In many nations, healthcare reforms are moving towards universal cost coverage. As the world's largest developing country, China's healthcare reforms attract considerable international attention.
The Cooperative Medical Scheme
Historically, the Cooperative Medical Scheme (CMS) was implemented in rural China in the 1950s. Organized at a village level, CMS benefits typically included free medical consultations and free or discounted medicine from village health clinics, and a co-payment for hospital referrals1. Rural CMS healthcare financing relied on a pre-payment plan supported by three sources: (i) premiums of between 0.5% and 2% of yearly income were paid per farmer's household to the commune fund system, as decided by the plan's benefit composition and the local community's economic level; (ii) each village contributed a certain portion of its income from shared agricultural production or rural ventures to a welfare fund, according to state guidelines; and (iii) government subsidies were used to compensate health workers and purchase medical equipment2. As promoted by the Chinese government, the CMS experienced dramatic expansion in the 1960s and 1970s. At its peak in 1978 the CMS covered 90% of China's rural population1 ensuring access to basic health care, and was widely considered one of the more successful healthcare models in a developing nation.
Since the 1980s and China's move towards a market economy, economic reform and the replacement of collective agricultural production with the 'household responsibility system' have drastically reduced financial support for the CMS. Most schemes collapsed when the CMS's financial base and funding eroded, and coverage rates fell sharply from 90% in 1980 to 5% in 19851. Despite various attempts to rebuild an insurance system, coverage rates remained low and the majority of rural residents were uninsured between 1985 and 2003. Following the CMS's collapse, many rural residents, particularly those economically disadvantaged, were in a difficult position. Usage charges and high medical costs hindered access to even basic health care, and medical expenses were the cause of financial catastrophe for many rural families2, to the point where medical expenditure was a major cause of poverty in rural China3.
The new government-supported CMS (NCMS)
The China National Rural Health Conference in Beijing on 29 October 2002 sought to address these issues. This meeting proposed nine national policies to support and strengthen rural healthcare financing and delivery, with the decision to develop a new government-supported CMS a key plank among them2. Subsequently the New Rural Cooperative Medical Scheme (NCMS) was implemented, incrementally, on a county-by-county basis from early 2003.
The primary aim of the NCMS is to improve rural residents' access to healthcare services and prevent impoverishment due to medical expenses. The NCMS follows three design and implementation guidelines: (i) voluntary enrollment; (ii) county level administration; and (iii) a focus on catastrophic illness, funded from central and local government and individuals. Enrollment as a family unit is required to reduce the risk of enrolling a disproportionate number of individual members with high medical expenses due to voluntary enrollment4. The number of NCMS programs across China has grown rapidly and by the end of 2004 there were 333 county programs, increasing to 2319 by March 20075. At the end of 2008, almost 91% of the rural population was covered by the NCMS6.
In general, the NCMS focuses on inpatient care reimbursement and before the 2009 healthcare reforms, the NCMS made high copayments and had high coinsurance rates. Outpatient care was typically covered by household savings, creating no risk for the scheme7.
The authority to design and implement NCMS programs rests with local government, therefore the scheme differs among regions, with research showing disparities in health service use and outcomes among China's ethnic minority groups, as in other countries8-10.
Guangxi Zhuang Autonomous Region
Guangxi Zhuang Autonomous Region (hereafter referred to as Guangxi) is a typical ethnic minority region in southern China. Bordering Vietnam to the south, it covers 236 700 km2. Guangxi has 11 ethnic minority groups (the highest number in China), including the Zhuang, Yao, Miao, Dong and Mulao, accounting for 38% of its population, or 19.57 million people. The Zhuang are China's largest ethnic minority group and they live mainly in Guangxi. There are 14 prefecture-level cities and 110 county-level jurisdictions in Guangxi. In the region 82% of the 51.59 million inhabitants are farmers. In 2011, Guangxi's per capita domestic product was 25,315 Yuan (approximately US$3,997) and the average net income of farmers was 5,231 Yuan (approximately US$826)11.
Guangxi commenced a pilot NCMS program in 2003, with financial risk pooling at the county level to protect individual members. All counties established a management center responsible for enrollment, financing and managing NCMS funds.
Ethnic minority regions in China have undeveloped social economies, with special cultural policy circumstances and environments, and little is known about the NCMS's operation in these regions. An exploration of the NCMS and its application in Guangxi will provide important lessons for other countries moving towards universal health care.
NCMS key aspects in Guangxi
As in all regions, the Guangxi NCMS fund comprises three parts: outpatient, inpatient and reserve. Fund management follows the pay-as-you-go principle. It allocates 10% of fund revenues to a reserve used to cover unforeseen costs. Remaining revenue is used to reimburse healthcare costs. Generally, the surplus fund (including the reserve) accounts for less than 15% of total annual revenues. Total accumulated surplus funds are generally less than 25%.
There are four key aspects to China's rural health insurance scheme: population coverage, revenue collection, reimbursement and healthcare use. These will be discussed with reference to the Guangxi NCMS.
Population coverage: The government regarding NCMS population coverage as a key performance indicator. In Guangxi, where ethnic minorities have their own lifestyles, languages, cultures and religions there is a low level of NCMS comprehension. In addition, low levels of education and literacy contribute to poor awareness of the benefits of joining of the NCMS. Therefore publicity is vital among ethnic minority groups to promote the scheme, and this is done at meetings, and in broadcasts and handouts in an attempt to increase farmer knowledge and awareness.
In February 2003, Guangxi initiated three county NCMS pilots programs which expanded rapidly into many different areas. By the end of 2008, NCMS coverage included all 110 of Guangxi's counties, with 35.42 million enrollments or 86.6% of the population. This continued to rise and by 2011 enrollments included over 90% of Guangxi's population (Fig1).
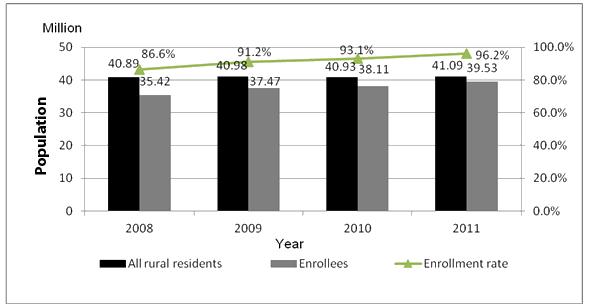
Figure 1: China's New Rural Cooperative Medical Scheme coverage.
Revenue collection: With the NCMS financed by central and local government and individual contributions, as the scheme's benefits expand, continuous political and financial government support is critical for NCMS's sustainability, particularly in ethnic minority regions. As is shown (Fig2), the largest portion of Guangxi NCMS revenue (approximately 80%) is provided by all levels of government.
Individual participation fees were initially set at 10 Yuan per person. However, along with an increase in government contributions, annual member contributions increased from 80 Yuan in 2008 to 230 Yuan in 2011, and these account for between 13% and 20% of NCMS funds. The initial low individual contribution costs aimed to ensure that health care was affordable; however, some impoverished rural residents still had difficulty paying their premiums. A case in point are the many ethnic minority populations who live in remote border areas where there are disadvantaged economies and low income levels. To address this issue, the government established a 'free insured' policy, where rural residents living within 20 km of a geographic border are granted free NCMS membership, with the government paying their participation fees.
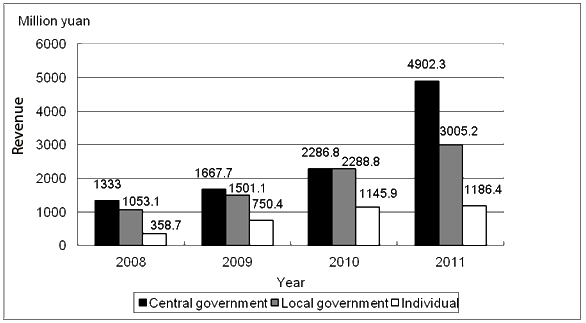
Figure 2: New Rural Cooperative Medical Scheme revenue collection.
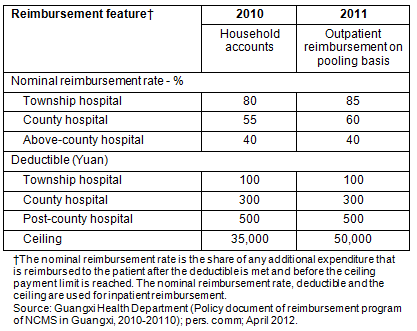
Reimbursement: The NCMS aims to prevent catastrophic healthcare expenditure; therefore, reimbursing inpatients is vital. As is shown (Table 1) the bulk of NCMS reimbursement is for inpatient costs. Complex procedures govern inpatient reimbursement. They are designed to protect the funds financial stability. Typically, reimbursement rules are less generous for care delivered in higher level facilities. Deductible and coinsurance increases from lower to higher level hospitals (Table 2). This feature aims to encourage NCMS members to initially seek health care at lower level facilities.
Total revenue grew significantly between 2010 and 2011 and the nominal reimbursement rate and ceiling increased accordingly. The reimbursement ceiling is set at least six times higher than a local rural residents' annual income. If the total accumulated surplus is more than 25% of total revenue, NCMS management should implement secondary compensation to improve the usage rate of funds (secondary compensation uses surplus funds at the end of a year to further compensate patients who had large medical expenses in that year).
Prior to 2011, Guangxi implemented a 'household savings' model to reimburse outpatients in which a fixed ratio of funds was drawn from individual contributions to cover outpatient care. If a household member did not consult a doctor during one whole year, all the allocated money was reserved and could not be used to reimburse the medical expenditure of other enrollees. However, using this model, less than half the outpatient fund was used. In 2011 the household model was replaced by outpatient reimbursement on a pooled basis, and this has greatly increased the use of the outpatient funds. In 2011 up to 94.45% of outpatient funds were accessed for reimbursement.
Table 1: Use of New Rural Cooperative Medical Scheme funds according to the years 2008-2011
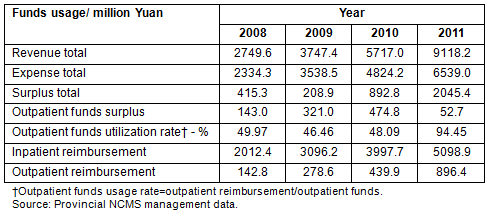
Table 2: Features of New Rural Cooperative Medical Scheme reimbursements, 2010 & 2011
Health service usage: The complexities of Guangxi's 11 ethnic minority population over time resulted in a pluralistic medical system and culture where varieties of Traditional Chinese Medicine (TCM) are prevalent among particular ethnic groups (eg Zhuang medicine and Yao medicine). To encourage utilization of traditional medicine, the reimbursement rate increases 10% if the enrollees use TCM or ethnic minority traditional medicine for treatment.
The reimbursement program is standardized at the provincial level, so NCMS county offices can adjust benefit packages and administrative arrangements to suit local conditions, as long as national and provincial guidelines are followed. However, county NCMS managers may lack the skills to adequately redesign benefit packages for local conditions, often setting reimbursement rates too low out of concern for potential deficits. This produces large surpluses at the end of the year, forcing the implementation of secondary compensation in many counties to balance the funds.
Engagement with, and use of, health services has increased significantly with the introduction of the NCMS, promoting the development of rural health facilities, particularly township hospitals which were struggling for financial survival before the NCMS. While outpatient care is primarily provided by village and township healthcare providers, inpatient care is chiefly delivered in these township and county hospitals.
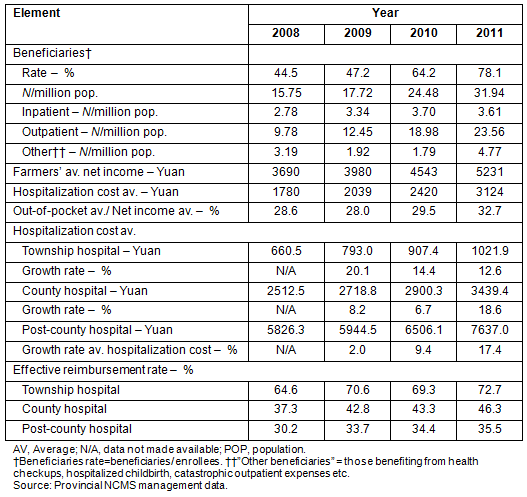
Most rural residents use inpatient services (Fig3), and between 2008 and 2011 admissions to township and county hospitals accounted for more than 80% of all hospitalizations. However, admissions to township hospitals were falling while admissions to county and post-county level hospitals are increasing. As is shown (Table 3) between 2008 and 2011 outpatient numbers increased significantly and there was a significant corresponding increase in healthcare costs. In recent years average costs at township hospitals have increased dramatically while admissions have declined. Costs and patient numbers at county and post-county level hospitals increased while the effective reimbursement for county and post-county level hospital treatment was low. For inpatients, the ratio of average out-of-pocket payments to average net income increased from 28.6% in 2008 to 32.7% in 2011, meaning patients are paying more for hospitalizations and the economic burden on individuals and households is increasing.
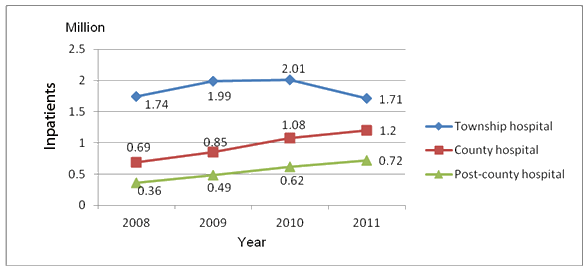
Figure 3: Inpatient usage of Guangxi's New Rural Cooperative Medical Scheme according to hospital type, 2008-2011.
Table 3: Guangxi's New Rural Cooperative Medical Scheme healthcare usage elements, 2008-2011
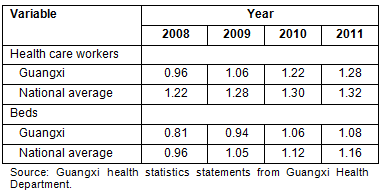
Inadequate healthcare resources affect a population's engagement with, and use of, health services. Prior to 2008 greater attention was needed to the inadequate health resources in rural areas, a common and long-standing problem in ethnic minority regions. As is shown (Table 4), the average number of beds and healthcare workers in Guangxi's township hospitals is much lower than the national average, although the gap has decreased between 2008 and 2011. The reason for this is the NCMS advances since 2008, under which government resources targeted for township hospitals have increased in terms of labor-force, medical equipment and capital expenditure. Qualified healthcare workers are still in obvious shortage, particularly in remote areas.
Fee-for-service, the major payment system in NCMS, encourages health workers to provide unnecessary services. However, NCMS managers lack the capacity to adequately supervise healthcare facilities and the drug management practices of providers. To more effectively control the escalation in medical costs, health authorities are planning to introduce payment reforms, including 'diagnosis related group' (DRG) payment.
Table 4: Number of beds and personnel (per 1000 rural population) at township hospitals, 2008-2011
Guangxi is a low socioeconomic region with a high ethnic minorities population. The regional economy is relatively weak. The population has low education levels and includes many low-income rural residents. In Guangxi the NCMS has expanded rapidly with significant progress but challenges remain. The lessons from NCMS implementation in this region are particularly valuable for those wishing to achieve universal health care for ethnic minority regions in developing countries.
The role of government
China's local and central governments have a dominant role in the implementation and development of the NCMS. The government is the main capital contributor to the scheme and oversees operational management. Although NCMS participation is voluntary, population coverage is extensive. This is primarily because the government assumes main responsibility for the scheme, including finance and management. Standard procedures have been established at central and local government levels for the implementation of budgets, fund allocation and management. The establishment and management, and associated management costs, of the NCMS clearly sit with government. Further, the NCMS's operational management is considered an important local government public administration duty.
Previous studies found that compared with developed areas, in underdeveloped areas the management and fund-raising costs of the NCMS are higher12. In Guangxi, ethnic minorities live in concentrated areas with poor transport and communication links. NCMS policy is more difficult to implement in these rural and remote areas because of these infrastructural difficulties which are compounded by weak economic foundations, low levels of literacy and language barriers. It has been proven that per capita financing costs of NCMS should be less than 1 Yuan12 but per capita financing costs are higher in Guangxi at 4-5 Yuan. For poor farmers and border-dwellers, government offers individual contribution fee exemptions. This not only reduces the financing costs, but also improves the enrollment rate. Due to the governments' main contribution, Guangxi's NCMS has had remarkable achievements in the few years from the pilot stage to a stable institutional operation.
Reimbursement design
NCMS policy aims to 'treat minor illnesses within the village, common diseases within the township, severe diseases within the county, and difficult diseases outside the county'13. In Guangxi's healthcare scheme there is no strict referral system. The ability to adjust the flow of patients, and transfer patients from high to low level hospitals, through the reimbursement system, is crucial. Different deductible and reimbursement rates are set for admissions at the various hospitals. Admission into a higher level hospital attracts a higher deductible and a lower reimbursement rate. This method is particularly useful for adjusting the flow of patients and more than 80% of inpatients are treated in township and county hospitals.
In earlier years, 'household accounts' covered outpatient care, a feature designed as an incentive to rural residents to join the NCMS. It reduced the social pooling function of the scheme and caused large surpluses within the outpatient fund because of low use of outpatient care. With the development of the NCMS, which uses outpatient reimbursement on a pooling basis, enrollment rates are no lower than when household accounts were used14. Studies have showed that outpatient reimbursement on a pooling basis can increase outpatient numbers and optimize fund use15,16. Therefore, once the NCMS is established, outpatient reimbursement, on a pooling basis to cover outpatient care, will provide more favorable results than the household account program.
Traditional Chinese Medicine is a national cultural treasure with an extensive history. It is convenient, simple, cheap and effective. Guangxi, compared with other ethnic minority regions, has allocated greater resources to medicines so those living in remote areas have greater opportunities to access various traditional therapies. To maintain medical pluralism and promote TCM, local government has implemented a policy to develop TCM within the NCMS. The reimbursement rate therefore has been increased by 10% for using TCM as treatment. This local policy contributes to the provision of culturally competent systems of care in Guangxi.
Publicity work
Social and cultural traditions and people's awareness affect the establishment and operation of the health insurance system. Due to the influence of their own religions, some ethnic minority groups believe that fate determines their health and considers that health insurance is unnecessary. In addition, one researcher found households in disadvantaged regions with a high ratio of migrant workers who are less likely to use the NCMS program17. In rural Guangxi, many families have migrant workers due to the poor local economy and there are 600 million migrant workers in Guangxi. Therefore, NCMS publicity is a long-term and continuous process.
The Guangxi government regards NCMS publicity as of great importance and supports advertising administratively. Based on an in-depth understanding of ethnic minorities populations, targeted publicity and educational programs are provided in order to eliminate misunderstandings and increase awareness of NCMS, utilizing press, radio and television. Of particular publicity focus are changes in the benefits package, financing and reimbursement policy, and fully explaining NCMS benefits. These efforts have enhanced enrollments.
Major challenges facing the NCMS
The lack of healthcare resources in Guangxi is a major challenge facing policy-makers. Policy measures need to address human resource issues. Shortages of primary healthcare workers and managers are particularly concerning, but to date complaints about a lack of suitably qualified healthcare employees and management have not been heeded. As discussed, NCMS county management offices exercise considerable discretion regarding reimbursement design and implementation. Therefore, effective management skills are vital, particularly for the success and development of the scheme's funds. Programs are needed to attract health workers to rural and remote areas, and management training is required for county NCMS personnel.
Finally, the rapid growth in medical costs in Guangxi is a serious issue. Although reimbursement levels rose with increasing NCMS financing, hospitalization costs also grew rapidly. Therefore, the effective reimbursement rate is low, particularly for care in higher level hospitals. Rising medical costs decreases the protection afforded by the NCMS against financial catastrophe and household impoverishment resulting from medical expenses. The government has prioritized the containment of healthcare costs and plans to implement payment reforms for the NCMS. A capitation payment method will be explored for outpatient care, while the DRG payment method will be used for inpatient care.
Reform of the healthcare system is needed. The shortage of skilled healthcare workers and an underdeveloped healthcare system creates major challenges for the local Guangxi government. Relevant resources and technical assistance is widely needed.
Conclusion
Guangxi has successfully developed a rural health insurance scheme, although some limitations and problems remain. To maintain the system's sustainability, special institutional arrangements and effective policy measures for the ethnic minorities in the region should be further considered and addressed.
References
1. Liu X, Cao H. China's cooperative medical system: its historical transformations and the trend of development. Journal of Public Health Policy 1992; 13(4): 501-511.
2. Liu Y. Development of the rural health insurance system in China. Health Policy and Planning 2004; 19: 159-165.
3. Liu Y, Rao K, Hsiao W. Medical Expenditure and Rural Impoverishment in China. Journal of Health, Population, and Nutrition 2003; 21: 216-222.
4. Yi H, Zhang L, Singer K. Health insurance and catastrophic illness: a report on the new cooperative medical system in rural China. Health Economics 2009; 18: S119-S127.
5. Brown P, Brauw A, Du Y. Understanding variation in the design of China's New Cooperative Medical System. The China Quarterly 2009;198: 304-329.
6. Ministry of Health. [Statistics bulletin on the development of health service in 2008]. (Online) 2009. Available: http://www.moh.gov.cn/mohbgt/s3582/200812/38473.shtml (Accessed 15 May 2012).
7. Hou Z, Poel E, Doorslaer E, Yu B, Meng Q. Effects of NCMS coverage on access to care and financial protection in China. (Online) 2012. Available: http://papers.ssrn.com/sol3/papers.cfm?abstract_id=2040701 (Accessed 25 August 2012).
8. Fiscella K, Franks P, Doescher M, Saver B. Disparities in health care by race, ethnicity, and language among the insured: findings from a national sample. Medical Care 2002; 40: 52-59.
9. Li Y, Aranda M, Chi I. Health and life satisfaction of ethnic minority older adults in mainland China: effects of financial strain. International Journal of Aging & Human Development 2007; 64: 361-379.
10. Alegria M, Lin J, Chen C, Duan N, Cook B, Meng X. The impact of insurance coverage in diminishing racial and ethnic disparities in behavioral health services. Health Services Research 2012; 47: 1322-1344.
11. Guangxi Bureau of Statistics. Statistics bulletin on the economy and social development of Guangxi in 2011. (Online) 2012. Available: http://www.gxtj.gov.cn/tjsj/tjgb/201212/t20121210_25529.html (Accessed 20 May 2012).
12. Tan L, Tian Q, Hou Z, Li Y, Zhang L, Xiao J. Analysis of influencing factors of fund raising cost in New Rural Cooperative Medical System. Chinese Health Services Management 2012; 7: 517-519 (in Chinese).
13. Li B. The goal and principle of construction of new rural cooperative medical scheme. Journal of Hunan Agricultural University (Social Sciences) 2011; 6: 7-9 (in Chinese).
14. Zuo Y, Hu S, Liu B, Jiang Q. Comparative study on the models of outpatient reimbursement on pooling basis and household savings accounts in new rural cooperative medical scheme. Chinese Health Economics 2006; 25: 19-21 (in Chinese).
15. Yang H. Effect analysis for new rural cooperative medical scheme: two kind of outpatient service compensation in Dali. Chinese Health Economics 2009; 28: 42-45 (in Chinese).
16. Zuo Y, Hu S, Liu B, Jiang Q. The influence of outpatient reimbursement on pooling basis of new rural cooperative medical scheme in health services utilization and management. Health Economics Research 2008; 2: 18-20 (in Chinese).
17. Liu D, Tsegai D. The New Cooperative Medical Scheme (NCMS) and its implications for access to health care and medical expenditure: evidence from rural China. ZEF- discussion papers on development policy No. 155. (Online) 2011. Available: http://ssrn.com/abstract=1945173 (Accessed 26 August 2012).
Published 11 April 2013; modified 23 April 2013.
A correction (underlined) was made to the following sentence in the Context section: "The authority to design and implement NCMS programs rests with local government, therefore the scheme differs among regions, with research showing disparities in health service use and outcomes among China's ethnic minority groups, as in other countries 8-10."




