Introduction
Despite major advances in drug and device therapy in chronic heart failure (CHF), morbidity and mortality remain high1. The reasons for this are multifactorial but in part due to suboptimal diagnosis and treatment of patients2. The diagnosis of patients with CHF can be difficult and may be inaccurate if based on clinical findings alone. Furthermore, access to tests such as echocardiography may be restricted in remote and rural areas. Even when the diagnosis is confirmed, ensuring all patients receive appropriate therapies appears difficult2. The management of patients with CHF is best delivered by specialists3 in a disease management program that include a central coordinating figure, most commonly a CHF specialist nurse4-6.
Most CHF specialist nurses will facilitate drug initiation and titration, facilitate discharge from hospital, improve patient education and self-management and improve communication with, and access to, specialist hospital based services. Recently, there has been an increase in the number of CHF specialist nurses in many parts of the UK but there remain some areas where there is no provision for this. Access to CHF specialists (doctors and nurses) may be particularly difficult in remote areas where there are fewer (or no) specialists and travel times are long for both staff and patients. Identified barriers to the implementation of modern therapies are complex but include inadequate communication between primary and secondary care, restricted access to tests such as echocardiography and inadequate provision and access to specialists7. The design of nurse-led heart failure services is generally based on evidence derived from urban or large city practice8 but the difficulties of implementing an effective CHF disease management programme in remote and rural areas have not been specifically examined. Furthermore, the role of guidelines and telehealth in areas where access and exposure to specialists is more restricted is unknown.
In 2005 a nurse-led heart failure service (3 whole-time equivalent nurse posts) was funded by the British Heart Foundation in the northern most part of mainland UK (Highland Region). This area represents 40% of the land mass of Scotland with less that 5% of the population and thus has many remote communities. The implementation of this CHF service faced significant challenges. Decisions about how to distribute nurses' time were difficult and resulted in a pragmatic balance between ensuring a nurse had a sufficient work load to maintain skills while at the same time striving to provide a local service. Travel time for home visits for remote patients was a particular challenge for some of the nurses.
Aims
This study aimed: first, to assess the perceived acceptability and effectiveness of a new community based nurse-led heart failure service by general practitioners (GPs) in an area with a dispersed population; second, to assess the knowledge and learning needs of GPs; and third, to assess perceptions of the use of national guidelines and telehealth on heart failure management.
Methods
Setting
The study was conducted in the Scottish Highlands, which covers a large geographical area including both rural and urban populations. The area has a total population of 240 000 and 260 GPs. Approximately 60% of the population live within 1 hour travel time of the largest urban centre. The region includes mountainous terrain and many islands with the consequent difficulties of poor communication and long travel times. There is one district general hospital and two rural general hospitals which offer echocardiography, although specialist cardiology services are centralised in the district general hospital. In addition, there are 12 community hospitals with no on-site access to echocardiography.
Study design and questionnaire
This was a postal survey of all GPs (n = 260) and structured email survey of all CHF specialist nurses (n = 3) in the Highlands. In the absence of a validated instrument a questionnaire was developed de novo in several iterative stages. Some questions were adapted from a previously used questionnaire3 and modified in several iterative stages by local managed clinical network team members. Questionnaires were distributed by surface mail once (Appendix I), and the structured e-mail survey was sent once to each of the CHF nurses (Appendix II).
Self-assignment to locality type by participants
For reasons of data protection and to achieve a maximum of data accuracy, this survey was anonymous to individuals although details of practice location were sought. The classification into 'rural', 'urban' or both 'urban & rural' locality was based on the self-assessment of the participants.
Formal ethical approval was not deemed necessary for this review of service provision. The concept and design of the questionnaire was guided by the local multidisciplinary cardiology managed clinical network.
Data collection and analysis
Questionnaires filled in by general practitioners were returned by fax or mail. The structured email responses from CHF specialist nurses were received electronically. All responses were entered into a Microsoft Excel spreadsheet, summarised and subjected to thematic analysis. Differences between GPs in 'rural', 'urban' or both 'urban & rural' were investigated using an F-test for continuous variables and a three-sample test for equality of proportions9 for nominal data.
Results
Questionnaires were returned from 83 GPs (32%) and all three CHF specialist nurses and the data were collated (Tables 1-3). This sample contained few differences among GPs from 'rural', 'urban' and 'urban & rural'. There also appeared to be little difference in the responses of those who had experience of the heart failure service from those who had not. A full results summary is provided (Tables 1-4).
Diagnosis and treatment of chronic heart failure
Overall, only 32 (39%) GPs wished for better, local access to echocardiography, while 63 (76%) wished for access to testing for brain natriuretic peptide (BNP). Only 27 GPs (33%) referred all patients with CHF to hospital. A number of GPs stated that it was dependant on individual circumstances and the patient's ability to travel as 'some are very elderly and frail don't want to go to hospital' (rural GP). It was clear that some GPs believed that referral to hospital is necessary 'in order to do an echo' (rural GP). Whereas other GPs stated that they 'managed the majority [of CHF patients] in the community' (urban & rural GP). Most GPs were confident to initiate standard heart failure drugs, although only 54 (65%) were confident in their initiation of beta-blockers (Table 1).
Acceptance of chronic heart failure specialist nurses by GPs
The GPs were given further opportunity to comment on a variety of different models for care delivery. The main area that received comment was that of the specialist nurse service where opinions varied greatly. Most GPs (69%) had had experience of the CHF specialist nurse service and generally the responses were positive (Table 2), although GPs who had experienced the service appeared less confident that it would lead to reduced admission of patients to hospital (51% vs 77%; p = 0.046). Some GPs stated that the specialist nurse service had 'improved care for patients and is an invaluable liaison with cardiology' (urban GP), while others stated problems with a 'disjointed service' (urban GP) and 'lack of clarity' (rural GP) regarding the specialist nurses role. The GPs appeared to value direct communication with consultants as 'most helpful' (rural GP) and 'very important' (rural GP), along with access to guidelines flow charts on the local National Heath Service intranet site.
Suggested improvements of existing chronic heart failure services
With regard to how the current service could be improved, the responses fell into two main themes. Communication was the most dominant theme where positive comments were reported, such as: 'excellent service - great communication and much appreciated by patients and me!' (rural GP) and 'all patients with heart failure should see a heart failure nurse' (rural GP). However, there were also a number of negative comments where 'better communication between GP and nurse' (urban & rural GP) and '...not clear what role the heart failure liaison nurse has' (urban & rural GP) demonstrate areas for improvement. The GPs also highlighted a preference 'for a locally based service' (urban & rural GP).
Table 1: Attitudes of 83 GPs in the Scottish Highlands towards the provision of care for patients with chronic heart disease, stratified by location
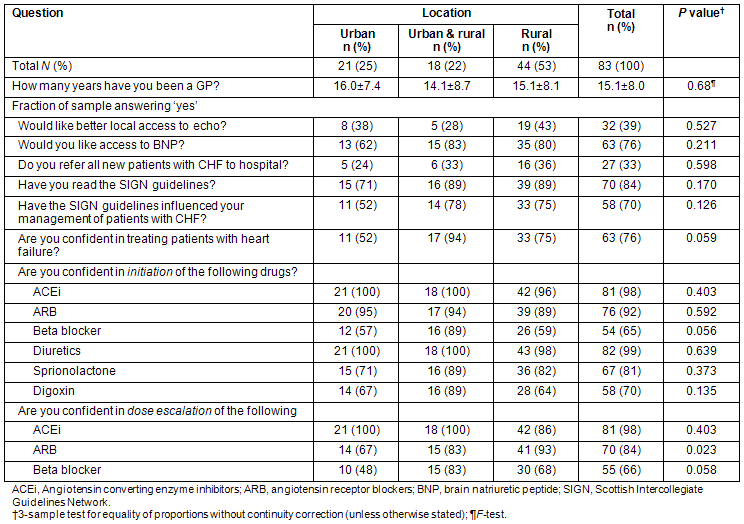
Table 2: General practitioners' views on community based chronic heart failure specialist nurse service, according to location
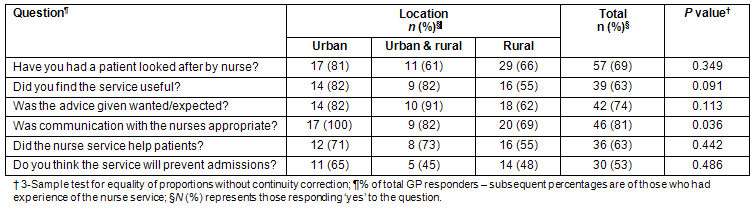
Table 3: General practitioners' views on general clinic provision for chronic heart failure patients, according to location
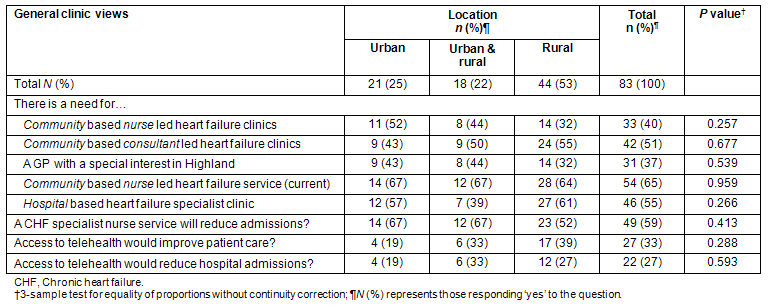
Table 4: Comments from GPs about the community based chronic heart failure specialist nurse service
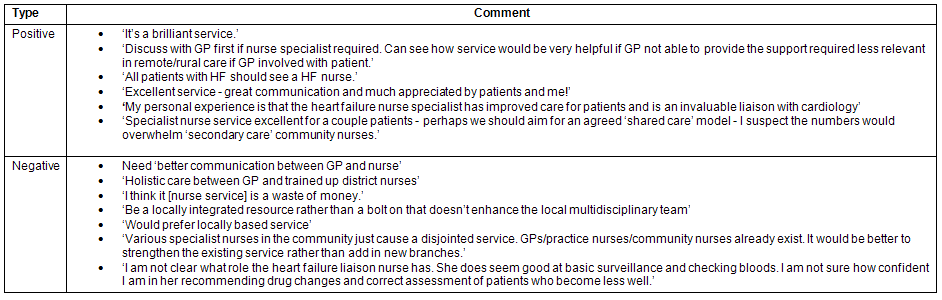
Perceived educational needs in primary care
All but one GP (n = 82; 99%) answered 'yes' to the hypothetical offer of additional training in heart failure. A majority of GPs also would appreciate training for their practice nurses (n = 60; 72%) and district nurses (n = 56; 67%). There were no statistically significant differences between urban, rural or urban & rural responses (all p>0.05). With regard to location and time of teaching sessions, many preferred local protected learning sessions within the working day, although evening meetings were also acceptable.
Responses from chronic heart failure specialist nurses
Three main themes emerged from the nurse responses: service planning, communication and attitudinal changes after service embedment. The CHF nurses consistently believed that greater pre-launch planning of the service could have helped implementation: '4-6 months of planning time' (nurse 1). It was a 'challenge trying to arrange to see all the GP practices' (nurse 2). 'Not a lot of research into how best to establish and maintain a heart failure service' had been conducted and that the implementation felt very 'ad hoc' (nurse 3). The nurses often felt that communication between the GP and the nurses was often suboptimal 'it was one way as we are not always kept in the loop' (nurse 1), another nurse commented that it felt like 'a one way road at times but I accept that this is just the way it is' (nurse 3). Access to GPs for urgent advice was also raised as an issue: 'communicating with GPs can be difficult, especially if you need to discuss a patient with them and they are in surgery' (nurse 2). The nurses collectively noted changes in GPs' attitudes after a period of time had passed. It was said that in the beginning of the service it was difficult to 'gain confidence and trust from the GPs' (nurse 2) and that 'some [GPs] feel that we complicate the picture' (nurse 1). However, it was noted that after some initial negative experiences, GPs were now 'happier with the service' (nurse 2) acknowledging that 'it takes time to develop a rapport with the GPs' (nurse 2).
Discussion
Implementation of community heart failure services is potentially difficult7. This study demonstrates that a community based heart failure nurse service was not universally valued, despite evidence from well-conducted randomised controlled trials which demonstrate their benefit8. This study also demonstrated some differences between urban and rural localities (communication) suggesting that models of care derived from evidence based practice in urban areas may not be directly transferable to remote areas. However, more striking were the similarity in responses between remote and rural GPs, despite great geographical diversity and relatively poor access to echocardiography in remote areas, that may reflect a negative adaptive response within primary care to historically poor access to tests.
Management of chronic heart failure in primary care and referral to hospital
In the current study a large number of GPs did not refer all patients with heart failure to a cardiologist and many appeared to see the hospital referral only as a mean to obtaining an echocardiogram. The widespread belief that heart failure can be treated without referral to specialists is despite evidence suggesting that management of heart failure by specialists is advantageous10. Important differences exist in the treatment of CHF patients between specialists and non-specialists3,11, while the skills and interest of GPs vary considerably12. This does not imply that GPs are not key to the diagnosis or the treatment of patients with CHF; however, unless GPs have a specialist interest they are unlikely to know which patients should be referred for more advanced heart failure therapies such as cardiac resynchronisation therapy, implantable defibrillators or transplant. This may be particularly true in more remote areas with small practice lists and fewer GPs.
Furthermore, although in the UK the 'new GP contract' aimed to standardise treatment with certain performance indicators12, these are extremely limited and include only the identification of patients, the documentation by echocardiography of left ventricular systolic dysfunction, and the use of angiotensin converting enzyme inhibitors (ACE-I) and, more recently, beta-blockers. Thus, even a GP score of 100% in these performance indicators does not necessarily represent comprehensive or high quality care in the modern era of CHF treatments.
In the current survey only 24% of urban GPs would refer all patients with heart failure while only 52% reported feeling confident in treating CHF. Referral rates from urban GPs were low, with a trend towards rural GPs being more confident in treating heart failure. This is in contrast to data from Australia where referral rates are significantly lower in rural towns compared with metropolitan areas13. It is of interest that in our study the referral rate appeared to be greater from GPs who were more confident in treating heart failure, which suggests that a lack of knowledge, perhaps regarding what specialist services might offer, results in fewer referrals. This deserves more study.
Access to diagnostic services
Reduced access to diagnostic tests such as echocardiography has previously been identified as a barrier to the delivery of good care14-17. In the present study the desire for better access to echocardiography was lower than expected. This may be due to the fact that a direct access service has already been established in this geographic area for some time and the comments regarding this service have been favourable. However, this service is only available at the 3 district/rural general hospitals and there is no local or domiciliary service. Indeed, echocardiography is not available for inpatients at any of the 12 community hospitals in this area. Nevertheless, surprisingly, fewer than 50% of rural GPs wished for better local access to echocardiography. Local audit data (S Leslie; pers data; 2009) found that patients who were most remote were least likely to have an echocardiogram; however, in the present study it was urban GPs who were least likely to refer all new patients with left ventricular systolic dysfunction to a hospital clinic (24%).
A high proportion of GPs expressed a wish for access to measurement of plasma BNP. The utility of BNP as a screening test for heart failure has been proven in a number of clinical settings including outpatients17,18, and is supported by many national CHF guidelines19-21. Nevertheless, the clinical use of BNP is not widespread in the UK, probably due to concerns about cost effectiveness. It might have been expected that GPs in more remote and rural practice would have greater support for the use of BNP, but in the current study, BNP appeared to be equally highly favoured by urban GPs. This support of the use of BNP is of particular interest in rural areas where access to echocardiography is less easy. For BNP could have a greater impact as a screening test in rural primary care and in remote community hospitals where there is no on-site access to echocardiography.
Role of guidelines
The majority of general practitioners in this survey reported having read the recent national guidelines21. This is encouraging, although it could be that the questionnaire responders were GPs with an interest in CHF. However, in the study sample, only 50% of urban GPs reported that their treatment of patients was influenced by guidelines. This is surprising because the new guidelines include significant changes to practice from previous guidelines. While the response of the present GPs may reflect that they had implemented these treatments already, it is possible that despite reading the guidelines, the GPs were not using current CHF treatments. Furthermore, it has been recognised that the impact of written guidelines on affecting management changes may be limited11,22. Alternative approaches to improving diagnosis and management have been attempted, including computer decision-support software, although these technologies are difficult to implement for a variety of reasons23. Implementing evidence based therapies is one of the key roles of CHF specialist nurses and the presence of clear national guidelines supports this process.
Confidence in treating chronic heart failure
As expected, there was a high level of confidence in the initiation of drugs such as loop diuretic and ACE-I and angiotensin receptor blockers, although confidence was somewhat lower for spironolactone, digoxin and beta blocker. These data are consistent with findings from previous studies7,13-16,24, with major concerns relating to side-effects, contraindications and co-morbidities. In particular, confidence in initiating beta-blockers was relatively low. Interestingly, confidence in initiation and escalation of angiotensin receptor blockers (ARBs) was lower than for ACE inhibitor despite almost identical 'risks' for these two therapies. Perhaps greater confidence with ACE inhibitors reflects greater familiarity with these less expensive drugs due to more widespread use in patients with renal disease and hypertension. While most GPs were happy to initiate ARBs, GPs were less confident in dose escalation and this represent a specific area of educational need.
Telehealth
In general, there was little confidence expressed in the role of telehealth from this cohort of GPs. There are several studies supporting the use of telehealth in the outpatient setting. However, the benefits were variable between studies25 and the cost-effectiveness of telehealth systems in CHF is not yet fully determined by the UK national health service. The appropriate use of technology has the potential to improve patient care, but the clinical usefulness of such technology in patients with heart failure is unclear.
Community based nurse-led heart failure service
The value of the specialist CHF nurses is well established8, and a national charity (British Heart Foundation) has been heavily involved in developing a network of CHF nurses throughout the UK. In the present study the GPs service ratings were generally lower than expected; however, when asked about need for a community based nurse-led heart failure service, the majority agreed there was a need.
A major 'theme' from the CHF nurses' responses was of initial resistance to the implementation of specialist nurse-led services in primary care by many GPs, which had lessened once the GPs experienced the benefits of the service. However, our study demonstrated that the views GPs who had personal experience of the service did not differ substantially from those of GPs with no personal experience of the service. This could either be because it is difficult to change views, or that the service was genuinely poorly received by GPs - although there was no reduction in support for the service in GPs who had used it, suggesting that the service at least met these GPs' expectations. The GPs seemed inappropriately pessimistic about the effects of the nurse-led heart failure service on readmission rates. There is compelling evidence that heart failure nurses reduce admissions to hospital by approximately 50%8, although only 53% of GPs in our survey thought the service would reduce admissions. Either the GPs were not cognisant of the data, thought that it did not apply to their patients, or did not believe that the local heart failure service could deliver this benefit.
'Primacy' or control remains an issue between GPs and specialist nurses. This may be more so in remote areas, where professional boundaries are likely to be more jealously guarded as GPs have traditionally been expected to treat a wide range of conditions with less easy access to specialist advice than their urban or city counterparts. In the study area, it was decided not to enable drug prescribing privileges for local heart failure nurses. Despite this, they are trained (and able) to make medication changes but this is done via the patient's GP, ensuring the GP remains in overall 'control' of a patient's treatment. The issue of control was echoed in the heart failure nurses responses, where difficulties in gaining GPs confidence and trust was reported. It was also noted that some GPs were happy for the nurses' involvement while others felt it complicated matters, a response supported by the GPS' qualitative comments.
Defining rurality
Defining rurality and remote medical practice is complex26,27. This current study took a pragmatic approach to this issue with individual doctors asked to report if they worked in a 'rural', 'urban' or both 'urban & rural' locality. Because the questionnaire was anonymous and no geographic information available, it was not possible to classify answers objectively according to location. This approach may have introduced some misclassification; however, there was no reason for GPs to classify themselves incorrectly (introduced bias). In fact, the Scottish Highlands as a whole is a very rural area when compared with conurbations around major cities in the south of England or central Europe. In this study, the term 'urban' therefore should be interpreted as 'relatively urban'. This may explain why the responses of GPs from rural and urban localities did not differ strongly. However, that a pattern of differences was observed, suggests that these differences would have been more pronounced if data had been collected from metropolitan areas as well.
Limitations
This study was conducted on a convenience sample in an overall sparsely populated area and so the sample size was small. Furthermore, the response rate was relatively low from GPs and this limits generalizability. Nevertheless, the low response rate probably reflects the comparatively low priority that heart failure is afforded in healthcare systems. This may be due, in part, to the historical lack of treatments and difficult diagnostic tests; however, this is no longer the case. Finally, this questionnaire was administered by some members of the heart failure service as well as the local managed clinical network for cardiology. While the questionnaire responses have been reported accurately, the authors accept there is a potential for bias.
Conclusions
This study demonstrates that a community based heart failure nurse service was not universally valued. Differences between urban and rural localities (communication) suggest that models of care which have been derived from evidence based practice in urban areas may not be directly transferable to remote areas. Clearly, good communication between staff groups at all stages of implementation is important, but despite best efforts and clinical trial evidence, specialist nurse services will not be welcomed by all doctors. Nevertheless, particular attention should be made to maximise clear aims and objectives of any new service prior to launch, and there should be surveillance of communication within the service. Service providers and commissioners should be cognisant of the different roles of urban and rural GPs when designing such services. Among GPs, there was a high degree of confidence with initiation and titration of drugs for heart failure with the exception of beta-blockers. Clearly this is an area of need for ongoing education and support. Education and support should also focus on ensuring that all doctors who care for patients with CHF have the skills and confidence to use medical therapies and specialist services as appropriate.
Acknowledgements
The authors thank the GPs and CHF specialist nurses who contributed to this study. The authors also thank Drs E Imray, R Aleeson and B Peters for comments made during the preparation of this manuscript. Author EM is supported by a Clinical Academic Fellow secondment funded by the University of Stirling. The community based CHF specialist nurses are part funded by the British Heart Foundation.
References
1. Clelland JGF, Gemmell I, Khand A, Boddy A. Is the prognosis of heart failure improving? European Journal of Heart Failure 1999; 1: 229-241.
2. Richard RFD, Korewicki J, Cleland JGF, Eastaugh J, Freemantle N on behalf of the IMPROVEMENT Investigators. The diagnosis of heart failure in European primary care: The IMPROVEMENT Programme survey of perception and practice. European Journal of Heart Failure 2005; 7(5): 768-779.
3. McKee SP, Leslie SJ, LeMaitre J, Webb DJ, Denvir MA. Management of chronic heart failure by cardiologists and non-cardiologist physicians. European Journal of Heart Failure 2003; 5: 549-555.
4. Göhler A, Januzzi JL, Worrell SS, Osterziel KJ, Gazelle GS, Diety R et al. A systematic meat-analysis of the efficacy and heterogeneity of disease management programs in congestive heart failure. Journal of Cardiac Failure 2006; 12: 554-567.
5. Gonseth J, Guallar-Castillón P, Banegas JR, Rodriguez-Artalejo F. The effectiveness of disease management programmes in reducing hospital re-admission in older patients with heart failure: as systematic review and meta-analysis of published reports. European Heart Journal 2004; 25: 1570-1595.
6. Wilson M, Leslie SJ. Models of care and disease management programmes. In: C Ward, M Witham (Eds). A practical guide to heart failure in older people. New York: Wiley, 2009.
7. Fuat A, Hungin APS, Murphy JJ. Barriers to accurate diagnosis and effective management of heart failure in primary care: qualitative study. BMJ 2003; 326: 196.
8. Blue L, Lang E, McMurray JJ et al. Randomised controlled trial of specialist nurse intervention in heart failure. BMJ 2001; 323: 715-718.
9. Newcombe RG. Interval estimation for the difference between independent proportions: comparison of eleven methods. Statistics in Medicine 1998; 17: 873-890.
10. Phillips CO, Singa RM, Rubin HR, Jaarsma T. Complexity of program and clinical outcomes of heart failure disease management incorporating specialist nurse-led heart failure clinics. A meta-regression analysis. European Journal of Heart Failure 2005; 7(3): 333-341.
11. McKee SP, Leslie SJ, LeMaitre J, Webb DJ, Denvir MA. Physician opinions on the implementation of the SIGN guideline for heart failure. Scottish Medical Journal 2004; 49: 10-13.
12. Leslie SJ, McKee SP, Imray EA, Denvir MA. Management of chronic heart failure - perceived needs of General Practitioners in light of the new GMS contract. Postgraduate Medical Journal 2005; 81: 321-326.
13. Clark R, Eckert K, Stewart S, Philips S, Yallop J, Tonkin A et al. Rural and Urban differences in primary care management of chronic heart failure: new data from the CASE study. Medical Journal of Australia 2007; 186(9): 441- 445.
14. Khunti K, Hearnshaw H, Baker R, Grimshaw G. Heart failure in primary care: qualitative study of current management and perceived obstacles to evidence based diagnosis and management by general practitioners. European Journal of Heart Failure 2002; 4(6): 771-777.
15. Philips SM, Marton RL, Tofler GH. Barriers to diagnosing and managing heart failure in primary care. Medical Journal of Australia 2004; 181(2): 78-81.
16. Gnani S, Gray J, Khunti K, Majeed A. Managing heart failure in primary care: first steps in implementing the national service framework. Journal of Public Health 2004; 26(1): 42-47.
17. de Lemos JA. Combining natriuretic peptides and necrosis markers in the assessment of acute coronary syndromes. Cardiovascular Medicine 2003; 4(Suppl4): S37-46.
18. Weber M, Hamm C. Role of B-type natriuretic peptide (BNP) and NT-proBNP in clinical routine. Heart 2006; 92: 843-849.
19. Remme WJ, Swedberg K. Comprehensive guidelines for the diagnosis and treatment of chronic heart failure. Task force for the diagnosis and treatment of chronic heart failure of the European Society of Cardiology. European Journal of Heart Failure 2002; 4: 11-22.
20. National Institute of Clinical Excellence. Management of chronic heart failure in primary and secondary care . NICE Guideline no.5. London: NICE, 2003.
21. Scottish Intercollegiate Guidelines Network. Management of chronic heart failure. SIGN no.95. Edinburgh: Royal College of Physicians Edinburgh, 2007.
22. Leslie SJ, Denvir MA. Best practice for chronic heart failure patients - writing guidelines is not enough. European Heart Journal 2008; 29: 1706-1708.
23. Leslie SJ, Hartswood M, Meurig C, McKee SP, Slack R, Procter R et al. Clinical decision support software for management of chronic heart failure: Development and evaluation. Computers in Biology and Medicine 2006; 36: 495-506.
24. Hickling JA, Nazareth I, Rogers S. The barriers to effective management of heart failure in general practice. British Journal of General Practice 2001; 51(469): 615-618.
25. Chaudhry SI, Phillips CO, Stewart SS, Riegel B, Mattera JA, Jerant AF et al. Telemonitoring for patients with chronic heart failure: a systematic review. Journal of Cardiac Failure 2007; 13: 56-62.
27. Muula A. How do we define 'rurality' in the teaching on medical demography? Rural and Remote Health 7(1): 653. (Online) 2007. Available: www.rrh.org.au (Accessed 29 September 2010).
27. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P, Baker L, Kelly M, Love C. Defining remote medical practice. A consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 159-161.
______________________________
Appendix I: Survey of Community Based Highland Heart Failure Service

Appendix II: Structured Questionnaire for CHF Specialist Nurses


