Antenatal care (ANC) and postnatal care (PNC) are significant determinants of maternal health and, particularly, safe motherhood. Antenatal care is an important predictor of safe delivery and provides health information and services that can improve the health of women and infants1,2. In addition, ANC has a positive impact on the utilization of postnatal healthcare services3, while PNC and intrapartum care significantly reduce maternal mortality because most maternal deaths occur in the first week after delivery4-6.
Bangladesh has strengthened its emergency obstetric care (EmOC) under the Directorate General of Health Services, through national and international collaborations7. In 1993, the United Nations Population Fund (UNFPA) commenced support of government improvement of 64 maternal and child welfare centers for EmOC8. In addition, the Obstetrical and Gynaecological Society of Bangladesh with the support of UNICEF improved EmOC in 11 district hospitals on a pilot basis in the period 1994-1998, with a subsequent expansion to other districts3. As a result, ANC and PNC visits increased substantially in Bangladesh from 1999-2000 to 2007.
Despite improvements, pregnancy-related complications remains the leading cause of death and disability among women of childbearing age8,9, disproportionately among different Indigenous, non-Indigenous and cultural groups. A study of inter-ethnic groups in the Chittagong Hill Tracts revealed that access to healthcare facilities, prevalence of contraception and ANC visits were lower among Indigenous groups, compared with Bengali people10.
The purpose of this study was to examine the factors associated with ANC and PNC visits among the Mru Indigenous community in Bangladesh and identify determinants, so that policy-makers can initiate strategies to improve this aspect of community health.
General information about the Mru people
The Mru people are the most underprivileged Indigenous group living on hilltops and cliffs and in ravines and deeply forested areas of the Bandarban District of Bangladesh. The Mru settled in this region several hundred years ago from the state of Arakan in Myanmar11. According to the Bangladesh Population Census 1991, the Mru Bandarban District population was 22 16712; however, a 1995 survey by the Mru Social Culture found the total Mru population to be 59 74813. It is not possible to determine the exact number of Mru people currently because the last Bangladesh population census did not enumerate Indigenous people.
Among the Mru, the level of education is low, with only 2.6% of boys completing the highest 9 years of schooling and only 1.1% of girls completing the highest 8 years. The distance from the Mru villages to the nearest school is 12.1 km. The Mru people live in 5398 households in 356 villages (known as paras) in the Bandarban District. Mru houses are built on wood or bamboo stilts and are different from other Bengali dwellings14,15.
Study design and sampling
This research adopted a cross-sectional study design with a mixed-method approach. The study was conducted in Bandarban District in the remote south-eastern part of Bangladesh where the Mru people live. The Bandarban District has 7 upazilas (administrative sub-districts), three of which were purposively selected for this study: Alikadam, Lama and Thanchi. The majority of the Mru people live in Alikadam, followed by Thanchi and Lama. Geographically, Thanchi's terrain is the most remote and hilly, followed by Alikadam and Lama. A diversity of religions is found in these regions, including Animism/Buddhism, Christianity, and Crama, a new religion created by Man Ley Mru in 1985. Finally, socioeconomic conditions differ among the districts studied, with those living in Lama Upazila being better off than those in Alikadam, followed by Thanchi.
For the quantitative data, a total of 374 currently married Mru women (133 from Alikadam, 170 from Lama and 71 from Thanchi) having at least one child aged 5 years or younger were selected purposively. An attempt was made to achieve a representative sample based on differences in religion, age, socioeconomic conditions and distance from living place to healthcare service centers. However, this was only partially successful due to the remote locations of the Mru villages, transportation issues and the lack of educated Mru female interviewers. Consequently most of the interviewers for women in the 3 upazilas came from Lama District.
For the qualitative data, a total of 26 respondents were selected for in-depth interviews according to the following criteria: currently married women with experience of delivery, traditional midwives, family welfare visitors (FWVs), family welfare assistants (FWAs), nurses, village 'doctors' (persons with no medical background and generally <10 years of general education), Mru leaders, school teachers and non-government organization (NGO) workers from the same upazilas.
Data collection and measures
A questionnaire with both closed and open-ended questions was used for the collection of primary information. The Mru have a distinct language and most of the women are unable to communicate in the Bengali language. This necessitated hiring 7 bilingual female interviewers from the Mru community to conduct the interview survey, and three of these were NGO health workers. One interviewer had been formally trained as a midwife in a private medical college hospital. Two interviewers were health workers, two were students and the remaining two were housewives.
A pilot survey was conducted before using the interview schedule for data collection. The independent variables for bivariate and multivariate analyses were place of residence, age, religion, education and occupation of the respondents, education and occupation of respondents' husbands, parity, place of services provided in the community, distance to the service centers, means of transportation, whether the women were accompanied to the service centers, and exposure to mass media. The response variables were: antenatal care visit (yes = 1, no = 0) and postnatal care visit (yes = 1, no = 0). An interview checklist was used for in-depth interviews. The study questions were in Bengali language.
The research was conducted anonymously with the informed consent of all subjects. The Mru informants were consulted about the research objectives and its benefits were presented to the respondents.
Data analysis
Data were analyzed using SPSS v16.0 (www.spss.com). Bivariate and multivariate analyses were employed. Multivariate analysis of PNC was not conducted due to the extremely low percentage of PNC visits among the Mru women. The explanatory variables used in the bivariate and multivariate analyses were demographic, socioeconomic and spatial factors of the respondents. All independent variables found to be significant at 1%, 5% and 10% levels in the bivariate analyses were used during the multivariate analyses. Significant variables were retained in the final regression model. Some variables found to be significant in bivariate analyses were not found to be significant in the multivariate analyses; in most cases this was because they were concentrated in one category of independent variable. Thematic analysis was used as the method of qualitative data analysis.
Qualitative results
Healthcare services: Access to healthcare services was extremely poor among the Mru people. The average distance to health facilities from the villages was 18.8 km for the Mru and 6.3 km for the Bengalis15. There is a government hospital known as Upazila Health Complex (UHC) in each upazila in Bangladesh. In the study upazilas the UHC had an obstetric and gynecology unit but no EmOC. There were no gynecologists in these hospitals due to Bangladesh doctors' preference for working in large cities. The UHCs in Alikadam and Lama had one FWV but Thanchi UHC had none. However, some FWAs and nurses in each UHC are instrumental in providing care when women are seeking maternal healthcare services. In addition, FWAs visit villages 8 times each month. However, most of the Mru villages are impossible to access due to the difficult terrain and communication issues. These villagers are most likely to go to untrained village 'doctors' and the pharmacy at the local market. Small scale village outreach projects have recently been started by NGOs in some areas of Lama and Thanchi, but Alikadam has not yet been included.
Non-utilization of existing healthcare services among Mru women is likewise due to large distances to service centers, illiteracy, lack of awareness of health issues and language barriers. The women may not know where to obtain treatment, or they may not visit service centers, even with serious health issues due to feelings of shame. Several women and key informants explained that they could not describe their problems and complications precisely to the doctors and staff because it made them feel embarrassed. One FWV reported:
Although the Mru women are usually open within the community, they are very shy to the Bengali society. They are ashamed to share their problems with us and so they do not come to the hospitals.
As a result, Mru women do not utilize health facilities even if their household is close to a service center.
Women's role in the Mru family: Although the Mru people live in a patriarchal society, it is customary for women to do more agricultural work in the jhum field (a 'slash-and-burn' or shifting agricultural technique), compared with men. Women also perform almost all household activities, waking early to pound rice, and cook and serve it to other family members. In the jhum field, almost all girls and women are involved in planting, weeding and harvesting. Sometimes they also help with the slashing and burning. Girls usually try to reach the jhum field before sunrise and stay into the evening. During winter, women collect firewood and are engaged in beer and liquor production. Older women usually stay at home to care for the babies of those who are working in the fields.
Women have no control over the household economy and other decisions. Female social mobility is very low due to community isolation. Very few women go to the local weekly market to sell and buy goods.
Antenatal care and practices: Mru mothers do not go to a healthcare center during the first and second trimesters of pregnancy, due to a perception that any problems or complications of pregnancy at this time are unimportant. The long distances and transportation problems due to their home terrain discourage health visits. Even in the third trimester of pregnancy and during complicated deliveries, women are unlikely to present to a health facility. A FWV from Alikadam said:
In my 17 years of service life, I found only two Mru women who came to the hospital due to their delivery complications.
Instead, women try to resolve their obstetric problems within the community, following an accepted protocol. First they go to traditional midwives. If the midwife is unable to assist, the patient's husband or father-in-law is sent to visit the traditional village healer (TVH). The TVH can only 'diagnose' and cannot suggest reasons for complications. At the TVH's suggestion, another type of TVH is consulted. This TVH discerns causes and provides a 'treatment offering' by worshipping and killing animals, particularly pigs. If this 'treatment' fails, the woman is referred to the village 'doctor'. If the village doctor is unable to assist they return to the TVH. If he cannot find a solution, he prays to Thurai - the Mru's god and they wait for the death of the mother.
Occasionally, if the village doctor fails, the patient is taken to a hospital or a private clinic using a stretcher made of thick cloth and two lengths of bamboo which is carried by at least four men. However the Mru people are animists who worship nature, for example the river or the mountain, and they are more likely to make animal sacrifices for healing than visit a hospital.
Postnatal care and practices: After delivery, women must stay in the inner kimma (a private room that is a bedroom for married couples, infants or smaller children) for 7-9 days, depending on clan practices and her birth parity (9 days for the first two deliveries and 7 days for subsequent births). During this time women sit by the fire, drink hot water, eat burning salt with rice, and place searing materials on their lower back (in most cases burning the skin).
After leaving the kimma their food practices continue for some months. For the first month after delivery women only drink hot water. This practice continues for 4-6 months, accompanied by salted rice. After one month, felong leaves (similar to spinach) are added to their diet for up to 3 months. After 3 months they may eat dried churi (a small sea fish) and this continues for 6 months to one year.
Once the postnatal dietary practices have ceased, women consume a free diet of rice, vegetables and fish, although meat is only eaten on special occasions. Eggs are usually reserved for hatching. Instead of oil for cooking their daily foods, Mru people use nappi, a liquid prepared from a small dry fish.
After delivery, Mru women often suffer from anemia, swollen legs, perineal tears, urinary tract infections, uterine prolapse, pelvic infection and postpartum sepsis.
Quantitative results
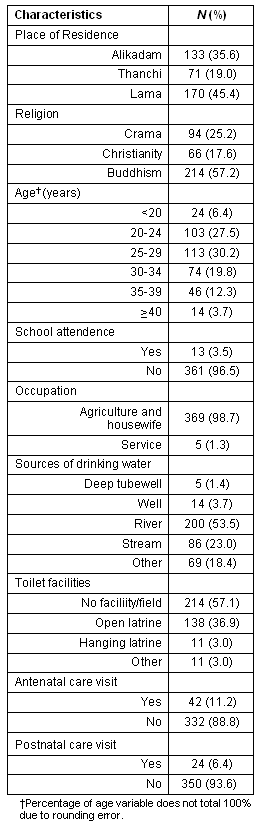
Sample characteristics: The survey respondents were mainly from Lama (45.5%) and Alikadam (35.6%), with 19% from Thanchi (Table 1). The majority (30.2%) were aged between 25 and 29 years, followed by 27.5% and 19.8% in the 20-24 and 30-34 age groups, respectively. Most of the survey respondents (96.5%) did not attend school. Regarding religion, the majority followed Buddhism (57.2%), followed by Crama (25.1%) and Christianity (17.6%). Some of those who self-reported as Buddhist were also animists. The Mru women were mostly engaged in jhum cultivation (98.7%) and household activities. Their main source of drinking water was the river (53.5%). Few had toilet facilities (Table 1). The rate of ANC was 11.2%, with 64.3% of these having had attended for one care visit and 2.4% for 4 visits. Only 6.4% had attended for PNC care.
Table 1: Percentage distribution of demographic and socio-economic characteristics among sample respondents
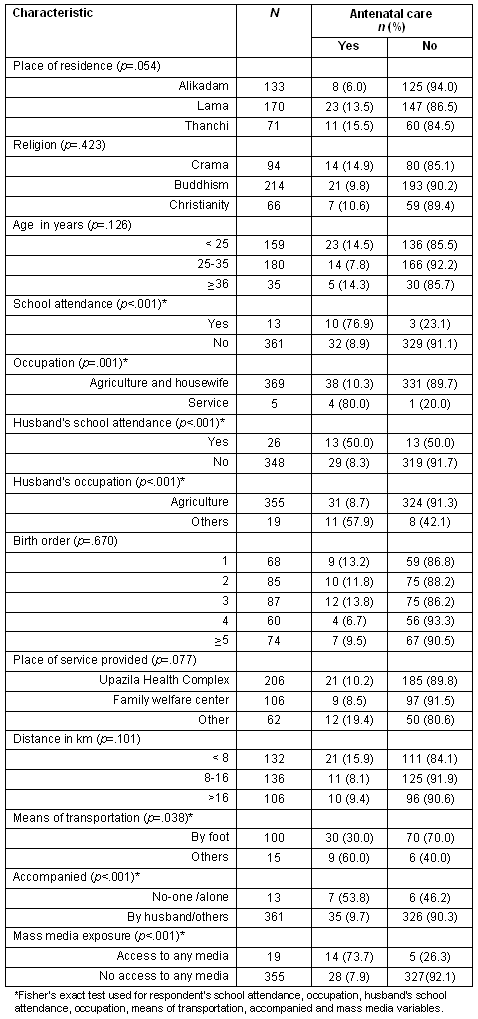
Antenatal care visits: The percentage distribution of women, and the association between ANC and background characteristics of women who had a live birth in the 5 years preceding the survey is provided (Table 2). The study revealed that an ANC visit had a significant association with a respondent's place of residence, school attendance, occupation, husband's school attendance and occupation, place of service provided in the community, means of transportation to the service center, and exposure to mass media. More than three-quarters (76.9%) of respondents who attended school received ANC during pregnancy, while this was so for only 8.9% of those who did not attend school. Antenatal care visits were high among women engaged in service jobs (80%), but low among those involved in agricultural and household work (10%). Similar results were found when a respondent's husbands attended school and was involved in other occupations, such as business or service. The study also revealed that 73.7% of respondents who had exposure to any mass media (radio, television or newspaper) received care during pregnancy, while this was so for only 7.9% of those who had no exposure to any media.
Table 2: Association between antenatal care visit and demographic and socioeconomic characteristics using Chi-square test
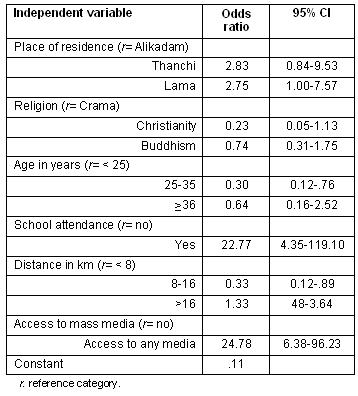
The results of the binary logistic regression analysis are shown (Table 3). The analysis suggested that respondents from Lama were more likely to visit service centers for ANC, relative to the respondents from Alikadam. A similar result was found for respondents from Thanchi. Respondents who were Christian or Buddhist were less likely to visit for ANC, compared with those who followed Crama. Respondents aged 25-35 years were less likely to visit service centers during pregnancy, compared with those under 25 years. Respondents who attended school full- or part-time were 22 times more likely to receive ANC relative to those who did not attend school. Respondents who resided within 8-16 km of a health service center were less likely to visit service centers, compared with those who lived less than 8 km away. Respondents with access to any mass media were significantly more likely to visit for ANC, compared with those who had no access to any media.
Table 3: Logistic regression estimates of demographic and socio-economic characteristics' effects on respondents' antenatal care visits
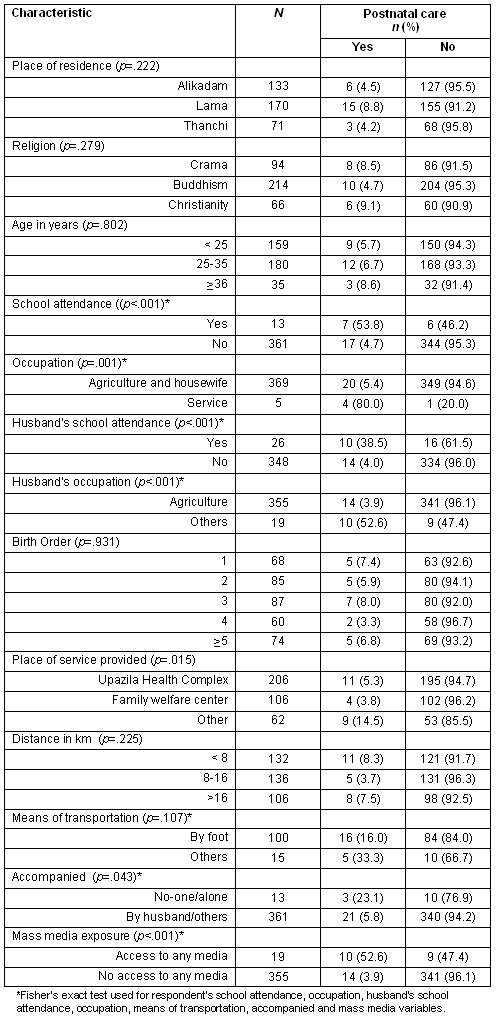
Postnatal care visits: The results of the bivariate analysis with regard to PNC visit is given (Table 4). A PNC visit was significantly associated with a respondent's school attendance and occupation, husband's school attendance and occupation, place of service in the locality, being accompanied on a service center visit, and exposure to any mass media. Only 4.7% of women with no schooling received care after delivery, while 53.8% of those who attended school did receive care. Care after delivery was high (80%) among service workers and low (5.4%) among women engaged in agriculture and household work.
The rate of PNC visit was higher among women whose husbands attended school and were involved in other occupations, compared with women with husbands were involved in agricultural work. Respondents who lived less than 8 km from a health service center had higher rates of receiving PNC than those residing further away. Over half the respondents (52.6%) who had exposure to any mass media received care after delivery, compared with 3.9% of those who had no exposure to any media.
Table 4: Association of demographic and socio-economic characteristics with postnatal care visits using Chi-square test
Reasons for not receiving antenatal care and postnatal care: When mothers were asked why they did not seek ANC and PNC a number of reasons were given (Fig1). First, 56.7% and 56.4% of the respondents reported that they did not seek ANC and PNC, respectively, because the service center was too far from their home. Approximately half of the respondents gave 'transportation problems' as the reason. One-third did not know that that care was needed. Other reasons included 'expensive', 'not beneficial', 'family didn't allow going to service center', 'better care at home', issues related to service quality and 'religious reasons'.
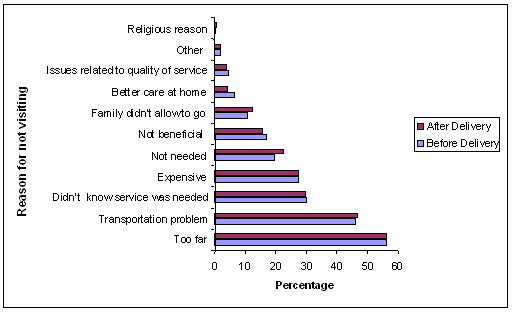
Figure 1: Percentage distribution of respondents' reasons for not visiting service centers before and after delivery.
Discussion
This cross-sectional study of a questionnaire survey and in-depth interviews, shows that both ANC and PNC visits among the Mru women are very low when compared with the general population of Bangladeshi women. For ANC visits, while the national Bangladesh level is 60.3%9, among the Mru women it was only 11.2%. This is consistent with a recent study from India that found ANC visits among the Indigenous women of Jharkhand were three-fold lower than the national average16.
In the present study, significant determinants of low ANC among the Mru women were: place of residence, age, educational level, distance to the health service center and access to mass media. The ANC visits were slightly higher among respondents from Lama and Thanchi, probably due to a 'door-step awareness program' conducted by NGOs in these areas. Several studies from other countries have demonstrated that a woman's education is the most important determinant of ANC utilization17-20, and in the present study this was the significant determinant of a ANC visit. A study in rural Bangladesh confirmed that higher education was associated with higher use of ANC3. Husband's education and occupation were also significantly associated with an ANC visit among Mru women.
Past studies have revealed that physical proximity to healthcare services and geographical distance are important determinants of healthcare service utilization21-24. Distance to the service center from the Mru women's homes was also a significant factor in their ANC visiting.
Care after birth is crucial for safe motherhood. The recent Jharkhand study in India demonstrated that PNC visits were less than half that of the national level16, and among the Mru respondents PNC was only 6.4%, three times lower than the national figure (21.3%)9. Variables positively associated with PNC were found to be the respondent's school attendance and occupation, the husband's school attendance and occupation, place of service provided in the locality, distance to the service centers and exposure to any mass media.
The reasons for not visiting services for ANC and PNC in the Mru respondents could be broadly classified as:
- Practical issues (eg distance to the service center, transportation problems)
- Normative issues (eg religious reasons, family did not allow the visit).
However, in the Mru situation, the practical issues were more influential, due to the restricted healthcare facilities and options available. In mainstream societies this is different9.
Recommendations
Healthcare delivery systems, for example satellite clinics, should be developed at village level to provide for the specific needs of women during pregnancy, delivery and in the postnatal period. In addition, community health volunteers' (CHVs) interventions should aim to improve maternal health status. This is because CHVs represent the community socio-economically, culturally, experientially and linguistically25,26.
A specialized EmOC should be developed within the UHCs as a secondary referral centre so high-risk mothers can receive better care when they reach the facility during an obstetric emergency.
There is also an urgent need for general and maternal health education for Mru women. Increasing awareness through training programs is especially important for these rural women, due to their restricted asses to mass media.
Pregnant women from the Mru Indigenous community of lower socioeconomic background and living at a distance from a health service center are less likely to visit for ANC and PNC. Because ANC and PNC are essential to reducing the risks of pregnancy and delivery, efforts should be made to improve maternal healthcare seeking behavior among the Mru women, with consideration for their socio-cultural beliefs and practices. Infrastructural issues should be addressed to allow healthcare delivery and appropriate education programs at the village level to improve the health of Mru mothers and their children.
Acknowledgements
The authors thank the Mru leaders, interviewers and especially the Mru mothers for their valuable information, assistance and cooperation during the field work. Also thanked are the Center for Sámi Studies, the Norwegian Higher Education Grant Program and the Department of Indigenous Studies, University of Tromsø for their financial support, which made this study possible.
References
1. Bloom S, Lippeveld T, Wypij D. Does antenatal care make a difference to safe delivery? A study in urban Uttar Pradesh, India. Health Policy & Planning 1999; 14(1): 38-48.
2. WHO & UNICEF. Antenatal care in developing countries: promises, achievements and missed opportunities. An analysis of trends, levels, and differentials 1990-2001. Geneva: WHO & UNICEF, 2003.
3. Chakraborty N, Islam MA, Chowdhury RI, Bari WA. Utilisation of postnatal care in Bangladesh: evidence from a longitudinal study. Health and Social Care in the Community 2002; 10: 492-502.
4. Campbell OMR, Graham WJ. Strategies for reducing maternal mortality: getting on with what works. Lancet 2006; 368: 1284-1299.
5. Hurt LS, Alam N, Dieltiens G, Aktar N, Ronsmans C. Duration and magnitude of mortality after pregnancy in rural Bangladesh. International Journal of Epidemiology 2008; 37(2): 1-8.
6. Li XF, Fortney JA, Kotelchuck M, Glover LH. The postpartum period: the key to maternal mortality. International Journal of Gynaecology and Obstetrics 1996; 54(1): 1-10.
7. Islam MT, Haque YA, Waxman R, Bhuiyan AB. Implementation of Emergency Obstetric Care Training in Bangladesh: Lessons Learned. Reproductive Health Matters 2006; 14(27): 61-72.
8. Gill Z, Ahmed JU. Experience from Bangladesh: implementing emergency obstetric care as part of the reproductive health agenda. International Journal of Gynecology and Obstetrics 2004; 85: 213-220.
9. National Institute of Population Research and Training, Mitra and Associates, Macro International. Bangladesh Demographic and Health Survey 2007. Dhaka, Bangladesh: NIPRT, 2009.
10. Ahmed SM. Health-care facilities, contraception and antenatal care services. In: M Rafi, AMR Chowdhury (Eds). Counting the hills: assessing development in hill tracts. Dhaka, Bangladesh: The University Press, 2001.
11. Brauns CD, Loffler LG. Mru: hill people on the border of Bangladesh. Boston, MA: Brikhauser, 1990.
12. Bangladesh Bureau of Statistics. Bangladesh Population Census 1991, Community Series: Zilla Bandarban. Dhaka, Bangladesh: BBS, Statistics Division, Ministry of Planning, Government of the People's Republic of Bangladesh, 1992.
13. Mahmud. Ang Ing Mru Rung. Bangladesh: Matri Productions, 2007.
14. Rafi M. Small ethnic groups of Bangladesh: a mapping exercise. Dhaka, Bangladesh: Panjeree Publications, 2006.
15. Rafi M, Chowdhury AMR. Counting the hills: assessing development in hill tracts. Dhaka, Bangladesh: The University Press, 2001.
16. Agrawal PK. How much the Indigenous Women of Jharkhand, India are in disadvantageous condition: finding's from India's National Family Health Survey. (Online) 2009. Available : http://paa2009.princeton.edu/download.aspx?submissionId=90455 (Accessed 21 June 2009).
17. Bhatia JC, Cleland J. Determinants of maternal care in a region of South India. Health Transition Review 1995; 5: 127-142.
18. Navaneetham K, Dharmalingam A. Utilization of maternal health care services in Southern India. Social Science & Medicine 2002; 55: 1849-1869.
19. Obermeyer CM, Potter J. Maternal health care utilisation in Jordan: A study of patterns and determinants. Studies in Family Planning 1991; 22: 177-187.
20. Taguchi N, Kawabata M, Maruo T, Aditiawarman, Dewata L. Influence of socio-economic background and maternal care programmes on maternal mortality in Surabaya, Indonesia. Tropical Medicine and International Health 2003; 8: 847- 852.
21. Stock R. Distance and utilisation of health facilities in rural Nigeria. Social Science & Medicine 1983; 17: 563-570.
22. Airey T. The impact of road construction on hospital inpatient catchment in the Meru district of Keneya. Social Science & Medicine 1989; 29: 95-105.
23. Paul BK. Health service resources as determinants of infant death in rural Bangladesh: an empirical study. Social Science and Medicine 1991; 32: 43-49.
24. Rahaman MM, Aziz KM, Munshi MH, Patwari Y, Rahman M. A diarrhoea clinic in rural Bangladesh: influence of distance, age and sex on attendance and diarrhoeal mortality? American Journal of Public Health 1982; 72: 1124-1128.
25. Love MB, Gardner K, Legion V. Community health workers: Who they are and what they do. Health Education Quarterly 1997; 24(4): 510-522.
26. Swider SM. Outcome effectiveness of community health workers: an integrative literature review. Public Health Nursing 2002; 19(1): 11-20.

