Governments in developing countries, including Nigeria, have difficulty funding health care due to budget constraints, population size and competing demands for public expenditure1,2. Since independence, Sub-Saharan African countries have introduced a number of methods to fund health care. An initial goal to provide 'free health care for all' has never been achieved due to low and unstable tax revenue and subsequent reduction in public budgets3.
The economy of Nigeria is based on oil drilled from the Niger Delta region. Years of oil exploration activities with frequent oil spillage have led to severe environmental degradation resulting in the destruction of farmlands, and aquatic flora and fauna. The adverse effects of this on local people's fishing and farming occupations have led to poverty and its associated problems. Consequently the 'oil boom' has become 'oil doom', and today life in the rural Niger delta is one of hunger, poverty and injustice4.
With the high level of poverty in these rural areas, individuals who are ill rely on herbal remedies and/or self-medication with orthodox drugs. Where self-treatment is unsuccessful, patients are compelled to seek and pay for expensive outpatient services from traditional healers, private practitioners and pharmacists5,6. This can result in a large health expenditure among families seeking treatment for seriously ill relatives7. There have been reports of indigent patients presenting to some hospitals but being turned away without treatment, or being detained after treatment by hospital authorities because they could not pay their hospital bill8. Although direct payment for out-of-pocket expenses is most common, this has been heavily criticized for its impact on health inequity and access, healthcare uptake or utilization, and the cost-effectiveness of the healthcare system3.
To improve healthcare funding, the Nigerian government commenced implementation of a social health insurance scheme (National Health Insurance Scheme; NHIS) in 1999. In contrast to user fees, the NHIS encompasses risk-sharing in an attempt to reduce unforeseeable or unaffordable healthcare costs to calculable, regularly paid premiums. Despite the NHIS advantages, most people in Nigeria continue to rely on direct payments to finance their healthcare needs because only a small segment of the population is covered by the scheme (mainly federal government public servants in urban areas)9. The informal sector and those in rural areas (approximately 50% of the population), where 80% live below the poverty line, are not covered10. Unfortunately, high burden of disease is found in this population, and 11% to 15% is surgical11.
Existing government hospitals in these rural areas are poorly equipped and sparsely staffed with qualified personnel. Profit-oriented private clinics collect fees at the point of service in the form of out-of-pocket payment, as a cost-recovery strategy. In response to these persistent issues in the cost of health care, non-profit, voluntary insurance schemes for urban and rural self-employed and informal-sector workers have recently emerged12.
In Bethesda Clinic, Ngo, a rural Niger Delta community in South-South Nigeria, length of hospital stay is usually beyond the expected 7 days among surgical patients because of their inability to pay treatment bills. This extended stay impacts adversely on the hospital's economic management due to bed shortages. Little is known about the source of payment when patients manage to pay out of pocket. More than a decade ago, Akande et al's descriptive survey of healthcare financing among in-patients (excluding women from the maternity section) in a tertiary health facility in Ilorin, North Central Nigeria, reported the health care was financed by relatives (46.6%), loans (29.8%), savings (13.1%) and the sale of property (2.1%)6. No similar study appears to have been conducted in the South-South geographic zone of Nigeria.
The aim of the present study was to determine the socio-demographic characteristics of these surgical patients, the pattern of hospital bills and sources of finance for payment, in order to determine ways to reduce this financial burden.
Permission was obtained from the Management Committee of Bethesda Clinic, Ngo Andoni, Rivers State, Nigeria before the study commenced. Ethical clearance was obtained from the Ethical Committee of the University of Port Harcourt Teaching Hospital. A detailed explanation of the importance of the research was provided to subjects eligible for the study, and verbal approval and written consent was obtained before their inclusion in the study. Confidentiality was assured by restricting access to the data collected, and by using these data only for the agreed scientific purpose.
This cross-sectional study spanned 5 years (2004-2009) at Bethesda Clinic, located in Ngo, a rural Niger Delta town that lacks basic amenities such as electricity, pipe-borne water and well equipped health facilities. The clinic had a full staff of efficient primary-care medical team. The service was general-practice, primary-care oriented, and therefore a wide range of patients (surgical, medical, gynecological and pediatric) were seen. Ngo town had a population of approximately 10 000 people whose major occupation was fishing.
Data were collected by the consultant family physician who administered a questionnaire to each recruited patient immediately after discharge and settlement of their bill. Information were sought on their: biodata, estimated monthly income, type of surgical procedures, duration of hospital stay, total hospital bill, source/s of funds used for payment of the hospital bill, and knowledge of the health insurance scheme. Participants' hospital records were also reviewed to confirm length of stay, total bill paid, type of surgical procedure and any complications. Patients with surgical complications such as wound infections and co-morbidities that caused them to stay longer than 7 days were excluded from the study. Also excluded were those who did not consent to participate.
A pre-test study resulted in some corrections to the initial questionnaire for ease of administration and extraction of adequate information. A pilot review of patients' record data was also performed to reduce variations in patient-level data collection.
The data obtained were entered into a personal microcomputer and analyzed using SPSS v.14 (www.spss.com) to produce frequency tables, percentages, χ2 and relative risk. Continuity correction was applied where necessary.
A total of 3712 patients were seen in the clinic during the study period. Of 245 surgical patients (6.6%), 229 consented to participate in the study, comprising 166 males and 63 females (ratio 2.6:1). Their ages ranged from 4 to 97 years (mean 45.6±13.5). Most of the patients (72.93%) were between 21 and 60 years. A high percentage of the women (80.95%) stayed more than 7 days following admission to the clinic. The occupation of most of the participants (79.91%) was fish farmer, a high percentage (56.33%) had secondary education and most were of the Christian religion (86.03%). The association between duration of stay with age, sex, educational level and religion was statistically significant (p<0.05; Table 1).
The most common surgical procedure performed was herniorrhaphy; however, the longest staying patients were those who had an ectopic pregnancy (23.32±7.52 days), caesarean section (19.51±6.73 days), appendectomy (18.46±6.82 days) and exploratory laparotomy (17.33±8.32 days). The association of duration of admission with type of surgery was statistically significant (p=0.004; Table 2). A large percentage (56.25%) of the emergency patients and 20.54% of the non-emergency patients stayed more than 7 days in the clinic. The association of duration of admission with emergency status was statistically significant (p<0.05; Table 3).
Participants' hospital bills ranged from US$33.3 to $500 with a mean of $105.7±0.043 (exchange rate: US$1 = 150.0 Naira). The association between hospital bill and duration of stay was not statistically significant (p>0.05; Table 4). The sources of financing hospital bills were multiple but most frequently personal savings (71.18%; Table 5). Only very few (3.06%) had knowledge of the NHIS (Fig1), but when educated about its benefits 84.28% were willing to enroll if it was introduced (Fig2).
Table 1: Socio-demographic characteristics and duration of admission of the patients
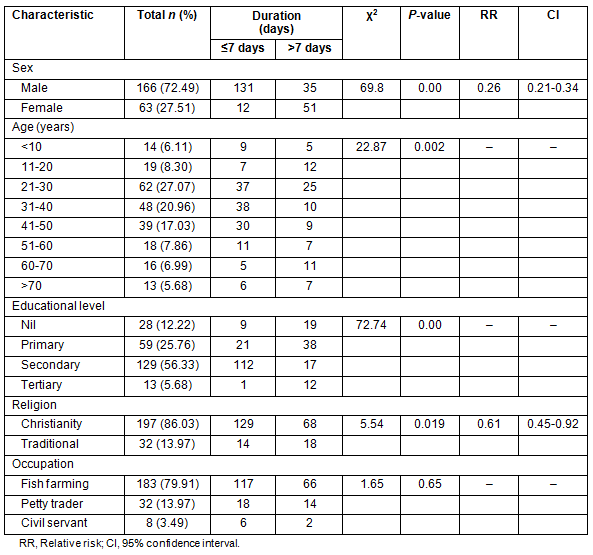
Table 2: Types of surgery and duration of admission
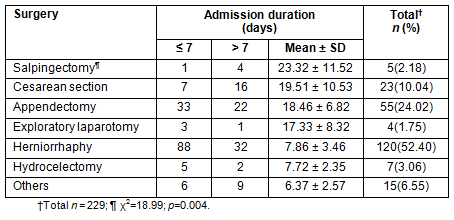
Table 3: Emergencies, non-emergencies and duration of admission
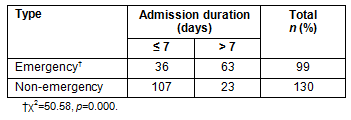
Table 4: Distribution of hospital bills by duration of stay on admission
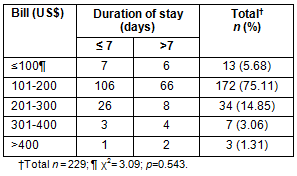
Table 5: Sources of payment for hospital bills
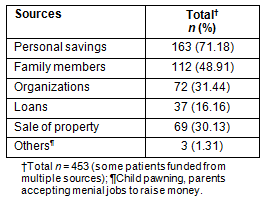
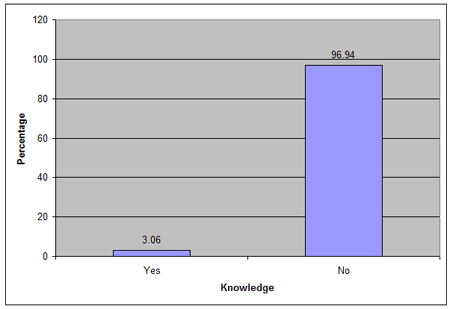
Figure 1: Knowledge of National Health Insurance Scheme.
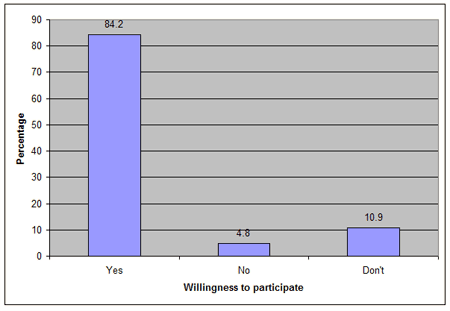
Figure 2: Willingness to participate in National Health Insurance Scheme (NHIS).
Discussion
The findings in this study suggest that sociodemographic characteristics are significantly associated with long stay following hospital admission while, surprisingly, the size of the hospital bill is not. The most common source for paying hospital bills was participants' savings.
The greater proportion of males in the study population may have affected the indentified disease pattern, for example more than 50% underwent herniorrhaphy, a more common procedure among males13,14. This could be related to the large fish farmer occupation group in the sample, whose canoe paddling, and casting and pulling of nets would increase intra-abdominal pressure and predispose to abdominal hernia14. Their shorter duration of stay may have been because most were non-emergency cases, allowing them opportunity to prepare financially for their surgery.
Some common health issues among women in the developing world that may have affected the results were detected in the current sample. There is a general non-acceptability of non-vaginal delivery for cultural reasons15,16, making such women liable to abandonment in hospital. In addition, few of the women had paid employment, so family economic power rested with already impoverished men17,18 who may have been unwilling to pay for women's healthcare bills. The clinical implication of this is grave. If sick women are unable to go to hospital, this will increase their morbidity and mortality. This finding underscores the importance of financial empowerment of women - in this case, to improve their health status.
The high population of participants in the 21-50 years age bracket and a low elderly study population may have been due to the low life expectancy (47 years) in the Niger Delta environment19.
Participants' low level of education excludes them from well paid jobs and explains their dependence on fishing as an occupation. A high level of poverty was therefore the norm and attributable to the environmental degradation caused by oil exploration. This has negatively impacted on the fishing industry, and so their inability to pay hospital bills was not unexpected.
The financing of hospital bills from personal savings is at odds with the findings of Akande et al6 that family members paid most of the bills. Cultural differences between the two study populations could have accounted for this disparity. In addition, Akande et al studied all in-patients, compared with only surgical patients in the present study, with a likely difference being that non-emergency surgical patients can make financial preparation for a planned hospital admission.
It is important to understand that payment from personal savings may be at the expense of competing family demands, such as money for education, food, shelter and clothing. Thus a payment from savings may have serious financial consequences for a household. Even among those who paid from their savings in the present study, some still depended on family members and other sources of finance to make the complete bill payment. In this study environment, relatives are often involved when patients cannot pay their bills, for a prolonged stay in hospital is seen as an embarrassment to family members. This is one advantage of the typical African extended family structure in which considerable sacrifices in terms of consumption and investment may be made to satisfy the health needs of a family member6.
Religious organizations are the most likely local organizations to assist in the payment of hospital bills and this increases the bond between members. Selling properties and securing of loans to pay a hospital bill was a common finding, and a source of economic stress in the family. These call for alternative sources of healthcare financing to be made available to those in need.
Hospital stay was more prolonged among emergency surgical patients with conditions such as salpingectomy for an ectopic gestation, cesarean section for obstructed labor and appendectomy for appendicitis. Difficulty in mobilizing funds to settle subsequent hospital bills in this group of patients may be aggravated by lack of financial preparation because those with low incomes often rely on their own labor productivity to generate income, and this is affected in the event of illness20.
The 96.94% of patients in this study who had no knowledge of health insurance is in agreement with a report by Sekhri et al21, and could be attributed to the low level of education among the study population. Although 84.28% of the patients were willing to participate in an insurance scheme, their willingness to pay monthly premiums cannot be guaranteed because it is affected by factors such as socioeconomic status (income), gender, education and place of residence9. For health insurance to be successful in this locality, the government must commence an intensive education campaign and also address factors that influence willingness to pay.
A limitation of this study is that the interpretation of results cannot be extrapolated to the whole country because only those in the Niger delta were studied. It is therefore recommended that similar studies be conducted in other locations in Nigeria.
Some questions warranting further research remain. Do the different seasons affect the ability of patients to pay their bills? Does the ability to pay a hospital bill depend on their income?
This study showed that the sources of payment for medical bills may be multiple but the most common were from personal savings and family members. Most of those who stayed beyond 7 days in hospital had undergone emergency surgical procedures. However, despite gaps in knowledge about NHIS due to poor education, many of those studied were willing to participate if such a scheme was introduced. There is a need to strengthen the educational system by empowering teachers, religious and community leaders with information about health insurance so that such knowledge can be passed on to school children and adults in the community. This will promote acceptance of health insurance schemes if these are introduced in rural areas.
References
1. Anyaehie UB, Nwobodo ED. Administrative responsibilities of community-funded health insurance scheme in Nigeria. Nigerian Medical Practitioner 2004; 45(3): 26-28.
2. Shaw PR, Griffin PC. Financing health care in sub-Saharan Africa through user fees and insurance. Washington, DC: World Bank, 1995; 13-30.
3. Wiesmann D, Jütting J. The emerging movement of community based health insurance in Sub-Saharan Africa: experiences and lessons learned. Afrika Spectrum 2000; 35(2): 193-210.
4. Udonwa NE, Ekpo M, Ekanem IA, Inem AV, Etokidem A. Oil boom and AIDS doom in the Niger Delta of Nigeria. Rural and Remote Health 4: 273. (Online) 2004. Available: www.rrh.org.au (Accessed 21 March 2011).
5. Inem AV, Fatayi-Williams AA, Ayankogbe OO. A short history of rural health service development in Nigeria. A tribute to Dr C Andrew Pearson. Nigerian Medical Practitioner 2003; 43: 90-95.
6. Akande TM, Ogunrinola EO. Health care financing among in-patients of a tertiary health facility in Ilorin, Nigeria. Nigerian Journal of Clinical Practice 2000; 2(1): 1-4.
7. Russel S. Ability to pay for health care: concepts and evidence. Health Policy and Planning 1996; 11(3): 219-237.
8. Kippenberg J, Sahokwasama JB, Amon JJ. Detention of insolvent patients in Burundian hospitals. Health Policy and Planning 2008; 23(1): 14-23.
9. Onwujekwe O, Okereke E, Onoka C, Uzochukwu B, Kirigia J, Petu A. Willingness to pay for community-based health insurance in Nigeria: do economic status and place of residence matter? Health Policy and Planning 2009; 25(2): 155-161.
10. International Fund for Agricultural Development. Rural poverty in Nigeria. (Online) 2009. Available: www.ruralpovertyportal.org/web/guest/country/home/tags/nigeria (Accessed 16 December 2009).
11. Debas H, Gosselin R, McCord C, Thuid A. Surgery. In: D Jamison (Ed.). Disease control priorities in developing countries, 2nd edn. New York: Oxford University Press, 2006; 1245-1260.
12. Jütting J. Social security systems in low income countries: concepts, constraints and the need for cooperation. International Social Security Review 2000; 4: 3-25.
13. Schumpelick V, Treutner KH, Arit G. Inguinal hernia repair in adults. Lancet 1994; 344: 375-379.
14. Dienye PO, Akani AB, Gbeneol PK, Jebbin NJ. Anterior abdominal wall hernias in a rural practice in Rivers State, Nigeria. Port Harcourt Medical Journal 2009; 4(1): 29-34.
15. Olusanya BO, Solanke OA. Maternal and neonatal factors associated with mode of delivery under a universal newborn hearing screening programme in Lagos, Nigeria BMC Pregnancy and Childbirth 2009, 9: 41.
16. Onah HE, Ikeako LC, Iloabachie GC: Factors associated with the use of maternity services in Enugu, South Eastern Nigeria. Social Science and Medicine 2006; 63: 1870-1878.
17. Izugbara CO Ngilangwa DP. Women, poverty and adverse maternal outcomes in Nairobi, Kenya. BMC Women's Health 2010; 10: 33.
18. Centers for Disease Control and Prevention. HIV transmission among Black Women - North Carolina, 2004. Morbidity & Mortality Weekly Report 2005; 54(4): 89-94.
19. Mathers CD, Iburg KM, Salomon JA, Tandon A, Chatterji S, Ustun B et al. Global patterns of healthy life expectancy in the year 2002. BMC Public Health 2004; 4: 66.
20. Creese A, Bennett S. Rural risk-sharing strategies. In: G Schieber (Ed); Proceedings, Innovations in health care financing; World Bank Conference; 10-11 March 1997; Washington, DC; 1997.
21. Sekhri N, Savedoff W. Private health insurance: implications for developing countries. Bulletin of the World Health Organization 2005; 83: 127-138.


