A rural remote area is a 'frontline' not only of medical practice but also of medical research. A new technology, although perhaps first introduced in an urban center, can only have its real-world efficacy confirmed after widespread use: its use in rural areas will provide important data. Observations by rural doctors may lead to 'discovery' of a new clinical entity: Huntington's disease was first reported by a rural doctor1. In this context, conducting research and writing a paper in a rural remote area is quite important. But is this working well?
It is hard for any young doctor to continually produce academic publications2. In rural and remote areas, it is even harder3. Lack of mentorship is one of the largest barriers for young practitioners to conduct research2. Some government- and university-based research support programs for rural practitioners in which mentorship and other services are provided have been reported, mainly from Australia and Canada, but not from Asian countries4-8.
Jichi Medical University (JMU) in Shimotsuke, Tochigi, established in 1972, is a unique medical university that aims to produce doctors who engage in rural remote practice in Japan. In most cases, JMU graduates work as general practitioners in rural areas for about 6 years after their residency training. The rural practice is conducted as an obligatory service in exchange for exemption of medical school tuition9,10. During this rural service, there is no or little opportunity to receive advice on research or writing a paper. JMU, thus, established the Clinical Research Support Team (CRST)-Jichi, in which JMU faculty members support JMU graduates in designing a study or writing a paper. During a 3-year period since its beginning in July 2010, support requests to CRST-Jichi have increased, resulting in the publishing of 12 English papers in peer-reviewed international journals and two papers in Japanese journals. Here, we briefly describe the system and its significance.
Why was CRST-Jichi founded?
One graduate's bad experience and a faculty member's sympathy for it triggered the establishment of CRST-Jichi. At a conference for JMU graduates, a faculty member of JMU, who later became the director of the CRST, was moved by a young graduate's experience, 'I wrote a paper based on my experience in rural practice and submitted it to a journal without success; I have no experience to publishing an English paper and have no support, and thus the paper will surely be buried in my desk'. The faculty member, also a graduate of JMU, had a similar experience 30 years ago, when he was a rural doctor. Therefore, he and a few other JMU-graduated faculty members decided to make a 'system' to support such rural doctors.
How did CRST-Jichi start?
The founding director and vice-director are both obstetrics/gynecology physicians. Although obstetrics/gynecology is one of the main themes of rural and remote medicine, many studies and papers from rural areas are naturally not confined to obstetrics/gynecology, and thus as a research support team, CRST-Jichi requires a number of experienced researcher-clinicians from various medical fields. For example, if a rural doctor encounters some insect bite disorders and wishes to write about it, then specialists in parasitology, pharmacology, and infection medicine are required. Specialists for medical statistics are needed for studies requiring statistics.
CRST-Jichi started with the director asking some experienced JMU staff researchers to join the 'support team' (later becoming CRST) in a person-by-person manner. Twenty-one researchers, all well experienced both in study design and writing papers, joined, forming the core of the present CRST. Among the 21 members, 19 were JMU graduates. Later, via email and periodical JMU newsletters, we asked all JMU academic staff members to join this support team on a voluntary basis. Approximately 60 members accepted this proposal within a couple of days after emailing and then the CRST started on 1 July 2010. The CRST members currently number 88, including 43 JMU graduates.
How does the CRST system work?
Figure 1 shows how CRST-Jichi supports the client, a JMU graduate who asks CRST for advice on study design or about editing a paper.
- The client e-mails the CRST that he/she wishes the CRST to support designing or modifying a study, or editing a paper.
- Usually, the director reviews the study design or reads the draft of the paper, and appoints an appropriate staff member ('responsible supporter'), based on the topic dealt with there. The core members of the CRST also review the request on the day it arrives and help the director to find a candidate. If the theme happens to be a core member's specialty, then, the core member takes on the role of a responsible supporter who is responsible for guiding the client through the authorship process.
- After the candidate specialist accepts the role of the supporter, the client then emails the details of the study to him/her, yielding a 'happy engagement'.
- If a candidate chosen by the director does not accept the offer, or the director is not sure who best knows the corresponding issue, then all CRST members will be emailed, and asked if they wish to become a responsible supporter of the client. To date, steps 2-4 have always resulted in a 'happy engagement'.
- If a responsible supporter has some difficulty in performing their job (designing a study or writing a paper), then they raise an 'open question' via the CRST mailing list to all 88 CRST members. If the theme is multidisciplinary, a second or third supporter in the relevant specialties provides assistance.
- The responsible supporter and the client discuss the issue by email and complete the final paper, which means a 'happy engagement' of the supporter and the client. As mentioned, on an open mailing list forum among CRST members, the issue in progress is sometimes discussed, and the theme is shared by all CRST members. CRST members advise whenever they want to do so, and are regarded as 'cooperating witnesses'.
- If the paper has been accepted, the responsible supporter is listed as a co-author. Depending on their contribution, the responsible supporter can become the corresponding author. The second or the third supporter, if they have contributed significantly, can also become a co-author of the paper. Who becomes a co-author is not strictly defined by the CRST. Simply, those who significantly contributed to the study/paper become co-authors. Therefore, those only giving advice via email (cooperating witnesses) do not become co-authors. The director can decide the authorship in the event of disagreement, but this has never happened.
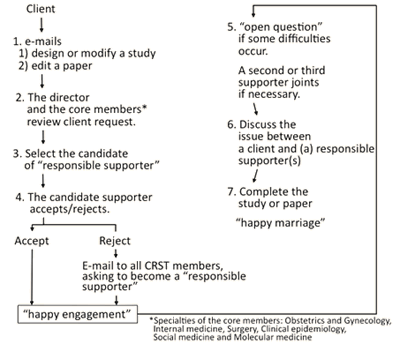
Figure 1: How the Clinical Research Support Team supports a client.
What are the CRST outcomes?
Table 1 shows the achievements of CRST-Jichi at the time of writing. So far, we received a total of 27 requests; all have already been published or are in progress. Of them, 12 English papers1,11-21 and two Japanese papers have been accepted for publication in peer-reviewed journals. Of the 12 English papers, seven were accepted in rural medicine journals. The median time from client email request to paper acceptance was 7 months (range 1-32 months). Table 2 shows the research (13 themes) currently under the guidance of CRST-Jichi.
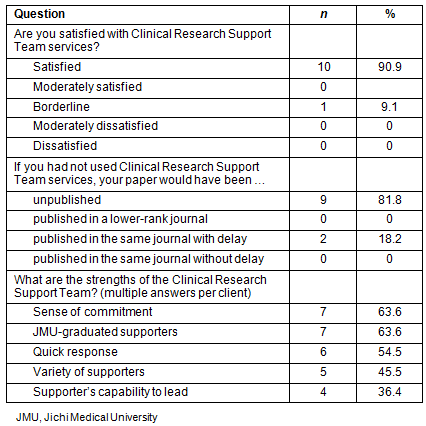
In September 2013, CRST sent a questionnaire to all the 11 clients (one client wrote two English papers) whose papers were accepted. All have responded; 91% were satisfied with CRST service, and 82% considered their papers would not have been published if they had not used the service (Table 3). A sense of commitment, access to JMU-graduated specialists, and quick response were reported by clients as the major strengths of CRST (Table 3). The variety of specialists and their ability to lead research consultation were also cited as strengths.
Table 1: Clinical Research Support Team-supported English papers published in peer-reviewed journals
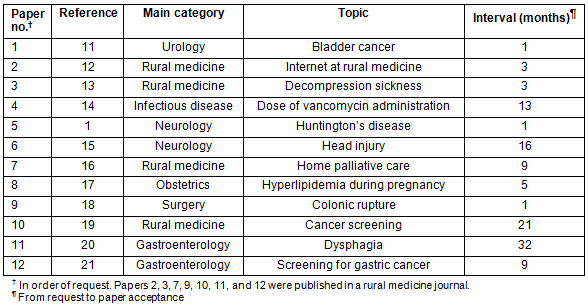
Table 2: Research themes under the guidance of the Clinical Research Support Team, as of March 2014
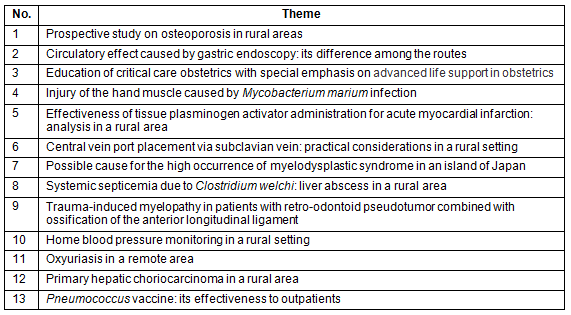
Table 3: Summary of questionnaire responses from the 11 clients whose papers were accepted by peer-reviewed journals
Three possible reasons for success
CRST-Jichi was successful in supporting rural doctors. As shown in the results of the client survey (Table 3), the following are possible reasons why CRST worked well.
First, rapid response on the CRST side is important. For example, within a day after a manuscript's arrival, the director usually reads the manuscript, retrieves the references via the PubMed database, reads UpToDate (an evidence-based clinical support resource) for the corresponding theme, and then roughly estimates the significance of the study. It is usually within 1 week that a responsible supporter is selected. The client continues to be informed at each step. Designing a study and writing a paper is better performed while both a client and CRST members have a keen interest. Delays may weaken the motivation of the client. Thus, a rapid response at this stage is paramount to success. After a responsible supporter has been selected, progress depends on the client and the supporter.
Second, a sense of commitment of CRST members is essential. Even without the CRST system, the university staff may advise a client if asked. However, merely receiving advice is by no means sufficient for eventual acceptance of the paper. The responsible supporter must be responsible and commit to the paper. This becomes in some ways a burden to the supporter. This is unavoidable, and so, in a sense, may be a necessary evil for the paper acceptance. However, being an author is important to one's academic career, especially for university posts. Thus, a win-win relationship develops between the client and the supporter. This is important for the system to continue.
Third, many CRST members are JMU graduates (note that it is a custom of Japanese medical schools that graduates of a school return to the school to work as faculty). The JMU-graduated specialists not only provide knowledge and experience but also bring a rural perspective to the paper, which adds value to the paper, particularly for readers of rural health journals. Also a sense of community and strong volunteerism are easily fostered among CRST members and clients. This may be partly because JMU is a unique school in which all the students live in the same dormitory and all the graduates serve in rural areas, often in the same hospitals. This enables the members to voluntarily devote themselves to the time- and energy-consuming job. Thus, JMU may be in a better position in this sense. We believe that a strong sense of confidence becomes fostered both between a client and the supporter, and among CRST members during the effort required to study or to write a paper. CRST has created a strong bond among the participants.
Potential impact and future plan
CRST- Jichi has made a good start; however, there may be many more JMU graduates who seek help. Members of CRST wish them to ask for support. Being involved in the current issues in rural health makes a refreshing change for CRST members, many of whom used to be rural doctors but now are in academic posts. Thus, supporting and being supported will become a real win-win relationship, making this system more sustainable.
The 3-year trial of CRST has a potential impact on schemes that produce rural doctors in other medical schools in Japan. Since 2008 the government has implemented JMU-like rural medical education programs at most of the 80 medical schools in Japan. The number of entrants to these programs has now reached 15% of medical school entrants in Japan22. Although these programs are currently only for undergraduate students, their graduates will need systemic academic support in the future. The experience of CRST may be helpful for these new programs to create such a support system.
Some medical schools and public sectors support research conducted by rural health professionals4-8. The support includes providing mentors, short courses such as research design and statistics, research funds, conferences, and arrangement of research groups4-8. Flinders University in South Australia, for example, utilizing government funding scheme, provided funds and mentoring to rural health professionals and achieved a substantial effect7. Because CRST-Jichi is a voluntary group, it neither uses nor provides funds. However, the experience of the CRST showed that providing responsible and rural-minded mentors in a timely fashion is of crucial importance.
The CRST system is applicable to other institutions under some conditions. It needs a substantial number and variety of rural-experienced clinical/academic specialists. This does not necessarily apply to all research support institutions. However, many medical schools or hospitals in the world may have a role to academically support rural practitioners. At the same time, many of them may have limited funding resources and thus have to provide the service on a voluntary basis. However, in such institutions, there may be specialists who had once worked in rural areas and are now working as academic or specialist clinicians. This situation is quite similar to that of JMU. JMU has some features favoring the success of this CRST trial, and our experience can be applied to this type of institution both in Japan and other countries.
References
1. Nakamura K, Ota M, Kawata A, Isozaki E, Muramatsu S, Matsubara S. Careful clinical observation is essential for diagnosis of Huntington's disease. Arquivos de Neuro-psiquiatria 2012; 70(8): 646.
2. Reid MB, Misky GJ, Harrison RA, Sharpe B, Auerbach A, Glasheen JJ. Mentorship, productivity, and promotion among academic hospitalists. Journal of General Internal Medicine 2012; 27(1): 23-27.
3. Cusick A, Lannin N. On becoming a practitioner-researcher in remote northern Australia: personal commitment and resources compensate for structural deterrents to research. Disability and Rehabilitation 2008; 30(26): 1984-1998.
4. Macleod ML, Dosman JA, Kulig JC, Medves JM. The development of the Canadian Rural Health Research Society: creating capacity through connection. Rural and Remote Health 7(1): 622. (Online) 2007. Available: www.rrh.org.au (Accessed 31 March 2014).
5. Birden HH. The researcher development program: how to extend the involvement of Australian general practitioners in research? Rural and Remote Health 7(3): 776. (Online) 2007. Available: www.rrh.org.au (Accessed 31 March 2014).
6. Miller J, Bryant Maclean L, Coward P, Broemeling AM. Developing strategies to enhance health services research capacity in a predominantly rural Canadian health authority. Rural and Remote Health 9(4): 1266. (Online) 2009. Available: www.rrh.org.au (Accessed 31 March 2014).
7. Ried K, Farmer EA, Weston KM. Bursaries, writing grants and fellowships: a strategy to develop research capacity in primary health care. BMC Family Practice 8: 19. (Online) 2007. Available: http://www.biomedcentral.com/1471-2296/8/19 (Accessed 24 March 2014).
8. Taylor J, Hughes C, Petkov J, Williams M. Unique issues in research and evaluation in rural and remote locations: is there a place for specific research training? Rural and Remote Health 5(2): 351. (Online) 2005. Available: www.rrh.org.au (Accessed 31 March 2014).
9. Inoue K, Hirayama Y, Igarashi M. A medical school for rural areas. Medical Education 1997; 31(6): 430-434.
10. Matsumoto M, Inoue K, Kajii E. Contract-based training system for rural physicians: follow-up of Jichi Medical University graduates (1978-2006). Journal of Rural Health 2008; 24(4): 360-368.
11. Ohzawa H, Arai W, Kondo Y, Endo S, Morita T, Matsubara S. Urinary bladder rupture associated with squamous cell carcinoma of the bladder; a cause of acute peritonitis. Internet Journal of Urology 7: 2. (Online) 2010. Available: http://ispub.com/IJU/7/2/13354 (Accessed 24 March 2014).
12. Tateno Y, Sato T, Matsubara S: Sharing area-specific information via an internet forum benefits rural clinicians: a lesson learned from a case with decompression sickness on a remote island. Rural and Remote Health 11(3): 1856. (Online) 2011. Available: www.rrh.org.au (Accessed 31 March 2014).
13. Sato T, Iga T, Nagashima K, Matsubara S. Is centralization in emergency rural medicine always right? Lessons learned from two cases of decompression sickness. Rural Remote Health 11(2): 1711. (Online) 2011. Available: www.rrh.org.au (Accessed 31 March 2014).
14. Maki N, Ohkuchi A, Tashiro Y, Kim MR, Le M, Sakamoto T, et al. Initial dose of vancomycin based on body weight and creatinine clearance to minimize inadequate trough levels in Japanese adults. European Journal of Clinical Microbiology and Infectious Diseases 2012; 31(10): 2537-2543.
15. Tokushige J, Matsubara S, Tanaka Y, Kato S. Trephination for acute epidural hematoma using stainless wire on a remote island. Journal of Emergency Medicine 2012; 43(6): e489-490.
16. Tateno Y, Ishikawa S. Clinical pathways can improve the quality of pain management in home palliative care in remote locations: retrospective study on Kozu Island, Japan. Rural Remote Health 12: 1992. (Online) 2012. Available: www.rrh.org.au (Accessed 31 March 2014).
17. Sato S, Ohkuchi A, Kawano M, Iwanaga N, Furukawa Y, Matsumoto H. Effect of eicosapentaenoic acid agent on aggravated hypertriglyceridemia during pregnancy. Journal of Obstetrics and Gynaecology Research 2013; 39(11): 1541-1544.
18. Okada Y, Okamoto D, Matsubara S. Successful drainage for life-threatening colonic perforation by a young physician on a remote island. Rural and Remote Health 13(2): 2638. (Online) 2013. Available: www.rrh.org.au (Accessed 31 March 2014).
19. Tateno Y, Miyazaki Y, Tsuboi S. Can screening invitations from primary care physicians increase participation in cancer screenings on remote islands? General Medicine 2013; 14(1): 40-47.
20. Murata K, Ishikawa S, Sugioka T. Investigation of dysphagia symptoms and their association with subjective symptoms in inhabitants of an island. General Medicine 2013; 14(1): 32-39.
21. Matsumoto S, Ishikawa S, Yoshida Y. Reduction of gastric cancer mortality by endoscopic and radiographic screening in an isolated island: a retrospective cohort study. Australian Journal of Rural Health 2013; 21(6): 319-324.
22. Ministry of Education, Culture, Sports, Science and Technology. Survey on community health. (Japanese) (Online) 2014. Available: http://www.mext.go.jp/component/a_menu/education/detail/__icsFiles/afieldfile/2013/07/11/1324090_6.pdf (Accessed 24 March 2014).


