Access to health care in rural and remote communities is a persistent and widespread challenge. This is so regardless of how rurality and remoteness are defined, or of any particular national, cultural and social circumstances surrounding rural life1. Difficulties recruiting and retaining physicians and other healthcare professionals to rural and remote areas have compounded the problems associated with health service access in these places2,3. One of the strategies to address this problem has been to locate medical education training within underserved rural, remote, or northern communities rather than in large urban areas. It is anticipated that exposing students to the challenges and conditions in practicing medicine and the general lifestyle in these settings will increase their confidence and interest in choosing to practice there4.
Much attention has focused on the economic and human capital required to support this approach. Future research and policy will be likely to explore its success in terms of addressing geographic mal-distribution of healthcare personnel. There is some evidence that the northern communities in Canada where training occurs also benefit from a substantial boost in pride and confidence5,6.
There has been much written about social capital over the past two decades, including a wide literature employing the concept to explain persistent health differentials at a variety of social scales, from the very local to the global7-10. Concern has been raised that the concept of social capital has become too broadly conceptualized, measured, and applied to retain any explanatory power. Portes proposes that this vast body of literature falls into one of two categories of use11. First, following the seminal work of Pierre Bourdieu and James Coleman, social capital is viewed as a resource that is accrued to individuals by virtue of their ties to others and enables them to achieve a particular goal (eg access to persons with specialized knowledge and/or degrees of influence with those in positions of authority)12,13. A second use, expressed most famously in the work of Robert Putnam, is when social capital is seen as 'features of social organization such as networks, norms and social trust that facilitate cooperation and cooperation for mutual benefit'14. Following Carpiano and Portes, this article views network characteristics, or the 'features' that Putnam writes about, as social cohesion. That is, high levels of trust and reciprocity are important bases for the formation of social capital, but are not the actual resources that members draw on to get something done.
In the current study the role of social capital in supporting the regional training site was explored, as were the benefits accrued to a broad range of stakeholders and network partners. The conceptual framework for this research was based on the view that social capital is derived from the particular set of individuals comprising a network11,12. Social capital is regarded as productive resources that are available to individuals or small groups as a result of their membership in a particular network12,13. The impact of a regional medical education program on social capital in the community was expected to be multifaceted due to complex interactions within and beyond the community more generally, as well as among the local and non-local stakeholders directly associated with the regional training site.
Context
In 2004, the University of British Columbia (UBC) Undergraduate Medical Education Program admitted the first 24 students to the Northern Medical Program (NMP), a regional medical education campus of its fully distributed MD undergraduate program15. The program is located at the University of Northern British Columbia (UNBC) in the natural resource-dependent community of Prince George, British Columbia (BC), which has a population of approximately 72 40016. Prior to the intake and arrival of students, the NMP enjoyed a considerable level of local support and commitment from a variety of stakeholders and sectors of local society. This support has continued to grow throughout the program implementation process. Research conducted in 2005 indicates that early perceptions of the broader impacts of the NMP on Prince George include extensive partnership formation and a sense of community connectedness5,6,15. The present study aimed to decipher and clarify these themes in this context through the application of the concepts of social capital and social cohesion.
Conceptual framework - social capital and social cohesion
In this study, social capital is understood as the stock of available productive resources, in both potential and realized form, that resides in a stable social network. These resources are held by the group but are available to its individual members. Such resources might include endorsements and authorization (eg to mobilize in-kind labour and voluntary support), access to privileged or specialized information, and expertise to draw on directly in various aspects of governance and decision-making. According to Bourdieu, the benefits of membership in a cohesive network extend further still by enabling the conversion and exchange of other forms of capital (eg economic, political, cultural) held by members of the group and useful in achieving a collective goal. In this sense, the productive capacity of a given network is clearly enhanced by the addition of members who occupy positions of authority or professional expertise. To empirically describe how social capital was produced and mobilized within and among networks during the planning and implementation of the NMP, Carpiano's framework of 'neighbourhood' social capital7 was adapted. Like Carpiano, this article distinguishes social capital from its antecedent factors (eg social cohesion) and outcomes (ie benefits), Figure 1. In the present study, the concept of social cohesion is regarded as a quality or characteristic of networks; more specifically, the degree to which values are shared among a group, or their sense of connectedness, trust and familiarity. In this sense, social cohesion is an important antecedent of social capital; that is, without network cohesiveness, social capital resources are nowhere near as readily mobilized for a particular purpose.
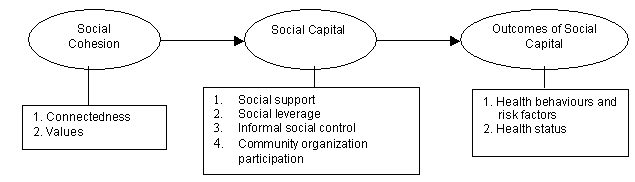
Figure 1: Modified version of Carpiano's Bourdieu-based model of neighbourhood social capital7.
While Carpiano's work focuses on the links between social capital and health, the present use of the concept to understand health services in general, and medicine in particular, is not without precedent7,17-21. However, a geographic scale that differs from Carpiano's study was employed; the context in which the present study was implemented is a relatively small and spatially remote urban centre, whereas Carpiano's work is based in neighbourhoods nested within larger metropolitan entities7. Although the socioeconomic composition of Prince George is considerably less homogeneous than many urban neighbourhoods, Carpiano's conceptual framework is relevant because the present study is interested in the networking potential of a spatially referenced group of individuals7. In fact, it is argued that this particular framework is more amenable to the study of networks in a spatially distinct (ie isolated) locale, such as Prince George, where a greater breadth (ie inter-sectoral diversity) of network formation and less spatial overlap with (or infiltration by) other networks is likely to be present. In this sense, following Carpiano's framework, the 'structural antecedents' for the formation and operation of social capital in the present study are the social and spatial conditions of remoteness, resource-dependency, and traditional under-servicing that characterize the NMP's host community and the wider region in which it is based7.
Approach
This was a qualitative study that combined purposeful and snowball sampling to recruit local leaders in the broad areas of health care, education, industry, media and local government. In total, 23 semi-structured interviews were conducted by the lead author in September and November 2007. Purposeful sampling was used both to create and expand the study sample. All eight participants from a study of the NMP conducted in 2005 were initially contacted5. These leaders represented the sectors of business, healthy administration, medicine, education, politics and media; all were involved with the establishment of the NMP to some extent. Six agreed to participate; two declined citing lack of time. A combination of snowball and purposeful sampling was employed to identify leaders representing Aboriginal health services, social services, allied health (ie nursing) and community development, sectors whose perspectives were judged integral to the study of the impact of the NMP. The aim was to broaden the sectors represented and to include participants who were not intimately involved with the implementation or administration of the NMP. Twenty additional leaders were identified, seventeen of whom consented to participate. Three representatives in the social services sector declined participation citing lack of knowledge of the topic. Many participants held multiple positions in the community and thus represented a variety of sectors; their demographic characteristics are shown (Table 1).
A semi-structured interview guide was constructed to ask participants for their perceptions of current and anticipated impacts of the NMP in Prince George (Fig2). Participants were specifically probed regarding both positive and negative perceived impacts.
Table 1: Participant demographics
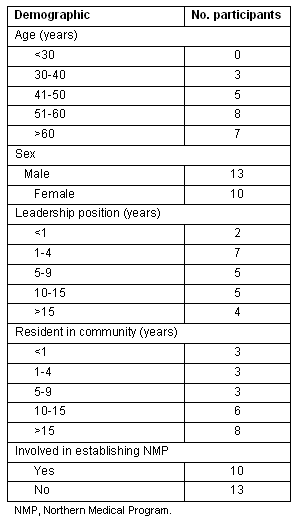

Figure 2: Semi-structured interview questions used to explore perceptions of current and anticipated impacts of the
Northern Medical Program in Prince George.
The key informant interviews were conducted in-person, and were of approximately 40 min duration. Despite reaching information saturation (n=12) after 16 interviews, the remaining seven leaders were interviewed to ensure a broad and inclusive community perspective.
All interviews were audiotaped and transcribed verbatim by the lead author and analyzed using NUD*IST v6.0 (www.qsrrinternational.com) software. Data analysis was an iterative, ongoing process that began after the first interview. Transcripts were read and re-coded several times by PT, CL and JB. Disagreements were resolved through discussion and consensus. Comprehensive 'member checking' was employed to ensure findings accurately depicted the thoughts and perspectives of participants; this included: (i) a summary document of findings sent to interviewees; and (ii) active solicitation of comments and perspectives from community leaders in attendance at the BC Rural and Remote Health Conference in Prince George22.
Initially, a descriptive content analysis based on Patton's analytic induction procedure was employed to create thematic codes23. Consistent with Carpiano's development of a resource-based conceptualization of community-focused social capital, participants' perceptions were categorized into social cohesion (connectedness, values), forms of social capital (social support, social leverage, informal social control, community organization participation), access to social capital and outcomes of social capital7. Perceptions of the impact of the NMP on particular community sectors were also coded and categorized and are discussed elsewhere by Toomey6. The perspectives of community leaders who were and were not directly involved with the implementation of the NMP were compared and contrasted. In the interests of preserving confidentiality, participants' names were replaced with an identification number. All quotes extracted from the transcript are identified by the line from which they came (ie text unit [TU]). Ethics approval was obtained from the Behavioural Research Ethics Board at UBC.
Results from this study revealed that the operation of social capital and the related concept of social cohesion are multifaceted, and that benefits extend in many directions, resulting in somewhat unanticipated benefits for other key stakeholders and network partners of this medical education program. Following Carpiano, the results are described in terms of: (i) social cohesion; (ii) social capital resources (social support, social leverage, community mobilization, social learning and communal sense of empowerment); (iii) access to social capital; and (iv) outcomes of social capital (Fig3).
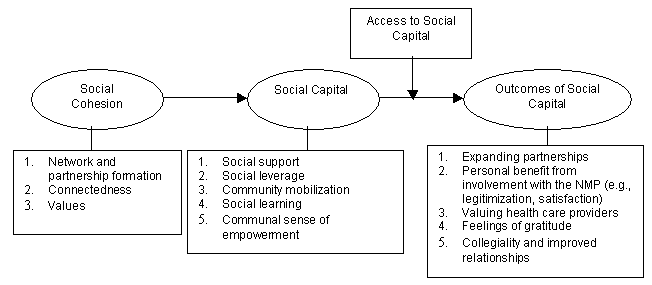
Figure 3: A schema representing the impact of the Northern Medical Program on social capital in
Prince George in the present study (modified from Carpiano's framework of neighbourhood social capital7).
Social cohesion
In this context, social cohesion manifests as a sense of connectedness and common values that characterize networks and also by the extensive formation of networks associated with the NMP. Partnerships are described at both an organizational level and a community level.
At the organizational level, partnerships formed between the administration of the NMP and the local health authority in northern BC, as well as between the Northern Medical Society (which represents local and northern physicians) and UNBC, the NMP's host university. As illustrated by the following quotes, participants describe how trust grew from the partners' common commitment to a goal for the community and how this fosters a strong network. One participant describes a sense of connectedness within the network:
I think there's a cohesive element to the Northern Medical Program. I think the whole medical community has gotten behind teaching...the [NMP] is something that helped bring Northern Health [Authority] and physicians together. Both had a common interest in making this program as successful as possible. If you have common interests it's much easier to build that common ground...working together becomes a way of being... (ID: 01, TU: 118-135).
This partnership's connectedness was made possible because members shared a common value: trust. An administrator of the Northern Medical Society believed that:
...if it wasn't for [name of NMP administrator] the NMP would have been in a shambles in three months. The northern docs decided that they could trust [name of NMP administrator] (ID: 10, TU: 337-340).
Networks at the community level were also described. Citizens of the NMP's host community of Prince George comprised one deeply connected network. Many citizens were involved in all stages of the planning and implementation of the NMP. The community's connectedness with one another was characterized by shared interest, awareness and excitement about the program: 'The engagement of ordinary citizens in this program was nothing short of astonishing. I think part of that was that people believed in [the NMP]' (ID: 10, TU: 126-132). A common value that banded Prince George citizens together was the belief in educating 'northern people for the North. That's a value that's held very deeply' (ID: 06, TU: 206-207).
Social capital
Social support: In the context of the NMP, social support was exemplified in several ways. For example, offers from Prince George citizens to help incoming NMP students and their families integrate into the community were abundant. As described by one community leader:
It was a very heart-warming thing to see. People wanted to make sure that these kids, that somebody got them out to the right restaurant in town...that they had a best-friend right away, that, if any one of them wanted to go moose hunting, there would be a line-up of trucks to take them moose hunting...anything that could be done, people were willing to do (ID: 10, TU: 135-143).
The NMP is also attracting physicians with interests in teaching. By itself, this is sufficient to make a positive impact on the local community of physicians by helping stabilize some of the specialties that had experienced chronic shortages:
I think physicians derive significant professional strength by having other individuals to share their practice, to help deal with the pressures of being on-call, and to maintain the professional stimulation ... it has an intrinsic value, having more colleagues to practice with them (ID: 11, TU: 121-127).
Moreover, the combination of teaching, academic, and clinical responsibilities that come with the NMP means that physicians who are drawn to locate in Prince George will bring a more diverse set of skills, resources and outlooks to the local professional community.
Social leverage: In the current study, 'social leverage' is illustrated by Prince George community leaders' use of their positions of leadership in society to leverage support for the medical program. One participant explained his involvement:
I mean in the early days [of the NMP planning phases]...I went across the north [of British Columbia] talking to the community and community leaders about the program, about the potential impacts, soliciting their support. First of all, I needed the political alliance to move this forward and secondly I wanted to build their interest in the [Northern Medical] program. I didn't want to create a medical school that was disconnected from the communities it serves (ID: 04, TU: 210-216).
At the local level, community leaders reported lobbying to raise money for the NMP Trust Fund, which was established to alleviate the financial burden of the NMP students. This entailed knowledge of municipal processes and making use of personal networks:
The last $300,000 [of our 2 million dollar goal] came from the city [of Prince George]. [Name] and I went up to City Council...we told them that we were at $1.7 [million] and asked them to top up. We gave a presentation, told them why we thought it was in their best interests to do that, and they agreed. It was kinda neat because we lobbied each councillor before [the meeting]... (ID: 03, TU: 412-420).
The NMP also created new opportunities for local leaders to influence central government officials (in this case, the provincial government). Due to links with the medical community, local leaders learned of the importance of postgraduate medical residency placements in recruiting and retaining recent medical graduates, particularly those trained at the NMP:
We found out that the statistics really say that about 70% of students in residency end up living and practicing in the area where they took their residency. So guess what? We got a problem here [laughter] because these kids [NMP students] are going somewhere else for their residency in a lot of the cases, and not necessarily in northern British Columbia (ID: 03, TU: 77-81).
Local leaders thus began lobbying using various NMP social functions in an attempt to influence provincial government officials to expand residency programs in the region:
...we asked [the government] for the eight additional residency spots, I think it was at the last Bob Ewart Memorial Lecture (NMP/Northern Trust fundraising event) ...one of the guests is [the] premier of the province...I asked for more residency places in the northeast and northwest and we got them (ID: 07, TU: 182-187).
Community mobilization: Community mobilization was exemplified by the formation of grassroots committees initiated in Prince George by community members to help address anticipated challenges of NMP implementation. One community-based organization formed was the fundraising committee for the NMP Trust, which was created to provide financial support to NMP students who would have to travel to outlying rural and remote communities to complete the clinical training phase of the program. One participant described the committee's work:
...we co-chaired a committee for the [Northern Medical] program to raise 2 million dollars for Prince George. That was part of a 6 million dollar goal for all northern communities [in BC], ...so our goal was to raise our 2 million and try to support the other [Northern BC] communities' effort [in fundraising]...so we did that and we actually accomplished that in 3 years and the 2 million dollars (ID: 03, TU: 6-16).
The NMP Community Action Group, consisting of various local officials, was formed to advise the program on a range of issues related to the implementation of the program and its long-term viability:
The committee, which consisted of the city manager, the mayor, sort of leaders of the community, tried to address...potential issues. A lot of it centered around fiscal issues...We talked about recruitment issues, we talked about capital plans...a variety of things over an extended period of time (ID: 13, TU: 41-49).
Social learning: While local leaders in Prince George were clearly learning firsthand about different aspects of undergraduate medical education, a two-way exchange also began to occur as medical faculty, medical students and university administrators learned more about the social realities of small towns, First Nations' reserves and resource-dependent economies of northern BC. This holds promise for enhancing trust and rapport among different populations in the region. This was most apparent in First Nations communities throughout northern BC, and among First Nations and Aboriginal individuals residing in Prince George, many of whom experience the most pressing health and social challenges in the province. As was heard from one participant:
...the feedback we're getting from ... the Aboriginal community is that there is a growing understanding about what Aboriginal people's experience is in northern British Columbia (ID: 02, TU: 226-230).
In spite of the persistence of long-standing issues of poverty, disenfranchisement, and social marginalization for many First Nations individuals and communities, there was a growing sense of optimism that the NMP model, based on a more comprehensive and community integrated approach to medicine, would lead to improved dialogue about other intractable social issues:
I think the Northern Medical Program adds...now we have people who are well-educated, they're part of the community, they have something to say...they raise issues and they talk about things in a different way...the dialogue just gets elevated...we're talking about things in a more intelligent and meaningful way (ID: 02, TU: 354-363).
Finally, for local leaders in Prince George, there was also the sense that the NMP has opened up a greater dialogue with, and understanding from, leaders of the UBC Faculty of Medicine based in the populous centres in BC's lower mainland:
When they were training doctors only in the larger centres like Vancouver...I don't think they ever really gave it a thought, as to what situations were actually being dealt with by physicians in the outlying areas...but when they're actually involved...with the administration of the [NMP]...they're going to start rectifying some of the inequities. Even in Vancouver, not only will we bring some Vancouver culture here, but in fact some of the cultural benefits of the north will be transposed to the south (ID: 21, TU: 280-296).
Communal sense of empowerment: The NMP has contributed to enhancing a sense of positive self-image and collective self-esteem in Prince George:
I think [the NMP] is about how a community views itself. I think when you're a community that's training physicians, that changes even your own sense of who you are (ID: 03, TU: 117-125).
Many individuals described a collective sense of accomplishment and optimism resulting from the implementation of the NMP. One community leader described his feeling by reflecting on a 'health crisis rally' held by community members in Prince George prior to the implementation of the NMP to protest the state of health care in the north:
...the thousands of people that went to that rally, they felt they had an impact, finally! They feel good about it. It is brought up [in conversation]. You know, people say 'We made [the NMP] happen'. Just like we made the University [of Northern BC] happen, we made the medical school happen. So you know, as individuals, you can do something if you work collectively (ID: 02, TU: 128-135).
As described by another study participant: ...the Northern Medical Program...has, I think, enabled the community to take more of a futuristic focus rather than a 'cup half empty', 'it's all bad', and 'we don't have enough practitioners in the north' focus. [The NMP] has allowed a more 'we can do something about this [physician workforce and access to health care]' perspective in the community (ID: 06, TU: 107-111).
Or, as one local leader put it: 'The NMP has certainly made us feel better about ourselves. There can't be too much wrong with us if we can have a medical school...' (ID: 13, TU: 216-219).
Local leaders were keenly aware of the importance of making sure the NMP is successful. Failure of the program, for them, would equate to failure of the local environment as a destination for innovation:
[the NMP] means a lot just in terms of the credibility of the north and these communities. The fact that we can have a program of this sophistication operate here successfully does legitimize other potential opportunities (ID: 08, TU: 167-170).
Having learned much from the various efforts on behalf of the program, and having widened their personal networks to include influential offices of higher education and provincial government, local leaders were anxious to continue to secure new resources, programs, and technologies for the benefit of the community.
Access to social capital
Bourdieu's theory of social capital emphasizes that the resources possessed within a network are only as good as the ability of network members to access them12. In the present study, access to social capital was illustrated in the context of access to knowledge and social learning. Many participants perceived that knowledge gained as a result of NMP implementation might be confined to members of more elite networks in the community, with ordinary citizens not benefitting as they should. This was particularly apparent in participants' descriptions of how NMP involvement has increased their awareness of the medical education process and the likelihood that NMP-trained physicians will remain in the region on graduation, given that many students have to leave the region to complete post-graduate residency training.
To this effect, participants believed that lines of communication between community leaders and the general public needed to be further opened to curb citizens' expectations of future physician workforce gains in the region and to minimize potential disappointment. One leader explained:
It's going to be partially an education thing, where we will have to explain to people that a lot of [NMP students] when they graduate will go elsewhere...maybe they've finished their [medical doctor degree], they're not gonna specialize, so they're leaving the region. We're going to have to have something in place, in terms of tracking [NMP students] over the next 40 years...There's going to be a real expectation on May 10th [2008, when the first cohort of NMP students graduates]...(ID: 15, TU: 554-568).
As explained by another participant:
The people 'in the know' understand it. I don't think the general public understands it. I mean, we didn't understand it until we got involved...you know, to understand what [medical]residencies were, and how important they are, you know that's nebulous to a lot of people. You know that doctors go to school for a long time...but lots of other things decide where they will practice (ID: 03, TU: 167-174).
Outcomes of social capital
Diverse outcomes of social capital emerged from the interview data. For the community leaders closely involved in securing and supporting the NMP, there were obvious personal and professional benefits that accrued from these efforts. In particular, to the extent that a member of this network is regarded to have played a positive role in establishment of the NMP, they stand to enhance their own reputation as a leader in their field. But there were clear indications that the outcomes of these activities have benefits beyond the immediate networks of local power. Expanding partnerships and bridging within and among groups was a pervasive theme. The creation of formal, professional networks to address issues around the NMP appeared to have laid the foundation for the development of informal, personal relationships (eg between NMP students and community leaders). Network expansion was further believed to promote community involvement and volunteerism by NMP students, the creation of professional medical networking opportunities for NMP students with community physicians, and research partnerships and links between the health and education sectors. Additional outcomes of social capital included personal satisfaction from involvement with the NMP, the valuation of healthcare providers and community organizations, feelings of gratitude toward the program, and improved collegiality, particularly between the local medical community and the Northern Health Authority.
Findings from this study suggest that the partnerships and networks formed in the NMP planning and implementation phases were in fact the foundation for social capital mobilization (ie productive resources being drawn upon to achieve collective goals). These results support previous findings that a key early impact of the NMP was the degree of partnership formation noted in the wider community5.
The extensive formation of new partnerships and networks in the context of the NMP reflects the degree of social cohesion in the community. It is clear that social cohesion did not solely manifest as the common values and connectedness which characterize a network. It is also reflected in the shear abundance of networks and connections already in place prior to the arrival of the NMP, which laid the groundwork for future creation of social capital18. Accordingly, the program and its key stakeholders (ie students, faculty, administrators, funders) were as much the beneficiaries of social capital mobilization as were members of the wider community hosting the program.
As described elsewhere, participants' ties with multiple community sectors and the overlap between their personal and professional interactions reflect the multilayered relationships in the NMP community6. Bourdieu explained that each member of a network contributes the social capital s/he possesses to the group12. Each network member also has access to the social capital contributed by all other group members. Therefore, if an individual belongs to several networks, s/he can utilize the social capital of one group to serve the purposes of a second group, leading to infinite social capital potential in a given community. In this context, the NMP's success in the early planning and implementation phases was likely to be due, in part, to its ability to capitalize on existing social capital and social cohesion in the host community; its continued success appears to have stemmed from the subsequent proliferation and mobilization of social capital.
The use of Carpiano's spatially-bounded model of social capital was adaptable, applicable and useful in this context because it permitted characterization of the relationships and networks within a tight-knit community body7. Following Carpiano, it was found useful to differentiate between social capital (ie the productive resources potentially or actually present in a given network) and social cohesion (ie the network ties of trust, familiarity, and shared values that allow for social capital mobilization)7. This conceptualization of social capital formation was helpful to advancing the present understanding of the breadth and interconnectivity of a local network mobilized to establish, administer and sustain this medical education program.
Limitations
A limitation of the current study concerns the degree to which the perceptions of participants represent those of the general community. As Baum noted in his study of community-university partnerships, community leaders in positions of power may only speak for a few24. However, soliciting the perspectives of community leaders is important for studies evaluating community-wide impact. Goodman suggested leaders are important because they direct local service organizations, understand local processes and machinations of power, and have an important influence on local public opinion, allocation of resources, and policy development25. Because many community leaders in Prince George were involved in supporting the NMP, every attempt was made to obtain a sample of community leaders from a wide range of community sectors and to include individuals who were not directly involved with the implementation of the NMP.
Future research
Further theorizing around the role of the NMP in influencing social capital is needed. The perceptions of several participants regarding differential access to social capital in the community necessitates further exploration in terms of: (i) elucidating the types of social capital resources possessed by different networks; (ii) access to social capital; and (iii) the way in which these resources are shared and propagated within and between networks. Future research into the outcomes of social capital is also warranted to adequately assess the broader, community-wide impacts of the NMP on its host community of Prince George as the program matures.
Community benefits from the Northern Medical Program
The social cohesion present among community leaders in Prince George played an important role in the networking efforts undertaken to secure the program, and in the ability of NMP directors to continue to draw widely on local productive talents and capacities in the program's formative years. The students, faculty and administrators of the NMP have benefitted greatly from access to the social capital mobilized to make the NMP operational. Undoubtedly, local leaders have themselves received tangible benefits as a result of the part they played, or more importantly were perceived by others in the community to play, in efforts to establish and implement the NMP (eg enhancing their local standing, legitimizing their authority, broadening the pool of social and other forms of capital available to them for use in other realms of activity). However, it is evident that the NMP represented a unifying cause that local leaders took up to leverage additional local and non-local resources. Taking account of the dynamic, multifaceted and recursive operation of social capital helps one move beyond a view of geographic communities as simply containers or sinks of capital investment, and to appreciate the degree to which they (capital investment) may act as a platform for productive network formation and expansion.
Acknowledgements
The authors thank the participants interviewed in this study for their contribution. Also thanked are Dr Daniel Pratt for his consultation regarding the interview procedures, and Ms Joan Gray for her editorial assistance. This study was partially supported by the Evaluation Studies Unit, University of British Columbia, Faculty of Medicine. Grant support for this research was provided by the Canadian Institutes of Health Research (CIHR) Canada Graduate Scholarship - Master's Award (Project Grant #17W33879).
References
1. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 9: 1060. (Online) 2009. Available: www.rrh.org.au (Accessed 10 October 2011).
2. Ricketts TC. The changing nature of rural health care. Annual Review of Public Health 2000; 21: 639-657.
3. Smith KB, Humphreys HS, Wilson MG. Addressing the health disadvantage of rural populations: how does epidemiological evidence inform rural health policies and research? Australian Journal of Rural Health 2008; 16: 56-66.
4. Curran V, Rourke J. The role of medical education in the recruitment and retention of rural physicians. Medical Teacher 2004; 26: 265-272.
5. Lovato C, Bates J, Hanlon N, Snadden D. Evaluating distributed medical education: What are the community's expectations? Medical Education 2009; 43: 457-461.
6. Toomey PC. Evaluation of the Northern Medical Program on the community: perceptions of local leaders (MSc thesis). University of British Columbia, Canada, 2008.
7. Carpiano RM. Toward a neighborhood resource-based theory of social capital for health: can Bourdieu and sociology help? Social Science and Medicine 2006; 62: 165-175.
8. Islam MK, Merlo J, Kawachi I, Lindstrom M, Gerdtham U-G. Social capital and health: does egalitarianism matter? A literature review. International Journal of Equity in Health 5: 3. (Online) 2006. Available: http://www.equityhealthj.com (Accessed 10 October 2011).
9. Kawachi I, Kennedy BP, Lochner K, Prothrow-Stith P. Social capital, income inequality and mortality. American Journal of Public Health 1997; 87: 1491-1498.
10. Lomas J. Social capital and health: implications for public health and epidemiology. Social Science and Medicine 1998; 47: 1181-1188.
11. Portes A. The two meanings of social capital. Sociological Forum 2000; 15: 1-12.
12. Bourdieu. P. The forms of capital. In: J Richardson (Ed.). Handbook of theory and research for the sociology of education. New York: Greenwood, 1986; 241-258.
13. Coleman JS. Social capital in the creation of human capital. American Journal of Sociology 1988; 94: S95-S120.
14. Putnam R. Bowling alone: the collapse and revival of American community. New York: Simon and Shuster, 2000.
15. Bates J, Casiro O, Fleming B, Frinton V, Towle A, Snadden D. Expanding medical undergraduate education in British Columbia: a distributed campus model. Canadian Medical Association Journal 2005; 173: 1-7.
16. Statistics Canada. Community Profiles: Prince George; 2001 Census Data. Ontario: Statistics Canada, 2002.
17. Ahern MM, Hendryx M. Social capital and trust in providers. Social Science and Medicine 2003; 57: 1195-1203.
18. Hanlon N, Halseth G, Snadden D. "We can see a future here:" Place attachment, professional identity, and forms of capital mobilized to deliver medical education in an underserviced area. Health and Place 2010; 16: 909-915.
19. Hanlon N, Ryser L, Crain J, Halseth G, Snadden D. Establishing a distributed campus: Making sense of disruptions to a doctor community. Medical Education 2010; 44: 256-262.
20. Hendryx MS, Ahern MM, Lovrich NP, McCurdy AH. Access to health care and community social capital. Health Services Research 2002; 37: 85-101.
21. Kilpatrick S, Cheers B, Gilles M, Taylor J. Boundary crossers, communities, and health: exploring the role of rural health professionals. Health and Place 2009; 15: 284-290.
22. Creswell JW, Miller DL. Determining validity in qualitative inquiry. Theory into Practice 2000; 39: 124-130.
23. Patton M. Qualitative research & evaluation methods (3rd edn). Thousand Oaks, CA: Sage, 2002.
24. Baum H. Fantasies and realities in university-community partnerships. Journal of Planning Education and Research 2000; 20: 234-246.
25. Goodman R, Wandersman A, Chinman M, Imm P, Morrissey E. An ecological assessment of community-based interventions for prevention and health promotion: approaches to measuring community coalitions. American Journal of Community Psychology 1996; 24: 33-61.


