With nearly half of all persons in the USA reporting one or more chronic conditions1,2, meeting the needs of these individuals has become a challenge for the current healthcare system. In particular, rural communities face challenges in regard to access to health care and chronic disease self-management programs. Smith et al. found that rural populations generally display a greater prevalence of less healthy behaviors that impact chronic illnesses, including sustained unhealthy nutrition, increased prevalence of smoking, lower levels of physical activity, and greater levels of psychosocial distress3. Rural elders have been reported to have significantly worse physical and mental functioning and more restrictions in activity due to chronic conditions than urban elders4,5. Yet research has also suggested that rural individuals who have a chronic disease are twice as likely as adults residing in inner cities and suburbs to be more ready to change their behaviors in order to promote their health on the stages of change model6. Prevalent chronic conditions, such as arthritis, diabetes, and heart disease, entail self-management regimens of medication and behavioral change7, which can reduce mortality and disability and improve quality of life.
As the number of chronic conditions that individuals experience increases, so does the complexity of care. To address this challenge, health professionals have begun to promote a chronic care model in which the active involvement of individuals in making decisions about health care and the need to promote self-care is emphasized8,9. 'Chronic disease self-management' refers to the daily activities that individuals undertake to keep their health conditions under control - activities that minimize the impact on their physical health status and enable them to cope with the psychological effects of their condition7,10. Von Korff et al. noted that self-management activities include the following tasks: engaging in activities to promote health and that also build up physiological reserves; interacting with healthcare providers; adhering to treatment protocols; monitoring physical and emotional status and making appropriate management decisions on the basis of self-monitoring; and managing the effects of the illness on the individual's ability to function in important roles, as well as activities that have an impact on emotions, self-esteem, and relationships with others11.
Rurality and chronic disease self-management
While rurality is defined by the size of community, population density, or geographical location12, the classification of 'rural' is most appropriately described within the context of people, culture, environment, and healthcare access13. Past research on rural health has painted a narrow picture of rural life. As a consequence, research focused on rural health and prevention typically describes the rural environment as a detriment to the health of individuals.
Encouraging self-management may be important in rural communities for a variety of reasons. The effect of chronic diseases on morbidity and mortality is disproportionate in rural populations and other underserved groups when compared to the rest of the USA14. It has been suggested that self-management may be important in rural areas for a variety of reasons. Preventive care is less available in rural towns, and rural areas tend to have fewer primary care physicians and specialty healthcare providers15,16. Rural residents are less likely to have insurance coverage and may be less educated about their chronic conditions3,14,17. Rural areas have a higher proportion of aging adults, the population most likely to be affected by chronic disease4,18,19. Studies have noted that a greater percentage of adults in rural communities report living with chronic pain and depressive symptoms, and that the number of chronic illnesses varies between farm-dwellers and town-dwellers in rural communities20,21. Based on these factors, it may be appropriate to provide programs to help rural residents self-manage their chronic conditions if necessary, as well as to offer a general chronic disease self-management program, rather than disease-specific programs, in rural settings.
Chronic Disease Self-Management Program
The CDSMP was developed and refined by researchers at Stanford University22 and has potential benefits for rural residents dealing with chronic healthcare issues23,24. The CDSMP was conducted from September 2007 to June 2009 and consisted of six weekly sessions (2.5 hours each) led by two trained lay leaders using a standardized leader manual that delineated the content and the process22. These six sessions emphasized the patient's central role and responsibility in managing his/her illness22. The program presented individuals who had chronic conditions with three types of self-management techniques: medical management, role management, and emotional management22. Topics addressed included exercise, cognitive symptom management techniques, nutrition, fatigue management, use of medication, and emotion management. It also taught the participants how to communicate with their healthcare providers, how to problem-solve, and how to make decisions about their health and health care25.
The CDSMP has been widely studied with a variety of populations, and results indicate that this program can be very effective at promoting self-efficacy, increasing the use of self-management behaviors, and improving health status while reducing hospitalizations and emergency room visits22,26,27. Although self-management programs such as the Chronic Disease Self-Management Program (CDSMP) are considered effective, not much literature is available regarding this program with rural residents25.
Understanding the challenges facing a rural population with chronic conditions offers greater meaning and relevance to community health research. Much more information needs to be collected about the participants' perceptions of the program and benefits in other rural communities. The purpose of this qualitative study is to conduct an in-depth examination of the perceived benefits that rural residents receive from participating in the CDSMP study. The specific aim of the project was to gain an understanding of the various types of self-management strategies used by individuals who completed the CDSMP, and how the CDSMP promoted behavior change in the respondents.
Design
The study was guided by a exploratory, qualitative data-collection method using focus groups. Focus groups were chosen for data collection because they could provide a rich source of information. For this study, focus group data were collected from a homogenous group of individuals (ie enrollees of the CDSMP) using a predetermined, structured sequence of questions in a focused discussion28. Pre-existing groups, such as support groups, form representational data because respondents have already shared a collective experience and have been shaped by a unique social context (ie chronic conditions)29. Using focus groups for this study was particularly important for understanding the qualitative articulation and relational expectations for interacting with other CDSMP group members.
Procedure
The eligibility criteria for participation required that the individuals: be 18 years of age or older; self-report at least one chronic condition; be currently enrolled in a chronic disease self-management program; and have no cognitive impairment, as determined by the site director at each of the data collection locations. Respondents were invited to participate in the focus groups in their community after completing the CDSMP. Each focus group was located at the same site that housed the program and was facilitated by the same skilled moderator. Six focus groups were conducted from January 2008 to August 2009.
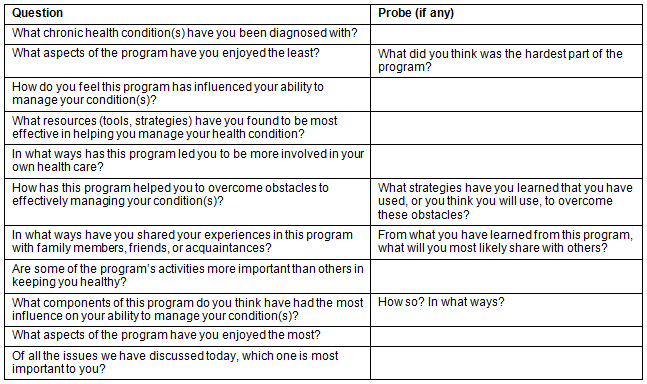
Before the first focus group, the moderator received approximately 10 hours of training in focus-group facilitation and reviewed the specific focus-group guides for this study. After describing confidentiality measures and obtaining written informed consent from the respondents, the moderator conducted the focus groups. Each focus group session lasted approximately 2 hours. The trained moderator began the focus group session with introductions and asked respondents to state their chronic conditions. Krueger and Casey's guide for conducting focus group sessions was used30. First, the topic to be addressed was introduced and then the respondents asked to briefly discuss their various chronic conditions and symptoms. Next, the respondents discussed how participating in this group helped them to manage their chronic conditions. Focus group interview questions are given in Table 1. Finally, the session moderator provided a summary of the findings after all the topics had been covered, and the respondents were asked to add any additional information they believed to be important and to comment on the accuracy of the reflection. Persons who attended a focus group session were given a $5 gift card to thank them for their involvement. All focus groups were audio-taped. Each session was transcribed verbatim by a research assistant and verified by a second research assistant.
Table 1: Focus group interview questions
Data analysis
Phenomenological and consensual qualitative approaches were used in the data analysis for the present study31,32. Of particular interest was capturing essential elements of the phenomenon (ie lived experience of completing the CDSMP) as narrated and given meaning to by the respondents. At the same time, the multiple perspectives of the research team members were honored by consensus.
To begin, the first author and a graduate research student read the initial transcript in its entirety to gain an overarching sense of the focus group sessions. Afterwards, the first author and a graduate research assistant read each transcript independently and identified units of phrases and sentences that emerged from their readings. Each person began analysis independently by inserting first-level codes in the transcript margins. To do the analysis, each reader bracketed the data by focusing on the phenomenon of interest (eg experience in a group program, context of disease management). Then, during team meetings, these individual codes were compared and contrasted to develop a coherent coding scheme. Through team analysis, the number of categories or themes were collapsed and refined to best reflect what the participants had reported. After the categorization was fully developed, the codes were analyzed to develop major themes. The team discussed each identified theme and highlighted exemplars for each theme to ensure that the respondents' experiences were captured and were not being solely guided by personal biases and assumptions. The team then developed a table reflecting the themes and exemplars from each transcript. Next, the team talked about agreed-upon themes. This portion of the process was similar to cross-analysis, as described by Hill et al31, but differed in that tracking the frequency of themes and subthemes was not a goal and therefore not documented. Instead, consistency in themes across transcripts reflected emerging meaning units of the phenomenon of interest33. Differing perspectives on themes were acknowledged and welcomed. Where disagreement existed, the authors engaged in a consensus process similar to that proposed by Hill et al31 to reach conclusions.
The final agreed-upon themes and raw data were compiled and given to an external qualitative auditor. The qualitative auditor was used to establish inter-rater reliability. The role of this external qualitative auditor was to confirm that multiple perspectives of the data were honored and discussed, and to help ensure that the analysts' assumptions, expectations, and biases did not unduly influence the findings31,32. An auditor with no connection to the study examined the themes and assessed their accuracy. In developing the themes, the auditor examined whether or not the findings, interpretations, and conclusions were supported by the data34. Upon completion of the auditor's review, the full team met and discussed the results of the study. An additional meeting of the primary team took place to review and discuss the auditor's feedback. This feedback included suggestions for additional themes and lack of consensus between some proposed themes and the raw data. The auditor's feedback was reviewed and incorporated, with changes based on thorough discussion and investigation. At the final stage of data analysis, the team discussed the final themes and arrived at conclusions. The extant literature was reviewed to determine the extent to which the study findings were consistent with those in the literature35. The analysis of the focus group session transcripts yielded two major themes: relational interaction in behavior change and self-reliant behaviors. Examples of results from the focus group sessions used verbatim wording.
Ethics approval
The Institutional Review Board at the University of Illinois at Urbana-Champaign approved all procedures for this research project; ethics approval IRB # 08089.
Profile of participants
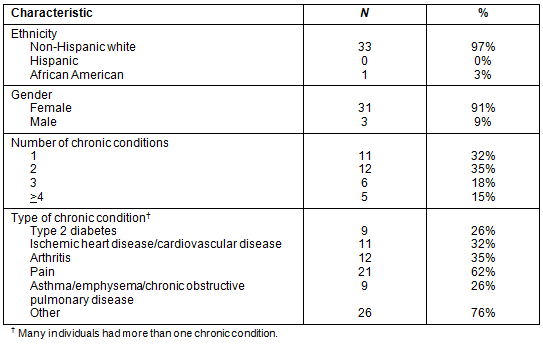
Thirty-four of the 45 individuals (75%) who completed the CDSMP participated in one of the six focus groups. The focus groups ranged in size from four to eight respondents, meeting the recommended size requirements suggested by Kitzinger36. Adult ages were 31-81 years, with an average age of 64.29 years (standard deviation (SD) = 10.24 years). The majority of the sample was non-Hispanic white (97%) and female (91%). Forty-two percent were widows, 39% were married, and 19% reported being either divorced or never married. As expected, 68% of the respondents reported two or more chronic conditions. Approximately 85% of the respondents reported having two or more chronic conditions. Most of the respondents had osteoarthritis (35%), followed by cardiovascular disease (32%), type-2 diabetes (26%), and chronic obstructive pulmonary disease (COPD)/emphysema (7%)(Table 2).
Table 2: Sociodemographic characteristics of focus group participants (N=34)
Themes
Findings from the focus group sessions were presented using verbatim comments (ie themes are presented without grammatical correction); however, names were changed to maintain focus group confidentiality. Themes relevant to the articulation of behavior change were the focus of the current study: self-management strategies and self-regulatory activities.
Respondent interaction in behavior change: Many of the focus group members discussed living with chronic illnesses day after day, as well as the importance of supportive relationships in the face of addressing these chronic conditions. They noted the need to have someone who was a strong advocate for them and the importance of having someone in their lives who is knowledgeable about chronic conditions. Peer relationships with persons who have chronic conditions can provide an opportunity to identify with similar individuals who are currently making positive health changes. The two major behavior changes noted in this study were increased physical activity and improved eating habits. Within three of the six focus groups, respondents discussed how the weekly meetings supported and encouraged them to increase their levels of exercise. The most mentioned form of physical activity was walking:
[The support group members] got me out to walk. I can't be too physical because of my arthritis, but I go out and walk. (Daisy, focus group 1, diagnosed with chronic obstructive pulmonary disease and osteoarthritis)
The focus group members discussed how the social interactions in this program created a community of learners who were empowered to improve their health behaviors. An example of the positive aspects of the CDSMP was the interrelationship between collective knowledge and supportive relationships. Respondents in another focus group discussed how they encouraged one member to identify the challenge to walk for weight reduction:
Walking ... I have had type-1 diabetes since I was 15 so I have had that for 25 years. And then in the last 3 or 4 years, they said that I have type-2, also because of your weight gain, maybe like 100 pounds over the course of the years, the last 4 years. (Natalie, focus group 6, diagnosed with juvenile type-1 diabetes and adult onset type-2 diabetes)
We cheered you on [speaking to Natalie] because we thought you were doing wonderful, you are up to 5, right? Five days. (Wynn, focus group 6, diagnosed with reflex sympathetic dystrophy syndrome)
I started out with 10 minutes, then 20, then 30. (Natalie, focus group 6)
Your very first action plan was how many days? Three? (Jasmine, focus group 6, diagnosed with type-2 diabetes)
Three, 10 minutes. Keep on exercising ... The doctor got on me and said if I lose 100 pounds and didn't have the weight, I would be able to not take some of these medications. I think maybe it is still in the back of my head and I just need to be proactive. I always say this. But I guess it was a start. [I started] walking like that was after we started the class. (Natalie, focus group 6)
Another focus group member described how small changes improved her physical activity levels. Respondents reported they improved their fitness level as they continued with the program. They also recounted that they were confident that they would continue to exercise even when the program ended:
Well, for me, it was the exercise. I've never been a person to do any exercise, which is probably where my biggest problems are. But with my diabetes, they [doctors] told me that I needed to lose weight ... I just needed to walk. And I have done that because of this class. (Nina, focus group 2, diagnosed with type-2 diabetes)
The focus group members mentioned their social environment and the positive influences of the social environment on health-related decisions and behaviors. In particular, reporting back to the group, regarding action plans each week, encouraged the respondents to adhere to their lifestyle changes:
Reminding me and making sure I do the exercises I signed up to do. I don't have an answer for it [group laughs]. (Mary, focus group 5, diagnosed with fibromyalgia)
Someone's checking on us [laughing]. (Naomi, focus group 5, melanoma cancer survivor)
Yes, when you know you're being checked on, you're more active. (Mary, focus group 5)
Participants also mentioned changes in their eating habits - improved skills to choose healthy foods and learning about portion control - which helped them stabilize the symptoms of their chronic condition. The focus group members briefly discussed self-monitoring their dietary habits by improving their selection in food choices. The reinforcement of healthy eating, both through discussions and by example from the lay leaders, appeared to have a positive influence on some of the participants:
Well, it is basically portion control and carbohydrates and the exercise. (Tim, focus group 6, diagnosed with type-2 diabetes)
So do you see more instant response then, or are you better able to understand for you what keeps that down? (moderator)
Yes, even when I went uptown this last weekend, I went to two buffets and I made a point to keep my carbohydrates down. I may have eaten a little too much protein, but I made a point to keep the carbs down ... Before, I think we discussed it in class, I had a great fear of taking insulin shots so I didn't check it. Well, if you don't check it, you don't know what it is, but I took self-management and said I'm going to start doing it and I did it [applause from group], and I said to the group, if I didn't have this course, I didn't know if I would still have done it. But finally it was an acceptance that I had to do it. (Tim, focus group 6)
Although limited resources challenge managing chronic conditions in rural areas, the respondents made the time to participate in preventive health events. To reinforce health-seeking nutritional behaviors, the peer leaders brought healthy food to the weekly meetings:
The healthy foods that they brought in ... I have been looking for some of the stuff like some of the nuts, vegetables, fruit ... the good stuff for you. (Penny, focus group 3, diagnosed with chronic pain, fibromyalgia and chronic fatigue syndrome)
[Group leader] brought some of the food in and we're all appreciative of it. And I was determined to stop at the health food store and get some raw nuts ... [Group leader] brought in stuff every week ... soy dip, tofu. (Gilda, focus group 3, diagnosed with chronic pain)
The respondents supported each other through a variety of cooperative learning strategies. These strategies empowered the group to make health behavior changes (in relation to exercise and diet) using healthy practices. The focus group members understood the need to change their eating habits and physical activity levels. However, they often felt they were not able to make the changes until they had a supportive network of peers who were struggling with the same issues.
Prioritizing health behavior change: As expected, the focus group members used different strategies to manage their chronic health problems. Common strategies noted by the participants included breaking down goals into smaller tasks and increasingly monitoring their health and behaviors. Action planning was the most discussed strategy used to monitor chronic conditions and change health behaviors. Making plans for the week was encouraged, even required, in the CDSMP, with respondents helping each other brainstorm ways that they could achieve their goals. Participants believed that action plans helped them to take responsibility for their own health. They each noted that it was important to listen to their body and to understand the meaning of cues that provided personal patterns of health and wellbeing:
The sessions helped me to refocus. I can only have self-discipline for short periods of time and then I kind of fall off and don't do it, and then I need to get refocused and start in again and do it again and become self-disciplined again for however long that lasts. So this helped me to refocus and start doing the things I know I should be doing. (Lawrence, focus group 5, diagnosed with type-2 diabetes)
I think it helped us focus or helped me focus on things that I could do to help myself. (Janice, focus group 5, diagnosed with hypertension)
Well, as a diabetic, the exercise and the eating properly, I mean, is directly related to the lower blood sugar readings and lack of complications from the disease. So, yes, it's very important to keep that up. (Lawrence, focus group 5)
Individual and community self-reliance was an important rural value pertaining to health. Several focus groups members described how the CDSMP emphasized autonomy, which allowed them to monitor and regulate actions toward their goals through information acquisition, expanding expertise, and self-improvement. They mentioned the importance of being prepared to deal with their illness. Each focus group member was cognizant of his/her strengths and weaknesses, as well as the ability to build a repertoire of strategies to use to tackle health situations that might arise. This conversation between two focus groups members showed how they managed their health problems on their own. It demonstrates how the small goals established by the participants - such as those identified in their weekly action plans - helped make changing their health behaviors seem more manageable:
The program has helped me considerably in one [respect], [in that] I now break things down to things I can handle instead of being overwhelmed. Because when we first talked, they said, and the book also said that if you can't walk about 10 steps what [about] 5 until you feel good about it, then you try 6 steps, 7 steps. And that is now my approach to almost everything now. If I can't walk the two miles like I had promised, then I walk one mile and feel good about it rather than feel depressed and have an anxiety attack because I didn't do the two miles ... So I feel good about myself when I'm able to do things ... It has been a lot of help to me. Just little steps, little goals that eventually you hope to work up to big goals. (Tim, focus group 6, diagnosed with type-2 diabetes)
You have to take one day at a time. I'm learning that even though I have the chronic pain, I have so much guilt and frustration and I have to take the meds, and I get tired of going around in circles and circles. I'm learning that the pain is going to be there no matter what. I'm learning to work with things day-by-day, step-by-step, around the pain instead of the pain working into my lifestyle ... I want to be able to do things, yes it does, and it is not going to happen overnight. It didn't get here overnight and it is not going to go away overnight. By using these planning steps in this toolbox that we have, it has helped me a lot to stick with the plans I say I'm going to do. It has really opened my eyes to say wow! It's just a fantastic feeling. (Pamela, focus group 6, diagnosed with chronic pain)
One of the main goals of enhancing self-regulatory activities among individuals with chronic health issues is to improve their health behaviors. Participants in this study articulated a variety of behavioral changes that they considered relevant to their health and wellbeing and that resulted from their participation in the CDSMP. They made concrete references to health behavior changes, such as reporting weight loss, monitoring glucose levels, and managing pain. Of course, specific self-regulatory activities varied among the participants. However, each activity seemed to have produced a personalized achievement in the health outcome. One man's vivid description of his major achievement illustrates him finding solutions to meet his healthcare needs:
[My glucose level] is down to 141; it started at 300 [and] I dropped it within less than a week ... And I thought I was doing all that right before I read my blood sugar so I lost 5 pounds. I figured if I lost another 5 to 10 pounds, I'll get even more control. (Tim, focus group 6)
In these discussions of focus groups 5 and 6, the respondents told their stories about their health-seeking behaviors, problem-solving mastery, and action plans to deal with and cope with their various conditions. The respondents found these skills to be beneficial, and they noted that they would continue to use them after the program had ended.
In this qualitative exploratory study of rural residents in the Chronic Disease Self-Management Program, two key themes emerged that provided useful information for understanding the factors used to promote behavior change and the strategies rural individuals learned from participating in the program. Although opportunities for health promotion in rural communities are limited37, the importance of health promotion and interpersonal relationships was clearly seen, with the focus group participants as significant facilitators of behavioral change. Similar to other research findings, a positive link between social support and health promotion was discovered38-40. This study found that the respondents became more engaged as the program progressed. The participants became more comfortable expressing their feelings and frustrations regarding their disease experience without censoring their thoughts. Consequently, they felt more support among the group members. This may be particularly important in rural communities where individuals may feel more socially isolated19. Several of the respondents stated they felt their CDSMP group was a safe and comfortable space to share feelings about their conditions.
Considerable evidence suggests that the adoption of healthy behaviors by individuals is a necessary component in the management of chronic conditions, and personal beliefs have been linked to the adoption of healthy behaviors41-44. In terms of behavioral changes, the present qualitative study found that self-management practices included two behaviors: physical activity and healthy eating habits. The improvement in some areas of health behavior demonstrated potential benefits of the program for rural adults. Rural researchers who have implemented CDSMP with adults residing in rural communities have found positive findings23,24. Similarly to the current study, Jaglal et al. found that participants experienced significant changes in their self-efficacy, health behaviors (eg in relation to exercise, cognitive symptom management, and communication with physicians), social role function, psychological wellbeing, energy and fatigue levels, health distress, and self-reported health after participating in a tele-CDSMP23. Stone and Packer24 also found an increase in exercise post-implementation of the CDSMP in rural areas of Australia. Other CDSMP studies also found that respondents benefited from participating in the program, in particular by increasing exercise behaviors45,46. Exercise (eg walking) was one of the areas in which many of the rural respondents in this study focused on changing, and focused on this behavior change in their action plans. The potential ability for CDSMP to increase the physical activity of rural adults is important given the research that suggests this population typically engages in lower levels of physical activity than suburban- and metropolitan-dwelling adults3. In addition, given that rural communities often have limited facilities to promote or support physical activity, it is important to note that the majority of program participants noted walking as their form of exercise, which does not require this type of resource. One area where participants noted improvements in this study that has not been present in other studies was healthier dietary habits23,24,46. This health behavior change is important given research that suggests rural adults generally sustain unhealthy nutritional diets3.
The benefits of the CDSMP included prioritizing behavior change, which increased self-regulatory activities. Many participants verbalized how they enjoyed using these newly developed skills and stated that they felt better as a result of using them. Similar to those of Stone and Park24 this study's findings indicate that the individuals reported significant improvements in self-monitoring and insight, as well as health service navigation, as a result of their participation in the program24,45. Similar to findings of Fu et al45, the focus group members felt that goal-setting, as well as getting advice from other group members, helped them to follow their specific plan for the following week. Although opportunities for health promotion in rural communities are limited37, the importance of prioritizing behavior change was clearly seen with the focus group members. However, it is important to note that this study did not collect follow-up data; it is therefore not known if the behaviors were sustained after the completion of the program.
Research suggests that adults in rural communities are receptive to health prevention and promotion programs that assist with the management of their chronic conditions. Potvin et al. found that rural individuals who had a chronic condition were twice as likely as adults residing in inner cities and suburbs to be at a stage closer to 'action' in terms of self-care6. Their results indicated that rural individuals with chronic conditions might be more ready to change their behaviors to promote their health. Another, more recent, study47 noted that while time is a barrier to involvement, rural adults diagnosed with a chronic condition made the effort to participate in preventive health events, and these adults understood the value of preventive health services in managing their illness47. Given all the barriers to health promotion faced by rural individuals, and potential interest of these individuals in learning more about preventive health measures and management of chronic conditions, dissemination and evaluation of programs and information in these areas are crucial.
The principal limitation of this study was the use of qualitative methodology. Focus groups, which are recognized as valuable in soliciting individuals' viewpoints in a non-judgmental, unbiased environment, tend to generate responses through deductive reasoning. However, because the focus groups were conducted using a small, non-randomly selected convenience sample, the ability to generalize the findings of the focus groups to a larger population is limited. However, generalizability is rarely the goal of focus groups. Because respondents are rarely randomly selected, it is not possible to take inferences from data to a larger population due to the bias of the respondents choosing to participate in the focus group. Additional studies are needed in a variety of settings to determine whether or not people with chronic conditions experience the benefits, as noted by this study's respondents. Another limitation was the lack of ethnic/racial diversity within the sample. With 97% of the focus groups being non-Hispanic whites, it is impossible to generalize these findings to a diverse population of rural adults.
Acknowledgements
The University of Illinois Extension Service supported this project. The authors wish to thank graduate research assistants Meredith Schwartz and J. Michael Wallace for transcribing the focus group members' interviews and analyzing the qualitative data. The authors also wish to thank Drs Laura Payne and Robin Orr (posthumously), as well as the coordinators, master trainers, workshop leaders, and volunteers who made the program.
References
1. Anderson G. Chronic care: making the case for ongoing care. (Online) 2010. Available: http://www.rwjf.org/content/dam/farm/reports/reports/2010/rwjf54583 (Accessed 28 May 2013).
2. Schneider KM, O'Donnell BE, Dean D. Prevalence of multiple chronic conditions in the United States Medicare population. Health & Quality of Life Outcomes 2009; 7(82): 82-92.
3. Smith KB, Humphreys JS, Wilson MGA. Addressing the health disadvantage of rural populations: how does epidemiological evidence inform rural health policies and research? Australian Journal of Rural Health 2008; 16(2): 56-66.
4. McManus MM, Norton CH. Background tables on demographic characteristics, health status, and health services utilization. Health Service Research 1989; 23(6): 725-756.
5. Mainous AG, Kohrs FP. A comparison of health status between rural and urban adults. Journal of Community Health 1995; 20(5): 423-431.
6. Potvin L, Gauvin L, Nguyen MN. Prevalence of stages of change for physical activity in rural, suburban and inner-city communities. Journal of Community Health 1997; 22(1): 1-13.
7. Clark NM. Management of chronic disease by patients. Annual Review of Public Health. 2003; 24(1): 289-313.
8. Kane RL, Kane RA. Emerging issues in chronic care. In: Binstock RH, George LK (eds). Handbook of aging and the social sciences. 5th edn. Binghampton, NY: Academic Press, 2001; 406-425.
9. Coleman K, Austin BT, Brach C, Wagner EH. Evidence on the chronic care model in the new millennium. Health Affairs 2009; 28(1): 75-85.
10. Clark NM, Becker MH, Janz NK, Lorig KR, Rakowski W, Anderson L. Self-management of chronic disease by older adults: a review and questions for research. Journal of Aging & Health 1991; 3(1): 3-27.
11. Von Korff M, Gruman J, Schaefer J, Curry SJ, Wagner EH. Collaborative management of chronic illness. Annals of Internal Medicine 1997; 127(12): 1097-1102.
12. Bushy A. Women in rural environments: consideration for holistic nurses. Holistic Nursing Practice 1994; 8(4): 67-73.
13. Phillips CD, McLeory KR. Health in rural America: remembering the importance of place. American Journal of Public Health 2004; 94(10): 1661-1663.
14. Farrell K, Wicks MN, Martin JC. Chronic disease self-management improved with enhanced self-efficacy. Clinical Nursing Research 2004; 13(4): 289-308.
15. Andrus MR, Kelley KW, Herndon KC. A comparison of diabetes care in rural and urban medical clinics in Alabama. Journal of Community Health 2004; 29(1): 29-44.
16. Dansky KH, Dirani R. The use of health care services by people with diabetes in rural areas. Journal of Rural Health 1998; 14(2): 129-137.
17. Hartley D, Quam L, Lurie N. Urban and rural differences in health insurance and access to care. Journal of Rural Health 2008; 10(2): 98-108.
18. Bethea TN, Lopez RP, Cozier YC, White LF, McClean MD. The relationship between rural status, individual characteristics, and self-rated health in the behavioral risk factor surveillance system. Journal of Rural Health 2012; 28(4): 327-338.
19. Baernholdt M, Yan G, Hinton I, Rose K, Mattos M. Quality of life in rural and urban adults 65 years and older: findings from the National Health and Nutrition Examination Survey. Journal of Rural Health 2012; 28(4): 339-347.
20. Jones C, Parker T, Mishra A, Ahearn M, Variyam J. Health status and health care access of farm and rural populations. (Online) 2009. Available: http://www.ers.usda.gov/media/155453/eib57_1_.pdf (Accessed 24 May 2013).
21. Ploncyznski DC, Yao P, Hartman J, West M, Salacinski A, Mannion M. Interpersonal and background influences on health promotion of older rural adults. Journal of Rural Community Psychology 2012; E15(1): 1-15.
22. Lorig KR, Gonzalez VM, Laurent DD. Chronic disease self-management workshop leaders manual (revised). Stanford, CA: Stanford University, Stanford Patient Education Research Center, 1999.
23. Jaglal SB, Haroun VA, Salbach NM, Hawker G, Voth J, Lou W, et al. Increasing access to chronic disease self-management programs in rural and remote communities using telehealth. Telemedicine and e-Health. 2013; 19(6): 467-473.
24. Stone G, Packer TL. Evaluation of a rural chronic disease self-management program. Rural and Remote Health 2010; 10(1): 1-14.
25. Cudney S, Sullivan T, Winters CA, Paul L, Oriet P. Chronically ill rural women: self-identified management problems and solutions. Chronic Illness 2005; 1(1): 49-60.
26. Lorig KR, Ritter PL, Stewart AL, Sobel DS, Brown BW, Bandura A, et al. Chronic disease self-management program: 2-year health status and health care utilization outcomes. Medical Care 2001; 39(11): 1217-1223.
27. Lorig KR, Ritter P, Gonzalez VM. Hispanic chronic disease self-management: a randomized community-based outcome trial. Nursing Research 2003; 52(6): 361-369.
28. Kohler CL, Dolce JJ, Manzella BA, Higgins D, Brooks CM, Richards JM, et al. Use of focus group methodology to develop an asthma self-management program useful for community-based medical practices. Health Education & Behavior 1993; 20(3): 421-429.
29. Wilkinson S. Focus groups. Psychology of Women Quarterly 1999; 23(2): 221.
30. Krueger RA, Casey MA. Focus groups: a practical guide for applied research (4th edn). Thousand Oaks, CA: Sage Publications, 2009.
31. Hill CE, Thompson BJ, Williams EN. A guide to conducting consensual qualitative research. The Counseling Psychologist 1997; 25(4): 517-572.
32. Hill CE, Knox S, Thompson BJ, Williams EN, Hess SA, Ladany N. Consensual qualitative research: an update. Journal of Counseling Psychology 2005; 52(2): 196-205.
33. Creswell JW. Qualitative inquiry and research design: choosing among five approaches (2nd edn). Thousand Oaks, CA: Sage Publication, 2007.
34. Creswell JW. Qualitative inquiry and research design: choosing among five approaches (3rd edn). Thousand Oaks, CA: Sage Publications, 2013.
35. Patton MQ. Qualitative evaluation and research methods (3rd edn). Newbury Park, CA: Sage Publications, 2002.
36. Kitzinger J. Qualitative research: introducing focus groups. British Medical Journal 1995; 311(7000): 299-302.
37. Williams RD, Lehbridge DJ, Chambers WV. Development of a health promotion inventory for poor rural women. Journal of Family and Community Health 1997; 20(2): 13-23.
38. Glass TA, Dym B, Greenberg S, Rintell D, Roesch C, Berkman LF. Psychosocial intervention in stroke: families in recovery from stroke trial (FIRST). American Journal of Orthopsychiatry 2000; 70(2): 169-181.
39. Hurdle DE. Social support: a critical factor in women's health and health promotion. Health and Social Work 2001; 26(2): 72-79.
40. Adams MH, Bowden AG, Humphries DS, McAdams LB. Social support and health promotion lifestyles of rural women. Journal of Rural Nursing and Health Care 2000; 1(1): 28-40.
41. McAuley E. Self-efficacy and the maintenance of exercise participation in older adults. Journal of Behavioural Medicine 1993; 16(1): 103-113.
42. Sallis JF, Pinski RB, Grossman RM, Patterson TL, Nader PR. The development of self-efficacy scales for health related diet and exercise behaviors. Health Education Research 1988; 3(3): 283-292.
43. Barlow J, Wright C, Sheasby J, Turner A, Hainsworth J. Self-management approaches for people with chronic conditions: a review. Patient Education and Counseling 2002; 48(2): 177-187.
44. Chen K, Chen M, Lee S, Cho H, Weng L. Self-management behaviours for patients with chronic obstructive pulmonary disease: a qualitative study. Journal of Advanced Nursing 2008; 64(6): 595-604.
45. Fu D, Ding Y, McGowan P, Fu H. Qualitative evaluation of chronic disease self management program (CDSMP) in Shanghai. Patient Education and Counselling 2006; 61(3): 389-396.
46. Rose MA, Arenson C, Harrod P, Salkey R, Santana A, Diamond J. Evaluation of the chronic disease self-management program with low-income, urban, African American older adults. Journal of Community Health Nursing 2008; 25(4): 193-202.
47. Murimi MW, Harpel T. Practicing preventive health: the underlying culture among low-income rural populations. Journal of Rural Health 2010; 26(3): 273-282.
