Introduction
Most emergency medicine (EM) residency programs are located in metropolitan areas in the USA with the majority of resident clinical experience occurring at the primary institution's urban emergency department (ED). Some programs also include a 'community ED' rotation, but these experiences typically occur in a suburban or urban environment in close proximity to the sponsoring institution. Few EM residency programs provide the opportunity to participate in a clinical rotation in a rural ED and only one, to the best of our knowledge, requires a rural EM month. Studies describing low numbers of EM residency trained/board certified emergency physicians (EPs) practicing in rural EDs has led to various initiatives intended to encourage residency graduates to consider a rural practice setting1,2. The development of clinical experiences in rural EM, limited to a few programs nationally, seeks to impact the EM residency graduate's choice of future practice location. However, beyond the perceived benefit of exposing EM residents to a rural practice environment, the clinical experience in a rural ED must provide a sufficient number of patients and adequate acuity to serve as a legitimate training site for EM resident physicians.
The purpose of this study was to compare the clinical experience of EM residents participating in a rural ED rotation with that of an urban university-based ED rotation.
Methods
The urban ED is located in a mid-western US city with a population of 404 267 and a metropolitan area population of 716 998. The ED serves a tertiary referral center with 31 beds including 4 trauma bays and a four-room fast-track area with an annual census of 42 647. The rural ED is located in a community of 14 814, approximately 480 miles (722.5 km) from the metropolitan area of the primary ED. The rural ED is a Level II trauma center and serves as a regional referral center for a four-state area. The ED is a 12 bed facility, including 3 trauma bays, with an annual census of 15 283.
Post-graduate year 2 (PGY2) EM residents completing both urban and rural clinical ED rotations self-reported the number of patients evaluated, number of patients admitted and admitting bed type, and the number and type of procedures performed over a 6 month period. Total admission rates, telemetry admission rates, and intensive care unit (ICU) admission rates were calculated and compared by z-test for two proportions. Total numbers for central venous access, procedural sedation, dislocation or fracture relocation/reduction, endotracheal intubation, laceration repair, lumbar puncture, tube thoracostomy, adult medical resuscitation, adult trauma resuscitation, pediatric medical resuscitation, pediatric trauma resuscitation, and the total number of ED hours completed at each clinical site were collected. Procedure and resuscitation numbers were calculated per 100 resident-hours in the ED.
Results
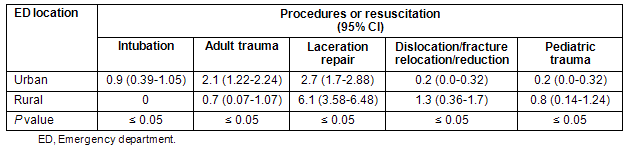
Five of six residents (83%) completed the clinical data forms. Patients evaluated per hour in the rural versus urban EDs were not different by a statistically significant margin at 1.22 and 1.21, respectively. Rural versus urban ED total admission rates were 21.74% (95% CI, 19.01-24.47) versus 33.35% (31.50-35.20), telemetry admission rates were 3.40% (2.28-4.52) versus 14.24% (12.87-15.61), and ICU admission rates were 0.9% (0.31-1.49) versus 4.38% (3.58-5.18), with the differences in all admission rates determined to be statistically significant (Table 1). Rural versus urban procedures/100 resident-hours in the ED were 0 versus 0.6 for central venous access (p = 0.087), 0.8 versus 0.3 for procedural sedation (p = 0.170), 1.3 versus 0.2 for dislocation or fracture relocation/reduction (p = 0.001), 0 versus 0.9 for endotracheal intubation (p = 0.026), 6.1 versus 2.7 for laceration repair (p < 0.001), 1.0 versus 1.0 for lumbar puncture (p = 0.845), 0.4 versus 0.2 for tube thoracostomy (p = 0.720), 2.4 versus 3.6 for adult medical resuscitation (p = 0.135), 0.7 versus 2.1 for adult trauma resuscitation (p = 0.023), 0.6 versus 0.3 for pediatric medical resuscitation (p = 0.642), and 0.8 versus 0.2 for pediatric trauma resuscitation (p = 0.034). The higher frequency of endotracheal intubations and adult trauma resuscitations per 100 resident-hours in urban versus rural EDs was statistically significant by z-test, while laceration repair, dislocation/fracture relocation/reduction, and pediatric trauma resuscitations occurred more frequently in the rural ED by statistically significant margins (Table 2). All other procedure and resuscitation types did not differ significantly.
Table 1: Percentage rural and urban emergency department total admission rates
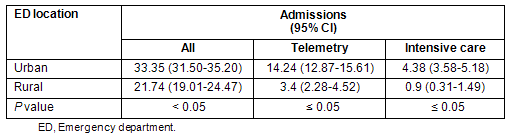
Table 2: Rural and urban emergency department procedures and resuscitations
Discussion
Past studies demonstrate a discrepancy between the numbers of urban and rural ED physicians in terms of American Board of Emergency Medicine (ABEM) certification and completion of EM residency training. One regional study found 65.2% ABEM certification for physicians in urban EDs versus 30.8% for those at rural sites and 48.3% versus 12.3% for EM residency training for urban versus rural practitioners3, while others report differences of 80% versus 29% for ABEM certification between urban and rural ED physicians at the state level4. On a national level for the USA, studies found ABEM certification rates for urban versus rural ED physicians of 72% versus 13.5%5, and EM residency training in 57% and 31% of physicians practicing in urban and rural EDs, respectively1. A recent study examining the supply of board-certified EPs for each US state reported an association between higher percent rural population and lower population density of EPs6. National estimates of the future supply of residency trained board certified EPs suggest a possible worsening of rural demand versus supply of residency trained EPs. Of EM trained or EM board-certified physicians practicing in rural areas in 2008, only 5% graduated from residency within the previous 5 years, while 15% graduated 20 or more years earlier1. In view of this discrepancy, the shortage of EPs practicing in rural areas is likely to increase in the future as these older physicians leave the workforce.
Recent reports from the Institute of Medicine (IOM) suggest strategies for increasing the EM workforce in rural areas, including increasing the number of residency programs located in rural areas2. The strategy of locating residency programs in areas lacking an adequate supply of qualified EPs seems logical. Steele et al. found that 43% of EM residency graduates chose initial practice locations in close proximity to their training program, and of these graduates 46% reported no prior personal associations with the area7. However, EM residency programs are relatively underrepresented in the rural states most in need of EPs, and, when present, these programs are typically located in the most urbanized area of the state8. One possible solution to this problem is to provide clinical experiences in rural EDs near the primary training program hospital in these rural states. Unfortunately, to the best of the authors' knowledge, few offer rural ED electives, no other EM programs in the USA requires a rural ED month, and no studies to date address the impact of such rural ED experiences on resident choice of initial practice location.
Recent reviews recommend financial support for rural EM residency programs or hybrid urban-rural programs2. The University of Nebraska Medical Center Emergency Medicine Residency Program is an example of an urban-rural hybrid. Meek found an increased likelihood of a rural ED as an initial practice choice for registrars completing greater than 12 months in hospitals in rural Australia, but no studies address rural experiences of shorter durations that would be typical of a hybrid program9. Future studies should address the impact of urban-rural hybrid programs with rural experiences of shorter durations on initial choice of practice location.
Not only are rural ED rotations a rarity for most EM residency programs in the USA, but also internationally. A recent review of the medical literature indicates that formal postgraduate medical education in EM is either lacking in rural clinical experiences as a required curricular component or rather that these rural rotations are underreported. Rural ED rotations likely occur in other countries, but are not specifically referenced as such. Notably, the Australasian College of Emergency Medicine (ACEM) requirements for graduate medical education in EM are flexible, allowing trainees to design their own programs. The individualized training programs often include clinical experiences in a variety of hospitals which may include rural EDs10. Some countries have focused on fellowship programs to improve the clinical skills of primary care physicians responsible for ED staffing in rural communities. Specifically, New Zealand and Canada offer postgraduate training programs designed to enhance the EM skills of non-EM residency trained practitioners11.
The relative scarcity of rural ED clinical experiences in the USA may result from past concerns regarding the adequacy of resident clinical experience in a low volume ED, leading to the program requirement of a minimum patient volume initially set at 36 000 per year in 1975, and later decreased to 30 000 annual ED patients12. The requirement sought to ensure adequate patient numbers, acuity, and procedures for a full complement of residents, but also resulted in the unintended consequence of limiting the options of ED rotations in smaller rural communities. The University of Nebraska Medical Center Emergency Medicine Residency Program first required rural ED rotation was initiated in 2004, after the Residency Review Committee for Emergency Medicine (RRC-EM) revised the minimum ED patient volume requirement to allow for 'educationally justifiable exceptions, such as clinical sites in a rural setting'12. The change in program requirements removed one major regulatory obstacle to rural EM rotations, but a lack of experience and familiarity with rural rotations may lead to a psychological obstacle that is difficult to overcome. Residency program directors and other decision-makers in the EM academic community may question whether the clinical experience would be feasible or worthwhile. However, no studies to date have reported the actual clinical experience of an EM resident rotating in a rural ED since the initiation of the exception to the 30 000 patients per year requirement.
Using data obtained from the only required rural ED rotation for EM residents in the USA at the time of the present study, the clinical experience of a single resident at a rural site- as determined by patients per hour and frequency of most procedures and resuscitation types was found to closely approximate that of a resident rotating in the primary ED of the residency program located in an urban area. A nearly identical number of patients per hour was found in residents rotating at the urban and rural sites, and similar procedure numbers for four out of seven procedures. Of the three procedures with statistically significant differences between the urban and rural sites, two occurred more frequently in the rural ED (fracture/dislocation management and laceration repair), while only intubations were performed more often in the urban ED. Likewise, resuscitations yielded a mixed result, with no statistically significant differences between two of four types (adult and pediatric medical), but resident experience with adult trauma occurring more frequently at the urban site and pediatric trauma at the rural ED.
Although residents rotating at both urban and rural sites reported a similar number of patients evaluated per hour, statistically significant differences in the acuity measures of telemetry and intensive care admissions - 14.24% versus 3.40% and 4.38% versus 0.9% for the urban and rural sites, respectively - indicate a rural site may not provide adequate ED critical care opportunities to serve as a primary training site. Furthermore, the statistically significant differences in the frequency of certain critical procedures and resuscitation types (such as intubations and adult trauma) require an assessment of the amount of time allocated for a rural ED experience in order to ensure adequate clinical experience during the course of residency training. However, while the residents included in this study performed fewer intubations than their urban counterparts during the 6 month study period, other procedures, such as the management of fractures and dislocations and complex laceration repair, were performed more frequently in the rural ED by statistically significant margins. In view of these findings, recommendations for locating EM residencies in rural areas may require specific modifications emphasizing the urban-rural hybrid approach, with balanced clinical experience incorporating the benefits available at both types of training sites.
Conclusion
A rural ED rotation provides an active clinical experience, with patients per hour and most procedure frequencies being similar to those at urban sites, but with lower patient acuity, as determined by both total and intensive care admission rates.
References
1. Ginde AA, Sullivan AF, Camargo CA. National study of the emergency medicine workforce, 2008. Annals of Emergency Medicine 2009; 54(3): 349-359.
2. Handel DA, Sklar DP, Hollander JE, Asplin BR, Hedges JR. Executive summary: The Institute of Medicine report and the future of academic emergency medicine: the Society for Academic Medicine and Association of Academic Chairs in Emergency Medicine panel. Academic Emergency Medicine 2007; 14(3): 261-267.
3. Wadman MC, Muelleman RL, Hall D, Tran TP, Walker RA. Qualification discrepancies between urban and rural emergency department physicians. Journal of Emergency Medicine 2005; 28(3): 273-276.
4. Reames J, Handel DA, Al-Asssaf A, Hedges JR. Rural emergency medicine: patient volumes and training opportunities. Journal of Emergency Medicine 2009; 37(2): 172-176.
5. Counselman FL, Marco CA, Patrick VC, McKenzie DA, Monck L, Blum FC et al. A study of the workforce in emergency medicine: 2007. American Journal of Emergency Medicine 2009; 27: 691-700.
6. Sullivan AF, Ginde AA, Espinola JA, Camargo CA. Supply and demand of board-certified emergency physicians by U.S. state, 2005. Academic Emergency Medicine 2009; 16(10): 1014-1018.
7. Steele MT, Schwab RA, McNamara RM, Watson WA. Emergency medicine resident choice of practice location. Annals of Emergency Medicine 1998; 31(3): 351-357.
8. Cheng D, Fernandez J. Emergency medicine residency underrepresentation in rural states. American Journal of Emergency Medicine 2005; 23: 92-93.
9. Meek R, Doherty S, Deans A. Factors influencing rural versus metropolitan work choices for emergency physicians. Emergency Medicine Australasia 2009; 21(4): 323-328.
10. Taylor Dm, Jelinek GA. A comparison of Austalasian and United States emergency medicine training programs. Academic Emergency Medicine 1999; 6(9): 972.
11. Arvier PT, Walker JH, McDonagh T. Training emergency medicine doctors for rural and regional Australia: can we learn from other countries? Rural and Remote Health 7: 705. (Online) 2007. Available: www.rrh.org.au (Accessed 4 April 2007).
12. ACGME. Program requirements for graduate medical education in emergency medicine. (Online) 2007. Available: http://www.acgme.org/acWebsite/downloads/RRC_progReq/110emergencymed07012007.pdf (Accessed 1 September 2009).
Abstract
Introduction:
Strategies for increasing the numbers of American Board of Emergency Medicine certified/emergency medicine (EM) residency trained physicians practicing in rural emergency departments (EDs) include providing rural EM experiences during residency training. However, no studies to date describe the clinical work of EM residents rotating in a rural ED. The objective of the study was to compare the clinical experience of EM residents participating in a rural ED rotation with that on an urban university-based ED rotation.Methods: Second-year EM residents completing both urban and rural clinical ED rotations self-reported the number of patients evaluated, number of patients admitted and admitting bed type, and the number and type of procedures performed over a 6 month period. Total admission rates, telemetry admission rates, and intensive care unit (ICU) admission rates were calculated and compared by z-test for two proportions. Total numbers for central venous access, conscious sedation, dislocation or fracture relocation/reduction endotracheal intubation, laceration repair, lumbar puncture, tube thoracostomy adult medical resuscitation, adult trauma resuscitation, pediatric medical resuscitation, pediatric trauma resuscitation, and the total number of ED hours completed at each clinical site were collected and procedure/resuscitation numbers calculated per 100 resident-hours in the ED.
Results: Five of six residents completed the patient data forms requested. Patients evaluated per hour in the rural versus urban EDs were 1.22 and 1.21, respectively. Rural versus urban ED total admission rates were 21.74% (95% CI, 28.19.01-24.47) versus 33.35% (31.50-35.20), telemetry admission rates were 3.40% (2.28-4.52) versus 14.24% (12.87-15.61), and ICU admission rates were 0.9% (0.31-1.49) versus 4.38% (3.58-5.18), with the differences in all admission rates determined to be statistically significant. Rural versus urban procedures/100 resident-hours in the ED were 0 versus 0.6 for central venous access (p = 0.087), 0.8 versus 0.3 for conscious sedation (p = 0.170), 1.3 versus 0.2 for dislocation or fracture relocation/reduction (p = 0.001), 0 versus 0.9 for endotracheal intubation (p = 0.026), 6.1 versus 2.7 for laceration repair (p < 0.001), 1.0 versus 1.0 for lumbar puncture (p = 0.845), 0.4 versus 0.2 for tube thoracostomy (p = 0.720), 2.4 versus 3.6 for adult medical resuscitation (p = 0.135), 0.7 versus 2.1 for adult trauma resuscitation (p = 0.023), 0.6 versus 0.3 for pediatric medical resuscitation (p = 0.642), and 0.8 versus 0.2 for pediatric trauma resuscitation (p = 0.034). The higher frequency of endotracheal intubations and adult trauma resuscitations per 100 resident-hours in the urban versus rural EDs was statistically significant by z-test, while laceration repair, dislocation/fracture relocation/reduction, and pediatric trauma resuscitations occurred more frequently in the rural ED by statistically significant margins. No other procedure or resuscitation type differed significantly.
Conclusion: A rural ED rotation provides an active clinical experience, with patients per hour and most procedure frequencies being similar to those at urban sites, but with lower patient acuity as determined by admission rates.
Key words: emergency medicine, residency education, rural rotation.
You might also be interested in:
2015 - Halter traction for cervical spine injuries - initial treatment in the district hospital
2009 - The impact of recession on the health care of rural citizens in the northwest United States



