There is an acknowledged shortage of rural doctors in Australia1. It is also evident that, worldwide, fewer graduates are selecting a general practice career than formerly. Allen indicates that only 26% of British medical graduates wanted to enter general practice in the early 1990s, compared with 46% a decade earlier2. In Australia, work with a South Australian intern cohort showed a correspondingly low figure, with a little over 20%, of interns interested in a general practice career3. Goldacre also indicated that where training opportunities in a hospital specialty were limited, doctors were more inclined than in the past to select an alternative specialty to general practice4.
Both Kamien5 and Field6 have indicated that one factor in solving the rural medical workforce shortage is to foster the interest of medical students in a rural medical career by providing greater exposure to rural medicine.
In Australia, undergraduate medical education is the province of the university system, and vocational training the province of the medical colleges. In between these two systems, junior doctors work as medical officers in the public hospital system. There have been a considerable number of Commonwealth government initiatives at the undergraduate level to interest students in a career in rural medicine7. Likewise, significant Commonwealth funds have been applied to encouraging registrars to undertake training in rural locations8. Between these two points there has been a notable gap in the recruitment of rural doctors at the junior doctor level, there being limited opportunities for junior doctors to undertake rural community rotations at that stage of their training.
The Rural and Remote Area Placement Program (RRAPP), funded by the Commonwealth Department of Health and Ageing, was established in April 2000, as a national pilot program, built on the experience of an intern training initiative at Cleve in South Australia9 and a resident placement at Albany in Western Australia10. Its principal objective was to provide a high quality and positive training experience in rural community practice for junior doctors in their first 3 years following graduation and prior to their vocational training. The RRAPP has provided a community-based experience at a point where most junior doctors train within the hospital system and has developed an option for rural experience at a point where most junior doctors train in an urban setting.
RRAPP junior doctors moved from an urban or regional public hospital for a term of 10-13 weeks to a private rural practice. Two sites provided an exception to this: being based predominantly in indigenous communities in northern Australia for either 4 or 26 week terms. RRAPP began with three operating sites in Australia, progressing to its current scope of 14 sites, funded for 2004. The program currently uses over 25 training locations and has the capacity to provide up to 70 junior doctors per year with a rural community training experience. Within these training locations there are a number of different models in terms of service delivery and scope of practice. The range includes procedural medicine, working with doctors who have visiting medical officer (VMO) rights to their local hospitals, Aboriginal health care in remote communities, experience with the Royal Flying Doctor Service and experience with highly qualified rural doctors of both genders providing a range of services in women's health, paediatrics and population health.
For simplicity, the term rural community practice is used to describe the RRAPP experience. While technically delivered mainly in the general practice/primary care setting, the RRAPP experience contains a broader and deeper range of practice, including secondary care, remote medicine and aboriginal health, associated with meeting the extended needs of rural and remote communities, also involving procedural medicine in practice and hospital settings and practising at some distance from broad specialist support. The additional and different aspects of rural medicine, as contrasted with basic urban general practice are inherent to RRAPP, making it a relevant experience for junior doctors destined for all vocational disciplines.
This study examined the influence of RRAPP experience on junior doctors' decisions about subsequent training and careers.
Methods
Design
Data for this study was collected as part of the internal evaluation of RRAPP, developed in collaboration with the Department of Health and Ageing. The National Advisory Committee of the RRAPP, consisting of representatives of the Australian College of Rural and Remote Medicine, the Rural Doctors Association of Australia, the Royal Australian College of General Practitioners, the Confederation of Post-Graduate Medical Education Councils, the Committee of Presidents of Medical Colleges, and the Department of Health and Ageing, acted as an Advisory Group, providing input to the direction of investigations and critique of interim results.
Data collection instruments: De-identified questionnaires were routinely administered to all RRAPP junior doctors (n = 107) at the close of their training terms, to October 2003. In terms of confidentiality and ethical practice with data management and analysis, the University of Queensland ethical guidelines were followed. Each questionnaire covered perceived effectiveness of training, major outcomes and priority issues. The questionnaire responses were analysed using SPSS; data entry and primary analysis were undertaken by a project administrator.
In addition, a series of structured interviews, using a common question template, was administered by telephone to 54 RRAPP junior doctors who were representative of the cohort in terms of gender, training year and location. The interview themes covered background, impressions of training and future plans. These interviews were conducted by one investigator, taped and transcribed by other personnel. Each transcript was returned to the contributor for validation and/or amendment. The interview transcripts were analysed using text analysis techniques for emerging themes. The Program Manager and Research Officer analysed 50% of the interview material each using a common methodology, and nominated 25% of this material to be analysed jointly to check the reliability of the analysis. Issues emerging from the data analysis were routinely fed back to participants for comment and review in order to minimise researcher bias.
This feedback loop was also necessary to ensure the accuracy of recollection and recording with the participant-observer methodology used in the fieldwork. Visits of at least 2 days' duration were made to training practices, feeder hospitals and fundholders, and interviews with administration and training personnel and RRAPP doctors in the training setting were undertaken. Observations were made of the training setting and of the support provision in terms of education, linkage with the peer group at the hospital, technology provided and accommodation.
Further methodological issues
There were several further issues considered by the authors when designing this study. The participant-observer design introduced the possibility of bias. This was mitigated by the use of an external reference group, triangulation of data from multiple sources, the use of a strict study protocol, and feedback on the data and analysis from the junior doctors at multiple points during the study. The study was retrospective and no pre-intervention data collection was possible. Due to the timing of the interviews close to the completion of the attachments, the main plans outlined by junior doctors were expressed as career intentions, rather than actual practice locations/choices. Studies of career intent at this post-graduate stage have, however, shown good correlation with eventual practice location4. While it would have been helpful to the findings to be able to make comparisons between the RRAPP cohort and the general junior doctor population at the feeder hospitals, this was not possible within the design of this study owing to a directive from the fundholder who limited the enquiry to RRAPP doctors only. The ability to compare both status and the process of choice between the two groups is recognised as a potential asset to studies of this type.
Results
The results are based on a 98% response to the evaluation survey enabled by the voluntary nature of participation in both the training and the responding evaluation by RRAPP junior doctors. This high response rate strengthens the overall picture developed by the data and compensates, in part, for the relatively small number of junior doctors (n = 107) involved in the study at the time of publication.
Aspects of decision-making
In results of the questionnaire, over 70% (n = 75) of junior doctors felt that RRAPP had played a role in their training and career choice. This was reflected in a number of ways (n = 106):
- Changing or confirming choices by being impressed by the range of work, its organisation and autonomy (27.4%).
- Confirming an already established preference for community/general practice and/or rural practice (24.5%).
- Providing time to reflect and decide that a specialty career and/or a hospital based career was the appropriate choice (18.9%).
- Having the time to reflect on, and assess, workload and type of work at a key decision-point of training (16.0%).
- Having the opportunity to experience and assess issues of lifestyle and levels of satisfaction (13.2%).
Training plans
The study also examined the role of RRAPP in providing a stepping-stone to other forms of training. The cohort surveyed to October 2003 intended to enrol, or had enrolled to train in a number of generalist and specialty disciples of which general practice was the most frequent choice and physician training, emergency medicine, anaesthetics and surgery and were the most prevalent alternative specialties.
The group showed a strong inclination to continue training in a rural location. Almost 60% (n = 64) of respondents who were certain of their ongoing training location forecast a training location that inferred a regional or rural component to this training in the coming phase. Over 45% (n = 25) of those electing for general practice as a first choice, specified rural practice.
RRAPP doctors expected their training choices to lead to a range of career pathways (Table 1).
Table 1: Expected career pathway of RRAPP doctors (n = 107)
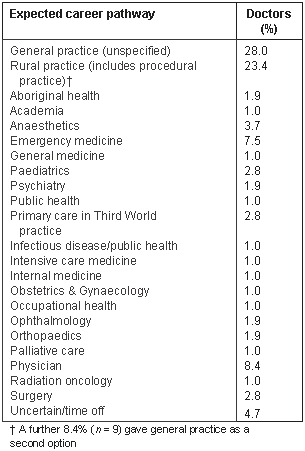
Rural choice
The majority of RRAPP doctors (90%), whether choosing generalist or specialist tracks would have liked further experience in rural areas. The issues (n = 177) that were most influential in junior doctors' continued interest in rural practice were:
- Diversity, breadth and autonomy of practice; interest and challenge (39%)
- Lifestyle, beauty and pace of life for self and family (24.3%)
- Duality of roles in practice, hospital and community (20.3%)
- Being appreciated, known and valued and having less stress than in the hospital environment (11.9%)
- The opportunities for good income base, especially with access to procedural medicine (4.5%).
A small proportion of RRAPP doctors (6.5%, n = 7) identified some barriers to training (n = 32) or working in rural practice. Many of these were embarking on a specialty or subspecialty pathway or had partners in training or in urban-based lines of employment. The issues raised by these doctors were:
- Partner's training and work requirements limited the doctor's choice (25%)
- Lack of capacity to step away from the medical role (lifestyle, privacy, anonymity) (25%)
- Perceived lack of professional support facilities (21.9%)
- Factors of isolation or separation from family (18.8%)
- Specialty choice limits the capacity to work in a rural area (9.3%).
Choosing vocational training and career
The junior doctors in RRAPP indicated their lack of sympathy with an inflexible training system. This was characterized by their comments on the lack of junior doctor input into choice with regard to how training terms were designed and structured, the hierarchical structures of work that routinely delegate lesser roles to junior staff, and the perceived resistance to change of the well-established 'rites of passage' in the hospital for interns and junior doctors. A further lack of flexibility in some cases is perceived in difficulties for junior doctors in taking time away from study and having a smooth re-entry into training after a period of 1 or 2 years. The 107 RRAPP doctors expressed strong multifaceted views providing a total of 376 separate issues on the importance of building a quality lifestyle (20.2%) and a challenging and interesting career (49.2%). Included in RRAPP doctors' definitions of these items were:
- Flexibility and portability of options and the ability to change tracks
- A sense of challenge and stimulation in serving a community
- Good access to support, training and upskilling opportunities
- Selecting viable, commercially sound practices for a sustainable income.
- Flexibility of hours and capacity for part time work.
- Employment available in practice or community for partner.
Factors in the determination of a career path also emerged from the process of reflection and consultation with rural doctor mentors as outlined below. The role of the rural generalist as teacher provided another layer of influence on the junior doctors to supplement that of their hospital based consultants. RRAPP training practices are carefully selected and well supported. Excellence in teaching is closely monitored. There are benefits in the view of RRAPP doctors and their rural supervisors, in providing an alternative teaching setting and teaching personnel to that normally available at this stage of training. Rural doctors appreciate the opportunity to demonstrate that teaching within the community can maintain an equally high quality to that delivered in hospitals. By tracking the ratings of effectiveness provided by RRAPP doctors, it is clear that these teaching settings are highly effective. Issues often emerging from the exit interview data indicated that junior doctors considered that RRAPP had enabled them to:
- Confirm or discover a leaning towards holistic, community-based practice and the particular relationships with patients, leading to a general practice career choice.
- Have a greater opportunity to gain better understanding of the administration/ support factors bearing on a career choice.
- Realize how much their career choices were influenced by positive training experiences, and that a lack of rural practice opportunities resulted a previously unrecognized bias in this process towards hospital specialties.
In terms of their choice of a RRAPP term in the first instance, junior doctors indicated that the three principal factors involved were: (i) peer recommendation; (ii) family/social circumstances; and (iii) prior interest in rural medicine through undergraduate exposure. In addition to this, RRAPP doctors found that their subsequent conversations about their experience with hospital-based peers who had not undertaken a RRAPP rotation were perceived as a positive influence on this wider group of doctors.
Discussion
These data provided evidence that the RRAPP filled a gap in the vertical integration of rural training and provided a valued opportunity for young graduates interested in continuing their involvement with rural medicine. It also provided a testing ground for potential primary healthcare and community-based doctors to explore or confirm a career option outside the specialty and hospital setting.
Influencing choice
The community practice experience, currently absent from the junior doctor terms, was to some extent provided by RRAPP, both directly to successful candidates, and indirectly, through their feedback to peers on their return to the hospital.
An unexpected outcome of the study was the degree to which peer recommendation and positive feedback became the most effective marketing tool for the program. In a setting where general practice was often viewed as the least attractive option, the importance of positive feedback to the junior cohort could not be over-estimated.
In addition, RRAPP provided access for junior doctors to a different type of medical practice, different community options, peer groups and value systems. The sense of being valued by both patients and supervisors, epitomised by the 'my name on my own consulting room' comment, is consistent with relationship-based motivational factors identified in successful undergraduate rural medical education programs11,12. This apparently trivial comment is underpinned by a depth of feeling by young doctors of the importance of attainment of some professional territory at a stage when their identifiable space in the hospital may be a pigeon hole. In addition to their own professional space, junior doctors cite as highly significant the equality of their treatment as a colleague by peers, the professional status afforded them by practice management and reception staff and the opportunity to develop a doctor/patient relationship in a setting that does not immediately label them as a 'junior' member of the profession. Broadening experience and the provision of a positive, challenging and well-supported professional term were the bases of RRAPP's influence on decision-making.
Time for reflection
Decision-making also requires reflection. A number of RRAPP doctors identified the need for both time and space to reflect on their future. The authors noted that, in common with another study13, the change of pace in the RRAPP and change of scene provided junior doctors with the capacity to undertake this process and to consult mentors. RRAPP largely allowed for doctors to confirm prior choices, but it also initiated a change of mind in some, towards rural practice and general practice in most cases, but in four instances the procedural work undertaken in rural practice re-invigorated a love of a particular specialty and provided the incentive for these doctors to pursue a place in specialty training programs (each application was successful).
Changing patterns of career choice
Doctors brought similar priorities to a choice of both training and career. Over 70% of respondents felt that RRAPP had influenced their career choice. The need for a career choice in which the doctor was genuinely interested was a key point emerging from the study. However, many doctors felt that their junior training years provided little time to reflect on the issues that would facilitate this decision-making and little access to objective advice.
If young doctors are to be assisted to make choices that will take them into a long-term and fulfilling vocation, then the influence of early experience on decision-making and choice must be better understood.
Conclusion
This study provided evidence for the positive influence of RRAPP on the perceived career choices of junior doctors. It also revealed further insight into the process of these career decisions.
Decision-making was precipitated by taking junior doctors 'outside their comfort zone' of the tertiary hospital and providing a different perspective on both the present and the future. Hospital care is, by nature, episodic and deals with patients outside their normal environments. One of the tenets of RRAPP was the opportunity to practice holistic care, continuity of care and to experience the full range of opportunities to serve and sustain a rural community. Even in a term as short as 13 weeks, RRAPP doctors report their capacity to see patients through to the resolution of their medical condition, to treat their family members and to become a well-known and much appreciated part of the care of a rural family. This proved a revelation to many RRAPP doctors, affecting their sense of autonomy, relationship with colleagues, personal space and sense of involvement with patients and with rural and community issues.
In addition to the contrast in setting and the expansion of knowledge about rural community practice, RRAPP junior doctors identified the change of place, the change of pace, and the change of status as instrumental in their decision-making about future training and careers.
The affect of providing an alternative setting for junior doctors, in addition to the hospital, appears to be a catalyst for reflection and decision-making. This suggested that our findings may well be transferable to other primary care settings, for instance in urban centres, and this issue should be the subject of further research.
References
1. Australian Medical Association, Rural Doctors Association of Australia. Increasing rural medical services - discussion paper. Canberra: AMA and RDAA, 1998.
2. Allen I. Career preferences of doctors. BMJ 1996; 313 (7048): 2.
3. Laurence C. Potential GPs: characteristics and career aspirations of interns in South Australia. In: Proceedings, National General Practice Education Convention, August 2003. Melbourne, VIC, Australia.
4. Goldacre MJ, Lambert TW. Stability and change in career choices of junior doctors: postal questionnaire surveys of the United Kingdom qualifiers of 1993. Medical Education 2000; 34: 700-707.
5. Kamien M. A comparison of medical student experiences in rural specialty and metropolitan teaching hospital practice. Australian Journal of Rural Health 1996; 4: 151-158.
6. Field J, Kinmonth AL. Learning medicine in the community. BMJ 1995; 310 (6976): 343-344.
7. Norington M. An update on rural general practice education initiative to meet rural workforce needs: progress and recent developments. Australian Journal of Rural Health 1997; 5: 204-208.
8. Thomson J. A framework for the vertical integration of general practice education and training. GPET Discussion Paper. Canberra: GPET, 2002.
9. Mugford B, Martin A. Rural rotations for interns: a demonstration programme in South Australia. Australian Journal of Rural Health 2001; 12 (Suppl 1): S27-31.
10. Vickery AW, Tarala R. Barriers to prevocational placement programs in rural general practice. Medical Journal of Australia 2003; 179: 19-21.
11. Worley P. Relationships: a new way to analyse community-based medical education? (Part 1) Education for Health 2002; 15: 117-128.
12. Worley P. The immediate academic impact on medical students of basing an entire clinical year in rural general practice (PhD thesis). Flinders University, Adelaide, Australia, 2003.
13. Crump WJ, Barnett D, Fricker S. A sense of place: rural training at a regional medical school campus. Journal of Rural Health 2004; 20: 80-84.



