'The world is changing and so are our caseloads' (p4)1. Internationally, medical and allied health professions have recognized that with these changes comes a responsibility to ensure accessible, equitable and appropriate services for all citizens, while at the same time developing a sense of academic and service leadership among students. This commitment is reflected in the UN Millennium Development Goals and the WHO's goals related to equity in health care. In addition, current methods of teaching and training need to be reviewed in order to best prepare students to meet these prerogatives.
The task of educating and preparing students for clinical practice has become increasingly daunting for a number of reasons, some of which relate to changing caseloads and student bodies2,3. The South African context provides some particularly compelling examples of changing caseloads and research in this setting provides valuable insights for clinicians and educators working in other contexts. The country is diverse in terms of its people, languages and cultures, geography and socio-economic statuses. In recent years, the country has witnessed the devastating effects of social inequalities, in part linked to the HIV/AIDS epidemic. These include the deterioration of the traditional nuclear family and an increasing number of orphans; startling increases in poverty and malnutrition; an ongoing lack of basic service delivery; an increasing number of immigrants entering South Africa from neighbouring countries; and an increase in physical, sexual and substance abuse. Rural areas in particular remain underdeveloped with limited access to basic services and health care4.
Defining the concept of 'rural' is a difficult task. Both local and international authors have acknowledged the ongoing debate in this regard5-7. The complexities of the South African context seem to make it even more difficult to consolidate a definition and the Department of Health has acknowledged the need to formally define concepts such as 'rural', 'rurality' and 'remoteness'8. In South Africa, the concept of 'rural' generally refers to a sparsely populated area outside of a metropolitan area with limited access to healthcare services5. Rural areas include, but are not limited to, large settlements in former homelands that were created during the apartheid regime9, or tribal villages, homesteads and rural farmland10. Forty-six percent of the population in South Africa resides in rural areas11. It should be noted that many rural areas in South Africa face conditions of extreme poverty, and rurality and poverty are thus intertwined8.
For the purpose of this study, 'rural' is considered to refer to remote areas with poor infrastructure, poor basic service provision (water and electricity), low levels of literacy, high levels of unemployment, limited access to health and education services, and high incidence of communicable diseases such as HIV/AIDS. These factors are compounded by restrictions in employment opportunities, lifestyle choices and access to services, and poverty.
Rural areas have become increasingly common workplaces for medical and allied healthcare graduates in South Africa as a result of the introduction in 2003 of a compulsory community service year for all allied health professionals. Although work in such contexts might be considered 'non-traditional' by some authors, in a climate of ever-increasing internationalization and globalization there is a need to prepare graduates to embrace the challenges of work in these contexts12.
The task of providing services in challenging contexts may be daunting to new graduates if adequate preparation is not provided through the curriculum13-15. In addition, students may feel anxious about providing therapy to clients with different linguistic and cultural backgrounds to their own16. It is clear that students need to be prepared in a way that enables confidence, leadership and reflective practice rather than one which provokes a sense of anxiety or inadequacy. Although curricula around the world have increasingly attempted to provide students with the necessary support17-20, challenges persist and implementing training in a meaningful and practical manner remains demanding, especially when the needs of students are in flux3.
A number of approaches to preparing students for work in challenging contexts and rural settings have been employed over the past few decades. One of the most common approaches involves rural fieldwork placements or experiential practica and this approach has been documented in both the local and international literature across a number of health professions15,21-24. However, research into fieldwork placements and experiential practica has predominantly focused on whether students benefited from such practica and whether the practica influence students' decisions to work in a rural area25-28. There appears to be limited research that provides insights into how exposure to rural community work through a practicum might shape students' responses to the challenges and realities of working in these contexts. This study therefore aimed to explore the shifts in perception of a group of speech-language therapy and audiology students towards rural community work before and after completing a practicum in a rural community in South Africa. The authors attempt to answer the question of how exposure to rural work in challenging contexts has an impact on these shifts in perception, and they consider the implications of this research for training and service provision.
Background to the practicum
A four-day practicum took place in a rural community in Bushbuckridge, Mpumalanga (this community is described extensively in the literature29). This area is characterized by extreme poverty, lack of development, poor infrastructure and limited provision of municipal services. High levels of unemployment have resulted in a large number of older women living in the area as men migrate to the cities in search of work. The area is also characterized by limited access to education and information; a lack of basic services in the area, including health care; and a high incidence of HIV/AIDS.
The students who participated in this study were being trained via a four-year undergraduate degree. Despite plans to promote transformation, most students spoke English as their first language and had limited knowledge of other official languages. By the end of their third year, students had received most of their theoretical input on communication disorders and management; health principles; and the cultural, linguistic and ethical aspects of community work. They had also engaged in a variety of practica at various urban and suburban sites; however, at this stage of their study they had had limited exposure to rural communities and opportunities to provide services in such contexts.
Prior to the practicum, the students received a series of lectures on ethnographic research methods and the outcomes for the practicum were presented. These outcomes included: conducting ethnographic observations; engaging with community members; learning how to identify barriers, needs and resources in a community; learning how to critically reflect on experiences within the community; and considering modifications to traditional therapy approaches.
The practicum also incorporated basic audiological clinical tasks as part of an established, sustainable service programme in the community, as well as a programme of structured observations with the aim of sensitizing students to rural community work and contextual issues. Speech-language therapy services were not included in this practicum for a number of reasons, including the fact that such a service was not at the time established in this community and there would have been little chance of follow-up if a service were offered on the practicum. Although a primary healthcare clinic had recently been built in this particular community, the clinic lacked staff and equipment and only basic nursing services were offered. The closest centre for comprehensive speech therapy and audiology services was approximately 70 km away.
Through this practicum it was hoped that the students would develop a better sense of professional identity and insight into how they might go about establishing and providing services in a rural community. The authors were under no illusions that this brief practicum would thoroughly prepare the students for rural community work, but rather expected that it would start a process of preparation and encourage awareness of some of the challenges inherent in such contexts.
As part of the practicum, the students conducted observations on a rotational basis in various contexts, including a primary healthcare clinic, nursery school, primary school, the waiting area outside the audiology clinic, and during home-based care visits and community activities such as market day. An example of the observation guidelines given to students is provided (Fig1). Observations were followed by group debriefing discussions, which were facilitated by both authors in their capacity as educators. The students were required to journal and reflect on their observations, their perceived professional role and their engagement with the audiology activities.

Figure 1: Example of structured observation guidelines provided to students.
The study used qualitative methods of analysis to allow for detailed exploration of the students' insights. One week prior to the practicum, the students were required to complete an anonymous open-ended questionnaire (Fig2). This questionnaire explored aspects such as their expectations of the practicum; perceived challenges and benefits of working in rural communities; expectations of the type of cases they might encounter; perceptions of preparedness for the practicum; considerations that might need to be taken into account when working in rural areas; and adaptations that may need to be made to therapy equipment. Immediately after the students' return from the practicum, they completed a follow-up questionnaire that probed the same areas as the pre-practicum questionnaire, which enabled the authors to note how exposure to rural community work through a practicum shaped students' responses to the realities of working in these contexts (Fig2). The questionnaires were based on both local and international literature that documents some of the most common difficulties facing new graduates working in challenging contexts, as well as on the authors' own anecdotal experiences of coordinating community work practica14,15,23.

Figure 2: Pre- and post-practicum questionnaires.
Twenty-five third-year students took part in the practicum. All students in the class were invited to participate in the study, although it was stressed that participation was voluntary. Those students who chose to participate were asked to complete the questionnaire and submit it anonymously into the authors' assignment boxes. All of the students completed the pre-practicum questionnaire while only 22 post-practicum questionnaires were completed. The student group was all female and the average age of the students was 20 years.
Each questionnaire was assigned a number ('Pr' denotes a pre-questionnaire response and 'Po' denotes a post-questionnaire response). The questionnaires were analysed qualitatively using principles of coding30 and thematic analysis31. To ensure objectivity of findings and a rigorous analytic process, both authors conducted the analysis simultaneously32. The results have been presented in a tabular format in order to better make sense of the data and highlight the salience of the themes. The data were tabulated according to the students' responses to the questions and a comparison of the pre- and post-practicum questionnaires was conducted. Thereafter, relevant themes emerged and were categorized according to the frequency in which they appeared. It is important to note that the tables include the number of responses counted across the data set and not the number of students who gave those responses. It was decided to analyse and present the data in this manner in order to highlight the salience of the themes that emerged.
Ethics approval
Ethical clearance was received from the University of the Witwatersrand Ethics Committee for the various research activities that took place during the practicum (clearance number M10125). Verbal and written information regarding the study was provided to, and consent was sought from, the students. It is acknowledged that power differentials between students and lecturers do exist in this type of research, which may have had an impact on the veracity of the students' responses. Students were not allocated marks for this practicum because it was felt that any evaluation might have interfered with their engagement in the activities.
There appeared to be a clear distinction between students' emotional and personal expectations of and responses to the practicum and their clinical expectations of and responses to the practicum. Although these types of responses are perhaps not unexpected, the envisioned outcomes for the practicum had focused heavily on clinical experience outcomes rather than on emotional and personal growth. As the results demonstrate, emotional responses seem to drive the processes involved in students' appreciation and understanding of the realities of work in a rural community in the South African context.
Emotional and personal expectations and responses
Anxieties: Students indicated a number of anxieties before the practicum, as detailed (Table 1). Anxieties typically focused on unsanitary conditions, language and cultural issues, and intra-personal issues. Some students were unsure of what to expect from the practicum - 'I'm not entirely sure what to expect. I'm nervous at this stage' [Pr19] - while others focused on issues such as 'being away from home' [Pr23, Pr24] or indicated anxiety about 'not knowing enough' [Pr12].
Table 1: Anxieties expressed pre- and post-practicum
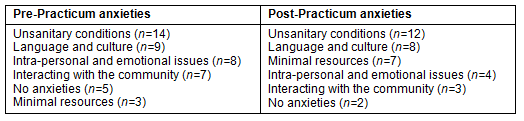
The most commonly expressed anxiety was that of infection control and fear of unsanitary working conditions: '[I could work in a rural community] if I get over my germ issues' [Pr20] and '[I'm concerned about] infection control, sanitation, hygiene' [Pr4].
Despite the heavy burden of HIV/AIDS in this area, only one student specifically mentioned a fear of contracting the virus, although others alluded to it by expressing a fear of transmission of communicable diseases. The students' anxieties are also interesting in light of the fact that they were well prepared for the infection control necessary for audiological work and they received input on infection control and HIV/AIDS from the time they entered the degree. Their focus, however, seemed to be exclusively on how they might be affected by a communicable disease and poor infection control rather than on the effect that these diseases have on communities.
Although the number of anxieties expressed by the students decreased somewhat across the pre- and post-practicum questionnaires, an increase was noted in anxieties related to working in a resource-poor setting in the future. A slight decrease was noted in fears of a personal nature (eg hygiene) and anxieties related to interacting with the community.
It was interesting to note that 5 students pre-practicum and two students post-practicum listed no anxieties. For some students, the desire to make a difference and the challenges presented by the practicum may have overridden any sense of anxiety. However, the apparent lack of anxieties among some students is concerning given the fact that the challenges posed by rural community work can be anxiety-provoking and emotionally draining even for qualified and experienced therapists.
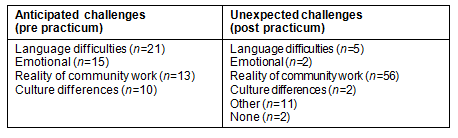
Challenges: Before the practicum, students generally indicated that they felt well prepared theoretically and they were able to realize the benefits of previous practica in urban contexts. However, they did not necessarily feel emotionally prepared for this practicum, as indicated by the high number of emotionally-related responses (Table 2). Pre-practicum, a number of students indicated that they expected to be emotionally challenged by the practicum and several students expressed feelings of inadequacy in this regard. For example, some students felt that the practicum would be emotionally difficult for them, were nervous about being forced out of their comfort zone and fearful about being confronted with the reality of patients' situations and life stories (eg 'sad cases where something tragic has happened' [Pr22]).
In the post-practicum questionnaires, only two students specifically mentioned emotionally-based challenges experienced on the practicum. Most challenges related to issues such as the reality of community work and coping with language barriers.
Table 2: Perceived challenges of the practicum
Shifting from an intrapersonal to an interpersonal focus: A shift from an intrapersonal to an interpersonal focus was noted in the post-practicum questionnaires. In the pre-practicum questionnaires, a number of responses focused on students' personal fears, anxieties and emotional responses. In the post-practicum questionnaires, this intrapersonal outlook seemed to shift towards more of an interpersonal focus on the community's challenges, lack of resources and lack of access to health care.
The pre-practicum questionnaires also highlighted a focus on intrapersonal factors in terms of expectations and perceived benefits of the practicum, rather than on altruistic factors such as offering a service to the community (Table 3). For example, students tended to focus on how the practicum would provide them with improved skills, exposure and preparation for community service. Students also tended to focus rather naively on the personal growth they expected to receive: for example, the practicum would be 'eye opening' [Pr5], allow them to 'make a difference' [Pr10], remind them to be 'grateful for what I have' [Pr23], provide 'spiritual growth and personal growth' [Pr21] and provide opportunities to 'experience how other less fortunate communities live' [Pr20]. In the pre-practicum questionnaire, students could not identify with the community and did not have any prior understanding of the community's needs, and as a result they seemed unable to prioritize goals in terms of how they might make a difference in the community.
This focus on intrapersonal benefits was also reflected in the post-practicum questionnaires, but with some subtle changes whereby students acknowledged how much they take for granted, both in health care and in everyday life. In the post-practicum questionnaires, several students indicated a greater understanding of how they fit into a common humanity, with statements such as 'no matter where we are all from, everyone is still human' [Po25], 'all people have the same needs' [Po24] and 'I live in a bubble in my little community' [Po20]. Although students still tended to adopt a somewhat ethnocentric viewpoint, they portrayed a greater sense of altruism and humility, reflected in statements such as 'there are people much worse off than us yet they have more smiles on their faces than we do' [Po2] and 'I realize how many other people need our help' [Po22]33. Ten students described their experience on the practicum as 'amazing', which reflects the significant personal impact that the practicum had on many of the students.
Table 3: Perceived benefits and expectations versus actual experience of the practicum

Clinical expectations and responses
Preparedness: As described in other studies, most students indicated that they felt prepared theoretically for the practicum13. Despite this, the pre-practicum questionnaires revealed a great level of anxiety in terms of putting into practice what they had learnt in theory and generalizing skills learnt in one setting into another setting. The students were concerned about how they would interact with the community given language and cultural differences, and one student was concerned that she might have to interact with a traditional healer.
When asked about the type of cases the students might expect to see, concerns about interacting with people with brain damage or psychological disorders were noted, as were concerns about encountering 'unusual cases'. In addition, a few students indicated insecurity regarding treating patients who did not ascribe to a biomedical viewpoint. Some responses indicated a distorted expectation that students would encounter completely different kinds of cases to what they would typically see in an urban setting: for example, one student expected to 'see cases from a rural area and how they differ from what we've been exposed to' [Pr26].
Post-practicum, most students indicated that the practicum had provided excellent learning opportunities and tremendous benefit in terms of clinical skills, such as taking a case history, working with ad hoc interpreters, engaging with stakeholders and healthcare workers in the community, and performing specific audiology tasks. The practicum appeared to give students confidence in their abilities and a greater degree of flexibility in their clinical work: 'It taught me to think on my feet and improvise' [Po19].
Considerations for rural community work: Before the practicum, students seemed to have an idea of basic contextual issues that may need to be taken into account when working in rural community contexts, such as gender, access, ethics, religion, education level, transport, follow-up care, infrastructure, basic resources, community expectations, openness to urban views and consideration of patient needs, among others (Table 4). However, there seemed to be a mismatch between the students' sociological understanding and how they might offer clinical services that incorporate a consideration of these issues. Students showed a lack of understanding of rural community contexts, despite receiving theoretical input and working with people from impoverished communities during practica in urban contexts.
Post-practicum, a substantial change was noted in students' understanding of the realities of rural community work. For example, one student stated that 'I was made very aware of how difficult it is to get healthcare in a rural area and how limited resources as well as skills are in a rural area. I knew that obviously a rural area would not have the same resources as a city but I was still shocked as to how limited it really is' [Po7]. Another student indicated that she had 'learnt to prioritise for the community and not stick to learned structures' [Po21], thus demonstrating an awareness of the need for flexibility and problem-solving skills in this context.
Table 4: Considerations that need to be taken into account when working in communities
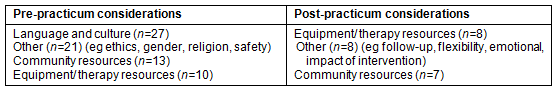
Language and cultural issues: Students' perceived challenges pre-practicum focused heavily on language and cultural differences - issues that are often emphasized in lectures - and not on issues of access, health care or poverty. In the pre-practicum questionnaires, students tended to recite what had been discussed in lectures, indicating superficial insight into these issues. For example, comments were made about '[community] members who cannot communicate in English' [Pr22] and 'the perception we get is that they are steeped in their culture' [Pr17]. These comments link to what some authors have called 'cultural tourism' or the idea that people from other cultures are somewhat exotic34.
The issue of language and cultural considerations and adaptations was a strong focus in the pre-practicum questionnaires. Language barriers were mentioned by 21 students as a pre-practicum anxiety, with comments such as '[I'm anxious about working with] ... patients who have never even spoken English before' [Pr20]. However, students generally indicated that they felt able to cope with the challenge of language barriers, perhaps as a result of an increased curricular focus on these issues. Although students mentioned the need to avoid cultural bias, to have respect for and develop trust with the community, to have 'cultural considerations' [Pr25] and 'cultural sensitivity' [Pr16, Pr23], it did not appear that they had a full understanding of what these terms meant or implied in a practical sense.
Post-practicum, a shift in students' perceptions of these challenges was noted. These included taking cultural and linguistic considerations into account, taking time to become familiar with language and culture, and showing respect for the community's beliefs and views. However, the general lack of apparent growth in insight and understanding into language and cultural issues even after the practicum was concerning, as evidenced in comments such as 'I would just try change my case history questions to their language or perhaps use more layman's terms to try break the language barrier' [Po4] and 'I would learn in a different language how to say 'listen for the beep, don't swallow and keep still'' [Po20].
Equally concerning was the fact that both pre- and post-practicum, students believed that adapting their therapy approach and materials to make them culturally and linguistically appropriate meant simplifying what they were doing (eg using simple English), 'trying the words of a different language' [Pr7], vague suggestions such as 'multicultural adaptations' [Pr20], 'more pictures and simpler instructions' [Pr24], '[focusing on] very basic needs' [Po13] and 'not using pictures of BMWs and laptops' [Po21]. One student, however, did indicate that 'the best equipment in this setting is the therapist - her imagination, use what's available in the community for the community - that way it's more relevant' [Po9].
Discussion
The need to prepare students for work in challenging contexts and rural areas is undisputed. Importantly, this study confirms that such preparation cannot be achieved through lectures alone and that this type of work is probably best learnt as part of a practicum. In the pre-practicum questionnaire, the students' responses were often stereotypical and vague, and it seemed that they were merely repeating much of what they had heard in lectures. Their pre-practicum responses also appeared to be influenced by deeply ingrained perceptions, their upbringing and background, and minimal exposure to poverty and the realities of challenging contexts.
The practicum described in this article appeared to be a largely positive learning experience for students, as evidenced in some of the perceived changes in clinical and emotional perspectives, and the changes from an intrapersonal to an interpersonal focus. Students demonstrated some growth in application of knowledge, flexibility, creativity and sensitivity towards contextual factors. The practicum also allowed the students to begin to consider their professional role as well as practical and personal issues involved in working in challenging contexts. In the words of one student, the practicum provided a powerful opportunity to witness and experience 'the reality of poverty and the real priorities of the community' [Po21]. The study thus confirms the findings of other authors who have concluded that rural practica hold significant potential to shape students' choices about working in rural contexts35,36.
These results are important when one considers the notions of academic and service leadership, both of which are crucial for building capacity in rural healthcare systems and achieving improvements in rural healthcare provision37,38. There is a need to develop rural health leaders who are not only clinically competent but who are accountable, understand the 'bigger picture' of community goals and collaboration, and are able to devise innovative solutions to community problems38. The results of this study also highlight the link between social accountability and the different kinds of leadership required for work in rural healthcare contexts, including theoretical, ethical, policy, academic, servant and clinical leadership39.
The findings of this study do raise a number of additional issues for discussion, which are of relevance not only to the professions of speech therapy and audiology, but also to other health and social service professions. While many curricula around the world include a focus on working in rural communities and challenging contexts, and while there has been a rise in the popularity of service learning, the results of this study point to the need to reconsider how students are prepared for this type of work. A one-off practicum is probably not going to provide adequate preparation, as reflected in some of the students' post-practicum responses, which reflected significant anxieties related to work in a rural context as well as a lack of understanding of how to implement appropriate therapy and make suitable modifications to materials. The results suggest the importance of repeated early exposure to challenging contexts, as suggested by other authors, or pre-placement visits to prepare students emotionally and theoretically for longer placements40.
Students need to be taught how to provide sustainable, quality interventions in communities but this requires a comprehensive understanding of the priorities, challenges and social contexts of communities. Earle's suggestion41 that sociological principles should be included in the speech-language therapy curriculum seems valid here and it may also prove valuable to involve community members in curriculum development and teaching in order to promote community-oriented and community-based learning42. In addition, a 'token' course on rural work is clearly not going to equip students adequately; rather, the approach to preparing students for work in challenging contexts and rural communities should be a sustained and integral philosophy that is introduced early on in the curriculum12.
While it is acknowledged that the students' background and lack of experience of such contexts may have contributed to their anxieties, the unfamiliarity and uncertainty of working in challenging contexts may also have been a contributing factor16. The real-world experiences of working in challenging contexts can never be fully prepared for in the classroom and challenging contexts may still evoke anxiety despite theoretical preparation43-45. If students do not receive sufficient exposure to, hands-on teaching in and debriefs about community settings, their anxieties and fears may lead to avoidance of work in such contexts, thus perpetuating the lack of much-needed service delivery in these communities46. Without appropriate preparation, graduates who must complete community service or who choose to work in such settings may take longer to adjust to their role in the community in which they work or may face burnout14. Preparation of students, educators and communities is key to ensuring that rural practica provide positive learning experiences, as highlighted by other authors47-49.
In order to sensitize students to challenging contexts and equip them to work effectively in these settings, educators need to understand and engage with these contexts too. However, this can only be done in collaboration with community informants and clinicians working in the field, as well as through sustained research efforts that explore the needs of communities. An important part of the teaching and learning process involves modelling and directing students towards community strengths and challenges, as well as teaching students how to acknowledge and overcome their anxieties about working in challenging contexts43. This requires that educators reflect on their own attitudes, experiences, biases and anxieties towards community work.
Study limitations
Although limited to a small group of students from one particular university, the data presented in this study provide valuable insights into how rural practica shape student perceptions and experiences of rural work. While it would have been optimal to have probed student responses further via interviews or focus groups, ethical obligations meant that the authors, as educators, could not engage in such data collection. For this reason, responses were limited to what was expressed in the questionnaires.
Given the inherent challenges linked to poverty and resource limitations, the South African context provides an interesting learning opportunity for students and educators. The findings of this study offer some important implications for student training both locally and internationally. A review of curricula is required, with a specific focus on issues such as the particular outcomes for rural placements as well as at what point and over what time period such placements are introduced. Future research should strive to extrapolate the underlying reasons behind the findings of this study using a combination of methods such as participant observation, interviews, focus groups and reflective journaling. Although the way in which teaching and practica are approached is university-specific and some institutions may have already developed better models and approaches to preparing students for rural community work, the results of this study highlight the opportunities that rural practica provide at an undergraduate level for growth in sensitivity to community issues and clinical and leadership skills.
Acknowledgements
The authors' involvement in this practicum was funded by the School of Human and Community Development at the University of the Witwatersrand. The authors thank the group of student participants for their candid responses.
References
1. Penn C. Cultural safety and the curriculum: recommendations for global practice. Perspectives on Global Issues in Communication Sciences and Related Disorders 2011; 1: 4-11.
2. Goldstein E. Social work education and clinical learning: yesterday, today, and tomorrow. Clinical Social Work Journal 2007; 35: 15-23.
3. McAllister L, Bithell C, Higgs J. Innovations in fieldwork education: current trends and future directions. In: L McAllister, M Paterson, J Higgs, C Bithell (Eds). Innovations in allied health fieldwork education: a critical appraisal. Rotterdam: Sense Publishers, 2010; 1-16.
4. Coovadia H, Jewkes R, Barron P, Sanders D, McIntyre D. The health and health system of South Africa: historical roots of current public health challenges. The Lancet 2009; 374: 817-834.
5. Couper I. Rural hospital focus: defining rural. Rural and Remote Health 3: 205. (Online) 2003. Available: www.rrh.org.au (Accessed 26 November 2012).
6. Muula A. How do we define 'rurality' in the teaching on medical demography? Rural and Remote Health 7: 653. (Online) 2007. Available: www.rrh.org.au (Accessed 26 November 2012).
7. Peters J, Jackson R. The impact of rurality on health: systematic review. Rural Evidence Research Centre. (Online) 2005. Available: http://www.rerc.ac.uk/findings/documents_health/H2Rreview_Short.pdf (Accessed 26 July 2012).
8. Department of Health. Human resources for health South Africa: HRH strategy for the health sector: 2012/13 - 2016/17. (Online) 2011. Available: http://www.info.gov.za/view/DownloadFileAction?id=152486 (Accessed 26 July 2012).
9. Development Bank of South Africa (DBSA). Comprehensive rural development programme: DBSA partners and stakeholder forum. (Online) 2010. Available: http://www.dbsa.org/PartnersForum/Documents/CRDP%20PRESENTATION%20DBSA.pdf (Accessed 26 July 2012).
10. Statistics South Africa. Census 2001: Investigation into appropriate definitions of urban and rural areas for South Africa - discussion document. (Online) 2003. Available: http://www.statssa.gov.za/census01/html/UrbanRural.pdf (Accessed 26 July 2012).
11. University of Cape Town. The WHO global policy recommendations on increasing access to health workers in remote and rural areas through improved recruitment and retention: the South African Context. Discussion Document Version 1. Cape Town: University of Cape Town, 2011.
12. McAllister L, Penn C, Smith Y, van Dort S, Wilson L. Fieldwork education in non-traditional settings or with non-traditional caseloads. In: L McAllister, M Paterson, J Higgs, C Bithell (Eds). Innovations in allied health fieldwork education: a critical appraisal. Rotterdam: Sense Publishers, 2010; 39-48.
13. Loud J. Recent graduate preparedness for rural employment. In: Proceedings, 6th National Rural Health Conference; 4-7 March 2001; Canberra, ACT; 2001.
14. Penn C, Mupawose A, Stein J. From pillars to posts: some reflections on community service six years on. South African Journal of Communication Disorders 2009; 56: 8-16.
15. Trembath D, Wales S, Balandin S. Challenges for undergraduate speech pathology students undertaking cross-cultural clinical placements. International Journal of Language and Communication Disorders 2005; 40: 83-98.
16. Kai J, Beavan J, Faull C, Dodson L, Gill P, Beighton A. Professional uncertainty and disempowerment responding to ethnic diversity in health care: a qualitative study. PLoS Medicine 2007; 4: e323.
17. American Speech-Language-Hearing Association. Knowledge and skills needed by speech-language pathologists and audiologists to provide culturally and linguistically appropriate services. (Online) 2004. Available: www.asha.org/policy (Accessed 1 March 2012).
18. Hammond C, Mitchell P, Johnson M. Academic and clinical preparation for cultural and linguistic diversity in speech-language pathology: program director perspectives. Contemporary Issues in Communication Science and Disorders 2009; 36: 63-76.
19. Reid S, Cakwe M. Collaboration for health equity through education and research. The contribution of South African curricula to prepare health professionals for working in rural or under-served areas in South Africa: a peer review evaluation. South African Medical Journal 2011; 101: 34-38.
20. Rourke J. How can medical schools contribute to the education, recruitment and retention of rural physicians in their region? Bulletin of the World Health Organisation 2010; 88: 395-396.
21. Reid S, Couper I, Volmink J. Educational factors that influence the urban-rural distribution of health professionals in South Africa: a case-control study. South African Medical Journal 2011; 101: 29-33.
22. Reid S, Cakwe M. The contribution of South African curricula to prepare health professionals for preparing to work in rural or under-served areas in South Africa: a peer review evaluation. South African Medical Journal 2011; 101: 34-38.
23. McAllister L, Paterson M, Higgs J, Bithell C (Eds). Innovations in allied health fieldwork education: a critical appraisal. Rotterdam: Sense, 2010.
24. Maley M, Worley P, Dent J. Using rural and remote settings in the undergraduate medical curriculum: AMEE Guide No. 47. Medical Teacher 2009; 31: 969-983.
25. Bushy A, Leipert B. Factors that influence students in choosing rural nursing practice: a pilot study. Rural and Remote Health 5: 387. (Online) 2005. Available: www.rrh.org.au (Accessed 26 November 2012).
26. Johnson G, Blinkhorn A. Student opinions on a rural placement program in New South Wales, Australia. Rural and Remote Health 11: 1703. (Online) 2011. Available: www.rrh.org.au (Accessed 26 November 2012).
27. MacRae M, van Diepen K, Paterson M. Use of clinical placements as a means of recruiting health care students to underserviced areas in Southeastern Ontario: part 1 - student perspectives. Australian Journal of Rural Health 2007; 15: 21-28.
28. Tolhurst H, Adams J, Stewart S. An exploration of when urban background medical students become interested in rural practice. Rural and Remote Health 6: 452. (Online) 2006. Available: www.rrh.org.au (Accessed 26 November 2012).
29. Tollman S, Kahn, K. Health, population and social transitions in rural South Africa. Scandinavian Journal of Public Health 2007; 35: 4-7.
30. Rapley T. Some pragmatics of data analysis. In: D Silverman (Ed). Qualitative research: issues of theory, method and practice, 3rd edn. Los Angeles: Sage, 2011; 273-290.
31. Braun V, Clarke V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006; 3: 77-101.
32. Patton M. Qualitative research & evaluation methods, 3rd edn. Thousand Oaks, CA: Sage, 2004.
33. Daniels K, Swartz L. Understanding health care workers' anxieties in a diversifying world. PLoS Medicine 2007; 4(11): e319.
34. Ramsden I. Cultural safety and nursing education in Aotearoa and Te Waipounamu (PhD thesis). Wellington, New Zealand: Victoria University of Wellington, 2002.
35. Eley D, Baker P. The value of a rural medicine rotation on encouraging students toward a rural career: clear benefits from the RUSC Program. Teaching and Learning in Medicine 2009; 21: 220-224.
36. Kaye D, Mwanika A, Sewankambo N. Influence of the training experience of Makerere University medical and nursing graduates on willingness and competence to work in rural health facilities. Rural and Remote Health 10: 1372. (Online) 2010. Available: www.rrh.org.au (Accessed 26 November 2012).
37. Size T. Leadership development for rural health. North Carolina Medical Journal 2006; 67: 71-76.
38. Habjan S, Kortes-Miller K, Kelley M, Sullivan H, Pisco L. Building capacity in rural health services: the effect of continuing education. In: J Kulig, A Williams (Eds). Health in rural Canada. Vancouver: UBC Press, 2012; 118-136.
39. Worley P, Murray R. Social accountability in medical education - an Australian rural and remote perspective. Medical Teacher 2011; 33: 654-658.
40. Littlewood S, Ypinazar V, Margolis S, Scherpbier A, Spencer J, Dornan T. Early practical experience and the social responsiveness of clinical education: systematic review. BMJ 2005; 331: 387-391.
41. Earle S. Teaching sociology within the speech and language therapy curriculum. Education for Health 2001; 14(3): 383-391.
42. Iputo J. Faculty of Health Sciences, Walter Sisulu University: training doctors from and for rural South African communities. MEDICC Review 2008; 10: 25-29.
43. Kai J, Spencer J, Wilkes M, Gill P. Learning to value ethnic diversity - what, why and how? Medical Education 1999; 33: 616-623.
44. Dalton L. Time as a source of conflict: student nurse experiences of clinical practice in a rural setting. Rural and Remote Health 4: 256. (Online) 2004. Available: www.rrh.org.au (Accessed 26 November 2012).
45. Denz-Penhey H, Murdoch C, Lockyer-Stevens V. 'What makes it really good, makes it really bad.' An exploration of early student experience in the first cohort of the Rural Clinical School in the University of Western Australia. Rural and Remote Health 4: 300. (Online) 2004. Available: www.rrh.org.au (Accessed 26 November 2012).
46. Orpin P, Gabriel M. Recruiting undergraduates to rural practice: what the students can tell us. Rural and Remote Health 5: 412. (Online) 2005. Available: www.rrh.org.au (Accessed 26 November 2012).
47. Bennett P, Jones D, Brown J, Barlow V. Supporting rural/remote primary health care placement experiences increases undergraduate nurse confidence. Nurse Education Today (in press).
48. Gupta S, Murray R, McDonell A, Murphy B, Underhill A. Rural internships for final year students: clinical experience, education and workforce. Rural and Remote Health 8: 827. (Online) 2008. Available: www.rrh.org.au (Accessed 26 November 2012).
49. Killam L, Carter L. Challenges to the student nurse on clinical placement in the rural setting: a review of the literature. Rural and Remote Health 10: 1523. (Online) 2010. Available: www.rrh.org.au (Accessed 26 November 2012).

