South Africa has the dual burden of Human Immunodeficiency Virus (HIV) and tuberculosis (TB) in catastrophic proportions: in 2009 the public health sector antenatal HIV prevalence was 29.4%1 and the reported cases of TB were 782 per 100 0002. There are inequities in health service provision which predominantly follow a rural-urban divide, which in part reflects and is aggravated by a public-private sector divide3. In this context South African has made a policy decision to integrate HIV and TB programs4. How this has been implemented and the possible implications for rural-urban equity in access to integrated, quality care is examined in this study.
Integration is defined in the literature as 'a variety of managerial or operational changes to health systems to bring together inputs, delivery, management and organization of particular service functions'5 as a means of improving access, quality, user satisfaction, equity and effectiveness. This study used this definition and applied it to both the primary prevention of HIV and TB, and to the care of infected individuals. The integration of HIV and TB programs is a logical step towards greater health system efficiency and a more patient-centered approach6,7. These are attractive incentives in a country such as South Africa where the health system at primary-care level is bedeviled by stark inequities in access3, poor quality of care8-10 and inefficiency11. Vertical programs are criticized for fragmenting the health services and creating competition for limited human and management resources12,13. There is limited evidence available from controlled studies on the efficiency and impact of integration5 but operational research suggests that integrated services are desirable. For example, intensified case-finding and treatment of TB in a mother-to-child HIV transmission prevention program has been shown to prevent mortality14, and HIV testing of patients with TB has increased access for co-infected patients to antiretrovirals15. A 2010 systematic review of integrated HIV/TB services found evidence that integration increases coverage of key services16, though few studies reported on relevant outcome indicators. Field experience of implementing integrated HIV and TB services has identified setting-specific operational barriers. Friedland et al describe the challenges in Malawi and South Africa, and warn against a ''one size fits all' public health approach'17, a sentiment echoed by others18,19. In the field of maternal and child health, Bhutta et al stress the need to consider existing infrastructure, and the types and numbers of health workers available when comparing the efficacy of integrating various interventions20.
A large program evaluation of HIV and TB services in a deep rural and an urban district in South Africa was conducted, and the individual results have been reported in separate publications21,22. In this article the implementation of HIV and TB integration is described and the rural and urban results are contrasted in relation to access to and quality of services to explore possible implications for equity.
Setting
South Africa has a district health system based on a primary healthcare approach in which clinics provide nurse-driven primary care, referring patients to district and regional hospitals for secondary-level care. Sampling was purposeful to select one urban and one deep rural district. Both districts were known to the researchers who had supported previous studies and built relationships with the respective district managers who were open to this evaluation process as part of a quality improvement initiative.
The sparsely-populated rural district was located in Kwa-Zulu Natal and had an antenatal HIV prevalence of 39.5%, with 46 geographically dispersed primary-care facilities serving 320 000 people (population density = 28/km2) and a primary-care utilization rate of 1.8 visits per person/year23. The densely-populated urban district was located in the Western Cape Province and had a lower, though still extremely high, antenatal HIV prevalence of 16.9%. This urban district is recognized as being better covered by health services than other urban areas, with its 146 primary-level facilities serving 3.4 million people (1318 people/km2) and a primary-care utilization rate of 2.7 visits per person/year24. In the rural district all facilities were run by the provincial authority, whereas in the urban district a historical division meant that both the provincial and local authority health services rendered services.
Data sources and analysis
In describing the model of integrated service delivery, the researchers drew from their observations gained through working in these two districts for over 5 years. This description was confirmed by local managers. In contrasting the access and quality of integrated services, secondary data were used that had been generated from two large evaluations of HIV/TB/Sexually Transmitted Infections (STI) programs, the rural evaluation conducted in December 2008 and the urban evaluation in May 2009. All the urban facilities and just over half the rural facilities were audited by audit teams consisting of local program supervisors and facility managers. The large geographical distances in the rural district prohibited the auditing of all clinics. Purposive sampling was performed to select rural clinics with a high burden of HIV/TB/STI disease and to ensure a geographic spread of facilities across the administrative sub-districts. The rationale was that the rural facilities should benefit maximally from a quality improvement initiative. Local knowledge ensured that both more and less remote facilities were included.
Audit tools were developed in an urban setting21 and then modified for use in rural areas22. The framework for the tools was based on an expanded health systems approach which UNICEF/WHO proposed for evaluating Prevention-Mother-to-Child-Transmission of HIV (PMTCT) programs25. The four evaluation domains were the: (i) extent to which clients receive integrated services; (ii) quality of care; (iii) availability of key resources; and (iv) system capacity to support quality care. In this study integration outputs was measured as the extent to which HIV or TB clients received other HIV/TB/STI prevention and care interventions. Tracer indicators were identified as, in an evaluation of this magnitude and scope, it was not possible to measure all aspects of the programs. While there was substantial congruence between the urban and rural indicator sets, some minor differences were necessary to ensure adequate construct validity in the different contexts and these affected two variables (mean number of professional nurses and doctors per facility, and percentage clinical staff trained in HIV Counselling and Testing [HCT]). Furthermore, the tools were amended between 2008 and 2009, which meant that two composite variables in the 2008 version (administered in the rural area) were separated into their component parts in the 2009 version (administered in the urban area). These differences are clearly indicated in the results.
A variety of data collection tools were used. The first part of a structured facility manager interview was self-administered by each facility manager or their nominated second-in-charge and was used to collect information on staffing and training. The second part of the structured facility manager interview was administered by the evaluation team. The team sought evidence of functional recall systems (defined as a locally-appropriate process with responsibility allocated to a person in a specific position and keeping to a pre-set time schedule for recall and follow up of patients who did not respond to original recall) and evidence of a drug stock control mechanism (a paper or electronic system with at least minimum and maximum stock levels and a defined trigger for ordering more drugs). Data collection tools further included a review of data in the routine health information system, an observational checklist for availability of drugs, equipment and supplies, and a series of patient folder (health record) reviews which collected clinical data on access and quality of care. The variables measured in the first part of the facility manager interview were all integers, and for the other tools the variable responses were 'yes', 'no' or 'not applicable'. Ten folders for review were randomly sampled from each of the following registers in each facility: HCT, antiretroviral therapy (ART) and TB. HIV patients who were in care but not yet receiving ART were sampled from the HCT register which shows which patients test positive. Their clinical notes were then reviewed to verify that they were in care (defined as at least two clinical visits) and not yet receiving ART. It was not possible to perform a full patient folder review for patients accessing HCT in the rural district because a patient folder was not issued for this service and notes were only kept in the HCT register.
Data were entered into excel spreadsheets and proportions calculated. Confidence intervals for proportions were calculated using a statistical calculator.
Ethics approval
Ethical approval for the research was obtained from the Senate Research Committee of University of the Western Cape (# 07/2/19).
The health services which were partners in designing and administering the tools gave consent, set the research agenda and agreed on the participatory methodology. They were also the main users of the research data. Managers and staff from the health services were involved in their official capacity with a mandate from their organization in accordance with their job descriptions which detail their role in monitoring and evaluating and quality improvement. All patient records were treated with confidentiality and the data extracted were recorded anonymously.
In the rural district, 26 of the 46 facilities (57%) were audited and in each of the 26 facilities the facility manager (or the nominated second-in-charge if the facility manager was not available) was interviewed; 52 consulting rooms were inspected and 569 folders reviewed. In the urban district all 146 primary-care facilities were evaluated and in each facility the facility manager (or the nominated second-in-charge if the facility manager was not available) was interviewed; 461 consulting and 224 counseling rooms were inspected and 5147 folders were reviewed.
In both districts the dominant model of integrated service delivery was co-location of the HIV prevention and TB diagnosis services in the same general primary-care facility which also offered other services such as child care, family planning, treatment of STI and chronic non-communicable disease care. This applied to all facilities in both settings. In the urban district, given the density of facilities, TB treatment was only offered in 63% facilities (n=92) but a number of facilities (defined as having a separate management and staff complement, even if a building or site might be shared) were on the same geographic site (eg a city and a provincial primary-care facility, a separate youth clinic and a primary level obstetric facility) which meant that 79% of the facilities (n=115) had TB treatment on-site. ART was offered at 18.5% of facilities (n=27). In the rural district TB treatment was co-located at all primary care facilities and ART was at 28% of facilities (n=13). In the rural district nurses provided these services with doctor support only at the district hospital. Urban facilities run by the provincial authority (one-third of urban facilities) were staffed with both nurses and doctors who all provided first-line services; urban facilities run by the local authority were staffed by nurses who provided first-line services and referred to doctors (either on site on a full or session basis, or at a neighboring facility). Doctors initiated antiretrovirals in both districts. Rural professional nurses tended to offer all services within their scope of practice within the same consultation; whereas urban doctors and nurses offered components of care at separate service points in the facility. In both settings HCT was offered at all facilities by nurses with lay counselors providing counseling support and ART was initiated by doctors only in a subset of accredited sites. Referral to a doctor in the rural district required additional transport and a journey of up to 100 km on roads in poor condition, while in the urban district it was available on-site or within 10 km on tarred roads.
Both districts had active, formal district management teams who were proactive in using health information and were using the audit results to improve services. Supervision was weaker in the rural area with only 46% of facilities having been visited by a Primary Health Care (PHC) supervisor and none by a HIV/TB program coordinator, compared with 100% in the urban area. The facilities were smaller in the rural area with smaller staff complements. Most rural facility managers were professional nurses responsible for clinical and managerial work; whereas urban facility managers had dedicated managerial roles.
Training coverage was fair, as shown (Table 1); however, there were many instances, especially in smaller rural facilities, where no-one had been trained in a particular service component. Assessment of system capacity is shown (Table 2). Stock-outs of drugs (ie no supply of drugs in the facility) were much more extensive in the rural district than the urban district (83% vs 23%, respectively, of the setting-specific basket of tracer drugs and stocks). In part this could be attributed to weaker stock control systems which could be addressed by facility-level action, but further enquiry also suggested deficiencies at district level related to transport logistics, and at regional and provincial level related to bulk procurement of drugs.
Table 1: Staffing levels and relevant training at primary care facilities
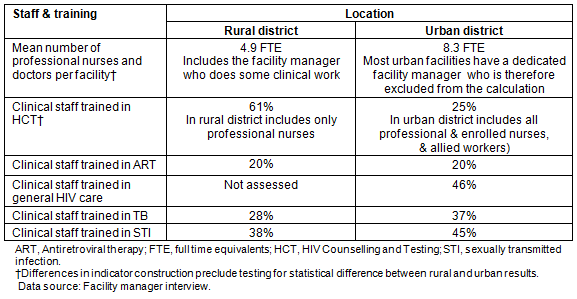
Table 2: Assessment of key systems (drug and stock procurement, and patient recall) at primary care facilities
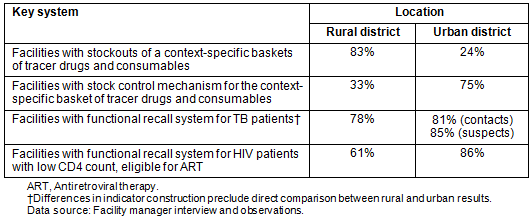
The extent of integrated service provision received by HCT, HIV positive (and in-care but not yet receiving ART), ART and TB patients is shown (Table 3). HIV testing was routinized in the care of TB patients in both the rural and urban districts (86.5% and 92.1%, respectively). Symptomatic screening for TB and STI was high in HCT patients in the urban district (both approximately 90%). Symptomatic TB screening in HIV positive patients not yet receiving ART and those on ART was poor in both the rural and urban settings (varying from 52% to 62%) but symptomatic STI screening was higher in these patients in the rural setting. Health workers' enquiry into clients' family planning requirements was poorly integrated across all patient groups in both settings (ranging from 27% to 48%) with the exception of ART patients in the rural setting (69.9%).
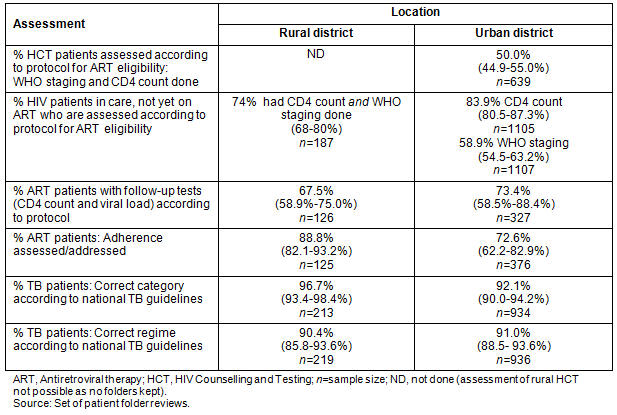
The quality of care is shown (Table 4). Patients gained access to ART through an eligibility assessment (based on their CD4 count and clinical stage) and appropriate referral. In the urban setting only 50% of HCT clients were adequately assessed; often they had a CD4 count performed but were not staged. In the patients who were HIV positive but not yet receiving ART, there were worrying gaps in both settings in assessment for eligibility. Likewise, routine laboratory monitoring of ART clients was sub-optimal in both settings (67% & 73% patients in the rural and urban settings, respectively). Assessing and addressing adherence was good in the rural setting (88.8%) and better than in the urban setting (72.6%). The management of diagnosed TB patients was good in both settings.
Table 3: Assessment of extent to which patients access integrated services
(combining HIV, TB, reproductive health preventative and early detection activities)
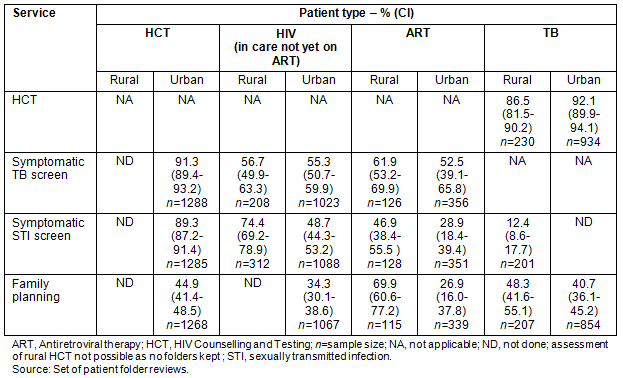
Table 4: Assessment of access and quality of care received by patients at primary care facilities
Discussion
The discussion considers the implications of locating HIV and TB services in the general primary care platform and the possible implications this has for rural-urban equity in access to integrated, quality care. It also discusses the dimensions of integration that have been implemented, again applying a rural-urban equity lens. Finally, the limitations of this study are discussed.
Equity implications of HIV/TB integration in rural and urban South Africa
This study describes the extent to which integration of HIV and TB services was achieved by co-location of services in the primary-care platform. It found there were a number of strengths in the primary-care platform across both rural and urban settings. This form of integration has been found to require more initial set up resources in terms of infrastructure (eg space for HCT counseling) and training of staff when compared with models of integration based on referral between services16. However, in South Africa the existing physical health infrastructure is strong with an extensive network of general primary-care facilities in both the rural and urban districts. Where existing health infrastructure and management are weak, vertical disease-specific programs may have the advantage of being targeted and have a higher chance of success6; however, in this study the physical infrastructure was found to be robust. These facilities offered a wide range of primary care services including immunization, antenatal care, family planning, TB case-detection and Directly Observed Treatment (DOTS), adult and child curative care, mental health. The location of HIV and TB services on this service platform meant that the scope of integrated HIV/TB care could potentially be extended to include other services which offer synergies with the HIV/TB program, such as family planning services and care for chronic non-communicable diseases (patients on long-term ART are at higher risk of developing certain chronic non-communicable diseases).
Co-location of services has been found to improve access and offer efficiency gains in areas where referral patterns and mechanisms are weak16. This is important in the South African context. Despite a heavy investment in a clinic building program11 sparsely-populated rural areas are still constrained in geographic access (seen in the lower PHC utilization rate) and this represents a major fault line in the rural HIV and TB services. In this context integrated services can promote equity as they maximize the benefit possible at each facility visit. However, in this study there were instances in the rural district where no nurse in a facility had received formal training for a particular aspect of HIV or TB prevention or care. Rural nurses worked without the support of a doctor, meaning that the opportunity for clinical mentorship was lost, and supervision was also weaker. There were more instances of essential drugs not being available in the rural district, which potentially undermines clinical care. This possibly points to a difference in management capacity within and beyond the districts. These factors could undermine the quality of care and need to be specifically addressed to ensure equity. It was, however, noteworthy that patients in rural care actually received more integrated care (symptomatic STI screening in HIV positive patients and assessment of family planning requirements in ART patients) as well as better quality of care (higher rates of adherence assessment and support in ART patients) than their urban counterparts. This is counter to the commonly held assumption of poorer care in rural areas. However, in general, the study showed that in both settings the integration and quality of HIV services could be improved. Family planning in particular is often neglected in the care of HIV and TB clients. The quality of care in the TB services (a more established service) was high in both settings, which at least suggests that there has not been a deterioration within integrated service settings.
Different dimensions of service integration and their equity implications
In this study the first dimension of integration found was across different diseases, in contrast to disease-specific services. Co-infected HIV/TB patients received care for both conditions from the general primary-care facilities. Furthermore, STI diagnosis and care and reproductive health services were also integrated into the services received by HIV and TB patients. This broader approach of integrating across a cluster of related services is significant when many references to integration in the literature have been confined to simultaneous treatment of co-infected patients requiring both anti-tuberculous and ART.
The second dimension of integration was that of bringing together prevention and care activities. For example, HIV patients were being screened for STI (an activity to reduce further transmission of HIV) and also their contraception needs were addressed (an activity which reduces unwanted pregnancy contributing to prevention of mother-to-child transmission). In this way it was possible to 'facilitate early detection and prevention of problems, even in the absence of explicit demand'26. Facility-based activities to detect and treat HIV, as well as to prevent new HIV infections, are likely to have impacted positively on population health by reducing the incidence of new cases of HIV27. Likewise, integrated TB case-detection strategies are likely to expedite appropriate care and reduce new infections. Although there are empirical studies on the integration of HIV prevention and care (eg Walton et al's work in rural Haiti28) - it is notable that in this evaluation the integration of prevention and care goes beyond a single program to involve the entire HIV/TB/STI/reproductive-health cluster of services. To date little has been written about this dimension of integration, the implementation of which could serve as a model for use in other high prevalence settings.
Limitations
A before-and-after study would have provided a stronger design. The authors are not able to comment on the effect that integration has had on quality, but rather provide a 'snapshot assessment' of quality within a service which intends to be integrated.
In this study two indicators were specifically modified to maximize their relevance to the rural context, which meant they could not be compared with the urban findings. These are 'Mean number of professional nurses and doctors per facility' and '% clinical staff trained in HCT'. The primary purpose informing the evaluations was to provide locally-relevant data as part of a district-led quality improvement process. Both districts had strong management teams committed to quality improvement. While the results are thus not representative of all rural and urban districts in South Africa and cannot be generalized the findings in these two districts, as an instance of HIV/TB integration, nevertheless throw up interesting issues for discussion and have important policy implications.
Purposive sampling of high HIV/TB burden facilities in the rural district may have introduced a bias skewed towards better service delivery as they may have received more management attention; however, this is a relative assessment since high levels of HIV and TB through the district have made improvement of HIV/TB services a district priority.
A further limitation is that the enquiry is limited to HIV, TB and STI patients. It would, for example, be informative to know what percentage of 'general' patients, such as those who are hypertensive or diabetic, were tested for HIV and to be able to compare this with the percentage of TB patients who were tested for HIV. It is likely, given the weight of HIV and TB in the burden of disease in South Africa, and the corresponding resources and attention allocated, that the integration of HIV and TB services has occurred more generally within primary-care services, but this was not measured.
There are two further dimensions of integration which have not been investigated because the focus of the evaluation was only on primary-care facilities in the two selected districts and did not extend to the community-based services, the referral hospitals and the other sectors which take health-related action. First, integration operating between the levels of service provision from community to primary, secondary and tertiary levels29; second, integration linking health services with health-related actions outside the health sector. This latter idea was put forward in an early ground-breaking WHO document on integration which argues that the primary health care approach defined in the Alma Ata Declaration broadens the challenge of integration to move from 'that of bringing together tasks and functions within health services to mobilizing health-related activities in other sectors, as well as the activities of families and communities, and linking them with health services' (p2)7. These last two dimensions of integration have the potential to improve health outcomes significantly but have not received sufficient attention in the recent international literature on integration. Integration of health services with intersectoral action for health together with community involvement can address the social determinants of health so fundamental to health outcomes30. In the South African context, despite a commitment to a comprehensive primary health care approach, these dimensions are seldom translated into policy and management decisions within the district health system (p11)31.
In both the districts evaluated, integration across programs and of the prevention-care-rehabilitation axis of services was achieved through co-location at primary care level. Coupled with health system strengthening, this has the potential to improve access across the HIV/TB/STI cluster of services. The benefit is likely to be greater in rural areas. Quality of care was maintained in the long established TB programs in both settings.
Acknowledgments
The authors acknowledge the role of the Cape Town HIV/TB/STI task team who designed and implemented the evaluation tools. This team has an ad hoc membership and the following members have contributed significantly to the work: Juanita Arendse, Virginia Azevedo, Judy Caldwell, Karen Jennings, Pren Naidoo, Vera Scott, Brenda Smuts, Virginia Zweigenthal. Marian Loveday and Jenny McLoughlin facilitated the rural adaption. The authors commend the vision and commitment of the district managements, the sub-district TB HIV coordinators and mentors and the facility staff who collected data and analyzed them at facility and sub-district level as part of an internal quality improvement process. The authors thank Hilton Snyder for his meticulous work in cleaning and formatting data, and also Dr Brian van Wyk for his contribution in commenting on a draft of this manuscript.
References
1. South African Department of Health. National Antenatal Sentinel HIV and Syphilis Prevalence Survey in South Africa, 2009. Pretoria, South African Department of Health, 2010.
2. Day C, Gray A. Health and Related Indicators. In: A Padarath, S Fonn (Eds); South African Health Review 2010. Durban: Health System Trust, 2010.
3. Sanders D, Chopra M. Key challenges to achieving health for all in an inequitable society: the case of South Africa. American Journal of Public Health 2006; 96(1): 73-78.
4. South African Department of Health. HIV and AIDS and STI Strategic Plan for South Africa, 2007-2011. Pretoria, Department of Health, 2007.
5. Briggs CJ, Garner P. Strategies for integrating primary health services in middle- and low-income countries at the point of delivery. Cochrane Database of Systematic Reviews 2006; (2): CD003318.
6. Atun RA, Bennett S, Duran A. When do vertical (stand-alone) programmes have a place in health systems? Policy brief written for the WHO European Ministerial Conference on Health Systems, 25-27 June 2008. Denmark: WHO Regional Office for Europe, 2008.
7. World Health Organization. Integration of health care delivery. WHO Technical Report Series 1996; 861: 1-68.
8. Steyn K, Levitt N, Patel M, Fourie J, Gwebushe N, Lombard C et al. Hypertension and diabetes: poor care for patients at community health centres. South African Medical Journal 2008; 98: 618-622.
9. Tollman SM, Kahn K, Sartorius B, Collinson MA, Clark SJ, Garenne ML. South Africa: a population-based surveillance study. Lancet 2008; 372(9642): 893-901.
10. Uys LR, Naidoo JR. A Survey of the quality of nursing care in several health districts in South Africa. Biomedicine Central Nursing 2004; 3(1): 1-7.
11. Coovadia H, Jewkes R, Barron P, Sanders D, McIntyre D. The health and health system of South Africa: historical roots of current public health changes. Lancet 2009; Available: http://www.globalhealthscholar.yale.edu/sites/31581_Coovadia_2009_The-Lancet.pdf (Accessed 23 May 2013).
12. Mills A, Rasheed F, Tollman S. Strengthening health systems. In: DT Jamison, JG Breman, AR Measham, G Alleyne, M Claeson, DB Evans et al (Eds); Disease Control Priorities in Developing Countries, 2nd edition. New York, Oxford University Press, 2006; 1-6.
13. Chopra M, Lawn JE, Sanders D, Barron P, Abdool Karim SS, Bradshaw D et al. Achieving the health Millennium Development Goals for South Africa: challenges and priorities. Lancet 2009; 374: 1023-1031.
14. Nachega J, Coetzee J, Adendorff T, Msandiwa R, Gray GE, McIntyre JA et al. Tuberculosis active case finding in a mother-to-child HIV transmission prevention programme in Soweto, South Africa. AIDS 2003; 17: 1398-1400.
15. Lawn SD, Fraenzel A, Kranzer, K, Caldwell J, Bekker L-G, Wood R et al. Provider-initiated HIV testing increases access of patients with HIV-associated tuberculosis to antiretroviral treatment. South African Medical Journal 2011; 101: 258-262.
16. Legido-Quigley H, Montgomery CM, Khan P, Fakoya A, Getahun H, Grant AD et al. Integrating tuberculosis and HIV services in low- and middle income countries: a systematic review. In: First Global Symposium on Health Systems Research; 16-19 November 2010; Montreux, Switzerland. 2010.
17. Friedland G, Harries A, Coetzee D. Implementation issues in tuberculosis/HIV program collaboration and integration: 3 case studies. Journal of Infectious Disease 2007; 196: S114-123.
18. Van't Hoog AH, Onyango J, Agaya J, Akeche G, Odero G, Lodenyo W et al. Evaluation of TB and HIV services prior to introducing TB-HIV activities in two rural districts in western Kenya. International Journal of Tuberculosis and Lung Disease 2008; 12(3): 32-38.
19. Wang Y, Collins C, Vergis M, Gerein N, Macq J. HIV/AIDS and TB: contextual issues and policy choice in programme relationships. Tropical Medicine International Health 2007; 12(2): 183-194.
20. Bhutta Z, Ali S, Cousens S, Ali TM, Haider B, Azra R et al. Interventions to address maternal, newborn, and child survival: what difference can integrated primary health care strategies make? Lancet 2008; 372(9642): 972-989.
21. Scott VE, Chopra M, Azevedo V, Caldwell J, Naidoo P, Smuts B. Scaling up integration: development and results of a participatory assessment of HIV/TB services, South Africa. Health Research Policy and Systems 2010; 8: 23.
22. Loveday M, Scott V, McCoughlin J, Amien F, Zweigenthal V. Assessing care for patients with TB / HIV / STI infections in a rural district in KwaZulu-Natal South Africa. South African Medical Journal 2011; 101(12): 887-890.
23. Health Systems Trust. KwaZulu-Natal Province. In: District Health Barometer. Durban: Health System Trust, 2008; 159-172.
24. Health Systems Trust. Western Cape Province. In: District Health Barometer. Durban: Health System Trust, 2008; 256-271.
25. United Nations Children's Fund, and World Health Organisation: Local Monitoring and Evaluation of the Integrated Prevention of Mother to Child HIV Transmission in Low-income Countries. Geneva: UN, 2001.
26. World Health Organization. The World Health Report 2008 Primary Health Care - Now More Than Ever. World Health Organization, Geneva, 2008.
27. Granich RM, Gilks CF, Dye C, De Kock KM, Williams BG. Universal voluntary HIV testing with immediate antiretroviral therapy as a strategy for elimination of HIV transmission: a mathematical model. Lancet 2009; 373(9657): 48-57.
28. Walton DA, Farmer PE, Lambert W, Léandre F, Koenig SP, Mukherjee JS. Integrated HIV Prevention and Care Strengthens Primary Health Care: Lessons from Rural Haiti. Journal of Public Health Policy 2004; 25(2): 137-158.
29. World Health Organization. Declaration of Alma-Ata. International Conference on Primary Health Care; 6-12 September 1978; Alma-Ata, USSR. 1978.
30. Commission on Social Determinants of Health. Closing the gap in a generation: health equity through action on the social determinants of health. Final Report of the Commission on Social Determinants of Health. Geneva: World Health Organization, 2008.
31. Chopra M, Lawn JE, Sanders D, Barron P, Abdool Karim SS, Bradshaw D et al. Achieving the health Millennium Development Goals for South Africa: challenges and priorities. Lancet 2009; 374(9694): 1023-1031.
