Introduction
The rising cost of health care is often a concern among individuals seeking care in the USA, with the healthcare inflation rate outpacing the growth in personal incomes since 20001. To compound the issue, the proportion paid by the individual has also grown as insurers shift to cost sharing mechanisms to reduce their expenses2,3. A higher out-of-pocket spending burden, as calculated by the ratio of out-of-pocket expenditures to total income, can be an indicator of underinsurance, and places an individual at risk for hardships such as deferring necessary medical care or the inability to pay debts due to their medical debt load4-12.
Previous studies have found that insurance coverage, sex, age, income, race/ethnicity, health status, and employment status all play a significant role in this increased burden6-12. Previous work has also indicated that individuals in rural areas are more likely to face a higher out-of-pocket spending burden than urban residents13,14, even after controlling for the listed factors. The reasons for this rural disparity may be due to the different characteristics of these rural counties themselves, and not patients' individual characteristics15,16.
In addition, these studies tend to rely on dichotomous rural definitions, based upon either the Metropolitan Statistical Area (MSA) designation of the county or the census bureau's definition of rural. Dichotomous rural definitions, while often utilized, are problematic for several reasons. Rural counties vary widely in population density, insurance rates, racial distributions, health resource availability and many other factors16 that affect healthcare utilization and, subsequently, spending. Therefore, if the aggregated and imprecise dichotomous rural definitions are used without additional county-level contextual factors included, inappropriate conclusions regarding rural areas may result.
Thus, this analysis had two goals. The first is to further define the out-of-pocket healthcare spending to total income ratio for rural residents by utilizing a more precise and multi-level definition of rurality. The second was to explore the impact of county-level factors that may contribute to the urban-rural differences, and may be affected by policy changes and interventions.
Methods
This analysis pooled 3 years of Medical Expenditure Panel Survey (MEPS) data (2003, 2004, and 2005). The MEPS data, which are drawn from a subsample of the National Health Interview Survey, provides nationally representative estimates of healthcare utilization and expenditures among non-institutionalized residents. Data is obtained by interviewing the subjects then selectively supplemented by querying involved healthcare providers. All analyses were weighted to account for the complex structure of the sampling frame. Analyses were performed at the household level, with the demographic characteristics of the reference person for each household attributed to the entire family, and utilized for categorization, estimation, and weighting.
The dependent variable for this analysis was the ratio of out-of-pocket healthcare expenditures to total household income, expressed as a percentage. Total out-of-pocket expenditures included all expenses related to the provision of health care, and was calculated by summing these expenses paid by each member of the household. Premiums were excluded from expenditures because of the manner in which they are expended; for a vast majority of individuals, these premiums are paid via payroll deduction (or as a deduction from Social Security). Also, the premium amount paid is not related to actual utilization, but is fixed. Thus, the inelasticity of the premium cost, combined with its dissociation from actual utilization of health care, led to the premium costs from out-of-pocket spending estimates being excluded from the present study. Household income was calculated by summing the income of all members of a household unit.
The main independent variable of interest was the rurality of the household's residence. This was defined according to the 2003 Urban Influence Codes (UIC), developed by United States Department of Agriculture17. Rurality was subdivided into 4 categories: (i) Urban (UIC Codes 1 & 2) included counties that have significant metropolitan areas; (ii) Micropolitan (UIC Codes 3, 5 & 8) included counties that had a town with 10 000 to 49 000 residents; (iii) Small Adjacent (UIC Codes 4, 6 & 7) included counties with a town of 2500 to 9999 residents; and (iv) Remote (UIC Codes 9, 10, 11 & 12) included counties with towns of less than 2000 residents. 'All Rural' was defined as the aggregate of Micropolitan, Small Adjacent, and Remote rural counties.
Additional independent variables of interest were chosen according to Anderson's Model of Health Services Use18. This model describes predisposing characteristics that interact with enabling characteristics and an individual's perceived need for healthcare services, which will determine if that individual seeks services. For this analysis, the predisposing characteristics were obtained from the head of household, and attributed to all members of the household. These included sex, race/ethnicity (White, African American, Hispanic, and Other), age group (19-44, 45-64, >65 years), and self-reported health status (very good/good/excellent vs fair/poor). The enabling characteristics include employment status (employed vs unemployed), insurance status and type (Private health maintenance organization (HMO), Private Non-HMO, Medicare, Medicaid, Uninsured, and Other), having a usual source of care, having prescription drug insurance coverage, and poverty level (expressed as a percent of the federal poverty level).
Because earlier works found a significant affect of living in a rural area (ie rural residents had a higher out-of-pocket to income ratio13,14, several county-level variables were included in an attempt to discover those factors contributing to rural differences. These variables included the number of hospital beds per county, expressed in quartiles; Health Professional Shortage Area (HPSA) designation (full county, partial county, or none); and the percent of the population employed in white collar occupations. Finally, a dichotomous indicator was included indicating if a member of the household had at least one inpatient visit during the year.
The initial analysis estimated the distribution of the sample's characteristics and county-level characteristics, by levels of rurality. Differences across rurality were tested using Wald χ2 tests. Subsequent analyses estimated the median household income, out-of-pocket spending, and ratio by the levels of rurality and selected characteristics. These differences were tested using Wilcoxon rank-sum tests for independence, while pair-wise comparisons were tested using Tukey's adjustment.
The multivariate ordinary least squares regression analysis used the ratio variable as the dependent variable, with rurality as the main independent variable of interest. Because the ratio of out-of-pocket expenditures to income was not normally distributed, the dependent ratio variable was log-transformed for the modeling. The predisposing, enabling, and county-level variables were included in both models as the independent factors. The unadjusted and bivariate analyses utilized SAS-Callable SUDAAN (RTI International; Research Triangle Park, NC, USA), while the multivariate analyses utilized STATA-IC v10.0 (StataCorp LP; College Station, TX, USA).
Results
More than 83% of the households in this analysis lived in urban areas; of the almost 17% who lived in rural areas, a majority lived in Micropolitan rural areas (Table 1). The heads of household for the sample were predominately female, white, between 19 and 45 years, in good or better health, privately insured, had prescription drug coverage, were employed, and had incomes greater than 300% of the federal poverty level. When compared with urban, rural heads of household were more likely to be male, white, older, in poorer health, to have publically funded insurance, not to have prescription drug coverage, to have incomes less than 400% of poverty, unemployed, or to have an inpatient stay.
The distribution of the sample by county-level characteristics is shown (Table 1); all measures differed by levels of rurality. Notably, more rural households resided in counties with fewer hospital beds, with a higher percentage of white-collar occupations, or that were a partial HPSA.
The median household incomes, out-of-pocket spending, and ratio by selected characteristics of the head of each household are displayed (Table 2). Overall, income was higher among whites, those in good or better health, those with private non-HMO insurance, those with prescription drug insurance, and those with a usual source of care. Out-of-pocket spending was higher among whites, those in fair to poor health, those with Medicare, those with prescription drug insurance, and those with higher incomes. The ratios were higher for households whose head were white, in fair or poor health, had Medicare, lacked prescription drug coverage, or had lower incomes as a percent of poverty. In general, out-of-pocket spending was higher, as was the spending to income ratio, among those households with at least one inpatient visit.
Several differences were noted by levels of rurality. Overall, rural households had lower median household incomes, but not significantly different out-of-pocket spending or ratios than urban residents (Table 2). Differences did exist, however, when levels of rurality were considered; households in small adjacent and remote rural counties had lower incomes, and higher ratios, than urban households. Urban-rural differences for income, out-of-pocket spending, and the ratios also existed across race/ethnicity, health status, insurance type, poverty levels, usual source of care, and utilization.
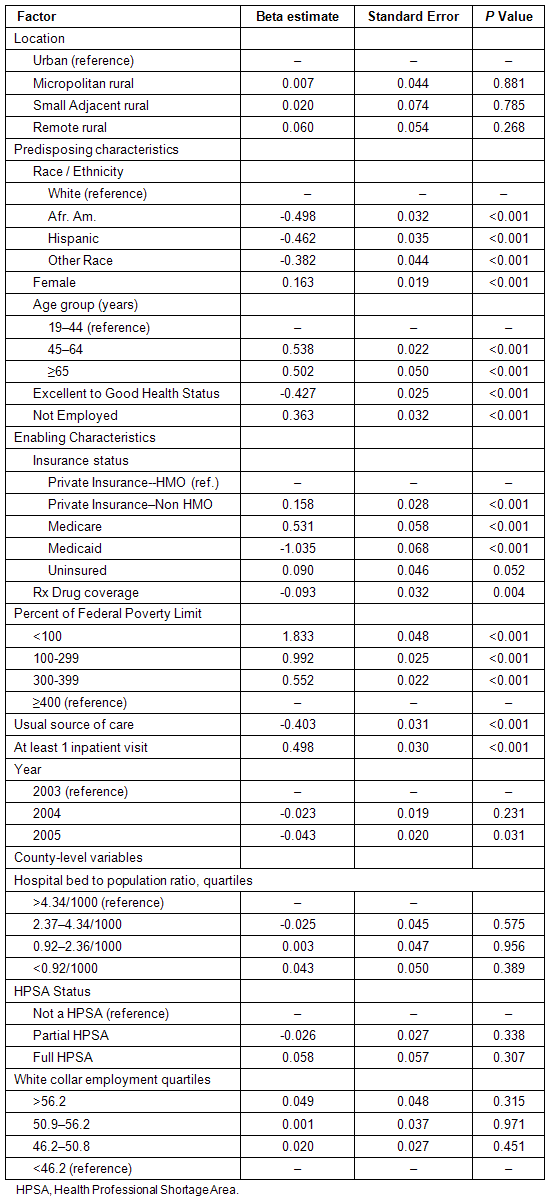
The multivariate results identified the factors significantly associated with the out-of-pocket spending to total income ratio. In this adjusted analysis, households who lived in rural counties, regardless of type, were not more likely to have a higher out-of-pocket to total income ratio than any other household. Factors associated with a lower ratio included non-White race, being in excellent to good health, having Medicaid, having prescription drug insurance, and having a usual source of care. Factors associated with a higher ratio included older age, not being employed, not having a private HMO insurance plan, being below 400% of the federal poverty limit, and having at least one inpatient visit in the year. None of the county-level variables, however, were significant (Table 3).
Table 1: Characteristics of the head of household, by county type
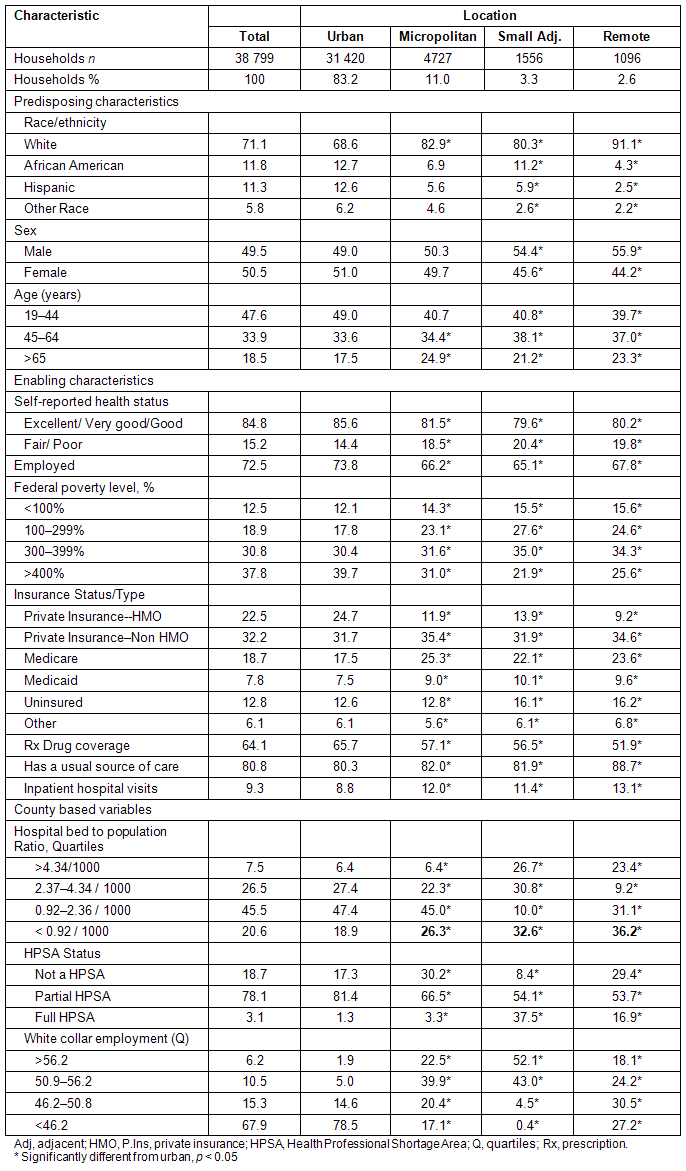
Table 2: Mean household income, mean out-of-pocket expenditures, and mean ratio, by rurality and selected characteristics
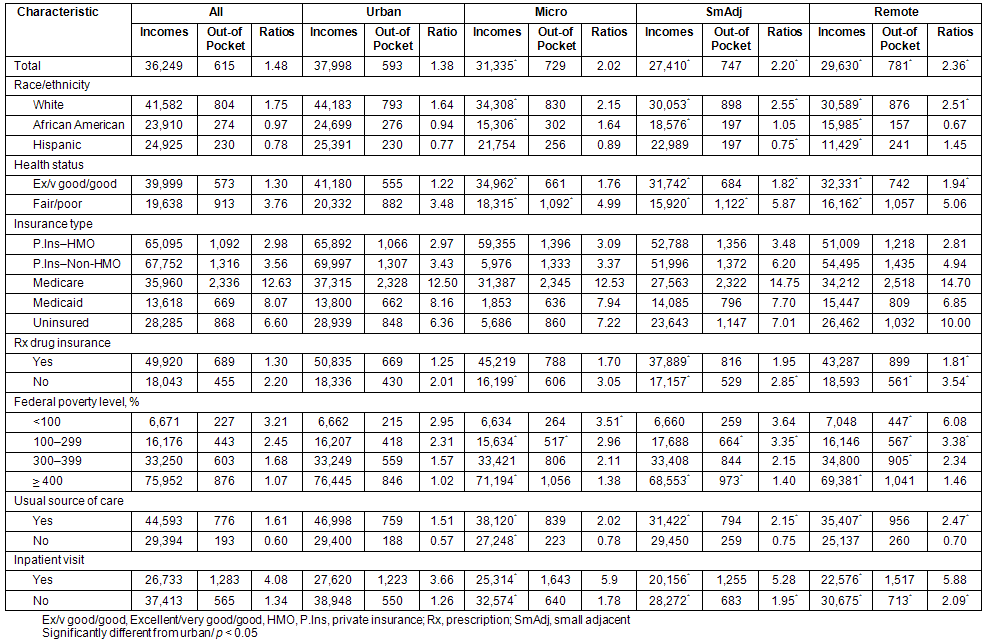
Table 3: Estimates of factors associated with the out-of-pocket healthcare spending to total household income ratio (r2 = 0.3027)
Discussion
This analysis sought to further examine the higher out-of-pocket to total income ratios previously documented among rural residents13,14. While a higher ratio was found among small adjacent and remote rural residents, this difference did not persist when other factors were accounted for in the multivariate models. Notably, demographic characteristics including race/ethnicity and age, health status, healthcare utilization, and insurance type, and not the rural location in and of itself, were found to be associated with the spending ratio.
The type of insurance coverage was a significant factor, in both the unadjusted and adjusted analyses. The unadjusted analysis estimated large ratios among those with Medicare and Medicaid, with private HMO plans having the lowest. After holding other factors equal, however, patients with Medicaid had ratios that were lower than those with Private HMO type plans. All other insurance types were more likely to have higher ratios, indicating the protective effect of managed care on out-of-pocket spending. It is also worth noting that uninsured individuals were slightly more likely to have higher ratios, despite their low out-of-pocket spending levels. Uninsured households' out-of-pocket spending was only 16% that of insured households (Table 2), in large part due to the dramatically lower rates of utilization (data not shown). Thus, these data suggest that the uninsured lowered their burden (as measured by the ratio) by reducing their utilization and subsequent out-of-pocket spending.
The unadjusted analysis found that those who had a usual source of care had significantly higher ratios; not surprisingly, a usual source of care is also strongly associated with a higher number of office-based visits and inpatient hospital visits (data not shown), which can increase out-of-pocket costs. However, those with a usual source of care were also more likely to be in poorer health, which was a significant contributor in the final model. Thus, after controlling for health status and actual utilization, having a usual source of care was associated with lower ratios, indicating a protective effect of provider continuity and care coordination.
It was surprising that none of the county-level variables were found to be significant contributors to the spending ratio. The fact that rurality of the county was not significant, despite other studies showing a significant effect13,14, may be due to two factors. First, we utilized county-level variables in the analysis to try to account for the county-level effects that would contribute to the ratio. We had hypothesized that counties with more hospital beds would have higher spending due to more inpatient visits; HPSA-designated counties would have lower spending due to lower utilization; and that counties with higher white collar employment rates would have lower spending due to more generous healthcare benefits (ie lower out-of-pocket sharing). The fact that these hypotheses were not upheld indicates that the other factors, such as actual utilization and insurance type are more important than these county-level variables. Secondly, the log-transformed dependent variable, which was not utilized in previous works, may account for the difference in the outcomes.
These results indicate potential interventions that may alleviate increased financial burdens. Lower out-of-pocket payments, and thus lower ratios, may be achieved by reducing utilization (either office based visits or inpatient visits), particularly if that utilization is unnecessary (such as non-acute visits to the emergency department). These types of visits are common when primary care providers are not available, as is the case in HPSA areas. Additional program implementations, particularly in underserved areas, may entail the using of electronic visits (such as email disease and medication management), the use of telephone communications, or even the more extensive telemedicine programs that are being tested throughout the country. These programs may be useful in reducing the out-of-pocket payment burden for patients as well as extending existing providers (such as physicians, physician extenders, advanced practice nurses, and pharmacists) to better care for their patient population19-21.
The recent passage of the US Patient Protection and Affordable Care Act (2010) will put many of these concepts to the test. Provisions within this act will effective lower out-of-pocket healthcare spending for some groups, either through reduce copayments, deductibles, or increased spending caps. Also, by encouraging uptake of insurance via mandates, Medicaid expansion, and increased coverage options individuals who previously did not have insurance will begin to carry coverage, effectively reducing their out-of-pocket spending burden at the point of care. It remains to be seen, however, how effective this legislation will be on spending ratios.
This analysis was limited by several factors. First, the characteristics of the head of household were applied to the entire household, which may be inappropriate if the members of the household are not similar demographically to the head. In a homogenous demography, this assumption would not be problematic; however, in the current society, households of mixed race/ethnicity, educational levels, employment statuses, and ages are not uncommon. In addition, it was decided not to include premium expenses in the calculations. It is possible that these premium costs would affect healthcare seeking behavior; however, their exclusion assumes an indirect relationship that is mirrored in previous studies13,14. Premium costs may serve as a proxy for the generosity of the healthcare plan itself, because plans with higher premiums may have lower out-of-pocket responsibilities. Thus, it would be ideal to include other variables related to the insurance market, type and generosity of benefits, out-of-pocket responsibilities, and managed care penetration of the area.
Despite these limitations, this analysis found that living in a rural area, in and of itself, was not associated with a higher healthcare spending burden, as measured by the ratio of out-of-pocket healthcare expenditures to total income. Rather, other factors such as income, health status, insurance type, provider availability and continuity, and service utilization were strongly associated with the ratio, explaining the lack of adjusted urban/rural differences.
References
1. Bureau of Economic Analysis, US. Department of Commerce. Personal income and its disposition. (Online) 2009: Available: http://www.bea.gov/national/nipaweb/SelectTable.asp?Selected=N (Accessed 1 April 2009).
2. Catlin A, Cowan C, Heffler S, Washington B. National Health spending in 2005: the slowdown continues. Health Affairs 2007; 26(1): 142-153.
3. Claxton G, Gabel J, Gil I, Pickreign J, Whitmore H, Finder B et al. Health benefits in 2006: premium increases moderate, enrollment in consumer-directed health plans remains modest. Health Affairs 2006; 25: w476-w485
4. Goldman DP, Joyce GF, Escarce JJ, Pace J, Solomon M, Laouri M et al. Pharmacy benefits and the use of drugs by the chronically ill. JAMA 2004; 291(19): 2344-2350.
5. Wright BJ, Carlson MJ, Edlund T, DeVoe J, Gallia C, Smith J et al. The impact of increased cost sharing on medicaid enrollees. Health Affairs 2005; 24(4): 1106-1116.
6. Banthin JS, Bernard DM. Changes in financial burdens for health care: national estimates for the population younger than 65 years, 1996 to 2003. JAMA 2006; 296(22): 2712-2719
7. Banthin JS, Cunningham P, Bernard DM. Financial burden of care, 2001-2004. Health Affairs 2008; 27(1): 188-195.
8. Blewett LA, Ward A, Beebe TJ. how much health insurance is enough? Revisiting the concept of underinsurance. Medical Care Research and Review 2006; 63(6): 663-700.
9. Bodenheimer T. Underinsurance in America. New England Journal of Medicine 1992; 327(4): 274-278.
10. Schoen C, Collins SR, Kriss JL, Doty M. How many are underinsured? Trends among U.S. adults, 2003 and 2007. Health Affairs 2008; 27(4): w298-309.
11. Shen Y-C, McFeeters J. Out-of-pocket health spending between low- and higher-income populations. Medical Care 2006; 44(3): 200-209.
12. Short PF, Banthin JS. New estimates of the underinsured younger than 65 years. JAMA 1995; 274(16): 1302-1306.
13. Bennett K, Powell M, Probst J. Relative financial burden of health care expenditures. Social Work in Public Health 2010; 25: 6-16.
14. Bennett K, Dismuke C. Families at financial risk due to high ratio of out-of-pocket health care expenditures to total income. Journal of Health Care for the Poor and Underserved 2010; 21(10): 691-703.
15. Hart LG, Larson EH, Lishner DM. Rural definitions for health policy and research. American Journal of Public Health 2005; 95(7): 1149-1155.
16. Probst J, Moore C, Glover S, Samuels M. Person and place: the compounding effect of race/ethnicity and rurality on health. American Journal of Public Health 2004; 94(10): 1695-1703.
17. Economic Research Service. Urban influence codes. US Department of Agriculture. (Online) 0000. Available: http://www.ers.usda.gov/Briefing/Rurality/NewDefinitions/. Accessed 06/28/2008 (Accessed 28 June 2008).
18. Anderson RM. Revisiting the behavioral model and access to medical care: does it matter? Journal of Health and Social Behavior 1995; 36(1): 1-10.
19. Green BB, Cook AJ, Ralston JD, Fishman P, Catz S, Carlson J et al. Effectiveness of home blood pressure monitoring, web communication, and pharmacist care on hypertension control: a randomized controlled trial. JAMA 2008; 299(24): 2857-2867.
20. Ragucci K, Fermo J, Wessell A, Chumney E. Effectiveness of pharmacist-administered diabetes mellitus education and management services. Pharmacotherapy 2005; 25(12): 1809-1816.
21. Shea S, Weinstock RS, Teresi JA, Palmas W, Starren J, Cimino J et al. A randomized trial comparing telemedicine case management with usual care in older, ethnically diverse, medically underserved patients with diabetes mellitus: 5 year results of the IDEATel Study. Journal of the American Medical Informatics Association 2009; 16(4): 446-456.
Abstract
Introduction: This analysis sought to define the out-of-pocket healthcare spending to total income ratio for rural residents, as well as to explore the impact of county-level factors that may contribute to urban-rural differences.
Methods: Three years of pooled data were utilized from the Medical Expenditure Panel Survey (2003-2005). The dependent variable was the ratio of total out-of-pocket healthcare spending to total income, at the household level. Unadjusted and adjusted analyses estimated the factors associated with this ratio, including rurality, socio-demographics, and county-level factors.
Results: The unadjusted analysis indicated that small adjacent and remote rural residents had higher out-of-pocket to total income ratios than urban residents. The adjusted multivariate analysis indicated that when other factors are held equal, rurality is no longer a significant factor. Other factors such as insurance type, healthcare utilization, and income, which differ significantly by rurality, are better predictors of the ratio.
Conclusions: The identification of factors that contribute to a higher ratio among some rural residents is necessary in order to better target interventions that will reduce this financial burden.
Key words: household income, out-of-pocket expenditures, USA.
You might also be interested in:
2014 - Rural Nursing: Concepts, Theory and Practice, 4th edn

