Shortage of female rural doctors
The shortage of doctors in rural and remote areas has been widely reported in Australian and international literature1-5. Excessive workloads, particularly after hours and on call, the lack of locums, and poor access to professional support have dominated these reports as contributors to this geographic disparity6-8. Although in 1998 women comprised 33% of all medical practitioners9, 32.5% of all GPs and 59.9% of GP registrars10, this proportion is not yet reflected in rural medicine. In 1994 only 17% of all female GPs worked in a rural or remote area11. However, more recently, Wainer12 reported that 40% of young doctors taking up rural general practice in Victoria, Australia, were female. This suggests that female medical students and graduates are at least being attracted to rural areas.
The importance of family relationships
Historically, women have been reluctant to work in rural areas for a range of reasons13. Most of these are related in some way to the career ambitions of female doctors being modified by the development and maintenance of personal and family relationships. The National Rural General Practice Study (NRGPS)14 reported that significantly more female than male rural doctors rated 'opportunities for their spouse' in their current location as an important retention factor, and also rated 'partner satisfaction' in their current location more highly than did the men. This supports the idea that retention of female rural doctors is linked to opportunities and satisfaction for the doctor's partner.
Personal and professional needs of female rural doctors
A number of recent studies particularly addressed the needs of rural women doctors 12,15-18. The doctors involved in these studies discussed the prime issues of work practices, health and personal safety, conflicts between professional and personal roles, lack of social supports and difficulty accessing continuing medical education. It is interesting that in spite of these issues, 90% of the women surveyed or interviewed by Tolhurst et al.15 planned to remain in rural practice for at least 2 more years, implying that there are some overriding positive aspects that keep women in a rural practice. Humphreys et al.19 reported survey results from 677 rural and remote GPs (184 female) in Australia who were asked to stratify the importance of six retention factors in the decision to remain in rural practice. The authors reported that good on-call arrangements were considered to be the most important factor contributing to the decision to remain in rural practice, irrespective of the sex of the respondent. Variety of rural practice was considered next most important among male GPs, but women ranked the availability of professional support more highly.
Aims and objectives
The present study aimed to identify the positive aspects of rural medical practice that attract and retain women doctors, to provide information to rural communities and workforce planners that could be used to sustain and increase the rural female medical workforce. It examined, in depth from a female perspective, information that has been generated from rural and general practice research, by describing the work and personal experiences of 10 women general practitioners. In describing these experiences we wanted to define specific personal and professional phenomena occurring for women working in rural South Australia and the relationship experiences of these women with work, the community and the family. It is in the nature of qualitative research that great depth and breadth of information can be gained from a single subject. For a research project of this type, 10 interviews were therefore appropriate.
Methods
The methodology of the present study was informed and adapted from the work of van Manen20. Van Manen's methodological premise is that human knowledge and understanding may be gained by analysing the reflective descriptions of people who have lived an experience. In the present study the description of an experience was analysed in the context of the woman's stage of life, for example newly graduated, recently married, single, established in her own home, children at school, children left home. The study took into account the context of where the doctor was living and working at the time (an isolated small community, a large provincial centre) and the context of how she was feeling at the time (eg confident, frustrated, socially isolated, professionally valued). The data were manually analysed by two separate researchers. Each researcher independently reviewed full transcripts of the interviews and marked experiences or descriptions of experiences common to the women's stories. The findings of the two researchers were compared for validity.
The names of 10 women doctors working in general practice in rural South Australia in 1999 were selected using a process of systematically excluding alternate names from a list provided by the South Australian Rural and Remote Medical Support Agency (SARRMSA). The list of names was divided into three groups representing up to 5 years in a rural location, between 6 and 10 years in a rural location, and greater than 10 years in a rural location, and 3-4 names were selected from each group. Rural locum relief service doctors, temporary resident doctors and GP registrars were excluded prior to selection.
A letter of introduction and an information sheet with an invitation to participate was sent to each woman at her practice address. The letters were followed up by a phone call 1-2 weeks later at which concerns were clarified and an interview time was arranged. No doctor declined to be interviewed, and all of the women signed consent forms for the interview. Face-to-face interviews occurred at a location of the doctor's choice, which may have been at home, at their surgery at a time when they were not consulting, or in a nearby café. The interviews were facilitated by focussed but open-ended prompt questions addressing various facets of the women's experiences (Fig 1).

Figure 1: Areas addressed by prompt questions.
Both the University of Adelaide Ethics Committee and the Royal Australian College of General Practitioners Research and Evaluation Ethics Committee approved the study.
Results
Demographics
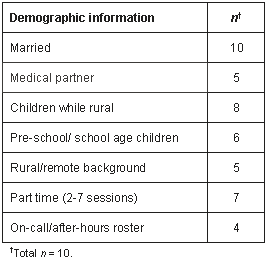
The women who participated in the study were aged between 35 and 65 years, and had worked in rural general practice between 4 and 24 years, in their current location between 4 and 14 years (Table 1). Two had worked in solo practice; none was currently working solo; a few currently provided anaesthetic or obstetric services although most had done so at some time.
Table 1: Demographic information regarding participants at time of interview (unless otherwise specified)
Attractive features of rural practice
The common features attracting the women to rural general practice were a belief that rural medical practice provided a variety of work and the opportunity to use a range of skills; the opportunity to provide continuity of care and know the community relationships; a sense of being valued by the community, and a perception that this is different from city practice; the chance to provide the 'female' medical option; and lifestyle issues, particularly that of a healthy environment for young children.
I always had this idea that the rural lifestyle was attractive and enjoyable.
Similarly, the professional issues that influenced the women to remain in rural general practice were essentially those that originally attracted them to rural practice, that is, the opportunity to use a range of skills, to provide a wider variety of medical care, and to provide continuity of care.
You're there when they have their serious [event] up in hospital but you're also there for their follow up afterwards and people really feel that you're the one that knows them best.
Professionals 'fitting into the model'
Most doctors addressed dealing with a practice structure that possibly had never had to accommodate a female doctor before. Although many described negative experiences, they showed remarkable adaptability to 'fit into the model'.
They could understand that I had these commitments and they were happy as long as I did my job right and didn't ring up and say I've got a migraine today or the kids are sick or whatever.
Issues developed at different stages of the women's rural practice careers. Most commonly they were at the time that the women were having a family and experiencing a change in their priorities, although establishing a new practice or developing a female presence in a previously all-male practice were also significant events. The women commented on the value of good mentors and feeling supported by professional organizations, and particularly highlighted the importance of having supportive colleagues at these times. Practices that were unable to accommodate the requirements of a woman did not keep that doctor for long - occasionally meaning they lost the male doctor spouse as well.
I was in a very chauvinistic group who didn't seem to recognise my skills and that was very very frustrating, but we just took care of that situation and got out of it.
The general pattern was that the women shared an equal load of on call with the other doctors until they had a family, at which time they cut back to part-time hours and where possible left the on-call roster. Clearly the benefit here was working in a larger practice, or a town with several practices so that leaving the on-call roster was not seen as a great imposition on the other doctors.
It was fairly soon accepted but I think I had to get the courage to say, well, this is what I am prepared to do and not feel like I was letting everyone down by not doing what everyone else was doing.
The importance of having a mentor or some other form of professional support was a powerful common theme. Related to this was the importance of being part of a practice that shared common ideas about the management of patients.
Older GPs who were my mentors and taught me a lot of things about practical procedures, were always there for advice... I wouldn't like to go into rural practice on my own.
Although most of the women were happy with the support of their Division of General Practice or local medical associations, some women felt poorly supported by professional medical organizations, and indeed their colleagues.
The attitude of male practitioners and or hospital boards and so on, who don't accept that the way women work is a legitimate way to practice in rural areas.
Social interactions - the community
Community and family/social relationships were increasingly influential in the decision to remain in the country. Feeling welcomed by the community was a very important common theme for the doctors. Not many of the women stayed in a town where there was no sense of being welcomed by the community.
The other thing that stood out... was the social isolation, the suspicion that the townsfolk had towards newcomers and the lack of welcoming.
In contrast:
Everyone's stopping saying hello, how are you... being so involved in a very - I don't find it intrusive, just a friendly welcoming way.
The depth and the continuity of the relationships that the women developed with their patients, were considered a real benefit of working in rural practice. The women emphasised the importance that was placed on the doctors becoming involved in the social aspects of community life. For some of the women, this involvement developed naturally out of the relationships with their patients, for others it required a specific effort. They all felt that it was an integral part of becoming accepted into the community.
You should really get involved in something when you come, you really need to be involved in something. I would say either a sport or a church or Tidy Towns or something that you're really involved in, not just as a spectator...
Patients as friends
The women noted that the need to maintain a professional role could affect their ability to relax after hours. The closeness these women felt to their patients in view of this continuity and privileged knowledge overflowed into the development of friendships. This was often seen as a double-edged sword. The doctors identified a blurring of boundaries between 'patients' and 'friends'. The women all felt a need to debrief after difficult clinical situations, but felt inhibited in using their friends because of the need for confidentiality. This often contributed to a sense of isolation, in spite of the positive social interactions.
I suppose it's the difficulty in those sort of situations is that you have this balance between getting the care you need and having a confidentiality so there are those issues that you sort of juggle.
An alternative reason offered for the difficulty confiding in friends was the need to be seen as a confident professional. The women were highly aware of the potential for friendships to compromise medical decisions.
I couldn't do that to my close friends here because I deliver their children and they'd ask about skin spots and they relied on the fact that I was invincible to a certain extent...I was still their doctor and I had to protect that relationship for them and for me.
Many of the women recognised that they were seen as 'the female option'. The GPs felt that there were assumptions and expectations of what the 'lady doctor' would and should do which collided with the doctor's desire to provide a wide variety of services. These expectations stemmed from the community, and often from the other doctors in the practice.
The women married to doctors were particularly sensitive to these expectations, for example:
They actually probably wanted [my husband] as a main partner and just me to offer that option of female general practitioner.
The family - counting the cost
The family issues that influenced the women in the present study to remain in a particular rural location reflected the decision to move in the first place. For some the major influence was that of spouse employment. The farmer husband was established or would have difficulty finding employment somewhere else. The doctor husband was established and satisfied in his employment, or alternatively difficulties in finding replacement doctors restricted the opportunities of the family to move.
The more common themes that emerged when discussing family relationships and influences on the women's practices did not address the positive factors influencing their decision to remain in a rural area, but the challenges that they faced as rural doctors who were also wives and mothers. They highlighted the change in the women's priorities with marriage and/or the birth of children, the importance of having a supportive spouse and appropriate arrangements for child care when working.
After marriage it's hard I think as a female because you've got your commitments to your husband and your family.
The return to work after having babies was marked by decreased contact hours with patients, often simply to 'keep a hand in' or maintain clinical skills until the grown family allowed the woman to return to full-time work.
For a period of [several years] I didn't do a lot. [But] I didn't have one single year when I didn't have some medical income to put when I did my tax return.
Some of the most powerful statements from these women related to maintaining a happy family in the face of the inevitable demands of rural practice. The women were all dedicated to their patients and their communities, and felt guilty when they put their families first, and yet guilty when their families perceived that the women put their work first.
You spend so much of your day...caring about other people and putting your energy into that, when you get home what have you got left for your husband or your son?
The women identified their spouse/partner as their major source of support. The women with non-medical partners in particular were distinctly aware of the cost to their partner of placing the woman's career first, and the cost to their families of their professional choices. One doctor described her concern about the potential consequences of this type of prioritising:
Not that his job is less important but it is easier [for him] to take time off and have that covered and so he, I suspect at times feels that I don't take his job and his occupation as significantly.
Discussion
Many issues facing rural general practitioners are the same irrespective of the gender of the doctor: workforce, income, on call commitments; family issues such as education7,15,21,22. The measures that the women in the present study used to enable them to continue in rural general practice were remarkably similar. The women all worked part time at some point in their careers, for a variable period; they all ceased to participate in on-call rosters for variable times, in the main they worked in group practices when possible. The women developed a network of friends on whom they relied for personal and social support, and made alternative arrangements for child care and, in many cases, for domestic duties. In some cases, the husband or partner took on a significant share of the domestic workload, although more often this was delegated to someone outside the immediate family. The women emphasised the importance of having a supportive spouse and professional mentors or confidantes.
The doctors who participated in this study identified several factors that drew them to rural general practice: the professional issues of variety of work and the ability to provide continuity of care to the members of their communities figured strongly. They felt valued by their communities and by their colleagues. They believed that their chosen community provided a positive and nurturing environment for their children. In spite of the difficulties they faced in rural general practice, for example feelings of social or professional isolation, those women who married local men would not consider leaving, because they felt that their spouses would not have employment opportunities or be 'satisfied' in a city location. This supports the findings of several reports 12-14,18,23. The 'down side' of rural practice for all of these women was the same as in studies of rural women doctors in other Australian states and internationally: the guilt of role strain, pressure to work longer hours or participate in on-call and after-hours rosters8,24-26. Recent work from Queensland, Australia27 confirms the importance of clinical and social support for both male and female general practitioners in rural areas, while other work reports that urban women doctors also experience many of the issues contributing to role strain28-30. Young male doctors and medical students also report a desire to work more flexible hours and to participate in the care of their families. International research is already addressing the demand for maternity and parental leave policies in rural practices31, as well as in other areas of medicine32.
Conclusion
For the women in the present study, remaining in rural practice was generally a positive experience because they were accepted by their chosen communities as doctors, women and in most cases mothers. They acknowledge that personal supported elicited in various ways (through husbands and partners taking on a non-stereotypical role in the family; through the development of friendships that become extended families, with neighbours, friends and other paid community members taking on responsibility for child care, cooking and cleaning; and through broader community support with acceptance of the multiple roles of the female doctor) was crucial to their decision to remain in rural practice. Furthermore, support and understanding from colleagues in the practice was an essential component to the success of these women as rural medical providers, particularly at times of significant change in the family. Finally, professional support, both clinical and non-clinical, played a significant role in keeping these women in the country.
Recommendations - keeping women doctors in the country
Over the decades that women have become an increasing proportion of the workforce, the challenges of combining social and professional roles have been described by academics, with very little success providing workable solutions. It seems that in the country individual doctors and their communities (who are often ill-funded to develop and maintain formal support structures) have taken on the responsibility of generating local solutions, with little opportunity to investigate or explore how other women may have dealt with similar problems. On the basis of the findings in the present study, the authors suggest that government health departments actively fund an advisory body consisting of rural women, representing the community and the medical profession, to guide future efforts in addressing the needs of our female rural doctors. In particular, this group can work to identify potential local, State and national solutions to problems accessing child care and spouse support. Including community representatives will ensure that supporting a female rural medical service will also benefit the community, because women who live and work in the country are highly aware of the potential their communities have, if adequately funded, to set up practical and effective processes. More specifically, establishing an electronic network for rural women doctors would provide not only ongoing support for established doctors, but also the opportunity for mentoring of new rural practitioners. Developing appropriate support structures for female doctors may also result in other female professionals, for example nurses and teachers, considering relocating to or remaining in rural locations.
Acknowledgements
This work was supported by the Royal Australian College of General Practitioners Registrar Scholarship and Research Fund. Preparation of the manuscript was supported by the Primary Health Care Research Education and Development Program.
References
1. Australian Medical Workforce Advisory Committee. The medical workforce in rural and remote Australia, AMWAC Report 1996.8. Sydney, NSW: AMWAC, 1996.
2. Strasser R. How can we attract more doctors to the country. Australian Journal of Rural Health 1992; 1: 39-44.
3. Cameron I. Retaining a medical workforce in rural Australia. Medical Journal of Australia 1998; 169: 293-294.
4. Barnett JR. Foreign medical graduates and the doctor shortage in New Zealand, 1973-79. New Zealand Medical Journal 1987; 100: 497-500.
5. Crandall LA, Dwyer JW, Duncan PR. Recruitment and retention of rural physicians: issues for the 1990s. Journal of Rural Health 1990; 6: 19-38.
6. Hays B, Veitch PC, Cheers B, Crossland L. Why doctors leave rural practice. Australian Journal of Rural Health1997; 5: 198-203.
7. Hoyal FMD. Retention of rural doctors. Australian Journal of Rural Health 1995; 3: 2-9.
8. Barley GE, Reeves B, O'Brien-Gonzales A, Westfall JM. Characteristics of and issues faced by rural female family physicians. Journal of Rural Health 2001; 17: 251-258.
9. Australian Medical Workforce Advisory Committee. The general practice workforce in Australia, AMWAC Report 2000.2. Sydney, NSW: AMWAC, 2000.
10. Australian Institute of Health and Welfare. Medical labour force 1997. (National Health Labour Force Series). Canberra, ACT: AIHW, 1999.
11. Australian Medical Workforce Advisory Committee and Australian Institute of Health and Welfare. Female participation in the Australian medical workforce, AMWAC Report 1996.7. Sydney: AMWAC, 1996.
12. Wainer J. Female rural doctors in Victoria, 'It's where we live'. Melbourne, VIC: Rural Workforce Agency Victoria, 2001.
13. Australian Medical Workforce Advisory Committee. Influences on participation in the Australian medical workforce, AMWAC Report 1998.4. Sydney, NSW: AMWAC, 1998.
14. Strasser R, Kamien M, Hays R, Carson D. National Rural General Practice Study - quality of life. Melbourne. Traralgon, VIC: Monash University Centre for Rural Health, 1997.
15. Tolhurst H, Bell P, Baker L, Talbot J, Cleasby L. Educational and support needs of female rural general practitioners. Newcastle, NSW: School of Nursing and Health Administration, Charles Sturt University, 1997.
16. Wainer J. Women and rural medical practice. South African Family Practice 2000; 22(6): 19-23.
17. Wainer J, Bryant L, Strasser R. Sustainable rural practice for female general practitioners. Australian Journal of Rural Health 2001; 9(1): S43-S49.
18. McEwin K. Wanted: new rural workforce strategies for female doctors. Findings from a survey of women in rural medicine. Sydney, NSW: NSW Rural Doctors Network, 2001.
19. Humphreys JS, Jones MP, Jones JA & Mara PR. Workforce retention in rural and remote Australia: Determining the factors that influence length of practice. Medical Journal of Australia 2002; 176: 472-476.
20. van Manen M. Researching lived experience: human science for an action sensitive pedagogy. New York: The State University of New York, 1990.
21. Hays RB, Veitch PC, Cheers B, Crossland LJ. Why rural doctors leave their practices: a qualitative survey of Queensland GPs who left rural practice between January 1995 and March 1996. Brisbane, QLD: Centre for General Practice, The University of Queensland, 1997.
22. Kamien M. Staying in or leaving rural practice: 1996 outcomes of rural doctors' 1986 intentions. Medical Journal of Australia 1998; 169: 318-321.
23. Tolhurst H, Lippert N. The National Female Rural General Practitioners Research Project final report. Newcastle, NSW: University of Newcastle, 2003.
24. Spenny ML, Ellsbury KE. Perceptions of practice among rural family physicians - is there a gender difference? Journal of the American Board of Family Practice 2000; 13: 183-187.
25. Elley R. Women in rural general practice: the stresses and rewards. New Zealand Medical Journal 2001; 114: 358-360.
26. Johnston MT. Goin' to the country: challenges for women's health care in rural Canada. Canada Medical Association Journal 1998; 159: 339-341.
27. Joyce C, Veitch C, Crossland L. Professional and social support networks of rural general practitioners. Australian Journal of Rural Health 2003; 11: 7-14.
28. Myerson S. Seven women GPs' perceptions of their stresses and the impact of these on their private and professional lives. Journal of Management Medicine 1997; 11: 8-14.
29. Gautam M. Women in medicine: stresses and solutions. Western Journal of Medicine 2001; 174: 37-41.
30. Kilmartin MR, Newell CJ, Line MA. The balancing act: key issues in the lives of women general practitioners in Australia. Medical Journal of Australia 2002; 177: 87-89.
31. Mainguy S, Crouse BJ. Maternity and family leave policies in rural family practices. Minnesota Medicine 1998; 81: 22-24.
32. Lent B, Phillips SP, Richardson B, Stewart D on behalf of the Gender Issues Committee of the Council of Ontario Faculties of Medicine. Promoting parental leave for female and male physicians. Canada Medical Association Journal 2000; 162: 1575-1576.


