Maldistribution of physicians is an issue of concern worldwide1, and in Japan many political interventions have been applied2,3. For example, between 2007 and 2011 the Japanese government increased the number of medical school entrants by 17% (from 7625 to 8923)4.
Physicians gravitate toward urban locations, especially when they and their spouse are born, raised, and educated in cities5,6. The training location effect is often urban, and more physicians enter specialties that require the advanced technologies of large hospitals7,8. Physicians who wish to give their children a high quality education likewise tend to live in urban areas9. All of these factors combine to 'pull' physicians to serve in urban areas to the detriment of rural locations.
At the same time, there is also a market-derived force that 'pushes' physicians out of urban areas. Physicians are impacted by the maximization of profit and an increase in physician density will increase competition for profit in urban areas. This can move physicians towards service in rural areas with the result of improved equity of physician distribution (the spatial competition effect: Fig1)10-13. The effect of market-derived repulsion is particularly visible in countries such as Japan where there is no regulation (eg regional caps of physicians) on physicians' choice of practice location.
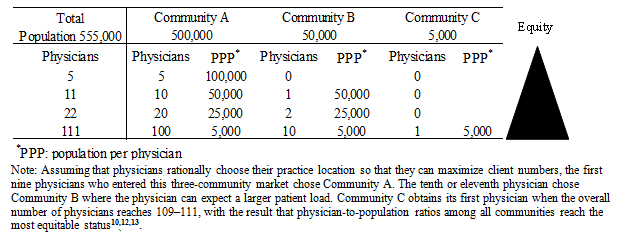
Figure 1: Simplified model of spatial competition.
It is thus hypothesised that an urban-rural distribution of physicians is determined by a power balance between attraction and repulsion. However, past studies have not succeeded in showing the repulsion effect of the implementation of policies aimed to increase the supply of physicians12,14-16. For example, between 1980 and 1990 Japan experienced a 30% increase in the number of physicians per unit population, but the equity of their distribution between urban and rural areas did not improve12,14,16. These statistics, however, do not deny the possibility that competition-based repulsion was influential in that period. Increasing overall demand for physician services can work against the rural distribution of physicians. The period 1980-1990 was a time of increasing physician demand as a result of economic expansion, demographic changes and the implementation of new technologies and services. If the increase in the supply of physicians matched the increase in demand, the two-force equilibrium would be unchanged and the equity of distribution would be constant. However, with physician supply falling behind increasing demand, the equity of physician distribution would worsen.
The attraction-repulsion balance, and the expected effect of an insufficient supply of physicians, may be shown by a comparison between two regions with different rates of physician increase. In a region with a lower rate of physician increase, the spatial competition among physicians in urban communities wound be weaker, and repulsion would be less dominant. This would lead to a greater movement of physicians from rural to urban communities, and a more skewed overall distribution to urban areas.
Japan is well suited to testing this hypothesis because physicians can freely choose their practice locations, unlike those in some European countries. Although the entire population is covered by public health insurance, most medical institutions operate on a for-profit basis17. In Japan, unlike countries such as the USA, only physicians can be the employers at medical institutions, as is prescribed in the Medical Service Act of 1948 (revised 2011). These conditions are necessary for the creation of market-based repulsion. In addition, in 2004 a new regional variation emerged in the rate of increase of physicians among Japanese prefectures as the result of a new government postgraduate clinical training scheme18,19. This intervention produced the conditions for a natural experiment by allowing observations of physician increases and their impacts on the urban-rural flow of physicians.
This study compared trends in physician distribution and the urban-rural flow of physicians between Hiroshima Prefecture, which has the lowest rate of increase in the number of physicians in Japan, and Nagasaki Prefecture, which has the highest. The aim was to show that an insufficient supply of physicians breaks the two-force equilibrium of attraction and repulsion and exacerbates an uneven urban-rural distribution of physicians.
Physician data were derived from the Physician Census compiled by the Ministry of Health, Labour and Welfare in 2002, 2004, 2006, and 2008 (with the permission of The Ministry to use the data for research purposes). In Japan, all those who hold a physician license are obliged to register for the census. For the purposes of the study, among all registered license holders, only those whose main employment was recorded as 'practice' in 'clinics' or 'hospitals (including university hospitals)' were recognised as 'physicians'. In short, all medical doctors in clinical institutions in Hiroshima and Nagasaki Prefectures were included in this study.
Population data were derived from 'Population and Population Dynamics Based on a National Census: National Basic Resident Register 2002-2008'20. Japan has three levels of government: municipal, prefectural and national. Data on municipal-level (city, town and village) populations in Hiroshima and Nagasaki prefectures were extracted from the whole data.
In Japan, the annual production of physicians has been almost constant (approximately 7700). The increase in the number of physicians per 100 000 population (physician-to-population ratio) during the study period in Hiroshima was the lowest among all 47 of Japan's prefectures. It is noteworthy that Hiroshima's physician-to-population ratio decreased for the first time between 2004 and 200621. Among the five prefectures with the highest rate of physician increase, Okinawa, Saitama, Chiba, and Ibaraki were excluded, either because of their isolation from the mainland or because of their proximity to Tokyo, leaving Nagasaki as the control for Hiroshima21. Neither Hiroshima nor Nagasaki is adjacent to metropolitan areas such as Tokyo and Osaka. In 2010, Hiroshima's population was 2 861 000 (12th among the 47 prefectures) and that of Nagasaki was 1 427 000 (27th)22. In 2008, the average annual income per person in Hiroshima was 2,834,000 yen (14th) and that in Nagasaki was 2,157,000 yen (44th)23 .
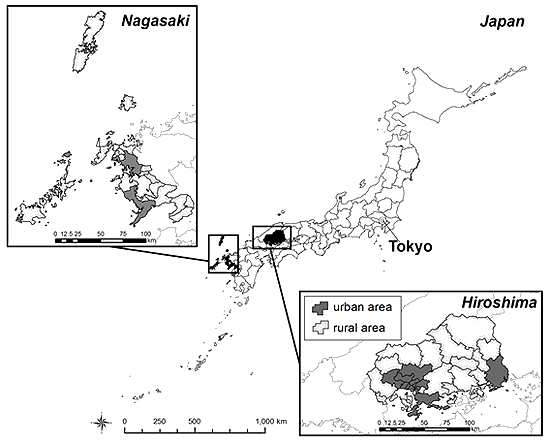
Figure 2: Map of Hiroshima and Nagasaki Prefectures, Japan
The Gini coefficient was calculated for each prefecture based on the number of physicians and the population size. All municipalities were ranked according to physician-to-population ratio, and the cumulative proportion of physicians and population in each municipality was plotted in a plane of coordinates. The plotted line is the Lorenz curve, and the Gini coefficient is the area between the Lorenz curve and the 45° line, divided by the triangle under the 45° line. The Gini coefficient varies between 0 (complete equity) and 1 (complete inequity) according to the degree of variation in physician-to-population ratio12,14,24.
All municipalities were then categorised as urban or rural and the flow of physicians between urban and rural areas was examined for each prefecture. Municipalities with a population greater than 200 000 or a population density of more than 4000 per km2 were defined as urban, and the others were defined rural. Among the 23 municipalities in Hiroshima prefecture, Hiroshima, Fukuyama and Kure cities, as well as Fuchu and Kaita towns were considered urban. Of the 23 municipalities in Nagasaki prefecture, Nagasaki and Sasebo cities were considered urban. Because many municipalities in both prefectures were merged during the study period, the geographic border of municipalities in 2008 was accepted as representative of earlier years.
Next a cohort of physicians (identified by their unique registration number) who worked in the same prefecture in 2002 and 2008 was created and the result was 4288 in Hiroshima, and 2483 in Nagasaki. Cross-table analysis was conducted comparing the numbers of physicians classified according to rural/urban and 2002/2008 categories in each prefecture. Differences in average career length, cross-tabulated by place and year, were also examined. A similar cross-table comparison was performed using the data of a cohort of young physicians with no more than 5 years career experience (who were registered in the 2008 census but not in 2002). The size of the young physician cohort was 802 in Hiroshima and 486 in Nagasaki.
Statistical analyses were performed using SPSS for Windows v18.0 (www.spss.com). In the cross-table analysis, the proportion of the number of physicians in each cell was compared between Hiroshima and Nagasaki using the χ2 test. The average career length was compared using a two-sample t-test. P-values of less than 0.05 were considered statistically significant.
This study was approved by the Ethics Committee of Epidemiological Studies, Hiroshima University in 2010 (#Epidemiology-332).
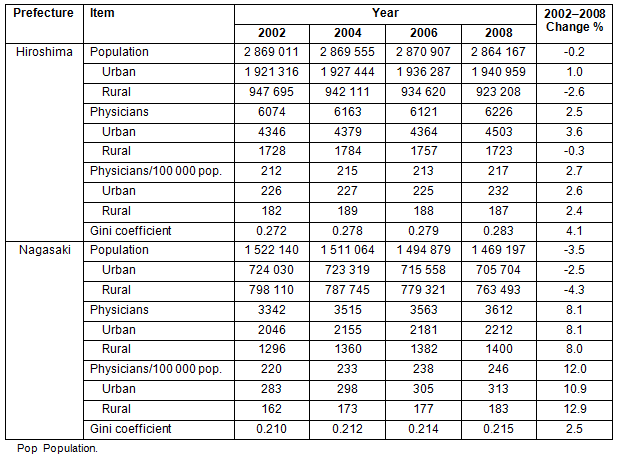
Physicians, population and Gini coefficients are shown (Table 1). The physician-to-population ratio was larger in Nagasaki than in Hiroshima. The increase of physician-to-population ratio in Nagasaki between 2002 and 2008 (12.0%) was greater than that in Hiroshima (2.7%). The increase of physician-to-population ratio in urban Nagasaki (10.9%) was greater than that in urban Hiroshima (2.6%). The increase in rural Nagasaki (12.9%) was greater than that in rural Hiroshima (2.4%). During the period, the Gini coefficient in Hiroshima Prefecture increased toward greater inequity (from 0 toward 1) by 4.1% while the increase for Nagasaki was 2.5%. This indicates that the geographic equity of physicians has worsened in Hiroshima compared with that observed for Nagasaki.
Table 1: Transition of population, number of physicians and Gini coefficient
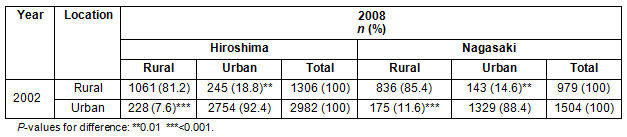
Flows of physicians between urban and rural areas for each prefecture are shown (Table 2). In Hiroshima, 18.8% of rural physicians moved to urban areas, while the proportion was 14.6% in Nagasaki (p=0.01). In contrast, 7.6% of urban physicians moved to rural areas in Hiroshima, compared with 11.6% in Nagasaki (p<0.001). The net flow of physicians was from rural to urban in Hiroshima (17 physicians). The reverse was true for Nagasaki where net flow was 32 physicians from urban to rural areas.
The average career length of physicians moving from urban to rural areas was longer than that of physicians moving in the opposite direction in Hiroshima although this did not reach statistical significance (19.1 [standard deviation 10.3] vs 17.6 [8.8] years; p=0.067). The career length for Nagasaki was not significantly different (17.9 [10.1] vs 18.7 [9.8] years; p=0.442). Of the young physicians with no more than 5 years career experience, 18.3% worked in rural areas in 2008, which was 34% less than the proportion of physicians of all ages (27.7%) in Hiroshima. In Nagasaki, 30.2% of the early-career physicians worked in rural areas, which was 22% less than that of all physicians (38.8%).
Table 2: Flow of physicians between urban and rural areas
Discussion
In Hiroshima Prefecture, which had a smaller increase in physicians, the equity of geographic distribution of physicians deteriorated, the flow of physicians from rural to urban areas was more pronounced, and the career length of physicians going from rural to urban areas tended to be shorter than in Nagasaki Prefecture where the physician increase was more rapid.
The attraction-repulsion hypothesis predicts that regions with smaller increases in physicians will have less spatial competition in urban areas, and thus repulsion would be less dominant in the attraction-repulsion equilibrium compared with regions of larger increases. The net flow of physicians from rural to urban areas in such regions would be more obvious. The results of this study support this prediction. Flow from rural to urban areas in Hiroshima was 1.3 times larger than that in Nagasaki, and the flow in the opposite direction in Hiroshima was 0.7 times that of Nagasaki. The inequity of physician distribution deteriorated in Hiroshima compared with Nagasaki.
The attraction-repulsion hypothesis also predicts that physicians who move from urban to rural areas tend to be younger than those who move from rural to urban areas. This can be explained in terms of barriers to entry into job markets25. New physicians in locations where the job market is saturated have difficulty finding employment. In addition, a longer career may add value in attributes such as experience, board certifications, or advanced degrees. Repulsion from urban areas, therefore, would affect younger physicians more strongly than older physicians. Attraction to urban areas would affect physicians of all ages.
In a region with an adequate supply of physicians, younger physicians would be more likely to move from urban to rural areas. A greater number of new physicians who have just entered the job market would start their careers in rural areas, but this would not be true in a region with an insufficient physician supply. This was supported by the results of the present study. In Nagasaki, physicians who moved from urban to rural areas were younger than those who moved in the opposite direction in the same prefecture, and younger than those who moved in the same direction in Hiroshima. A higher proportion of new physicians started their careers in rural areas in Nagasaki compared with Hiroshima.
Despite a rapid increase in physicians in Japan since 1980, the equity of physician distribution has not improved12,14,16,19,26. This seems to contradict the attraction-repulsion hypothesis. The findings of this study, however, suggest that even with attempts to increase the supply of physicians dramatically, the rate at which physicians have graduated since 1980 did not exceed the increase in demand. Based on the two-force hypothesis, if the supply exceeded the demand, the urban-rural distribution of physicians would have improved, just as an insufficient supply would have worsened the distribution, as was shown in this study.
Limitations
Because the findings are embedded in Japan's unique healthcare system, they should be applied to the healthcare systems of other countries only with the greatest caution. Japan's entire population is covered by social health insurance. The fee for each health service is strictly regulated by the government and is uniform throughout the country. In this sense the Japanese health system is different from that of the free market. However, patients can choose the medical institution for their health care. Physicians, too, can choose their practice locations without any legal or economic regulations. Most of the medical institutions in Japan are private and operated for profit. It is expected, therefore, that the spatial competition shown in Figure 1 would reasonably affect the geographic distribution of physicians in Japan.
The Japanese situation can be contrasted with that of countries such as the UK where the both patients' and physicians' choices are much more regulated. Patients are limited to the medical institutions with which they are registered, and there is a regional cap on the number of physicians in each area that would increase repulsion. Not surprisingly the geographic distribution of GPs per population in the UK is twice as equitable as that of primary care physicians in Japan24. Even so, an insufficient supply relative to demand in such nations could still result in physician movement from rural to urban areas.
The study areas were only two of Japan's 47 prefectures and there is no indication that the movement pattern of physicians in these two prefectures can be generalized to the other prefectures. The results could be due to policies, geography and culture unique to Hiroshima and Nagasaki. The influence of geography may also be a consideration, because Nagasaki's rural areas include more isolated islands and less mountainous areas than the rural areas of Hiroshima.
The definition of 'rural' has always been an issue in physicians distribution studies27, and changing the rural definition may change the urban-rural flow. However, use of the Gini coefficient of physician-to-population ratio is not limited by an arbitrary rural definition.
Finally, the cohort of physicians created to measure urban-rural flow in this study did not account for physicians who relocated to or from other prefectures and so the movements of these physicians are unknown.
To achieve a fair distribution of physicians across locations, the production of physicians needs to keep pace with an increase in demand for their services. A rapid increase of physicians, however, incurs a substantial social cost and is not feasible in countries with struggling or stagnant economies (this includes Japan, among many other nations). Interventions that strengthen 'repulsion' can improve the cost-effectiveness of physician expansion. For example, regulations that set an upper limit or cap on the number of physicians in each area would lead to a more equitable distribution of physicians24. Such an intervention has never been attempted in Japan. In terms of weakening urban attraction, increasing the number of rural-origin students admitted to medical schools would be an effective strategy6. Changes to Japan's health insurance design that increase remuneration to rural medical facilities are likely to positively influence distribution. However, improved equity in the physician distribution in Japan is unlikely without attention to a number of these important strategies.
Acknowledgements
The authors acknowledge the Ministry of Education, Culture, Sports, Science and Technology (Tokyo, Japan) and the Satake Education and Research Fund (Hiroshima, Japan) which sponsored this research.
References
1. World Health Organization. Increasing access to health workers in remote and rural areas through improved retention: global policy recommendations. Geneva: WHO; 2010.
2. Matsumoto M, Inoue K, Kajii E, Takeuchi K. Retention of physicians in rural Japan: concerted efforts of the government, prefectures, municipalities and medical schools. Rural and Remote Health 10: 1432. (Online) 2010. Available: www.rrh.org.au (Accessed 23 April 2012).
3. Matsumoto M, Inoue K, Kajii E. Policy implications of a financial incentive programme to retain a physician workforce in underserved Japanese rural areas. Social Science & Medicine 2010; 71: 667-671.
4. Ministry of Education, Culture, Sports, Science and Technology. Koremadeno igakubunyuugakuteiinnzou no torikumi ni tuite [Policies for increasing the medical school entrants]. (Online) 2011. Available: http://www.mext.go.jp/b_menu/shingi/chousa/koutou/043/siryo/__icsFiles/afieldfile/2011/01/18/1300372_1.pdf (Accessed 1 November 2011; in Japanese).
5. Laven GA, Beilby JJ, Wilkinson D, McElroy HJ. Factors associated with rural practice among Australian-trained general practitioners. Medical Journal of Australia 2003; 179: 75-79.
6. Matsumoto M, Inoue K, Kajii E. Characteristics of medical students with rural origin: implications for selective admission policies. Health Policy 2008; 87: 194-202.
7. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24: 360-368.
8. Rabinowitz HK, Paynter NP. The role of the medical school in rural graduate medical education: pipeline or control valve? Journal of Rural Health 2000; 16: 249-253.
9. Matsumoto M, Okayama M, Inoue K, Kajii E. Factors associated with rural doctors' intention to continue a rural career: a survey of 3072 doctors in Japan. Australian Journal of Rural Health 2005; 13: 219-225.
10. Newhouse JP. Geographic access to physician services. Annual Review of Public Health 1990; 11: 207-230.
11. Schwartz WB, Newhouse JP, Bennett BW, Williams AP. The changing geographic distribution of board-certified physicians. New England Journal of Medicine 1980; 303: 1032-1038.
12. Matsumoto M, Inoue K, Bowman R, Noguchi S, Toyokawa S, Kajii E. Geographical distributions of physicians in Japan and US: Impact of healthcare system on physician dispersal pattern. Health Policy 2010; 96: 255-261.
13. Brown MC. Do physicians locate as spatial competition models predict? Evidence from Alberta. Canadian Medical Association Journal 1993; 148: 1301-1307.
14. Kobayashi Y, Takaki H. Geographic distribution of physicians in Japan. The Lancet 1992; 340: 1391-1393.
15. Goddard M, Gravelle H, Hole A, Marini G. Where did all the GPs go? Increasing supply and geographical equity in England and Scotland. Journal of Health Services Research & Policy 2010; 15: 28-35.
16. Toyokawa S, Kobayashi Y. Increasing supply of dentists induces their geographic diffusion in contrast with physicians in Japan. Social Science & Medicine 2010; 71: 2014-2019.
17. Ikegami N, Campbell JC. [The art of balance in health policy: maintaining Japan's low-cost, egalitarian system]. Tokyo: Chuko-shinsyo, 1996 (in Japanese).
18. Koike S, Ide H, Yasunaga H, Kodama T, Matsumoto S, Imamura T. Postgraduate training and career choices: an analysis of the National Physicians Survey in Japan. Medical Education 2010; 44: 289-297.
19. Toyabe S. Trend in geographic distribution of physicians in Japan. International Journal for Equity in Health 2009; 8: 5.
20. Ministry of Internal Affairs and Communications. Jumin kihon daichou jinkou [Population and population dynamics based on the National Basic Resident Register 2002-2008]. Tokyo: MIAC, 2002-2008 (in Japanese).
21. Ministry of Health, Labour and Welfare. Ishi Shikaishi Yakuzaishi Chosa [The National Physician Census 2008]. Tokyo: MHLW, 2009 (in Japanese).
22. Ministry of Internal Affairs and Communications. Kokusei chousa 2010 [The population census 2010]. Tokyo: MIAC, 2010 (in Japanese).
23. Cabinet Office, Government of Japan. Kenmin keizai keisan [Prefectural economic status]. Tokyo: The Office, 2008 (in Japanese).
24. Matsumoto M, Inoue K, Farmer J, Inada H, Kajii E. Geographic distribution of primary care physicians in Japan and Britain. Health & Place 2010; 16: 164-166.
25. Bain J. Barriers to new competition. Cambridge: Harvard University Press, 1956.
26. Tanihara S, Kobayashi Y, Une H, Kawachi I. Urbanization and physician maldistribution: a longitudinal study in Japan. BMC Health Services Research 2011; 11: 260.
27. Matsumoto M, Inoue K, Kajii E. Definition of "rural" determines the placement outcomes of a rural medical education program: analysis of Jichi Medical University graduates. Journal of Rural Health 2010; 26: 234-239.


