The burden of chronic disease is felt globally. Cancer, cardiovascular disease (CVD), chronic respiratory disease, and type 2 diabetes are responsible for over 50% of worldwide mortality1. Their prevalence is increasing especially in developing countries. It is estimated that, in 2020, chronic diseases will be the cause of 50 million deaths globally2. The prevalence of diabetes alone is predicted to rise to 366 million people in 2030, of which 298 million will live in the developing world3.
Chronic diseases have broad negative impacts in developing countries, for example, in terms of the health of their populations and on their national economies and budgets. CVD, diabetes and stroke could lead to losses of $200-$550 billion in the gross domestic product of China, India, and Russia in the next 10 years4,5. In 2005, the WHO projected that 60 million people would have died of chronic diseases in India by the year 20155. Diabetes is the most frequent chronic disease in India, with a prevalence of 3.8% in adults living in rural areas and 11.8% in urban areas, and 57.2 million cases projected for 20256. Deaths from diabetes are expected to increase by 35% in 20155. Ignoring this increase will potentially stall India's current development, especially since 42% of the population will be over 35 years in 2021, and 43% of the population will be urban dwellers6. Contributing to the development of chronic diseases are sedentary lifestyles, poor nutrition and eating habits, and air pollution, among other risk factors. These are also greatly increasing, and obesity has become a global phenomenon. Even developing countries have been struggling with this problem7.
Information and communication technologies (ICTs) have transformed the mode of healthcare delivery into patient-centered care, from an approach previously centered in the provider. The patient-centered point-of-care approach goes beyond the traditional clinical settings, and allows healthcare services to be delivered in geographical areas where they are most necessary, such as isolated communities8. Educating patients through computer technology use has been recognized as an effective measure to develop patient skills and knowledge, which increases likelihood of engaging in healthy behavior. The necessity of offering higher-quality services at lower costs makes the use of computer technology essential to support health education9.
Health promotion, and chronic disease prevention and surveillance, can be achieved through ICTs, which acquire, disseminate and store health-related information electronically10. These technologies can be presented and accessed in different formats, such as web-based applications, mobile phone and alert systems, and telephone and video conferencing with patients11,12. The mHealth field, related to the use of mobile technology, is expanding in developing countries, with numerous new applications being constantly designed. Health education and promotion, remote monitoring and data collection, healthcare workforce training, surveillance and patient support are key applications for developing countries. Common challenges to implement communication technologies in these countries are the lack of infrastructure and political support, trained health personnel, and access to the internet13.
Due to the advantages of accessibility and a user-friendly interface, the portable health information kiosk (PHIK) can be a powerful tool for promoting health education in communities in both urban and remote settings. Kiosks are usually built as freestanding units, which facilitates their transportation and increases the possibility of providing access. They can be placed in healthcare settings or a public space14,15. Computerized kiosks possess a simplified interface and are used by individuals from various backgrounds regardless of socio-economic status or education14. Health information programs can be designed with high interactivity and usability levels, and deliver tailored health information according to the specific needs of the users in a community, once they are integrated into health kiosks.
These kiosks vary on many different levels such as interactivity and feedback14. Kiosks relieve the burden of providing preventive and continuous health education from the healthcare providers, who can then concentrate on the quality of their human care, especially in circumstances that require immediate attention. The ability to continuously tailor kiosk information based on input could be the inexpensive bridge to addressing a patient's need for adequate information that is customized to his ever-changing health status. No studies have been found that assessed chronic conditions in remote tribal populations in India through the use of health kiosks.
Prevention is still scarcely supported financially or politically through public health programs, even though the potential damage on population health and economies worldwide is evident. Providing health care for millions of individuals with chronic CVD, diabetes, and other chronic diseases is an expensive endeavor, and it affects the economies of families, and society as a whole. It has been estimated by the World Bank that controlling CVD would lead to improved life expectancy more effectively than trying to achieve WHO's Millennium Development Goals related to selected infectious diseases and maternal and child health16. Unfortunately, global chronic disease surveillance has not been a priority until recently. There is a need for global risk factor surveillance that could include various health professionals from different backgrounds and supported by different organizations17.
The objective of the study was to utilize the PHIK as a tool to assess the burden of chronic disease and associated risk factors in diverse settings such as urban, slum and tribal settings in India.
A convenience sample was enrolled from three diverse geographical locations, urban, slum and tribal, to explore the utilization of a PHIK for chronic disease health-risk assessment in a community setting. Cross-sectional data was recorded for 429 participants during the period of March to May 2010 in the cities of Rourkela and Bhubaneswar, state of Orissa, India. The tribal population was enrolled from the Rourkela settings, whereas urban and slum populations were enrolled from Bhubaneswar. The targeted population was adults aged over 18 years, and included both males and females. The subjects' participation in the study was voluntary. Subjects were provided with a one-page summary of what the study involved if they express their willingness to participate.
Participants were asked to use the touch screen of an electronic kiosk that gathered subjective and objective data to understand the distribution of chronic diseases and associated risks in the community setting. Data gathered on participants included subjective data that included responses to a series of multiple-choice questions, including location of residence (urban/slum/tribal), age (years), gender (male/female), highest level of education attained (less than high school/some college/graduate and above/none), smoking (presently/in the past/never) and alcohol history (presently/in the past/ never), height (feet, inches), ever been told by a doctor about high blood sugar (yes/no/I don't know), and if yes are you currently being treated for your high blood sugar (yes/no/I don't know), ever been told by a doctor about high blood pressure (yes/no/I don't know), and if yes are you currently being treated for your high blood pressure (yes/no/I don't know).
The objective data was gathered using multiple physiological sensors such as weight (kilograms), blood sugar and blood pressure. All the three sensors would capture individual weight, blood sugar and blood pressure readings and automatically transmit the readings to the touch screen of the PHIK. The information gathered was de-identified and did not include any follow up by the study personnel, nor were individuals asked for a follow up visit. Assistance was provided to those who needed help during the use of the PHIK. Each participant spent 35 min on average using the touch screen kiosk program.
Descriptive analysis was performed using univariate statistics. Results for the continuous variables were reported as means and standard deviations while results for the categorical variables were reported as frequency statistics as appropriate. Analysis of variance was performed to determine if there were any significant differences in the continuous variables across the different geographic settings including urban, slum and tribal. Similarly χ2 analysis was performed to determine if there were significant differences in the proportion of the categorical variables and the geographic settings in which participants were living. All analysis was performed using SAS v9.1 (www.SAS.com) and the results have been reported as p-values.
Ethics approval
The study was approved by the Asian Institute of Public Health Institutional Review Board.
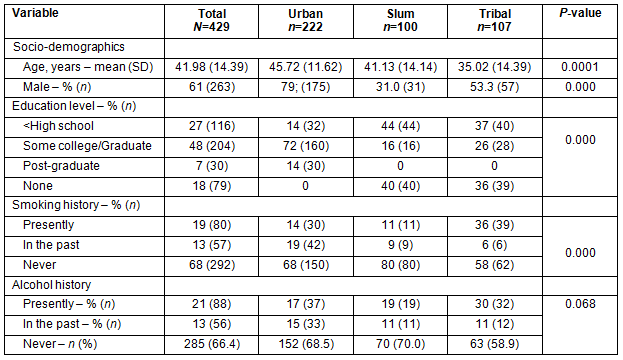
The study enrolled a convenience sample of 429 people aged 18 years and over across urban, slum and tribal settings of Bhubaneswar and Rourkela in the State of Orissa. Fifty-two percent (n=222) of the sample were from urban settings, 23% (n=100) were from slum settings and 25% (n=107) were from tribal settings. Those in the urban setting were older and the majority were female. Participants enrolled from the slum settings were predominantly female (Table 1).
Table 1: Main characteristics and history of the sample
There were significant differences in the weight of those living in urban settings compared with those in slum settings (p<0.001), with average weight and BMI 60 kg (SD=14) and 23 (SD=4.33), respectively. Similarly, those living in urban settings had significantly higher weights than those living in tribal and slum settings (p<0.001). However, no significant differences were seen between the weights of those living in the slum and those living in the tribal settings.
The average systolic and diastolic blood pressure of the overall population was 130/77 mmHg. Significant differences were seen in the systolic blood pressure of those living in the urban settings as compared with those living in either slum (p=0.04) or tribal settings (p=0.02). No significant differences were seen in the systolic and diastolic blood pressures for participants living in the tribal or slum settings (p=0.98). Participants in the urban settings had significantly higher diastolic blood pressure compared with those living in the slum settings (p<0.001). No significant difference was seen in the diastolic blood pressure of those living in the urban as compared with the tribal settings (p=0.51). However, participants in the tribal settings had significantly higher diastolic blood pressure as compared with those living in the slum settings (p=0.001). Significant differences in the blood sugar levels were seen only among those living in the tribal as compared with the urban settings (p=0.04).
No significant differences were seen for the blood sugar levels of those living in urban versus slum (p=0.9) or slum versus tribal (p=0.11) settings. Similarly, there was no significant difference in the BMI of participants living in slum versus tribal settings (p=0.09). However, participants living in the urban settings had a significantly higher BMI than those living in slum (p<0.001) or tribal settings (p<0.001) (Fig1).
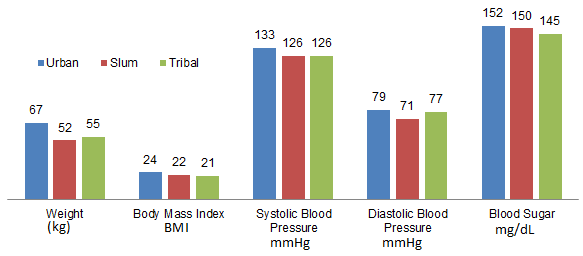
Figure 1: Comparison of variables according to setting.
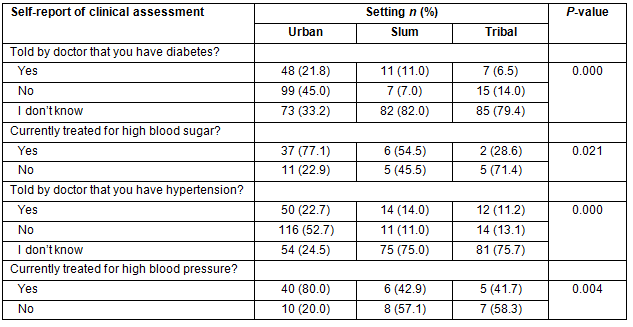
In the self-report clinical assessment, more than half of the participants didn't know if they had diabetes or not (56%; n=240). Similarly approximately 49% (n=210) of participants didn't know if they had hypertension or high blood pressure. Overall, the prevalence of diabetes was 16% (n=66) and that of hypertension was approximately 18% (n=76). Of those who had diabetes, 32% (n=21) of them were not treated for high blood sugar. Similarly, of those who had high blood pressure, 33% (n=25) of them were not treated for it. Significant differences were seen in the burden of diabetes, blood sugar and their current treatment among those those living in urban, slum and tribal settings. The burden of diabetes and hypertension was significantly high in the urban setting than in the slum and tribal settings (Table 2).
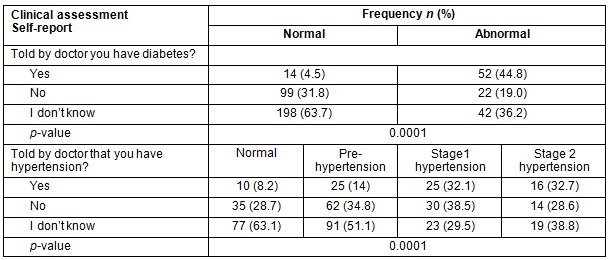
Table 2: Self-reported clinical assessment
Participants in the urban setting were significantly overweight (32%, n=70) compared with those in the slum (10%, n=10) and tribal settings (12%, n=13) (p=0.0001). Seventy-one percent (n=305) of participants had either pre-hypertension (42%, n=178), stage 1 hypertension (18%, n=78) or stage 2 hypertension (11%, n=49), and 27% (n=116) had abnormal blood sugar levels. A high prevalence of pre-hypertension, and stages 1 and 2 hypertension were found among those living in the slum and tribal settings (Table 3).
Concordance analysis (Table 4) was performed to determine the level of agreement among the participants who self-reported having diabetes and hypertension and had abnormal readings using objective assessments using medical sensors through PHIKs. Of those who did not know if they had diabetes, 36% (n=42) were found to have abnormal blood sugar levels. Similarly, among those who did not know if they had high blood pressure, more than half were found to have pre-hypertension, 29.5% were in stage 1 hypertension and 38.8% in stage 2 hypertension.
Table 3: Chronic disease assessment
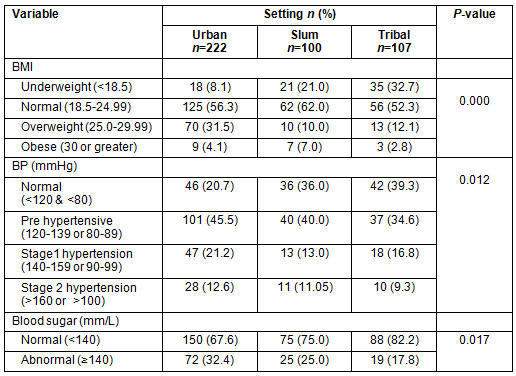
Table 4: Concordance analysis
Further analysis was performed to assess if those who had self-reported having diabetes had received any kind of treatment, and on the status of their blood sugar levels (Fig2). Results have shown that almost half of the people in slum areas (n=5) who had self-reported diabetes were left untreated, and 40% (n=2) of them had abnormal blood sugar readings. The reality is even more worrisome for inhabitants of tribal areas, where 71% (n=5) of positively self-reported diabetics were untreated, with 80% (n=4) of them actually presenting with abnormal levels of sugar in the blood. In urban areas, 77% (n=37) of the people who answered 'yes' to the diabetes self-report were treated, and the number who had abnormal readings was 81% (n=30). In the case of those who self-reported hypertension (Fig3) in the slum setting, 57% (n=8) went untreated and 62.5% (n=5) had abnormal blood pressure readings. Similarly, in the tribal setting 58% of the respondents hadn't been treated. Of those, 86% had abnormal blood pressure readings. Finally, in the urban areas, 20% of self-reported hypertensive participants were untreated, with 90% of this group having abnormal blood pressure readings.
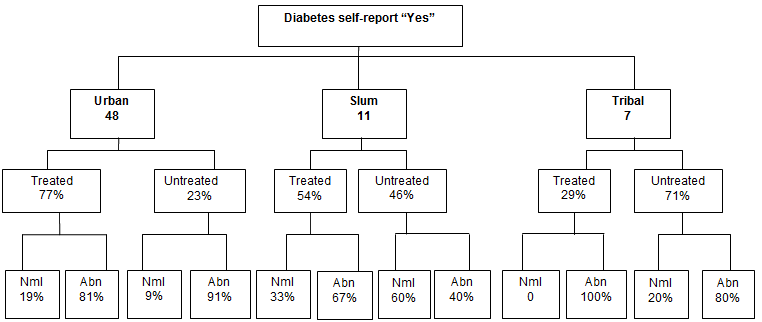
Figure 2: Frequency of 'yes' answer to having been told by the doctor that they have diabetes, according to setting and outcome. Nml, Normal; Abn, abnormal.
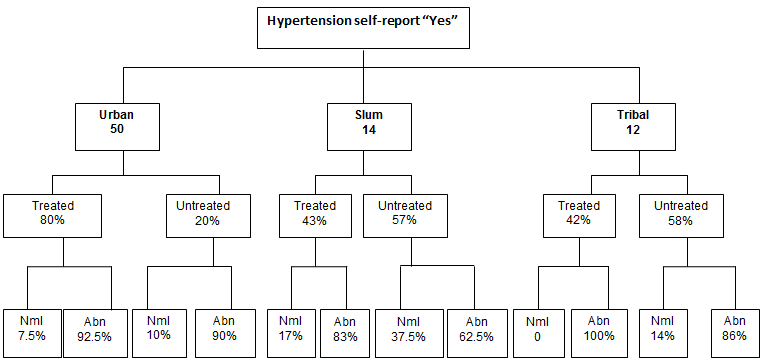
Figure 3: Frequency of 'yes' answer to having been told by the doctor that they have hypertension, according to setting and outcome. Nml, Normal; Abn, abnormal.
Discussion
The results of the study showed significant differences in systolic blood pressure between those living in the urban and slum or tribal settings. Those in urban settings also had significantly higher diastolic blood pressure than those living in the slum settings. For all participants, 56% didn't know if they had diabetes, and 49% didn't know if they had hypertension or high blood pressure. The overall burden of diabetes was 16% compared with 18% for hypertension.
Almost half of the people in slum areas who had self-reported diabetes were left untreated, and 40% of them had abnormal blood sugar readings. In tribal areas, 71% of positively self-reported diabetics were untreated and 80% of them had abnormal blood sugar levels. In the slum setting, 57% of self-reported hypertension was untreated, and 62.5% of respondents had abnormal blood pressure readings. Similarly, 58% of respondents in the tribal setting hadn't been treated, with 86% having abnormal blood pressure readings.
The study results have shown that the burden of chronic diseases in tribal and slum communities needs further investigation. Of the Indian tribal population, 25% doesn't have access to health services18. The state of Orissa, India, where Rourkela is located, has a population of over 40 million people19. According to the 2001 census, 85% lived in rural regions and 22% were tribal populations. According to the subjective assessments, 79.4% of people in tribal communities reported that they didn't know if the doctor had told them if they have diabetes, and 75.7% of tribal populations reported the same for hypertension. Therefore, the assessment of health conditions in these populations is insufficient. The results of the concordance analysis using PHIKs to measure abnormal levels of blood sugar and blood pressure demonstrated that 36.2% of people who didn't know about their diabetes status had abnormal blood sugar readings, and 51.1% of those who didn't know about their hypertension status had pre-hypertension, and 38.8% presented with stage 2 hypertension. One of the limitations was the use of self-report assessments on the various disease conditions reported. The objective measurements of blood pressure, blood sugar and weight at the point of care through the use of physiological sensors contributed towards an accurate health assessment. However, accurate information about the family history, prior diagnosis of various disease conditions, and information about smoking and alcohol consumption could not be validated because of self-reporting.
Poor infrastructure and lack of qualified personnel are challenges to providing a meaningful service, as low wages, poor living and working conditions are obstacles that prevent the trained staff from establishing themselves in these areas of extreme need20. Patient self-management support, group visits, automated registries, and primary care integrated with specialist support are important strategies to improve quality of care21. The interaction between patient and healthcare provider can be enhanced by various community resources, but little effort is currently made to implement multifaceted approaches, despite studies that establish their effectiveness22,23. Governments and institutions must act more decisively in addressing social determinants and health issues based on the past success of multifaceted health promotion strategies. Such strategies present the potential to address the global health problems that will predominate in the 21st century24,25. For governments and institutions to enact policies that can improve health outcomes in disadvantaged areas, they first need the data and the evidence to support it. It has been demonstrated that multifaceted interventions generate larger and more positive effects than single interventions.
Computerized kiosk systems could be the key to improving public health among diverse populations in varied settings around the world. ICTs can be utilized as a platform to assess risk, deliver multifaceted interventions tailored to the needs of the specific users after taking into account their health literacy levels. Future work should be explored to evaluate the impact of health kiosks in improving short- and long-term health outcomes in these diverse settings.
Health kiosks can be the multifaceted solution to overcome difficult obstacles when working in remote and resource-poor settings where there is poor infrastructure and a lack of qualified trained personnel. The use of health kiosks to communicate interactive health education modules created in a user-friendly interface can help to inform the populations in diverse settings about the risk factors of chronic diseases and the methods of prevention, monitoring and its management. Health kiosks can also be useful in determining a true epidemiological burden of disease conditions in remote and rural areas. Health kiosks can help to generate evidence-based, meaningful information to support key decisions for national and regional programs and policies throughout the developing world.
References
1. Yach D, Leeder SR, Bell J, Kistnasamy B. Global chronic diseases. Science 2005; 307(5708): 317. (Online) 2005. Available: http://www.sciencemag.org (Accessed 12 April 2012).
2. Murray CJ, Lopez AD. The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries and risk factors in 1990 and projected to 2020. Cambridge, MA: Harvard School of Public Health, 1996.
3. Wild S, Roglic G, Green A, Sicree R, King H. Global prevalence of diabetes: estimates for 2000 and projections for 2030. Diabetes Care 2004; 27(5): 1047-1053. Available: http://care.diabetesjournals.org (Accessed 12 April 2012).
4. Anderson GF, Chu E. Expanding priorities - confronting chronic disease in countries with low income. New England Journal of Medicine 2007; 356(3): 209-211.
5. World Health Organization. Preventing chronic diseases: a vital investment. Geneva, Switzerland: WHO, 2005.
6. Srinath Reddy K, Shah B, Varghese C, Ramadoss A. Responding to the threat of chronic diseases in India. Lancet 2005; 366(9498): 1744-1749.
7. Popkin BM, Doak CM. The obesity epidemic is a worldwide phenomenon. Nutrition Reviews 1998; 56(4 Pt 1): 106-114.
8. Humphreys JS, Wakerman J, Wells R, Kuipers P, Jones JA, Entwistle P. "Beyond workforce": a systemic solution for health service provision in small rural and remote communities. Medical Journal of Australia 2008; 188(8Suppl): S77-80.
9. Lewis D. Computer-based approaches to patient education: a review of the literature. Journal of the American Medical Informatics Association 1999; 6(4): 272-282.
10. Stroetmann KA, Robinson LKS, Stroetmann KC, McDaid D. How can telehealth help in the provision of integrated care? WHO Policy Brief 2010/13. Copenhagen, Denmark: WHO, 2010.
11. Lee RG, Chen KC, Hsiao CC, Tseng CL. A mobile care system with alert mechanism. IEEE Transactions on Information Technology in Biomedicine 2007; 11(5): 507-517.
12. Boulos MN, Wheeler S, Tavares C, Jones R. How smartphones are changing the face of mobile and participatory healthcare: an overview, with example from eCAALYX. Biomedical Engineering Online 10: 24. (Online) 2011. Available: http://www.biomedical-engineering-online.com (Accessed 12 April 2012).
13. Bukachi F, Pakenham-Walsh N. Information technology for health in developing countries. Chest 2007; 132(5): 1624-1630.
14. Kreuter MW, Black WJ, Friend L, Booker AC, Klump P, Bobra S et al. Use of computer kiosks for breast cancer education in five community settings. Health Education and Behavior 2006; 33(5): 625-642.
15. Pendleton BF, Labuda Schrop S, Ritter C, Kinion ES, McCord G, Cray JJ et al. Underserved patients' choice of kiosk-based preventive health information. Family Medicine 2010; 42(7): 488-495.
16. World Bank. Millennium development goals for health in Europe and central Asia. relevance and policy implications. Washington, DC: World Bank, 2004.
17. Choi BCK, Bonita R, McQueen DV. The need for global risk factor surveillance. Journal of Epidemiology and Community Health 2001; 55: 370.
18. Bala SM, Thiruselvakumar D. Overcoming problems in the practice of public health among tribals of India. Indian Journal of Community Medicine 2009; 34(4): 283-287.
19. Directorate of Census Operations, Orissa. Census of India 2011: provisional population totals - Orissa. Bhubaneswar, India: Ministry of Home Affairs, 2011. Available: http://censusindia.gov.in/2011-prov-results/prov_data_products_orissa.html (Accessed 12 April 2012).
20. Wagner EH, Austin BT, Davis C, Hindmarsh M, Schaefer J, Bonomi A. Improving chronic illness care: translating evidence into action. Health Affairs (Millwood) 2001; 20(6): 64-78.
21. Lehmann U, Dieleman M, Martineau T. Staffing remote rural areas in middle- and low-income countries: a literature review of attraction and retention. BMC Health Services Research 2008; 8: 19.
22. Piatt GA, Orchard TJ, Emerson S, Simmons D, Songer TJ, Brooks MM et al. Translating the chronic care model into the community: results from a randomized controlled trial of a multifaceted diabetes care intervention. Diabetes Care 2006; 29(4): 811-817.
23. Wagner EH, Groves T. Care for chronic diseases: the efficacy of coordinated and patient centred care is established, but now is the time to test its effectiveness. BMJ 2002; 325(7370): 913-914.
24. Jackson SF, Perkins F, Khandor E, Cordwell L, Hamann S, Buasai S. Integrated health promotion strategies: a contribution to tackling current and future health challenges. Health Promotion International 2006; 21(Suppl 1): 75-83.
25. Ziglio E, Hagard S, Griffiths J. Health promotion development in Europe: achievements and challenges. Health Promotion International 2000; 15: 143-153.
Published 28 March 2013; modified 16 January 2014.
A correction was made to the name of the approving IRB in the Methods section.
