The focus of this article is community perspectives on telemental health, using two rural and remote First Nations communities as a case-study. Telemental health - using information and communication technologies (ICT) (primarily videoconferencing) to support mental health and well-being - is a service offered to these communities through Keewaytinook Okimakanak Telemedicine (KOTM). Keewaytinook Okimakanak (KO) is the Northern Chiefs Tribal Council in Ontario, Canada.
By way of background, within the First Nations and Indigenous telemental health context, a small body of research exists on: (i) the advantages, disadvantages, and concerns of telemental health with First Nations communities; (ii) the perspectives of mental health workers who work with remote and rural First Nations communities on telemental health; and (iii) the experience of telemental health clients. However, there is a paucity of research about the relevancy of telemental health to remote and rural First Nations communities, and the perspectives of community members on using this approach to service.
We begin to address this gap by actually 'listening' to the community members. Within this study we are exploring the perspectives of rural and remote First Nations community members on the approach of using videoconferencing for mental health services - telemental health. What are seen as the advantages and the concerns?
Given that telemental health is accessible in many remote and rural First Nations communities in Ontario (and other provinces), and the KO tribal council sees value in it (as evidenced in the establishment of KO Telemedicine), it seemed important to explore community members' own thoughts and concerns about using telemental health. This could allow for increased discussion about using the service in communities, and how telemental health services might help support the community's needs and interests. This in turn could facilitate positive and mindful engagement with the technology.
In the following sections, there will be a review of the topic of mental health in remote and rural First Nations communities, followed by a review of the area of telemental health with First Nations communities, including the advantages, disadvantages or challenges, and past studies on the topic.
Mental health and First Nations communities
First Nations communities, like all communities, have goals related to mental health and wellbeing. Due to the legacy of colonization, First Nations people may especially be seeking change and interventions at different levels. In an examination of problematic issues such as levels of suicide, violence and alcoholism within communities, Kirmayer et al1, in common with other authors2,3, found the origins of the wellness issues to be a result of colonization. At the 2007 symposium on the Social Determinants of Health, Indigenous representatives from the Americas, Asia, Australia, New Zealand and the Philippines listed 'colonization' as one of the most fundamental and underlying determinants of health4. The Residential School legacy in particular has had a widespread negative impact on the wellbeing and mental health of First Nations individuals and communities (for a critical analysis5).
It is important to emphasize the impact of colonialism on Indigenous peoples in Canada. At the same time, this is not mentioned to position First Nations communities as disempowered; for indeed there are self-governing, empowered and healthy Indigenous communities in Canada. However, the impact of colonialism on individual and community wellbeing, and on cultural, social, political and economic aspects of Indigenous communities in Canada cannot be denied. Further, some communities that are isolated (ie remote or rural) can experience greater difficulty in fostering healthy communities when confronted with a lack of resources.
Mental health resources within the communities themselves are sometimes limited and other challenges can present themselves as barriers to help-seeking (eg lack of anonymity and confidentiality due to the small size of communities). For instance, in certain First Nations communities in Northwestern Ontario, mental health professionals visit a community only a limited number of times per year. Community resources for addressing mental health issues are often strained, for a variety of reasons (eg limited funding, lack of infrastructure)6. Often, individuals need to leave their communities to seek treatment. This often places individuals at greater risk for health and wellness problems, and indeed this has been recognized as a problem by mental health professionals who have experience working with remote and rural First Nations communities7.Therefore, telemental health provides a mechanism to connect individuals and communities with a wide variety of mental health services.
Remote and rural First Nations communities could benefit from culturally-safe8 and appropriate mental health services and resources for individuals seeking intervention at that level. Many traditional First Nations cultures have holistic conceptualizations of health and wellness9. Although an examination of how telemental health can be integrated into a holistic framework, or the specific content of any interactions through telemental health are not a focus of this article, these are clearly issues that need to be addressed both in research and practice.
It is important to emphasize that the authors do not believe that outside help and telemental health is 'the answer' to the communities' need for resources or change; instead, telemental health offers an option to help support certain goals. If the various levels of conditions in the community (cultural, social, political, economic) could be improved so that the community was no longer in need of telemental health services, or if all issues could be appropriately dealt with within the community, that would be ideal. However, a detailed discussion of interventions of this type is outside of the scope of this article. Further, healthy communities and all communities always have individuals who sometimes need services.
As Varadharajan proposes, there are a variety of levels at which these issues can be addressed, including the individual, family, community, spiritual, social, economic, and political levels, among possible others (p143)10:
Because colonization in all its complexity affects all our lives on many levels, from the trivial to the profound, the process of 'de-colonization' cannot but be equally intricate and multidimensional.
Telemental health is a tool that can be used in supporting change and development at many if not all of these levels. Using telemental health at an individual and group level - connecting people for therapy, group support, sharing circles, and education - is the focus of this article.
Telemental health in a First Nations context
The Grand Chief of the Nishnawbe-Aski Nation, Stan Beardy, made the following statement at the United Nations Conference on Indigenous Peoples' Communications for Development in 200711:
My presentation to you today [via streamed video] represents a remarkable achievement by our people to not only harness the power of information and communication technologies but also adapt these technologies to address our political, social and economic agenda.
Telehealth, conceptualized as the use of ICT and broadband networks to deliver health services and support wellness, has been a focus of interest and expansion in rural and remote First Nations communities in Canada12-14. Tribal councils (eg KO), various levels of government, non-government organizations, and academic and research organizations have all been engaged to some degree in this venture. Recently, the Assembly of First Nations (AFN) passed several resolutions recognizing and attempting to address the need for First Nations in Canada to have sufficient broadband networks and access to ICT15.
Telemental health is a mental health service approach which uses videoconferencing (and potentially other ICT) to connect those engaged with the service for a variety of activities, including (but not limited to): support groups and group therapy, assessments, individual therapy, and psycho-education. Since the mid-1990s the use of telemental health in Canada and in First Nations communities across Canada has been growing12. Telemental health has been conceived of as a vehicle for connecting remote and rural communities to mental health services where otherwise access to certain resources within their own communities would not be possible6,7,12,16,17.
For instance, the KO telepsychiatry pilot project16 was a ground-breaking venture that sought to connect certain rural and remote First Nations communities in Northwestern Ontario with psychiatric services. A driving force behind the project was the objective of supplementing current mental health services and reducing wait times. At that time (and arguably still today) mental health clients in the communities were often dependent on external regional services with limited presence in the communities, and/or they were often required to leave their home community to receive care. Currently, both in-person (again, as provided by external regional services, and certain in-community resources) and telemental health services are available in KO communities18. Other service providers have also opted for this modified model of service delivery. For example, Brasfield and Clement19 describe how a stress and anxiety clinic in British Columbia works with a variety of remote and rural First Nations communities, harnessing the utility of telemental health and incorporating in-person visits to allow for greater continuity of care.
A report by the AFN states (p20)20:
For Aboriginal people, an integral component restoring balance and wellbeing to communities, involves community empowerment as well as individual wellbeing. To this end, health and social services delivery must be under Aboriginal control, and services delivered by trained Aboriginal people. The ultimate expression of an Aboriginal Health system that embodies both individual and community empowerment is self-government.
Perhaps an excellent example of an ehealth/telehealth project that follows this creed is the Fort Chipewyan Project21. Specifically, remote First Nations communities in Alberta are working together using videoconferencing to provide traditional medicine to Aboriginal communities. This project started out with a typical health and physiotherapy focus, and has evolved into 'tele-spirituality', connecting spiritual Indigenous leaders to various communities. Indeed, according to Gideon, Aboriginal leaders view ehealth as a tool and a means to improve 'access to, and control over, health services'. Further, telemental health and ehealth in general in First Nations communities has been touted as having the potential to facilitate a new environment that is healthy, empowering, and key to social change21. Indeed, the AFN has proposed a strategy for increased broadband network connectivity which could help support these initiatives15. However, the success of any community's telemental health initiative will depend on how the tool is engaged with. Therefore, it is critical that First Nations communities be involved in the development of health, mental health, and telemental health policies.
Advantages and challenges of telemental health with First Nations
First Nations communities that have been able to access telemental health services have experienced and reported many benefits6,16. These include increased access to services, client satisfaction, and decreased costs. Telemental health has also been proposed as a mechanism for facilitating networking and support among community mental health workers and mental health workers outside the communities, in addition to allowing increased flexibility at the local level for the management of mental health services16. Furthermore, in Northwestern Ontario videoconferencing can provide the means to connect communities and individuals speaking Native languages, which can help create a space where individuals can communicate, share and heal in their own Native language. Keewaytinook Okimakanak Telemedicine facilitates regular elder visitations, an activity that allows elders from different communities to communicate and interact using their Native language, allowing an important cultural tradition to continue22. Carpenter and Kakepetum-Schultz emphasize the importance of integrating First Nations values and beliefs into an information technology health system for rural and remote First Nations23. Further, they assert that First Nations ownership and control of the service is central to the success of the initiative.
In 2003, Jennett and colleagues conducted a systematic review of the socio-economic impacts of telehealth24. One of the areas that Jennett et al. focused on was First Nations telehealth. Of the eight studies that met their criteria for review, it was concluded that access to appropriate healthcare was the most commonly identified socio-economic benefit among this population. Being able to access this healthcare while staying in the home community can lead to greater quality of life and mental health24,25. Another Canadian study concluded that telehealth is a viable means for providing access to health care in light of the real shortage of healthcare providers evident in Canada today26.
Health Canada produced a status report on telemental health in 200412. Within this document, it is noted that key informants viewed telehealth as a (p.iii)12:
...strategic tool, capable of improving the access to and quality of mental health services at the local or community level. They foresee a great potential for rural and remote communities in particular, where serious shortages of health professionals are felt.
The report outlined a number of key challenges to reaching this potential. These include: a lack of service providers, underdeveloped ICT infrastructures, insufficient funding, a lack of capacity to implement projects, and 'cultural issues'. In addition, as in the general telehealth climate, difficulties also exist related to reimbursing service providers and licensing; some mental health associations have developed guidelines for telemental health use by practitioners, and others have yet to do so.
Looking beyond Canada, telemedicine and telemental health is used with Indigenous peoples in Australia25,27. In the USA, Shore et al have explored telemental health for rural American Indian communities28 . They concluded that 'safety nets' and emergency protocol (support resources and a plan to respond in the case of crisis or necessity) in addition to guidelines are necessary to facilitate telemental health for these rural communities. Furthermore, collaboration with local service providers can be beneficial, because their knowledge of and connection to the community can help inform the process. Shore et al also underscored the importance of obtaining an understanding of the community's culture and their experiences with different organizations (at different political levels), as well as their tribal history. According to Shore et al, all of these factors are important for successful telemental health initiatives.
Shore et al also pointed out an interesting dynamic that can exist within telemental health for rural American Indian communities (and often in telemental health in general) - the greater interpersonal space that exists within telemental health encounters can have different impacts28. The distance can sometimes facilitate disclosure in some clients who might feel more comfortable being more physically distant from the clinician. The same effect has been documented in telepsychiatric services involving First Nations communities in Northern Ontario16 and British Columbia19. Nevertheless, in some circumstances the distance can potentially detract from the therapeutic relationship if a sense of connection is lacking. Of course, a sense of connection could be understood in multiple ways, including 'social presence'29 (the level of awareness of the other person in the social interaction, a concept often studied in ICT mediated communication) or other aspects of the therapeutic relationship (eg rapport, trust).
Participation in previous studies on telemental health in First Nations
It appears that no research or literature exists on First Nations community members' perspectives on telemental health, or even on community perspectives on the broader area of technologies for mental health services, or technologies in general.
Within the Canadian context, there are a handful of studies that have explored the experience of First Nations telemental health clients6,16,30. As mentioned earlier, a telepsychiatry pilot project was conducted in Northern Ontario in 2001. According to the evaluation, telemental health clients reported high levels of satisfaction with the service (p.iv)16:
...almost all the clients indicated that the psychiatrist had helped them with their emotional problems, and that they would recommend the service to people they care about who have emotional problems.
In addition, clients found it beneficial to have access to the opportunity of receiving mental health services in their home community without the requirement for travel. It was also concluded that (p.iii)16:
In contrast to western cultural expectations, the distance created by not being face-to-face with the psychiatrist appears to have helped clients feel comfortable with the psychiatrist.
Advancing a few years and moving to Eastern Canada, during 2004 and 2005 the Mawi-Wolakomiksultine project (Maliseet for 'together, let's have good healthy minds') was underway in New Brunswick30. This partnership project focused on extending telemental health and teleaddictions to 5 First Nation communities in the area. First Nations clients who participated in this initiative reported very positive experiences with telehealth. Understandably, many clients reported feeling somewhat uncomfortable with the telehealth set-up at first; however, after they became engaged in the session they reported feeling as if they were in the room with the provider. Specifically, according to the evaluation, 96% of the clients reported being satisfied with the telehealth session, 89% reported ease of communication during the session, and 82% of the clients reported that they preferred the telehealth sessions to travelling to the urban center for services.
Finally, studies on telemental health that have explored the experience of mental health professionals who work with First Nations clients and communities will be reviewed. Recently, Gibson et al examined the experiences of and attitudes toward telemental health in mental health professionals who work with First Nations7. Individual interviews with mental health professionals who had experience in telemental health with remote and rural First Nations clients informed the study. Additionally, there was an online survey component. Participants were mental health professionals Canada-wide who had experience working with remote and rural First Nations communities (but not necessarily telehealth experience). The researchers found that overall, participants in the online survey reported finding telemental health a useful tool for connecting with remote and rural First Nations clients. Further, there were a variety of concerns about using telemental in the clinical context, including the appropriateness of using videoconferencing with certain clients (eg individuals who are experiencing psychosis), the uncertainty of conducting certain interventions (eg exposure therapy) through video, and the need for 'safety nets' and resources at client's site. Finally, the authors noted that professionals who had participated in the interviews tended to have significantly more clinical experience with the telemental health approach, and had discovered useful strategies for addressing therapeutic challenges (eg relationship building) in telemental health.
The review of background and previous literature identified the need to understand the community perspectives on this topic, which led us to our research question for the study: What are the perspectives of remote and rural First Nations community members on telemental health? Specifically, what do community members identify as advantages and concerns related to telemental health and its place in their community?
Understanding community members' perspectives on telemental health is crucial because as we know from the technology acceptance literature31, users' perceptions of the technology - especially in relation to its usefulness - will influence whether the approach is actually adopted and used. Past research has explored how perceptions of usefulness and ease of use of telemental health influence the use of telemental health among mental health professionals who work with remote and rural First Nations clients7. Despite the fact that we are not specifically investigating the 'constructs' of perceived usefulness and perceived ease of use in the current study, the underlying goal remains the same: to understand community members (users) perspectives of the technology, as this will be a contributing influence to their intention and actual use of it. At this point, it is also important to distinguish that this study is exploring attitudes toward the use of telemental health as an approach, and is not addressing the actual content of the services or therapy that will transpire during the session.
VideoCom is a collaborative research project exploring how remote and rural First Nations communities are using ICTs. VideoCom (http://videocom.firstnation.ca) is a partnership of three First Nations organizations and two research organizations that spans the Atlantic, Quebec, and Ontario regions. The current study was conducted with the support of KO, the authors' partner in Northwestern Ontario.
This partner representatives provided expertise, feedback and support throughout the various stages of this initiative, including the design of the project and interview guide, helping foster connections with the communities, aiding with recruitment, and other activities.
Participants
In total, 59 remote and rural First Nations community members participated. All participants were over 18 years; however, specific age information was not collected. Participants reported holding a variety of roles and positions in the communities, including health workers, teachers, family members and caregivers (eg mothers), elders, leaders (Band Council members), community workers, part-time workers, technology support workers, and others. Our sample was 56% female and 44% male. In addition, certain participants spontaneously reported having personal experience with telemental health when the specific interview questions were asked. However, the interviewers did not ask about personal experience with the approach (as the interviews were not about personal or sensitive information), and therefore reporting how many participants had past experience would be an invalid and inappropriate representation. Furthermore, even though participants in the current study lived in communities that had access to telemental health, not all participants were aware of it and the majority had never used videoconferencing.
Materials
The structured interview guide had 12 sections; those relevant to this study include demographic and introductory information, and technologies for community health and wellness. Specifically, participants were asked about their thoughts on using technologies like videoconferencing for telemental health and counselling services in their communities. As a further exploration, interviewees were asked about their perspectives on whether mental health services that take place through video are less personal, or if instead the space created by video can make people feel more comfortable.
Procedure
In autumn 2009, in collaboration with KO, the research team sent invitational letters to the Chiefs of 33 First Nations in the Sioux Lookout Zone in Northwestern Ontario. Communities were invited to participate in the greater VideoCom initiative and host a community visit. The community visits involved research and outreach components. Interviews with community members regarding their current use of ICTs, and how the technologies could better meet individual and community needs, was the focus of the research.
One rural First Nation community (Northwestern Ontario) and one remote (fly-in) First Nation community (Northern Ontario) accepted the invitation. These First Nations fall under Nishnawbe Aski Nation, a 'political territorial organization representing 49 First Nation communities throughout the province of Ontario'32. Nishnawbe Aski Nation spans the territory that includes James Bay Treaty 9, as well as the portion of Treaty 5 that is within Ontario's borders. The Chiefs appointed a community liaison to work with us to organize the visits and provide feedback and collaborate on research and outreach activities. The community liaisons distributed posters and helped raise awareness around the communities about the research and outreach activities. They also gave guidance in regards to procedural plans around the interviews (possible locations to conduct interviews, people to invite for interviews) and other activities. Currently, the VideoCom team is still working with both of these communities to collaboratively prepare articles and chapters on the topic of ICT use by community members that are relevant and useful to the communities.
The research team was welcomed into the communities in February and March 2010. To recruit interview participants, researchers employed the following methods: circulating posters prior to our visit; visiting community centers (eg resource center, health center, Band office) to meet community members and invite them to participate; advertising the study at a parallel outreach event (community video festival); and, in one community, placing an advertisement on the community television channel. Finally, the 'snowball approach' was quite effective: community members who participated in the research often (and spontaneously, without our direction) recommended the study to their family and friends.
Interviews lasted between 20 min and one hour and participants were given a $20 honorarium. Participants were advised that participation was voluntary, anonymous, and confidential.
The research protocols complied with Canadian (Tri-Council) guidelines for research with Aboriginal participants, and all participants (and their data) were treated in accordance with the ethical guidelines outlined by the American Psychological Association. Ethics approval was sought and obtained from the University of New Brunswick and the National Research Council. Ownership, Control, Access, and Possession (OCAP) principles also informed the design of the study33. In total, 56 in-person interviews were conducted in the communities, and 3 telephone interviews were conducted afterwards.
All 59 interview audio-recordings were transcribed and the transcripts imported into the qualitative analysis software program NVivo (www.qsrinternational.com). The transcript sections related to telemental health were coded thematically for advantages and perceptions of usefulness, and concerns. Typically, when performing a thematic analysis, subthemes and data are only reported if more than one individual has raised the same issue, so as to avoid 'n of 1' issues. However, because this is new and exploratory research, all concerns of community members were identified, even if the point was only raised by one participant.
Because the researchers were interested in community members' attitudes toward telemental health, during the analysis the researchers chose to categorize responses as either positive (eg telemental health is a good idea, useful), negative (eg telemental health is not a good idea, is not appropriate), or neutral (eg not sure if it is useful or not). The data were then entered into SPSS (www.spss.com) to facilitate a descriptive analysis. Two researchers were involved with the coding/categorization, and several components of the interviews were coded, in addition to the telemental health question. An inter-rater reliability check was completed for the overall process. The analysis demonstrated a 97% agreement rate. This inter-rater analysis was completed based on 10% of the data (6 complete interviews).
Finally, in addition to the quantitative and qualitative analyses that are offered and described above, a 'ways forward' section was also developed in collaboration with the KOTM staff (including the community telehealth coordinators for the two communities). Once the initial draft of this article was complete, the co-authors met by telephone to discuss and determine possible ways to address the concerns that were being raised by community members. Based on that discussion, we offer possible 'ways forward'. We would encourage communities and organizations who are engaged with telemental health to consider whether actively engaging on the topic (eg discussion) might also be useful for them. The ideas we will discuss are not intended to be prescriptive, or exhaustive.
Thematic analysis
The interview responses were coded for advantages and disadvantages/concerns. Within each of these domains, several subthemes were identified. Advantages will be explored first. Under the umbrella of usefulness, telemental health was seen as a way to increase access to helpful mental health services, and provide continuity of care to clients. For the approach to be considered useful, trust was identified as essential. Further, telemental health was associated with decreases in expenditures in terms of travelling time and expenses. Last, participants reported that clients may feel free to disclose when participating in telemental health, compared with in-person services.
Advantages of telemental health
Usefulness: Community members reported that they viewed telemental health as being potentially very useful in their communities. Telemental health was seen as a tool to enable: (i) greater continuity of mental health care for community members; and (ii) greater access to mental health services overall, as demonstrated by the following quotes.
The first quote also speaks to the theme of trust - trust in the technology/approach and trust that the approach will 'honour them':
I think that actually would be really good [telemental health]... Of course, if people were comfortable with it where we would have a place in the social program, maybe, or in the health centre where ... You know, say if somebody had a counsellor in Sioux Lookout that they really need to talk to because they're experiencing flashbacks or they're experiencing a kind of a dip in the road, they could go there and interact with that counsellor and they could see them on the video and just go back and forth and be able to overcome whatever it is that's bothering them at that time... I think the first thing is that people need to know they can trust the service, it's confidential. Because, of course, you know that in healing, the first thing that needs to be restored and the hardest thing to be restored is trust....If people know that they can trust the system to honour them - their healing - I think people would be apt to use it ... You need to be able to have it accessible. If something does happen ... Like our resource centre is supposed to be 24/7, so people can go there anytime if they need help. (Community member participant)
I think it would be a really good idea because...say this person has kids and can't go out of town for counselling...they could just make an appointment with [the community telehealth coordinator] and she could do her counselling there. (Community member participant)
One participate noted their perception of the lack of in-community mental health resources and reported that telemental health could help address that issue:
I think that would be a good idea if there was a mental health worker working with people on their [using telemental health] because we never have a mental health worker here. (Community member participant)
Reductions in travel: Participants noted that telemental health could allow an individual to remain in one's home community when accessing certain mental health services that most times would require travelling. If using telemental health, an individual has the option of remaining in their home community while working on increasing their mental health, instead of facing different challenges associated with leaving their community to access services. Participants also indicated that the reduction in travel time and travel costs would be a benefit of telemental health.
I think that's a good idea. It would cut down on travel costs. (Community member participant)
It [telemental health] sure beats...flying back and forth. (Community member participant)
Well, it [videoconferencing] would make stuff a lot easier for people, because most of them don't really want to leave home to go out there [outside of the community to access services]. It's a lot easier for them just to stay where there's a videoconference set. (Community member participant)
Client comfort/facilitation of disclosure: Community members commented on how telemental health (as opposed to in-person sessions) may actually allow mental health clients to feel more comfortable, and talk more openly. This finding has also been documented in the literature7,16,19,28.
Personally, I went through that [telemental health] myself. I was in counselling and at that time, I wasn't very comfortable with seeing [a therapist] like face-to-face, in person, until we started going on telemedicine. So I got a little more comfortable saying what I wanted to say. (Community member participant)
I think that's why kids like Facebook so much, because there isn't that face-to-face interaction. And I find a lot of people, especially in the community, they tend to wear their hoods up to kind of hide their identity. And by using Facebook, they can do that, even though it's coming from them, they can still say what they want without having someone kind of talk back to them. So I think with video that definitely plays out too. They can somewhat still hide their identity and still be braver than what they would normally be. (Community member participant)
Concerns/disadvantages of telemental health
In addition to the positive attitudes toward the use of telemental health, community members also voiced a variety of concerns about it. These included concerns about the appropriateness of using videoconferencing for mental health services, and concern that the approach may not be culturally appropriate. In addition, again the theme of trust was raised - this time in the context of how building trust (an important component of the therapeutic relationship in any kind of therapy or in interactions in general) over video is likely difficult, and how it is better done with a community member. Further, the theme of preferring to leave the community for service was identified. In addition, the concern that telemental health may detract from capacity building within the community was raised, along with the issues of problems with the technology, and concerns about privacy. The criticism was raised that if people do not have running water in their homes, how helpful is telemental health? Despite the fact that many people reported positive views toward telemental health, clearly many concerns were present as well.
Concern about the appropriateness of using videoconferencing: Several participants were wary about the appropriateness of using videoconferencing for accessing mental health services. Participants who voiced these concerns often noted that mental health work and healing is something that needs to be done 'in person'. One participant explained that the importance of human contact was imbedded in First Nations culture, and just because the service approach may benefit certain stakeholders, does not mean that it is appropriate.
Expected difficulty with building trust over video was noted as well. The quotes below demonstrate these concerns:
I really couldn't speak on behalf of [First Nation community], but for myself, I think it's an inappropriate use of the video technology. I think it unnecessarily removes the psychiatrist as a human caregiver ... or a psychologist. And I don't think that you can ever really fully gain rapport with somebody that you see on screen. It doesn't matter how good the technology is. It could be a plasma TV. It doesn't matter. There needs to be some level of human contact in order to fully win somebody's trust and to make some useful changes... (Community member participant)
That [telemental health] would be alright, but I think you're better served with that with somebody in community ... because you gotta build some trust there. (Community member participant)
It's easier for service providers 'cause it's cheap. It doesn't cost a lot of money and you can potentially reach more people and save a lot of cost and money. But that's not our First Nations people either. Our culture really means talking to somebody face-to-face in your own language and then using...cultural stuff. More and more we're sort of de-personalizing our citizens. You know, for a physical diagnosis, or in an emergency, that's fine [telehealth]. (Community member participant)
For counselling... it would be better if that person's there. You know what I mean, [more] comforting. (Community member participant)
One participant noted their preference for leaving the community for treatment, despite the perceptions by some other participants that leaving the community was an inconvenience.
Well, I think it's better if you go out. Go out of town. (Community member participant)
Another participant raised the point that if telemental health is being used, the mental health professional would not be there in person to see what environment the individual is actually living in. This participant explains the issue below, and also appears to be questioning the utility of using telemental health when people are missing the very basic necessities.
How do they [person connecting with client through telemental health] actually get to know that person? Like, with just seeing them and talking and that, how do they know, unless they're here to experience what that person is going through, and what their conditions of their house and their waters and things like that. Because there's tons of Natives that don't even have running water, and they don't have hydro, and there could be like 20 people living in one room. And if they don't have that in their house, then how would videoconferencing help that particular family? (Community member participant)
Some participants commented on how developing a relationship over videoconferencing could be difficult and perhaps not appropriate, but that meeting 'in person' first could help address this issue.
Probably just for follow up but not for initial visits ... Probably follow up will work, once they've already established that relationship with a person. (Community member participant)
Privacy and security issues: Community members raised some valid and important concerns about privacy, security, and confidentiality. Some participants noted the difficulty of achieving privacy in the office setting where the videoconference unit was located. Other participants voiced concern over who would be able to access and view their private video session while it was taking place, and what exactly would be happening with the video transmission.
I tried it and I didn't feel comfortable talking on there because I feel like a [staff person] would hear what you're saying...she closed the door but I still didn't feel comfortable with it. (Community member participant)
The last participant was asked if her experience of telemental health would have been different if she could have accessed it within her own home:
VideoCom interviewer: ...If you had it in a more private place, like in your own home, would that be better?
Community member participant: Yeah, for me it would be.
Safety concerns: Some participants also voiced concern around the safety of telemental health, and what would happen if an individual was in a crisis or was unsafe and the mental health worker was only connected through video at a distant site. This participant discusses how in a time of crisis they would prefer to be with someone in person.
I think that it's just so impersonal using technology. That's just my personal opinion. If I was going through a mental health crisis, I'd prefer to have someone there to touch me or just to say, it's okay, rather than doing it over the video. (Community member participant)
Interference with capacity building: One participant raised an important point of consideration - could telemental health detract from capacity building in the community, since the typical set-up involves connecting a client with a therapist who is elsewhere? This is related to the premise that a community should develop resources with mental health workers or healers in the community to address any issue that comes up, instead of having community members seek services outside of the community.
The following individual reported concerns around the use of telemental health and when asked if telemental health would be more appropriate for helping with the continuity of in person, regional services:
I don't think it [telemental health] should be used in the mental health field. Secondarily, I don't think there should be any regional services [therapists who work in an urban centre and visit the community periodically] because I think we need to build a capacity in each community. We need to have our own mental health counselling in the community. (Community participant)
Problems with the technology: A minority of participants reported actual personal experience with telemental health (please note that the participants were not asked whether they had personally used the service, but some described their experiences spontaneously). Of those who did, one participant noted that she found it positive and helpful but noted an issue with using the technology. Fortunately, she also noted that she did not perceive the technical issues to detract from her overall positive experience:
I wish it [the image transmitted by video] would just stop freezing. That's about it. (Community member participant)
Ambivalence/uncertainty
Some participants were unfamiliar with the concept of telemental health; another participant recognized how it might not be appropriate for everyone, but there are likely some people who would find it useful for accessing support.
I've never heard of that before. Well, because I know that there was a girl taken out of this community this week and sent to Sioux Lookout for treatment because she was talking about suicide. So I know here, they've always taken them out of the community to get them help. So she's at a hospital right now. So I don't know how that would work. I've never heard of that before. But you know, if they don't have anyone locally, that would be great, so then at least they have someone to talk to. (Community member participant)
Everybody is different. It doesn't really make a difference for me if it's video or face-to-face, as long as I got the help that I needed. (Community member participant)
Overall diversity of opinions
As illustrated, the quantitative results demonstrate a diversity of opinions (Fig1). Specifically, 47% of the participants were categorized as having a positive response toward telemental health, 32% as having a negative response, and 21% as neutral or undecided.
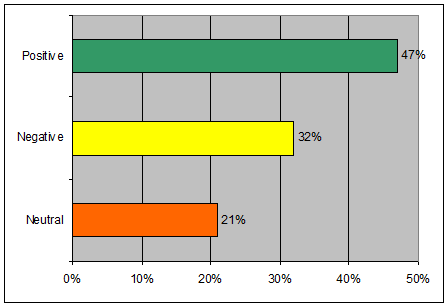 Figure 1: Telemental health responses: overall percentages (n=53)
Figure 1: Telemental health responses: overall percentages (n=53)
Based on the thematic analysis of interview responses, we now have considerable information to help us begin to understand different perspectives and concerns about telemental health. To begin with the advantages of using the approach, participants associated the use of telemental health with the potential increase in access to mental health services, and an increase in continuity of mental health care. Participants noted that the need to travel outside of the community to access resources would be reduced, as would the time and cost associated with travel. Additionally, some participants also felt that communicating with a therapist through videoconferencing would facilitate client comfort and disclosure. Indeed, this same benefit has been noted in past research7,16,19,28. In summary, many participants saw telemental health as being potentially very useful for their community.
In contrast, however, a number of participants also felt that it would not be useful or helpful for their community. Many questioned the appropriateness of delivering mental health services over video, instead of 'in person'. One participant questioned the real benefit of using telemental health when some individuals in the community do not have the basic necessities of daily living (eg running water). Another participant raised the point that telemental health (and other in-person mental health services from professionals outside of the community) could potentially detract from capacity building in the community since individuals are connecting with individuals outside the community for support. Others were concerned about privacy and safety issues. Finally, other participants reported feelings of ambivalence and indecision about telemental health services, acknowledging that it is not a solution for everyone but some may find it helpful. It appears that this observation is quite valid, especially when taking into account the wide range of attitudes that were demonstrated.
These important concerns deserve further consideration, and some have been addressed in the 'ways forward' section. With regard to telemental health and capacity building - does it have a negative impact on capacity building, or could it actually support it? For instance, KOTM currently has an ongoing telehealth project that seeks to build the capacity of health professionals within remote and rural communities. Videoconferencing can be used to support the communities in the ways that are deemed most appropriate by the community. Therefore, videoconferencing could be used to connect community members with mental health professionals in other communities, or videoconferencing could just as easily be used to connect professionals within the community with consultative resources outside of the community, thereby potentially supporting capacity building. It could also be used for family visits, helping to connect separated family members, for elder visits, and to connect with other communities for discussions in relation to health and wellbeing. It can be as creative as the community would like to be.
Many of the concerns raised by community members have also been raised by mental health service providers7. Within the literature, certain options have been raised for addressing some of the concerns that were raised by community members. For example, mixed models of service delivery have been discussed, where videoconferencing complements (rather than replaces) in-person services7. In the current study, a participant explained an initial in-person meeting could be helpful. Further, respecting and integrating First Nations beliefs, values, and traditional practices into telehealth and telemental services can also be helpful7,23. For instance, in the study of Gibson et al, one mental health professional described how she had been involved in facilitating sharing circles that evolved using videoconferencing7.
Both advantages and disadvantages need to be taken into consideration when communities are deciding whether telemental health may be a useful tool for their community, and whether it may help the community to meet its goals. Further, concerns about and barriers to use must be addressed by telemental health initiatives if increased engagement with the service and positive experiences are goals.
Limitations
This study assessed the usefulness of the approach of telemental health, the tool of using videoconferencing to connect communities and individuals for mental health services. It was not evaluating the effectiveness of the mental health therapy or any service that would transpire via that service. Further, because of the limited number of participants and the nature of the non-random and non-representative sample, the results of this study should not be generalized in any way. Instead, hopefully this work can serve as an impetus to communities and organizations to engage with openness in exploring the perspectives of their own community members.
Future research
This study is a starting point for exploring how remote and rural First Nations community members perceive telemental health and its place in their community. Further investigations are needed because First Nations communities in Canada are diverse and varied, and community engagement on the topic can help better determine whether this approach to service is a useful and appropriate tool in helping meet community needs and goals. It would also be highly beneficial to have a critical analysis of the role of telemental health in First Nations communities, with an exploration into the cultural, social, political and economic factors involved. The important issues of whether telemental health could interfere with capacity building, and how useful it is in light of some individuals not having access to basic resources, deserve greater attention. This appears to be a complex issue, because telemental health - if owned and managed by the communities and used for supporting community goals - could potentially support the community in capacity building. Future investigations will hopefully provide more insights about this.
Ways forward
First and foremost, any ways forward for community telemental health initiatives need to be community driven and community led. This will increase the likelihood of initiatives being successful and experiencing a higher level of engagement, and the community experiencing positive benefits from using the tool. Communities need to have the opportunity to tailor the use of the technology so that it fits their needs, and the use may be different from current mainstream Western use of the technology. For example, recall the 'tele-spirituality' Indigenous telehealth initiative that formed out of a previous physiotherapy telehealth initiative.
Consequently, telemental health needs to be a community's choice, and an individual's choice; it cannot be something that is imposed. Telemental health needs to be one of many options (ie services within the actual community, traditional medicine, in-person therapy, among other possibilities) that an individual or community can use in attempting to address goals of mental health and wellbeing. If a community is interested in increasing engagement in telemental health as a tool for accessing services and/or using it for their own interests (eg a tele-spirituality clinic), the following possibilities could be considered.
Education about telemental health, and raising awareness about the approach, is an important first step. One possible way of increasing awareness may be by having brochures about telemental health available in community health centers, the Band Council office, or other areas that display information in the community. Interested individuals can be offered the opportunity to speak with the community telehealth coordinator (or someone else in the community who is trusted and aware of the service) in a confidential setting to discuss any questions or concerns they may have about telemental health. Further, brief videos about telehealth featuring community members who have found it useful and beneficial or community leaders discussing the service (eg the Chief or Band Council Members, the community telehealth coordinator) could help in communicating the benefits, of telemental health to individuals seeking more information. Of course, it is not suggested that such videos would feature any private or sensitive information, or be about any personal telemental health experience.
Participants raised concerns about privacy and safety in using telemental health. Increasing privacy and safety needs to be a top priority in telemental health. Resources (like a 'safety net', a counsellor or contact available for the client in the community) and a safety plan need to be in place for any telemental health clients. Further, there are a variety of things that could be done in a health center setting to help increase privacy. Ideally, the individual who is using telemental health would be aware of all precautions taken to ensure their privacy and would be asked if a sufficient level of privacy was achieved. For example, headphones could be used, or a 'white-noise maker' could be set up outside the room. The room used for telemental health consultations needs to be as sound-proof as possible.
Addressing issues of privacy underscores the need for flexibility in the setting of telemental health. Currently, the majority of (if not all) telemental health sessions take place at the community health center or nursing station. ,, , , Som, e individuals may fear the stigma that could be attached to their seeking mental health services, and some may not feel comfortable going to the nursing station for fear that their anonymity will be compromised. In some areas of telehealth, home-visits are possible, and in this study one participant noted that she would have felt more comfortable accessing telemental health from her home. However, using videoconferencing at a nursing station, or at home, is not always ideal. For example, depending on the home situation and how many people reside there, privacy may be even more limited. Therefore, communities and organizations need to be open to increasing the flexibility of telemental health and engaging the client in co-determining aspects of the setting that may be safest and most beneficial for them.
Finally, it is necessary to 'think outside the box'. Using telemental health in the typical Western way of connecting a client with a mental health professional may or may not be useful for a community. Instead, using the tool for peer support (eg quitting smoking groups, community discussions/connections), group work or sharing circles about certain issues, easing transitions from institutions or healthcare facilities, and facilitating family visits with family members who are out of the community due to illness, school, or other reasons, are examples of creative applications of the tool. Further, telehealth can be used to foster wellbeing in a community by connecting Elders and other community members with other communities to provide the opportunity to speak traditional languages and engage in traditional practices. In fact, this last activity is currently offered by KOTM. There are endless possibilities, and the communities and their leaders know their own interests and needs best.
Conclusion
If communities decide to engage with telemental health and find it rewarding, participation in telemental health will increase naturally over time as people experience its benefits and usefulness. Al though First Nations communities are forging new models for telehealth delivery, the introduction of telehealth into remote and rural First Nations communities is relatively new given the history of the communities and their familiarity with other technologies. One KOTM staff author recalls that a couple of years ago the idea was raised to use telehealth to facilitate first-aid and CPR training in remote and rural First Nations communities. The response at the time was that it may not be possible or appropriate. Currently, this type of training is offered via videoconferencing and the initiative has been reported as very successful.
Valuing Indigenous knowledge can help us understand community members' experiences of and concerns with telemental health and inform more successful and appropriate initiatives. Most importantly, any ways forward for community telemental health initiatives need to be community driven and community led.
Acknowledgements
First, the authors thank the leadership and communities of the two participating First Nations communities in Ontario for partnering with them in this study. In addition, the authors acknowledge the help and support of the community liaisons in these two communities. The authors also thank all 59 community members who took the time to participate in this research. Further, this article would not have been possible without the participation of the community telehealth coordinators. The authors thank Keewaytinook Okimakanak, K-Net, the KO Research Institute and KO Telemedicine for their valuable support of this project. They also thank all members of the VideoCom team for their involvement and helpful feedback along the way. The VideoCom project is funded by the Social Sciences and Humanities Research Council of Canada (SSHRC), with in-kind contributions from project partners including Keewaytinook Okimakanak (KNET, KORI, KOTM), the First Nations Education Council, Atlantic Canada's First Nation Help Desk, the University of New Brunswick, and the National Research Council of Canada, Institute for Information Technology. Finally, the authors thank the helpful Rural and Remote Health reviewers for their excellent feedback.
References
1. Kirmayer LJ, Bras GM, Tait CL. The mental health of Aboriginal peoples: transformations of identity and community. Canadian Journal of Psychiatry 2000; 45(7): 607-616.
2. Hill DM. Traditional medicine and restoration of wellness strategies. Journal of Aboriginal Health 2009; 5(1): 6-25.
3. Vickers, PJ. Ancestral law and community mental health. In: Canadian Institute for Health Information (Ed.). Mentally healthy communities: Aboriginal perspectives. Ottawa: CIHI, 2009; 17-20 .
4. King M, Smith A, Gracey M. Indigenous health part 2: the underlying causes of the health gap. Lancet 2009; 374: 76-85.
5. Chrisjohn R, Young S, Maraun M. The circle game: shadows and substance in the Indian Residential School experience in Canada. Penticton, BC: Theytus, 1997.
6. Keewaytinook Okimakanak Research Institute. MMW mental health project evaluation 2005/2006 and 2006/2007. Thunder Bay, ON: Keewaytinook Okimakanak Research Institute, 2008.
7. Gibson K, O'Donnell S, Coulson H, Kakepetum-Schultz T. Mental health professionals' perspectives of telemental health with remote and rural First Nations communities. Journal of Telemedicine and Telecare 2011; (in press).
8. Dion Stout M, Downey B. Nursing, Indigenous peoples and cultural safety - So what? Now what? Contemporary Nurse 2006; 22(2): 327-332.
9. Hunter LM, Logan J, Goulet J, Barton S. Aboriginal healing: rRegaining balance and culture. Journal of Transnational Nursing 2006; 17(1): 13-22.
10. Varadharajan A. The "repressive tolerance" of cultural peripheries. In: K Landezelius (Ed.). Native on the net: Indigenous and Diasporic peoples in the virtual age. Abingdon, Oxon: Routledge, 2006; 143-150.
11. O'Donnell S, Perley S, Walmark B, Burton K, Beaton B, Sark A. Community-based broadband organizations and video communications for remote and rural First Nations in Canada. In: Proceedings of the Community Informatics Research Network Conference (CIRN) 2007; 5-7 November 2007; Prato, Italy, 2007.
12. Health Canada. Telemental health in Canada: a status report. (Online) 2004. Available: http://www.hc-sc.gc.ca/hcs-sss/alt_formats/iacb-dgiac/pdf/pubs/2004-telemental/2004-tele-mentale.pdf (Accessed 1 October 2009).
13. O'Donnell S, Molyneaux H, Gorman E, Milliken M, Chong C, Gibson K et al. Information and communication technologies to support health and wellness in remote and rural First Nations communities: literature review. Fredericton: National Research Council, 2010.
14. Romanow RJ. Building on values: the future of healthcare in Canada (The Romanow Report). Saskatoon, SK: Commission on the Future of Healthcare in Canada, 2002.
15. Whiteduck J. Building the First Nation e-community. In: JP White, J Peters, D Beavon, Dinsdale P. (Eds.). Aboriginal policy research VI: Learning, technology and traditions. Toronto: Thompson Educational , 2010; 95-103.
16. Keewaytinook Okimakanak. Evaluation of the Keewaytinook Okimakanak tele-psychiatry pilot project report, Balmertown: Keewaytinook Okimakanak, 2002.
17. Muttitt S, Vigneault R, Loewen L. Integrating telehealth into Aboriginal healthcare: the Canadian experience. International Journal of Circumpolar Health 2004; 63: 401-414.
18. Keewaytinook Okimakanak Health. (Online) no date. Available: http://health.knet.ca/ (Accessed August 1 2010).
19. Brasfield C, Clement C. Beyond the pilot studies: cognitive behavioral therapy in a remote Aboriginal community. Canadian Society of Telehealth Conference: Telehealth: Empowering Primary Care; 4-6 November 2007; St John's, Newfoundland and Labrador, 2007.
20. Assembly of First Nations. An Aboriginal health info-structure: critical issues and initiatives. Ottawa: AFN, 1998.
21. Gideon V. Canadian Aboriginal peoples tackle e-health: seeking ownership versus integration. In: K Landezelius (Ed.). Native on the net: Indigenous and Diasporic peoples in the virtual age. Abingdon, Oxon: Routledge, 2006; 61-79.
22. Wawatay News. KOTM reunites families through elder visits. (Online) 2009. Available: http://www.wawataynews.ca/archive/all/2009/12/10/KOTM-reunites-families-through-elders-visits_18744 (Accessed October 1 2010).
23. Carpenter P, Kakepetum-Schultz T. Above and beyond: embedding community values and beliefs into an evolving First Nations IT health system. E-Health COACH Conference; 29-31 May 2010; Vancouver, British Columbia, 2010.
24. Jennett PA, Affleck Hall L, Hailey D, Ohinmaa A, Anderson C, Thomas R et al. The socio-economic impact of telehealth: a systematic review. Journal of Telemedicine and Telecare 2003; 9: 311-320.
25. Lessing K, Blignault I. Mental health telemedicine programmes in Australia. Journal of Telemedicine and Telecare 2001; 7: 317-723.
26. Watanabe M, Jennett P, Watson M. The effect of information technology on the physician workforce and health care in isolated communities: the Canadian picture. Journal of Telemedicine and Telecare 1999; 5(Suppl2): S11-19.
27. Griffiths L, Blignault I, Yellowlees P. Telemedicine as a means of delivering cognitive behavior therapy to rural and remote mental health clients. Journal of Telemedicine and Telecare 2006;12:136-140.
28. Shore JH, Bloom JD, Manson SM, Whitener RJ. Telepsychiatry with rural American Indians: Issues in Civil Commitments. Behavioral Sciences and the Law 2008; 26: 287-300.
29. Cukor P, Baer L, Willis SB, Leahy L, O'Laughlen J, Murphy M et al. Use of videophones and low-cost standard telephone lines to provide a social presence in telepsychiatry. Telemedicine Journal 1998; 4(4): 313-321.
30. River Valley Health. Telemental health and teleaddictions partnership project - Mawi Wolakomiksultine evaluation report: Fredericton, NB: River Valley Health, 2006.
31. Davis FD. Perceived usefulness, perceived ease of use, and user acceptance of information technology. Management Information Systems Quarterly 1989; 13(3): 319-340.
32. Aski Nation. Land, Culture, Community. (Online) 2011. Available: http://www.nan.on.ca/article/land-culture-community-120.asp (Accessed 12 April 2011).
33. Schnarch B. Ownership, control, access, and possession (OCAP) or self-determination applied to research: a critical analysis of contemporary First Nations research and some options for First Nations Communities. Journal of Aboriginal Health 2004; 1: 80-95.





