Background
One hundred years ago in the USA, Abraham Flexner introduced a 'reform' of medical education that standardised medical training. He defined the role of the 'Academic - with a research role' as being responsible for training future doctors and suggested that private clinicians with the pressures of practice would have insufficient time to teach1. Unwittingly these reforms were to produce the divide that currently exists between clinicians and academics today2.
Medical education in Australia largely followed a similar path. The traditional structure of medical schools focused on large specialised teaching hospitals in capital cities as the way to deliver medical education. Senior university-funded staff progressed their academic careers via sub-specialised research. The structure of medical education and training has been identified as one of the key reasons for a mal-distribution of the medical workforce in Australia where in 1998 there were only 15.6% who worked in rural and remote areas caring for 28.7% of the population3.
In the last decade there has been a multitude of Australian Government programs aimed at increasing and retaining the medical workforce in rural settings in Australia3. Most recently, the Federal Government has funded UDRHs and Rural Clinical Schools (RCS) in an effort to decentralise the delivery of medical education, and in so doing increase the future rural medical workforce. The UDRH northern New South Wales is a multidisciplinary academic department of the Faculty of Health of the University of Newcastle and was established in 2001 in Tamworth4. Its brief includes allied health, research, health promotion and innovative clinical service delivery. The delivery of undergraduate medical education is a priority of UDRH.
In 2001, there were two groups of eight students who completed their 'country term' in Tamworth. It was determined that the UDRH would attempt to teach the entire fourth year curriculum in Tamworth as an educational pilot program in 2002. Four students who came to Tamworth in 2001 as third year students and an additional two students volunteered for the pilot program. So successful and popular with the students and the teachers was the program that all six students from 2002 asked if it would be possible for them to stay in Tamworth for their final year in 2003. This article will describe how curriculum delivery was achieved and adapted to enable effective local delivery.
Tamworth area
Tamworth is a regional centre with a population of 55 000 in the expanded local government area that includes all small villages within a 20 km radius of the town centre. Tamworth, located 30 km north-west of Newcastle, is the largest centre in New England, a region of northern New South Wales with a population of 175 000. Tamworth Base Hospital is a 254 bed general hospital facility offering most services, aside from cardiac and neurosurgery. It is the referral hospital for the New England region. The hospital is staffed by 13 staff specialists and has 30 visiting specialists who reside locally and another 32 local general practitioners who all have admitting rights to the hospital. The House staff consist of 10 interns, 10 first year residents and a further 20 senior resident, registrar and career medical officer staff. The hospital has a busy accident and emergency department, treating 35 000 patients, including 10 000 children, annually.
The clinical program of Newcastle University Medical School
The final two years of the bachelor of medicine program consist of 36 weeks of integrated clinical attachments and approximately 3-4 weeks for written and clinical assessments each year. The attachments include: medicine, paediatrics, reproductive medicine, psychiatry, anaesthetics, intensive care, palliative care, general practice, oncology and surgery. Specific details of the medicine program can be found through the University of Newcastle's website (http://ccdb.newcastle.edu.au/courseinfo).
Selection of initial students into rural cohort
It was determined that Tamworth Base Hospital would be a suitable site for a group of 6-8 students who would undergo the pilot program. The principles of the program were set out in an internal faculty document4 which stated:
- That students based in Tamworth would receive the same amount teaching as those students who were attached to John Hunter Hospital in Newcastle.
- Wherever possible, local clinicians would deliver the tutorials that made up the program.
- That academics from the disciplines based in Newcastle would offer the local clinicians assistance in the delivery of the tutorials.
- That students would have the same access to the Internet and Newcastle Library resources as do Newcastle students.
- That assessments would take place locally and that Newcastle-based academics would co-assess with Tamworth-based clinicians to ensure standardised results were obtained in the 'viva' examinations.
- That participation in the program would be voluntary and that students would be allowed to return to the Newcastle-based program at any stage of the year for any reason, if they chose.
To act as an incentive for the first cohort of students to volunteer, a scholarship worth AU$2500 per annum was offered. Students were responsible for their own accommodation arrangements. The UDRH assisted students in setting up private rental accommodation. There were six volunteers for the first cohort of students. Two students had their secondary education in the New England area, two from rural Queensland, one from state capitals Brisbane and Sydney. One Indigenous student had completed a degree prior to entry in medicine, one transferred after one year of occupational therapy and four had no prior tertiary experience before entry into the Newcastle program. All six students had successfully completed the first 3 years of the degree in Newcastle without failure. The average age at the time of completion of the medicine program was 24.6 years.
Delivery of the program
The fourth year program in 2002 in Tamworth required organising 322 h of teaching sessions (Figure 1). These sessions included a mixture of fixed resource sessions, bedside tutorials, case-based discussions and problem-based learning tutorials. The details of the course can be found on the faculty web page (www.newcastle.edu.au/health). There were an average of 8.9 h of organised teaching sessions each week of the 36 week program. In addition, students completed clinical clerkships in medicine, paediatrics, reproductive medicine and surgery.
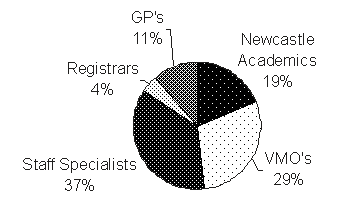
Figure 1: Distribution of staff who taught 322 scheduled teaching hours of the 4th year program in Tamworth in 2002. VMO, Visiting medical officer.
All sessions were delivered locally. Twenty percent of the sessions were delivered by Newcastle-based academics. The course delivery was supported through 13 visits by Newcastle staff in the first two rotations, and via a weekly 2 h video-conference case-based tutorial in the final rotation. A video-conference link between Tamworth and Newcastle was established at the end of the second rotation in July 2002. The UDRH successfully recruited 40 of the local senior medical staff (60% of all doctors working in Tamworth) to deliver tutorials to the students. A formal partnership agreement was reached between New England Area Health Service (NEAHS) and the UDRH which allowed NEAHS to participate as teachers in the program while being paid by NEAHS.
There is no direct air link between Tamworth and Newcastle. The distance of 300 km is a 3.5 h drive. The most cost- and time-efficient method of transport was to offer Newcastle academics a hire car with driver at a cost of approximately $550 per visit. This allowed the visiting academics to spend up to 5 h in Tamworth teaching and networking with local clinicians. It also allowed for more than one academic to visit at once at no extra cost. This method compared favourably with air transport via Sydney which takes 4 h and costs $780 per passenger, plus taxi fares. Videoconferencing in 2002 was via a 384 Kb ISDN link that cost approximately $100/h to run.
An offer to remunerate private medical practitioners employed as casual academics was made to encourage the participation of the local medical community at either Visiting Medical Officer (VMO) rates or General Practice divisional rates of between $110 and $140 per hour. It is interesting that only 50% of the private medical practitioners claimed payment for the delivery of teaching sessions. Local clinicians who agreed to teach various sessions were put in contact with the relevant Newcastle academic who would help them ensure the content they were delivering to the Tamworth-based students was adequate.
In total, the extra teaching costs associated with the delivery of the fourth year program to engage the combination of teaching staff (Figure 1) was $20 000. There was $15 000 spent on scholarships to help students with the cost of private rental accommodation. The collection of the library of Tamworth Base Hospital was upgraded and automated and linked to the University of Newcastle collection at a cost of $40 000 in 2002. The key academic support included the appointment of the director, executive officer, secretary and the education co-ordinator as well as the fit-out and establishment of a video-conferencing link and tutorial room in Tamworth.
Multi-professional education in Tamworth
At the same time as the fourth year medical student program was being established, the Faculty of Health was establishing long-term clinical placements in the final year of the Occupational Therapy, Radiography and Dietetic programs in Tamworth. Consequently, there were approximately 20 senior health students from a range of disciplines co-located in Tamworth, thus providing the opportunity to trial the delivery of several multi-professional learning modules where the students have learned and developed key competencies and skills together. In 2002, the fourth year students participated in a module in clinical ethics5, and the 2003 fourth year medical students participated in modules in communication, child protection6 and medical error7. The multi-professional aspects of training have largely dealt with professional and personal development aspects of health care. The workforce impact of this team approach is already evident. Upon graduation, seven of these allied-health students chose to commence work in New England in 2004.
Student assessment
Students were assessed in Tamworth. They underwent the same assessment procedures as the students in Newcastle. The students were assessed by a pair of examiners in each long-case viva. Local clinicians assessed with the Newcastle based academics to standardise the results. If students were not satisfactory at first assessment they were automatically allowed to re-sit the viva at the end of the year. Students must pass all four vivas to be allowed to progress from fourth to final year. Students completed long cases in medicine, surgery, paediatrics and reproductive medicine in 2002. All the fourth year students based in Tamworth in 2004 received a satisfactory result in their long-case vivas at first assessment, compared with a 20% rate of students based in Newcastle being assessed 'not satisfactory' in at least one of the four long-case vivas. In 2003 students completed long-case vivas in interactional skills, medicine and psychiatry. Five of the students completed all four of their clinical rotations in Tamworth and one student completed one clinical rotation in intensive care at the John Hunter Hospital and the other three rotations in Tamworth. In 94% of assessments (17 of 18), students were 'satisfactory' at first assessment with one student passing the medicine viva at second assessment. In 2003, the Newcastle-based academics co-assessed via video-conference. All students passed their final written and objective structured clinical evaluation (OSCE) examinations at first assessment.
Student feedback and outcome
In 2002, the six students were asked to provide feedback at the end of each 12&3160;week clinical rotation using a 5 point Likert scale. A total of 222 teaching sessions were assessed by the six students, 5 sessions were rated as unhelpful (score 4, 5), 22 sessions were rated as a score of 3, and 195 items (88%) were rated as helpful or very helpful (score 1 or 2).
Three major themes emerged from the written comments. The students appreciated the ease with which they had access to patients. They also valued the personal nature of the tutorials. Video-conferencing sessions were not as popular as the sessions where the tutor was teaching face to face. All six students were very keen to return to Tamworth in 2003 to complete their medical studies. In 2003, the feedback from the students was similar to 2002, with 100% of the qualitative feedback being very positive.
In 2004, two of the six students chose to complete their internship in Tamworth. One student each is completing internship in Canberra, Adelaide, Brisbane and Newcastle. Each students will be tracked to determine the effect of completing their undergraduate training in Tamworth on their career choices.
Discussion
The experience discussed in this article demonstrates that it is possible for students to sucessfully complete the entire clinical component of their undergraduate medical training in a large regional town. The Commonwealth Government has challenged medical schools to make it possible for 25% of their students to achieve 50% of their clinical training in the rural sector by 2004. Other medical schools have used different approaches to meet this challenge. Clinical schools were established in Townsville and Darwin during the 1990s. These regional cities have larger populations and significant university campuses.
Further RCS have successfully used primary care as the major vehicle for the delivery of the curriculum8, or a patient-based approach where students learn by longitudinally following clinical cases in detail9. The Tamworth experience demonstrates that a 'traditional' teaching hospital curriculum can be delivered effectively with a high level of student satisfaction and academic success, by decentralising resources and taking advantage of the underutilised academic capacity in large regional referral centres. The regional town is able to provide students exposure to 'general specialists' as well as primary care in the community, to give a broader view of health care. Newcastle University's success should provide considerable encouragement to medical schools, clinicians, students and policy makers involved in this significant national undertaking.
This multidisciplinary approach has been well accepted by the community of Tamworth, and this has enabled the program to recruit tutors from a wide range of disciplines.
It is hoped that involving over 40 local clinicians is more sustainable than relying on only a select few. Because each was required to teach a small amount, and this teaching was funded, the impact of any one clinician leaving Tamworth should not destabilise the program. The director was the only full-time Department of Education, Science & Training (DEST) funded clinical medical academic in Tamworth. He has a broad range of responsibilities and was only required to teach 10% of the students sessions. The effectiveness of a structure which values the time and effort of its clinical teachers can not be underestimated. The program, however, relied on the willingness of the Newcastle-based academics to allow local clinicians access to the academic materials that underpinned locally delivered tutorials.
As local capacity and confidence increases, one challenge in coming years will be to maintain sufficient links between the clinical staff in Tamworth and Newcastle, to ensure consistency of the basic curriculum.
With the continued development of UDRH and RCS in regional towns, it is important that the issues of student capacity are recognised so the same problems of over-crowding of teaching hospitals in metropolitan areas are not repeated in Tamworth and other towns. To date, the Tamworth program has been sucessful with volunteer students. This has resulted in 10-12 clinical medical students in Tamworth at any one time. This appears to be sustainable in the longer term.
Conclusions
Developing a sustainable health professional workforce in regional and rural areas is one of the key long-term outcomes of programs such as the Newcastle University UDRH. The multi-professional platform of the Newcastle program has meant that outcomes are being seen across several disciplines within 2 years of commencing operations. The challenge for the UDRH is to grow each of these innovations to the level where they are sustainable.
International evidence suggests that undertaking medical training and living in a rural area is the best way to address the issue of recruiting medical staff in the long term10,11. This pilot data from the Newcastle program suggests that this may hold true across the professions, and that a broadening of the RCS concept should be considered across the breadth of health professions to achieve the best outcomes for health-service delivery.
References
1. Osler RA. Vindicated: the ghost of Flexner laid to rest. Journal of the Medical Association of Canada 2001; 164: 1860-61.
2. Barasanzky B. Abraham Flexner: lessons from the past and applications for the future. Beyond Flexner; medical education in the twentieth century. New York: Greenwood, 1992; 190.
3. Dunbabin J, Levitt L, Rural Origin and rural medical workforce exposure: their impact on rural and remote medical workforce in Australia. Rural and Remote Health 3: 212. (Online) 2003. Available: hhtp://rrh.org.au (Accessed 22 June).
4. Jones PD. Guiding principals of education placements in the University Department of Rural Health. Newcastle, NSW, Australia: Faculty of Medicine and Health Sciences, University of Newcastle, 2001.
5. Jones PD. The role of parternships in the development of Rural Based Curricula. In: Towards Equity in Education, Training and Health Care Delivery . Newcastle, NSW, Australia: The University of Newcastle, 2003; 54-55.
6. Cooper R, Brown L, Smith T, Dalton R, Walker J, Bull R. Meeting the Challenges of multi-professional education. In: Towards Equity in Education, Training and Health Care Delivery . Newcastle, NSW, Australia: The University of Newcastle, 2003; 162.
7. Brown L, Cooper R, Smith T, Jones P, Thornberry P, McPArlane J. Implementing Education in Child Protection for Rural Health Professional students. In: Towards Equity in Education, Training and Health Care Delivery . Newcastle, NSW, Australia: The University of Newcastle, 2003; 160.
8. Worley P, Silagy C, Prideaux D, Newble D, Jones A. The parallel rural community curriculum: an integrated clinical curriculum based on rural general practice. Medical Education 2000; 34: 558-565.
9. Sturmberg, Reid AL, Thacker JL, Chamberlain C. A community based, patient centred, longitudinal medical curriculum. Rural and Remote Health 3: 210. (Online) 2003. Available: hhtp://rrh.org.au (Accessed 22 June).
10. Wilkinson D, Evidenced based rural workforce policy: an enduring challenge. Rural and Remote Health 3: 224. (Online) 2003. Available: hhtp://rrh.org.au (Accessed 22 June).
11. Brooks RG, Mardon R, Clawson A. The Rural Physician Workforce in Florida: a survey of US and foreign born primary care physicians. Journal of Rural Health 2003; 19: 484-491.


