Barriers to health care in rural Appalachia
The Appalachian region of Southwest Virginia is known for its scenic landscape, and its poor quality of health. The region of interest consists of six Virginia counties: Lee, Scott, Wise, Dickenson, Russell, and Washington. These counties are all located near the border of Virginia, Tennessee, and Kentucky. In general, Southwest Virginia can be characterized in terms of increased prevalence of chronic disease, lower income compared to the rest of the state, a lack of sufficient insurance coverage, and limited access to healthcare services1. Initiatives such as telemedicine have increased the availability of health care in remote areas; however, availability does not guarantee access2. To effectively treat those living in Appalachia, physicians and researchers must understand the various determinants of health status of those living in this region. Due to the Appalachian terrain, people are physically isolated from others, and from general and specialty healthcare services. Many residents cannot afford a car, and transportation concerns make it less likely they will seek medical attention3. Additionally, environmental risk factors make areas of Appalachia a hazardous place to live or work. Cancer clusters have been identified in Appalachia, and although residents may understand the elevated risk of living in those regions, many choose to stay because of their job and family ties4. Many Appalachians are also socially isolated from others due to geographic barriers. Isolation has been associated with a higher incidence of depression, with 33% of individuals reporting feeling depressed or having a depressed family member in their household1.
In a survey of 922 households, 80% reported members of their household were uninsured1. Those fortunate enough to have physical access to healthcare services may not have enough coverage to afford medical attention. The combined effect of limited insurance coverage and limited healthcare access causes this population to be primarily medically underserved, increasing their risk for chronic disease and premature death. In 2007, the Graduate Medical Education Consortium (GMEC) presented a study of population health over an area consisting of 13 counties and three cities in Southwest Virginia. The report revealed that the age-adjusted death rate is 18% higher in Southwest Virginia than in the rest of the state. According to data from the Virginia Health Statistics, people in Southwest Virginia were 30% more likely to die from diabetes, 44% more likely to die from lung disease, and over 50% more likely to die from liver disease, unintentional injury, or suicide5. A separate survey of 922 households reported diseases such as hypertension (47%), arthritis (41%), obesity (41%), and diabetes (21%) as major health concerns. The incidence of hypertension and diabetes is three times greater in this region than the rest of the state1.
Remote Area Medical
To meet some of the needs of this population, The Health Wagon, a local non-profit healthcare provider, contacted the Remote Area Medical (RAM) organization for help in 1999. RAM, a non-profit, volunteer-based organization, works to provide free medical, dental, and vision services to medically underserved areas of the USA and abroad (http://www.ramusa.org). All medical supplies, medication, facilities, and medical services are provided through charitable donations and volunteer service. This collaboration allows care to be brought to people living in rural areas with geographic isolation and limited access to care. The first RAM event in Wise County was held in 2000, and by 2005 the RAM Wise event had grown to 6400 patient encounters in 36 hours. Of those 6400 encounters, 59% were for medical services6. Despite the enormous amount of care provided, patients were still turned away due to the time constraints, a limited amount of medical resources, and variable availability of the volunteer healthcare providers.
In a survey conducted by Barish and Snyder7, a random sample of 125 RAM patients were questioned about their health and economic status. The results revealed that only 44% of patients surveyed have at least a high school diploma, and 75% of those interviewed are unemployed. Additionally, 62% of patients reported being uninsured, and most of those insured have public healthcare coverage through Medicare or Medicaid. In this survey, 46% of patients reported having a chronic health problem that needs continual treatment. However, patients must travel approximately 16 km (10 mi) on average (with an upwards range of 112 km (70 mi)) to the nearest healthcare provider, many times through mountainous or rough terrain.
The objective of this study was to gain insight into the number and needs of potential patients served at the yearly 3-day RAM Wise clinic by creating a dataset from the medical records of those patients seen at the clinic over a 3-year period that data was available, and recording pertinent medical information. This information, along with qualitative recommendations by RAM volunteers, provides suggestions for RAM and other similar clinics to treat patients with higher quality and greater efficiency.
The data were collected in Wise, Virginia, a small town located in the mountains of rural Virginia near the Kentucky and Tennessee state border. The dataset was compiled from 2834 medical records of patients seen at the RAM Wise Clinic in July 2006, 2007, and 2008. Only patients with physically accessible charts were included in this study. Data were manually recorded from paper records, which include basic population demographics, previous medical history, family history, new diagnoses made at RAM, services provided at RAM, and laboratory results. A complete list of recorded metrics can be found in Table 1.
Data from each year were analyzed separately, and then compared and averaged across the 3-year period. Patients were excluded if they were electronically registered for the RAM clinic through the University of Virginia medical record system but did not receive any medical services. Duplicate patient encounters from the same year were consolidated into a single patient record. However, duplicate patients seen at RAM in different years were kept as separate patient encounters. In accordance with Institutional Review Board (IRB) regulations, each patient was assigned a unique study number to ensure patient anonymity. Since diabetes, hypertension, and obesity were three of the most prevalent diseases in the area, the data pertaining to these diseases from RAM 2008 were analyzed in-depth.
The complete dataset was used to develop an accurate view of the patient population served at the RAM clinic. The recommendations for improving clinical operations were formulated based upon existing clinical practices, an informal survey of RAM volunteers, and the quantitative analysis previously discussed. The informal survey consisted of 10 free response questions asking participants to identify their roles at the clinic, clinical processes and logistics that were successful, and things that could be improved upon in the future.
Ethics approval
The University of Virginia Institutional Health Sciences Review Board reviewed and approved this research; ethics approval number IRB-HSR 13756.
Table 1: Data collected from patients at Remote Area Medical, 2006-2008 (n=2834)?
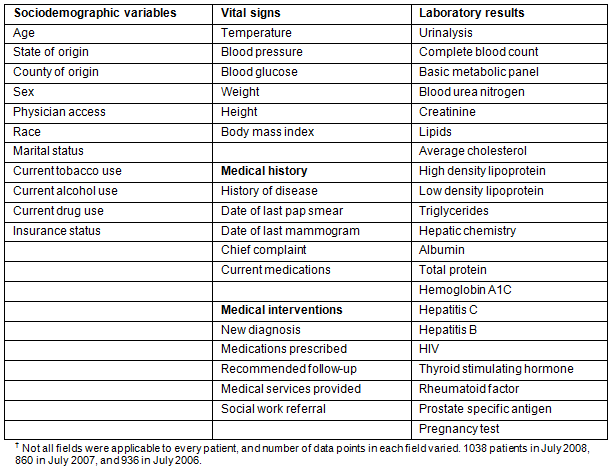
Most people served by the RAM Clinic are from Virginia (84.3%), Tennessee (10.6%) or Kentucky (2.8%), with the largest representation from Wise County, Virginia. Although a majority of patients are residents of Virginia, patients came from all over the Appalachian region, and from states as far as New York and Florida. A basic description of the patient population seen at the RAM clinic from 2006 to 2008 can be found in Table 2.
The data in Table 3 summarizes the types of services provided at RAM from 2006 to 2008, with a focus on medical services. Variation in number of reported services is due to variation in funding, resources, and volunteers available each year for the specific services. Patient and family histories were acquired for most patients (some charts were incomplete) seen in medical triage, and are shown in Figure 1. The most common ailments patients reported were arthritis, hypertension, asthma, diabetes, and heart problems. Patients were also asked to self-report their insurance status. Of the 727 patients who reported an insurance status in 2008, 62% were uninsured, 16% used Medicare, 14% used Medicaid, 7% had private or employer provided insurance, and 1% had veteran's benefits.
The blood pressure measurements taken at the RAM clinic in 2008 are shown in Figure 2. Of those who reported having hypertension and are currently on medication, 62% had blood pressure values greater than 130/85 mmHg. Approximately 40% of those patients with hypertension complained of needing refills on their blood pressure medications. In 2008, 5.3% of patients seen by a physician at RAM were newly diagnosed with hypertension.
In 2008, 25.6% of blood glucose readings at RAM were greater than normal. According to the Mayo Clinic, in a random blood glucose test, values between 3.89 and 7.78 mmol/L (70 and 140 mg/dL) are considered normal, and a value greater than 11.11 mmol/L (200 mg/dL) suggests diabetes8. Of the patients seen, 3.7% of patients were diagnosed as new diabetics, and 19% of known diabetic patients required major adjustments to their medication to better control their blood sugar. Haemoglobin A1C (HbA1c) was used to quantify long-term diabetes management. The results in Figure 3 show that 52% of patients tested had a HbA1c level greater than 7%, indicating the patient is not managing his or her diabetes well8. The positive correlation between a random blood glucose test and high HbA1c values show that those with poorly managed diabetes presented with higher glucose levels. The variance in blood glucose levels and HbA1c values as shown by the red variance bars is also an indication of diabetes management. Those patients with well-controlled diabetes had less variance in their blood glucose and HbA1c values as compared to those with poorly controlled diabetes. Diabetic patients also had a high incidence of comorbidities: 71% of diabetic patients were also obese, and 64% reported having hypertension. Of the total sample, 74% of patients were either overweight or obese on average.
The average number of patients who reported using tobacco was investigated in-depth. The total sample size was 2165 patients: 755 in 2008, 628 in 2007, and 782 in 2006. Tobacco products include cigarettes, cigars, and forms of smokeless tobacco. On average, 48 ± 2.5% of the total sample size reported using tobacco products on a regular basis. Compared to the total sample size, 13% of patients used half a pack or less daily, 23% used one pack per day, and 9% consumed greater than one pack per day.
The results of the qualitative survey included suggestions for improvements to the RAM clinic in the future. Out of approximately 200 volunteers, 36 surveys were completed from RAM 2008. Out of the 36 respondents, 17 are nurses or nursing students, 5 are physicians or medical students, 2 are social workers, and 12 served as general volunteers. The respondents highlighted several different problems, the most pervasive (having more than one respondent) being poor availability of glucometers and test strips, patients and charts being lost or misplaced, long wait times for patients, and unavailability of lab results.
Table 2: Demographic information collected from Remote Area Medical patient records (body mass index
measured and calculated according to guidelines from the Center for Disease Control and Prevention9)
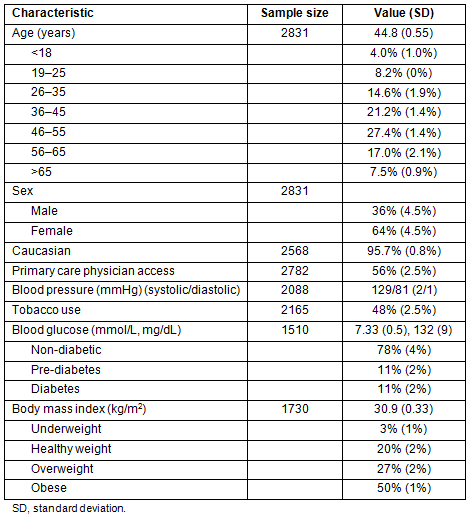
Table 3: Remote Area Medical data compiled from the dataset
and reported from the University of Virginia Health System?
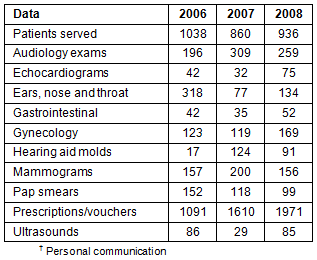
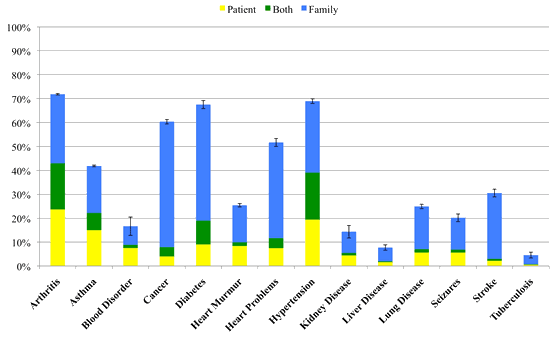
Figure 1: Average number of patients with a history of various health conditions
(n=2081; 727 patients in 2008, 604 patients in 2007, and 750 patients in 2006).
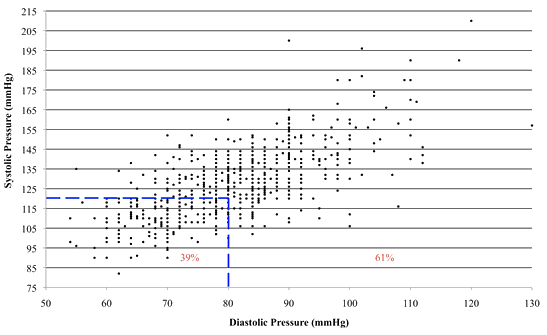
Figure 2: Scatter plot of all blood pressure measurements at Remote Area Medical 2008 clinic
(n=737) (average: 128/81 ± 17/11; median: 128/80; range: 82/62-210/120; dotted lines
indicate the recommended normal blood pressure according to the National Institutes of Health of 120/8010).
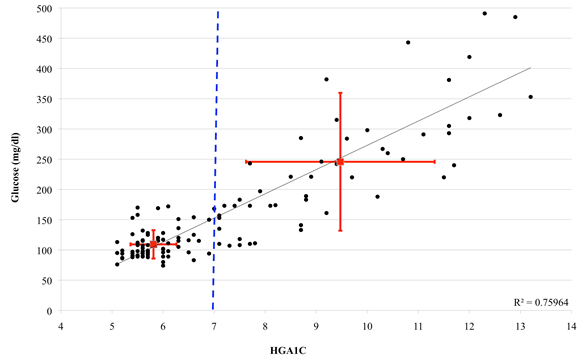
Figure 3: Scatter plot of correlated HgA1C values and blood glucose from the Remote Area
Medical 2008 clinic (n=120) (target HgA1C value <7%, indicating adequate glucose control8;
average 7.3±1.62%; median 6.3%; range 5.1-13.2%). 1 mg/dL = 0.056 667 mmol/L.
Discussion
The RAM clinic was established to provide screenings and basic medical, dental, and vision services for uninsured or underinsured people in Appalachia. One of the primary goals of the clinic is to refer patients into long-term, sustainable medical care. Services provided at RAM Wise depended upon availability of practitioners, equipment, supplies, and donations. Providers have no way of assessing in advance the patients' potential needs, or how many patients may come for medical care. Consequently, there is no identified intrinsic, quantitative factor causing the fluctuation of the various services provided. Outside factors such as more local screenings and incomplete records may have lowered patient encounters for some years, whereas better organization and more staff may have caused an increase in provided services. Although the clinic is advertized as a free clinic patients may have a fear of still being billed. Anecdotal evidence from volunteers and providers reported several patient charts being discovered in bins and portable bathroom commodes. This study reports that 93% of patients seen at the RAM clinic are uninsured or have government-provided health insurance. This is most likely because most of the working class in this region cannot afford to purchase coverage. In 2008, the average per capita income for Southwest Virginia was $28,17611. With the cost of health insurance approximately 28% of the average yearly income per person, it is not surprising that many either cannot afford private insurance, or choose not to purchase it.
The prevalence of disease reported at the RAM clinic is significantly greater than state and regional averages1,12. Considering approximately 90% of patients at the clinic are working-age adults (18-65 years), they should have a lower incidence of chronic health problems than the reported findings. The higher prevalence and poor management of chronic diseases may be due to infrequent doctor visits and an inability to afford the prescribed medication. In 2007, 25.2% of all Virginians were considered obese (body mass index >30), whereas at the RAM clinic the rate was nearly twice the state average. The high obesity rate is most likely the largest contributor to the high prevalence of hypertension, diabetes, and heart problems in the region. The diabetes rate is over twice the Virginia average, with 1 out of 13 Virginians and 1 out of 5 RAM patients reporting a personal history of diabetes. The Virginia state average prevalence of hypertension in 2008 was 27%12, compared to 39% of RAM patients. The increased prevalence in the Appalachian region may be due to tobacco use, high obesity rates, and limited access to primary care due to the rurality of the region to help patients manage and treat their hypertension. Tobacco use is also a major health concern in the Appalachian regions. The data showed that almost 50% of patients interviewed use tobacco products regularly. There is little variation in this data, signifying that the number of tobacco users has not significantly decreased between 2006 and 2008. The average rate of adult tobacco use in Virginia from 2006 to 2008 is 18.1%12. Tobacco use is linked to an increased risk of several types of cancer, coronary heart disease, stroke, peripheral vascular disease, abdominal aneurysms, and chronic obstructive pulmonary disease13.
Limitations
Although only 2834 patients were included in this study, 3284 patients were registered through the RAM medical record system over 3 years. Some patients were documented through the registration database, but their medical charts could not be located. This discrepancy is most likely due to lost charts, patients leaving the clinic with their medical chart, or patients becoming impatient and leaving because they spent so much time waiting in line. Additionally, there are variations in the sample size due to incomplete charts and inconsistent documentation due to the nature of the clinic, being volunteer-staffed with very limited orientation. Another major problem was patients leaving before all recommended screenings and medical visits were conducted. Ineffective communication between doctors and exit nurses caused patients to leave prematurely, and several patients would get lost traveling between different areas of the clinic. Most of the patients at this temporary clinic were first-time visitors and were unfamiliar with the logistics of receiving care. Surprisingly, there was minimal patient redundancy in subsequent years, with only approximately 12% of patients who had been treated at the RAM clinic at least twice over the 3-year period.
As in any study, there are certain inherent biases present in this study design that may affect the validity and generalizability of the results. The study sample was a convenience sample of patients seen at this episodic clinic, not a random sample of people living in this region. This makes the data valid when describing characteristics of patients who seek free care in this region; however, it is not necessarily generalizable to the entire population of Southwest Virginia. Also, those seeking care at a free clinic are likely to perceive a need of medical care, which would overestimate the prevalence of disease if generalizing the data to the population in the entire region. There is also the potential for information bias since data about medical history and health behaviors was self-reported and not observed or quantitatively documented.
Recommendations implemented at subsequent rural clinics
Although these recommendations are based on a single clinic operation over three consecutive years, many of these recommendations could be extended for other clinicians planning similar outreach clinics in rural areas. To counter logistical problems and resistance to patient flow through the clinic, it was suggested that mini medical clinics be placed at the vision and dental sites to treat patients with high blood pressure or high blood glucose at these satellite locations so patients would not lose their spot in line, and could obtain treatment faster. Several patients receiving services at areas other than the primary medical area were not properly interviewed or registered. By registering all the patients and conducting thorough medical interviews, medical volunteers in subsequent years were better able to screen and treat patients for undiagnosed conditions, and also provide local, long-term, healthcare options in the area for continual treatment.
Due to a long waiting period between obtaining blood samples and communicating lab results to the patient and his or her physician, bedside HbA1c tests were implemented in 2009 to help clinicians working with diabetic patients, offering instant feedback about how well they are managing their diabetes. This allowed physicians to properly counsel patients and adjust any medications as needed. Finally, in 2010, an exit review was added at patient discharge, which decreased the number of patients that left the clinic prematurely. To reduce loss to follow-up from lost medical records, patients are not allowed to carry their medical records, and are escorted between clinic areas by general volunteers or providers. Based upon feedback from previous patient exit surveys, in 2011 a 'medical only' entrance was implemented to streamline patients that did not require dental or vision services, and would spare chronically ill patients from waiting for several hours in extreme weather conditions.
The results of 3-year comparisons of data from this yearly episodic clinic have shown an increase in the incidence of disease in Appalachia compared to state and regional averages1,12. Conditions such as obesity, heart and vascular disease, diabetes, and arthritis plague the area and are now a focus for the medical team. The RAM clinic seeks to provide medical aid to this underserved region, but many patients are unable to receive care due to the limited capacity of the clinic. However, increasing patient and physician awareness of available services, improving throughput to decrease the wait time, and improving medical record keeping can increase the efficiency of the clinic and quality of patient care.
The discussed results reflect an accurate summary of patients served at the annual RAM clinic weekend event in Wise, Virginia over a 3-year period. These results provide novel insight into a largely uninsured population of Americans seeking health care at a free clinic. Furthermore, it provided recommendations for RAM medical clinic coordinators and for other healthcare providers attempting to organize or serve a similar patient population. With data about the number and type of diseased patients, both RAM volunteers and permanent healthcare providers can anticipate the amount of medical supplies, prescriptions, specialty medical staff, educators and other resources needed to serve the area. The presented analysis could also facilitate collaboration between policy-makers and local healthcare providers to target funding to the areas with the greatest need.
Rural outreach clinics such as the RAM clinic are not a solution to the health crisis felt by Americans living in rural, isolated parts of the county. They are a non-sustainable, temporary solution to a deep-seated medical, political, and cultural issue. A report from the US Census Bureau stated that in 2011, over 48 million American people were uninsured14. In Virginia, the unemployment rate doubled from 3.5% to 6.6% from February of 2008 to 2009, and still remains high at 5.7% as of October 201215. As a consequence of increased unemployment, millions of Americans have lost their health insurance. The demands on free clinics and health outreach events similar to RAM will increase, making it essential that these clinics perform optimally and at maximum capacity.
References
1. Huttlinger K, Schaller-Ayers J, Lawson T. Health care in Appalachia: a population-based approach. Public Health Nursing 2004; 21(2): 103-110.
2. Morgan A. A national call to action: CDC's 2001 urban and rural health chartbook. Journal of Rural Health 2002; 18(3): 382-383.
3. Gesker W, Sherman J, Spencer J, Preisser J, Arcury T, Perin J. Exploring inequalities in health care coverage by degree of rurality in western North Carolina. Southeastern Geographer 2006; 46(1): 97-120.
4. Behringer B, Friedell GH. Appalachia: where place matters in health. Preventing Chronic Disease (Online) 2006. Available: http://www.cdc.gov/pcd/issues/2006/oct/06_0067.htm (Accessed December 2012).
5. Southwest Virginia Graduate Medical Consortium. Report to the General Assembly, January 2007. Available by request: http://gmec.uvawise.edu (Accessed December 2012).
6. Merwin E, Snyder A, Katz E. Differential access to quality rural healthcare: Professional and policy challenges. Family Community Health 2006; 29(3): 186-194.
7. Barish R, Snyder A. Use of complementary and alternative healthcare practices among persons served by a remote area medical clinic. Community Health 2008; 31(1): 221-227.
8. Mayo Clinic. Diabetes: tests and diagnosis. (Online) 2012. Available: http://www.mayoclinic.com/health/diabetes/DS01121/DSECTION=tests-and-diagnosis (Accessed December 2012).
9. Center for Disease Control. Defining overweight and obesity. (Online) 2012. Available: http://www.cdc.gov/nccdphp/dnpa/obesity/defining.htm (Accessed December 2012).
10. US Bureau of Economic Analysis. CA1-3: personal income summary by county. (Online) 2012. Washington, DC. Available: http://www.bea.gov/iTable/iTable.cfm?ReqID=70&step=1 (Accessed December 2012).
11. Centers for Disease Control. Prevalence and data trends Virginia - 2007. (Online) 2012. Available: http://apps.nccd.cdc.gov/brfss/page.asp?yr=2007&state=VA&cat=TU#TU (Accessed December 2012).
12. Centers for Disease Control. Smoking and tobacco use fast facts. (Online) 2012. Available: http://www.cdc.gov/tobacco/data_statistics/fact_sheets/fast_facts/index.htm (Accessed December 2012).
13. United States Census Bureau. Table HIB-4. Health insurance coverage status and type of coverage by state all people: 1999 to 2011. (Online) 2012. Available: http://www.census.gov/hhes/www/cpstables/032012/health/toc.htm (Accessed December 2012).
14. United States Department of Labor. Over-the-year change in unemployment rates for states. (Online) 2012. Available: http://www.bls.gov/web/laumstch.htm (Accessed December 2012).
15. National Institutes of Health. 2012. High Blood Pressure. Bethesda, MD. Available: http://www.nhlbi.nih.gov/health/dci/Diseases/Hbp/HBP_WhatIs.html. (Accessed December 2012).
