Over the past 30 years, China has experienced unprecedented economic growth, resulting in substantial increases in household income and a reduction in the proportion of households living below the poverty level. The benefits of growth, however, have not fully translated into equitable social development. The inequity in healthcare services between urban and rural areas has increased, generating widespread public dissatisfaction1,2. To address this issue, the national health system reform plan was launched by the Chinese central government in early 2009, incorporating new guidelines to address the core issues of equity and accessibility affecting the reasonable distribution of healthcare resources3,4. To this end, much attention was given to specialist outreach, defined as planned, regular visits by specialists from their usual practice locations (usually high-level hospitals in urban areas) to patients in primary care or rural hospital settings3-5.
Worldwide, specialist outreach, also referred to as visiting-specialist services, is employed to increase patient access to medical specialists. Australia's government-funded Specialist Outreach Service (SOS) has been in operation since the mid-1990s6-9. Similar outreach programs in England, Spain, and Canada have been providing this expanded healthcare service to residents in rural areas for years10-14. In the USA, similar programs called 'community-based programmes' have been introduced15,16. This type of program could bring surgical services even to rural areas in developing countries such as Ethiopia, Zimbabwe, and Ecuador17-19. As demonstrated in previous studies, the benefits of such programs for patients include reduced elective referral rates, easy access to specialists, higher satisfaction and convenience, and reduced waiting time8,12. Specialist outreach can have a positive influence on the professional skills of primary care physicians11,20.
The large-scale practice of specialist outreach in China, distinguished by the deep involvement of health authorities, is extensive but sustainable. Historically, specialist outreach can be traced back to the foundation of the People's Republic of China. It has evolved with China's social and economic development, and culminated in the long-term outreach project titled 'Thousands of outreach specialists to the rural areas', initiated by the Chinese Ministry of Health in the mid-2000s. Since the late 1990s, new incentives for physicians have been introduced into specialist outreach programs. Participation can significantly influence career progression for doctors, as doctors in urban hospitals are required by the Chinese Ministry of Health to practise in rural areas for at least 6 months before they are eligible for promotion to senior professional (a rank equivalent to associate professor)3-5. However, the benefits were less than expected due to a conflict of interest with the hospitals.
Recently, an increasing number of specialist programs have been initiated within medical consortiums (vertically integrated organisations administered by a single governing unit to serve a defined area). On average, these consortiums comprise one tertiary hospital, several secondary hospitals and primary care clinics, and public general hospitals21,22. Patients requiring sophisticated surgery available in only tertiary hospitals benefit greatly from this system, which provides referrals from outreach specialists to the tertiary hospitals. Costs for treating severe diseases could also be reduced as a result of the strengthened collaboration between outreach specialists and local doctors, herein referred to as the 'green referral channel', through which patients can enjoy reservation of medical services like hospitalisation to cut down the length of stay.
In many countries, the costs of specialist outreach programs have been investigated, particularly health service costs for patients (treatment and overhead costs), personal costs for patients (eg travelling and opportunity costs), and management costs for outreach teams (staff, consultant travel, and associated opportunity costs). A national evaluation of specialist clinics in primary care settings in England showed that while patients' personal costs were lower in outreach programs than in outpatient clinics, health service costs in the outreach programs were higher per patient12. In another study, specialist outreach in dermatology was found to have significantly lower health service costs (treatment and overhead costs) but higher marginal costs (management costs for additional patients)13.
Against this background, the present study examines the impact of referrals from outreach specialists on hospitalisation costs in rural patients requiring advanced surgery at a tertiary hospital to treat digestive tract cancer.
District
A retrospective study of hospitalisation costs and length of stay was carried out on data collected from patients receiving surgical treatment for digestive tract cancer within the Taiyuan Central Hospital Consortium. Digestive tract cancers (oesophagus, gastric, colon, and rectum cancers) have high incidence and high mortality rates in China23; their treatment commonly requires surgery in a tertiary, rather than secondary, hospital with certified surgeons and the necessary surgical equipment.
The capital of Shanxi province in central China, Taiyuan city contains three million residents in the urban district and 1.2 million in its four affiliated counties: Gujiao, Loufan, Yangqu, and Qingxu (Fig1). In 2007, a medical consortium was formed consisting of Taiyuan Central Hospital, a tertiary hospital, along with three secondary hospitals: Gujiao People's Hospital, Loufan People's Hospital, and Yangqu People's Hospital. Outreach specialists from Taiyuan Central Hospital travel to these three secondary hospitals to serve local residents, especially in cases of rare and refractory disease. Patients requiring further diagnostic evaluation or sophisticated surgery were referred to tertiary hospitals (ie through the aforementioned green referral channel).
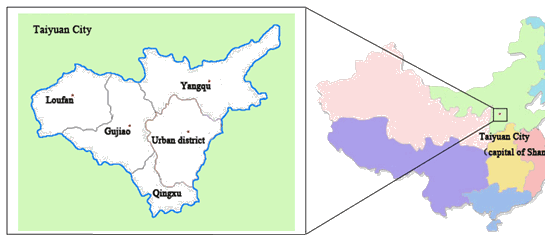
Figure 1: Taiyuan city, capital of Shanxi province, located in central China. Study areas indicated by red dots.
Sample
Patients from Gujiao, Loufan, and Yangqu counties admitted for surgical treatment of digestive tract cancer within the general surgery department of Taiyuan Central Hospital were sampled from January 2008 to December 2010. Patients directly admitted without referral were designated as the control group. Patients referred from secondary hospitals within the consortium were grouped into referral by outreach specialists (RO) and referral by local doctors at secondary hospitals (RL), respectively.
Patients were considered eligible for participation if their medical records contained International Classification of Diseases-9 (ICD-9) diagnosis codes for digestive tract cancers: oesophagus, gastric, colon, and rectum cancer (150.xx, 151.xx, 153.xx, 154.xx, 159.xx). Patients with mid-stage cancer as defined by Medstat's Disease Staging algorithm24 (the spread of neoplasm within the affected organ system or extensive display of carcinoma symptoms but no metastasis to other organ systems) were also included in the study. A Charlson Comorbidity Index (CCI) score was compiled for each patient25.
Data
Data on patients' demographic characteristics (gender, age, health plan, referral type) and clinical characteristics, including cancer stage, comorbidities, and length of hospitalisation, were collected from Taiyuan Central Hospital's medical database. Total costs of hospitalisation, drugs, surgery, diagnostic testing, and room and board-related costs, were also calculated. For referred patients, the cost of diagnostic testing performed by the secondary hospitals (gathered from their records) was included in the calculations of total cost.
All charges for medical services were checked to ensure compliance with the standard charges set by the Shanxi Province Health Bureau and published in the Shanxi Province Medical Price List.
Statistical analyses
Chi-squared and two-tailed t-tests were performed for categorical and continuous variables, respectively. Regression-adjusted costs were estimated using a multivariate model that controlled for gender, age, type of cancer, CCI, and referral type. All patients were covered under the New Rural Cooperative Scheme health plan.
An ordinary least squares model with a natural logarithmic transformation of the dependent variable (five designated costs) was found to be the most appropriate according to total explained variance of the costs. The logged predicted values were then transformed into actual costs via exponentiation and application of a smearing estimate26. Retransformed and predicted costs were then compared using an analysis of variance (ANOVA) utilising the Student-Newman-Keuls test for post-hoc analyses.
Ethics approval
Data were collected with the permission of the medical consortium and its component organisations. The Ethics Committee of Taiyuan Central Hospital approved this study; ethics approval number XHEC-2011(co)-21.
The distribution of patients according to cancer type is shown in Figure 2. Demographic and clinical characteristics are presented in Table 1.
The length of stay (LOS) values for both the RO (19.2 ± 3.7 days) and RL (24.2 ± 5.9 days) groups were significantly lower than that of the control group (28.3 ± 4.9 days) (p<0.01, RO vs control; p<0.01, RL vs control); the LOS of RO was lower than that of RL (p<0.01; Fig3).
The regression-adjusted costs are included in Table 2. After adding referral type as a factor in the comparison of cost, significant differences were found between the three groups (Table 3) for total hospitalisation costs and drug costs. Both of these costs were the highest for the control group, followed by the RL and then the RO groups. There was at most a weak significant difference found between the three groups (Table 3) for surgery costs. Significant differences in diagnostic testing costs were found between the groups, with the highest costs seen in RL followed by the control group; the lowest costs were seen in RO (Table 2). Regarding room and board-related hospitalisation costs, the average costs of RL and RO were significantly lower than that of the control group but there was no significant difference between RL and RO (Table 3).
Table 1: Demographic and clinical characteristics by group
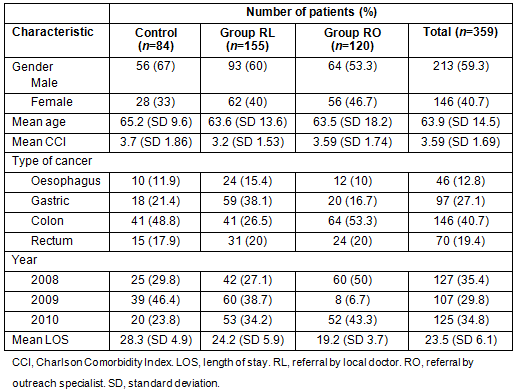
Table 2: Regression-adjusted mean hospitalisation costs? between groups
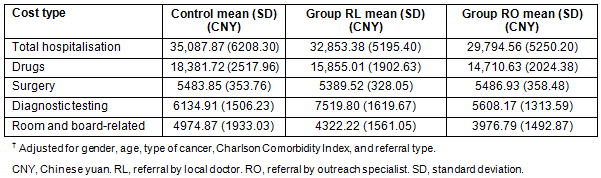
Table 3: p-values of comparisons between groups
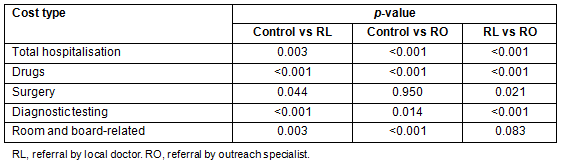
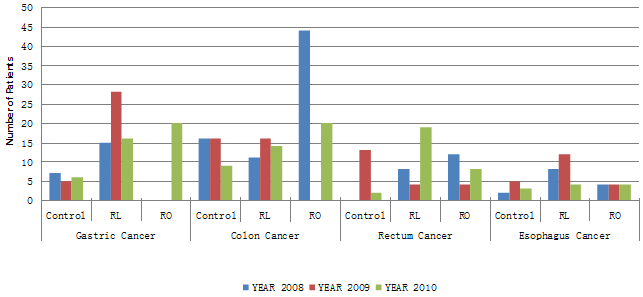
Figure 2: Distribution of patients by cancer type, 2008-2010.
RL, referral by local doctor. RO, referral by outreach specialist.
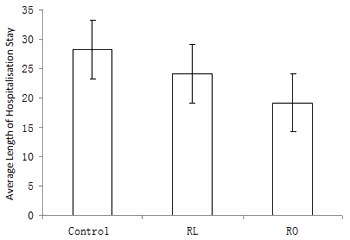
Figure 3: Mean length of hospitalisation (and standard deviation), by group.
RL, referral by local doctor. RO, referral by outreach specialist.
Specialist outreach mainly consists of coordination and interaction between specialists and primary care providers. Gruen7 pointed out that it is important to identify the types of interaction most beneficial for patient outcomes; and studies are needed that test the effectiveness of specialist outreach interventions as compared to that of typical modes of care, as well as in comparison to other forms of case management in primary care settings without visiting specialists. The present study addressed these points. The study's target population was rural patients suffering from severe diseases requiring surgical treatment available at only tertiary hospitals. These people could obtain access to surgeons in the Chinese healthcare delivery system, either by referral to tertiary hospitals by local primary care doctors in secondary hospitals or by self-referral directly to the tertiary hospitals.
Public hospitals are the cornerstone of the healthcare delivery system in China. These consist of hospitals at different levels: tertiary hospitals at the provincial, urban, or university level; secondary hospitals at the county level; and health centres at the town or community level. This system is designed to offer continuous healthcare services and promote effective utilisation of healthcare resources. However, the implementation of this system has not brought about as many improvements as expected. This problem arose not only because doctors in secondary hospitals and community health centres lacked sufficient professional skills, but also because there was no coordination between hospitals at the different levels. As a result, elective referrals, which refer to unnecessary and unreasonable referral, largely handled by healthcare insurance systems in developed countries (not likely in China in the near future), were occurring unchecked.
A popular measure to minimise elective referrals is the specialist outreach program, which utilises the green referral channel; this program has shown to be effective in reducing patients' waiting time and costs. It is logical to assume that outreach specialists could offer better-qualified diagnoses and treatments, and thereby minimise elective referrals. Transaction costs could also be minimised through this program. In China, the specialist outreach program was initiated and guided by the authorities; it could therefore be regarded as the redistribution of healthcare resources to reduce disparities in healthcare. As a result, however, data on the management costs of this specialist outreach program were not available for analysis in this study.
The aim of vertical integration of the healthcare delivery system was to improve coordination between doctors across the different tiers of hospitals. This was intended to help them rationally allocate medical service resources and manage the flow of patients by creating efficient referral channels. Conceptually, a medical consortium in China is similar to an integrated healthcare system in the USA, comprising components such as stepped care systems and accountable care organisations (ACOs)27. In the stepped care system, specialists consult with patients and primary care physicians to recommend changes in medication and/or lifestyle; specialists might provide several visits, preferably within the primary care environment. In ACOs, primary and specialty care systems and hospitals work closely together, often as single governing units. These organisations were developed to achieve three major healthcare goals - improvements in access to care, quality of care, and patient outcomes - while reducing total healthcare costs. In fact, the specialist outreach program implemented as part of these Chinese medical consortia and the improved availability of medical resources did provide local residents suffering from severe diseases easier access to high-quality medical resources at a greatly reduced cost.
In the present study, LOS was assessed first because it is directly related to hospitalisation costs. The data showed that the LOS of RO and RL was significantly lower than that of the control group, with the LOS of RO lower than that of RL. It was thus concluded that referrals made by outreach specialists (RO) were more efficient than those made by local doctors (RL) in reducing LOS. In most cases, outreach specialists practising at secondary hospitals and surgeons have privileges at the same tertiary hospital and have a cordial professional relationship. They are usually dispatched to secondary hospitals by turn and present papers at the same academic meetings; therefore, surgeons could schedule surgeries according to diagnoses from outreach specialists quickly, thereby reducing waiting times for surgery from the usual 5-7 days to 1-2 days. This is the core of the green referral channel.
Standard clinical pathways for surgery are also applied to coordinate the referrals between hospitals in China28. Tertiary hospitals dominate the healthcare system and possess the best healthcare resources in terms of quality, including doctors, instruments, and certified surgical facilities designed to serve emergent patients. Through the green referral channel within the consortium, patients are allocated to different levels of hospital care depending on need. When basic diagnostic testing and surgical preparation are performed at the secondary hospitals, the tertiary hospitals can maximise their capacity to provide the advanced critical treatment.
Drug costs accounted for roughly half of total hospitalisation costs and were closely associated with LOS. Thus, these costs decreased in the same pattern as LOS, being highest for the control group, followed by the RL and RO groups. This pattern was also observed in room and board-related costs, which were a small proportion (approximately 13-15%) of total costs. However, these costs did not significantly differ between the RL and RO groups. Patients in all groups underwent the same surgical procedures; thus, surgery costs, roughly 15-18% of the total amount, were not significantly different or had only a weakly significant difference between groups.
Diagnostic testing costs were significantly different between groups. The pattern was reversed in this category, however, with the highest costs found in the RL group, followed by the control group and then the RO group. For patients with referrals from secondary hospitals, regardless of whether they belonged to the RO or RL groups, testing was partially conducted by the secondary hospitals at costs approximately 15% lower than those of tertiary hospitals, in accordance with regional price guidelines set by the health authorities. The advantage of the green referral channel was evident in the RO group, in which the results of most testing performed at the secondary hospitals were accepted by surgeons from the tertiary hospitals because of their existing professional relationship, thereby reducing costs for such patients. In the absence of this professional respect, as in RL when the surgeons were not as likely to be familiar with the local physicians, most testing performed at secondary hospitals was rejected by the surgeons. This resulted in repeat testing and therefore increased costs, even greater than those of the control group, despite the lower LOS. Fortunately, diagnostic testing expense accounted for only about 20% of total costs, too little to affect the trend of average total hospitalisation costs by group.
Therefore, it was concluded that referral by outreach specialists operating as part of a medical consortium could reduce total hospitalisation costs, with the green referral channel playing a key role. Referrals from local doctors were observed to reduce costs, although the extent of this reduction was less than that resulting from referrals from outreach specialists. The outreach specialists served to integrate the consortium. The present results are consistent with findings indicating that the closer the integration, the lower the total costs, as a result of minimised transaction costs29, which include time and costs of patients saved by outreach specialists from the medical consortium. The green referral channel was intended to benefit all doctors, not just the outreach specialists but, as previously discussed, this channel works against local doctors. Therefore, the green referral channel should be improved and expanded through increased opportunities for collaboration between local doctors and outreach specialists so that the medical consortium may realise its full potential.
One of the goals of the medical consortium was to establish local doctors as links between secondary and tertiary hospitals through referrals. However, as this study has shown, this goal was not achieved in terms of cost savings. To reap the full benefit of the consortium structure and the green referral channel, additional opportunities and incentives for collaboration (eg training programs) could be introduced to encourage outreach specialists to assist local doctors. This would facilitate communication between local doctors and tertiary surgeons and thus make surgery reservation easier. As suggested by this study's results, these professional relationships can lead directly to lower treatment costs. Therefore, the green referral channel has the potential to benefit both outreach specialists and local doctors, significantly improving the quality of care for rural residents, particularly those requiring advanced surgical treatment, while lowering total costs.
The specialist outreach program is a product of the current imbalance of healthcare resources in China. Until healthcare resource distribution is truly equalised, specialist outreach programs, especially those operating as part of a medical consortium, are an effective way to provide equitable access to health care to residents in rural and remote areas.
References
1. Tang S, Meng Q, Chen L, Bekedam H, Evans T, Whitehead M. Tackling the challenges to health equity in China. Lancet 2008; 372: 1493-1501.
2. Chen Z. Launch of the health-care reform plan in China. Lancet 2009; 373: 1322-1323.
3. Hu ZC, Liu XM, Sun ZY, Yao H, Hou Y. Problems and answers for deepening reform of health sector. [in Chinese] Beijing: People's Publishing House, 2009 .
4. Wang C, Xian M. Political analysis project of thousands of doctors supporting for the rural area. [in Chinese] Zhong Guo Yi Yuan Guan Li [Chinese Hospital Management] 2008; 28: 9-12.
5. Wang C. Practice and research of project of thousands of doctors supporting for the rural area. [in Chinese] Zhong Guo Yi Yuan Guan Li [Chinese Hospital Management] 2007; 27: 22-24.
6. Thomas CL, O'Rourke PK, Wainwright CE. Clinical outcomes of Queensland children with cystic fibrosis: a comparison between tertiary centre and outreach services. Medical Journal of Australia 2008; 188: 135-139.
7. Gruen RL, Weeramanthri TS, Knight SE, Bailie RS. Specialist outreach clinics in primary care and rural hospital settings. Cochrane Database of Systematic Reviews 2004; (1): CD003798.
8. Gruen RL, Bailie RS, Wang Z, Heard S, O'Rourke IC. Specialist outreach to isolated and disadvantaged communities: a population-based study. Lancet 2006; 368:130-138.
9. Gruen RL, Bailie RS, d'Abbs PH, O'Rourke IC, O'Brien MM, Verma N. Improving access to specialist care for remote Aboriginal communities: evaluation of a specialist outreach service. Medical Journal of Australia 2001; 174: 507-511.
10. Garrido-Elustondo S, Molino-González AM, López-Gómez C, Arrojo-Arias E, Martín-Bun M, Moreno-Bueno MA. Coordination between primary and specialist care. Satisfaction with consulting specialist project. Revista de Calidad Asistencial 2009; 24: 263-271.
11. Kates N, Craven MA, Crustolo AM, Nikolaou L, Allen C, Farrar S. Sharing care: the psychiatrist in the family physician's office. Canadian Journal of Psychiatry 1997; 42: 960-965.
12. Bowling A, Bond M. A national evaluation of specialists' clinics in primary care settings. British Journal of General Practice 2001; 51: 264-269.
13. Black M, Leese B, Gosden T, Mead N. Specialist outreach clinics in general practice: what do they offer? British Journal of General Practice 1997; 47: 558-561.
14. Helliwell PS. Comparison of a community clinic with a hospital outpatient clinic in rheumatology. British Journal of Rheumatology 1996; 35: 385-388.
15. Drew J, Cashman SB, Savageau JA, Stenger J. The visiting specialist model of rural health care delivery: a survey in Massachusetts. Journal of Rural Health 2006; 22: 294-299.
16. Israel BA, Coombe CM, Cheezum RR, Schulz AJ, McGranaghan RJ, Lichtenstein R, et al. Community-based participatory research: a capacity-building approach for policy advocacy aimed at eliminating health disparities. American Journal of Public Health 2010; 100: 2094-2102.
17. Kifle YA, Nigatu TH. Cost-effectiveness analysis of clinical specialist outreach as compared to referral system in Ethiopia: an economic evaluation. Cost Effectiveness and Resource Allocation 2010; 8: 13.
18. Ceaser M. Taking surgical services to rural Ecuador. Lancet 2006; 368: 1563-1564.
19. Cotton MH. Five years as a flying surgeon in Zimbabwe. World Journal of Surgery 1996; 20: 1127-1130.
20. Zhou B, Li JS, Shen W, Chen XQ. Research on functional orientation of tertiary public hospital to aid community healthcare service. [in Chinese] Zhong Guo Yi Yuan [Chinese Hospitals] 2008; 12: 57-59.
21. Shi G, Wu T, Xu WG. A survey on the attitudes of doctors towards health insurance payment in the medical consortium. [in English] Chinese Medical Journal 2011; 124: 223-226.
22. Xu ZH, Xu WG. Study on the establishment of medical consortium linked by every annual budget of medical insurance. [in Chinese] Zhong Guo Wei Sheng Jing Ji [Chinese Health Economics] 2011; 30: 54-56.
23. China Health Statistics Year Book. 2010 (Online). Available: http://www.moh.gov.cn/publicfiles/business/htmlfiles/zwgkzt/ptjnj/year2010/index2010.html (Accessed 8 October 2010).
24. Barnes CA. Disease staging: a clinically oriented dimension of case mix. Journal of the American Medical Record Association 1985; 56: 22-27.
25. D'Hoore W, Bouckaert A, Tilquin C. Practical considerations on the use of the Charlson comorbidity index with administrative data bases. Journal of Clinical Epidemiology 1996; 49: 1429-1433.
26. Duan N. Smearing estimate: a nonparametric retransformation method. Journal of the American Statistical Association 1983; 78: 605-610.
27. Lowell KH, Bertko J. The Accountable Care Organization (ACO) model: building blocks for success. Journal of Ambulatory Care Management 2010; 33(1): 81-88.
28. Luo Y, Xu WG, Zhou X, Zhou B, Liu JJ, Deng XM. Dual referral function and guideline between municipal hospital and primary hospital for chronic obstructive pulmonary disease. [in Chinese] Zhong Guo Yi Yuan [Chinese Hospitals] 2010; 14: 45-46.
29. Conrad DA, Dowling WL. Vertical integration in health services: theory and managerial implications. Health Care Management Review 1990; 15: 9-22.
