Sparsely populated areas like Australia's Northern Territory, the northern provinces of Canada, and the Arctic north of Europe are likely to have inherently inefficient labour markets because they lack sufficiently large core population centres to produce surplus labour which can be redeployed to more rural and remote areas1,2. As a consequence, it is difficult to provide adequate labour for large development ventures such as those in the resources sector3. One mechanism to address labour shortages while pursuing large projects has been to use non-resident labour (fly-in/fly-out, drive in/drive out etc). Non-resident labour can be defined as consisting of people who work in the sparsely populated area but are normally residents of another area. Non-resident labour live in multiple worlds4 - the world of work, the world 'at home', and the commuting world in between. Both social and professional capabilities and adaptations are affected by the movement between these worlds5.
Non-resident labour is not limited to the resources sector or related activities such as construction and transport. Wakerman, Curry and McEldowney recently called attention to the non-resident health workforce in remote Australia6 with concerns about the implications for quality and continuity of care, the performance of inter-professional primary healthcare teams, cost of service provision, and retention of resident workers who may experience increased workloads and changed scope of practice as they become part of a reduced 'on the ground' presence. Nonetheless, Wakerman, Curry and McEldowney acknowledge that the use of non-resident labour has helped address severe workforce shortages, enables services to be provided in locations where resident services are unviable because of patient numbers or the demand for complex skill sets6,7, and is therefore likely to not only continue but to expand in size and scope over time.
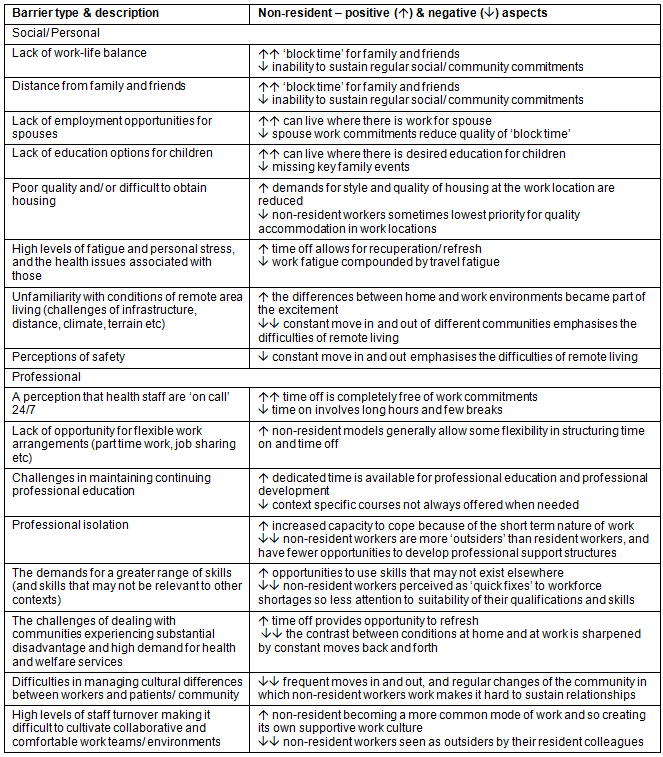
The purpose of this research was to assess the extent to which the use of non-resident labour in the health sector, specifically non-resident nurses, might address the well-known barriers (Table 1) to recruitment and retention of remote health professionals (eg8,9). In-depth interviews were conducted with a small number of non-resident nurses who were working in remote communities in Australia's Northern Territory in 2011. As yet, there have been no published studies of the non-resident nursing workforce in remote Australia or elsewhere, despite an increasing interest in the application of such workforce models10,11.
Table 1: Established barriers to recruitment and retention of remote area health professionals12-27

Many identified barriers are becoming more substantial over time as the health professional workforces age (and so have increased personal and professional demands) and the sources of health professionals become more diverse (including increasing numbers of overseas trained professionals)28. Workforce modelling by Health Workforce Australia29 suggests that the gap between demand and supply is likely to increase rather than decrease in coming years, in part because of these barriers but also due to increasing competition for labour from rural and urban areas.
There is a tradition of using various forms of non-resident health professional labour in remote areas10. This includes flying doctor services, locum services, specialists who 'rotate' through a number of practice locations, and the use of 'agency' nurses to fill short-term shortages. Indications are that the use of such models is increasing, and particularly that the use of 'agency' and short-term contract nurses has become the norm in a number of locations across the Northern Territory6.
Research from the resources sector has identified a range of positive and negative impacts from non-resident work practices on the workers themselves. A useful summary of these from a health perspective can be found in Torkington et al30. Positive impacts include financial gain, as non-resident workers tend to be paid more than resident workers in equivalent positions31, blocks of time away from work32, and the ability to experience 'the best of both worlds'33 provided by the differences between home and work environments34. The negative impacts include difficulties in establishing and sustaining personal relationships35, difficulties in engaging in regular social and leisure activities31, and impaired personal health30. These positive and negative impacts are not universally experienced by non-resident workers, who are required to (but often fail to) develop strategies to maximise positive impacts and minimise negative ones36.
Much of the non-resident workforce literature has focussed on social/personal barriers, rather than professional. Most commonly, non-resident work is seen as a 'fast track' to career advancement for the individual3,37, and questions about whether that is at the expense of work quality are rarely asked. Similarly, while it is acknowledged that remote health services often consist of a mix of resident providers, visiting specialists, and even telehealth applications10, there has yet to be critical examination of what mix delivers optimum outcomes for patients or service providers, what roles are best suited to resident, non-resident or not-present modes of work, and little examination of how health service teams can work effectively within a 'mixed mode'.
The status of female non-resident workers is also of interest for those nursing in the remote Northern Territory, given that over 80% of that workforce is female38. Pirotta argued that female, non-resident workers in the resources sector did not enjoy all the benefits that accrued to their male colleagues, largely because of the additional responsibilities females carry for maintaining family and social relationships, and particularly caring for children37. To balance this, females may benefit more from the ability to maintain their families in residential locations which have good schools and other amenities, while benefiting from the financial rewards of working in remote areas37.
In summary, there is emerging concern in the health literature about the impacts of non-resident work modes on the quality of service delivery particularly in sparsely populated areas, but little is known about what non-resident health workers themselves see as the advantages and disadvantages of their modes of work, and whether non-resident workers face the same or different social/personal and professional barriers to rural and remote practice as their resident colleagues. Literature from the resources sector provides insights into the expected social/personal advantages and disadvantages, but very little is said about professional issues. The current research begins to address some of these gaps in the literature through in-depth interviews with a small number of non-resident nurses working in the more remote parts of Australia's Northern Territory.
Approach
In-depth, semi-structured interviews were conducted with seven nurses who were working in remote communities in the Northern Territory (outside greater Darwin, Alice Springs, Katherine, Tennant Creek and Nhulunbuy) during the second half of the year 2011. Nurses self-selected to be interviewed following a research announcement in the monthly e-newsletter distributed by the Northern Territory Department of Health to all nurses registered in the Northern Territory. Nurses were included in the sample if they considered themselves to normally live in a community apart from the one in which they worked, and if they stayed away from their home community for the periods in which they were working. Participants were interviewed about their life and professional histories, their work patterns in the Northern Territory, and their perceptions of the impacts of non-resident work on their professional and private lives.
Interviews were analysed thematically using themes drawn from the literature (Table 1) and aligned with the social/personal and professional aspects of the nurses' experience. Interviews were separately analysed by each of the two researchers involved in the project, and thematic groupings compared. Differences in allocations of themes were resolved jointly.
Participants
A sample of seven nurses self-selected for the research. The sample size was limited by a number of factors, including difficulties in making contact with nurses appointed by agencies based outside the Northern Territory (ie not all non-resident nurses would be on the Department of Health contact list), the small size of the total population (estimated from 2006 Census data to be approximately 100 nurses) and the high mobility of non-resident nurses not only between jobs in the Northern Territory, but elsewhere in Australia (most agencies place nurses in a variety of jurisdictions). The sample size was also limited by the resource constraints of the research (limited time and financial resources to travel to remote locations to interview nurses) and the desire to extract in-depth and often personal stories and insights from research participants. However, the generalisation of the results of these interviews to the total non-resident nursing workforce in remote Northern Territory (or elsewhere) was not the primary function of this research. Rather, a small number of detailed cases have been used to explore the issues raised in the literature and to establish a base for further research.
The sample included one male nurse, five nurses who were in steady personal relationships, (four with children), and three had previous experience as resident nurses in the Northern Territory. All participants were aged over 35 years, and each had more than 10 years of nursing experience.
Context
The Northern Territory as a context for remote nursing practice has been well described previously18,38. It covers an area of approximately 1.5 million km2, and has an estimated resident population of approximately 220 000 people. Over half of the population (120 000) live in the capital city of Darwin, meaning a population density of less than 0.1 person/km2 in the remaining areas. Approximately half of the residents of remote Northern Territory identify as Indigenous Australians, and many of these people live in discrete 'Indigenous communities' with populations between 200 and 2000 people39. There are very few Indigenous health professionals, meaning that the vast majority of doctors, nurses, and allied health professionals come from outside remote Northern Territory, and there are consequently severe workforce shortages and high rates of workforce turnover40.
Participants in this research generally were recruited to the Northern Territory via nursing agencies headquartered in the more populous eastern state capital cities (Brisbane, Sydney, Melbourne). They generally worked short-term 'placements' in the Northern Territory, moving from one location to another for each new placement (although some returned periodically to previous placement locations). Placement duration varied from one to 6 months, and some of the participants also took on placements in locations outside the Northern Territory (including urban locations as well as rural or remote locations). Periods away from work varied, but were typically no more than one month.
Ethics approval
Ethics approval for the research was obtained from the Charles Darwin University Human Research Ethics Committee (#H11067).
Social/ personal
Participants generally agreed on the benefits of non-resident work in terms of higher incomes, more time off, and the ability to balance time in remote areas with time away. One participant commented that 'the money can be almost twice as much as what you get normally working in hospital' (Nurse 5). Besides higher incomes, the clear benefit of non-resident work to all participants was a sense of work-life balance. Periods at home and the periods at work were clearly differentiated, with 'home time' dedicated to socialising with friends and family, fulfilling family obligations, and undertaking 'projects' that benefit from having a block of time available. For example, Nurse 7 commented on the positive impact non-resident work had on the capacity to undertake house renovations, and Nurse 3 used a block of 'off' time to do a short course in a completely different professional field. Importantly, in terms of relationships with family and friends, participants felt that the length of time off allowed them to clear the stress and problems of work and have a block of time to devote to maintaining relationships.
There were some challenges to the work-life balance. Participants commented that it was difficult to commit to regular activities, such as being involved in sporting teams or community groups. This was the case in both home and work locations. Some participants missed the opportunity to engage with their communities in this way, but others felt compensated by the ability to use 'block time' usefully.
Those participants who were in a relationship and/or had children of their own perceived additional benefits. Nurse 5 recognised the difficulty of trying to find work for a spouse in remote Northern Territory. Non-resident work meant that the spouse could remain in the home location and pursue their own work (or education, or social/ community commitments). Similarly, children's education was taken care of in the home location, addressing the difficulty of finding quality education services in the nurses' work locations.
'Block time' also presented challenges because, while it was available to the non-resident worker, it was not always available to spouses, children or friends. Nurse 1 also commented on the pleasure experienced in being accompanied by the spouse on one placement, but recognised that the spouse's commitments at home made this a rare occurrence. Other participants recognised that missing key events like birthdays, or not being on site when there were family problems was a disadvantage of non-resident work. As a result, participants such as Nurse 4 claimed that non-resident work suited nurses with older families:
My last daughter (aged 19 years) was still living with me. Now she is living with her boyfriend so I don't have to care that much anymore.
Older nurses also tended to have more friends who are retired or semi-retired and so more able to allocate 'block time' to coincide with the non-resident worker's 'time off'.
Most of the participants were satisfied with the quality of housing in their work locations. They felt they had fewer demands about the style and quality of housing than resident workers because it was temporary accommodation. However, and because most housing is provided as part of the work contract, non-resident workers did run the risk of being lowest priority when it came to housing allocation. Nurse 7, for example, had the following experience:
They gave me this place to live in. It hadn't been cleaned, had almost no kitchen, the television didn't work, the washing machine didn't work, there was no ironing board.
Nurse1 confirmed, 'it's a basic level of accommodation'.
Participants did experience high levels of fatigue arising both from the intensity of work during the 'on' time and from the difficulty of travelling between their home and work locations. Nurse 5 gave the following example:
Getting there and coming back, it is four hours on the plane to Darwin then you have got another four hours on the coach to get to Katherine. Then it is another couple of hours on a little plane to fly to where I am supposed to stay. And then you do it all again to come back. I wish they'd get some way like a 'beamer' [instantaneous transport] to step in and step out the other side and you'd be there.
Again, 'block time' away from work was seen as compensating the stress and fatigue of the work environment and that of travel. Block time, for example, allowed Nurse 5 to take 'a few days just to chill out and catch up some sleep' when returning home.
Moving back to work was also stressful and time was needed at the start of a work period to get used to the different living conditions again (including a harsh climate) and relationships experienced there. Participants also noted that while the regular moves between home and work ensured that the challenges of the work environment remained exciting rather than depressing, those challenges were all the more noticeable because of regular absences from them. Challenges included threats to personal safety, and perception of the risk of living in remote communities. Nurse 5 used the story of being unable to leave the house except to go to work due to a fear of dogs which roamed freely around the remote community. Nonetheless, 'loving the community' and the experience of working with Aboriginal people were common motivations for all participants.
Professional
In addition to the social advantages of 'block time' off work, the non-resident model provided periods of time where nurses could disengage professionally from the pressures of working in remote Northern Territory. These pressures included challenging roster patterns, confined living\working conditions, loneliness, and isolation from professional support. 'On' time, however, was dominated by work to an extent that may be greater than that experienced by resident workers. Nurse 4 complained that non-resident work represented 8 weeks of 'working and working'. Nurse 5 also acknowledged that non-resident workers worked more hours, but that 'you are paid well for it'. The flexibility of work arrangements was one of the main reasons for choosing non-resident work models. While time 'on' was full-time work, there was the capacity to have some control over the length of time on and off.
The intensity of time 'on' made it difficult for participants to access professional development/ professional education while in remote areas. However, there was great emphasis placed on development and education by some of the nurses' agencies, and the general feeling was that, overall, they were at least as well supported as resident nurses. Non-resident nurses were funded to attend professional education activities during 'on' and 'off' times (more often during 'off' times), and they also saw value in the range of locally provided activities such as 'four-wheel -driving, computers, satellite phone, medication, the emergency equipment...' (Nurse 1). In fact, several participants saw the range of professional development opportunities available as one of the key advantages in this mode of work.
Professional isolation remained one of the most concerning aspects of their work. Nurse 7 noted that it was difficult to find help when confronted with unfamiliar situations. Nurse 6 asked 'Where is my back up, where is my nearest hospital, who can I call to help?', and Nurse 3 noted that 'there are no colleagues here with me except the pilot, I am always here by myself'. Compensating for professional isolation involved adopting a 'can do' mindset. According to Nurse 4, 'I had to stop crying and realize that, maybe I can do this... I can settle down and do this'.
Isolation meant the need to do work for which the practitioner was not trained or qualified. This included maternal and neonatal work, trauma management, and dealing with unfamiliar diseases and health conditions. Participants generally embraced this challenge, and it became one of the drivers for their increased engagement in professional education. There were concerns, however, about the timing of some of the key professional education activities associated specifically with remote area work. Several participants noted that they were not able to access emergency care and maternity care courses targeted specifically at remote health practitioners until several months after they had been in the field. One of the reasons for this was perceived to be the need for agencies and the Department of Health to get nurses into the field quickly in response to workforce shortages, irrespective of their level of preparedness to be deployed.
However, some participants felt that working in remote communities was one of the few contexts providing opportunities to use their favourite skills. This was particularly the case for those with midwifery training. Nurse 4 described how low fertility rates in urban Australia was reducing the demand for midwifery skills, while continuing high birth rates in remote Aboriginal communities sustained demand.
Working with Aboriginal people was clearly one of the main reasons for choosing remote area work, but also one of the main professional and social challenges. There were mixed perceptions about how well cultural awareness courses prepared participants for the realities of working in remote Aboriginal communities. Outside the clinical setting there were concerns about 'fitting into the community' and managing relationships with local people. This was particularly problematic for those participants who usually worked in different locations on each placement. Nurse 6 declared:
Coming into a new community can always be a bit of a challenge ... fitting in with ... the routines, the way they do things ... how the clinic runs, the politics, the personalit[ies].
The periods of time away from remote settings, while helping manage some of the stress associated with the challenging professional, social, and cultural environments, perhaps made it more difficult to get to know and be comfortable with not just specific communities, but also the overall context of remote Aboriginal health.
The challenge of developing effective work teams and clinical settings was not only exacerbated by the movement in and out of different locations by the non-resident nurses, but also by the continuing high levels of staff turnover among their resident colleagues. Even when non-resident nurses returned to the same community for consecutive placements, often the resident staff had changed, and the process of team building had to begin again. Nurse 2 noted that there was 'not one person here at the clinic that was here when I started'. Nurse 7 also claimed that long-term resident workers were often unwilling to befriend non-resident workers because of the temporary nature of any relationships that would be created. There was some evidence that the continuing status of non-resident nurses as 'outsiders' (Nurse 6) made it more difficult to develop positive professional relationships and deal with the inevitable personality clashes and tensions that exist in small and isolated work teams. However, non-resident work was perceived as becoming more common among remote area staff, and so procedures to integrate non-resident workers into work environments (eg induction check-lists) were becoming more widely used. Non-resident workers were supportive of one another and there was a common understanding of the challenges faced.
Discussion
On balance, non-resident workers thought that the benefits of the work model outweighed the burdens. This is not a surprising result given that the participants had self-selected the role of non-resident workers and were intending to continue in that work mode. In general, however, the perceived benefits of non-resident work were largely related to personal and social issues (Table 2). Professional barriers to recruitment and retention were less likely to be addressed through non-resident work. In some areas - particularly professional isolation, and familiarisation with the challenging work environment - non-resident work may exacerbate the barriers. On the personal/social level, non-resident work allowed participants to maintain a 'home' far away from where they worked, but it did not provide a sense of having 'two homes' - the place of work was very much compartmentalised and social interactions there were limited.
Table 2: Positive & negative aspects to non-resident work, according to barriers to recruitment and retention of remote area health professionals
Our participants felt that non-resident work was a sustainable choice for them in the longer term. This was in part because it is becoming increasingly common in remote areas, so participants felt that they would have more control over work conditions as time went on. There were some concerns about the compatibility of current human resources procedures and the reality of non-resident work, for example, that were perceived as likely to be resolved in time as non-resident work became the norm. Participants were also beginning to exercise more control over where they worked (eg whether they could return to favourite communities or move to new communities each time), and how their on and off time was structured.
Interestingly, non-resident work was seen as most suitable for older nurses, who had less urgent family responsibilities at home (particularly for young children or for commencing partnerships and family life). Given an ageing nurse workforce nationally, and an historical difficulty in attracting older and more experienced nurses to work in remote areas18, non-resident work may open new recruitment markets for places like the Northern Territory. What was have learned in this research, however, is that these new markets, while more able to deal with the social/personal challenges of remote area work, will still present substantial professional challenges.
The apparent tensions between resident and non-resident workers are something that has not yet been well explored in the literature. Eilmsteiner-Saxinger reported that non-resident workers in the hydrocarbon industry in northern Russia were determined to be valued to the same extent as their resident colleagues4, which suggests a perceived undervaluing of their contribution by at least some people some of the time. Wakerman et al suggested that the presence of non-resident workers serves to increase pressures and stresses on their resident colleagues6, and this dynamic may be reflected in the concerns expressed by the participants in the present research. Overall, this factor emerged as the only additional potential barrier to recruitment and retention of a non-resident nursing workforce, compared with a resident nursing workforce.
This research investigated the ways in which non-resident modes of nursing work in remote Northern Territory compensate for the well-established barriers to recruitment and retention of resident nurses. The greatest area of concern is with the impacts of non-resident work on professional competence. While non-resident nurses had similar social/personal experiences to other non-resident workers, the idea that some types of work are context-specific and so require the sorts of immersion in a location that is best facilitated by being resident there is a new contribution to the general literature. It may well be that much of the work previously discussed in the literature (largely in the resources sector) is considered relatively independent of the context in which it takes place, and so the motivation to research professional impacts of different modes of work has been low.
While this research has commenced the process of understanding non-resident nursing work from the non-resident worker's perspective, there are many questions yet to be answered about how patient communities, professional colleagues, managers and employers perceive the challenges and benefits associated with non-resident workforces. The evidence from this research is that non-resident modes of work do have the potential to at least partially address remote area workforce challenges by extending the range of workers who could be recruited and retained (ie not just those who can work and live in sparsely populated areas, but also those who might work there while living elsewhere). To take real advantage of this extended range of candidates, attention needs not only to be paid to the filling of workplace vacancies as the desired outcome, but also to ways in which non-resident workers can be better prepared professionally for the challenges of remote area work, and the ways in which resident and non-resident work teams can be effectively developed.
References
1. Carson D. Skilled labour migration flows to Australia's Northern Territory 2001-2006: beyond periphery? Australian Journal of Labour Economics 2011; 14(1): 15-33.
2. Ensign PC, Giles A, Reed MG. Labour migration: what goes around comes around. In: Carson D, Rasmussen R, Ensign P, Huskey L, Taylor A (Eds). Demography at the Edge: Remote human populations in developed nations. Farnham, UK: Ashgate; 2011; 189-212.
3. Storey K. Fly-in/ Fly-out: implications for community sustainability. Sustainability 2010; 2(5): 1161-1181.
4. Eilmsteiner-Saxinger G. 'We feed the nation': Benefits and challenges of simultaneous use of resident and long-distance commuting labour in Russia's Northern Hydrocarbon Industry. Journal of Contemporary Issues in Business and Government 2011; 17(1): 53-67.
5. Reuschke D. Job-induced Commuting between Two Residences - Characteristics of a Multilocational Living Arrangement in the Late Modernity. Comparative Population Studies 2010; 35(1): 107-134.
6. Wakerman J, Curry R, McEldowney R. Fly in/fly out health services: the panacea or the problem? Rural and Remote Health 12: 2268. (Online) 2012. Available: www.rrh.org.au (Accessed 18 June 2013).
7. Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia - a systematic review. BMC Health Services Research 8(276). (Online) 2008. Available: http://www.biomedcentral.com/1472-6963/8/276 (Accessed 18 June 2013).
8. Francis KL, Mills JE. Sustaining and growing the rural nursing and midwifery workforce: Understanding the issues and isolating directions for the future. Collegian: Journal of the Royal College of Nursing Australia 2011; 18(2): 55-60.
9. Molinari DL, Bushy A. The Rural Nurse: Transition to practice. New York: Springer, 2012.
10. Birks M, Mills J, Francis KL, Coyle M, Davis J, Jones J. Models of health service delivery in remote or isolated areas of Queensland: a multiple case study. Australian Journal of Advanced Nursing 2010; 19(1): 36-45.
11. Hanley P. The FIFO conundrum. Australian Journal of Rural Health 2012; 20: 48.
12. Buchan J. Nurses' turnover: reviewing the evidence, heeding the results? Journal of Advanced Nursing 2012. Available: http://onlinelibrary.wiley.com/doi/10.1111/j.1365-2648.2012.06080.x/pdf (Accessed 18 June 2013).
13. Wood PJ. Historical imagination and issues in rural and remote area nursing. Australian Journal of Advanced Nursing 2010; 27(4): 54-61.
14. Aylward M, Gaudine A, Bennett L. Nurse Recruitment and Retention in Rural Newfoundland and Labrador Communities: The Experiences of Healthcare Managers. Online Journal of Rural Nursing and Health Care 11(1). (Online) 2011. Available: http://rnojournal.binghamton.edu/index.php/RNO/article/view/9 (Accessed 18 June 2013).
15. Roberge CM, Lavoie JG. Who Stays in Rural Practice?: An International Review of the Literature on Factors Influencing Rural Nurse Retention. Online Journal of Rural Nursing and Health Care 8(2). (Online) 2008. Available: http://rnojournal.binghamton.edu/index.php/RNO/article/view/107 (Accessed 18 June 2013).
16. Roger AR, Andrilla CHA, Thomas C, Hart LG. Shortages of medical personnel at community health centers: implications for planned expansion. JAMA 2006; 295(9): 1042.
17. Opie T, Dollard M, Lenthall S, Wakerman J, Dunn S, Knight S et al. Levels of occupational stress in the remote area nursing workforce. Australian Journal of Rural Health 2010; 18(6): 235-241.
18. Voit K, Carson D. Retaining Older Experienced Nurses in the Northern Territory of Australia: A Qualitative Study Exploring Opportunities for 'Post-Retirement' Contributions. Rural and Remote Health 12: 1881. (Online) 2012. Available: www.rrh.org.au (Accessed 18 June 2013).
19. McCullough KM, Williams AM, Lenthall S. Voices from the bush: remote area nurses prioritise hazards that contribute to violence in their workplace. Rural and Remote Health 12: 1972. (Online) 2012. Available: www.rrh.org.au (Accessed 18 June 2013).
20. Stewart NJ, D'Arcy C, Kosteniuk J, Andrews ME, Morgan D, Forbes D et al. Moving On? Predictors of Intent to Leave Among Rural and Remote RNs in Canada. Journal of Rural Health 2011; 27(1): 103-113.
21. Moseley A, Jeffers L, Paterson J. The retention of the older nursing workforce: A literature review exploring factors which influence the retention and turnover of older nurses. Contemporary Nurse 2008; 30(1): 46-56.
22. Andrews ME, Stewart NJ, Pitblado JR, Morgan DG, Forbes D, D'Arcy C. Registered nurses working alone in rural and remote Canada. Canadian Journal of Nursing Research 2005; 37(1): 14-33.
23. Leipert B, Anderson E. Rural nursing education: a photovoice perspective. Rural and Remote Health 12: 2061. (Online) 2012. Available: www.rrh.org.au (Accessed 18 June 2013).
24. Lenthall S, Wakerman J, Opie T, Dunn S, MacLeod M, Dollard M et al. Nursing workforce in very remote Australia, characteristics and key issues. Australian Journal of Rural Health 2011; 19(1): 32-37.
25. Mullei K, Mudhune S, Wafula J, Masamo E, English M, Goodman C et al. Attracting and retaining health workers in rural areas: investigating nurses' views on rural posts and policy interventions. BMC Health Services Research 2010; 10(S1). Available: http://www.biomedcentral.com/1472-6963/10/S1/S1 (Accessed 18 June 2013).
26. Muecke A, Lenthall S, Lindeman M. Culture shock and healthcare workers in remote Indigenous communities of Australia: what do we know and how can we measure it? Rural and Remote Health 11: 1607. (Online) 2011. Available: www.rrh.org.au (Accessed 18 June 2013).
27. Hayes LJ, O'Brien-Pallas L, Duffield C, Shamian J, Buchan J, Hughes F et al. Nurse turnover: A literature review - An update. International Journal of Nursing Studies 2012; 49(7): 887-905.
28. Mills J, Birks M, Hegney D. The status of rural nursing in Australia: 12 years on. Collegian: Journal of the Royal College of Nursing Australia 2010; 17(1): 30-37.
29. Health Workforce Australia. Health Workforce 2025. Adelaide, SA: Health Workforce Australia, 2012.
30. Torkington AM, Larkins S, Gupta TS. The psychosocial impacts of fly-in fly-out and drive-in drive-out mining on mining employees: A qualitative study. Australian Journal of Rural Health 2012; 19(3): 135-141.
31. Carter T, Kaczmarek E. An exploration of Generation Y's experiences of off-shore fly-in/fly-out employment. Australian Community Psychologist 2009; 21(2): 52-66.
32. Gallagos D. Aeroplanes Always Come Back: Fly-in Fly-out Employment: Managing the Parenting Transitions. Perth, WA: Murdoch University, 2006.
33. Watts J. Best of Both Worlds: Fly in Fly out Research Project Final Report. Karratha, WA: Pilbara Regional Council, 2004.
34. Guerin P, Guerin B. Social Effects of Fly-in-Fly-out and Drive-in-Drive-out Services for Remote Indigenous Communities. Australian Community Psychologist 2009; 21(2): 7-22.
35. Taylor J, Simmonds J. Family Stress and Coping in the Fly-in Fly-out Workforce. Australian Community Psychologist 2009; 21(2): 23-36.
36. van der Klis M, Karsten L. The commuter family as a geographical adaptive strategy for the work-family balance. Community, Work and Family 2009; 12(3): 339-354.
37. Pirotta J. An Exploration of the Experiences of Women Who FIFO. Australian Community Psychologist 2009; 21(2): 37-51.
38. Garnett ST, Coe K, Golebiowska K, Walsh H, Zander K, Guthridge S et al. Attracting and Keeping Nursing Professionals in an Environment of Chronic Labour Shortage: A Study of Mobility among Nurses and Midwives in the Northern Territory of Australia. Darwin: Charles Darwin University Press, 2008.
39. Taylor A. Current evidence of 'female flight' from remote Northern Territory Aboriginal communities - demographic and policy implications. Migration Letters 2011; 8(2): 77-88.
40. Carson D, McConnel F. Indigenous health and community services employment in remote Northern Territory: a baseline examination of 2006 and 2001 Census data. Australian Journal of Rural Health 2011; 19: 255-258.

