Dementia
Dementia is an important public health challenge. In many countries, the proportion of older people in the population is increasing1,2. As rates of dementia increase with age, this results in a rapid rise in the number of people with dementia3,4. Some risk factors associated with higher rates of dementia are also increasing, and so the prevalence of dementia may increase faster than previously expected5-7. At the same time, international financial problems have reduced the resources available for investment in health and social care services.
This combination of increasing numbers of affected people, a smaller proportion of younger people in the population and reduced public finances has created a context in which services need to be delivered as efficiently and effectively as possible in order to maximise the health gain from the money available for investment in services. Buying more of the existing services is not an available option in many countries8.
Dementia services have often been a low priority for service investment in the United Kingdom9. Many services have been delivered by relatively unskilled staff9. Where trained social or healthcare staff have delivered services, there has often been a limited service capacity and restricted investment10. Staff who work in dementia care services have often felt marginalised and undervalued11.
The Scottish Government has identified people with dementia, and the services they require, as being of national importance. The Government recently produced a National Dementia Strategy that guides the development of services12. At the same time, a series of national standards for dementia care have been developed, and the National Health Service (NHS) and local authorities are expected to deliver services to these required standards even in a time of reducing resources12.
Knowledge transfer
Academic research on dementia is now well established13. While much work is primary research relating to the aetiology and medical treatment, health service research and social care research has also developed. There are challenges in translating academic knowledge into service change and incorporating research into practice may be particularly difficult in rural areas where practitioners are geographically separated and may have limited access to training opportunities14,15. In addition, many staff work with more than one client group and so may have to be familiar with a wide range of conditions and their management.
Knowledge transfer, also termed knowledge translation, has developed in an attempt to move academic knowledge into practice: 'The primary purposes of (Knowledge Transfer is) to increase the likelihood that research evidence will be used in policy and practice decisions and to enable researchers to identify practice and policy-relevant research questions' (p729)16.
Traditionally, university departments often assumed that it was the task of the knowledge recipient to seek out and use academic knowledge. There is considerable evidence of the weaknesses of this model and the context and characteristics of the research of the academic organisation, and of the receiving organisation, all seem to be important in affecting the translation of research into practice17-19.
The United Kingdom's 'Rural Economy and Land Use Programme' recommends a 'continuous two way model of knowledge exchange' (p5)20. It identifies four levels of knowledge exchange in research: (i) the linear model, in which information is transmitted from the academic research base to the recipient organisation that will use it in practice; (ii) the feedback model, where the recipients comment on research and so seek to influence future research; (iii) the collaborative model, where there is active discussion of methods and results throughout the process; and (iv) the joint production of knowledge, where service providers and other stakeholders contribute to the production of knowledge, and in which different approaches and insights are valued and encouraged.
The project described here was intended to operate at the third and fourth levels of this framework, integrating with service processes and structures in a process that could be described as embedded engagement. Interaction between the academic centre and the end user is thought to be the most effective means of transferring knowledge and influencing practice18,21. Ideas seem to be more influential than data, although evidence plays an important role21.
NHS Highland and the Dementia Services Development Centre
NHS Highland is the largest geographic health authority in the United Kingdom. It delivers healthcare services to one-third of the land area of Scotland, although the area includes only about 5% of the Scottish population. The area includes many inhabited islands and numerous small towns, villages and isolated hamlets.
The University of Stirling's School of Applied Social Science, and its Dementia Services Development Centre (DSDC), have expertise on dementia services research and on training on dementia.
Knowledge Transfer Partnership
NHS Highland identified dementia as an important strategic concern and, with the University of Stirling, agreed to apply for a Knowledge Transfer Partnership (KTP). This is a UK Government funded scheme that provides matched funds to pay for academic input to industry or to public sector organisations. A 2 year project was agreed, with a University staff member (PS) dedicated to the project, supported by a senior academic (AI) and an NHS Highland manager (LF).
The project sought to use the collaborative and joint production models identified. The program was mainly concerned with knowledge transfer and utilisation of knowledge, but also aimed to undertake local research to produce new knowledge, driven by rural area interests and jointly guided by local service staff and academic experts.
A steering group was established, chaired by NHS Highland's Executive Lead for Mental Health Services. This embedded the work within NHS Highland's organisational structures. In addition, the KTP worker was based on NHS Highland premises and attended monthly operational meetings that included decision making on attaining national dementia targets. These meetings were attended by specialist mental health staff, as well as public health and service planning staff to ensure that work was grounded in clinical concerns. Independent sector input was obtained by meetings with representatives of the largest Scottish dementia charity, Alzheimer Scotland.
The overall method is presented (Fig1). The steering group agreed priorities for local work. As the purpose of the project was to learn from existing knowledge, a systematic review of the rural dementia service literature was conducted. A range of issues found to be important in other areas were identified, including delayed presentation related to stigma; recognition of dementia, including the importance of staff skills; efficiency and effectiveness of diagnostic processes; immediate post-diagnostic support, including information giving; treatment availability, including access to psychological services; longer term support and monitoring; management of challenging behaviour; and end-of-life care22. Training needs were a frequently identified issue and the project team anticipated that this would be of local relevance as well.
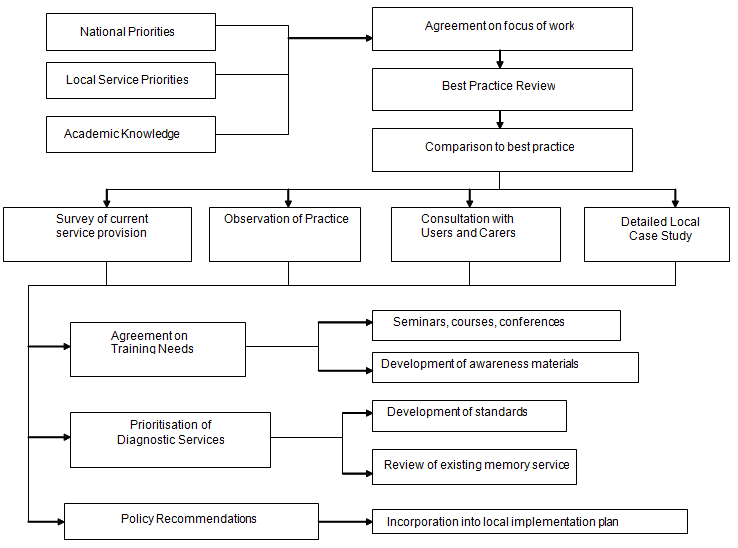
Figure 1: Project process.
The steering group decided to compare existing practice to the information from the review. Four pieces of work were undertaken, which were:
- a survey of community mental health services to identify current practice
- observation of practice in community, clinic and ward settings
- consultation with service users and carers (this part of the work was approved by the relevant ethics committee and is described in detail elsewhere23)
- a detailed case study in one rural area (Fig1).
Ten of 13 community teams (77%) responded to the survey. The survey found that psychiatric nurses formed the core of most teams but that there were marked variations between teams in the involvement of other staff, such as healthcare assistants, support workers, occupational therapists and support workers. Almost all teams reported a role in diagnosis, assessment, post-diagnostic support and support for carers, but there were marked differences in how this was delivered. Notably, six teams already used telehealth delivery to some extent. Only half of the teams reported joint working with charity organisations, such as Alzheimer Scotland. Teams saw better joint working, early diagnosis and good post-diagnostic support as important areas for improvement.
Detailed interviews were conducted with 13 family carers, and seven people with dementia. The individuals were identified from across the area to ensure geographic coverage. Interviews were recorded and transcribed or, in two cases where permission was not given for recording, hand written notes were kept with the permission of the interviewees. A thematic analysis was conducted. The main issues raised in these interviews were identification of memory problems; the diagnostic process; post-diagnostic support; and information access and service access, including long-term support. Resources were raised as an issue by both staff and family members.
A detailed case study with the small community team in one very rural area identified access issues, partly related to distances and population sparsity. These included the impact of travel time on staff availability and the need to keep resources under review as the needs within an area changed. The role of generic mental health and community staff in delivering care, and therefore their training needs, was also identified.
The steering group reviewed these findings and decided to concentrate on training to improve awareness and knowledge; diagnostic process; and support for local policy makers, who influenced the priority accorded to dementia services and investment in those services. Activities and outcomes are shown (Table 1).
Table 1: Project activities and outcomes
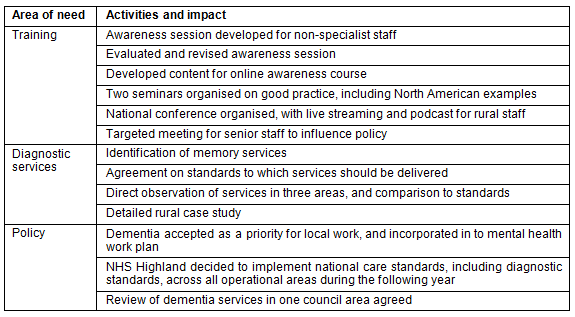
Training
In the surveys, training needs were identified for non-specialist staff, specialist staff and policymakers. Non-specialist care staff need to be aware of dementia and to know how to refer to diagnostic services. They also require information on routine care of people with dementia in their day-to-day working. Specialist staff, both in the community and in institutions, need more detailed knowledge. In addition, policy makers require a good level of understanding of dementia and associated care services.
A face-to-face awareness session was designed for non-specialist staff. This was piloted, evaluated and revised24. Evaluation of this course was very positive and confirmed the widespread desire for access to such material. It became clear, however, that the volume of need was very large and that providing exclusively face-to-face content in a large rural area in the volume required would not be practical.
Content from other sources was used to develop content for an on-line awareness course. In the course of this work, a very similar program developed by an urban NHS Scotland area was identified. This was already available on an electronic learning platform. NHS Highland purchased access to this system, both for this and for other educational resources. Rather than duplicate resources, the local content was provided to the developers of the existing system so that information on rurality could be added.
To influence specialist staff and policy makers, two seminars on good practice were organised. These presented the results of the literature review and survey, and work on diagnosis, referral pathways and post-diagnostic support. A conference was arranged and webcast so that staff who were unable to attend could watch or access a podcast. A final event summarising the work was organised for an invited audience of senior staff.
Diagnostic services
Access to diagnostic services, and speed of diagnosis, emerged as an important issue. The survey identified current diagnostic practice and confirmed wide variation across the area. As part of the project, a group of senior clinical staff were brought together to agree on diagnostic standards, including the use of imaging. These standards were then used to compare current practice, and to identify gaps, including direct observation of some services and of components of service delivery. Following this work, NHS Highland agreed to prioritise the development of diagnostic clinics in each area which met the identified standards.
Policy
Influencing policy makers was a key aim of the project. During the project, a National Dementia Strategy was published, and this would have influenced policy makers. In advance of the strategy, however, the senior management team at NHS Highland endorsed work on dementia diagnosis and post-diagnostic support, and agreed that all community mental health teams in the NHS Highland area should implement an agreed integrated care pathway. Funding has been identified for Alzheimer Scotland workers, who will work as part of psychiatry of old age teams, supporting people in the year after diagnosis. The NHS Highland Mental Health Strategy Group also commissioned work to look at the balance of resources between in-patient and community care, and this work is ongoing. The project contributed to a national target on dementia recognition, and during the course of the project, the number of people identified in primary care in Highland as having dementia increased from 2108 to 2656, an increase of 26%. An independent report identified the NHS Highland area as being in the top 10% of UK Health Authority areas, as ranked by the proportion of predicted dementia sufferers know to services25. A final report on the KTP project was produced for distribution to other NHS areas.
Discussion
This project sought to harness academic knowledge and expertise, and to use it in local service re-design. Supported by a national Knowledge Transfer Partnership program, the project engaged staff in NHS Highland to use established academic knowledge and to work with academic staff to establish a rich understanding of the local system.
The joint ownership of the project by NHS Highland and a specialist University department was essential in producing a shared agreement on priorities and actions. This embedded engagement model brought academic influence to the heart of local decision making, while also providing a valuable service context for the academic staff. The initial literature review provided a template against which to compare Highland practice. The team survey, observation and shadowing, and interviews with family carers and people with dementia did a great deal to provide a local context and to demonstrate the relevance of the previous academic work.
The decision to segment training to target different groups was important and NHS Highland has now commissioned a dementia training strategy for its workforce. The changed national context, with a new dementia strategy, is likely to have increased the influence of the project. The existence of this work meant that the local healthcare system was well placed to respond when the national strategy was produced.
Translating academic knowledge into practice is often challenging. Staff in rural areas may feel that work produced in large centres, or in different rural areas, is not relevant to their practice. Involving staff in the project design, collecting local information to supplement national knowledge and disseminating the results as widely as possible increased ownership and resulted in clear organisational actions.
Acknowledgements
The authors thank Dr Karen Blagden, Morag Bramwell, John Dreghorn, Shirley Duff, Neil Duncan, Kate Earnshaw, Teresa Green, Fiona MacLean, Ruth Mantle, Anne Mason, Debbie Sutherland, Joe Taylor and Norman Young. This project was funded by the United Kingdom Technology Strategy Board Knowledge Transfer Partnership program and by NHS Highland.
References
1. Rocca WA, Petersen RC, Knopman DS, Hebert LE, Evans DA, Hall KS et al. Trends in the incidence and prevalence of Alzheimer's disease, dementia, and cognitive impairment in the United States. Alzheimer's & Dementia 2011; 7(1): 80-93.
2. Ng TP. The unparalleled challenge of aging populations. Dementia and Geriatric Cognitive Disorders 2010; 30(6): 454.
3. Gao S, Hendrie HC, Hall KS, Hui S. The relationship between age, sex and the incidence of dementia and Alzheimer's disease: a meta-analysis. Archives of General Psychiatry 1998; 55: 809-815.
4. Siewert U, Fendrich K, Doblhammer-Reiter G, Scholz RD, Schuff-Werner P, Hoffmann W. Health care consequences of demographic changes in Mecklenburg-West Pomerania: projected case numbers for age-related diseases up to the year 2020, based on the Study of Health in Pomerania (SHIP). Deutsches Arzteblatt International 2010; 107(18): 328-334.
5. Jorm AF, Dear KBG, Burgess NM. Projections of future numbers of dementia cases in Australia with and without prevention. Australian and New Zealand Journal of Psychiatry 2005; 39: 11-12.
6. Anstey KJ, Cherbuin N, Budge M, Young J. Body mass index in midlife and late-life as a risk factor for dementia: a meta-analysis of prospective studies. Obesity Reviews 2011; 12(5): e426-437.
7. Beydoun MA, Beydoun HA, Wang Y. Obesity and central obesity as risk factors for incident dementia and its subtypes: a systematic review and meta-analysis. Obesity Reviews 2008; 9: 204-218.
8. Henderson EJ, Caplan GA. Home sweet home? Community care for older people in Australia. Journal of the American Medical Directors Association 2008; 9(2): 88-94.
9. All-Party Parliamentary Group on Dementia. Prepared to care; challenging the dementia skills gap. London: The Stationery Office, 2009.
10. Royal College of Psychiatrists Centre for Quality Improvement. Report of the National Audit of Dementia Care in General Hospitals 2011. London: Royal College of Psychiatrists Centre for Quality Improvement, 2011.
11. Vernooij-Dasssen MJ, Faber MJ, Olde Rikkert MG, Koopmans RT, van Achterberg T, Braat DD et al. Dementia care and labour market: the role of job satisfaction. Aging and Mental Health 2009; 13(3): 383-390.
12. Scottish Government. Scotland's National Dementia Strategy. Edinburgh: Scottish Government, 2010.
13. Innes A. Towards a holistic approach for understanding dementia. In: A Innes, F Kelly, L McCabe (Eds). Issues in evolving dementia care: international theory-based policy and practice. London: Jessica Kingsley, 2012; 24-37.
14. Innes A. Dementia studies: a social science perspective. London: Sage, 2009.
15. Morgan D, Innes A, Kosteniuk J. Dementia care in rural and remote settings: a systematic review of formal or paid care. Maturitas 2011; 68(1): 17-33.
16. Mitton C, Adair CE, McKenzie E, Patten SB, Perry BW. Knowledge transfer and exchange: review and synthesis of the literature. The Millbank Quarterly 2007; 85(4): 729-768.
17. Agrawal A. University-to-industry knowledge transfer: literature review and unanswered questions. International Journal of Management Reviews 2001; 3(4): 285-302.
18. Cummings JL, Teng B. Transferring R&D knowledge: the key factors affecting knowledge transfer success. Journal of Engineering and Technology Management 2003; 20: 39-68.
19. van Wijk R, Jansen JJP, Lyles MA. Inter- and intra-organizational knowledge transfer: a meta-analytic review and assessment of its antecedents and consequences. Journal of Management Studies 2008; 45(4): 830-853.
20. Phillipson J, Liddon A. Common knowledge: an exploration of knowledge transfer. Newcastle: Rural Economy and Land Use Programme, 2007.
21. Lavis JN, Robertson D, Woodside JM, McLeod CB, Abelson J. How can research organizations more effectively transfer research knowledge to decision makers? The Millbank Quarterly 2003; 81(2): 221-248.
22. Szymczynska P, Innes A, Mason A, Stark C. A review of diagnostic process and postdiagnostic support for people with dementia in rural areas. Journal of Primary Care & Community Health 2011; 2(4): 262-276.
23. Innes A, Szymczynska P, Stark C. Dementia diagnosis and post-diagnostic support in Scottish rural communities: experiences of people with dementia and their families. Dementia 2012; http://dem.sagepub.com/content/early/2012/11/04/1471301212460608 (in press).
24. Szymczynska P, Innes A. Evaluation of a dementia training workshop for health and social care staff in rural Scotland. Rural and Remote Health 11: 1611. (Online) 2011. Available: www.rrh.org.au (Accessed 5 November 2012).
25. Alzheimer's Society and Alzheimer Scotland. Mapping the dementia gap 2011: progress on improving diagnosis of dementia 2010-2011. London, Alzheimer's Society, 2012.



