Introduction
A qualified and motivated health workforce is a key component for health system strengthening and achieving the UN Millennium Development Goals (MDGs)1. Recommendations suggest a minimum ratio of 2.5 health workers per 1000 people to achieve MDGs for health2. Nonetheless, most countries experience health staff shortages and maldistribution. This problem is aggravated in poor countries, where resources for producing health workers are scarce and retaining them in rural and remote areas is challenging. Health workers have tended to be concentrated in urban areas, while large rural populations remain under-served2,3. The scale of this problem varies considerably: Nepalese data show marked differences in physician-to-population ratios in urban (1:1000) and rural (1:41 000) areas3. In India, 74% of physicians practise in urban areas, where only 26% of the population live4.
Rural health staff retention is associated with several factors: financial rewards, career development, continuing education, work environment, resource availability, recognition/appreciation, and social factors (education for children, political stability, and rural upbringing)3,5. Economic incentives are used to motivate and retain health workers, but other strategies, such as improved working conditions, supervision and management, and education opportunities, have also influenced staff motivation and retention6,7.
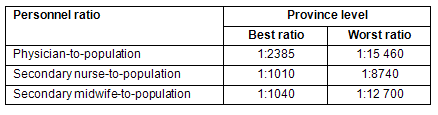
As in other low income countries, Cambodia faces challenges to ensure healthcare delivery to people in rural and remote areas because of the unequal distribution of doctors and increasing shortages of midwives8. Health staff distribution is heavily skewed toward urban areas, with approximately 54% of physicians employed in the capital city, Phnom Penh, where only 9.3% of the population live8 (Table 1).
Table 1: Health personnel-to-population ratio disparities in Cambodia9
The Cambodian public health system
Prolonged civil war devastated the Cambodian health system. Fewer than 50 of the 600 doctors who practised medicine before 1975 survived 'the killing fields', health facilities were damaged, and medical equipment was ruined10,11. After post-Khmer Rouge remodelling of the health system, the 'Health Coverage Plan' was launched to address health reform in 1995. This involved building new facilities in areas where none existed, and transforming existing hospitals and commune clinics into health centres. Concurrently, capacity in managing local health services was developed at provincial and operational district (OD) levels. Cambodia was divided into 77 ODs, each serving 100 000-200 000 people and containing one referral hospital (RH) and several health centres12. The health centre is the closest public health facility to the population, with each serving 8000-12 000 people. It provides basic preventive and curative services through the Minimum Package of Activities (MPA), including the treatment of common diseases (malaria, diarrhoea, sexually transmitted diseases), TB, leprosy, and minor injuries; child immunization; antenatal care and family planning; and refers cases to the hospital if necessary12. In addition to the MPA, the RH provides a Complementary Package of Activities (CPA), including treatment of complicated TB cases, referred cases, and medical, surgical and obstetrical emergency cases; in addition to surgery, maternal and child health, provision of X-ray, ultrasound and laboratory services, and rehabilitation services13.
Despite these reforms, health services in rural areas have yet to attain government benchmarks for health provision. The profound shortage of qualified health staff has contributed to poor performance. Two-thirds of the health centres in the country were unable to deliver full MPA because of shortages of midwives and nurses, while the upgrade of some RHs to fully implement the CPA was delayed because of shortages of qualified physicians13,14.
The root cause of these shortages is staff concentration in urban areas, strongly related to inadequate and irregular salaries, personal feelings about security, poor working conditions, shortages of drugs and medical supplies, and inadequate management of the rural government facilities8,14. Staff shortages in rural areas have also led to a rise in the informal health sector. Approximately 10 000 traditional birth attendants, and some thousands of untrained individuals, including traditional healers, work parallel with the formal health system in Cambodia; the majority are unlicensed9. When sick, most patients consult a private provider in their community, often a drug-seller or private practitioner whose convenience is related to proximity, availability and flexibility of payment by instalment15-17. Patients often perceive government services as low quality, with long waiting lists and unexpected high costs from informal payments18,19. These perceptions lead to delayed health-seeking from the public health centres.
Several factors contribute to poor performance and inhibit access to public health facilities in Cambodia. Financial incentive strategies, such as contract management and health equity funds, were introduced to address these, to specifically improve performance and encourage the utilization of the public sector19-23. However, little is known of how health workers struggle with institutional and financial challenges to remain in rural public health services. In this article, the various barriers that limit access to rural public health services are elaborated, and the way rural health workers maintain public health service delivery to the population they serve, while meeting their family's economic needs is elucidated.
Methods
The data used in this article derive from a larger ethnographic study conducted in 2008 with 32 tuberculosis (TB) patients, 12 family members, 10 health workers, two traditional healers, seven health volunteers, 24 key informants (village heads and community leaders), three policy makers and 240 community members in Kampong Speu Province, Cambodia. Kampong Speu province (population 722 605) is divided into three ODs with three RHs and 50 health centres (Fig1). The private health sector in the province comprises 140 chemist stores, 47 private clinics, 16 dental clinics, two maternity clinics, and two nursing clinics. In addition, Kru Khmer (traditional healers), unregistered providers without medical qualifications, and individual health workers, who run private clinics after office hours, provide health advice.
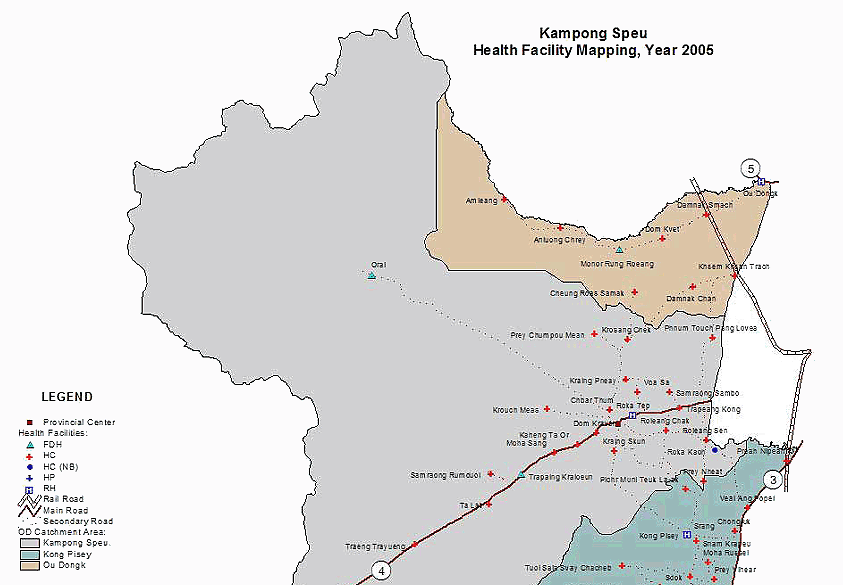
Figure 1: Map of Kampong Speu. Reproduced with the permission of the Ministry of Health, Cambodia.
In this article, data from the 10 health workers involved in TB control activities is drawn on. Participants were purposively recruited from health centres, the provincial hospital, and the provincial TB program; only health workers who had been involved in TB control activities were invited to participate. Data were collected using exploratory descriptive methods by the first author, and were derived from 10 in-depth interviews, participation in meetings and workshops, and observation of daily activities at select health centres and the hospital. An iterative approach was employed in data collection, whereby a theme that arose in one interview was used to inform subsequent interviews24,25. This was also used to determine data saturation and, therefore, to determine the sample size26. Data were imported into NVivo software (www.qsrinternational.com) for management and were analysed using a grounded theory approach27,28. Data analysis commenced by carefully reading individual transcripts, and identifying the themes and sub-themes which arose. Themes were cross-checked by all authors. A check was made for themes that emerged across transcripts, which allowed the identification of commonalities25. Themes were identified inductively24 and were used in developing the theory when approximately half of the participants spoke about them29. The main themes that arose related to:
- how rural health staff maintained health service delivery and family economic status
- barriers and incentives for retaining staff as government health workers undertaking TB control activities
- the impact of challenges of rural health workers on provision of public health services.
Rigour and validity were ensured by methodological triangulation and involving all authors in data analysis30. Ethical approval was obtained from human research ethics committees at Monash University, WHO/TDR, and the National Ethics Committee for Health Research, Ministry of Health Cambodia.
Results
Nine of the 10 health workers who participated in this study were men. Seven were secondary nurses (3 years training); the remainder included a laboratory technician, a pharmacist's assistant and a physician's assistant. Four worked in the provincial capital and six worked in rural health centres. All had been employed in their current position for 10 or more years and all worked on TB-control activities. Interviews indicated that rural health workforce retention was influenced by institutional factors relating to the structure of the health system, capacity building and staffing issues, competition from the private health sector and, significantly, issues concerning medical supplies. Personal factors proved central to individual health workers' decision-making about working in rural areas. These included work responsibilities and motivation, and issues around financial needs. Many of these factors overlapped, and each is now discussed.
Institutional factors
Service delivery and structure: Each health centre attempted to achieve quantitative targets set by the provincial health department. The main objectives of the National TB Control Program (NTP) for 2006-2010 were to attain a smear-positive TB case detection rate of over 70% and a cure rate of greater than 85%31. To reach these targets, each health centre was required to diagnose at least two patients each month. This implied variable workloads, with many patients screened in some months and few in others; achieving targets was influenced significantly by staff motivation and supervision. In 2006, Kampong Speu achieved a 73% smear-positive TB case detection rate and 89% cure rate32.
While health centres provided the basic MPA, they lacked facilities to diagnose many conditions. All X-ray, ultrasound or pathology tests, including for TB, were undertaken at the RH, often located some distance from the health centre. This contributed to increased workloads for participants, who had to travel to follow-up test results:
Each health center has an appointment date (eg Monday) with the laboratory to submit sputum and collect results, but in practice I have to travel many times per week to the lab because I can't get results on the appointment date.
In TB diagnosis, sputum collection often occurred at a different site to laboratory analysis, although some patients were sent directly to the RH. People seeking blood tests tended to be sent straight to the hospital or private laboratory. This fragmentation affected health centre utilization because patients went regularly to other providers, and motivation of staff who felt that their services were hindered and that their skills were underutilized.
Capacity building and staffing issues: All health centre staff underwent some formal training, recognized by the government for professional registration. This included short courses on MPA delivery, with additional, more specialised training delivered by different national programs (eg the NTP). However, limited capacity due to shortages of highly-qualified health staff contributed to difficulties in providing health care, including diagnostic delays:
TB diagnosis is based on lab sputum test, but at the health centre we don't have enough physicians to examine patients. We have a primary [one year training] or secondary nurse. So the capacity for diagnosis is limited.
At the same time, questions arose concerning staff capacity to perform their job responsibilities (eg diagnose) and regarding their efficiency, which resulted in poor health centre performance. This poor performance was widely known in the community, thus public health services were underutilized, affecting staff morale, responsibility and personal ethics:
The weak point of public health services is staff behaviour... Patients complain that they wait a long time to see staff, so don't want to come again, so we have fewer clients. Sometimes we don't have any drugs, so we refer them to the pharmacy. At the hospital, patients come when they are very sick but staff are slow to admit them, so they have to wait... These are our weak points.
Long waiting times did not necessarily reflect patient numbers, but were due to staff neglecting their patients, prioritizing other tasks (often meetings), and lack of organized systems (ineffective reception processes). With inadequate management and monitoring, these factors tended to undermine staff performance, making public health services less popular.
Competing with private providers: Although very poor people did not always have a choice, most people opted to go to a pharmacy or a private clinic when illness occurred:
I think people like to use private services first when they are sick... If their problem is severe, they go to hospital. Those who are very poor may use the health centre, because it is cheap and they can get medicine.
Because people associated use of the public health service with penury, there was considerable stigma associated with its use, encouraging people to use private services to avoid being stigmatized. However, staff also believed that public services were undermined by growth in the private sector, influencing patient choices and thus de-motivating public staff:
The private sector is strong and attractive. Pharmacy and drug stores are everywhere, drugs are sold like candies and some pharmacies offer other services such as injections, serum perfusion, and blood test. This can attract patients to use pharmacies more than health centres because we don't have those services... Private providers have good facilities and good drugs, and most are located around a health centre or hospital.
Public clinics lacked flexibility to offer convenience of care. This was a central attraction of private providers, many of whom also provided public services. For example, one nurse worked in a public clinic in the morning, and operated a flexible, private fee-for-service clinic in the evening. Although parallel private sector jobs competed with public health services, health staff believed that their involvement in both sectors provided community members with better healthcare choices:
We do private practice to get additional income, but at the same time we serve clients with a quality of care according to our skill and professional knowledge. I believe that our service is more reliable than unregulated providers or traditional healers... We always provide services with responsibility, no matter if it's private or public.
This presented a dilemma: parallel jobs contributed to staff retention in the rural health services because the fees supplemented low public sector salaries. At the same time, in addition to potential conflicts of interest, private practices took clients away from public services, thereby undermining the capacity of the public health service to deliver quality care (itself a de-motivating factor).
Medical supplies: At the time of the study, each health centre received monthly drugs and medical supplies from the Ministry of Health, through the OD. However, medical equipment and drugs were often in short supply (late, missed or reduced):
We see 10 to 20 clients daily when we have drugs, but if there are none, we have two or three... We meet drug shortages almost every month, so it is quite frustrating for us.
This frustration only occurred in the public sector and was heightened because staff could access these supplies through their private practices. Insecure supplies resulted in fluctuations in patient presentation, indicating that people sought medication rather than consultation in the public health centre. When drugs were unavailable, people saw little point in presenting to the health centre for advice. This reduced the health centre's role to that of a dispensary and contributed to job dissatisfaction.
Lack of supplies also hindered health providers' performance. The shortages of basic materials, such as alcohol, sputum cups, gloves and masks, contributed to poor prevention practices in the workplace - often already an issue due to providers' failure to implement correct infection control procedures:
We don't worry much about transmission because we know that after 15-20 days of treatment, TB does not transmit anymore. But I once had a severe TB case. I had to save him urgently so I did not take serious precaution... My work could put me at risk.
Health centres attempted to overcome supply shortages through user fees. However, this revenue was usually low compared with the market price of supplies; thus, health centres could not fully alleviate shortages:
We often have shortages, but our user-fees revenue was low. We used it to buy what is necessary for the health centre: alcohol, cotton, photocopying... We can't afford to buy everything [as] it is expensive.
Reliance on user fees to fulfil drug shortages was therefore an ineffective strategy, although it was often necessary to ensure health centre functioning. User fees also helped motivate staff:
Each month... [from] user-fee revenue, we use 49% for running costs, 1% for the government, and the rest is divided between staff: around 20 000 riels [$US5] per month.
However, chronically low user fees led to the ineffectiveness of this strategy to improve staff motivation.
Personal factors
Work responsibilities: Despite dissatisfaction with salaries, rural health staff enjoyed their jobs and believed they fulfilled their responsibilities:
I like my job, I have been working in the health centre for 12 years. The health centre has gradually improved... But the problem is that our salary remains very low. This makes staff not so productive at work... staff are always busy with their other job [so they can] earn their living.
Appreciation and optimism towards their jobs inspired health staff to stay for extended periods (>10 years). Participants attempted to maintain working hours in the morning, from 0800 to 1100 h; this varied depending on client numbers or other responsibilities (eg attending training or workshops). Staff mobile phone numbers were displayed at the health centre, so that patients could call them after hours:
I come to the hospital every day, but I have to finish around 1 or 2 pm, so that I can go back home and look after my other work.
Public phone booths are available in front of the health centre. Patients can call health staff if they need help. We display staff phone numbers on the wall at the entrance of the health centre.
Short and variable opening hours strongly undermined access and discouraged patients from seeking public services because of uncertainty about staff availability. In addition, relying on telecommunications to ensure access proved impractical for very poor patients, who tended to be reluctant to call clinic staff for assistance. Again, this presented a dilemma for the public health services; workers prioritized their private job which undermined their positions as public providers, and diminished patients' trust in and utilization of the wider public health system.
While acknowledging the conflict of interest posed by parallel jobs, and the implications of this for public health services, participants were reluctant to modify their own working patterns. They perceived that improvement in the public health sector was beyond their capacity, and was the responsibility of higher levels of the health system:
At lower levels, we respect and follow directions of the higher levels. If they assign us to do something, with adequate support, we can do it. I think that there are no problems at the lower level, we are committed, we know the problems, but we can't solve them. It is beyond our ability to deal with it.
Health workers' perceptions of powerless implied a culture of following top-down approaches without individual autonomy. It also highlighted their lack of motivation to take personal responsibility to improve the public health service, a manifestation of their conflict of interest.
Coping with financial need (personal coping): Rural health staff often faced the dilemma about how to manage their financial needs on a salary far below what they need to live. Despite recent increases, government salaries for health workers did not adequately reflect the cost of living. The net monthly government salary of health staff participating in this study ranged from approximately $US40 to $110 (average $US60) depending on qualification and position. Therefore, all staff had second jobs. This was not unusual; Sin indicated that most health workers in Cambodia had at least one private source of income33. Some staff in the present study were private providers, as noted; others (usually with lower qualifications) provided home-based care to patients:
I also have my private clinic in the market... After work, I stay at my clinic or I go to clients' places. It is legal to run a private practice. I have asked permission from the local authority and the provincial health department. We have to do many things to survive.
The opportunity to profit from private consultation varied, depending on clinic location, size, and staff expertise, as well as providers' strategies to maximise profits. Medical doctors earned at least $US200 monthly through private practice; specialists and dentists could earn even more33. However, private providers in rural areas were not always successful. Two participants closed their private practices and supplemented their income through farming or other businesses:
At first, I ran a private practice at home, but it was difficult. Many patients could not pay up front, they would pay by instalment. It was difficult for me to collect money, some have never been able to pay... I did not have money to buy new stock, I did not make profits. I decided to stop... [Now] I farm and raise chickens with my family.
As noted, parallel jobs enabled participants to meet the costs of everyday living expenses: informal payments and gifts also supplemented government incomes19,34-36. Not surprisingly, rural health staff reported that informal payments were uncommon and often patient-initiated to show gratitude, encourage better quality care, or to request additional services:
Informal payments may happen, but I don't think it is significant. Some patients give money to health staff as a gift. In some cases, when a patient is very sick, family members bring money to get more effective treatment, but we always tell them that we help according to our ability, and we give patients whatever we have at the facilities... I don't think providers force them to do that; we know it is not acceptable.
Lack of confidence in the quality of care provided at public facilities also prompted patients to initiate under-the-table payments in order to get better care. Although TB diagnosis and treatment was provided free of charge, some patients negotiated payments with providers:
I paid the health centre, because I negotiated with them to bring TB medicine for my father for every 2 weeks. (Daughter of TB patient)
I paid for my X-ray. Each time I submitted sputum, I paid so that I could get results quickly. If I didn't pay, I would have to wait longer. (TB patient)
Informal payments mainly resulted from patient-provider negotiations ensuring that TB patients did not have to attend the health centre daily during the first 2 months of treatment. Such practices were consistent with Khmer culture, where small gifts express gratitude and respect.
Although they described frustration and discouragement from low salaries and poor supplies, health staff advocated for the provision of public health services, particularly for the poor:
Our service is much cheaper than private services and beneficial for poor people. Our user-fees are low [and] set up according to the living standards of our local people.
Benefits to remaining in public health service: Institutional barriers meant that health providers underperformed in their public service positions; within the workplace, however, various factors were crucial in their decisions to remain in these positions.
Having a government position was valuable for participants, offering lifetime job security and acknowledging the importance of their qualifications and professional skills. Few vacancies and complex recruitment procedures also encouraged participants to retain their positions. In addition, staff could potentially increase their job responsibilities; holding interesting assignments was rewarding. One participant, for example, appreciated a job that fitted her qualifications:
I have worked as a lab technician for the hospital since 1981, with no promotion. But I like my work... Each day I read around 50 sputum smears, but there are still a lot more. I'm rarely absent from work, unless it is very necessary.
Government employment also conferred status, which was recognised and appreciated by community members, and facilitated access to other government services (eg school, police). In addition, a government job provided employees with opportunities to update their knowledge through participating in training or workshops:
The health centre is where the activities of all national programs gather to transfer to community members. I think I have a great opportunity to learn new things... We need to have knowledge on common health problems in the community.
Opportunities for professional improvement were important, providing education for individual staff to perform their work more effectively; however, unequal opportunities to access professional improvement may have de-motivated those with fewer opportunities.
In addition, recognised qualifications and work experience in the public system was important for staff pursuing private work. Seniority was attractive: community people preferred to go to private clinics to seek help from senior health providers who had worked at public services:
I've worked at the hospital for quite long, so that many patients know me and refer their friends to my private clinic. In private practice, we have to ensure quality and continuously upgrade our services and equipment otherwise clients don't want to use our service.
Staff built their networks, reputation and capacity at government facilities, then applied these for personal benefit in private practice. Government jobs also offered flexible working environments, without strict regulations regarding absence or punctuality, and staff could set their own working hours. This supported the institutionalization of parallel jobs, even though it adversely limited provision of public services.
Strategies were in place to compensate staff on especially low incomes: people were paid allowances to motivate work performance or to participate in training or workshops. Although the rates were small, participants regarded these opportunities as a kind of motivation to retain them in public facilities:
The NTP provides $US32 to follow-up patients, supervise sputum preparation, and provide health education. RHAC [an NGO] provides $US16 for health education. This amount is small but it can help us to supply fuel to travel to villages. More importantly, this budget never been cut or missed.
To go to villages for child immunization, staff get around $US1-2, a low amount not good for a living, but is an incentive for their work.
Financial incentives were important. Performance-based incentives, combined with supportive monitoring, motivated staff, encouraged them to take on increased responsibility, and might have been the most practical way to ensure quality staff performance and retention. However, social reasons were also important. Family acceptance into the local community was crucial in participants' decisions to remain in rural areas. Working in the public health service meant that health workers were able to keep their families together: all had a rural upbringing and were well accommodated by their local communities, even those originally from a different community.
Discussion
The delivery of primary health care services in rural Cambodia relied on the retention of mid-level health providers (midwives and nurses). Although low salaries contributed to staff dissatisfaction, other financial strategies motivated staff to work in rural areas and undertake TB activities. These included: job security, recognition and status in society, capacity building opportunities, flexible working environments, and allowances. This echoes research in Vietnam, Africa and Nepal which found that health workers were motivated through non-financial incentives such as appreciation and support from managers and colleagues, job and income stability, and provision of professional development opportunities3,37,38.
In Cambodia, the opportunity to hold parallel jobs - where health staff occupied positions in both public and private health services - played a central role in keeping health workers in rural areas7,39-41, yet also undermined their satisfaction with working in the public health system. Parallel jobs enabled health workers to earn a sufficiently high family income, and was widely accepted as necessary to meet economic demands. However, this created a conflict of interest, where health workers, either intentionally or not, diverted clients from public services to their private clinics8. Although the providers did not see it as problematic, this promoted increasing use of unregulated private facilities. This was exacerbated by poor access to and irregular supplies in public services, which drove community members to seek help from private providers, and contributed to high costs of health care and delayed access to appropriate care. Although TB diagnosis and treatment were provided free of charge at public clinics, patients usually chose private providers and only presented to public services when their health had deteriorated significantly.
Institutional barriers impacted significantly on rural health staff, hampering performance and contributing to poor utilisation of health services, particularly among the poor. The provision of basic care at public health centres was strongly influenced by staff motivation and input from higher levels: supplies, allowances to support activities, and appropriate supervision. Addressing these issues by providing secured supplies of drugs and equipment, implementing regular monitoring and supporting outreach activities would give staff motivation to achieve provincial targets.
Strategies to improve retention should balance the potential of non-financial benefits, financial opportunities, and staff workload. Institutional reform may not work, if the financial needs of health workers are addressed inadequately. The recent government decision to cease all salary incentive schemes from January 2010 potentially jeopardizes the current public health system42, unless alternative plans to ensure adequate financial benefits for public health workers are implemented. Ultimately, this decision will increase the health burden for people, particularly the poor, placing adequate health care further out of reach. This concern may be reflected through the reinstatement of salary incentives provided through donors until the issuance of a new government incentive modality43.
Limitations and implications
Several issues related to sampling and sample size may limit the generalisability of the study findings. First, our study only recruited staff actively involved in TB-control activities, who received regular governmental support (drugs, facilities). In consequence, it may include an overrepresentation of motivated health staff. Second, the small sample size may limit the generalisability of the findings; however, our use of theoretical saturation in determining sample size suggests that our findings may be relevant for other health workers in this province.
Conclusion
The data from this study provides important insights into how personal and institutional factors influence the motivation and retention of health workers in rural areas of Kampong Speu Province, Cambodia. The findings reported here also highlight an important direction for future research, within Cambodia and elsewhere, in order to understand whether issues around parallel jobs and public health system performance are applicable in other contexts. This research has implications for the delivery of health care to people in rural and remote areas, where access to services is already limited, and provides important insights into redressing the social and structural barriers affecting the provision of quality, affordable health care.
Acknowledgement
This research was supported by UNICEF/UNDP/World Bank/World Health Organization Special Programme for Research and Training in Tropical Diseases (WHO/TDR).
References
1. World Health Organization. The World Health Organization report: Working together for health. Geneva: World Health Organization, 2006.
2. Chen L, Evans T, Anand S, Boufford JI, Brown H, Chowdhury M et al. Human resources for health: Overcoming the crisis. Lancet 2004; 364(9449): 1984-1990.
3. Butterworth K, Hayes B, Neupane B. Retention of general practitioners in rural Nepal: A qualitative study. Australian Journal of Rural Health 2008; 16(4): 201-206.
4. Biswas R, Sarkar N, Umakanth S, Singsit J, Hande M. Medical education and the physician workforce of India. Journal of Continuing Education in the Health Professions 2007; 27(2): 103-104.
5. Brooks RG, Walsh M, Mardon RE, Lewis M, Clawson A. The roles of nature and nurture in the recruitment and retention of primary care physicians in rural areas: A review of the literature. Academic Medicine 2002; 77(8): 790-798.
6. Fritzen S. Strategic management of the health workforce in developing countries: What have we learned? Human Resources for Health 2007; 5(1): 4.
7. Henderson L, Tulloch J. Incentives for retaining and motivating health workers in Pacific and Asian countries. Human Resources for Health 2008; 6(1): 18.
8. Oum S, Keat P, Saphonn V, Oum P. Country reviews: Human resources for health and child survival in Cambodia. Bankok: Asia Pacific Action Alliance on Human Resources for Health, 2005.
9. Ministry of Health, Cambodia. Second biennial review of the health workforce development plan 1996-2005. Phnom Penh: Ministry of Health, Cambodia, 2001.
10. Mam B, Key PJ. Cambodian health in transition. BMJ 1995; 311(7002): 435-437.
11. Hill PS, Eang MT. Resistance and renewal: Health sector reform and Cambodia's national tuberculosis programme. Bulletin of the World Health Organization 2007; 85(8): 631-636.
12. Ministry of Health, Cambodia. Guidelines on minimum package of activities for the development of the health centre 2008-2015. Phnom Penh: Ministry of Health, Cambodia, 2007.
13. Ministry of Health, Cambodia. National guidelines for complementary package of activities for development of referral hospital 2006-2010. Phnom Penh: Ministry of Health, Cambodia, 2006.
14. Ministry of Health, Cambodia. Health achievements report 2004. Phnom Penh: Ministry of Health, Cambodia, 2005.
15. Khun S, Manderson L. Health seeking and access to care for children with suspected dengue in Cambodia: An ethnographic study. BMC Public Health 2007; 7. Available: http://www.biomedcentral.com/1471-2458/7/262 (Accessed 13 July 2010).
16. Saly S, Onozaki I, Shikawa N. Decentralized DOTS shorten delay to TB treatment significantly in Cambodia. Kekkaku 2006; 81(7): 467-474.
17. Yanagisawa S, Mey V, Wakai S. Comparison of health-seeking behaviour between poor and better-off people after health sector reform in Cambodia. Public Health 2004; 118(1): 21-30.
18. Khun S, Manderson L. Poverty, user fees and ability to pay for health care for children with suspected dengue in rural Cambodia. International Journal for Equity in Health 2008; 7: 10.
19. Barber S, Bonnet F, Bekedam H. Formalizing under-the-table payments to control out-of-pocket hospital expenditures in Cambodia. Health Policy and Planning 2004; 19(4): 199-208.
20. Hardeman W, Van Damme W, Van Pelt M, Por I, Kimvan H, Meessen B. Access to health care for all? User fees plus a health equity fund in Sotnikum, Cambodia. Health Policy and Planning 2004; 19(1): 22-32.
21. Van Damme W, Van Leeput L, Por I, Hardeman W, Meessen B. Out-of-pocket health expenditure and debt in poor households: Evidence from Cambodia. Tropical Medicine and International Health 2004; 9(2): 273-280.
22. Soeters R, Griffiths F. Improving government health services through contract management: A case from Cambodia. Health Policy and Planning 2003; 18(1): 74-83.
23. Grundy JJ. The impact of health system reform on remote health in Cambodia and the Philippines. Rural and Remote Health 1:84. (Online) 2001. Available: www.rrh.org.au (Accessed 5 July 2010).
24. Markovic M. Analyzing qualitative data: Health care experiences of women with gynecological cancer. Field Methods 2006; 18(4): 413-429.
25. Ryan G, Bernard H. Techniques to identify themes. Field Methods 2003; 15: 85-109.
26. Guest G, Bunce A, Johnson L. How many interviews are enough? An experiment with data saturation and variability. Field Methods 2006; 18(1): 59-82.
27. Strauss A, Corbin J. Basics of qualitative research: Techniques and procedures for developing grounded theory. Thousand Oaks: Sage, 1998.
28. Charmaz K. Constructing grounded theory: A practical guide through qualitative analysis. London: Sage, 2006.
29. Sandelowski M, Barroso J. Finding the findings in qualitative studies. Journal of Nursing Scholarship 2002; 34(3): 213-219.
30. Tobin GA, Begley CM. Methodological rigour within a qualitative framework. Journal of Advanced Nursing 2004; 48(4): 388-396.
31. National Centre for Tuberculosis and Leprosy Control (CENAT). National health strategic plan for tuberculosis control in the Kingdom of Cambodia: 2006-2010. Phnom Penh: Ministry of Health, Cambodia, 2006.
32. Hourt T. Achievements in 2006, Kampong Speu provincial health department. Kampong Speu: Provincial Health Department, 2007.
33. Sin S, Moeung P, Hun R, Ros S, Ros H, Leach K, Brosbst C. Cambodia health workers incentive survey. The Newsletter of Medicam 2005; 4(14): no page nos.
34. Lewis M. Informal payments and the financing of health care in developing and transition countries. Health Affairs 2007; 26(4): 984-997.
35. Vian T, Burak LJ. Beliefs about informal payments in Albania. Health Policy and Planning 2006; 21(5): 392-401.
36. Annear LP. Study of financial access to health services for the poor in Cambodia. Phnom Penh : Ministry of Health, WHO, AusAID and RMIT University, 2007.
37. Dieleman M, Pham VC, Le VA, Martineau T. Identifying factors for job motivation of rural health workers in north Viet Nam. Human Resources for Health 2003; 1(10). Available: http://www.human-resources-health.com/content/1/1/10 (Accessed 13 July 2010).
38. Mathauer I, Imhoff I. Health worker motivation in Africa: The role of non-financial incentives and human resource management tools. Human Resources for Health 2006; 4(24). Available: http://www.human-resources-health.com/content/4/1/24 (Accessed 13 July 2010).
39. Ferrinho P, Van Lerberghe W, Fronteira I, Hipolito F, Biscaia A. Dual practice in the health sector: Review of the evidence. Human Resources for Health 2004; 2: 14.
40. Gruen R, Anwar R, Begum T, Killingsworth JR, Normand C. Dual job holding practitioners in Bangladesh: An exploration. Social Science and Medicine 2002; 54: 267-279.
41. Jan S, Bian Y, Jumpa M, Meng Q, Nyazema N, Prakongsai P, Mills A. Dual job holding by public sector health professionals in highly resource-constrained settings: Problem or solution? Bulletin of the World Health Organization 2005; 83(10). Available: http://www.who.int/bulletin/volumes/83/10/771.pdf (Accessed 13 July 2010).
42. Royal Government of Cambodia. Sub-decree on ending of priority mission package and merit-based performance incentive. Phnom Penh, December 2009.
43. Council for the Development of Cambodia. Response to Royal Government's decision to review incentive arrangements and pay reform to accelerate public administration reform. Phnom Penh, January 2010.


