Despite progress towards the health-related UN Millennium Development Goals, improvements remain elusive in maternal and newborn health (MNH) in Tanzania1. In 2009 the maternal mortality rate was estimated to be 790 per 100 000 live births1, while the neonatal death rate was put at 33 per 1000 live births2. The causes of these persistently poor outcomes are related to the health system and overall human resource policy and management3-5 . The absolute shortage and mal-distribution of skilled health workers are contributory factors6, as are the performance and motivation of current health workers7.
Motivation is the psychological process that gives behaviour purpose and direction8. A conceptual framework of health worker motivation in low-resource countries has been developed9, and widely adopted7,10-13. It proposes a multi-level approach spanning organisational and policy level influences, as well as the broader cultural context. At the individual level, a health worker's own goals and expectations play a role, as does their training and experience of work outcomes9.
Background on Tanzania
Situated in East Africa, Tanzania covers 947 300 km²14 and has an estimated population of 43 188 00015. Despite ongoing migration to major urban areas, 74% of the population still reside in rural areas15. The country has a comprehensive network of primary health care facilities which the ongoing Primary Health Services Development Programme continues to expand. However, many such facilities lack the skilled health workers and resources necessary to deliver quality health care. The total available health workforce is 35 202, which is only 35% of what is needed, according to defined staffing norms16. There is also an imbalance between the proportion of skilled health staff and lower-level cadres, with 43% of the health workforce made up of lower-level cadres such as maternal and child health aides, assistant clinical officers and attendants16. The lower the level of the facility and the more rural the setting, the greater the shortages are. This reflects the difficulty of placing and retaining staff in remote facilities16. Lindi and Mtwara regions in the South of the country are among the most affected in this regard.
Significantly, the Ministry of Health and Social Welfare has launched a Human Resources for Health Strategic Plan (2008-2013) which provides an in-depth analysis of the problem, projections of required staffing needs, and outlines strategies for improved health worker training and management16. Health worker motivation is declared to be the 'cornerstone' of the current human resources policy and a call is made for more research in this field (p26)16. In particular there is interest to explore the motivation of mid- and lower-level health workers13,17.
This article describes an exploratory study undertaken at the start of the project 'Quality of prenatal and maternal care: Bridging the know-do gap' (QUALMAT; Appendix I). The research questions were:
- what is understood by the term 'motivation'
- what encourages and discourages providers of MNH care in rural areas
- which factors influence their performance and job satisfaction.
Due to the study's exploratory nature, in-depth interviews were chosen as the method of data collection. In an ideal situation an emergent design and highly flexible interview technique would have been employed. However, as the research project required that the same research questions be later explored in rural Ghana and Burkina Faso, a more structured and replicable approach was taken.
The first draft of the interview guideline was produced by the authors who come from, or are highly familiar with, the Tanzanian context. Members of the team have worked on health worker motivation issues in practice in Tanzania and have undertaken previous research focusing on hospital staff18. Reference was made to a review of the literature and, in particular, the above-mentioned conceptual framework on health worker motivation9. The 'grey literature' was consulted as well as scientific literature retrieved from searches of the PubMed, Science Direct and PsyNET databases, using the MeSH terms 'motivation', 'job satisfaction' or 'personal satisfaction', 'health personnel' and 'developing countries'.
Following previous experiences of conducting similar interviews with health providers in Cameroon, care was taken to allow respondents the opportunity to vent any frustrations with their working situation before enquiring about more subtle issues, such as personal satisfaction19. The guideline was further discussed, elaborated and validated using a participatory approach. This involved psychologists, social scientists and health professionals from Tanzania, Ghana and Burkina Faso. While this approach was time-consuming it was considered essential to ensure the guideline was rooted in the socio-cultural settings of its future application.
The guideline was piloted among health workers at primary care level in Tanzania before being finalised, adapted for the different levels, and translated into Kiswahili. Respondents from differing levels were targeted in order to compare and contrast views and opinions.
Given the intention to provide a detailed, close-up view20, it was decided to interview 25 health workers. The sampling framework was purposive, focusing on the intervention and non-intervention districts of the QUALMAT study (Lindi Rural and Mtwara Rural in Southern Tanzania) and on primary level facilities. Health centres in rural settings (located >10 km from a town), and with a maternity unit equipped to deliver basic emergency obstetric care, were identified. A judgement approach was used to select a 'productive sample'21 from among the staff of ten public and two faith-based facilities that fulfilled these criteria. For example, care was taken to include providers of all ages, and some male providers. While QUALMAT's interventions will only be introduced in public facilities, five health workers were also included from the faith-based sector to capture their perceptions. No distinction was made regarding the health providers' training; rather, all those actually delivering MNH were approached. Hereafter these health workers will be referred to as 'MNH providers'.
Beyond the interviews with MNH providers, interviews were planned with two district medical officers, two district reproductive and child health-coordinators and four rural facility managers, as well as two informants from the Ministry of Health. This brought the total number of interviews to 35.
The interviews were held in June and July 2010. The duration of each interview was an average of 2 hours. Interviews were conducted after working hours at a neutral location to create a degree of distance from the workplace and ensure a relaxed atmosphere. Data quality was optimised by the use of only one interviewer who had extensive experience, and also by an assurance of strict confidentiality. No respondent appeared to feel uncomfortable, although some were not able to answer all questions. There were no objections to the interviews being recorded.
The interviews were transcribed into English by the interviewer. The software NVivo v9 (www.qsrinternational.com) was used to facilitate analysis. Before proceeding the transcripts were read thoroughly. Topics were then identified directly from the responses in a descriptive coding stage22. Subsequently further coding was undertaken to capture cross references and identify dominant themes. Several rounds of analysis and interpretation followed during which themes were broken down, cross-cutting issues and patterns sought and apparently contradictory statements discussed in relation to more widely held views. Analytical memos were written to stimulate reflection and thought. These were then condensed and finalised under the guidance of the Tanzanian researchers to ensure plausibility in the country-context.
During these steps care was taken to search for associations with the variables sex, age-group, profession and facility ownership, and to compare the perceptions of respondents of differing levels. Attention is drawn to these differences as the findings are presented. Quotes are used to illustrate the general tendency of the responses.
Ethics approval
Written consent was obtained from all respondents. All interview data were de-identified during the process of analysis. Ethical clearance was granted by the Muhimbili University of Health and Allied Sciences Ethical Review Committee (MU/AEC/VOLXIII/96).
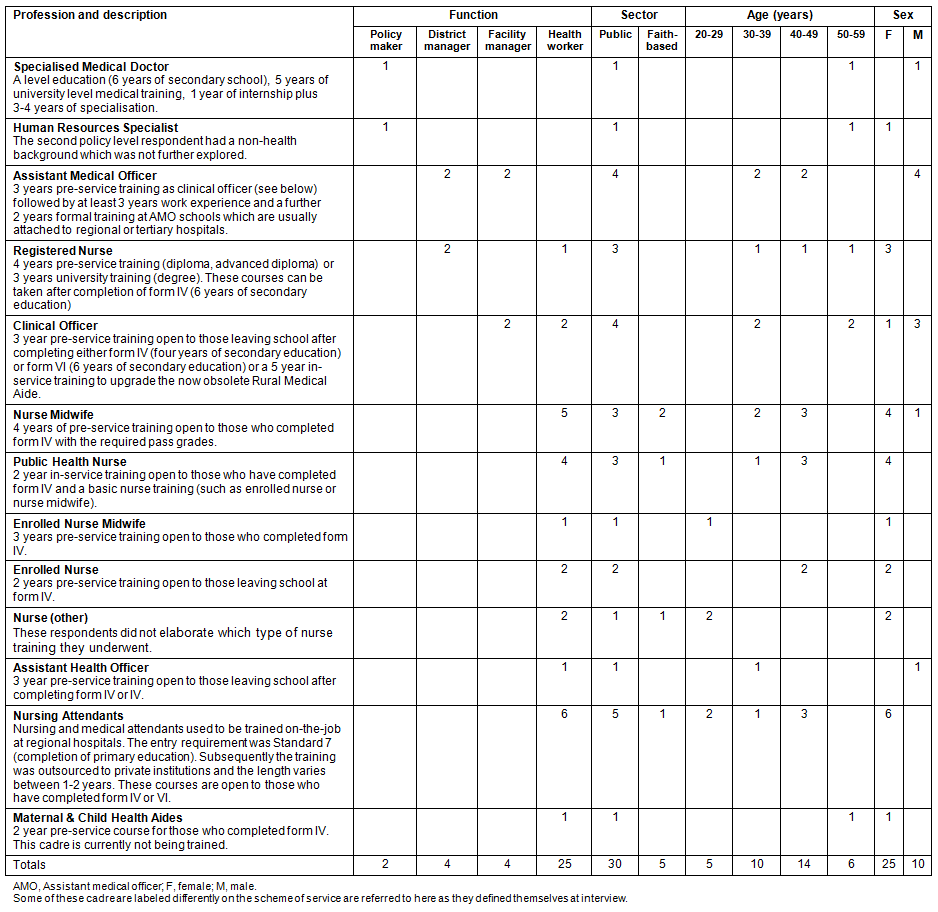
All MNH providers and facility managers had a workplace located in a rural area. The policy and district level respondents were based in towns. The rural facilities were led by assistant medical officers or clinical officers, two sub-cadres of physician. Maternal and neonatal health care was largely provided by public health or enrolled nurses or nurse midwives, as well as by the lower cadres nursing attendants and maternal and child health aides. The full characteristics of the respondents are shown below (Table 1).
Table 1: Profile of in-depth interview respondents (data sources:23,24; Tanzania National Nurses Association, 2011; and QUALMAT project data, 2011)
How people became maternal and newborn health providers in rural facilities
A dominant theme across the interviews was the strong wish of all the respondents to serve the community:
I was always attracted by the way health staff provided services to the community. When one works in the health sector it is really a way to help people. This very much influenced my choice of profession. (Public Health Nurse, female, public facility)
The specific wish to help mothers and children also emerged as being important, including for the male MNH providers:
Above all I like to help the mothers and their children. It grieves me if I see that they are suffering. (Nurse Midwife, male, public facility)
Most reported not having chosen but rather having been posted to their rural workplace. Among those affected, the repeated reference to the discouraging effect of open-ended rural postings was notable.
I requested for transfer on the grounds of staying here for 9 years. It is a long time to be apart from my parents. They are old and I have a responsibility to them. It is very far to visit them and takes time and money. It worries me how long this separation will go on. Unfortunately I was told, that length of time alone is not a convincing reason for a transfer. (Enrolled Nurse, female, public facility)
Maternal and newborn health provider motivation
The majority of respondents described motivation as something given to encourage providers to work harder, without being watched or forced. Many appeared to understand the term as a positive incentive given in addition to one's salary:
Motivation is the extra income a person receives from his/her superior after doing the job well. (Nurse Midwife, female, public facility)
However, elements of other understandings were also revealed:
Motivation comes when we appreciate someone's work. The person feels that their work has been seen and valued so they can proceed to give good services. (Clinical Officer, male, public facility)
Motivation may be a matter of mere words when you are told that you have done a good job. (Nurse Midwife, female, faith-based facility)
Most of the references to MNH provider motivation from all the types of respondents described it as being 'fair' or 'low':
The level of motivation is low. We work long hours at this facility and our salaries are meagre. Even if you go back home for a rest someone will call you and you have to go back to work in your private time. (Public Health Nurse, female, public facility)
Across the responses, the use of the term 'morale' was worthy of note:
Even the attendants may work much better than a nurse officer or nurse midwife if they have good morale. (Facility Manager, Clinical Officer, female)
In the end it's all a question of morale. If you do this work and are looking for things like money, promotion, prestige or the like then you will only be disappointed. (Public Health Nurse, female, faith-based facility)
Factors that encouraged and discouraged maternal and newborn health providers
Community appreciation was identified as being extremely encouraging and the most important source of appreciation for MNH providers by all the respondents, with the exception of those at policy level. Seminars and workshops and the per diems that are received for attendance also encouraged staff. Additionally, several respondents, including all those from the lower cadres, stated that the process of learning itself is encouraging:
When we learn on-the-job we can practice our skills and discuss areas of weaknesses. It is so helpful. If I forgot to do something they remind me. (Nursing Attendant, female, public facility)
The majority referred to recent improvements in the availability of MNH working tools and services having been made free, as reflecting government and development partner support and being encouraging.
The overwhelming sources of discouragement were financial in nature. The majority of respondents referred to low salary levels and inconsistencies in the payment of overtime and leave. The discourse was pervaded by a sense of unfairness. Salary levels were said to be not only too low, but also unfair considering the amount of work and responsibility expected. Providers working in faith-based facilities resented being paid less than their counterparts in the public service. Lower-level cadres considered that they were paid less to do largely the same work as others. Most respondents considered they did not receive the allowances they were entitled to.
Beyond complaints about financial aspects, the respondents were discouraged by facility understaffing, the resulting workload and how it is distributed, by unsupportive management, inflexible work schedules, infrequent promotion and not knowing when one will be transferred next. Complaints about poor security and health and safety and problems with accommodation marked the interviews and were felt to be illustrative of an unwillingness to take care of MNH providers:
We are expected to work without gloves when the supplies dry up. Imagine you have to take a delivery and will come in contact with blood and stool. There is a risk of infection. I ask myself will they pay me if I get a problem, and who will take care of my children? When you think of that you won't do your work as its supposed to be done. (Public Health Nurse, female, public facility)
The respondents also begrudged being left feeling helpless:
The district people delayed in sending the car for so long that the woman died. I was with her, trying to help but I do not have the ability to perform a caesarean section. This caused me much distress and for a long time I didn't want to work anymore. (Enrolled Nurse Midwife, female, public facility)
Maternal and newborn health provider job satisfaction
The main theme that emerged from the responses of the facility managers and MNH providers, was that quite a strong degree of satisfaction was derived from their work:
I feel very satisfied when I perform my job well. It gives me a tender feeling to see a healthy mother and baby after the delivery. The community here congratulate me on my work and that is when I feel happy with my job. (Enrolled Nurse, female, public facility)
Overall a clear association between job satisfaction and factors that are intrinsic in nature was revealed. These included helping the community, enjoying one's work and believing it to be important, liking to see a job done well and feeling competent in one's role:
I am satisfied because I like to do my work and I know how to do it. I see that I can help these people and that is my reward. (Public Health Nurse, female, public facility)
Maternal and newborn health provider performance
The responses show that basic steps which could improve MNH provider performance may have been overlooked. For example, several of the MNH providers reported not being introduced to their post:
I just watched. Sometimes I asked. The explanations came from workers who were at the facility a long time. I copied the behaviour of the nursing attendants. (Public Health Nurse, female, public facility)
Only a small number of participants, none of whom belonged to the lower cadres, reported receiving a written job description. References were further made to the tasks thus defined failing to match the actual demands made:
I received instructions when I reported to this centre. They were put clear but verbally. Since then though we have become very few and I now have more to do; I assist with the clinics and do the cleaning if the nursing attendant is absent. (Enrolled Nurse, female, public facility)
Regarding familiarisation with the overall goal of their facility, most of the MNH providers reported that this was not discussed during their orientation. Nonetheless, the majority stated clearly that their facility existed to serve the surrounding community.
The supervision and performance appraisal processes were portrayed as problematic:
Whenever they come for supervision they just blame us without considering the working conditions. (Nurse Midwife, female, public facility)
The importance of rank and who may supervise whom and the logistical arrangements predominated. Only the policy level respondents referred to quality of care and standards. The public sector respondents, with the exception of the lower cadres, reported familiarity with the annual Open Performance and Review Appraisal System. Many relayed poor experiences, such as not receiving feedback or lack of confidentiality. When it came to setting goals during appraisal, the lack of control some providers exercise over their work environment was revealed:
I cannot achieve the goals or even do my job properly due to so many things which are out of my responsibilities. (Nurse Midwife, female, public facility)
All respondents described how the performance of MNH providers in rural facilities is negatively impacted by shortages of skilled staff and the resulting workload:
My working conditions are very difficult and sometimes I get so tired I feel dizzy. If there were more of us then everything could be better because we would be able to work in shifts. (Enrolled Nurse Midwife, female, public facility)
The respondents referred to gaps being filled by staff with lower-levels of training. This was described as contributing to an environment where mistakes may happen. The performance of less skilled staff was portrayed as lower:
It is difficult as some providers do not follow instructions and guidelines. They fail to see the importance. Especially the nursing attendants who are there since long, they just say, 'We do it like this'. (Clinical Officer, male, public facility)
It was reported to be particularly difficult for lower cadres to access training courses and the facility managers called for more on-the-job training to improve clinical skills.
The difficulties faced by facility managers in balancing discipline and showing understanding for their staff became apparent.
You have to understand that their lives are unpredictable. They may have a sudden need for money and so there will be absence. Yet we cannot act like there is no absence. It has to be discussed and a warning given. (Facility Manager, Clinical Officer, male)
The cultural difficulties of correcting older staff were also mentioned: 'You cannot give punishment to the elder for having done the mistakes, only instruction' (Facility Manager, Clinical Officer, female), as well as the experience of correcting staff in general:
You must not scold them in front of patients. They will feel bad and everything will be stopped and patients will not get services on that particular day. (Facility Manager, Assistant Medical Officer, male)
Respondents at all levels mentioned that the search for cash for immediate needs or to repay loans distracted providers from their work. Indeed, the majority of the providers described parallel involvement in agricultural activities, with smaller numbers engaged in petty trade, such as selling soap or ice-cream or in private practice:
You hear that 210 000 Tanzanian Shillings [approximately $US150] is needed. Then you ask yourself where will I get even a half of it. Whilst at work my mind is not working as I am still thinking on how to get such an amount. (Public Health Nurse, female, public facility)
It emerged that provider performance was considered to be particularly transparent in the area of MNH:
If an expectant mother has complications it can't wait, so you have to have enough skills to solve it. You cannot guess, you must know what to do and do it. (Public Health Nurse, female, public facility)
This effect was felt to be intensified at remote facilities:
For us who work in the village, it is much easier to be noticed by the community than in the town. (Facility Manager, Clinical Officer, female)
The interviews revealed professional associations to be extremely weak with most of the respondents, except for some of the nurses, reporting either not being members or not being eligible to join. Such bodies were not described as playing any role in improving the conditions of providers.
Despite the difficulties associated with working in MNH, the majority of respondents had not ever considered leaving their profession. A small group of providers made reference to the difficulties they faced at their current, rural workplace and expressed a wish to be transferred.
Discussion
Motivation
Throughout the public health literature, work motivation is cited as 'an individual's degree of willingness to exert and maintain an effort towards organisational goals' (p1255)9. The majority of the respondents were clear that the goal of their facility was to serve the patients and demonstrated considerable commitment to the community. Thus, it might be expected that the MNH providers would be reasonably motivated. However, the impression gained was that levels of motivation were only fair or low. This could indicate scope to better align the provider's readiness to serve communities with the goal of their workplaces, an alignment which has been shown to have a motivating effect9.
However, this interpretation is cautious because the term 'motivation' appeared to have been understood as a tangible incentive. A review of the translating process led to the observation that in Kiswahili the word motisha, although formally meaning motivation, has a variety of meanings in common usage, including both motivation and incentive. A similar understanding of motivation was also found among some healthcare providers in Benin and, to a lesser extent, in Kenya11. Explanations for this could lie in the particular importance of extra payments in contexts where salaries are low. However, other dimensions of the concept of motivation were also referred to such as the motivation derived from having one's work noticed or appreciated, meaning that further clarification is required.
The use of the term 'morale' in the responses also requires closer attention. A researcher of motivation in the workplace in Nigeria observed that although the term is not frequently found in the literature it is widely applied25. It has also been suggested that in the absence of a common definition, it may be helpful to refer to motivation with another term, such as morale or boosting one's work spirit11.
Job satisfaction
The MNH providers and facility managers largely reported being satisfied. This was due to factors that included serving the community, the importance attached to MNH work, having the opportunity to learn, liking to see a job well done, and feeling competent in one's role. Personal achievement at work and job satisfaction itself have been identified as intrinsic rewards among health staff in low-resource settings26,27.
It is possible that intrinsic rewards are particularly pronounced for MNH providers in rural facilities. The respondents all concurred that theirs was a critical work area where community members were quick to express anger in the case of poor outcomes, but also gratitude when things went well. This may serve to intensify feelings of achievement and work meaningfulness. However, others stressed that the presence of intrinsic rewards should not be interpreted as meaning that the situation regarding extrinsic rewards can continue to be neglected13,28.
Performance
In this study it was not possible to gain any objective measure of the overall performance of the MNH providers who participated. The productivity of health workers in Tanzania has been found to be low29 and it is arguable that the felt burden of work could be partly due to poor organisation and lack of recovery time. Absenteeism was reported to be a problem and facility managers implied that the reason behind this was often the need to seek extra income.
The findings that the very nature of MNH work and working in rural areas in general made the providers' performance more transparent could be further developed. For example, community feedback could be better integrated in quality improvement and performance appraisal processes30,31.
Performance and quality of care have been shown to be undermined by a lack of staff, staff assuming multiple roles12 and gap-filling with lower-level staff. The present situation is compounded by the lack of skills-based training and the particular difficulties that lower cadres face in accessing training at all, as also observed in other research in Tanzania32.
Although the policy level respondents were of the opinion that MNH providers would most value appreciation from their managers, this was not the case. This may be because some of the processes where managers would be expected to play a key role and which should lead to benefits (such as the appraisal and promotion systems) were shown to be malfunctional. Facility managers struggled to appropriately correct staff mistakes and manage appraisal and supervision tools. Moreover, key tasks such as introducing new staff to their posts, putting job descriptions in place and arranging on-the-job training were not consistently applied. De-motivating factors such as lack of professional development and career advancement33,34 need to be addressed, as do health, safety and security concerns which make providers feel undervalued35. Poor general management and human resources management skills23,36 as well as cultural constraints, such as the inhibiting effect of hierarchies or cultural deference to age37 may explain these shortcomings.
Factors that encouraged and discouraged maternal and newborn health providers in rural facilities
The results of this study suggest that the effort invested in recent years to improve the availability of MNH working tools, which gave particular focus to the Southern regions (B Schmidt-Ehry, pers.comm., 2011), has encouraged these providers. Community appreciation was also a source of encouragement. The effect of this may be magnified in rural areas38. Moreover, the act of learning was shown to be encouraging, as affirmed by other studies in low-resource settings31,39.
With regard to the factors that discouraged these MNH providers, the situation of the lower cadres gives cause for concern. Their responses showed that they were less likely to have a job description or be familiar with appraisal processes, had a limited grasp of the importance of standards, had lower access to seminars and were frustrated that they are paid less to do what they perceived to be the same work as others.
Assessment of the factors that discouraged these MNH providers suggests they can be divided into those that have to do with conditions of employment, and those which pertain to the organisation of work processes. The former are broadly policy level tasks, whereas the latter depend on facility management.
Addressing the major conditions of employment, such as salaries, allowances and promotions, as well as facility staffing levels and transfers are largely policy level tasks. The 2006 salary rise was not mentioned by any of the public sector respondents, which probably indicates that wages are still not in line with the cost of living. The providers working at faith-based facilities resented the higher salaries earned by those in the public sector. Some nurses mentioned having moved to their current rural facility from one of faith-based ownership. Such reports may illustrate the current difficulties described by the faith-based sector in keeping pace with employment conditions in the public sector40. They therefore underscore the importance of inclusive, sector-wide employment measures. Eligibility criteria for many of the allowances appeared to be unclear and a source of jealousy. It would be helpful to make the situation more transparent, for this would counter entrenched feelings of unfairness12,32,41. Provider preference for fixed duration rural postings has been noted in other low-resource settings42.
The managers of rural facilities appeared to lack support, skills and status. Stronger managers could improve the organisation of work and counter the heavy, felt workloads and perceived unfair distribution of tasks35. Experiences whereby facility managers have established solidarity funds to cushion providers against financial emergencies could also be shared43. Moreover, managers could be supported, perhaps by the regional level, to arrange skills-based, on-the-job training so as to bring tasks and competencies into better alignment. Given the increased reliance on staff with lower-levels of training, the importance of this is now greater than ever. Older, experienced and respected members of the Ministry of Health could support managers in advocating the use of tools such as performance appraisal at facility level.
The relevance of professional associations was found to be extremely limited, in line with findings from other regions of the country13. An association for rural managers could hold important potential. In other settings this has led to enhanced social recognition and improvements in the skills of members44,45. Further research could usefully be undertaken to examine the situation of rural managers in greater detail.
Limitations
The respondents displayed a set of features which may strike a chord with those familiar with the context, making some wider recognition possible46. It is also possible that the views raised by these respondents reflect broader phenomena that could be further explored by those working to address rural staffing issues in Tanzania. However, the findings cannot be generalised in a statistical sense.
The influences on MNH provider motivation, performance and satisfaction were shown to be complex and to span the different levels outlined in the conceptual framework. Variations in the use of terms and concepts pertaining to motivation were revealed, and further clarification is needed. Intrinsic rewards played a role in continued provider willingness to exert an effort at work. The critical nature of MNH and the rural setting readily exposed health workers' performance. The causes of discouragement could be broadly divided into those requiring renewed policy attention and those which could be addressed by strengthening the skills of rural facility managers, enhancing the status of their role and increasing the support they receive from higher levels of the health system.
Acknowledgments
The authors' deepest gratitude is extended to the respondents who gave their time to partake in these interviews. Ms Christiane Wiskow, Dr Bergis Schmidt-Ehry and Ms Cornelia Becker all provided comments on an earlier draft of this paper which were extremely helpful and greatly appreciated. An overview of these findings was presented at the Irish Forum for Global Health international conference, Dublin Ireland, 2-3 February 2012.
References
1. World Health Organization. Trends in maternal mortality: 1990-2008. Estimates developed by WHO, UNICEF, UNFPA and The World Bank. Geneva: WHO, 2010.
2. World Health Organization. World Health Statistics 2010. (Online) 2010. Available: http://www.who.int/whosis/whostat/EN_WHS10_Full.pdf (Accessed 8 December 2011).
3. Hoope-Bender P, Liljestrand J, Mac Donagh S. Human resources and access to maternal health care. International Journal Gynaecology and Obstetrics 2006; 94(3): 226-233.
4. Gerein N, Green A, Pearson S. The implications of shortages of health professionals for maternal health in sub-Saharan Africa. Reproductive Health Matters 2006; 14(27): 40-50.
5. Dogba M, Fournier P. Human resources and the quality of emergency obstetric care in developing countries: a systematic review of the literature. (Online) 2009. Human Resources for Health 7(7): doi:10.1186/1478-4491-7-7.
6. Anon. High Level Forum on the Health MDGs. (Online) 2004. Health workforce challenges: lessons from country experiences, 2004. Available: http://www.amddprogram.org/conference/assets/Resources/Day%201/Human%20Resources%20for%20MDG%205/Abuja%20Conference_Health%20Workforce%20Challenges_High-Level%20Forum%20on%20Health%20MDGs_2004.pdf (Accessed 2 December 2011).
7. World Health Organization. The World Health Report 2006: Working together for health, Geneva: WHO, 2006.
8. Kreitner R. Management, 6th edn. Boston: Houghton Mifflin,1995.
9. Franco L, Bennett S, Kanfer R. Health sector reform and public sector health worker motivation: a conceptual framework. Social Science and Medicine 2002; 54: 1255-1266.
10. Rowe AK, de Savigny D, Lanata CF, Victora CG. How can we achieve and maintain high-quality performance of health workers in low-resource settings? Lancet 2005; 366: 1026-1035.
11. Mathauer I, Imhoff I. Health worker motivation in Africa: The role of non-financial incentives and human resource management tools. (Online) 2006. Human Resources for Health 4(24): doi:10.1186/1478-4491-4-24.
12. Mbindyo P, Gilson L, Blaauw D, English M. Contextual influences on health worker motivation in district hospitals in Kenya. (Online) 2009. Implementation Science 4(43): doi:10.1186/1748-5908-4-43.
13. Chandler CIR, Chonya S, Mtei F, Reyburn H, Whitty CJM. Motivation, money and respect: A mixed methods study of Tanzania non-physician clinicians. Social Science and Medicine 2009; 68: 2078-2088.
14. Central Intelligence Agency. The World Factbook: Tanzania 2009. (Online) 2009. Available: https://www.cia.gov/library/publications/the-world-factbook/geos/tz.html (Accessed 8 December 2011).
15. National Bureau of Statistics, Ministry of Finance, United Republic of Tanzania: Tanzania in Figures. Dar-es-Salaam, Tanzania: Ministry of Finance, 2010.
16. Ministry of Health and Social Welfare, United Republic of Tanzania. Human Resources for Health Strategic Plan 2008-2013. Dar-es-Salaam, Tanzania: MOHSW, 2008.
17. Ministry of Health and Social Welfare, United Republic of Tanzania. Health Sector Strategic Plan 'Partnerships for Delivering the MDGs' 2009-2015. Dar-es-Salaam, Tanzania: MOHSW, 2009.
18. Leshabari MT, Muhondwa EPY, Mwangu MA, Mbembati N. Motivation of health care workers in Tanzania: a case study of Muhimbili National Hospital. East African Journal of Public Health 2008; 5(1): 32-37.
19. Wiskow C. Personalmanagement im Gesundheitssystem Kameruns - Wenn Reformen auf Menschen treffen. Lage: Verlag Hans Jacobs, 2001.
20. Mason J. Qualitative Research. Thousand Oaks, CA: Sage, 1996.
21. Marshall MN. Sampling for qualitative research. Family Practice 1996; 13(6): 522-525.
22. Hsieh HF, Shannon SE. Three Approaches to Qualitative Content Analysis. Qualitative Health Research 2005; 15: 1277-1288.
23. Manongi RN, Marchant TC, Bygbjerg C. Improving motivation amongst primary health care workers in Tanzania: a health worker perspective. (Online) 2006. Human Resources for Health 4(6): doi:10.1186/1478-4491-4-6.
24. Leonard KL, Masatu MC. Professionalism and the know-do gap: exploring intrinsic motivation among health workers in Tanzania. Journal of Health Economics 2009; 19:1461-1477.
25. Robinson EI. The implication of adequate motivation on workers' productivity in an organization. (PhD thesis). St. Clements University, 2004.
26. International Council of Nurses, International Hospital Federation, International Pharmaceutical Federation, World Confederation for Physical Therapy, World Dental Federation, World Medical Association. Guidelines: Incentives for health professionals. Geneva: ICN, 2008.
27. Seera D, Serneels P, Barr A. Intrinsic motivations and the non-profit health sector: Evidence from Ethiopia. Personality and Individual Differences 2010; 51(2): 309-314.
28. Sarakas S, Jamaluddin R. Demotivating factors among government doctors in Negri Sembilan. Medical Journal of Malaysia 1999; 54(3): 310-319.
29. Mæstad O, Torsvik G, Aakvik A. Overworked? On the relationship between workload and health worker performance. Journal of Health Economics 2010; 29: 686-698.
30. Naimoli J, Vergeer P. Results-based financing for health, verification at a glance. Washington: The World Bank, 2010.
31. Toonen J, Canavan A, Vergeer P, Elovainio R. Learning Lessons on Implementing Performance Based Financing, from a Multicountry Evaluation. Amsterdam: Royal Tropical Institute, CORDAID and WHO, 2009.
32. Gunnar-Songstad N, Rekdal OB, Massay DA, Blystad A. Perceived unfairness in working conditions: The case of public health services in Tanzania. (Online) 2011. BMC Health Services Research 11(34): doi:10.1186/1472-6963-11-34.
33. Dieleman M, Toonen J, Touré H, Martineau T. The match between motivation and performance management of health sector workers in Mali. (Online) 2006. Human Resources for Health 4(2): doi:10.1186/1478-4491-4-2.
34. Willis-Shattuck M, Bidwell P, Thomas S, Wyness L, Blaauw D, Ditlopo P. Motivation and retention of health workers in developing countries: a systematic review. BMC Health Services Research 2008; 8: 247.
35. International Council of Nurses. Positive practice environments: quality workplaces = quality patient care. Information and Action Tool Kit. Geneva: ICN, 2007.
36. Lindelow M, Serneels P. The performance of health workers in Ethiopia: Results from qualitative research. Social Science and Medicine 2005; 62: 2225-2235.
37. Mutizwa-Mangiza D. The Impact of Health Sector Reform on Public Sector Health Worker Motivation In Zimbabwe. Partnerships for Health Reform Project. Major Applied Research 5, Working Paper 4. Bethesda, MD: Partnerships for Health Reform Project, Abt Associates, 1998.
38. Dieleman M, Viet Cuong P, Vu Anh L, Martineau T. Identifying factors for job motivation of rural health workers in North Viet Nam. (Online) 2003. Human Resources for Health 1(10) doi: 10.1186/1478-4491-1-10 .
39. International Council of Nurses. Nurse retention and recruitment: developing a motivated workforce. Geneva: ICN, 2005.
40. Schwerzel P, Byamungu C. Framework for the development of a motivation package for rural health workers in voluntary agencies owned hospitals; Final Report. Dar-es-Salaam, Tanzania: Christian Social Services Commission, 2006.
41. McCoy D, Bennett S, Witter S, Pond B, Baker B, Gow J et al. Salaries and incomes of health works in sub-Saharan Africa. Lancet 2008; 371: 675-681.
42. Yumkella F. Worker Retention in Human Resources for Health: Catalyzing and Tracking Change. Technical Brief No. 15. Chapel Hill, NC: Capacity Project, 2009.
43. Munga M, Mbilinyi D. Non-financial incentives and the retention of health workers in Tanzania, Combined evidence from literature review and a focused cross-sectional study. Discussion Paper Series 61. Harare: EQUINET, 2008.
44. Wibulpolprasert S, Pengpaiboon P. Integrated Strategies to Tackle the Inequitable Distribution of Doctors in Thailand: Four Decades of Experience. (Online) 2003. Human Resources for Health 2003; 1(12): doi:10.1186/1478-4491-1-12.
45. World Health Organization. Increasing access to health workers in remote and rural area through improved retention: Global Policy Recommendations. Geneva: WHO, 2010.
46. Williams M. Interpretivism and Generalisation. Sociology 2000; 34(2): 209-222.
_________________________________
Appendix I: QUALMAT



