Introduction
Lateral Epicondylalgia (LE) is the term used to describe pain felt at the common origin of the wrist extensor muscles. The nomenclature of this condition includes lateral epicondylitis, humeral epicondylitis and colloquially 'tennis elbow' or 'rower's elbow'. LE is diagnosed by the presence of pain over the lateral epicondyle of the humerus and provocation of pain on resisted dorsiflexion of the wrist1-3. The annual prevalence of LE is 1-3% in the general population4,5. This article seeks to explore the impact of LE on rural work forces. Current treatment options will be discussed and a new direction for effective long-term management will be proposed.
Lateral epicondylalgia in rural areas
Scientific evidence exists to support the long-held clinical view that repeated activity of the upper limb is a major contributing factor to the development of LE5,6. Manual workers who are required to undertake repetitive or forceful tasks are at greater risk of developing LE7,8.
The link between repeated upper limb activity and overuse disorders such as LE is evident in many rural communities. For example, the manifestation of work-related wrist and forearm injuries is a recognized problem in vineyard workers9 who are involved in the intensive task of pruning. As well as the repetitive strain associated with manual pruning techniques, the processing plants associated with the vineyard and orchard industries require production workers to perform repetitive manual tasks (eg on bottling lines and in canneries). This type of work increases the risk of LE7.
Another rural industry seriously impacted on by cumulative trauma disorders of the upper limb is the meat packing and processing industry10. A study of wrist motion variables in both the left and right hands of bone-trimming workers found them to be at a high risk of developing an overuse injury of the forearm10. A study investigating the prevalence of upper limb disorders in the fish processing industry found that 14.5% of workers reported symptoms of LE11.
The risk of rural workers developing LE may be magnified by the seasonal nature of many rural industries; in the high season the workload rises dramatically. The impact of LE on both rural workers and their employers is a major concern because many of these businesses work under strict seasonal time constraints. Rural employers may not have the flexibility to vary duties employees' duties of larger and more diversified organizations. In rural communities where the local economy is built around industries involving peak seasonal workload, preventative management of work related upper limb disorders is essential.
Aetiology
Lateral epicondylalgia is not an inflammatory disorder
The aetiology and pathophysiology of LE are poorly understood12,13. However, there is evidence to implicate the extensor carpi radialis brevis (ECRB) muscle in the development of LE. ECRB is a small muscle that originates from the lateral epicondyle of the humerus and inserts onto the midcarpal joint in the wrist. ECRB predominantly imposes an extension and radial deviation torque over the wrist during movement. It is biomechanically relevant that ECRB often has to produce large forces and that it has only a small surface of origin over which to distribute the tension it generates. ECRB has a predominantly stabilising role in forearm function and is active during both extension of the wrist and in maintaining wrist position during gripping tasks14.
The morphological changes that occur at the ECRB origin in LE sufferers have challenged the traditional opinion that LE is an inflammatory condition. Degenerative rather than inflammatory changes have been noted in the common extensor tendon by several authors12,15. These findings are consistent with the changes observed using sonography16 and surgery17,18. This casts doubt on any treatment of LE that is based on the assumption that LE is an inflammatory condition.
How and why does lateral epicondylalgia develop?
Although the onset of LE appears to be related to repetitive and forceful activity of the forearm, the mechanism by which these forces induce degenerative changes at the common extensor origin remains uncertain. Some authors believe that a compression syndrome is partially or wholly responsible2,19,20. Such a mechanism would involve dynamic compression of neural and vascular structures with the prolonged and forceful action of the forearm extensors. The resultant changes in circulation throughout the region would lead to a metabolically destructive environment. Another hypothesis is that LE relates simply to the development of tendinosis as a result of overuse of the wrist extensors21,22. It has also been postulated that excessive eccentric force transmitted through the common extensor tendon causes degeneration through a process of cumulative trauma23-25. The influence of a neurogenic component to the condition, inferring that it is a clinical manifestation of a cervico-brachial disorder, has also been suggested by some authors26,27. A link has also been proposed between the neural structures of the cervical spine and the upper-limb muscle activity28. Such a link serves to implicate postural factors associated with the neck and trunk position when working.
In order to understand the morphological changes in the common extensor tendon, it is necessary first to understand how the contributing muscles function. Much research into LE has been undertaken among subjects who play tennis. Nevertheless, findings from these studies might reasonably be generalised to LE arising from occupational activities in which the wrist extensor muscles are required to perform repetitive forceful activities23-25. The significance of muscle activation patterns was illustrated in studies that revealed significant differences between skilled players and recreational tennis players24,25. More accomplished players were found to recruit a larger number of muscles in a smoother movement when performing tennis strokes, compared with less skilled players. Notably, accomplished and elite players rarely suffer from LE.
Another study comparing the surface electromyographic (EMG) activity in the forearm extensor muscles of patients suffering from LE with that recorded in a control group, noted that the muscles were activated earlier and for a longer period in the LE sufferers than in the control group23. These activation patterns were counterproductive to minimising stress through the muscle/tendon unit during impact with the tennis ball. Findings such as these support the hypothesis that abnormal activation patterns of the forearm extensor muscles, and perhaps the upper limb muscles in general, increase the likelihood of developing LE.
In generalising the findings of these tennis-related studies to rural workers it is important to recognise that only 5% of people suffering from LE play tennis, and their LE is therefore usually the result of activities other than tennis29. Further research into the muscle activation patterns in individuals with LE associated with other occupational tasks is required to develop a more complete biomechanical understanding of the cause of the condition.
The findings of EMG studies examining tennis players with LE demonstrated an increased activation of the forearm extensors23. In attempting to relate these findings to LE sufferers who work in rural industries, it could be argued that a precipitating factor in the development of LE is an excessive reliance on the small forearm muscles, especially the mechanically vulnerable ECRB. Alternatively, tension on the brachial plexus that can result from cervico-brachial muscle dysfunction can cause irritation along the nerve tract.
Much of the research investigating LE refers to a group of conditions termed 'work related upper limb mechanical disorders', to which LE belongs 6,11. The evidence presented in these occupationally based studies suggests that LE does not always occur in isolation and is often associated with shoulder and neck symptoms. The work of Abbott30 provides further evidence of a nexus between the elbow and the shoulder by demonstrating an increase in shoulder range of movement after mobilisation of the elbow in subjects with LE.
Management of lateral epicondylalgia
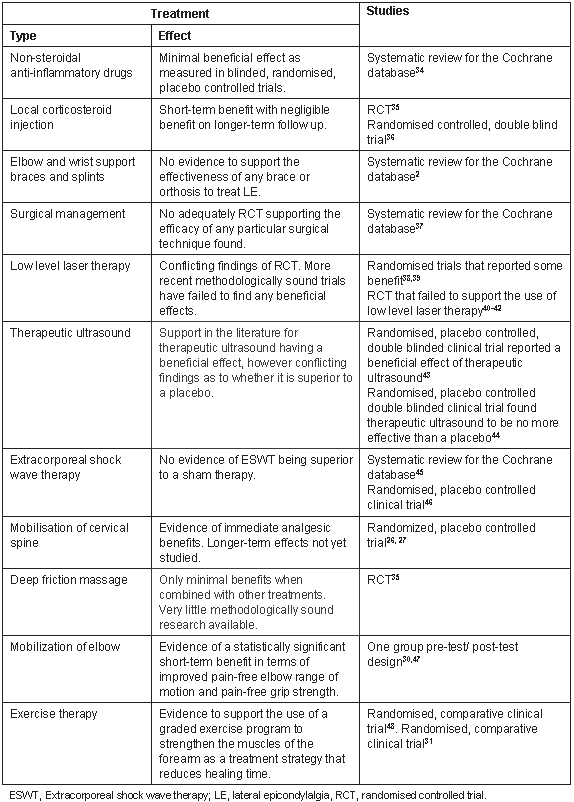
The management of LE remains problematic with the scientific literature failing to reach consensus on the most effective form of treatment2,3,19,31-33. A range of current treatment regimens have been addressed by various researchers and a summary of key findings is presented (Table 1).
Table 1: Summary of empirical evidence for various treatments for LE2,26-27,30-31,34-48
New direction in exercise prescription for lateral epicondylalgia
The absence of strong scientific evidence to support the treatments currently used by clinicians to treat LE, combined with evidence that highlights the link between LE and proximal structures such as the shoulder and cervical spine, suggests that clinicians might consider broadening the scope of exercise prescription for LE. Traditional exercises prescribed for LE have focused on the forearm extensor muscles and on the performance of either strengthening or stretching exercises31,48. If LE is a clinical manifestation of a neurogenic or biomechanical disorder involving more proximal structures, an exercise program should involve recruitment of more proximal muscles that work in synergy with ECRB to perform the functional tasks known to precipitate LE.
Clinical implications: In order to effectively address LE through graded exercise, the clinician should consider including the muscles of the upper arm and shoulder, as well as the muscles of the forearm. An effective program would seek to improve strength, co-ordination and endurance of the stabilizing muscles of the shoulder and upper arm. Specifically effective exercise prescription for LE sufferers would include exercises aimed at improving the strength and endurance of the scapular retractors, posterior deltoid, middle and lower trapezius and the muscles of the rotator cuff. These muscles are required to be active in many of the functional activities that elicit LE symptoms49. Prescribed exercises must be functionally focused and must specifically address deficiencies in muscle function exposed during the physical assessment.
Typically individuals suffering from LE and other work-related upper limb disorders exhibit shortening and over-development of the muscles associated with internal rotation and protaction of the shoulder. This group of muscles includes pectoralis major, pectoralis minor, upper trapezius, levator scapulae, the long head of biceps brachii and sternocleido mastoid. Effective management will include teaching patients to stretch these muscles and to avoid inappropriate levels of activation when performing functional tasks. Conversely, lower trapezius, the rhomboids, infraspinatous, teres minor, serratus anterior and the deep neck flexor muscles are typically weak and lengthened to the point where they are mechanically disadvantaged. To effectively address such deficiencies these muscles will have to be strengthened, and patients taught to recruit them appropriately when performing functional activities.
Although the need for further research into effective exercise prescription for LE sufferers is acknowledged, sufficient evidence exists to indicate that effective management of mechanical and neurodynamic influences from the neck and shoulder needs to occur if a timely and durable return to full function is to be achieved.
The available evidence in regard to treatment for LE should be encouraging to rural practitioners as it is likely that the most effective treatments will require minimal technology or resources, thus enabling intervention for LE to be effective in rural and remote locations where resources are limited.
References
1. De Smet L, Fabry G. Grip force reduction in patients with tennis elbow: influence of elbow position. Journal of Hand Therapy 1997; 10: 229-231.
2. Struijs PA, Smidt N, Arola H, Dijk v VA, Buchbinder R, Assendelft WJ. Orthotic devices for the treatment of tennis elbow (Cochrane Review). Cochrane Database Systematic Review 2002; 1: CD001821.
3. Verhaar JA, Walenkamp GH, van Mameren H, Kester AD, van der Linden AJ. Local corticosteroid injection versus Cyriax-type physiotherapy for tennis elbow. British Journal of Bone and Joint Surgery 1996; 78: 128-132.
4. Verhaar JA. Tennis elbow. Anatomical, epidemiological and therapeutic aspects. International Orthopedics 1994; 18: 263-267.
5. Kitai E, Itay S, Ruder A, Engel J, Modan M. An epidemiological study of lateral epicondylitis (tennis elbow) in amateur male players. Annales de Chirurgie de la Main 1986; 5: 113-121.
6. Pascarelli EF, Hsu YP. Understanding work-related upper extremity disorders: clinical findings in 485 computer users, musicians, and others. Journal of Occupational Rehabilitation 2001; 11: 1-21.
7. Lewis M, Hay EM, Paterson SM, Croft P. Effects of manual work on recovery from lateral epicondylitis. Scandinavian Journal of Work and Environmental Health 2002; 28: 109-116.
8. Pedersen LK, Jensen LK. [Relationship between occupation and elbow pain, epicondylitis]. Ugeskr Laeger 1999; 161: 4751-4755.
9. Roquelaure Y, Dano C, Dusolier G, Fanello S, Penneau-Fontbonne D. Biomechanical strains on the hand-wrist system during grapevine pruning. International Archives of Occupational Environmental Health 2002; 75: 591-595.
10. Marklin RW, Monroe JF. Quantitative biomechanical analysis of wrist motion in bone-trimming jobs in the meat packing industry. Ergonomics 1998; 41: 227-237.
11. Chiang HC, Ko YC, Chen SS, Yu HS, Wu TN, Chang PY. Prevalence of shoulder and upper-limb disorders among workers in the fish-processing industry. Scandinavian Journal of Work and Environmental Health 1993; 19: 126-131.
12. Albrecht S, Cordis R, Kleihues H, Noack W. Pathoanatomic findings in radiohumeral epicondylopathy. A combined anatomic and electromyographic study. Archives of Orthopaedic Trauma Surgery 1997; 116: 157-163.
13. Jansen CW, Olson SL, Hasson SM. The effect of use of a wrist orthosis during functional activities on surface electromyography of the wrist extensors in normal subjects. Journal of Hand Therapy 1997; 10: 283-289.
14. Lieber RL, Friden J. Musculoskeletal balance of the human wrist elucidated using intraoperative laser diffraction. Journal of Electromyogr Kinesiology 1998; 8: 93-100.
15. Alfredson H, Ljung BO, Thorsen K, Lorentzon R. In vivo investigation of ECRB tendons with microdialysis technique--no signs of inflammation but high amounts of glutamate in tennis elbow. Acta Orthopaedica Scandinavica 2000; 71: 475-479.
16. Connell D, Burke F, Coombes P et al. Sonographic examination of lateral epicondylitis. American Journal of Roentgenology 2001; 176: 777-782.
17. Leppilahti J, Raatikainen T, Pienimaki T, Hanninen A, Jalovaara P. Surgical treatment of resistant tennis elbow. A prospective, randomised study comparing decompression of the posterior interosseous nerve and lengthening of the tendon of the extensor carpi radialis brevis muscle. Archives of Orthopaedic Trauma Surgery 2001; 121: 329-332.
18. Owens BD, Murphy KP, Kuklo TR. Arthroscopic release for lateral epicondylitis. Arthroscopy 2001; 17: 582-587.
19. Junk BPJ, Prezelaskowski P, Grygiel M, Garbaczonek M. Surgical Decompression 2001; 52: 23-25.
20. De Smet L, Van Raebroeckx T, Van Ransbeeck H. Radial tunnel release and tennis elbow: disappointing results? Acta Orthopaedica Belgium 1999; 65: 510-513.
21. Jensen B, Savnik A, Bliddal H, Danneskiold-Samsoe B. [Lateral humeral epicondylitis--"tennis elbow". I. Epidemiology, clinical picture and pathophysiology]. Ugeskr Laeger 2001; 163: 1417-1421.
22. Roetert EP, Brody H, Dillman CJ, Groppel JL, Schultheis JM. The biomechanics of tennis elbow. An integrated approach. Clinical Sports Medicine 1995; 14: 47-57.
23. Bauer JA, Murray RD. Electromyographic patterns of individuals suffering from lateral tennis elbow.
24. Giangarra CE, Conroy B, Jobe FW, Pink M, Perry J. Electromyographic and cinematographic analysis of elbow function in tennis players using single- and double-handed backhand strokes. American Journal of Sports Medicine 1993; 21: 394-399.
25. Kelley JD, Lombardo SJ, Pink M, Perry J, Giangarra C. E. Electromyographic and cinematographic analysis of elbow function in tennis players with lateral epicondylitis. American Journal of Sports Medicine 1994; 22: 359-363.
26. Vicenzino B, Collins D, Wright A. The initial effects of a cervical spine manipulative physiotherapy treatment on the pain and dysfunction of lateral epicondylalgia. Pain 1996; 68: 69-74.
27. Vicenzino B, Paungmali A, Buratowski S, Wright A. Specific manipulative therapy treatment for chronic lateral epicondylalgia produces uniquely characteristic hypoalgesia. Manual Therapy 2001; 6: 205-212.
28. Balster SM, Jull G. Upper trapezius muscle activity during the brachial plexus tension test in asymptomatic subjects. Manual Therapy 1997; 2: 144-149.
29. Solveborn SA. ["Tennis elbow" is usually caused by other than tennis. The earlier the treatment the better; spontaneous remission occurs often within 8-13 months]. Lakartidningen 1999; 96: 483-485.
30. Abbott JH. Mobilization with movement applied to the elbow affects shoulder range of movement in subjects with lateral epicondylalgia. Manual Therapy 2001; 6: 170-177.
31. Solveborn SA. Radial epicondylalgia ('tennis elbow'): treatment with stretching or forearm band. A prospective study with long-term follow-up including range-of-motion measurements. Scandinavian Journal of Medical Science in Sports 1997; 7: 229-237.
32. Ko JY, Chen HS, Chen LM. Treatment of lateral epicondylitis of the elbow with shock waves. Clinical Orthopaedics 2001; 387: 60-67.
33. Burnham R, Gregg R, Healy P, Steadward R. The effectiveness of topical diclofenac for lateral epicondylitis. Clinical Journal of Sports Medicine 1998; 8: 78-81.
34. Green S, Buchbinder R, Barnsley L et al. Non-steroidal anti-inflammatory drugs (NSAIDs) for treating lateral elbow pain in adults. Cochrane Database Systematic Review 2002; 2: CD003686.
35. Smidt N, van der Windt DA, Assendelft WJ, Deville WL, Korthals-de Bos IB, Bouter LM. Corticosteroid injections, physiotherapy, or a wait-and-see policy for lateral epicondylitis: a randomised controlled trial. Lancet 2000; 359(9307): 657-662.
36. Newcomer KL, Laskowski ER, Idank DM, McLean TJ, Egan KS. Corticosteroid injection in early treatment of lateral epicondylitis. Clinical Journal of Sports Medicine 2001; 11: 214-222.
37. Buchbinder R, Green S, Bell S, Barnsley L, Smidt N, Assendelft WJ. Surgery for lateral elbow pain. Cochrane Database Systematic Review 2002; 1: CD003525.
38. Vasseljen O Jr, Hoeg N, Kjeldstad B, Johnsson A, Larsen S. Low level laser versus placebo in the treatment of tennis elbow. Scandinavian Journal of Rehabilitation Medicine 1992; 24: 37-42.
39. Simunovic Z, Trobonjaca T, Trobonjaca Z. Treatment of medial and lateral epicondylitis--tennis and golfer's elbow--with low level laser therapy: a multicenter double blind, placebo-controlled clinical study on 324 patients. Journal of Clinical Laser Medicine and Surgery 1998; 16: 145-151.
40. Lundeberg T, Haker E, Thomas M. Effect of laser versus placebo in tennis elbow. Scandinavian Journal of Rehabilitation Medicine 1987; 19: 135-138.
41. Krasheninnikoff M, Ellitsgaard N, Rogvi-Hansen B et al. No effect of low power laser in lateral epicondylitis. Scandinavian Journal of Rheumatology 1994; 23: 260-263.
42. Basford JR, Sheffield CG, Cieslak KR. Laser therapy: a randomized, controlled trial of the effects of low intensity Nd:YAG laser irradiation on lateral epicondylitis. Archives of Physical and Medical Rehabilitation 2000; 81: 1504-1510.
43. Binder A, Hodge G, Greenwood AM, Hazleman BL, Page Thomas DP. Is therapeutic ultrasound effective in treating soft tissue lesions? BMJ 1985; 290(6467): 512-514.
44. Lundeberg T, Abrahamsson P, Haker E. A comparative study of continuous ultrasound placebo ultrasound and rest in epicondylalgia. Scandinavian Journal of Rehabilitation Medicine 1988; 20: 99-101.
45. Buchbinder R, Green S, White M, Barnsley L, Smidt N, Assendelft WJ. Shock wave therapy for lateral elbow pain. Cochrane Database Systemic Reviews 2002; 1: CD003524.
46. Speed CA, Richards C, Nichols D et al. Extracorporeal shock-wave therapy for tendonitis of the rotator cuff. A double-blind, randomised, controlled trial. Journal of Bone and Joint Surgery British 2002; 84: 509-512.
47. Abbott JH, Patla CE, Jensen RH. The initial effects of an elbow mobilization with movement technique on grip strength in subjects with lateral epicondylalgia. Manual Therapy 2001; 6: 163-169.
48. Pienimaki T, Karinen P, Kemila T, Koivukangas P, Vanharanta H. Long-term follow-up of conservatively treated chronic tennis elbow patients. A prospective and retrospective analysis. Scandinavian Journal of Rehabilitation Medicine 1998; 30: 159-166.
49. Harvey R, Peper E. Surface electromyography and mouse use position. Ergonomics 1997; 40: 781-789.
Abstract
Lateral Epicondylalgia (LE) (tennis elbow) is a problematic condition for workers in labour intensive industries. The economies of many rural communities are founded on industries such as grape growing, meat and fish processing, fruit processing and winemaking. Workers in those industries are at increased risk of developing work-related upper limb mechanical disorders, including LE. This article reviews current understanding of the aetiology and management of this common condition as an aid to rural health professionals managing this presentation. A variety of treatment options exist for the management of LE with the literature divided on which approach is most effective. However, there is evidence that exercise is a key component of a management strategy. In addition to the current practice of prescribing exercises for the wrist extensor muscles, recent research suggests that appropriate activation of the stabilising muscles of the shoulder and cervical spine also needs to be considered by the rural practitioner.
Keywords: exercise therapy, lateral epicondylalgia, lateral epicondylitis, tennis elbow, upper limb exercise, upper limb mechanical disorder.
You might also be interested in:
2020 - Differences in US COVID-19 case rates and case fatality rates across the urban–rural continuum

