In contrast to the principles of WHO's Safe Motherhood Initiative1, hospital deliveries only account for a minority of births in many regions of Sub-Saharan Africa (SSA). As a consequence, maternal mortality rates (MMR) are among the highest in the world, comparing unfavourably with other regions that have relatively constrained resources, such as South-East Asia and South America2. In Kenya the 2008 MMR was estimated at 413 deaths per 100 000 births. In common with other regions of Africa, the minority of births are in Kenya hospital deliveries. The Kenya Demographic and Health Survey reported that children born in rural areas are twice as likely to be born at home than urban children3. The national average for hospital deliveries is 40%, while in Msambweni District, the rural area where the present study was conducted, only 18% of children are born in clinical facilities. The MMR for the District is 650 per 100 000 births4.
The majority of maternal deaths in SSA are associated with birth complications related to lack of trained supervision at delivery, with only 10% of maternal deaths attributable to infection or disease2. Factors associated with unsupervised deliveries include the education level and wealth of the mother, with 84% of children whose mothers have no education being born at home, compared with 30% of those whose mothers have secondary education.
Controlled hospital environments, hygienic conditions, skilled personnel and the availability of resources to manage possible complications are considered corner-stones for the achievement of safe motherhood. Despite support for this health message by Ministry of Health guidelines and international programs such as the United Nations Development Programme (UNDP), United Nations Children Fund (UNICEF) and the Centres for Disease Control and Prevention (CDC), there is little evidence of fundamental change in Kenyan maternal health statistics in the past decade3.
Identifying community attitudes and current practices are an important starting point for behaviour change5. The purpose of this study was therefore to identify perceived and actual barriers to the uptake of hospital care at community level, in order to identify points of intervention to improve the use of safe motherhood services in area studied and similar communities.
Study site
The current study took place in 2008 and 2010 in the catchment area of Msambweni District Hospital (MDH), the main tertiary care facility in Msambweni District. There are 12 other health centres with delivery facilities in the district, but no community-based midwife service; all skilled-attended births take place in health facilities. Msambweni District is located on the south coast of Kenya on the Tanzanian border. It has an estimated population of 283 658, with a doctor : population ratio of 1:76 741 and a nurse/population ratio of 1:20476. Healthcare professionals are often posted from areas outside the community in which they serve and may not, therefore, belong to the same ethnic or language group as their patients.
Fourteen of the 65 nurses working in MDH are assigned to the 40 bed maternity ward, amounting for 1-2 nurses on duty per shift. Delivery charges at the hospital are comparatively low, with a normal delivery costing KES 850 (US$11) compared with private hospitals in the region that charge KES 6,000 (US$75). Mothers who come for antenatal care are given information on reproductive and child health in daily health talks at the mother-child health clinic. Families attending are also provided with insecticide treated mosquito nets free of charge.
The community is largely rural with the main income source being cash crops (coconuts, bixa, oranges, cassava, mangoes and cashew nuts) grown beside food crops for family consumption. Employment opportunities are limited and include tourism, transport, and animal husbandry. While the majority religion is Islam (75%), the population also includes a significant Christian minority, as well as those who believe in ancestral gods. Alternative health care is widely accessible from various types of medicine men7, with traditional birth attendants (TBA) present at most home deliveries.
Procedures
The current study was conducted in the context of a larger program sponsored by the National Institutes of Mental Health entitled HIV, Malaria and Neurobehavioral Development in Early Childhood (MH80601). The larger program is an observational study investigating the link between features of maternal health in pregnancy and infant outcome at the age of 2 years. To facilitate sample collection, mothers volunteered to deliver in hospital and were provided with financial and logistical support to do so (including payment of hospital fees and provision of transport to hospital delivery in a project vehicle). This sub-study carried out a situational analysis of factors affecting participation in the main study program.
Data source
Data for the study were obtained from group discussions (2-21 August 2008), and structured interviews (24 May to 7 June 2010). Participant observations involved attending health management team meetings at MDH. Notes taken at the meetings helped obtain a clear understanding of healthcare provision system in the district and hospital.
A total of 12 group discussions were held. The first six meetings were held with 12 hospital staff of mixed sex and cadre. A facilitator and two note-takers attended each meeting. Each group was asked to discuss the question: What factors do you think prevent mothers from delivering in hospital?.
Meetings were then held with six community groups, attended by a total of 90 community members (36 males, 54 females) aged between 20 and 60 years. Meetings were of both mixed- and single-sex participants. The purpose of these meetings was to sensitize the community to the forthcoming study. Each group was presented with the main question for discussion. The group was then asked to consider the responses of the hospital staff groups, and community agreement or disagreement with each potential barrier was established. Other potential barriers were also elicited. Responses from the groups were recorded by hand and summarised by two team members [GB & PH].
Subsequently, structured interviews were conducted with individual mothers who had been recruited to deliver in hospital but had failed to do so. The interview sought to obtain the reasons for expectant mothers failing to take advantage of a supervised delivery, despite the opportunity provided by study membership.
Tool and interview
A structured interview schedule was developed through an iterative process. A sociology student independent of the study team devised the initial interview schedule and modified it according to discussion with the study team. The schedule was piloted on 10 mothers. The interview was carried out in Kiswahili; however, for mothers who preferred to respond in the local language Kidigo, a member of the local community acted as interpreter. Of the 298 participants identified as having delivered by end of May 2010, 39 deliveries (13%) occurred at home. Data collected was collated to identify common responses among respondents, and underlying themes.
Analysis
Themes were sought that: (i) summarised the nature of the barrier; and (ii) identified the target for an intervention to overcome the barrier. Two authors [FK & PH] independently derived themes from responses, and final themes were reached by consensus. Finally, the experience of mothers who had failed to deliver in hospital was summarised by all authors, and compared to these themes.
Ethics approval
Ethical Approval was obtained from The Kenya Medical Research Institute National Ethics Committee, and written, informed consent was obtained from study participants.
Responses to the group discussions are summarized in thematic categories (Table 1). While economic barriers were a major concern for all groups, other issues were also commonly raised, forming the basis for identified themes. These themes have been labelled 'resources' (individual and community); 'customer care' (aspects of care within the hospital setting); and 'knowledge and beliefs' (understanding and perceptions of treatment alternatives).
Table 1: Themes derived from group discussions
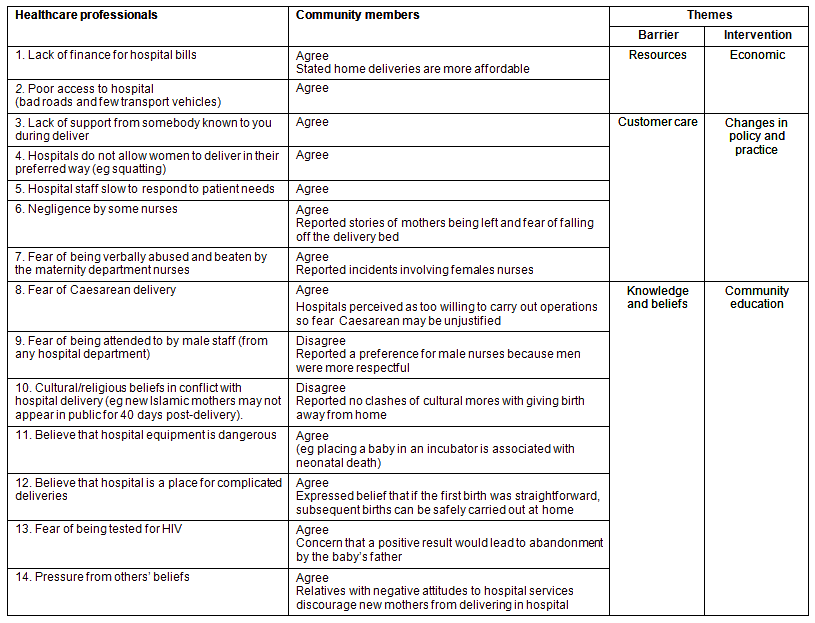
For comparison, enquiries were also made within the community about the cost of home deliveries, the primary charge being payment to a TBA. This typically involved payment in-kind, including food items and lesso (printed cotton cloth used as clothing). The combined cost of these required items was found to exceed the KES 850 (US$11) required by the hospital for delivery.
Contra to the 18% level of district hospital deliveries1, hospital deliveries among the study mothers was 86.5%. A total of 24 mothers (of 39 possible from the main study) who failed to deliver in hospital completed individual interviews. It was not possible to trace the 13 mothers who had changed address, and two mothers lived on islands and so were impossible to contact for interview.
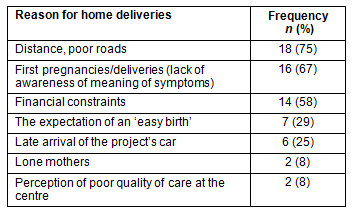
Most mothers identified more than one reason contributing to their failure to deliver in hospital despite the support provided. The mothers' responses are summarised (Table 2). Seven main reasons were elicited, the most common relating to access to resources and knowledge about the stages of delivery. Financial constraints included having insufficient funds to telephone for the project vehicle, or to find alternative transport when the vehicle was unavailable. Despite having been advised at several points during the study of the value of supervised delivery, some mothers reported they did not see a need to come to the hospital because they expected an 'easy' delivery. Some women experiencing their first pregnancy had not understood their symptoms indicated that they were in labour. Two mothers had no family support at the time of delivery and were unable to leave children alone at home.
Table 2: Reasons given for home deliveries
Discussion
The majority of women in Kenyan rural areas similar to the study district do not deliver under supervision of trained medical attendants. The attainment of the core principle of 'safe motherhood' is thus a distant goal1. However the consultation with community members and local medical staff did identify potential barriers and suggested relevant interventions to overcome them.
The main concern of all groups was the lack of resources within families to meet the cost of a hospital delivery, despite this being relatively low. Although the payment to the TBA exceeded the hospital delivery charge, the hospital requires payment in full before the mother can be discharged. Payment to the TBA occurs in instalments, lessening the perception of cost burden. Regardless, the cost of hospital delivery is major concern for those of low income, as is the difficulty of finding a sustainable solution8, and the MDH management team has highlighted this as a key issue for urgent action4.
A second resource-related barrier was the lack of access to transport to hospital, as has been raised in a number of studies9,10. This barrier includes not only the cost of the transport, but also problems of accessibility and distance that limit the potential role of emergency vehicles.
The real effect of these two barriers was observed in the four-fold increase in hospital deliveries among study participants who had both the cost of services covered, and access provided to transport to hospital. Nonetheless, distance to medical facilities and lack of adequate transport services remained the primary barriers, even when participants' economic burdens were lifted. As a senior hospital administrator stated:
...the problem of remoteness and geographic challenges threatens the lives of expectant mothers not only in Msambweni District but also in the whole region of Coast Province....
Regarding the barrier of remoteness, it has been suggested that improving access to centralised services may be inadequate11. Until and unless the transport infrastructure is improved, community based interventions may be required in order to significantly improve maternal and child outcomes at delivery.
Another theme in the category of customer care related to the care women wished to receive while delivering their baby. Poor interaction between medical staff and the pregnant mother can influence the maternal choice to remain at home. Both medical personnel and community members recognised the mothers' preference for social support during the delivery, as well as their wish for strategies to enable pain relief. Hospital regulations, however, did not allow the presence of family members in the delivery room, and mothers were required to remain on the hospital delivery bed throughout their labour.
Despite awareness of the negative community perceptions of these regulations, medical personnel followed hospital protocol rather than meeting the mothers' social and other care needs. In view of this and the low number of available staff, the perception that home may provide better support than hospital care during delivery may be well founded. In a study of urban Kenyan mothers, the participants questioned the safety record of hospitals with regard to maternal and neonatal deaths, as well as expressing fears about 'baby snatching'12. While neither of these issues was raised in the community part of the present study, nor was it suggested that hospital staff lacked medical expertise, it was clear from the participants that hospital staff must balance technical knowledge with good clinical practice and supportive emotional care.
Among the present study mothers, only two referred to 'quality of care' as the reason for not delivering in hospital. The support provided throughout participants' pregnancy by the study staff, such as escorting them to different MDH departments, and following-up to ensure timely access laboratory investigations, clinical reviews and ultrasound services, may have increased the mothers' satisfaction with hospital services. While study mothers were not provided with support during delivery itself, their experience within the study may have de-mystified procedures and lessened the perception of the hospital as an unfamiliar environment. This extra psychosocial support may have accounted for the large increase in hospital deliveries, rather than other interventions that merely covered costs8.
The third theme, knowledge and beliefs, included the issue of cultural practices and beliefs. While medical personnel were aware of the importance of these issues, they did not seem to be aware of the implications of community beliefs for behaviour. For example, hospital staff knew of the '40 day rule' requiring mothers to stay at home post-delivery, and suggested it might discourage delivery in a public facility. The community disagreed, clarifying that this rule impacts movement and travel only after mother and baby return home.
Another discrepancy between the two groups concerned attitudes to being attended by male staff. Hospital staff believed the presence of male staff members could be a deterrent to mothers from the Muslim community. Two religious leaders (Imams) attending a group meeting clarified that there was no such constraint in the Koran, and community members expressed a preference for male staff, perceiving them to be more sympathetic and less abusive to mothers than female staff. Whether this is so, and determining the skill-sets of highly rated staff require further investigation.
Thus, the differences between staff and community perceptions were most evident in responses relating to community beliefs. This highlights the importance of community consultation and the limitations of gathering community information by proxy through staff members. Policy-makers must, therefore, be aware of 'levels' of community membership when gathering representative opinions.
The individual interviews with mothers who failed to attend hospital generally supported the barriers described in earlier group discussions. In addition to underscoring the importance of resource constraints, these interviews also expanded on the problems encountered by women who are not be well prepared for delivery. Over half these mothers stated they began their journey to hospital too late, or were unwilling to make the journey to hospital for what they anticipated would be an uncomplicated delivery. These decisions, based on low knowledge or awareness, suggest a need for more detailed education and expanded antenatal information programs.
The discussion groups also identified that information/education on safe motherhood practices and the stages of pregnancy should be provided not only to pregnant women, but also to the family members who control access to health care. Also highlighted was the need for awareness of family support structures when planning for individual birth experiences. The preferred support structures may differ according to sociocultural context9, and specific family circumstances. For example, even with the small number of participants, there were indications from the present study that single mothers should be targeted for special support.
Limitation
While the present study interviewed women who attended clinic for antenatal care, the results may not provide an accurate profile of all women who deliver at home. Future investigations should explore the beliefs and attitudes of a community based sample to better identify the background factors that contribute to choices made for delivery13.
Recommendations
The discussions held support the need for a constructive, collaborative approach to promoting change. None of the suggested strategies listed below is unique to the context of the study. The need for a multi-level, multi-pronged approach to overcoming barriers to hospital delivery was clear. The recommended interventions target improved access to resources (economic), within the context of a national policy of cost-sharing for health services:
- payment for hospital services by instalment
- provision of ambulance services for pregnant women
- decentralization of delivery services
- improved road network
- higher hospital staffing levels
- provision of shelters for vulnerable mothers prior to delivery
- consideration of free maternal health facilities.
Recommended interventions that target knowledge and attitude change (information):
- links with community groups closer to homes to provide conduits for more regular information, advice and support to all family members
- individual 'birth plans' to meet individual needs, through partnership between mothers and medical staff
- improved staff training in good clinical practice and interpersonal skills
- introductory visits to delivery facilities prior to due dates for expectant mothers
- changes to hospital protocol to incorporate evidence-based strategies for delivery, including accompanied deliveries.
The community needs to be better informed about the true costs and benefits of hospital deliveries, while medical services must be more sensitive to community needs and preferences. These findings have already prompted the initiation of consultation groups on health and maternal issues between health service providers and community based organisations; however, continued efforts are required to increase the proportion of rural births conducted with the supervision of skilled birth attendants in hospitals, and so address the currently high MMR in Kenya.
Acknowledgements
The Medical Superintendent Msambweni District Hospital (Dr D Mwaura) is thanked for his cooperation and support, as are Msambweni District Hospital staff for taking part in the group discussions, and the Chiefs from Kinondo, Kingwede/ Shirazi and Msambweni locations for organising community focus groups and participants for this study.
References
1. World Health Organization. Mother-baby package: implementing safe motherhood in developing countries. Geneva: WHO, 1994.
2. Hogan M C, Foreman K J, Naghavi M, Ahn S Y, Wang M, Makela S M et al. Maternal mortality for 181 countries, 1980-2008: a systematic analysis of progress towards Millennium Development Goal 5. Lancet 2010; 375(9726): 1609-1623.
3. Government of Kenya. Kenya Demographic and Health Survey 2003: Central Bureau of Statistics. Nairobi: GoK, 2004.
4. Government of Kenya, Msambweni District Annual Operation Plan Six: Health Department in the Ministry of Health. Nairobi: GoK, 2010.
5. National Institute for Health and Clinical Excellence. Behaviour change and population: community and individual levels. London: NICE/NHS, 2007.
6. Government of Kenya, Msambweni District Development Plan 2008-2012: Ministry of State for Planning, National Development and Vision 2030. Nairobi: GoK, 2009.
7. Osogo JN. A Traditional History of Kenya. Nairobi: Longmans, 1968.
8. Kasenga F, Byass P, Emmelin M, Hurtig A K. The implications of policy changes on the uptake of a PMTCT programme in rural Malawi: first three years of experience. Global Health Action 2: (Online) 2009. Available: http://www.globalhealthaction.net/index.php/gha/article/view/1883/2136 (Accessed 22 February 2012).
9. Parkhurst J O, Rahman S A, Ssengooba F. Overcoming access barriers for facility-based delivery in low-income settings: insights from Bangladesh and Uganda. Journal of Health, Population and Nutrition 2006; 24(4): 438-445.
10. Jammeh A, Sundby J, Vangen S. Barriers to emergency obstetric care services in perinatal deaths in rural Gambia: a qualitative in-depth interview study. ISRN Obstetrics & Gynecology 2011; 98: 1096.
11. Montagu D, Yamey G, Visconti A Harding A, Yoong J. Where do poor women in developing countries give birth? A multi-country analysis of demographic and health survey data. PLoS One 2011; 6(2): e17-155.
12. Izugbara C O, Kabiru C W, Zulu E M. Urban poor Kenyan women and hospital-based delivery. Public Health Reports 2009; 124(4): 585-589.
13. Wanjira C, Mwangi M, Mathenge E, Mbugua G, Ng'ang'a Z. Delivery practices and associated factors among mothers seeking child welfare services in selected health facilities in Nyandarua South District, Kenya. BMC Public Health 2011; 11: 360.
