Context
Studies in the early to mid-1990s identified that approximately one-third of people aged 65 years and over, living in the community, report one or more falls in the previous 12 months1-3. In residential aged care and in hospital settings, the annual falls rate in this age group can be as high as 50%4,5. The number and severity of falls injuries also increases with advancing age and with the increased incidence of osteoporosis6. A person aged 85 years or older is 40-fold more likely to die or to be seriously injured in a fall than is a person in the 65-69 year age group7.
The costs of falls in terms of individual suffering8 and to the community are high, and these costs will increase markedly as the population ages9. There is therefore some urgency in implementing effective falls prevention strategies.
Research10 stresses that among strategies, approaches to falls prevention for healthy and for frail older people will differ, as will approaches within community, residential aged care and hospital settings. Multifaceted interventions are also preferable to single interventions in all settings.
The Project
This report presents the development and implementation of a falls and falls injury prevention strategy in a South Australian country region. A multifaceted intervention program covered all three settings (community, residential aged care and hospital) with initial outcomes available from the analysis of a 2-year falls reports database.
Development and implementation
The 3-year project was funded by the Limestone Coast Division of General Practice, South Australia, in collaboration with the regional Community Health Service. A project manager and a project officer met regularly with a stakeholder committee of an occupational therapist, physiotherapist, community health service manager, hospital nurse-manager, and the director of the day care centre of a residential care facility. No consumer representative was included due to the lack of a suitable candidate. The agreed action plan attempted both primary and secondary prevention of falls and falls injury in a multifaceted intervention program.
In the community: The action plan promoted the following elements:
- Public awareness of falls and falls injury through talks to target groups, media coverage, and by the development of falls information resources and a website.
- 25 Talks on falls and falls injury with individual take-home reinforcement material.
- Approximately 1300 people attended the talks.
- A total of 10 newspaper articles and 5 short radio sessions covered various aspects of the action plan and the results in progress.
- A divisional website was regularly updated.
- A falls hand-out package (including falls prevention strategies, safe footwear, getting up after a fall, the benefits of home assessment and modification, and local contact information), developed by physiotherapists, was available at accident and emergency departments of hospitals, community health centres and medical clinics.
- Lifestyle improvement with advice on diet, exercise and activity, smoking and alcohol. Tai Chi Quan classes were of most interest (attendance at a four-times-weekly class increased from 5 to 50 people during the project).
- A falls and balance clinic within the existing budget of the base hospital using the physiotherapy department's personnel.
- A physiotherapist completed a subjective and objective assessment of intrinsic risk factors for falls for each client.
- An 8-week individualised exercise and balance program.
- Follow-through was in a 'mature movers group' or a chair-based exercise group.
- The use of the Sahara ultrasound heel sonometer for assessment of 'risk of fracture'11.
- Home assessments for environmental falls hazards by occupational therapists.
- Supply of walking aids and hip protectors.
- Improved management of secondary prevention of falls and falls injury.
Bone densitometry Many country regions in Australia do not have ready access to bone densitometry (DEXA). However, large prospective studies have confirmed the fracture-predictive power of quantitative ultrasound (QUS) calcaneal measurements, particularly for hip fracture 12-14. QUS has many practical advantages in a rural area: portability, low cost, no radiation exposure, simplicity of operation and minimal space requirements. QUS can be considered a pre-screen for DEXA 15 to make the best use of the latter's availability. Wherever the measurement is used, however, it must be part of a full assessment of that patient's risk of falling and of fracture. Some 450 measurements were made in clinics and residential care accommodation, using staff trained by the project manager. Since the completion of the project, trained pharmacy staff have also become access points for measurement.
Issues associated with home assessment Enough money was donated by regional service and other clubs to provide for a subsidy of up to A$50 for any agreed home modifications following the assessment. It is difficult to get elderly people at home to accept the benefits of a home assessment of any sort, or to accept that aspects of their home and garden that may have been unchanged for years now present a falls hazards. Once access is gained, all home assessments should be comprehensive and contain an element of falls hazards assessment. The assessment should be performed by either a physiotherapist or an occupational therapist on the basis of a 'first-in, one-stop' assessment. (For too long, physiotherapists have been involved solely with the intrinsic risk factors of falling and occupational therapists with the extrinsic risk factors). During the study, 406 assessments were carried out with an average of $36 spent on modifications.
Secondary prevention of falls and falls injury The project highlighted secondary prevention of falls and falls injury as being poorly managed, with poor referral rates to allied health personnel or the usual general practitioner (GP) after a fall/fracture. Since the project, all persons over 65 years admitted to the base hospital after a fall/fracture are seen by the continuity of care registered nurse. On discharge, the patient has an appointment with his/her usual GP within a fortnight, and leaves with a completed checklist, combining the risk factors for falls and for osteoporosis, together with a lateral X-ray of thoracic spine for evidence of vertebral collapse, if necessary. This prior work-up allows the GP to move quickly into full assessment and management.
In residential care accommodation: The action plan promoted:
- 'Falls prevention' as a written policy
- The inclusion of a 'falls risk assessment' in the admission process and inpatient reviews (some residential care units already included this in their admission procedure; during the project this practice spread to all units).
- Multidisciplinary assessment of 'high-risk fallers' (the medical component of such an assessment was often missing).
- The promotion of use of calcium and vitamin D supplements among residents.
- Regular exercise for aged residents.
- The use of hip protectors among those residents at risk.
- Regular review of medication.
The use of calcium and vitamin D supplements Heavy promotion of this combination to lower the risk of fragility fracture in the frail elderly indoors16 resulted in a rise in those in residential care accommodation prescribed these supplements. In September 2001, 10% of the target population (those not bed-bound) of 319 people in residential care accommodation were taking daily calcium and vitamin D. However, 7 months later, those taking calcium had risen to 27% and those taking vitamin D to 23% (of a target population of 349 people). Cheap, acceptable liquid solutions of vitamin D in high dosage are available and should be promoted.
Hip protectors Staff in residential care accommodation were quick to appreciate the value of these garments and there was a significant increase in their use. Compliance was a problem17. The plastic shields were, in one instance, carefully taken out each night on retiring and placed beside the teeth on the bedside locker. The shields were once used behind a brassier, and once used as a 'saucer' for the morning tea! A significant problem, too, in many of the present models was the time taken to pull down the garment for toileting the wearer. Some models have a flap for this purpose. A crotchless model was designed by regional staff for particular use with those residents who suffer from incontinence or those who required frequent toileting.
In hospitals: The action plan mirrored that developed for residential care accommodation except in the promotion of calcium and vitamin D supplements and exercise.
Falls report: A falls report was designed for nursing staff's use in medical clinics, accident and emergency departments, hospital wards, hostels and nursing homes, and for ambulance officers as points of first contact after a fall.
The faller's name was not recorded. Tick-boxes indicated the patient data: age; sex; first language; postcode; point of first contact; description, time and location of fall; any injury; outcome (admission); and follow-up referral. After 6 months the following data were added: presence of dementia; ownership and wearing of hip protectors at the time of falling, and any resultant injury.
Completed forms were transmitted to the project officer within 24 hours.
Implementation of the action plans and falls reports: All regional participants were visited in a first 'grand round' to explain the action plan and to gain cooperation with falls reporting. The action plan and reporting commenced on 1 April 2000 (promoted as April Falls Day!).
The GP's role was highlighted in a distributed discussion document, together with a checklist of risk factors for falls and for osteoporosis, and was reinforced during grand rounds.
Workforce training included a one-day regional seminar on falls and falls injury. Training sessions on the use of the Sahara sonometer were undertaken. An endocrinologist updated the diagnosis, management and prevention of osteoporosis and reinforced the use of the Sahara sonometer in a rural setting.
The falls reports data were analysed monthly and 6-monthly (Table 1). Six-monthly grand rounds of all participants allowed for the presentation of the regional and individual statistics, with time for discussion on progress and problems with the action plan as it applied to the participant. A more comprehensive evaluation was carried out in the final grand round in May 2002.
Table 1: Falls, fractures and hospital admissions at 6-month intervals
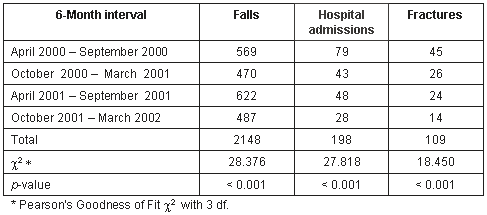
Results and Discussion: Issues
Falls
A total of 2148 falls were reported over the 2 years of the study in the region's population of 7553 people aged 65 years and over. Seventy more falls were reported in the second year. The regional monthly totals varied between 55 and 123 while any individual health unit's reported monthly totals varied between 0 and 34.
Fallers
The majority of fallers (55%) were in their 80s. The male : female ratio changed significantly from 3.4:1.0 in the 66-70 years age group, to 1.0:3.9 in the 91+ years age group. Mental confusion associated with the fall was noted in 4% of community, 39% of hostel, 67% of nursing home and 55% of hospital falls.
There was a seasonal variation, with more falls occurring each year (100 and 138) in the colder months (April to September). The majority of falls occurred in residential care accommodation (hostel 44%, nursing home 27%) with 18% in hospital, and 11% in the community. Six periods were identified in residential care units where a sudden rise in the number of reported falls was due to the frequent falls of one or two residents. The most common cause of a fall in the community was tripping (29%), whereas in residential and hospital care the most common cause was loss of balance (41% and 29%). Night falls (8 pm-8 am) accounted for 19% of community falls, 39% of residential care falls, and 42% of hospital falls.
Falls injuries
Of all falls over the 2-year period, 56% resulted in no injury, 39% in soft tissue injury, and 5% in a fracture. The fracture rate fell from 7% in the first 12 months to 4% in the second 12 months (p < 0.001) and the rate of hospital admissions in those who fell, dropped from 12% to 7% (p < 0.001) (Figs 1,2). Yearly hip fracture rates for the 2 years remained constant (25 and 27, respectively).
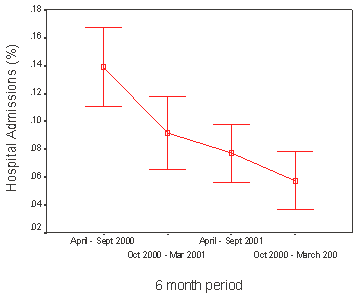
Figure 1: Percentage hospital admissions according to study intervals of 6 months.
The most common fractures were hip (n = 52) and wrist (n = 13) fractures. Eleven other fracture sites were recorded. Fractures were reported in 8% of community falls, 3.6% of hostel falls, 2% of nursing home and 1.25% of hospital falls.
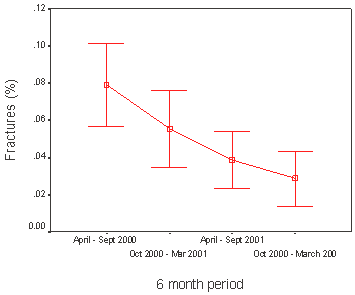
Figure 2: Percentage fractures according to study intervals of 6 months.
In hostels, the percentage of residents who were wearing hip protectors at the time of the fall rose from 15% to 29% over 18 months. One hip fracture occurred in 174 of such falls. In nursing homes, the percentage of residents who were wearing hip protectors at the time of the fall rose from 5% to 21% over the same period, with one hip fracture in 94 falls. In contrast, 24 fractures (of which 16 were hip fractures) occurred in 851 falls where the resident was not wearing a hip protector at the time of the fall, over the same period within the same facilities. Of those who wore a hip protector, 2% were admitted to hospital compared with 10.4% of those not wearing one (Fisher's Exact Test, p < 0.001). Wearing a hip protector was thus highly protective against fracture and hospital admission. Since the study was completed, one hostel has 75% of its 50 residents in hip protectors, and one nursing home has 90% of its 13 ambulant residents in hip protectors.
Follow up
Of 170 falls in the community, 16% were referred to the GP, 5% to a physiotherapist, and 7.5% to an occupational therapist. In residential care accommodation, of 1174 falls, the equivalent referral rates were 13%, 3% and 0.75%, respectively. In acute care, of 338 falls, the equivalent rates were all 5%.
Lessons
The project was associated with a significant (42%) decrease in hospital admissions after a fall and a significant (41%) decrease in total fracture rates during the 2 years of reporting (Figs 1,2). There was also a decrease in yearly hip fracture rates when compared with previous years. The yearly average for the region's hip fractures during the 5 financial years 1994-1999 was 40 (data from Mount Gambier Hospital records, South Australia). Over the 2 years of reporting, the average number of hip fractures was 26, a 35% reduction. In the year since the project ended, there were 30 hip fractures, still significantly below the pre-project average.
These percentage reductions can be compared with that of the Mission Statement of Osteoporosis Australia 2001 which expresses an aim 'to reduce the incidence of osteoporotic factures in the Australian community by 20%, by the year 2010'.
The following factors necessary to achieve such a result emerged from the project:
- A close collaboration between a body representing the regional GPs and the regional health service.
- An administrative officer who has good organisational, 'people' and computer skills, to run the program.
- A small committee of 8-10 stakeholders who meet regularly and represent the region's GPs, community health service, aged care accommodation, hospitals and community.
- A 'champion' - a person preferably with a medical or allied health professional background, credible within the community, with good people skills, committed to the project, who has time to devote to falls prevention.
- Champions within each health and accommodation unit, committed to the action plan and responsible for the accurate completion of falls reports. These staff members' continuing commitment and interest is crucial for the long-term success of the plan.
Limitations
This project's reporting strategy, comprehensiveness and mechanisms had limitations, the most obvious being where there was a faller in the community who had no contact with any service after a fall. Another limitation was that apart from hospital admission and injury, no other consequences of the fall were sought. Importantly, too, there was no 3-6 months of reporting before the interventions commenced.
The reporting was intended primarily as a feed-back and a motivational tool. It was recognised that it would be difficult to hold together a system of conscientious reporting of every fall in the region for longer than 2 years. Reporting in itself could be regarded as an intervention.
Achievements
The strategy has been successful in embedding falls and falls injury prevention in the workforce culture of those in daily contact with the elderly. It has been less successful in raising falls and falls injury prevention to a higher priority status with the region's GPs. Falls prevention, and the diagnosis and management of a 'silent' condition like osteoporosis, have to compete for the doctor's time with many other, perhaps more demanding, conditions in the elderly. However, the doctor's commitment is crucial in the longer term, in the assessment and management of risk factors, including medication taken, particularly after the first fall or fracture; in the prescription of calcium and vitamin D, particularly in residential care accommodation, and in the heavy promotion of hip protectors.
The value of hip protectors as a cheap, safe, effective and immediate protection against serious injury was confirmed. The cost of a hip fracture is approximately $15 00018; the cost of all models of hip protector is less than $150.
Most importantly, a decrease in regional falls injuries, if not overall falls numbers, was associated with the implementation of the multifaceted intervention program.
Conclusion
The decrease in regional falls injuries, if not overall falls numbers, was associated with the implementation of a multifaceted intervention program in a collaboration between the region's Division of GP, community health services, hospitals and residential care accommodation. The value of hip protectors as a cheap, safe, effective, and immediate protection against serious injury was confirmed. It is recommended that the cost of these garments is government subsidised - the South Australian State Government has already implemented this recommendation. There is scope for further study of the seasonal variation of more falls occurring in each year of the project in the colder months of April to September.
Acknowledgement
The project and its intermediate results received the Australian Injury Prevention Network's Award for 2001 for the best paper presentation at the Fifth National Conference on Injury Prevention and Control, held in Warrnambool in September, 2001.
References
1. Dolinis J, Harrison J, Andrews G. Factors associated with falling in older Adelaide residents. Australian and New Zealand Journal of Public Health 1997; 21: 462-468.
2. Kendig H, Helme R, Teshuva K, Osborne D, Flicker L, Browning C. Health status of older people project: preliminary findings from a survey of the health and lifestyles of older Australians. Melbourne: Victorian Health Promotion Foundation, 1996.
3. Lord S, Wrad J, Williams P, Anstey K. An epidemiological study of falls in older community-dwelling women: The Randwick falls and fractures study. Australian Journal of Public Health 1993; 17: 240-245.
4. Tinetti M, Williams C. Falls, injuries due to falls, and the risk of admission to a nursing home. New England Journal of Medicine 1997; 337: 1279-1284.
5. Forster A, Young J, Langhorne P. Systematic review of day hospital care for elderly people. BMJ 1999; 318: 837-841.
6. Access Economics. The burden of brittle bones: costing osteoporosis in Australia, a report for Osteoporosis Australia. Canberra, ACT: Access Economics, 2001; 8.
7. Commonwealth Department of Health and Aged Care. National Falls Prevention in Older People Initiative. Canberra, ACT: AGPS, 2000; 2-3.
8. International Osteoporosis Foundation. International Osteoporosis Foundation Annual Report, 2000 Geneva: Switzerland: International Osteoporosis Foundation, 2000; 6.
9. Moller J. New directions in health and safety: changing resource demands related to falls injury in an aging population. Report prepared for the NSW Injury Policy Unit. Sydney, NSW: Government Printer, 2000; 2-7.
10. National Ageing Research Institute. An Analysis of research on preventing falls and falls injury in older people: community, residential aged care and acute care settings. Report to the Commonwealth Department of Health and Aged Care Injury Prevention Section. Canberra, ACT: AGPS, 2000; xv.
11. Ho Y, Fan D, Hans J et al. Assessment of a new quantitative ultrasound calcaneus measurement. Osteoporosis International 2000; 11: 354-360.
12. Hans D, Dargent-Molina P, Schott AM et al. Ultrasonographic heel measurements to predict hip fracture in elderly women: the EPIDOS prospective study. Lancet 1996; 348: 511-514.
13. Stewart A, Torgerson DJ, Reid DM. Prediction of fractures in perimenopausal women: a comparison of dual X-ray absorptiometry and broadband ultrasound attenuation. Annals of Rheumatic Disease 1996; 55: 140-142.
14. Bauer DC, Gluer CC, Cauley JA et al. Broadband ultrasound attenuation predicts fractures strongly and independently of densitometry in older women. Archives of Internal Medicine 1997; 157: 629-634.
15. Langton CM, Ballard PA, Langton DK, Purdie DW. Maximising the cost-effectiveness of BMD referral for DEXA using ultrasound as a selective population pre-screen. Technical Health Care 1997; 5: 235-241.
16. Chapuy M, Arlot M, Duboeuf D et al. Vitamin D3 and calcium to prevent hip fractures in elderly women. New England Journal of Medicine 1992; 327: 1637-1642.
17. Villar MTA, Hill P, Inskip H, Thompson P, Cooper C. Will elderly rest home residents wear hip protectors? Age and Ageing 1998; 27: 195-198.
18. Cameron ID, Lyle DM, Quine S. Cost-effectiveness of accelerated rehabilitation after proximal femoral fracture. Journal of Clinical Epidemiology 1994; 47: 1307-1313.
