In a developing country like Bangladesh, almost one-third of the population lives below the poverty line. Various diseases are rampant due to lack of clean drinking water and sanitation1. Among the poorest, nearly one-third defecate in the open, making the everyday environment unsafe for children2. According to a World Health Organization (WHO) estimate, 1.5 million children die from diarrheal diseases each year worldwide, with 88% of these deaths occurring due to inadequate sanitation, hygiene, and drinking water3. Access to sanitation facilities alone does not indicate their hygienic use or adoption of other hygienic practices4. Awareness about safe drinking water, sanitary latrines, and of hygiene and related health issues are crucial factors in habituating practice in a particular context5. Hygiene practice becomes difficult in many parts of the world, including Bangladesh, due to lack of safe water and soap6.
Bangladesh has been facing a number of challenges in the water, sanitation, and hygiene sector. Only 26.7% people wash their hands with soap or ashes after defecation7. The main barrier to success of sanitation coverage is lack of awareness about the benefits of a safe latrine. Some other difficulties are poverty, lack of space, and preference for open defecation8. To this end, the government of Bangladesh initiated a program to achieve 100% sanitation by 2013. As a part of this program, the Bangladesh Rural Advancement Committee (BRAC) has been offering comprehensive interventions for water, sanitation, and hygiene (WASH) in rural areas of 150 of 482 upazilas (sub-districts) in the country since 2006. These intervention upazilas have been selected on the basis of criteria such as poor sanitation coverage, high poverty rate and arsenic contamination in the groundwater. The interventions are being carried out in three phases. Each phase covers 50 upazilas for 6 months. The program aims to improve the health and hygiene of the rural poor. The focus is on creation of conditions that will facilitate sustained behavioral change among people7.
The intervention is being offered in communities, religious groups, and educational institutions. To facilitate intervention activities, village WASH committees (VWCs) are formed based on a participatory community process. In order to stimulate bottom-up participation, one VWC consisting of 11 members (six women and five men) from different segments of the community is formed for an average of 200 households. Each VWC assesses local needs through participatory exercises and social mapping and then develops a village WASH plan to improve the overall hygiene situation. Some of the major activities of VWC are to install tubewells and sanitary latrines. Through activities such as health forums, folk songs, street plays, film and video shows, VWCs also help in creating awareness in order to change people's hygiene behavior. They select sites for community water sources, collect money, and monitor usage and maintenance of household latrines. The BRAC program organizers and programm assistants provide continuous support to the VWCs. They visit each VWC, oversee their meetings, and also organize their own meetings to encourage behavioral change among the community. Home visits are frequently made to motivate households to improve their hygiene behavior. During such visits, a demonstration of hand washing is given to members of the household.
Results of previous researches on baseline survey of BRAC WASH indicated a knowledge gap among rural women regarding water contamination, disease occurrence, and its prevention. Less than one-third of the people had access to sanitary latrines9. A midpoint survey of the same households conducted in 2009 after 2 years of WASH intervention indicated significant improvement in sanitation, hand hygiene, and a decrease in the prevalence of waterborne diseases. In order to examine the factors that contributed to this improvement, the authors explored factors that facilitate and/or impede hygiene knowledge and practice. A quantitative assessment of changes in knowledge and practice of hygiene has been carried out by Rabbi and Dey10. The present study utilizes the strength of data collection techniques for qualitative research and brings narrative information through in-depth interviews. The results are enriched through the use of quotes.
Study design and area
A qualitative descriptive study was conducted in 12 villages distributed over six upazilas under the BRAC WASH program. Upazilas were selected from different geographical areas in Bangladesh to capture the diversity in views and experiences. Data were collected from individual households.
Sample and sampling techniques
Each household was classified as ultra-poor (owned less than 404.7 m2 of land, had no fixed source of income or was a female-headed household), poor (had land holdings between 404.7 m2 and 4047 m2 and/or sold manual labour for a living) or non-poor (satisfied neither of the previous categories).
WASH program organizers and WASH managers identified successful and unsuccessful households from each of the three economic groups on the basis of their field experience. Households satisfying the following criteria were considered successful: regular attendance at cluster meetings, knowing and believing the health messages, and practicing them accordingly. Unsuccessful households were those showing irregular attendance at cluster meetings, lack of knowledge regarding health messages, denial to practice some of the messages, and irregular practice of hygienic methods (such as buying soap, ring slab) despite financial affordability. Identified households were validated by visits and interaction in the field.
Upazilas and villages were selected purposively. Two villages were chosen from each of the six upazilas. Two successful and two unsuccessful households from each economic group were selected from each village. Thus, 12 households were selected from each of the 12 villages. In all, 144 households (72 successful and 72 unsuccessful) were purposively selected for the study.
Data collection and quality control
Qualitative data were collected in April-May 2010 using in-depth interviews. Physical verification of the following verifiable indicators was carried out: cleanliness of the latrine; existence of soap, slippers, stored water, and a latrine water pot in or near the latrine; presence of a platform around the tubewell; cleanliness of tubewell surroundings and drinking water storage area at home; and presence of covered water-container.
The interview checklist was pre-tested in the field near the Gazipur district and necessary changes were made to the questionnaire. Enquiries were made with respect to various aspects of safe water use, latrine use, and hand washing. Six trained interviewers with master's degrees in anthropology conducted the in-depth interviews and took notes verbatim in the native language, Bangla. Immediately after the interview, a summary of collected field notes was made and transcribed to get a sense of respondents' knowledge and perceptions about hygiene practices. The principal author (TA) routinely visited the field sites to supervize data collection and ensure a high quality of work.
Data processing and analysis
All narrative data were collected under three pre-determined broad categories: safe water use, sanitation and hand washing. Data were translated from Bangla to English and checked for completeness. Responses were manually sorted into sub-themes such as hygiene indicators, perception of practices, and health-related issues. Moreover, proposed courses of action were identified from the respondents' responses with the assumption that they themselves could best describe their own problems and needs. The implicit meanings of the narrative responses were analysed to identify and understand factors influencing hygiene knowledge and practice. Facilitating and impeding factors were identified and described under some broad categories that emerged from the in-depth interviews (Table 1). Qualitative responses were quantified as frequencies in possible cases.
Ethics approval
Ethical approval for the study was given by the BRAC Research and Evaluation Division. Permission to conduct this research was obtained from the BRAC WASH programme. Informed verbal consent was obtained from each respondent by reading out the consent form and informing the participants of the general purpose of this study. Each respondent was assured that she could withdraw from the interview at any time, and this would not affect her receiving any services from BRAC. Strict confidentiality was maintained in data handling.
Table 1: Checklist of in-depth interview with various sub-themes
under the broad theme of safe water use, sanitation and hand-washing

A wide array of factors emerged from the in-depth interviews. These were grouped into the following broad categories: knowledge and awareness, financial aspects, physical infrastructure and living environment, personal and family aspects, and social recognition (Table 2). Based on responses obtained in the interviews and physical verification of some parameters, factors influencing hygiene-related behavior were categorized into two groups: factors that facilitated good hygiene practices and factors that impeded them.
Table 2: Factors influencing hygiene-related knowledge and practices
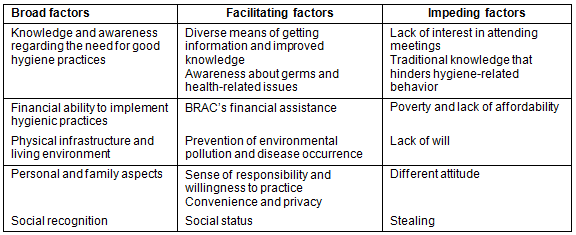
Factors that facilitated improved hygiene behavior
Attendance at motivational cluster meetings leading to improved knowledge: BRAC's frequent cluster meetings, home visits and other interventions such as posters, guidebooks, folk songs and street plays related to health and hygiene were instrumental in improving respondents' knowledge about hygiene-related behavior. A successful ultra-poor respondent who regularly attended motivational cluster meetings stated:
WASH brothers and sisters (ie BRAC staff) taught us during meetings and home visits that using soap for hand washing was safe. They told us to follow hygiene messages showing pictures from the guide book. All family members, including the children, are conscious now.
Awareness about 'germs' and health-related issues: Eighty-three percent of the total respondents from all economic groups were aware of the growth and transmission of 'germs' (the generic name used in this study to refer to pathogenic microorganisms) through unhygienic practices that would ultimately have an adverse effect on health. They believed that the growth and spread of germs could be prevented by keeping the water pitcher in a dry and elevated area rather than a wet place. They were of the opinion that water alone was not sufficient to wash out germs completely but their spread could be prevented if soap was used for washing hands. Some of them mentioned that hygiene practices were beneficial because they would prevent disease occurrence and hence save money in the long term. Poor respondents viewed sickness as a vehicle of wealth erosion of the households. Since they were now more aware than before, the ultra-poor households had the opinion that unsafe water contained dirt and germs and hence they used safe water for various purposes. Using soap specifically for washing hands after defecation was found to be a common practice among the respondents. Those who were irregular in this practice became more aware after they understood the hygiene messages. 'Earlier, people were less conscious and less educated. Though they had money, they did not build latrines. But nowadays people procure latrines even on a loan,' said a non-poor, successful respondent. 'We cannot see germs, so soap should be used to remove doubt. No fear of germs remains in the mind after a hand wash with soap,' said another poor, successful respondent.
BRAC's financial assistance: The poor respondents were motivated through loan support for latrine installation and tubewell platform construction, while latrines were provided free of cost to the ultra-poor respondents. Those who received BRAC's financial assistance believed that such support may have had a positive impact on their behavioral change. Other poor households that did not benefit financially were inspired about hygiene by observing the practices of their neighbors. Latrine ownership especially reduced women's anxieties of sharing a latrine with others or defecating in open places. A successful respondent in the poor economic group stated, 'We were motivated to install latrines looking at other neighbours' practice of safe latrines. Thus, we procured slab latrines from BRAC on credit and installed them. This especially reduced our women's problems of having to defecate in the open or in jungles.'
Prevention of environmental pollution and disease occurrence: According to 67% of total respondents, use of safe latrines prevents contamination of the environment by flies and worms. Excreta of children and adults were perceived to be equally harmful for health and environment. Respondents believed that chickens and ducks may spread germs, if human excreta were left in the open. A non-poor, successful respondent said:
Open defecation is not good for health and the environment. Human wastes may enter the pond and pollute water. People who drink dirty water may become sick or even die.
Sense of responsibility and willingness to practice: Respondents realized that practicing hygiene is necessary for the sake of their own and family members' health. Moreover, informing unaware neighbors about hygiene behavior was believed to be everybody's responsibility. This sentiment triggered procurement and ownership of safe latrines and/or tubewells. Over half of the successful respondents (57%) expressed strong willingness to maintain hygienic behavior despite difficulties in buying soap and carrying water. A successful ultra poor respondent said:
Though we have economic hardships, we buy soap for washing, resulting in improved health. We believe that this is less costly as compared to medicines. If we do not spend Tk. 20 for soap now, how will we be able to afford medicine at the cost of Tk. 500?
A number of non-poor and poor respondents mentioned the difficulties they had in carrying water, though they believed that it had to be done for their own benefit. A successful ultra-poor respondent said:
I had some difficulty in carrying water from others' tubewells. However, I didn't mind because carrying water was better than suffering from diseases due to unhygienic practices.
Convenience and privacy: Respondents were concerned about the lack of privacy during open defecation. A safe latrine with a fence ensured privacy and was considered convenient by the users. The characteristics that made the use of latrines convenient for any time and season were that it could be use easily by children, the latrine was surrounded by a fence, there was no need to publicly carry water and a latrine water pot, and required articles could be stored in or near the latrine.
Social status: Improved social status of households with safe latrines and tubewells could be a factor driving the implementation of hygienic practices. Narratives indicated that ownership of a latrine or tubewell raised social prestige and was a matter of pride for the respondents. Defecating in the open was regarded as awkward but normal in the past but is now considered shameful and risky for health. A successful respondent from the ultra-poor economic group stated:
Defecating in the jungle or open place was the tendency in the past. We felt embarrassed about it, but had no alternatives. Now we feel proud to own a safe latrine, and are ashamed of the old sanitation system.
Factors that impeded improved hygiene behavior
Lack of interest in attending meetings: The poor and ultra-poor households were less interested in attending cluster meetings mainly due to the workload of the household and concerns about leaving children alone at home. Many did not practice hygiene because of busyness and negligence. This lack of awareness about hygiene and health-related issues is evident in some of their statements. According to a poor unsuccessful respondent who could not attend meeting regularly due to household workload said:
I am always in a hurry and never cover my water vessel during transport. I have always collected water from the well and yet have never faced any diseases. I have brought up eight children this way. On the other hand, my daughter's family in Dhaka always uses boiled water but still suffers from diseases.
Traditional knowledge hinders hygiene behavior: Some respondents felt that a metal pitcher is of better quality and is more convenient than a clay pitcher. According to them, a metal pitcher could be kept anywhere on the floor, and it is not necessary to keep it in an elevated place. Some thought that if there is no visible dirt on hands, just water without soap is sufficient for hand washing. Respondents frequently used soap for washing hands after defecation, but not before food handling. There were varied perceptions regarding the use of water from various sources. Some preferred using soap when washing hands with pond water, but not when washing with tubewell water.
Poverty: Poverty was a main factor in lack of ownership of safe latrines, leading to use of shared latrine or defecation in the open. Poverty hindered buying of slippers, soap, brush, and latrine cleaning agents. Poor and ultra-poor households extensively cited poor economic condition as a barrier in practicing hygiene measures, rendering them as unsuccessful households. An unsuccessful participant from the ultra-poor economic group said:
Now we need more soap and water for cleanliness compared to the past. It is difficult to buy extra soap, so we do not have it all the time. We are poor, so it is difficult for us to practice hygiene behavior.
Attitude and lack of willingness to practice: Difficulty in carrying water was perceived by many as the cause of lack of willingness in consistently practicing hygiene behavior, such as hand washing at critical times and sanitation-related practices. Consequently, the respondents were unable to use enough water for latrine cleaning, and hand washing. An unsuccessful ultra-poor respondent stated:
Carrying tubewell water from a distant place was backbreaking. So, we used pond water for washing hands.
Another respondent from an unsuccessful household of the same economic group stated:
Hand washing with soap at all the time was not possible because much water was needed. If we did so, we would have to spend the whole day just carrying water.
A few respondents did not give up old, unhealthy habits in spite of having the financial ability to implement new practices. Thirteen percent of unsuccessful, poor households were not interested in getting a loan for a latrine but wished to procure one free of cost. They expected BRAC to differ the rule of providing free latrines only to the ultra-poor.
Stealing: Fifteen percent of the total respondents reported that children sometimes steal and sell latrine hygiene-related material (eg slippers, water pot) in order to buy sweets or nuts. Such behavior hampers hygienic use of sanitary latrines. However, few respondents reported alternatives such as using lockers in the latrines or keeping material inside the house or near the tubewell.
Discussion
This was a qualitative study exploring factors that facilitate and/or impede hygiene behavior in response to intervention.
The respondents' perceptions on hygiene behavior were found to vary mainly due to psychosocial aspects such as lack of affordability, doubts about germs and related diseases, sense of responsibility, willingness to practice hygiene, interest in attending cluster meetings, and expectations from the organizations (BRAC) for additional support. Successful households did not consider difficulties in buying soap or carrying water as major problems, but tried to practice hygiene for their own and the household's benefit. In another study, variations in hygienic practices between poor and non-poor households were also presumed to be influenced by psychosocial and motivational factors11. Aunger et al. have shown that there is an association between psychosocial factors and hand hygiene practices12.
BRAC's financial help, along with health and hygiene education, were found to be critical in changing hygiene behavior. Arif and Ahmed have reported that financial help from the BRAC WASH program had a positive effect on latrine ownership13. Activities such as motivational cluster meetings, home visits, street plays, and educational activities increased awareness among respondents in WASH intervention areas14. Another study has found that improved knowledge was associated with increased compliance with hygienic practices15. Sustained and accelerated interactive education through varied channels may help the unsuccessful households to practice hygiene.
Improved knowledge and practice of hygiene related to health and the environment can contribute to enhanced general well-being. Increased knowledge and hygienic practices in intervention areas can be attributed to the two-way learning system used in the WASH program, which includes follow-up cluster meetings, home visits, and practical demonstration of some practices. Findings from other studies support these observations. Nath et al. have shown that increased hygiene awareness is associated with increased level of education5. Increased use of safe water for drinking and cooking can also result in reduced disease occurrence16.
Maintaining hygiene behavior for a healthy life was believed to be everybody's responsibility. Such a sense of responsibility developed through motivational cluster meetings may encourage respondents to own latrines. Latrine ownership through BRAC's financial assistance enhanced the privacy and dignity of respondents. Other researchers have also described issues of responsibility and latrine ownership. Hygienic practices were perceived to be an individual's responsibility in a study of rural communities of South Africa17. Convenience, lack of fear, and privacy were also found to be important considerations for latrine ownership among Indian villagers18.
The factors impeding hygienic behavior in the present study were mainly poverty, traditional practices, irregular attendance at cluster meetings, lack of awareness, lack of will, and difficulty in carrying water. Other issues that emerged as causes for not practicing hygiene were preoccupation with day-to-day affairs, forgetfulness, and negligence. The traditional mind-set in rural areas is that all household tasks are the sole responsibility of women. Most men do not help the women with household chores. The resultant workload makes women of the household busy throughout the day, and often keeps them from attending cluster meetings. Consistent with the present study's findings, high workload, forgetfulness, and negligence about using guidelines were also perceived to be reasons of non-compliance among health workers19. Busyness and lack of knowledge have been described as barriers to following safe hygiene practices20. Disagreement with hygiene guidelines of the program was recognized as an influencing factor for not following recommended practices21.
Most respondents stated that some people could not give up their old habit of defecating in the open. Men often chose to defecate in the open, since women got priority for using the available latrine. Likewise, men working in farms mostly preferred to defecate in nearby fields rather than coming home to use the latrine. In addition to open defecation, not keeping designated slippers for the latrine and using the same slippers in the living area revealed a lack of affordability and will. Most respondents used soap in hand washing after defecation but not during food handling. The reasons for this could be economic, as most respondents could afford just one soap, which was kept in or near the latrine or tubewell and not in the house. Low income and water scarcity adversely influence adoption of hygienic practices. On the other hand, ownership of latrine or tubewell and regular adequate water supply motivate the adoption of hygienic practices15.
Some hygiene practices were believed to be more important than others, as evidenced by hand washing with soap after defecation but not before food handling. Transformation of hygiene-related knowledge into practice and practice into habit is hampered by some factors: lack of interest in attending cluster meetings, traditional knowledge, poverty and lack of willingness to practice. In spite of this, there was an improvement in knowledge retention and practice of hygiene in most cases. Frequent cluster meetings and home visits could be a promising approach for creating awareness and encouraging unsuccessful households to adopt hygienic habits. This approach will help them to remain in a continuous learning process and to practice hygiene regardless of poverty and other barriers.
Acknowledgements
The authors acknowledge all the respondents who gave valuable information and time for this study. They thank all the interviewers involved in data collection and field staff of the BRAC WASH program for their assistance in conducting this study. They wish to thank to Data Management Unit of Research and Evaluation Division (RED) for their support in data entering and cleaning, the Knowledge Management Unit of RED for reviewing the report, and the Nextgenediting Global Initiative for editorial assistance. Finally, they acknowledge the Government of Royal Netherlands for funding the WASH program.
References
1. Amin MR, Ahmed W, Kashem M. The status of safe drinking water and sanitation in Batabaria, Comilla, Bangladesh. Annals of Tropical Medicine and Public Health 2008; 1: 47-51.
2. UNICEF. Rural sanitation, hygiene and water supply. (Online) 2008. Available: http://www.unicef.org/bangladesh/RURAL_Water_Sanitation_and_Hygiene.pdf (Accessed 7 September 2011).
3. Lipson J. The public health benefits of sanitation interventions. EPAR Brief No. 104. University of Washington: Evans School of Public Affairs, 2010.
4. Samanta BB, WijkCAvan. Criteria for successful sanitation programmes in low income countries. Health Policy and Planning 1998; 13(1): 78-86.
5. Nath KJ, Chowdhury B, Sengupta A. Study on perception and practice of hygiene and impact on health in India. In: Proceedings of South Asia Hygiene Practitioners' Workshop, 1-4 February, Dhaka, Bangladesh. (Online) 2010. Available: http://www.ircwash.org/resources/study-perception-and-practice-hygiene-and-impact-health-india-paper-presented-south-asia (Accessed 10 July 2010).
6. Centers for Disease Control. Global WASH-related diseases and contaminants. (Online). 2010. Available: http://www.cdc.gov/healthywater/wash_diseases.html (Accessed 11 March 2011).
7. Kabir B, Barua MK, Karim R, Bodiuzzaman M, Rahman M, Mia HA. Contributions of village WASH committee in breaking the cycle of unhygienic behaviours in rural Bangladesh. In: Proceedings of South Asia Hygiene Practitioners' Workshop, 1-44 February, Dhaka, Bangladesh. (Online) 2010. Available: http://www.wsscc.org/sites/default/files/publications/9_barbarkabir_contributionsvillagewashcommittee_2010.pdf (Accessed 12 August 2014).
8. United Nations Development Programme and Government of the People's Republic of Bangladesh. Millennium Development Goals needs assessment and costing 2009-2015, Bangladesh. (Online) 2009. Available: http://www.plancomm.gov.bd//upload/2014/mdgreports/MDG%20Needs%20Assessment%20&%20Costing%202009-2015%20.pdf (Accessed 10 August 2012).
9. WASH Research Team. WASH programme of BRAC: towards attaining the MDG targets Baseline findings. Dhaka: BRAC, 2008.
10. Rabbi SE, Dey NC. Exploring the gap between hand washing knowledge and practices in Bangladesh: a cross-sectional comparative study. BMC Public Health 2013; 13: 89.
11. Rana AKMM, Barua MK, Kabir B. Measuring changes in self-reported hand washing practices with soap among women: a community based empirical study in rural Bangladesh. Dhaka: BRAC, 2010.
12. Aunger R, Schmidt W, Ranpura A, Coombes Y, Maina PM, Matiko CN, Curtis V. Three kinds of psychological determinants of hand washing behavior in Kenya. Social Science and Medicine 2010; 70: 383-391.
13. Arif T, Ahmed S. Exploring reasons of variation in target achievement in sanitary latrine construction under school sanitation programme of BRAC WASH. RED working paper no. 12. (Online) 2010. Available: http://www.bracresearch.org/workingpapers/red_wp12_new.pdf (Accessed 12 April 2010).
14. Rana AKMM. Effect of water, sanitation and hygiene intervention in reducing self-reported waterborne diseases in rural Bangladesh. RED research report (Online) 2009. Available: http://www.bracresearch.org/reports_details.php?scat=26&v=0&tid=539 (Accessed 25 April 2011).
15. Phaswana-Mafuya N, Shukla N. Factors that could motivate people to adopt safe hygienic practices in the Eastern Cape Province South Africa. African Health Sciences 2005; 5(1): 21-28.
16. Dey NC, Ali ARMM. Changes in the use of safe water and water safety measures in WASH intervention areas in Bangladesh. RED Working paper no. 27. (Online) 2011. Available: http://www.bracresearch.org/workingpapers/red_wp_27.pdf (Accessed 12 January 2012).
17. Phaswana-Mafuya N. Hygiene status of rural communities in the Eastern Cape of South Africa. International Journal of Environmental Health Research 2006; 16(4): 289-303.
18. Singh A, Arora AK. Knowledge, attitude and practices of villages regarding sanitary latrines in north India. Indian Journal of Preventive and Social Medicine 2003; 34(3 & 4): 118-123.
19. Pittet D. Improving adherence to hand hygiene practices: a multidisciplinary approach. Emerging Infectious Diseases 2001; 7(2): 234-40.
20. Barrett R, Randle J. Hand hygiene practices: nursing students' perceptions. Journal of Clinical Nursing 2008; 17(14): 1851-1857.
21. Boyce J, Pittet D. Guideline for hand hygiene in health care settings: recommendations of the healthcare infection control practices advisory committee and the HICPA/SHEA/APIC/IDSA hand hygiene task force. American Journal of Infection Control 2002; 30: 1-46.
