The June 2010 report Using locum doctors in hospitals1 from Audit Scotland (the body that provides the Auditor General and the Accounts Commission with the services they need to check that public money is spent properly, efficiently and effectively) highlights the NHS spending on locums and suggests that £6 million per year could be saved by reducing locum tenens usage to the national average. It also reports that the demand for locums has increased but the ability of locum agencies to meet requests has fallen. The report draws attention to the potential risks to patient safety of employing locums, indicating it is individual NHS Board's responsibility to ensure that risks are minimised. Data for all NHS Boards, including NHS Western Isles, were analysed and comment made about specific aspects of locum usage. In particular, for NHS Western Isles attention was drawn to the fact that 36% of the medical staffing budget is spent on locums, rural and island NHS Boards have difficulty recruiting, and that 97% of the locum expenditure was on consultant locums.
Other than the Audit Scotland report, the importance of locum consultants to the rural general hospitals has received little attention in Scotland. Recent reports relevant to rural health care in Scotland on the medical workforce2, NHS Scotland service change3 and remote and rural healthcare4 have made no mention of locum consultants. A statement suggesting that all locum consultants must be required to be on the specialist register appears in the Scottish Executive Health Department publication Securing Future Practice: shaping the new medical workforce for Scotland5.
The Rural Access Action team report to the national framework for service change in the NHS in Scotland states6:
Because of its size and the number of staff it employs the rural general hospital is fragile and has difficulty coping with absences of its employees. It is often necessary to employ a locum to cover annual, study, sickness or special leave. This is particularly true when one or two people provide a particular service. With new employment contracts and an increasing need to abide by the working time legislation the need for locums will increase.
Unlike hospitals based in larger towns and cities the rural general hospital has only limited access to locally based locum services. The ever-increasing cost of employing locums from a distance can place a severe financial burden on a health board. Limited availability and variable quality makes acquiring locums time consuming and unpredictable.
The use of locum tenens to support the consultant or specialist service of rural hospitals is not unique to Scotland. A recent study from New Zealand reported that 28 rural hospitals identified serious/critical shortages of appropriately qualified doctors with 10% of vacant posts unfilled and 25% filled by locums7. In addressing the difficulties of recruiting surgeons to practice in rural America, Doty et al indicated that although using locum tenens surgeons may allow a rural hospital to provide a surgical service the quality of care could be compromised8.
This article describes the consultant (permanent and locum) workforce of the Western Isles Hospital in Stornoway, one of Scotland's 6 rural general hospitals, over the 8 year period from 2002 to 2009. The data show the magnitude of the locum issue and indicate it is a serious problem that requires substantially more consideration.
For most weeks from the beginning of January 2002 to the end of December 2009 the Human Resources Department of NHS Western Isles produced a list of locum consultants which was circulated widely throughout the organisation. Data were extracted from these lists and analysed. Using this technique it is believed that all locum consultants employed in the Western Isles Hospital during this period were identified.
Permanent consultants are defined as those who have been appointed to a substantive post; long-term consultant locums are in a post for longer than 3 months; and short-term consultant locums are in a post for less than 3 months. The differentiation between long-term and short-term based on a 3 month cut-off relates to the need to review appointments which extend beyond 3 months, and at 3 monthly intervals thereafter9.
During the 8 year study period 239 separate people were employed as a consultant in either a permanent or locum position in the Western Isles Hospital. The number of consultant days per year, for both permanent and locum consultants, varied between 5875 in 2004 and 6895 in 2008 (Fig1). The permanent consultant days varied between 4631 (2003) and 2682 (2006); long-term locum days from 602 (2003) to 3220 (2006) and short-term locum days from 703 (2009) to 1214 (2004).
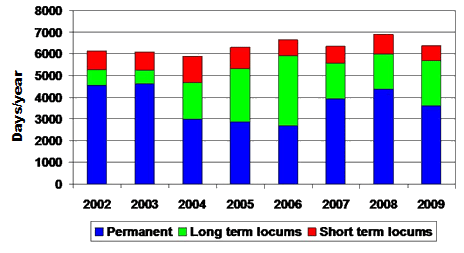
Figure 1: Total number of consultant days per year
for permanent, long-term and short-term locums.
Consultant posts
There were 20 different permanent contract consultants employed during the study period. The number of available positions increased from 15 in 2002 to 17 in 2009. One specialty, anaesthesia, has 4 consultants (increased from 3 in 2006); general surgery and medicine have 3 (surgery increased from 2 in 2004), obstetrics and gynaecology and psychiatry have 2; orthopaedics, paediatrics and radiology have one consultant. At no time during the 8 year period were all posts filled by permanent appointments. During 2003 and 2004, 13 of these posts were filled with permanent appointments; there were 9, 8 and 9 permanently appointed consultants in 2004, 2005 and 2006 consecutively; there were 12 in 2007 and 2008 and 11 in 2009. The decreases seen between 2004 and 2006 occurred because of retiring (n=4), moving to another job (n=2) and retiring on health grounds (n=1). During the 8 year period one consultant was suspended for nearly 2 years and 3 had prolonged episodes of sick leave.
Long-term locum posts
The number of days of long-term locum usage in the Western Isles Hospital are shown (Fig2). Thirty-one people had held long-term locum posts since January 2002. One had been in post for virtually the whole 8 years and 3 held post for longer than 3 years. Long-term locums have been in place since the permanent appointee left or retired in obstetrics and gynaecology (2004), orthopaedics (2001), paediatrics (2004), and radiology (2000 until 2004 after which short-term locums were employed) and have been required to fill un-appointed vacancies in anaesthetics, medicine, psychiatry and surgery. Four have been required to cover long-term sickness and 3 have been required to cover a consultant on suspension.
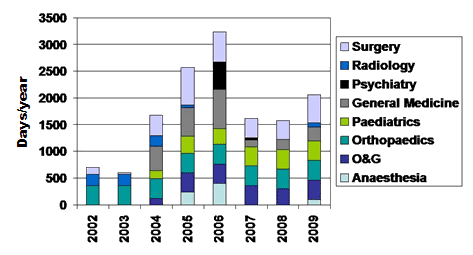
Figure 2: Total number of consultant days per year for
long-term locums in the various medical specialties.
Short-term locum posts
The number of days of short-term locum usage are shown (Fig3). The average number of days per year was 880 with a range of from 703 (2008) to 1214 (2004).
One hundred and eighty-eight different doctors worked 535 separate locum episodes during the 8 year study period. One hundred and three were employed for a single episode; 65 for 2-5 episodes; 12 for 6-10 episodes; 3 for 11-15 episodes; 5 for 16 episodes or more. Those individuals employed for 16 or more episodes worked 16 (orthopaedics), 17 (medicine), 20 (psychiatry), 24 (paediatrics) and 33 (obstetrics and gynaecology).
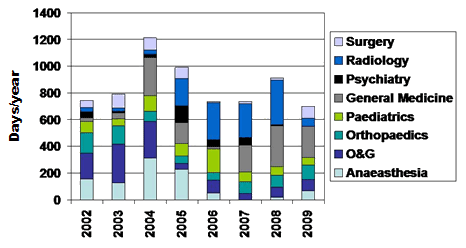
Figure 3: Total number of consultant days per year for
short-term locums in the various medical specialties.
Discussion
Consultant locums are required for a number of different reasons, but the essential underlying feature is that they cover the service during temporary periods of absence of a consultant appointed to a substantive contract. The problem of recruiting doctors to consultant or specialist posts, particularly in rural areas, is not unique to Scotland; however, the problems faced by the 6 Scottish rural general hospitals (sited in Fort William, Oban, Orkney, Shetland, Wick and Stornoway) are similar. Suitably experienced senior doctors capable of taking on the broad-based and varied-skilled posts required to serve the needs of the rural population are becoming increasingly difficult to find and locum tenens doctors capable of filling the gap until a permanent placement are also scarce and hard to find. This is not a new issue and problems of recruiting physicians for small and rural hospitals in Oklahoma were highlighted by Al Assaf and Wilson in 199110. The Royal Australasian College of Surgeons has tried to ease the problem of procuring locum surgeons by establishing a locum specialist service, but it is recognised that few city based surgeons are willing to undertake rural locum placements11.
In rural general hospitals the main problem caused by consultant absences is the compromised cover of the out-of-hours emergency service. All rural general hospitals have junior doctors in training posts and they are responsible for much of the day-to-day medical care. Over the period of this study the junior doctor on-call duties changed a number of times; however, for all the time there were 11 trainee doctors, 9 of whom could be on-call with consultant cover alone. Latterly the hospital was covered at nights and over weekends by a single resident trainee doctor working a one-in-nine rota. The junior doctors are all at an early stage of their career and none are in middle grade positions; as a consequence, all need consultant supervision. The out-of-hours structure requires 7 of the 8 specialties to be on call each night and weekend. During the period of study, one of these (paediatrics) had, from 2007 onwards, an arrangement where GPs with a specialist interest could cover some out-of-hours work; however, the remaining 6 specialties required a consultant to cover the out-of-hours on call.
Predictable absences occur for annual and study leave and amount to 10 weeks per consultant per year. Unless other arrangements are in place, these periods of absence are covered by short-term locum consultants. The filling of a vacancy occurring when a consultant leaves the service can be time consuming and locums are required to fill in until a replacement is found. Unpredictable vacancies arise with long-term sickness and consultant suspensions. The 6000-7000/year consultant days used to service the Western Isles Hospital has remained reasonably constant over the study period.
If an agreement is reached for consultants to cover colleagues' leaves of absence (prospective cover) this must, since the introduction of the new consultant contract in 2004, be factored into the agreed job plan. This usually applies to predictable forms of absence, such as annual, public holiday and study leave. Where a prospective cover agreement exists for a three-consultant service, the on-call commitment will increase from 1 day in 3 to 1-in-2.4. Many consultants find a 1-in-2.4 commitment too onerous and locum consultants are needed to ensure the service is covered during annual and study leave. Four consultant services with prospective cover arrangements will have a 1-in-3.2 on-call rota which may be more acceptable, but it is still considered high frequency. Clearly prospective cover is unwise for two-consultant services and impossible for services with only one consultant. Prospective cover agreements were in place for anaesthesia (from 2006), surgery (from 2006) and psychiatry (2002 and 2003 and from 2008). For a trial period (2006) the medical service was staffed as a four-consultant service (2 permanent appointees and 2 long-term locums) and a prospective cover arrangement was in place. As can be seen, the short-term locum usage during the periods of prospective cover agreement is markedly reduced (Fig3).
Internal locum cover, although not specifically addressed in this study, is sometimes used to cover shorter periods (1-4 days) of absence. Remuneration for internal locum cover is based on an hourly rate and claimed retrospectively. This internal locum cover is invariably from the existing consultant body as the trainee doctors in the Western Isles Hospital are at an early stage of their training and not of sufficient experience to take on consultant responsibilities.
Long-term locums are employed for the variety of reasons that cause consultant posts to be vacant for periods greater than 3 months. The commonest reason during the study was to cover the delay between a consultant leaving a post (retiring, moving to another post or ill health) and a replacement being appointed; 12 were employed for this reason. The remaining 19 were employed by NHS Western Isles as long-term locum consultants because they had the skills for the post but were not on the specialist register and could not be offered a permanent position (4); to cover long-term sick leave (4); to continue a service in its 'original' form until a long-term plan for that service has been agreed through the service redesign/clinical strategy process (3); to allow the locum an opportunity to work in the rural environment to see if they wanted a permanent appointment (3; with 2 consultants moving from locum to permanent status); to cover the work of a suspended consultant (3); or employed for the trial of a four-consultant medical service (2).
Although long-term locums provide the best solution to covering longer vacancies, there is not always someone available who will commit to a period as long as 3 months. In this circumstance, short-term locums have been employed to fill the gaps in service. Although the guidance is that locum consultant appointments should be limited to a maximum period of one year9, NHS Western Isles had to keep a number of long-term locums in place for more than a year.
Patient confidence and management are at their best when the healthcare service provides consistent continuity of care. This can be difficult with locums who are working in the Western Isles Hospital for the first and only time. Fifty-five percent of short-term locum consultants (103 of 188) worked for a single locum episode. This means that the majority of episodes (427) were worked by locums who completed more than one episode, with the majority of these (35%) working for between 2 and 5 episodes. Five individual consultants returned on numerous occasions and worked a total of 110 episodes; one obstetric and gynaecological consultant, who had previously held a permanent appointment in the Western Isles, worked 33 separate locum episodes. Although difficult to quantify, it is generally believed in the Western Isles Hospital that the contribution made by locums familiar with the way the hospital and its systems work is much greater than the contribution from those who work in the hospital for a single period. This can be seen in their handling of junior medical staff and undergraduate medical students. Those more confident with the local healthcare system are more likely to discharge patients from the wards and outpatient clinics and make more efficient use of available facilities. The standard of care provided by locum consultants can be variable and some administrators of small rural hospitals in the USA are reluctant to employ locum tenens surgeons for quality-of-care reasons, preferring instead to seek other solutions to the shortage of rural surgeons8. The Royal Australasian College of Surgeons has recognised the problem of locums meeting the requirement for participation in peer-reviewed surgical audit, and has set specific continuing professional development requirements for locums and established a Locum Evaluation and Peer Review Committee12.
The devastating effect of the loss of 7 consultants (6 substantive and one long-term locum) in 2 years (2004 and 2005) caused an immediate and dramatic increase in the need for short-term locums (Fig3); once long-term locum (2006, Fig2) and new permanent appointments (2007 and 2008, Fig1) were made, short-term locum usage decreased substantially. This demonstrated the fragility of a clinical service dependent on small numbers of consultants working in 'indispensible' posts and calls into question the wisdom of using this medical staffing model.
During the 8 year period of this study, 239 different consultants were employed for short, long or 'permanent' periods. This amounts to an average of 30 different people per year. After identifying suitable people through agencies, 'contacts' and advertisements, references must be obtained, interviews for the long-term locum and permanent appointments organised and the individual needs and difficulties of each doctor met. This adds up to a considerable amount of time for the relatively small medical personnel (human resources) department of the rural general hospital in the Western Isles.
Long-term locums are usually employed on standard NHS terms and conditions and consequently are often no more expensive than consultants in substantive posts. If a locum has not held a substantive post in the past he/she will be employed at the start point of the consultant scale and will not be paid or be eligible to be paid for any enhancements of salary by discretionary points, merit awards or clinical excellence awards. As a consequence the locum can be financially disadvantaged. Housing, subsistence and travel allowances may be payable and these can compensate for the salary short fall. Short-term locums, however, are more often paid at agency rates and these can be based on a sessional or hourly basis. If the short-term locums are paid the national contract average of £85/hour1, it will cost £14,280/week for a locum on a 1-in-1 on-call rota (1-in-1 rotas occured in NHS Western Isles in orthopaedics and paediatrics); and £8,840/week or £7,027/week for 1-in-2 or 1-in-3 rotas, respectively. Such sums of money would strain any health board's budget.
There is a disturbing perception that it is becoming increasingly difficult to identify suitable consultants for rural general hospital practice. If this is true, the requirement for long-term locums is likely to increase, at least in the short term. As rural general hospital practice becomes better defined and consultants are trained to have the specific skills needed for remote and rural practice, the number of doctors with the skills and broad based clinical knowledge required for rural general hospital work will become smaller, and finding locums with these skills will become increasingly difficult. This will not be helped by the increasing specialisation found in present day training programs.
The problems of locum usage in rural general hospitals will increase, it will become more difficult to find locums and they will continue to be a huge financial burden. For sustainable medical services to continue in rural general hospitals, avoidance of services which require locum cover for the predictable leaves of absence must be a goal. To have acceptable on-call rotas that meet European Working Time regulations, as many as 4 permanent consultants may be needed to provide prospective cover for their colleagues' leaves of absence. Vacancies must be filled rapidly, and if locums are required, long-term locums on NHS contracts must be employed where possible. Anything short of this will condemn the rural general hospital service to the vagaries of an unpredictable locum market which could bring about the demise of locally based effective secondary care.
Acknowledgement
The author acknowledges the assistance of Mrs Rhoda Morrison, Medical Staffing Officer, Western Isles Hospital in collecting the weekly locum lists.
References
1. Anon. Using locum doctors in hospitals. Edinburgh: Audit Scotland, 2010.
2. Temple JG. Future practice: a review of the Scottish medical workforce. Edinburgh: Scottish Executive Health Department, 2002.
3. Scottish Executive Health Department. Building a health service fit for the future: a national framework for service change in the NHS Scotland. Edinburgh: Scottish Executive Health Department, 2005.
4. Remote and Rural Steering Group. Delivering for remote and rural healthcare: the final report of the remote and rural workstream. Edinburgh: Scottish Government, 2008.
5. Temple JG. Securing future practice: shaping the new medical workforce for Scotland. Edinburgh: Scottish Executive Health Department, 2004.
6. Scottish Executive Health Department. Rural Access Action team report (Appendix). In: Building a Health Service Fit for the Future: a national framework for service change in the NHS Scotland. Edinburgh: Scottish Executive Health Department, 2005.
7. Lawrenson RA, Nixon G, Steed RH The rural hospital doctors workforce in New Zealand. Rural and Remote Health 11: 1588. (Online) 2011. Available: www.rrh.org.au (Accessed 7 November 2011).
8. Doty B, Andres M, Zuckerman R, Borgstrom D. Use of locum tenens surgeons to provide care in small hospitals. World Journal of Surgery 2009; 33: 228-232.
9. British Medical Association. The consultant handbook for Scotland. Edinburgh: British Medical Association Consultants (Scotland), 2006.
10. Al-Assaf AF, Wilson CN. Recruiting physicians for small and rural hospitals. Hospital Topics 1991; 69: 15-18.
11. Bruening MH, Maddern GJ. Rural surgery: the Australian experience. Surgical Clinics of North America 2009; 89: 1325-1333.
12. Royal Australasian College of Surgeons. Locum Evaluation and Peer review Committee terms of reference, v2. Melbourne, VIC: Royal Australasian College of Surgeons, 2010.
