Context
Because there are critical nursing shortages in rural settings, recruitment of nurses to these areas is vital1. Providing nursing students with positive learning experiences that include exceptional clinical experiences is one strategy that supports the recruitment of qualified nurses into these underserviced areas1-3. Critical shortages exist both in Canada and around the world. For instance, according to the Canadian Institute for Health Information4, only 17.9% of all registered nurses in Canada work in rural areas where 21.7% of the population lives. The USA and Australia also report shortages of nurses in rural and remote areas5-7.
While a number of recruitment strategies have been suggested to address the shortage of rural nurses, one that stands out is nursing education with its practice-based learning opportunities. Research has shown that students who have positive learning experiences in rural settings are more likely to work in rural settings after graduation8,9. As a result there is increasing interest in encouraging nursing students to pursue rural clinical placements during their education.
Issue
Urban students on rural clinical placement face unique challenges, whether they commute to the clinical environment or move there for the duration of the placement. In addition to the challenges of the actual setting, there are logistical and educational issues that involve the student and their educational institution. For educators, ensuring quality nursing education for students in rural areas can be challenging, and few nursing programs adequately prepare students for the distinct, diverse, and challenging nature of rural practice9.
While definitions of the term 'rural' vary, distinct characteristics of rural areas include isolation, limited access to healthcare resources, small populations, significant distances between services and providers, and informal social structures1,9. For example, in Canada rural settings are often in northern areas and this may pose unique challenges for students. However, southern rural placements may present students with contrasting but equally unique challenges. In short, rural placements regardless of geographical location can present students with unexpected challenges.
Purpose of this review
Nursing students' positive learning experiences in rural settings have been associated with their preparation for rural nursing placements2. If negative learning experiences are associated with poorer or less preparation, it is reasonable to assume that negative rural-setting learning experiences result in students choosing urban careers. If, though, nursing educators and others who support undergraduate nurse-learners understand the challenges for students in rural settings and develop strategies to ensure adequate preparation for rural clinical placements and support during the experience, there are important possibilities, among them the recruitment of these students to rural settings after graduation. Therefore, the purpose of this literature review was to explore the following question: 'What challenges do nursing students from urban communities experience during clinical placements in rural areas, respecting that 'rural' is conceptualized differently by different stakeholders?'
Theoretical framework
As a means of understanding the educational and resource issues of rural settings, the Ecological Model10 was chosen as the theoretical lens for this review. Although this model was first developed to examine health promotion, it can be applied to other domains including nursing education. The model enables consideration of students as individuals who are influenced by an ecosystem that includes political and other systems; community; institutional/organizational variables; interpersonal variables; and individual variables11. These categories were used in the present review, with the institutional/organizational category divided into: (i) nursing, to represent the nature of rural clinical placements; and (ii) educational, to represent the institution. In addition, the physical environment emerged as a system that influences the experience. Thus, the version of the Ecological Model used here includes 7 components defined by the findings: political, environmental, community, nursing, educational, relational, and personal.
Understanding the myriad of factors that influence student learning in a rural setting is vital to the development of quality learning experiences and, ultimately, the recruitment of nurses to rural areas.
Literature review
This literature review was structured according to the methodological strategies proposed by Whittemore and Knalf12. The review followed a 5 stage process including the following: (i) identification of the problem and purpose of the review; (ii) a structured literature search; (iii) data evaluation; (iv) data analysis; and (v) presentation of findings.
Search strategy
Computerized database searches of CINAHL and PubMed, reference chasing, and searches of specific rural health journals were conducted. Development of inclusion criteria facilitated the identification of relevant references. Quantitative and qualitative research studies and other relevant publications including program evaluations in English prior to February 2010 were considered. Selected articles examined the challenges faced by undergraduate nursing education students in rural areas. In some instances, these articles also examined the perspectives of educators.
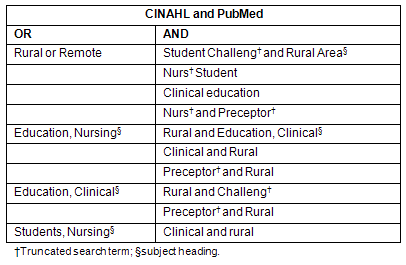
All definitions of 'rural' used in the literature were accepted because there is no single agreed definition13. Self-defined rural settings from any geographical region were included. No restriction was placed on the date of publication because a preliminary search yielded only a few results. Key terms were used in all searches (Table 1), resulting in the identification of 13 documents for inclusion: 8 qualitative research studies, 2 quantitative research studies, and 3 program evaluation reports.
Table 1: Search strategy for databases
Assessment of methodological quality
The qualitative studies were assessed for congruency, creditability, reflexivity, ethics, and auditability as defined by the Joanna Briggs Institute Qualitative Findings Critical Appraisal Scale14. This tool is part of the Joanna Briggs Institute Qualitative Assessment and Review Instrument (Fig1). The quantitative studies were assessed for sampling, use of a theoretical framework, discussion of reliability and validity, analysis methods, and generalizability of findings through use of a checklist designed for assessing the quality of descriptive and correlational studies15. This tool is a component of the Joanna Briggs Institute Meta Analysis of Statistics Assessment and Review Instrument (Fig2). Both tools contain 10 items (Figs1,2). The reviewers scored each item based on the presence (1) or absence (0) of each criterion. If a criterion was unclear, it received a score of 0. Studies then received a final score ranging from 0 (low quality) to 10 (high quality). The research studies were then classified based on their total appraisal scores as either low (1-3), medium (4-6), or high (7-10) quality.
The quality of the three program evaluation papers was determined based on clarity, support, and logical flow of arguments. Both reviewers conducted a separate quality assessment of the articles and discussed differences in their ratings.
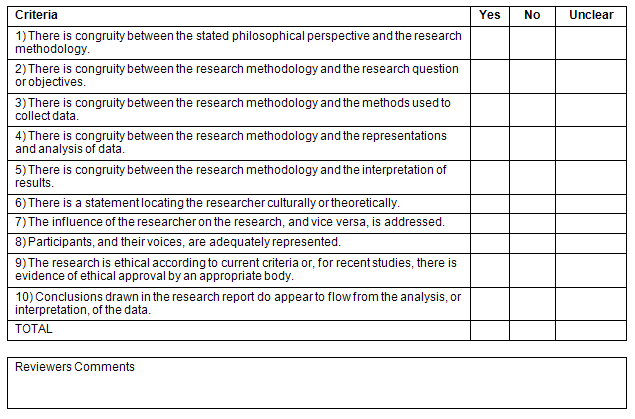
Figure 1: Qualitative Findings Critical Appraisal Scale. Reproduced with permission14.
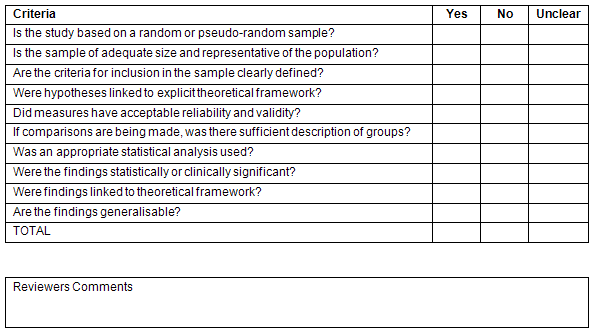
Figure 2: Checklist for Assessing the Validity of Descriptive/Correlational Studies. Reproduced with permission15.
Data collection
The Joanna Briggs Institute Qualitative Data Extraction Tool14 (Fig3) is part of the Joanna Briggs Institute Qualitative Assessment and Review Instrument, and it was used in the present study to document and organize data relating to methodology, interventions, setting, participants' geographical and cultural identities, data analysis methods, and authors' conclusions. Although not all the studies were qualitative, this tool was determined by the authors to be appropriate for data extraction from all studies. Many of the publications examined issues other than the challenges faced by nursing students on clinical placements in rural areas; however, for the purposes of analysis, only findings that answered the research question were extracted.

Figure 3: Qualitative Data Extraction Tool. Reproduced with permission14.
Data analysis
Results were compiled in tabular format using the aforementioned headings to facilitate analysis; findings were then examined and grouped under broad headings according to similarities. Then, challenges faced by students in rural settings were grouped according to the theoretical lens of the Ecological Model. The challenges that students may face were identified at seven levels: political, environmental, community, nursing, educational, relational, and personal. These categories as used for grouping the challenges emerged out of analysis of the findings and the model in general. They further enabled identification of challenges faced by nursing students engaged in rural clinical placements in several domains.
Extent and quality of literature
Thirteen studies were found: 8 qualitative studies, 2 quantitative studies, 2 reports on projects, and one program evaluation. The methods used for the 8 qualitative studies examined for this literature review included grounded theory3,16, ethnography2,17,18, and other qualitative methodologies9,19,20. Student challenges were described by students2,3,9,16-20, nurses9, clinical instructors9, and preceptors2,3. Data collection methods included semi-structured interviews, focus groups, field notes, journals entries, student essays, and document analysis. While, in general, the qualitative studies demonstrated methodological congruence, creditability, reflexivity, ethics, and auditability, 2 studies were unclear in their descriptions of research methods or limitations, leading to limited congruency and lower quality scores (Table 2).
Table 2: Quality assessment

The quantitative researchers used descriptive survey designs to examine the perceptions of 8 to 137 nursing students regarding their rural placements8,21. The 2 survey-based studies were determined to be of low and medium quality due to a lack of random sampling and limited or no discussion of reliability and validity (Table 2).
Two projects reports5,22 and one program evaluation6 were also included in the literature review. The reports focused on improving rural clinical placements5 and exposing students to rural experiences22, while presented an argument for financially supported clinical placements in rural areas for urban nursing students6. The quality of these articles was determined to be medium and high (Table 2); and while they included convincing and logical arguments, McDonough et al's22 report would have been strengthened had the findings been connected to existing literature.
Findings from the literature
In order to determine the challenges that nursing students from urban communities experience while on clinical placements in rural areas, the views of students and educators (including faculty and nurses) were examined. A total of 112 findings were extracted from the literature, analyzed, and grouped using the Ecological Model. As previously, the findings were grouped into the categories: political, environmental, community, nursing, organizational, relational, and personal. Within each category of the model, findings were synthesized and themes emerged.
Political: Students placed in rural areas often face challenges related to policies, influenced by governments and economics. In the literature, centralization of healthcare services and budget cuts were two areas students identified as challenging during their placements9. They also recognized that policy decisions often lead to decreased access in rural areas and that the limited funding affect the delivery of quality services in rural settings20. Students identified how policy decisions have led to the threat and realization of closures as well as reduction of emergency care and hospital services in rural areas9. Limited funding has also meant practical difficulties for students due to insufficient staff or materials20.
In one study, students indicated that nurses working in rural areas do not have voice in decision-making due to their isolation from administration20. This isolation limited input into funding as well as legislative and organizational decisions. As a result of this lack of voice, some issues that affect nurses at the bedside were not addressed.
Environmental: Students often contended with disincentives to rural practice including long driving distances and severe weather conditions3,9. Students in rural environments typically needed to travel further than their peers in urban settings to get to their clinical placements. In particular, northern areas in Canada are subject to longer winters, more freezing rain, and poorer road maintenance than other areas. In southern rural areas, weather conditions such as gusting winds and sudden storms (electrical, snow, and wind) may also result in unsafe driving conditions. Students from urban centres who must travel to rural areas may be unaware of important safety factors related to driving long distances or extreme weather conditions. These factors can affect the student's ability to get to clinical placements and cause considerable anxiety for the student. Client attendance at pre-arranged appointments and clinics was also reported to be affected by weather conditions and geography3.
Community: Transportation in rural areas was identified as an issue for the student nurse. Often there was a lack of transportation20 or elevated transportation costs5,6,9. Some rural communities did not have bus service, and those that did had limited hours of service. Additionally, in northern areas of Canada, the price of gas (petrol) is generally higher than in urban areas. These transportation variables affect not only the student nurse but also the client who may make treatment decisions based on inadequate services. This circumstance can be problematic for the student to witness19. For instance, the student may be troubled when a client cannot access treatment in the community and may not be able to afford to travel long distances to receive it.
For the students who lived in rural communities to complete placements, there was the reality of higher living expenses than elsewhere6,9. A student was required to pay for transportation, food, and accommodations, and, in the rural setting, these costs can be significant. Even finding suitable accommodation in a rural community was reported as difficult5,6,8,21.
Moving to a rural community for placement purposes can be a difficult transition for students because it requires them to learn about the community and its culture2. Students who have made this transition reported needing to spend significant time learning about rural nursing in order to practice effectively17. In a rural area where there is a large Aboriginal population, this learning curve can be particularly steep19. In the studies, students had to learn quickly to deal with the gossip and racism that can occur in rural settings16.
Due to the small nature of rural communities, students reported challenges related to privacy and confidentiality16,19,20. In the small communities cited in the studies, most people knew each other and their families well. The close-knit nature of rural communities can pique the curiosity of others and negatively impact a person's right to privacy. Moreover, the student nurse's private life can be scrutinized. Students commonly saw clients in public places such as the grocery store and bars16.
Nursing: Limited resources make rural placements challenging. As one example, students identified being isolated from other professionals and not having access to the same healthcare resources as in a larger centre. These resources included specialists, educational materials, and librarians3,9,16,20,21. In general, the services offered in rural communities were limited due to restrictions on service delivery9,20. Access to professional education was also reported as limited20. Students may need to travel long distances to attend conferences, workshops, and other continuing education sessions. Not only is this costly, it can also be problematic in that there may be no one available to replace the nurse during his or her absence. Some rural areas did not have access to the internet3. In such situations, continuing education and professional development opportunities supported by technologies such as learning management systems, web casting (live and archived), and web conferencing were inaccessible to the health professional. Furthermore, in some cases, even print resources and technologies were outdated or non-existent3,16.
A lack of human resources was reported as leading to short staffing and difficulty finding qualified clinical educators5,19. Students may be regarded to be part of the workforce and, therefore, asked or told to do things beyond their level of preparation and scope of practice. Alternately, this lack of human resources often meant that only essential work was completed, a situation that compromises nursing care19. It also caused students to feel that task completion takes priority over learning17. In short, due to time constraints and the unique demands of rural nursing, it can difficult for students to complete their work in a caring way17. Students also found themselves unable to write things down, evaluate, and reflect on practice16,17.
Students commented on the breadth and variety of caseloads and how challenging this was20. Patient numbers, workloads, and the types of clients needing care were noted as unpredictable in rural areas3. In addition, the small scale nature of rural hospitals meant that specialties were often combined19. The student nurse may discover more long-term care and palliative clients in acute areas than in other settings. This situation may be an outcome of limited accommodation in more appropriate places3. Moreover, in highly remote areas, nurses have a wider scope of practice than in urban settings. As an outcome, students may be asked to help diagnose and treat patients without appropriate educational preparation; students, in turn, expressed concern about the legal ramifications of practising beyond their perceived scope of practice. In some cases, the health professional and, by extension, the student nurse may be asked to treat animals if there is no veterinary service available in the community19.
Educational: Students expressed a need for more orientation, contact with, and support from faculty and administration than was provided3,16,18,21. This request emphasizes students' struggles with the unique and often demanding nature of rural practice. Due to geographical constraints, students in rural areas experienced isolation from faculty3,16,18. Additionally, communication between students in rural communities and their professors in the urban centres was often difficult. Students expressed concern that faculty cannot provide accurate feedback on clinical performance18. Since faculty were not in the actual setting to provide feedback, there was often a perceived disconnection between performance and grading.
Gum21 found that students were dissatisfied with both the quality and frequency of videotaped and audiotaped lectures which have been sometimes used as educational and communication supports for students in rural settings. In contrast, students on placement in urban areas tended to have access to more frequent and interactive lectures. The result of this was that students in rural areas were required to be more independent in their learning. Preparation for lectures requires that students learn more material at once and in single sessions because classes are generally held less frequently21.
A lack of financial assistance from the educational institution made rural placements challenging6,8,21. Students on placement in rural areas experienced financial burden because of elevated living costs. Some students had financial and employment obligations in urban areas, which made embarking on a rural placement especially burdensome8.
Relational: Students on placement in rural areas have described feeling isolated from peer and family supports3,20. McAllister et al. found that students were anxious about boredom in their social lives due to limited facilities and transportation difficulties. As a new person in the area, the student nurse may experience difficulty making friends. For a mature student, it can be difficult to maintain family responsibilities if the student's spouse or children remain in the urban setting8.
Sedgwick and Yonge2 report that, in general, students face challenges because of being new to the healthcare team. As newcomers, students are unfamiliar to the team as well as to clients. At times, clients in rural areas may not want to be cared for by a student nurse they do not know, and may ask to have the preceptor care for them3. Student participation in a rural area was also identified as being limiting because staff and clients were not accustomed to having students in the community19.
In a rural area, limited and small staffs were noted as disadvantages especially if the student does not work well with a particular nurse18. For example, not all nurses enjoy teaching18 and when this occurs in a rural setting a student may 'have to' work with this nurse because there is no one else. Complicating this, Armitage and McMaster19 found that staff in rural communities may be unfriendly to students.
It can also be difficult for students to maintain professional boundaries in rural areas. Because of the smallness of rural communities, staff members and others have been described as being interested in the personal lives of student on placement2. Also, in smaller communities, members of the town or village may be more inclined to be interested in the personal lives of others than in urban settings. In particular, newcomers may pique the interest of community members. This situation makes maintaining professionalism and personal relationships very difficult16.
Personal: Specific personal qualities and dispositions have been reported as helpful to students as they deal with the challenges of rural placements and as enablers of positive learning experiences. For example, in a number of studies it was reported that one needs to be prepared for increased autonomy and many and diverse responsibilities2,9,20. This means the students must demonstrate initiative, maturity, confidence, and independence as they provide care. A poor attitude, negative perceptions of the clinical venue, and a lack of enthusiasm, motivation, or initiative on placement are barriers to learning, especially in rural areas5.
Preparedness for the clinical placement is fundamental to a positive learning experience. One study indicated that it was difficult for students to know what knowledge and skills was required because they were unfamiliar with rural settings2. Similarly, students who were not adequately prepared tended to have negative experiences5. As well, students needed a broad range of knowledge, skills, and dispositions2,20; specifically, they needed to be motivated, self-directed learners and active consumers of available research. Such students continued their learning and generally acquired the skills and information they needed to provide safe care2.
Lessons learned
Given the urgent need to recruit and retain nurses in rural communities5-7, this review explored the challenges that nursing students from urban communities experience when they are on clinical placements in rural areas. The challenges were grouped into the 7 general categories: political, environmental, community, nursing, educational, relational, and personal. The diversity of these categories indicates that many and varied issues impact the clinical learning experience in the rural setting. At the political level, students are affected by decisions that centralize healthcare resources and lead to limited access in rural areas. Weather conditions and physical distance from the placement are environmental factors for which students may be unprepared. The community in which the placement occurs may pose financial, transportation, and accommodation challenges. Further, the student may experience cultural differences and increased difficulty maintaining personal privacy.
The nature of the nursing placement may also make it difficult to maintain professional boundaries. Students may be pressured to divulge confidential information or provide care beyond their scope of practice. Decreased access to specialists may further impact the learning experience. The literature also identifies insufficient educational preparation, isolation from faculty, and lack of financial assistance as barriers to positive learning experiences. Isolation from family and friends, being new to the setting, and conflicts with nurses in the setting may lead to possible relational challenges. Finally, specific personal dispositions and skills as well as preparation for the setting help the student deal with challenges that may arise.
It is important to recognize that challenges faced by students will vary dependent on the placement and available supports. For example, most northern areas in Canada are regarded to be rural23. Yet, being in a rural setting that is within driving distance of an urban area is an entirely different experience than being in a more remote rural community. Additionally, a student who has appropriate supports may have a positive experience regardless of the location.
Implications
The 7 groupings provide the framework for policy, education and practice implications. While these implications focus on students in rural placements, some will also be valuable for students in urban settings.
Policy implications: Students in rural areas are most certainly affected by government policy decisions which often result in decreased funding to rural areas and lead to reduced services9,20. While there is no easy solution to this situation, rural nurses and students are strongly encouraged to become politically involved and to advocate for increased funding to rural areas. Such funding will benefit not only the community but the student nurse. He or she will benefit because increased health resources are likely to lead to enhanced educational opportunities. Recruitment and retention of students when they have graduated may also be an outcome.
Opportunities for students to learn about policies in rural health as well as how to advocate for change are recommended for inclusion in nursing curricula. Because political advocacy is likely a new and unfamiliar experience for students, they require the leadership and support of their educators. Students and their nurse educators are thus encouraged to examine current policies and relevant research to identify the needs of nurses working in rural settings. Once these needs and related funding requirements have been identified, pursuit of diverse funding options such as support from professional bodies or other government sectors is recommended. Such efforts will benefit not only students but the entire rural community as well.
Implications for nursing education: Overall, the responsibility for preparation of student nurses resides with the educational institution. As reported in the literature, adequate preparation for clinical placements in rural areas is critical to positive learning experiences for students2,9,19. Policies of local nursing schools should be examined to ensure that students receive comprehensive orientation to both the clinical and community environments before they begin rural placements. When students are adequately prepared to face the challenges described in this review, rural nursing placements can provide rich and rewarding learning experiences9,19. Such orientation includes knowledge and skills in varied domains ranging from environmental conditions to community characteristics to the nursing setting to various relational and personal challenges.
As a practical example, prior to arriving in the rural clinical area, students require training for driving safely in extreme weather conditions, on poor roads, and in isolated areas. Teaching students what to do when driving in a snowstorm, on icy roads, or during deer season may decrease anxiety and potentially prevent car accidents. Students should also be made aware that they may have to travel longer distances to their placements than those in urban settings. With this knowledge, students will allot sufficient time for travel and be less inclined to speed or take chances.
Theoretical content addressing specific health and work-related issues of rural settings should also be incorporated within nursing programs. Some of these areas include how to safely work with limited resources as well as maintenance of confidentiality and professional boundaries. The benefits of rural placements should likewise be highlighted and this may encourage students to undertake rural clinical placements3,9,16. Learning about the culture and demographics of rural settings is also important. Strategies for dealing with potential challenges should be discussed prior to the placement.
Financial assistance in terms of scholarships or bursaries should be made available to students who travel to rural areas for clinical placements6,21. Ideally, schools should assist students in finding affordable accommodation and transportation options. Faculty and other staff are likewise encouraged to prepare students for the lack of resources they may experience in rural settings and to discuss the implications that policy and funding decisions have on rural areas. Students need to understand that their learning is important and be encouraged to seek every learning opportunity possible. Schools of nursing are encouraged to consult with distance education planners and instructional designers to discover ways to facilitate student learning on rural placement24,25. Educational experts may suggest strategies that faculty are unaware of, including those that involve technology-based communication. The availability of telehealth should also be explored because such technology can be used to provide health services as well as educational and administrative health supports across physical distance26. If telehealth is available in the rural community, it may help meet the educational and administrative needs of the student on placement.
Improved methods of communication between faculty and students are necessary to ensure that students feel supported despite the disincentives of distance and geography. Formal communication methods and times should be established with preceptors prior to the start of the clinical rotation3. While various communication technologies may be available, choosing and using a highly reliable modality such as telephone is recommended. On a related note, Gum21 advocates that course structures and designs may need to be examined to promote fairness and to ensure quality for students studying at a distance. Options such as teleconferencing and videoconferencing may be explored21,24. Schools of nursing should also ensure, as much as possible, that students have access to resources, including online databases, in order to conduct research for learning and clinical practice purposes.
Students also need to be prepared for dealing with interpersonal challenges in the rural setting2. If feasible, the student should meet the preceptor and view the clinical setting before placement in order to reduce anxiety; this experience also enables the student to plan appropriately2. Students may need assistance in learning how to deal with personal questions as well as difficult team members or clients. Furthermore, a discussion about options for entertainment and socialization will benefit the student and promote development of important connections and networks within the rural community20.
Students who want to study in a rural area should be screened to ensure they are appropriately prepared. This way, both the school and the student are aware of the student's level of readiness. This preparation is vital for ensuring that students practice safely in the clinical setting27. Sedgwick and Yonge2 recommend that students be required to prepare letters that indicate how rural placements support their learning objectives. These letters may also aid in assessing the student's readiness for dealing with the challenges of rural placements.
Nursing practice implications: Just as students in rural areas need supports, nurses in rural areas also require support. This way, they can better assist the students entrusted to them in clinical practice. Nurses likewise need to be supported by the school of nursing so that safe student learning is promoted and qualified instructors are retained27,28. In short, faculty from the educational institution should be accessible to educators as well as students. The presence of faculty in the rural placement enables the development of a professional relationship between the educator and student18. A strong relationship between the faculty and the nurse may also help the nurse value the experience.
As professionals, nurses working in the rural setting are encouraged to be kind and understanding so that students feel comfortable working with them19. Educator approachability is foundational in establishing a sense of shared responsibility for safety in the clinical setting27. As mentors for students, educators should promote mutuality, trust, and respect27. This relationship may be even more important in the rural setting than the urban setting as students are likely to experience new and different clinical challenges including a wider variety of patients and health needs than elsewhere.
Implications for research and limitations: The findings of this literature review are not generalizable due to the limited number of studies examined, as well as their different designs and settings. Also, the majority of studies are qualitative in nature, suggesting a need for future quantitative research with larger samples. Furthermore, the studies focused principally on Australia and Western Canada. Research in other rural areas including northern settings is recommended.
Other limitations in the review work may be attributed to the design and quality of the assessment tools. The interpretive nature of the review process also involves some subjectivity. Therefore, the quality scores may vary slightly dependent on the reviewer's perspective. Likewise, the reviewers' judgement skills played a role in the selection of the literature. In some instances, the primary purpose of the considered study was either narrower or broader than the challenges that student nurses experience in rural settings. At the same time, there are a number of common themes reflected in the articles which will be valuable to schools of nursing and students themselves. While the specific issues experienced by students in rural areas are likely to vary dependent on the specific setting, certain issues appear to be common: limited resources, isolation, and financial difficulties.
A further limitation is that the reviewed literature explored a variety of topics, not only challenges faced by students. In some of the articles, the challenges of students were not the primary focus of the study. Therefore, it is possible that not all challenges have been identified. For example, the study by Dalton17 examined how students experienced time in a rural placement. Hence, in this article, only challenges relating to time were described. There is a need for further research in order to complete the picture of what challenges nursing students face while they are on rural placements.
There is some literature that examines challenges in what are called 'innovative placements', examples of which include parishes, international settings, Aboriginal communities, corrections facilities, and community support groups29,30. This literature was not included in the review because it does not focus exclusively on the rural area. Additionally, challenges specific to rural placements are difficult to identify within these studies. However, because there may be relevant insights in this literature, their in-depth study may identify other challenges for students in rural settings.
Conclusion
Improving the quality of rural placements for nursing students is an ongoing and time-consuming process. However, through this and similar reviews of specific challenges, schools of nursing can take important steps towards facilitating positive rural learning experiences. This review has highlighted many challenges, as well as the importance of adequate preparation of students for rural nursing. The findings from the present review can be used as a starting point for evidence-based practice projects aimed at supporting urban students on placement in urban settings. Additionally, as changes are made to educational models, policies, and practices regarding rural nursing placements, evaluation and research are natural next steps. Ideally, these efforts will result in increased recruitment of nurses into rural areas where they are critically needed.
References
1. Bushy A, Leipert BD. Factors that influence students in choosing rural nursing practice: a pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: http://www.rrh.org.au (Accessed 21 July 2010).
2. Sedgwick MG, Yonge O. Undergraduate nursing students' preparedness to 'go rural'. Nurse Education Today 2008; 28(5): 620-626.
3. Yonge O, Ferguson L, Myrick F. Preceptorship placements in western rural Canadian settings: perceptions of nursing students and preceptors. Online Journal of Rural Nursing & Health Care 2006; 6(2): 47-56.
4. Canadian Institute for Health Information. Supply and distribution of registered nurses in rural and small town Canada - 2000. Ottawa, ON: CIHI, 2002.
5. Barnett T, Cross M, Jacob E, Shahwan-Akl L, Welch A, Caldwell A et al. Building capacity for the clinical placement of nursing students. Collegian 2008; 15(2): 55-61.
6. Neill J, Taylor K. Undergraduate nursing students' clinical experiences in rural and remote areas: recruitment implications. Australian Journal of Rural Health 2002; 10(5): 239-243.
7. Montour A, Baumann A, Blythe J, Hunsberger M. The changing nature of nursing work in rural and small community hospitals. Rural and Remote Health 9: 1089. (Online) 2009. Available: http://www.rrh.org.au (Accessed 21 July 2010).
8. Smith S, Edwards H, Courtney M, Finlayson K. Factors influencing student nurses in their choice of a rural clinical placement site. Rural and Remote Health 1: 89. (Online) 2001. Available: http://www.rrh.org.au (Accessed 21 July 2010).
9. Van Hofwegen L, Kirkham S, Harwood C. The strength of rural nursing: implications for undergraduate nursing education. International Journal of Nursing Education Scholarship 2005; 2(1): 1-13.
10. Kok G, Gottlieb NH, Commers M, Smerecnik C. The ecological approach in health promotion programs: a decade later. American Journal of Health Promotion 2008; 22(6): 437-442.
11. Gregson J, Forester SB, Orr R, Jones L, Benedict J, Clarke B et al. System, environmental, and policy changes: Using the Social-Ecological Model as a framework for evaluating nutrition education and social marketing programs with low-income audiences. Journal of Nutrition Education 2001; 33(Suppl1): S4-S15.
12. Whittemore R, Knafl K. The integrative review: updated methodology. Journal of Advanced Nursing 2005; 52(5): 546-553.
13. Bushy A. Orientation to Nursing in the Rural Community. Thousand Oaks, CA: Sage, 2000.
14. Pearson A. Balancing the evidence: incorporating the synthesis of qualitative data into systematic reviews. Joanna Briggs Institute Reports 2004; 2(2): 45-64.
15. Pearson A, Porritt K, Doran D, Vincent L, Craig D, Tucker D, et al. A systematic review of evidence on the professional practice of the nurse and developing and sustaining a healthy work environment in healthcare. International Journal of Evidence-Based Healthcare 2006; 4(3): 221-261.
16. Yonge O. Preceptorship rural boundaries: student perspective. Online Journal of Rural Nursing & Health Care 2007; 7(1): 5-12.
17. Dalton LM. Time as a source of conflict: student nurse experiences of clinical practice in a rural setting. Rural and Remote Health 4: 256. (Online) 2004. Available: http://www.rrh.org.au (Accessed 21 July 2010).
18. Sedgwick M, Yonge O. Students' perception of faculty involvement in the rural hospital preceptorship experience. International Journal of Nursing Education Scholarship 2009; 6(1): 1-14.
19. Armitage S, McMaster R. Rural and remote mental health placements for nursing students. Australian Journal of Rural Health 2000; 8(3): 175-179.
20. McAllister L, McEwen E, Williams V, Frost N. Rural attachments for students in the health professions: are they worthwhile? Australian Journal of Rural Health 1998; 6(4): 194-201.
21. Gum LF. Studying nursing in a rural setting: are students adequately supported and prepared for rural practice? A pilot study. Rural and Remote Health 7: 628. (Online) 2007. Available: http://www.rrh.org.au (Accessed 21 July 2010).
22. McDonough J, Lambert VA, Billue JS. A rural nursing practicum: making it work. Nurse Educator 1992; 17(4): 30-34.
23. Statistics Canada. Definitions of 'rural'. Rural and small town Canada analysis bulletin, cat no. 21-006-XIE, 2001; 3(3): 1-17.
24. Carter L, Rukholm E, Kelloway L. Stroke education for nurses through a technology-enabled program. Journal of Neuroscience Nursing 2009; 41(6): 336-343.
25. Luke R, Solomon P, Baptiste S, Hall P, Orchard C, Rukholm E, et al. Online interprofessional health sciences education: from theory to practice. The Journal of Continuing Education in the Health Professions 2009; 29(3): 161-167.
26. Carter L, Hudyma S, Horrigan J. Investigating the educational needs of nurses in telepractice: A descriptive exploratory study. Canadian Journal of University Continuing Education 2010; 36(1): 1-20.
27. Killam LA. Exploring the Nature of Clinical Safety in Undergraduate Nursing Education: A Q methodology study. Master's thesis; Laurentian University, Sudbury, Ontario; 2010.
28. Hrobsky PE, Kersbergen AL. Preceptors' Perceptions of Clinical Performance Failure. Journal of Nursing Education 2002; 41(12): 550-553.
29. Harwood CH, Reimer-Kirkham S, Sawatzky R, Terblanche L, Van Hofwegen L. Innovation in community clinical placements: a Canadian survey. International Journal of Nursing Education Scholarship 2009; 6(1): 1-19.
30. Reimer-Kirkham S, Van Hofwegen L, Hoe Harwood C. Narratives of social justice: learning in innovative clinical settings. International Journal of Nursing Education Scholarship 2005; 2(1): 1-14.
Abstract
Context: Positive learning experiences for students on clinical placement in rural settings have the potential for supporting the recruitment of qualified nurses to these areas1. Recruitment of such nurses is a global concern because current shortages have resulted in decreased healthcare quality for rural residents. By understanding the challenges faced by nursing students unfamiliar with rural settings, educational and organizational strategies can be developed to promote positive learning experiences and so enhance recruitment.
Issue: A broad literature review was conducted to explore the question: 'What challenges do nursing students from urban communities experience while they are on clinical placements in rural areas, respecting that 'rural' is conceptualized differently by different stakeholders?' The review followed a 5 stage process: (1) identification of the problem and purpose of the review; (2) structured literature search; (3) data evaluation; (4) data analysis; and (5) presentation of findings. Thirteen studies were evaluated independently using tools from the Joanna Briggs Institute. The Ecological Model was the theoretical framework used for consideration of student challenges.
Lessons learned: This literature review revealed a paucity of studies that addressed the research question, with mostly Canadian and Australian studies meeting the inclusion criteria. Findings were organized according to Ecological Model levels and suggested that students face political, environmental, community-based, nursing-related, organizational, relational, and personal challenges on rural placement. Challenges vary according to the placement setting and available student supports. Policy, educational, and nursing practice recommendations include that students should be aware of the impact of limited resources in rural settings; that comprehensive orientation should be provided to clinical and community settings; and that an exploration of financial and distance education supports prior to the placement would be beneficial. Rural practice nurse educators also require support, and it is critical that they and those at the educational institution be receptive to student questions and learning needs.
Key words: Baccalaureate nursing education, Canada, continuing nursing education, distance education, nursing students, rural communities, student challenges, training support.
You might also be interested in:
2021 - Health system strengthening for vision care in The Gambia
2015 - Re-orienting a remote acute care model towards a primary health care approach: key enablers

