Introduction
In 2008 in India 63 000 women died from pregnancy and child birth related causes, contributing to 18% of the global burden of maternal deaths1. Studies show that the risk of maternal death is high during labour, delivery and up to 24 hours postpartum2-4. Thus policies and programs to reduce maternal morbidity and mortality have mainly focused on strategies to cover this crucial period. A mapping of policies and programs in India over more than six decades (Fig1) illustrates the government's efforts, since 1946, to improve delivery care and reduce maternal deaths5.
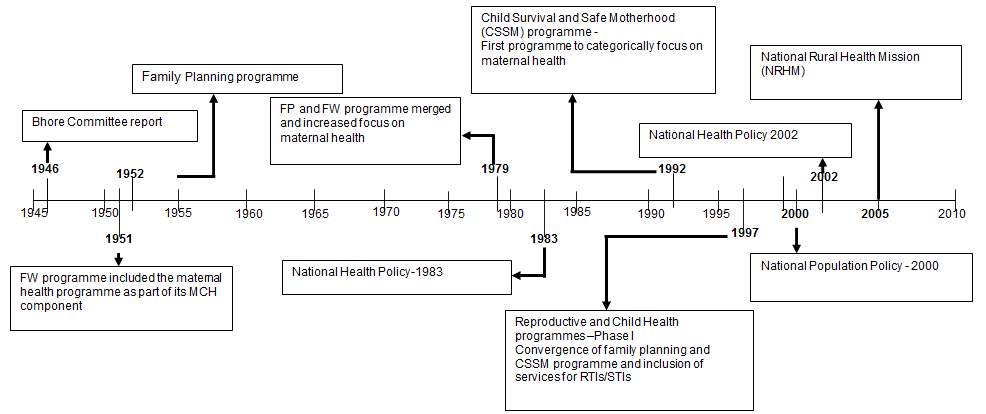
Figure 1: Policies and programs for reducing maternal mortality and morbidity in India from 1945 to 2010. FW, Family welfare;
MCH, Maternal and Child Health; FP, Family planning; RTIs, Reproductive tract infections; STIs, Sexually transmitted infections. (Data sources5,6).
With the introduction of the National Health Policy in 2000, several programs, such as the Reproductive and Child Health Programme, phases I and II7, and the National Rural Health Mission8 endeavoured to increase deliveries by skilled birth attendants (SBA) in health institutions. Since 2000 these strategies have had some impact on the maternal mortality ratio. The Maternal mortality ratio has reduced from 540/100,000 live births in 1998-1999 to 230/100,000 live births in 20081; however, eight women still die every hour in India due to causes related to pregnancy and child birth9. This suggests a need to examine the factors that affect the success of strategies aimed to promote skilled institutional delivery.
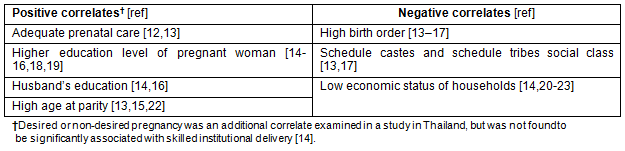
There is increased evidence from developed countries that for the strategies of institutional delivery to be effective, it is essential to understand the factors that influence individual and household decisions to utilise SBA and institutions for delivery10,11. A review of the published literature suggests that these factors can be divided into those that motivate women to undergo institutional delivery and those that act as barriers (Table 1). The objective of this study was to assess the prevalence of skilled institutional delivery and the factors that influenced decisions to utilise these services among a sample of rural, economically deprived women in the state of Andhra Pradesh (AP), India.
Table 1: Determinants of skilled institutional delivery12-23
Methods
Participants and study variables
Data was used from round one of the 'Young Lives' study in AP, India. Young Lives is an international longitudinal cohort study of childhood poverty which follows 12 000 children in four countries (Ethiopia, Peru, Vietnam and India)24. Each country has two cohorts, one consisting of 2000 children born in 2001-2002 and another consisting of 1000 children born in 1994-1995 to be followed over a 15 year period24.
The primary sampling methodology consisted of a multi-stage semi-purposive method, details of which are provided elsewhere25. Briefly, 19 mandals (administrative blocks) were selected as sentinel sites from six districts; two in each of the three regions of AP (Coastal, Rayalaseema and Telangana) based on their economic, infrastructure and human development indices25. The six selected districts comprised of three poor and three non-poor districts according to their relative level of development25. Of the 19 mandals, 15 were rural and four were urban defined based on the Census of India definition25. Each of the 15 rural mandals consisted of 20-23 villages which were divided into four groups based on their geographical distribution, and one village was randomly selected from each group to select the sample of rural households25. A list of households in each village was prepared based on two eligibility criteria: households with a one year-old child (born in 2001-2002) or an eight year-old child (born in 1994-1995)25. Using the same household eligibility criteria a separate list was prepared for the four urban mandals in six districts and for Hyderabad city25. Within each sentinel site, approximately 150 households (100 for the younger cohort and 50 for the older cohort) were randomly selected from the list of eligible households (total 3019 households in 20 sentinel sites) and were approached for participation in the study24,25. A total of 14 households refused to participate, leading to a participation rate of 99.5%25. Replacement sampling was performed to cover the 14 refusals24,25. Surveys are conducted every 3 years to collect data on a range of indicators related to the growth and development of the children in these households.
For this study, data from the 2001-2002 cohort were used, which consisted of 2011 households in six districts of AP. Of these, 505 urban households were excluded due to the study's focus on rural areas (which have higher maternal mortality ratio1). Of the 1506 rural households, 87 were excluded because either information on place of delivery and/or birth attendant was missing. The final sample consisted of 1419 mothers (referred to as 'pregnant women' in this article). The pregnant women excluded in the 87 households were not statistically significantly different from the rest of the study sample in terms of their baseline characteristics (not shown but provided on request).
Because the maternal health programs in India and AP primarily aim at increasing institutional delivery by SBA, the outcome of interest was institutional delivery conducted by SBA (definitions in Fig2). Most published studies focus either on institutional delivery or on skilled delivery as outcome12,14-16 except a study conducted in Mexico that used skilled institutional delivery26. This dichotomous outcome variable 'skilled institutional delivery' was derived from the two variables place of birth and birth attendant.

Figure 2: Definitions of institutional delivery and skilled birth attendant18,23,27
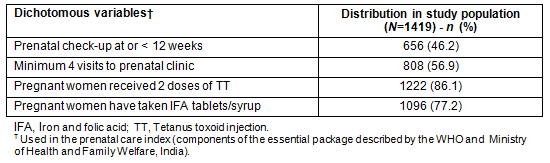
Variables were constructed for the positive and negative factors identified from literature (Table 1) using the Young Lives data. Adequacy of prenatal care is measured using different methods by several epidemiologists19. A prenatal care index to denote the adequacy of prenatal care of pregnant women was generated based on the guidelines of an essential package for prenatal care by the World Health Organisation (WHO)28 and Ministry of Health and Family Welfare, India29. Because it is not known that which components of the essential package are most important, a score of one was assigned to each of the four components of the essential package (Table 2) if the pregnant women received them. The index created had a range of scores from 0 to 4, where a score of '4' alone was considered as 'adequate prenatal care' to be consistent with the WHO and the national guidelines. Information on at least one of these four variables was missing for 240 pregnant women, who therefore were grouped as 'missing'. A limitation of this index is that it does not include other essential components of the prenatal package, such as whether the pregnant women were checked for their weight gain, blood pressure, haemoglobin level, and albumin and sugar in their urine. This information was not available from the Young Lives dataset used in this study. However, it is presumed that pregnant women receiving more than four prenatal check-ups would have received these services.
Table 2: Variables for the prenatal care index
Age at parity was defined as the age of the mother when she was pregnant with the index child (child enrolled in the Young Lives study24). This was then categorised into less than 20 years, 20-35 years, and more than 35 years to group the women into younger, average and older age groups, respectively, in relation to the childbearing age in India30. Birth order was calculated based on the number of children born alive prior to the index child and was categorised as first born, second born, third born and ≥4 live births.This did not include stillbirths and abortions. The survey questionnaire for the first round of the study included a question on whether the mothers desired to be pregnant and have the child. Data from this question were used to generate a dichotomous variable of desired pregnancy. The number of years of education of the mother was categorised as follows: no education, 1-8 years of education and more than or equal to 9 years, to correspond with no formal education, primary education and secondary education in India31. However, data on the husband's education was only available as a dichotomous variable categorised into two groups: no education and completed primary education.
Data on social class were used to categorise study participants into those belonging to under-privileged groups: (i) schedule tribe or schedule caste group (the Planning Commission of India classifies a number of socially disadvantaged tribal communities as schedule tribe and a number of non-tribal but equally disadvantaged groups as schedule caste); and (ii) non-schedule tribe/schedule caste group. Further, a wealth index was used to categorise households into different levels of poverty, as was done in other Young Lives studies24,25 (least poor households had a wealth index of ≥0.4; very poor 0.2 to <0.4; and poorest <0.2).
Data analysis
The characteristics of the sample population were defined and the prevalence of skilled institutional delivery was estimated for each independent variable. Odds ratios (OR) were calculated to estimate the probability of skilled institutional delivery through univariable and multivariable analyses. Multivariable analysis was conducted using a binary exploratory logistic regression model. Considering that there were only eight independent variables, all were simultaneously included in the model. In addition, the variable 'difficult labour' was added to the model. Women who experience difficult labour are more likely to go to hospitals for delivery irrespective of the influence of any individual or household factors. All statistical associations were considered to be significant at a p <0.05. All statistical analyses were performed using STATA version 10.1 (www.stata.com).
Ethics approval
Round one of Young Lives obtained ethics approval from the London School of Hygiene Ethics Committee and informed consent was obtained from all participants before administering the survey questionnaire.
Results
The sample population consisted of approximately 39% women belonging to the schedule caste or schedule tribe social class (Table 3). Most pregnant women in the study sample belonged to economically deprived households with a mean wealth index of 0.26 (±0.16). They were relatively young, with a mean age of 22 years (±4.36). Just over one-third of the women in the study sample had no prior live birth (37%) and a similar number had only one previous live birth (38%).
The prevalence of institutional delivery by SBA was 36.8%. The majority of the pregnant women did not receive adequate prenatal care during their pregnancy (Table 3). More than 91% of the pregnant women desired to have the child. Most pregnant women were uneducated (70%), but their husbands were relatively better educated with at least 44% having primary education (Table 3).
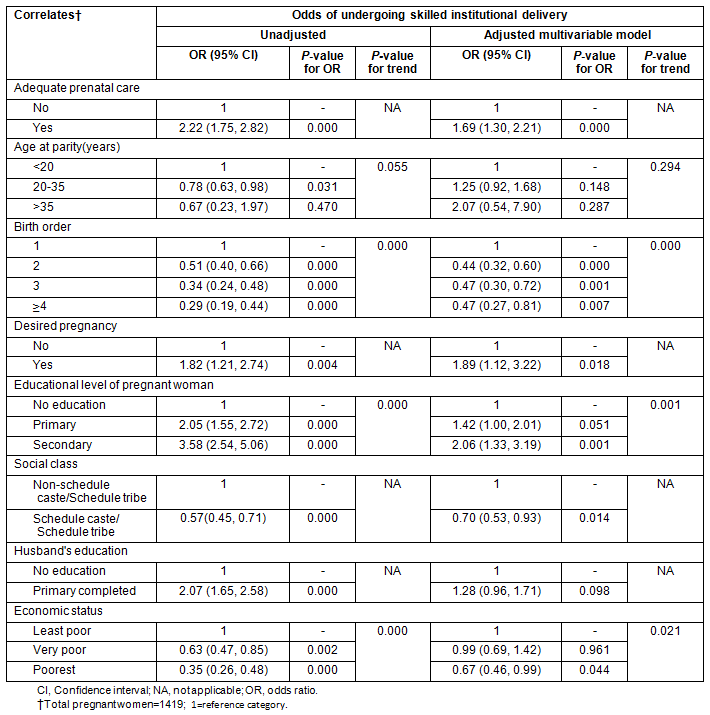
Women with prenatal care, desired pregnancy, or higher education were more likely to undergo skilled institutional delivery, but high birth order, schedule caste/schedule tribe background and low economic status were found to be the negative determinants (Table 4).
The odds of undergoing skilled institutional delivery decreased after the first birth but did not decrease further with increase in parity (Table 4). The likelihood of utilising these services decreased linearly with decrease in the economic status of the households, but the OR was statistically significant only for the poorest category of households after controlling for all other variables. Skilled institutional delivery was not found to be significantly different between the categories of husband's education and mother's age at parity in this study population (Table 4).
Table 3: Characteristics of the study population24
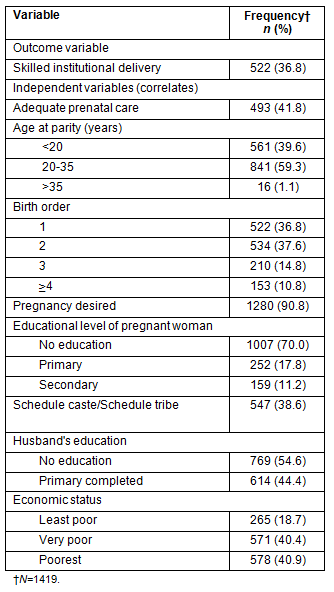
Table 4: Results of logistic regression models24
Discussion
The prevalence of institutional delivery by SBA in the study sample was 36.8%. An examination of the determinants of skilled institutional delivery showed that those pregnant women who had primary and secondary levels of education, desired to be pregnant and had received adequate prenatal care were most likely to utilise these services. The probability of utilising skilled institutional delivery decreased after the first child and was lower for women who belonged to a schedule caste or schedule tribe. However, age at parity and education of their husbands had no significant effect on skilled institutional delivery. Pregnant women from the poorest households were least likely to undergo skilled institutional delivery.
Andhra Pradesh, with a maternal mortality ratio of 154 per 100 000 live births (2004-2006)32, implemented the Phase-I of Reproductive and Child Health Programme in 1997 with two innovative strategies, (i) 'Women Health Centres' to conduct deliveries round the clock, 7 days a week; and (ii) a cash-incentive scheme known as Sukhibhawa to provide monetary assistance to economically deprived pregnant women living in rural areas to seek institutional delivery services33. Sukhibhawa is often referred to as a successor of the 'National Maternity Benefit Scheme' (1995)5 and predecessor of Janani Suraksha Yojana (2005)27, which are cash-incentive schemes. The implementation of these strategies in rural AP were deemed partially successful due to a proportional increase in the utilisation of institutional delivery (from 40% to 51.6%) between two District Level Household Surveys (DLHS 1998-1999 and 2002-2004)17,22, in contrast to which a much lower utilisation was found during the study period 2001-2002. The reasons could be that District Level Household Surveys focused only on institutional delivery, but this study examined institutional delivery conducted by SBA. While it is presumed by policy-makers that deliveries in health institutions will be conducted by SBA, it may not always be the case. Indeed, according to the study findings, about 5% of the pregnant women who went to a health institution for delivery did not receive the services of a skilled attendant. Compared with the rural households, the Young Lives round-1 report for AP showed that 83% of the women in urban households (n=505, excluded from the sample for this study) delivered their child in a hospital and 90% of the deliveries were conducted by a SBA34. Despite existence of favourable policies and programs directed towards improving utilisation of skilled institutional delivery among economically deprived pregnant women in rural areas, the prevalence of skilled institutional delivery in the rural population was almost 46% lower than that of their urban counterparts.
Educated women, particularly women with secondary education were more likely to utilise SBA and health institutions for delivery. This finding is consistent with studies conducted in Thailand14, Peru16, Bangladesh21, and rural Mexico26. In addition to education, a woman whose pregnancy is 'desired' is more likely to use these services presumably because she is more concerned about her pregnancy and the child's welfare than those whose pregnancy was not 'desired'. This is different from the findings of Raghupathy which showed no association between institutional delivery and 'desired' pregnancy14. This study confirms the positive correlation found in other studies between adequate prenatal care and utilisation of skilled institutional delivery12,21,26. A majority of women in the study were economically deprived and uneducated, but among them, pregnant women who had adequate prenatal care were almost twice as likely to undergo skilled institutional delivery compared with those without such care. It is likely that counselling on place of birth and provision of information during prenatal check-ups influenced the women's decision. However, it is also possible that women seeking prenatal care had underlying characteristics influencing their use of institutional delivery independent of information provided at pre-natal visits.
Contrary to other studies which show a linear decrease in the utilisation of institutions and SBA with increased birth order12,14-16,26,35 this study found that a substantial decrease occurred after the first child and did not change with further increases in the order of birth. Women in this study were relatively economically deprived and perhaps could not afford to undergo skilled institutional delivery after their first child or perhaps, after the first child, they were less likely to find the need for institutional deliveries.
The results of this study showed that women belonging to schedule caste/schedule tribe group were significantly less likely to have skilled institutional delivery even after controlling for all other determinants. The reasons for this could be high levels of poverty, lack of access to health institutions and lack of education and awareness about delivery in health institutions among these people. However, a study which used the 1992-1993 National Family Health Survey data did not find any difference in the utilisation of institutional delivery and SBA between the schedule caste/schedule tribe and other social groups in the state of AP, although they found a lower utilisation of antenatal care services among the schedule caste/schedule tribe group35. This could be due to the difference in the construction of the outcome variable in this study as discussed earlier (institutional delivery by SBA compared with only institutional delivery in National Family Health Survey).
Yet another interesting finding relates to the relationship between the economic status of the households and decisions to use institutions and SBA for delivery. Although the study population as a whole was relatively economically deprived, the utilisation of skilled institutional delivery was significantly lower among those who were the poorest. Most studies have shown a linear decrease with decrease in the wealth quintiles12,14,20,21,26.
Studies in India and other low-middle income countries15,16 show that older women are more likely to deliver in institutions, but age had no impact on the decision to undergo skilled institutional delivery in this study. This is consistent with the study findings of Raghupathy14 and Barber26. Again, husband's education was not important for women's childbirth decision. This was also shown in the study in Peru16; however, two other studies conducted in Thailand and Vietnam, respectively, showed a positive association14,15. One possible explanation is that, in India, men are mostly responsible for earning and providing for their family, while decisions on health and utilisation of health services are usually made by women.
The mothers in this study gave birth in the year 2000. Since then, Sukhibhawa, the conditional cash transfer scheme relevant to the period of this study, was replaced by Janani Suraksha Yojana in 2005, which is by far the largest cash incentive scheme in the world in terms of the number of beneficiaries27,36. Government of India spent more than US$300 million in the scheme in the financial year 2009-201036. Nevertheless, a recent study that analysed the impact of Janani Suraksha Yojana inferred that 'the poorest and the least educated women did not have the highest odds of receiving the incentive'36. The conditional cash transfer schemes have evolved, but this does not seem to have influenced the less educated and economically deprived women in rural areas to undergo skilled institutional delivery.
Limitations
A limitation of this study is its inability to analyse the quality or physical accessibility of these services due to non-availability of data. It is acknowledged that this may limit the findings of this study by excluding important determinants found in several studies11,37. Furthermore, data on prenatal care was missing for 17% of the study sample, a majority of whom did not undergo skilled institutional delivery. This may positively or negatively affect the association of prenatal care with skilled institutional delivery depending on whether these women had adequate care or not. This study is based on economically deprived pregnant women living in rural areas, so the findings cannot be generalised to the entire state of AP or the country. Nevertheless, this study helps elucidate the factors that influence women's decision to utilise skilled institutional delivery.
Conclusion
The present study showed that a number of factors could prevent women from undergoing skilled institutional delivery in rural areas. Based on the findings, it is suggested that a more holistic approach through integrated maternal health, family planning and education programs will help maximise delivery in health institutions. There is a need for policies and programs to focus on uneducated women in the poorest quintile from disadvantaged social groups. Further, there is an urgent need for research in countries with high burden of maternal morbidity and mortality to understand the individual and household factors that impact on decisions to undergo skilled institutional delivery for efficient and effective targeting of existing interventions, and to formulate more comprehensive maternal health programs.
Acknowledgements
The authors are grateful to the Young Lives team for making this data available, and to all the field and research staff involved in data collection and the management of the study. This article was written from the MSc thesis of the first author, successfully submitted towards completion of MSc Global Health Science which was funded by the Public Health Foundation of India (PHFI), New Delhi, India.
References
1. World Health Organisation. Trends in Maternal Mortality: 1990 to 2008. Estimates developed by WHO, UNICEF, UNFPA and The World Bank. Geneva: World Health Organisation, 2010.
2. Khan KS, Wojdyla D, Say L, Gülmezoglu AM, Van Look PFA. WHO analysis of causes of maternal death: a systematic review. The Lancet 2006; 367(9516): 1066-1074.
3. World Health Organization. Progress: in reproductive health research. Progress 2005; 71: 5-7.
4. Ronsmans C, Graham WJ. Maternal mortality: who, when, where, and why. The Lancet 2006; 368(9542): 1189-1200.
5. Planning Commission Government of India. Evolution of the family welfare programme. New Delhi: Planning Commission Government of India, no date. Available: http://planningcommission.nic.in/aboutus/committee/strgrp/stgp_fmlywel/sgfw_ch3.pdf (Accessed 31 October 2012).
6. Measham AR, Heaver RA. India's family welfare program: moving to a reproductive and child health approach. Washington, DC: World Bank, 1996; 73.
7. Department of Family Welfare Ministry GoI. Reproductive & Child Health Program. Secondary Reproductive & Child Health Program. New Delhi: Department of Family Welfare Ministry, 2012. Available: http://www.mohfw.nic.in/NRHM/RCH/Index.htm (Accessed 31 October 2012).
8. Ministry of Health & Family Welfare GoI, New Delhi. National Rural Health Mission Secondary National Rural Health Mission. New Delhi: Department of Family Welfare Ministry, no date. Available: http: //mohfw.nic.in/NRHM.htm .
9. World Health Organisation. Trends in Maternal Mortality: 1990 to 2008 Estimates developed by WHO, UNICEF, UNFPA and The World Bank. Geneva: World Health Organisation, 2010.
10. Brouwere VD, Tonglet R, Lerberghe WV. Strategies for reducing maternal mortality in developing countries: what can we learn from the history of the industrialized West? Tropical Medicine & International Health 1998; 3(10): 771-782.
11. Griffiths P, Stephenson R. Understanding user's perspectives of barriers to maternal health care use in Maharashtra, India. Journal of Biosocial Science 2001; 33(3): 339-359
12. Bloom S, Lippeveld T, Wypij D. Does antenatal care make a difference to safe delivery? A study in urban Uttar Pradesh, India. Health Policy and Planning 1999; 14(1): 38.
13. International Institute for Population Sciences (IIPS) and Macro International. National Family Health Survey (NFHS - 3), 2005-06: India: Volume I. Mumbai: IIPS, 2007.
14. Raghupathy S. Education and the use of maternal health care in Thailand. Social Science & Medicine 1996; 43(4): 459-471.
15. Toan NV. Utilisation of reproductive health services in rural Vietnam: are there equal opportunities to plan and protect pregnancies? Journal of Epidemiology and Community Health 1996; 50(4): 451-455.
16. Elo IT. Utilization of maternal health-care services in Peru: the role of women's education. Health transition review : the cultural, social, and behavioural determinants of health 1992; 2(1): 49-69.
17. International Institute for Population Sciences; Population Research Centre; Ministry of Health and Family Welfare. District level household survey (DLHS-2): reproductive and child health, Andhra Pradesh 2002-04. Mumbai: IIPS, 2002-2004.
18. World Health Organization. Skilled birth attendants, factsheet. Geneva: World Health Organisation, 2008.
19. Kirby R. The quality of vital perinatal statistics data, with special reference to prenatal care. Paediatric and perinatal epidemiology 1997; 11(1): 122-128.
20. Hadi A, Gani MS, Dhaka B. Socio-economic and regional disparity in the utilization of reproductive health services in Bangladesh. Working paper. Dhaka, Bangladesh: BRAC, 2005.
21. Anwar I, Sami M, Chowdhury ME, Salma U, Rahman M et al. Inequity in maternal health-care services: evidence from home-based skilled-birth-attendant programs in Bangladesh. Bulletin of the World Health Organization 2008; 86(4): 252-259.
22. International Institute for Population Sciences (IIPS) and ORC Macro. National Family Health Survey (NFHS - 2), 1998-99: India. Mumbai: IIPS, 2000.
23. World Health Organization. Reduction of maternal mortality: A Joint WHO/UNFPA/UNICEF World Bank Statement. (Online) 1999. http: //www.who.int/reproductive-health/publications/reduction_of_maternal_mortality/e_rmm.pdf (Accessed 24 May 2009).
24. Barnett I, Ariana P, Petrou S, Penny ME, Duc LT, Galab S et al. Cohort Profile: The Young Lives Study. International Journal of Epidemiology 2012; Epub ahead of print: doi:10.1093/ije/dys082.
25. Kumar N. An assessment of the Young Lives sampling approach in Andhra Pradesh, India. Young Lives technical note. Oxford, UK: Young Lives, 2008.
26. Barber S. Does the quality of prenatal care matter in promoting skilled institutional delivery? A study in rural Mexico. Maternal and Child Health Journal 2006; 10(5): 419-425.
27. Ministry of Health & Family Welfare GoI. Janani Suraksha Yojana: features & frequently asked questions and answers. Secondary Janani Suraksha Yojana: features & frequently asked questions and answers. (Online) 2006. Available: http://www.mohfw.nic.in/NRHM/RCH/guidelines/JSY_guidelines_09_06.pdf (Accessed 31 October 2012).
28. World Health Organisation. The world health report 2005 - make every mother and child count. (Online) 2005. Available: http: //www.who.int/whr/2005/en/ (Accessed 11 May 2009).
29. Maternal Health Division, Ministry of Health and Family Welfare, India. Guidelines for ante-natal care and skilled attendance at birth by ANMs and LHVs. Delhi: Ministry of Health & Family Welfare Government of India, 2005; 3-45.
30. International Institute for Population Sciences (IIPS). National Family Health Survey (MCH and Family Planning), India 1992-93. Bombay: IIPS, 1995.
31. Dreze J, Kingdon GG. School participation in rural India. London: The Suntory and Toyota International Centres for Economics and Related Disciplines London School of Economics, 1999.
32. Office of the Registrar General India. Special bulletin on maternal mortality in India 2004-06: Sample Registration System, 2004-06. Delhi: Office of the Registrar General India, 2009.
33. Government of Andhara Pradesh. Family Welfare Program - Improvement of Institutional deliveries scheme to assist pregnant women of below poverty line in the state to seek institutional delivery services - G.O.Rt.No.1173 Dated.9.07.1999. Secondary Family Welfare Program - Improvement of Institutional deliveries scheme to assist pregnant women of below poverty line in the state to seek institutional delivery services - G.O.Rt.No.1173 Dated.9.07.1999. (Online) 1999. Available: http: //www.aponline.gov.in/Quick%20Links/Departments/Health,%20Medical%20and%20Family%20Welfare/Govt-Gos-Acts/1999/GO.Rt.1173.1999.html.
34. Galab S, Reddy MG, Antony P, McCoy A, Ravi C, Raju DS, et al. Young Lives preliminary country report: Andhra Pradesh, India: Young Lives, 2003.
35. Navaneetham K, Dharmalingam A. Utilization of maternal health care services in Southern India. Social Science & Medicine 2002; 55(10): 1849-1869.
36. Lim S, Dandona L, Hoisington J, James S, Hogan M, Gakidou E. India's Janani Suraksha Yojana, a conditional cash transfer program to increase births in health facilities: an impact evaluation. The Lancet 2010; 375(9730): 2009-2023.
37. Sejfeskog L, Sundby J, Chimango J. Factors influencing women's choice of place of delivery in rural Malawi--an explorative study. African Journal of Reproductive Health 2006; 10(3): 66-75.


