The highest rates of child mortality continue to be found in sub-Saharan Africa, with the region accounting for half of the 8.8 million under-five year-olds' deaths globally in 20081. Kenya is one of the countries in the region with high under-five mortality rates (defined as ≥40 deaths per 1000 live births). According to the 2008-2009 Kenya Demographic and Health Survey, the country's under-five mortality was 74 deaths per 1000 live births while the disaggregated data revealed a significantly higher mortality rate in rural compared with urban areas2. These findings reflect the Kenyan and other sub-Saharan African countries' concern regarding the achievement of the UN Millennium Development Goal (MDG) 4, which aims to reduce under-five mortality by two-thirds by 20151. The Government of Kenya recognizes the need to address urban-rural disparities in order to fast track the progress toward achieving the MDGs by 2015. As part of the National Development Agenda - Kenya Vision 2030, one of the health sector objectives under the First Medium-term Plan (2008-2012) is to reduce under-five mortality from 120 to 33 per 1000 live births3.
Previous research has shown that various factors influence child health and survival, including place of residence, breastfeeding, place of delivery, access to postnatal care, and maternal age and education4-11. Geographic differences in maternal literacy levels and sociocultural practices are linked to the variations in child mortality rates within countries8. Evidence shows that breastfeeding, particularly in the first 6 months of a child's life, is critical for child survival because of the associated benefits, including a reduction in the risk of diarrheal diseases10,11. The likelihood of under-five mortality has also been linked to place of delivery, with evidence indicating that women who deliver at health facilities have a lower probability of reporting child death compared with those delivering in home settings4-12. These differences have largely been driven by the use of skilled delivery care at health facilities compared with the deliveries that occur at home, which in most cases are not attended to by skilled birth attendants. Conversely, studies conducted in Nigeria and South Africa found that place of delivery did not have an effect on perinatal and under-five mortality12,13. Access to postnatal care has also been associated with a reduction in under-five mortality, with a study in Bangladesh showing that postnatal home visits within the first 2 days after birth by skilled healthcare workers was significantly associated with a lower likelihood of child death14.
Studies conducted in the developing countries have found that maternal education and age are important determinants of child mortality4,10-12,15-17. Evidence shows that child mortality rates are higher among less educated mothers compared with mothers who have higher levels of education11,12,15,16. The importance of maternal education is based on the fact that education increases a mother's level of knowledge and skills, thus enabling her to effectively understand and utilize available information and resources critical for child health and survival. With regard to maternal age, previous studies have found this to have a significant effect on child mortality, with a higher risk of child death at young and old maternal ages4,10,17.
Other factors that have been found to have an effect on under-five mortality include birth order, sex of child and household socioeconomic status10,11,15,17-21. Previous findings on the effect of birth order were mixed, with some studies reporting that higher order births were associated with increased risk of under-five mortality10,17,18 but others finding no influence on child mortality15,19. With regard to the sex of child, a study in Malawi did not find a significant effect on child mortality10. In Kenya, a study in Nairobi slums showed that male children were significantly more likely to die than female children20. However, findings from a study conducted in India suggested that male children were less likely to die early than female children11.
The effect of household socioeconomic status on child mortality has also been examined by previous studies4,17,21. Existing evidence from studies conducted in the developing countries suggest that poverty is an underlying factor in many cases of child deaths4,21. A study using the 2008 Nigeria Demographic and Health Survey found higher odds of child death among the poorest households compared with the richest households in rural Nigeria4. However, a national study conducted in Tanzania did not find a significant effect of household socioeconomic status on infant and child mortality17.
The objective of this study was, therefore, to compare the influence of geographical location (province of residence) and key maternal factors on the probability of death before the age of 5 years among children in rural and urban areas in Kenya.
Study design and sampling
The study was based on the national cross-sectional demographic and health survey (KDHS) conducted in Kenya from 2008 to 20092. The KDHS collects nationally-representative data on women of child-bearing age (15-49 years) and their children. The sample frame included a total of 400 primary sampling units across the 8 provinces. Multi-stage cluster sampling was used to select 8444 women across the 8 provinces of Kenya with stratification for rural and urban residence. The study included a total of 16 612 children born in the 5 years preceding the survey.
Measures
The outcome variable was the risk of all-cause under-five mortality. This included all deaths among children aged 0-59 months born to mothers in the study. The period of inclusion spanned the 5 years preceding the date of interview. The risk factors examined in the study were selected based on scientific literature and included sex of child; age of mother, grouped as 15-20, 21-27, 28-31, and ≥32 years; mother's level of education, categorized as ≤ primary education, and ≥ secondary education; birth order of child grouped as 1, 2-3, or ≥4; household wealth categorized in low, middle and high tertiles; geographical province of residence (Nairobi, Central, Rift Valley, North Eastern, Coast, Nyanza, Western and Eastern); duration of breastfeeding categorized as <6 months, 6-12 months and >12 months; place of delivery (home, public health facility or private health facility) and postnatal visit 2 months after delivery (no or yes). The wealth tertiles were derived from an index computed using data on the ownership of consumer goods, dwelling characteristics, type of drinking water source, toilet facilities and other characteristics that relate to a household's socioeconomic status2. The variables on breastfeeding, place of delivery and postnatal visits were selected to examine some aspects of the child care and health seeking behavior of mothers in rural and urban areas. The enumeration areas were classified as urban or rural in the KDHS according to the national definition which includes a set of criteria on population density and availability of specific socioeconomic activities in the area2.
Data analysis
The differences in frequency of all-cause under-five mortality between rural and urban areas were assessed using bivariate (Pearson's χ2) analysis, and multivariate Cox proportional hazards regression was used to simultaneously investigate the effects of the demographic, geographic and maternal factors on survival rates. In the regression model, risk factors were included based on the likelihood of an association with childhood survival seen from a literature search and their level of statistical significance (p<0.25) from the bivariate analysis. Separate models were fit for the overall sample as well as rural and urban residents, and the relative effects were expressed as hazard ratios and the corresponding 95% confidence intervals.
Ethical considerations
The study involved secondary analysis of data from the 2008-2009 KDHS which excluded participant identifiers. The protocol for the KDHS had been previously approved by the Scientific and Ethical Review Committee of Kenya Medical Research Institute.
Bivariate analysis of risk factors for under-five mortality
The results of the bivariate analysis of risk factors for under-five mortality in rural and urban areas are shown (Table 1). Mortality among under-5 children was more frequent among rural mothers aged above 21 years compared with mothers of the same age range in urban areas. Similarly, deaths among under-five children differed significantly with the level of maternal education in rural areas compared with urban areas (p<0.001). The association of sex of child with under-five mortality was not significantly different in either residence location. The proportions of under-five deaths that included children of a birth order of 2 or higher were higher than those for similar children in urban areas (p<0.001).
Table 1: Selected characteristics of under-five mortality cases in rural and urban Kenya
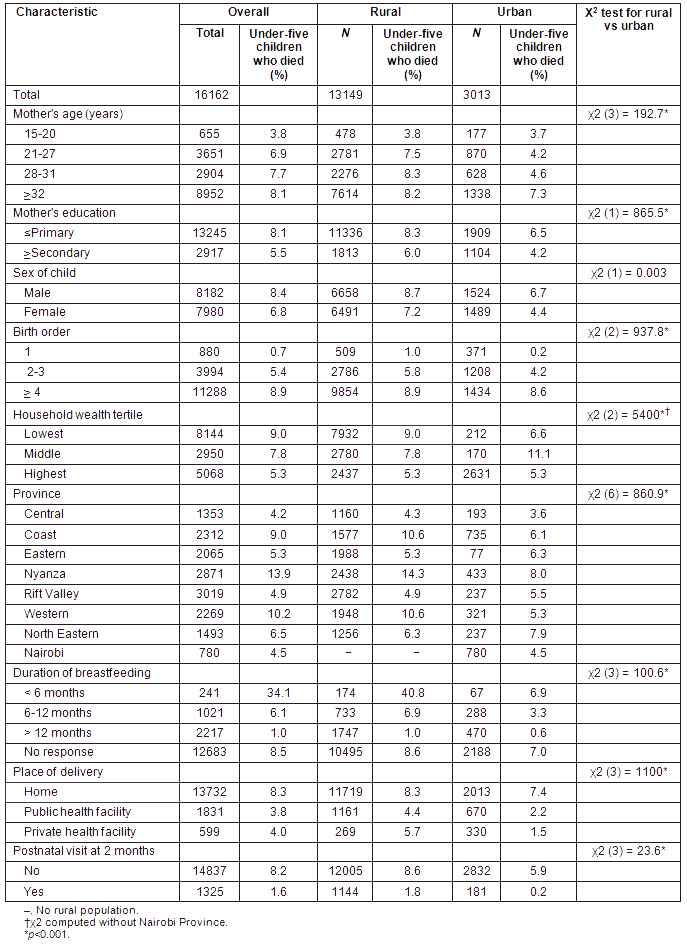
Among the deaths in rural areas, the proportion in households in the lowest wealth tertile was higher than in this category of households in the urban areas. High prevalence of under-five deaths was seen in the rural areas in the Coast, Nyanza and Western provinces, and in the urban areas of Nyanza Province. The prevalence of under-five deaths was higher in rural areas compared with urban areas when the child had been breastfed for less than 6 months, delivered at home, or not been taken for a postnatal check 2 months after birth.
Multivariate analysis of risk factors for under-five mortality
The results of the multivariate analysis of risk factors for under-five mortality in Kenya are shown (Table 2). In the model using the overall sample, place of residence was a significant (p<0.05) determinant of under-five mortality as seen in the hazard ratio of 3.6 for rural areas compared with urban areas.
Table 2: Hazard ratio estimates for determinants of under-five mortality in rural and urban Kenya
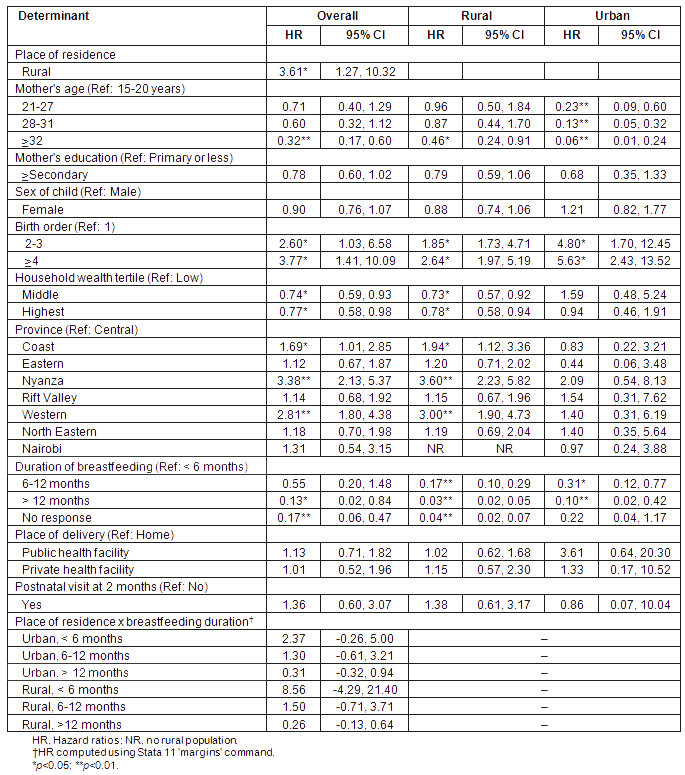
Overall, maternal age was a significant determinant of under-five mortality, with the highest likelihood of survival among children of mothers aged 32 years or more (p<0.01). This effect was seen in the overall sample as well as the rural and urban areas.
In both rural and urban areas, attainment of secondary education or higher by mothers and the sex of child were not significant determinants of under-five mortality. Higher birth order was significantly (p<0.05) associated with an increased likelihood of mortality in the overall sample but this result was only significant (p<0.05) in the urban areas.
Household wealth in Kenya was a significant (p<0.05) determinant of under-five mortality. In rural areas, households with greater wealth were less likely to have under-five deaths compared with the poorest households. This relationship was not seen among the urban households.
Among the geographic provinces of Kenya, Coast, Nyanza and Western had significantly greater likelihood (p<0.05) of under-five mortality compared with Central Province. When disaggregated by place of residence, this association was only seen in the rural areas in the 3 provinces. The place of delivery of the child and postnatal visit to a health facility 2 months after delivery were not significantly associated with under-five mortality in rural and urban areas in Kenya.
The influence of breastfeeding on the likelihood of under-five mortality was similar in rural and urban areas, with children who were breastfed for more than 6 months having significantly lower probability (p<0.05) of mortality than children breastfed for less than 6 months. In the model using the overall sample, there was no significant interaction between place of residence and duration of breastfeeding although the higher likelihood of mortality among rural children breastfed for less than 6 months was seen compared with urban children.
Discussion
This study compared geographic and maternal factors associated with under-five mortality in rural and urban areas of Kenya. It was found that the likelihood of mortality among under-five children was higher in rural areas compared with urban areas. This disparity, which has been observed in national surveys and studies in Kenya and other sub-Saharan countries2,13,16,22,23, has been ascribed to inequities in location, socioeconomic factors, sociocultural beliefs and practices, and individual level risk factors in these populations4,5. The results of the present study suggest that the probability of mortality within the first 5 years of life is associated with province of residence for rural children, but not for urban children. The association of under-five mortality with maternal variables, namely duration of breastfeeding, place of delivery and postnatal visit 2 months after delivery, was similar for both rural and urban children. The results of the multivariate analysis highlight differences in risk factors for under-five mortality between rural and urban areas in Kenya.
A lower likelihood of under-five mortality associated with older mothers was seen in both urban and rural areas, although this was significant at age 32 years or above among rural women compared with age 21 or above among urban women. This is consistent with other studies and may suggest that levels of awareness of child health care are greater among the more educated younger mothers in the urban areas in Kenya11,12,15,16. Younger mothers may also not be socially and psychologically mature enough to deal with the requirements of infant and child care, or they may lack the domestic decision-making authority that older mothers may have24. The absence of a relationship between maternal educational attainment and mortality in both rural and urban areas of Kenya is surprising, given the evidence in literature of lower child mortality rates being associated with higher maternal education11,12,15,16. However, in both areas the odds ratios were indicative of a lower risk of child mortality among mothers with higher education, although these were not statistically significant.
The risk of death of under-five female children was not significantly different from that of male children in both rural and urban areas. This is different from a trend reported in many national surveys and studies in sub-Saharan Africa, which show greater mortality rates among male children25-27. Similarly, the association of higher-order births with higher child mortality as reported in other studies in sub-Saharan Africa was found in both rural and urban areas in Kenya10,19. The likelihood of death among children in households in the middle and highest (wealthiest) tertiles of wealth was lower than that in households in the lowest (poorest) tertile in rural areas. However, this association was not observed among households in urban areas. This suggests that the differences in household wealth may have greater implications for population health outcomes in rural areas compared with urban areas in Kenya.
The province of residence was also significantly associated with under-five mortality. The high likelihood of under-five mortality in both rural and urban areas in Nyanza Province has been previously reported and may be attributed to a number of factors, including high HIV prevalence (at 14% this is more than double the national rate of 6.3%) and a high proportion of teenage pregnancies2. The rural areas in Coast and Western provinces had significantly higher under-five mortality than those in Central Province. The ethnocultural composition of these provinces may underpin the differences in likelihood of under-five mortality observed. Studies have shown that child mortality is lowest among the Kikuyu, who reside mostly in Central Province, compared with other ethnic groups18. Other factors that may underlie these observed outcomes include a higher proportion of the population in Central Province within the highest three wealth quintiles, and with higher literacy levels compared with other provinces2.
Of the maternal factors examined in this study, only the duration of breastfeeding was a significant risk factor for under-five mortality. Numerous studies show that children breastfed for less than 6 months are at greater risk of death compared with those fed for longer periods8,28. This effect was not different in rural and urban areas of Kenya even after controlling for various sociodemographic characteristics. The place of delivery and the postnatal visits 2 months after delivery were not significantly associated with under-five mortality in both rural and urban areas in Kenya although the association of these variables with perinatal mortality is well documented13.
A limitation of this study is the retrospective nature of the DHS data. This introduces recall bias in the reporting of events over the preceding 5 year period. In addition, the place of residence of some respondents at the time of the survey may have changed over the period from the date of birth of the child.
This study adds to understanding of the drivers of under-five mortality in rural and urban areas of Kenya. The evidence of greater risk of mortality associated with younger mothers, poorer households, inadequate breastfeeding and specific geographic provinces underscores the need to tailor interventions to address these factors in rural areas. The absence of policies aimed at reducing socioeconomic inequalities between rural and urban areas would likely reduce the impact of public health interventions in improving child health and survival in Kenya.
References
1. United Nations. The Millennium Development Goals Report. New York: UN, 2010; 1-77.
2. Kenya National Bureau of Statistics, ICF Macro. Kenya Demographic and Health Survey 2008-09: Calverton, MD: KNBS and ICF Macro, 2009.
3. Office of the Prime Minister Ministry of State for Planning National Development and Vision 2030. First Medium-Term Plan (2008-2012). Nairobi, Kenya: Ministry of State for Planning, National Development and Vision 2030, 2008.
4. Doctor HV. Does living in a female-headed household lower child mortality? The case of rural Nigeria. Rural and Remote Health 11: 1635. (Online) 2011. Available: www.rrh.org.au (Accessed 23 January 2012).
5. Swenson IE, Nguyen MT, Pham BS, Vu QN, Vu DM. Factors influencing infant mortality in Vietnam. Journal of Biosocial Science 1993; 25(3): 285-302.
6. Teka T, Faruque ASG, Fuchs GJ. Risk factors for deaths in under-age-five children attending a diarrhoea treatment centre. Acta Paediatrica 1996; 85: 1070-1075.
7. Edmond KM, Zandoh C, Quigley MA, Amenga-Etego S, Owusu-Agyei S, Kirkwood BR. Delayed breastfeeding initiation increases risk of neonatal mortality. Pediatrics 2006; 117: e380-e386.
8. Black RE, Morris SS, Bryce J. Where and why are 10 million children dying every year? Lancet 2003; 361(9376): 2226-2234.
9. Jones G, Steketee RW, Black RE, Bhutta ZA, Morris SS. How many child deaths can we prevent this year? Lancet 2003; 362(9377): 65-71.
10. Manda SO. Birth intervals, breastfeeding and determinants of childhood mortality in Malawi. Social Science & Medicine 1999; 48(3): 301-312.
11. Nath DC, Land KC, Singh KK. Birth spacing, breastfeeding, and early child mortality in a traditional Indian society: a hazards model analysis. Social Biolology 1994; 41(3-4): 168-180.
12. Worku Z. Factors that affect under-five mortality among South African children: analysis of the South African Demographic and Health Survey Data Set. Proceedings of the World Congress on Engineering and Computer Science 2009; 2: 1-3.
13. Oti SO, Odimegwu C. Perinatal mortality in Nigeria: do place of delivery and delivery assistants matter? Open Demography Journal 2011; 4: 1-10.
14. Baqui AH, Ahmed S, Arifeen EL. S, Darmstadt GL, Rosecrans AM, Mannan I et al. Effect of timing of first postnatal care home visit on neonatal mortality in Bangladesh: a observational cohort study. BMJ 2009; 339: b2826.
15. Deribew A, Tessema F, Girma B. Determinants of under-five mortality in Gilgel Gibe Field Research Center, Southwest Ethiopia. Ethiopian Journal of Health Development 2007; 21(2): 117-124.
16. Houweling TA, Kunst AE, Moser K, Mackenbach JP. Rising under-5 mortality in Africa: who bears the brunt? Tropical Medicine and International Health 2006; 11(8): 1218-1227.
17. Mturi AJ, Curtis SL. The determinants of infant and child mortality in Tanzania. Health Policy Planning 1995; 10(4): 384-394.
18. Brockerhoff M, Hewett P. Inequality of child mortality among ethnic groups in sub-Saharan Africa. Bulletin of the World Health Organisation 2000; 78(1): 30-41.
19. Ronsmans C. Birth spacing and child survival in rural Senegal. International Journal of Epidemiology 1996; 25(5): 989-997.
20. Mutisya M, Orindi B, Emina J, Zulu E, Ye Y. Is mortality among under-five children in Nairobi slums seasonal? Tropical Medicine and International Health 2010; 15(1): 132-139.
21. Lawn JE, Cousens S, Zupan J. 4 million neonatal deaths: When? Where? Why? Lancet 2005; 365: 891-900.
22. Ghana Statistical Service, Ghana Health Service, ICF Macro. Ghana Demographic and Health Survey 2008. Accra, Ghana: GSS, GHS, and ICF Macro, 2009.
23. National Population Commission (Nigeria), ICF Macro. Nigeria Demographic and Health Survey 2008. Abuja, Nigeria: NPC and ICF Macro, 2009.
24. Alam N. Teenage motherhood and infant mortality in Bangladesh: maternal age-dependent effect of parity one. Journal of Biosocial Science 2000; 32(2): 229-236.
25. Hill K, Upchurch DM. Gender differences in child health: evidence from the demographic and health surveys. Population and Development Review 1995; 21(1): 127-151.
26. Nielsen BB, Liljestrand J, Hedegaard M, Thilsted SH, Joseph A. Reproductive pattern, perinatal mortality, and sex preference in rural Tamil Nadu, south India: community based, cross sectional study. BMJ 1997; 314: 1521-1524.
27. Victora CG, Wagstaff A, Schellenberg JA, Gwatkin D, Claeson M, Habicht JP. Applying an equity lens to child health and mortality: more of the same is not enough. Lancet 2003; 362: 233-241.
28. Edmond KM, Zandoh C, Quigley MA, Amenga-Etego S, Owusu-Agyei S, Kirkwood BR. Delayed breastfeeding initiation increases risk of neonatal mortality. Pediatrics 2006; 117(3): e380-386.
