Dear Editor
Spinal cord injury (SCI) is one of the greatest calamities in the medical world, causing high mortality and serious aftereffects. The method of the trauma, type of transportation, time taken to reach hospital, and the resource level of the place of treatment chiefly determine SCI outcome. Limited resources and access to health care are challenges for SCI patients in rural India.
Socioeconomic transformation has led to lifestyle changes for India's rural population, for instance an improvement in road infrastructure has increased vehicular accidents. Of 2 million hospitalizations and 7.7 million minor injuries, 6% of patients will have an SCI1. However, the real incidence of SCI varies between 15 and 40 per million inhabitants each year in developed countries, and approximately 20% die before arrival at hospital2.
In a retrospective study, clinical and radiological features of SCI were analyzed for all 212 patients treated between 2006 and 2010 at Acharya Vinoba Bhave Rural Hospital, India, a tertiary hospital in a rural setting. When 57 patients who received primary treatment prior to transfer to this hospital were excluded, 155 patients remained. Of these, 80.6% were males in the 'productive' age group (18-65 years). A fall from a height was the commonest method of spinal injury (54.8%), followed by road traffic accident and then farm-related injuries (Fig1). In all, 88.7% patients did not receive any form of primary pre-hospital management on the journey between the site of injury and the tertiary care hospital. Ambulance services were used by only 15.5% of patients. Although type of transportation and time between injury and hospital arrival are important determinants of neurological outcome, mean injury to hospital arrival time was 74.4 hours.
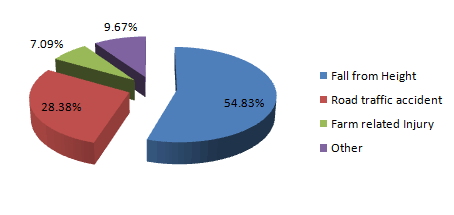
Figure 1: Method of injury for patients treated between 2006 and 2010 at Acharya Vinoba Bhave Rural Hospital, India.
The lack of pre-hospital services in rural India are likely to be responsible for poor SCI neurological outcomes seen in rural areas3. Considering the magnitude of the problem with reference to the method of injury in SCI patients, there is an urgent need for a comprehensive emergency spinal trauma care system nationwide, especially in underserved areas, such as the rural sector. A 'National Consultation on Pre-Hospital Trauma Care in India' in October 2006 at the National Institute of Health and Family Welfare, New Delhi4 recommended trauma care models (eg Ambulance Access for All [AAA] and Foundation and Centralized Accident & Trauma Services [CATS]), but these are only available for the urban population. The data presented in this letter is in contrast to the beneficiaries of such Government of India policies, for pre-hospital care and ambulance services are rarely available for remote and rural patients. This is a global issue5.
India needs to address both the prevailing and emerging trauma-care profile. A state-wide trauma-care system is urgently needed, including dedicated rural pre-hospital and SCI services. An SCI registry should also be developed to monitor the system and provide cost and epidemiological statistics. Epidemiological studies should be the basis of such a healthcare planning along with identified need for economic, social and political transformation.
Pradeep K Singh, MS1; Sandeep Shrivastva, MS2; and Rajesh Dulani, MS3
1,2,3Professor, 2and Vice Dean, Orthopaedics and Trauma Department
Jawaharlal Nehru Medical College
Datta Meghe Institute of Medical Sciences
Wardha, Maharashtra, India
References
1. Riska EB, von Bonsdorff H, Hakkinen S, Jaroma H, Kiviluoto O, Paavilainen T. Primary operative fixation of long bone fractures in patients with multiple injuries. Journal of trauma Trauma 1977; 17(2): 111-121.
2. Sekhon LHS, Fehlings MG. Epidemiology, demographics, and pathophysiology of acute spinal cord injury. Spine 2001; 26(24S): S2-S12.
3. Singh PK, Sakale H, Shrivastava S, Dulani R. Palliatve surgical approach to treat complete paraplegia in Indian rural setup. Indian Journal of Palliative Care 2010; 16(3): 151-154.
4. WHO India. National consultation on pre-hospital trauma care in India. Day 2 minutes. 26-27 October 2006, Munirka, New Delhi. Available: http://www.whoindia.org/LinkFiles/Diability,_Injury_Prevention_&__Rehabilitation_Pre_hospital_trauma_care.pdf
5. Grossman DC, Kim A, Macdonald SC, Klein P, Copass MK, Maier RV. Urban-rural differences in prehospital care of major trauma. Journal of Trauma 1997; 42(4): 723-729.


