducted with citizen or church groups, three with allied health professional students attending local community colleges, one with health care/social service professionals, and one with family members of dialysis patients. The focus groups were organized by the UNC KEOP and lay partners in each county.
Table 1: Description of the 17 focus groups by county
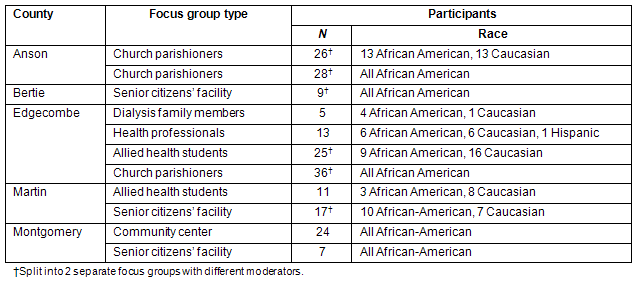
Purposive sampling was used to recruit community members who were at greater risk for developing kidney disease (African American, elderly) or who may have an impact on the health and wellbeing of their communities (allied health students, health professionals, community leaders). Five focus groups took place at senior citizens' centers to increase the recruitment of older participants and 6 groups were conducted at African-American churches to ensure a high level of recruitment for that population.
Recruitment was through collaboration with community liaisons. These community liaisons helped recruit participants through public announcements, phone calls, posters, and word-of-mouth. Participants received a $20 gift card for their participation. Approval by the UNC Institutional Review Board was obtained prior to implementation of the study.
Design
A scripted discussion guide was pilot tested with a group of colleagues and with church parishioners in a non-priority county. Each focus group session lasted between 45-60 min, was audiotaped and transcribed verbatim and co-moderated by two members of the research team. Topics for discussion were divided into 5 areas: (i) knowledge about kidneys, risk factors for CKD, and kidney failure: (ii) thoughts on kidney disease/kidney problems; (iii) barriers to health care; (iv) prior experience with the healthcare system and providers; and (v) preferences for health screening locations and modalities for CKD education.
Analysis
Individual recordings were transcribed and uploaded into ATLAS.ti software (ATLAS.ti Scientific Software; Berlin, Germany) for coding, organization and qualitative data interpretation. This research utilized a grounded theory approach to analyze focus group data, a qualitative method that allows the data to 'speak for itself'. In this way common topics emerge naturally from the data, rather than relying on testing a priori hypotheses16. Grounded theory uses open coding (free form coding for words, themes, expressions) followed by axial coding, which seeks to explore categories created through the open coding process. A 'base coder list' was devised after reviewing open coding on 2 transcripts by 3 different investigators to increase inter-rater reliability. Additional codes were added to the base list as the analysis of additional focus groups continued. Once coded, transcripts were categorized into sections based on the 5 core questions (stated above).
Sub-themes emerged in each section based on ongoing review and axial coding. Codes present in 5 or more groups per section were investigated by pulling those codes from the overall transcript and looking at codes that co-occurred within each theme section and compared codes across different types of focus groups, although there were not significant differences noted. The authors were satisfied that they had reached saturation and did not feel the need to conduct further focus groups.
Quotes that are representative of themes are provided in the results, with editing to increase readability and assure confidentiality.
Results
Of the 201 participants, 74% were African-American, 96.5% knew someone with diabetes or hypertension, and 76% of groups contained at least one participant with a family member or friend diagnosed with end-stage kidney disease (ESKD). General focus group racial demographics are provided (Table 1). Age and other socio-demographic information were not recorded. Main themes extracted from focus group responses are summarized (Fig1).

Figure 1: Summation of focus group themes.
Understanding what kidneys do and the importance of maintaining kidney function
When asked what they knew about kidneys, participants in several groups stated that there were issues with the back such as backaches. Participants in 8 focus groups understood that the kidneys acted as filters, and participants in 12 groups mentioned water or fluid: holding water as a risk factor for kidney disease or using water as a protective factor against kidney damage. Statements included:
You can't get your water out and it makes you real sick.
I think of frequent bathroom [visits].
A urination problem, it may not be normal, might be frequent.
Participants frequently noted that the kidneys clean the blood, kidney disease can be caused by 'thin blood', and blood filtering is needed by the kidney. One participant stated:
If you drink too much or and if you eat too much of certain foods, something about the blood itself, some people have thin blood and that will cause your kidney problems.
Lifestyle choices were routinely brought up by groups as a means to explain the occurrence of kidney disease, especially alcohol. Alcohol was noted by one person as a way to 'flush the kidneys out':
I've had an elderly person say, well, oh, just let him drink a little beer. If flushes his kidneys out.
Obesity, drinking sodas, and diet were also mentioned as factors attributed to kidney disease:
I think that some of the people that I have come in contact with, their eating habits are very, you know, you eat a lot of pork, different things, just eating anything that come along...and then the blood pressure.
Thoughts on kidney disease/kidney problems
In every group, dialysis was mentioned as something participants thought about when they heard the term kidney disease, and this was mainly due to family or friends' experiences with dialysis. Most participants who had experienced dialysis through others felt it was a bad, life-altering treatment that placed stress on patients and their family members. Public awareness of how difficult dialysis is was important to them. Statements included:
My mother is on dialysis...and it really is a draining process. Her whole complexion has changed.
Just from watching my uncle and other people go through dialysis, it just looks like something that could really take a toll on your body.
My father knew his [kidney] function was getting progressively worse but it went from 'your kidneys are slowly getting worse to, hey, we're starting you on dialysis.' He [went on dialysis and then] died.
Focus group participants consistently mentioned that it was important to know the risk factors for kidney disease, the symptoms of kidney disease, and how to prevent kidney disease by working on modifiable risk factors and exercising preventive health behaviors. Statements included:
People [need to be] aware of what the symptoms are. If you're breaking out in a sweat or you're really, really thirsty, that should key you in that something is not right with your body. We need to learn to listen to our bodies.
We have a lot of [kidney disease] here so everyone needs to know what causes it and how it can be stopped.
Barriers to health care
Affordability of insurance, medications and general medical care was ubiquitous in the focus group discussions on barriers to health care. While some mentioned that lack of insurance was a problem, many stated that even with insurance it was challenging to meet health plan deductibles and co-payments. Issues of affordability and access to health care primarily stem from the fragmented and costly US healthcare system, a mix of private insurance, subsidized care, and entitlement programs. One participant, when speaking of her daughter, explained:
She's 23 years old and whatever she looks into as a health plan, it would cost like $300 or $400 or more a month. It's not that they don't want it. A lot of them can't afford it. She's trying now to get a job that will give her some health benefits, but what's she going to do in the meantime about her blood pressure?
Another participant stated:
Sometimes I have to cut back a little bit until my check comes because my medicines are so expensive.
Another systematic barrier mentioned frequently in groups was lack of transportation, especially for the elderly population and in rural areas. Transportation out of town for specialty medical care was also seen as a problem. One participant stated:
My cousin living in [a small rural town], she has a severe case of diabetes and they want her to see a specialist on a regular basis but she doesn't have a car and that's a good distance to have to try to get somebody to take you, you know, every other week. She gets care, but it's not the best care that she needs for her condition.
Fear was mentioned in 11 groups as a psychosocial barrier to receiving health care. Specific fears frequently mentioned included knowledge of having a disease, fear of doctors and the medical community in general, and fear of losing one's job or missing work due to illness. Participant responses included:
People don't want to know because you can't do anything about it. If you tell me I've got all these things and I've got no health care, no money, what do I do then?
A lot of people approach doctors like they're God and are really fearful of them, whatever they say, okay.
I think a lot of what it is, is because it's such a poor area, people don't want to know if they have something, because if they know, then they feel like they have to treat it or, you know, they have to worry about it.
Experiences with the healthcare system
The quality of communication with physicians was a key aspect of participants' concern about health care and their ability to navigate the healthcare system. It was common for groups to express that not knowing what to ask their physician was a barrier to receiving good medical care. For example, one participant stated:
I think when we go to the doctor they don't tell you enough, if you don't ask specific questions which most of the time we won't know what questions to ask, they don't tell you.
Another pointed out that:
I've always gone to the doctor and I've never asked about my blood sugar. I'm just assuming it must be fine if he never said anything.
The issue of pride was also brought up as a reason why community members may not ask questions, even if they do know what to ask. Participants explained:
Sometimes it's a bit scary [going to] the doctor and [you] don't want to seem ignorant asking all these questions, or he'll explain it to you and then you won't understand it anyway because it's in Greek, right?
The [doctor] tells you a lot of things and uses a lot of big words that you don't understand, and not wanting to seem uneducated we just nod and say okay like we understand and really we don't.
Individual experiences with physicians were variable, but the overriding perception of physicians by focus group participants was that they do not have the time or resources to deal with inquiring minds and complex situations.
Community input on screenings and health outreach
Churches, local large store chains, health departments, health fairs and worksites were mentioned most frequently as sites useful for community screenings and the distribution of health education information. Some participants described good experiences with worksite wellness programs that did not consider participation in the program as time away from work. Health departments were mentioned as a place to link screenings with education, local health resources and social services. Participant responses included:
If I don't see some people at church, I see them at Wal-Mart [a chain of large, discount department and grocery stores]. If they don't go anywhere else they go to Wal-Mart.
I think the church is a good place if you want to start in the community because that's a common place, no matter how poor or rich we are
Canvassing, mail, newspaper advertisements, and television spots were mentioned as beneficial ways for community members to receive health information and advertise for community screenings. Many rural areas have free newspapers, and using those, combined with television advertising and going door to door, was mentioned as particularly good ways to reach the elderly population. Using word-of-mouth and local community participants to help with transportation for local kidney disease screenings was suggested as being important for getting people to participate.
In terms of what information about CKD should be learned and the preferred learning strategies, participants wanted to be able to identify symptoms, understand risk factors, and learn how to manage existing diseases. Those who had personal experiences with ESKD suggested having citizens tour dialysis facilities and speak with patients as an important educational experience. Statements included:
It needs to be emphasized what will happen and what you'll have to go through if you don't take care of yourself.
They need to take tours of hospitals and dialysis centers to be aware of these people who...you know they use water hoses, basically, to filter your blood. That's how big those needles are.
Keep it simple and just make it interesting. If citizens feel intimidated, then they'll block you out and not learn anything.
Discussion
This study illustrated that while community members are somewhat knowledgeable about how the kidneys work and have personal experiences with kidney disease, many do not understand risk factors and treatment options. Barriers to health care included poor communication with physicians and lack of access to specialty care, and community members described several outlets for marketing and distribution of health screenings and health information.
The use of focus groups was found to be an effective way to better understand perceptions of kidney disease, barriers to health care, and preferences for health education and screenings in high-risk, rural North Carolina communities. However, the use of purposive focus groups and qualitative data decreases the generalizability of these findings. Selective sampling was used to target high-risk participants for focus groups, which further limits generalizabilty to the general population. Group dynamics or participants uncomfortable speaking in groups may have also influenced participation rates within focus groups.
With respect to knowledge of kidney disease, focus group participants demonstrated some awareness about kidney disease and kidney failure but their knowledge about risk factors was poor. Those participants who did have knowledge about the disease had usually learned it second-hand from family members or friends afflicted with ESKD. Most participants were not aware that hypertension, diabetes, and family history of kidney disease are the primary risk factors for developing CKD. This low awareness has also been seen in larger cohort studies with at-risk populations11,13,14.
Participants' responses identified television and radio as the preferred media for receiving general health information and for learning about screening opportunities. Using television and radio lessen the need to travel and help expand outreach to those for whom transportation is an issue. Participants noted the value of taking at-risk community members to visit dialysis centers to better understand the challenges of living with ESKD. Educational interventions, including media campaigns, need to focus on helping participants recognize the primary CKD risk factors and relate early diagnosis and intervention as the best strategies to stop CKD or slow its progression17,18. Participants consistently cited lack of communication between themselves and their physicians along with uncertainty about what questions they should ask their physicians as barriers to health care. Public health interventions focused on educating community members about what kinds of questions to ask and how to advocate for one's self in a doctor's office may help remove some of the power differential between patients and providers.
Conclusion
Targeted, community-based focus groups are an effective way for public health educators to begin to assess a community's knowledge about a chronic health problem as well as to determine a community's preferences for ways to learn more about that particular condition. Future research efforts should measure the effectiveness and scope of community tailored health education programs for kidney disease and further explore preferences regarding the effectiveness of media messages versus delivery of factual health information.
Acknowledgement
This project was supported by grants from the UNC Ethnicity, Culture, and Health Outcomes Program and Abbott Laboratories.
References
1. Khan S, Amedia CA. Economic burden of chronic kidney disease. Journal of Evaluation in Clinical Practice 2008; 14(3): 422-434.
2. Schoolworth AC, Engelgau MM, Hostetter TH et al. Chronic kidney disease: a public health problem that needs a public health action plan. Prevention of Chronic Disease 2006; 3(2): 1-6.
3. United States Renal Data System. USRDS 2008 Annual data report: atlas of chronic kidney disease and end-stage renal disease in the United States. Bethesda, MD: National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, 2008.
4. Vupputuri S, Jennette CE. The burden of kidney disease in North Carolina 2007. Chapel Hill, NC: University of North Carolina Kidney Center, 2007.
5. Avorn J, Bohn RL, Levy E et al. Nephrologist care and mortality in patients with chronic renal insufficiency. Annals of Internal Medicine 2002; 162(17): 2002-2006.
6. Cass A, Cunningham J, Arnold PC, Snelling P, Wang Z, Hoy W. Delayed referral to a nephrologist: outcomes among patients who survive at least one year on dialysis. Medical Journal of Australia 2002; 177: 135-138.
7. Chan MR, Dall AT, Fletcher KE, Lu N, Trevedi H. Outcomes in patients with chronic kidney disease referred late to nephrologists: a meta-analysis. American Journal of Medicine 2007; 120: 063-1070.
8. Winkelmeyer WC, Glynn RJ, Levin R, Mittelman MA, Plisken JS, Avorn J. Late nephrologist referral and access to renal transplantation. Transplantation 2002; 73(12): 1918-1923.
9. Winkelmeyer WC, Mehta J, Chandraker A, Owen Jr, WF, Avorn J. Predialysis nephrologist care and access to kidney transplantation in the United States. American Journal of Transplantation 2007; 7: 872-879.
10. St Peter WL, Schoolwerth AC, McGowan T, McClellan WM. Chronic kidney disease: issues and establishing programs and clinics for improved patient outcomes. American Journal of Kidney Disease 2003: 41(5): 903-924.
11. Flessner MF, Wyatt SB, Akylbekova EL, Coady S, Fulop T, Lee F et al. Prevalence and Awareness of CKD Among African Americans: The Jackson Heart Study. American Journal of Kidney Disease 2009; 53(2): 238-247.
12. Nikolas TL, Gershon FD, Opotowsky AR, Arons R, Radhakrishnan J. Awareness of kidney disease in the US Population: findings from the National Health and Nutrition Examination Survey (NHANES) 1999 to 2000. American Journal of Kidney Disease 2004; 44(2): 185-197.
13. Plantinga LC, Boulware LE, Coresh J, Stevens LA, Miller III ER, Saran R et al. Patient awareness of chronic kidney disease: trends and predictors. Archives of Internal Medicine 2008; 168(20): 2268-2275.
14. Waterman AD, Browne T, Waterman BM, Gladstone EH, Hostetter T. Attitudes and behaviors of African Americans regarding early detection of kidney disease. American Journal of Kidney Disease 2008; 51(4): 554-562.
15. Bransford JD, Brown AL, Cocking RR (Eds). How people learn: brain, mind, experience and school. Washington, DC: National Academy of Sciences, 2001.
16. Glaser BG, Strauss AL. The discovery of grounded theory: strategies for qualitative research. Chicago, IL: Aldine, 1967.
17. Schwartz LM, Woloshin S. The case for letting information speak for itself. Effective Clinical Practice 2001; 4(2): 76-79.
18. Schwartz LM, Woloshin S. Marketing medicine to the public: a reader's guide. JAMA 2002; 287: 774-775.
