Millennium Development Goal 5 (MDG 5) is a global consensus to improve maternal health, aiming by 2015 to reduce the maternal mortality ratio (MMR) to three-quarters of the level of that in 1990. In Indonesia, however, in 2012 the MMR was 227 Indonesia wide1, still far from target of 102 per 100 000 live births. Skilled attendance at birth is an important strategy to reduce maternal mortality, particularly in low to middle income countries where most maternal deaths occur2-4. The utilisation of health services, including attendance for antenatal care, and health outcomes related to pregnancy and delivery, are determined by the social and environmental conditions of the places where people live5-7. Access to skilled birth attendants (SBAs) is a major concern in Indonesia8. Although there are different ways to measure this, geographic access is particularly relevant in rural areas and especially those in remote settings. Health services remain concentrated in central urban areas, and to reach these, many have to travel for extended periods from areas with poor road conditions and without public transport9.
Geographic analysis provides an invaluable tool to understand the spatial patterning of access to maternal health services and maternal health outcomes, Although research on spatial patterning has focused mainly on diseases rather than non-disease health conditions10-14, several studies have examined the association of maternal health outcomes with antenatal care, the demographic and socioeconomic characteristics of women, and types of birth attendance15-17. Studies in Zambia18-20, Kenya21, Ghana22 and Indonesia23 all indicate that proximity to health services increases the likelihood to deliver at a health facility although variations across the studies in the measurement of distance, perceptions of distance, and travel time all inhibit comparability. In Indonesia, delivery in rural villages commonly occurs at home with SBAs24, and in this context, in addition to distance to hospital for delivery, distance to nearest midwife needs to be taken into account to identify factors affecting their engagement at home deliveries.
While in general geographic factors are important, identifying clusters of health events has gained significance in population health13,25-28, because of the capacity of this approach to identify variations in environmental exposure, access, and the availability of health services. In addition, people and communities tend to cluster in space in systematic ways that may predict the risk of disease or another adverse health event29. Analysis using a geographic information system (GIS) enables public health researchers to explore geographic variations of both health behaviours and health outcomes, and so to examine geographic relationships between social and environmental factors pertaining to health outcomes. For example, understanding the geographical distribution of maternal health problems in public health policy formulation assists in identifying the occurrence of disparities by place, helping health providers to monitor health problems and decision makers to allocate resources on the basis of need29. Health outcomes are influenced variously by the availability and use of health services, the availability of transportation, ecological features of the environment including topography, and the social environment13,26,27,29.
Maternal health outcomes, including the decision about who will help to deliver, are influenced by individual, household and community factors30. The availability of health care, including village-based midwives, and cultural beliefs about the management of pregnancy, parturition, and the postpartum, may also influence women and their families in decision making. These factors differ for cultural, geographic and structural reasons and, accordingly, decisions about care during pregnancy and delivery also vary. Spatial methods allow identification of the spatial patterning of this variation, so identifying local level variability where women lack (or reject) assistance from SBA or lack antenatal care. The data so generated has the potential to assist local policy makers to target interventions.
A number of studies undertaken in diverse settings, which have focused on geographical patterns of behavioural risk factors31, antenatal care32 or maternal health outcomes7,33,34, provide the background to the research reported here. Two studies in particular focus on spatial patterns of antenatal care: Gayawan32 in Nigeria, and Charreire and Combier33 in France, the latter study highlighting that even in well-resourced settings, with good availability of services, attendance for prenatal care is unevenly distributed geographically. In addition, a study in Ghana34 identified the variable patterns of delivery at health centre facilities in different ecological areas, reflecting differences in geographic and socioeconomic factors.
These studies32-34 used aggregate rather than point data to distinguish place of birth when presenting the location of women associated with poor prenatal care. Atkinson and Kintrea35 argue that when health problems are mapped using aggregate data, cases are assumed to be distributed evenly. Smith and colleagues36 have argued that aggregating point base into quadrants results in a substantial loss of information about the distribution of events, and Meliker and colleagues13, in a study of cancer in Michigan, demonstrated the greater sensitivity of point data compared with aggregate data for cluster identification. The distribution of cases (of any condition under investigation) may be heterogeneous, as both urban and rural areas may have different ecological features and variations in infrastructure and local economy, any and all of which may affect health outcomes31.
In this article, drawing on research conducted in South Sulawesi, Indonesia, this enquiry is extended. The objectives are to (1) examine choice of birth assistant in association with place of birth, according to urban or rural residence, distance to nearest midwife and distance to hospital; (2) explore the spatial point patterns of women's antenatal care behaviours and birth assistance (because the authors obtained point data of respondents, the location is presented in point); and (3) visualize, interpret and explain clusters.
Study site
The study described below was conducted in Bantaeng, a district located in the southern part of South Sulawesi Province, Indonesia, about 120 km from Makassar, the provincial capital (Fig1). Bantaeng covers an area of about 400 km2, with 170 000 inhabitants (population density 435 per km2, 43 households per km2). The district is categorised by the Government of Indonesia as poor. The majority of its population live below the poverty line and are dependent on agriculture; coastal dwellers supplement farming with fishing. Infrastructure is also poor. According to the provincial maternal and child health report37, the district has one of the highest maternal mortality rates in the province; in 2007 the MMR was 267 per 100 000 live births compared with 105 per 100 000 for the province as a whole and 228 per 100 000 for Indonesia nationally38. Maternal health services in Bantaeng include 50 midwives, 12 community health centres (puskesmas) and one district hospital.
A list of potential respondents was obtained from village midwives, who are located at health posts and village maternity clinics. A total of 584 deliveries were recorded by midwives from March to June 2008; interviews were conducted in August 2008 and so women were recruited if they had delivered no more than 6 months prior to the interview to minimise recall bias. A quarter of potential participants (145) were excluded. These included 33 women whose estimated date of delivery was unclear, or whose reported date of delivery was discrepant with health service data; 62 women who had moved to other places; 35 women who could not be found at their addresses; seven women who had remote addresses which the research assistants could not reach; three women who refused to be interviewed; and five women who had died due to pregnancy complications. Additional to the village midwives' list, a snowball method was used to increase potential respondents. Each woman was asked whether she knew of one other woman who had delivered from May to June in her village, who may have delivered at home, unattended by a midwife, and so whose birth may not have been recorded in the administrative data base maintained by midwives. From this approach, 46 new cases were identified.
A total of 485 women who delivered their babies from March to June 2008 responded to a structured interview about antenatal care and birthing decisions, place of birth and choice of birth attendant. Antenatal care behaviour was operationalised in terms of the frequency of visits, measured by counting the total number of visits to any health provider in order to monitor their pregnancy, regardless of gestational age. A similar approach was used in a study in Bangladesh15.
Women's birthing decision refers to two items: place of birth and type of birth assistant. Place of birth included home-based and hospital-based delivery; type of birth assistance included SBA; doctors, midwives and obstetrician; and 'traditional birth assistant and/or family members' (TBA). At the time of the interview, the coordinate location of the respondent's house was recorded, using a Garmin Global Positioning System (GPS), which has precision up to 3 metres. Maternal health service locations were also recorded, including village midwives, community health centres and the sole hospital in the district, with their coordinate location established by visiting their individual location using GPS. No respondents gave birth at a community health centre. The hospital has 85 beds and is situated in the centre of urban Bantaeng.
A digital map of Bantaeng district was obtained from the Bantaeng District Planning Authority (BAPPEDA Bantaeng) with identification of urban (kota) and rural (desa) areas. The distinction between rural and urban areas was made using the statistical bureau classification, which includes administrative boundaries, road networks, topography, population density, infrastructure and percentage of people working in agriculture. A list of all midwives and their addresses was provided by Bantaeng District Health Office. This included two senior midwives who worked at the hospital, and who also provided private services outside hospital working hours.
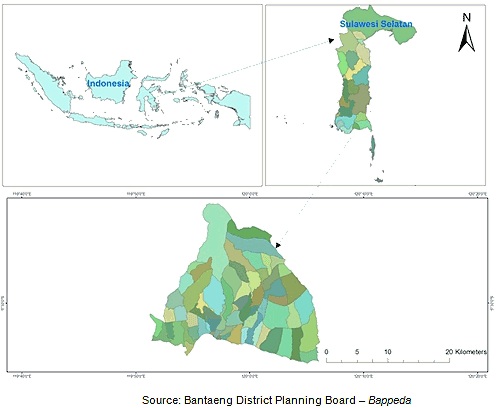
Figure 1: Map of study site - Bantaeng district, Indonesia.
Statistical analysis and spatial mapping
Statistical Package for the Social Sciences v17 (SPSS; http://www.spss.com) was used to analyse the association between area of residence and types of decision behaviours. Binary logistic regression was performed for multivariate analysis. The endpoints were frequency of antenatal care visit, place of birth and types of birth assistant at home. According to the WHO, women should have at least four antenatal care visits, and this recommendation has been adopted by the Government of Indonesia. The predictors included distance to hospital, distance to nearest midwife, and area of residence (urban or rural) as defined by the District Planning Authority to include population density and infrastructure. In this study, distance to hospital was related to whether the woman delivered at home or hospital (home vs hospital). Distance from the nearest midwife, on the other hand, was related to types of delivery assistance at home (TBA vs midwife/SBA). A GIS overlay analysis between the location of respondents and the classification of the area was conducted to identify whether each women was resident in an urban or rural area. To measure the distance between each study participant and nearest midwife, a Euclidean method (straight line) was used. To do this, a multiple buffer analysis using ArcGIS v9.3 (Environmental Systems Research Institute; http://www.esri.com/software/arcgis) was performed to measure the distance between study participants' households and hospital location, with 1 km distance to midwife and 4 km to the hospital. One kilometre distance from midwife was chosen as a walkable distance39,40; according to Moudon and colleagues41, there is no difference in perception of distance among people who live less than 1 km from a health service. To calculate adjusted odds ratio of types of residential area and distance to midwife and distance to hospital, variables shown in Table 1 were included in the model.
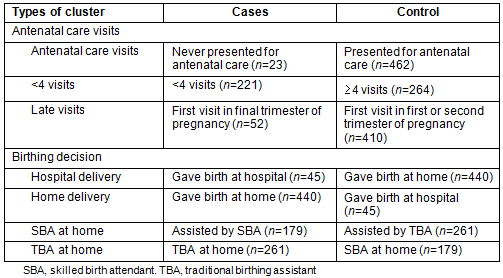
To identify spatial clusters of antenatal care behaviours and women's birthing decisions, the SaTScan v8 (http://www.satscan.org) was used. This software used data of cases and controls, and population data that combined cases and controls with coordinate location. Types of clusters, cases and controls for SaTScan software are shown in Table 1.
This method has been used widely for cluster detection among points31,42,43. Because household locations were available, the Bernoulli test-base model was used. A cluster was identified to be statistically significant by comparing the likelihood ratio test statistics against a null distribution based on Monte Carlo simulations using 999 iterations44,45. The spatial scan statistic is based on moving a circular window across the map. The window size varies continuously, from zero to a maximum of 50% of the total population at risk. For this analysis, the maximum spatial cluster size was set to include up to 50% of the total population at risk46. SaTScan produces cluster counts and statistics but does not provide any accompanying graphics such as maps. Geographical information system (GIS) technique was used to performed geographical analysis. ArcGIS v9.3 was used to map all participants, the locations of midwives and the community health centres in the study site, and was used to visualise the location of clusters produce by SaTScan.
Table 1: Clusters, cases and control definitions for SaTScan software
Ethics approval
Ethics clearance for this study was obtained from Monash University (CF08/0418 - 2008000175). In addition, permission was obtained from the South Sulawesi Provincial Government (Badan Kesatuan Bangsa - Provincial Unity Board) and the Bantaeng District Government (Bantaeng National Unity Board) before data were collected. Consent from all participants was established, and they provided permission to link geographic location and individual characteristics collected from this study.
Geographic distribution of women's behaviours on antenatal care and birth decisions
Two-thirds of respondents lived in rural areas and one-third came from urban areas. While the age distribution of participants was similar between urban and rural participants (Table 2), women from urban areas had a much higher educational level than women from rural areas. The majority of participants from urban areas came from households with a higher wealth index, while respondents from rural areas were mostly from the lowest and the second lowest category in terms of their household wealth index. Most women in both urban and rural areas identified as housewives.
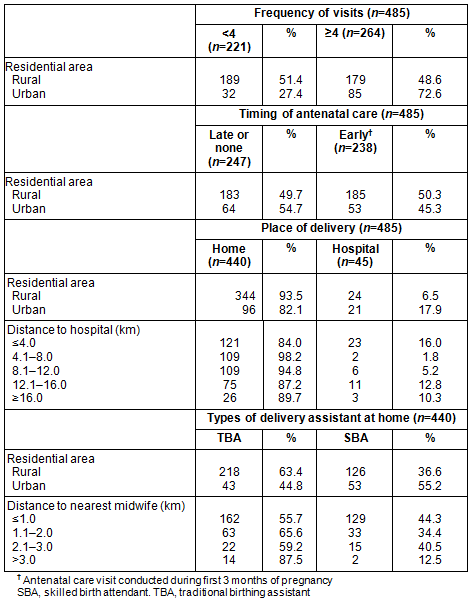
Among respondents from rural areas, about half had fewer than four antenatal care visits; in the urban area around two-thirds had at least four antenatal care visits. The proportion of women in urban areas who made their initial antenatal care visits in the first trimester was slightly lower than that for rural areas. Women in both urban and rural areas predominantly gave birth at home, although the percentage in rural areas was slightly higher (93.5% and 82.1% rural and urban respectively). Two-thirds of women who lived in rural areas and delivered at home were assisted by TBAs.
Women in urban areas resided much closer in distance to both midwives and the hospital. Almost all urban women (94%) could potentially access a midwife within a 1 km distance, compared to 57% of women in rural areas. No woman in an urban area lived more than 2 km from a midwife, whereas in rural areas, 17.4% of respondents lived more than 2 km from the local midwife and only a quarter were located within 1-2 km from a midwife. The percentage of women assisted by SBAs at home decreased as the distance to nearest midwife increased (Table 3).
Table 2: Sociodemographic characteristics, based on urban-rural areas
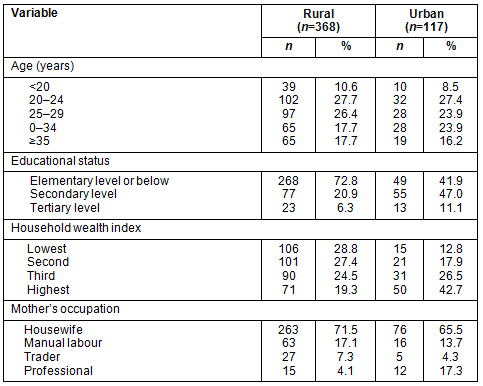
Table 3: Geographic distribution of women, antenatal care visits, place or birth and types of birth attendant
Multivariate analysis
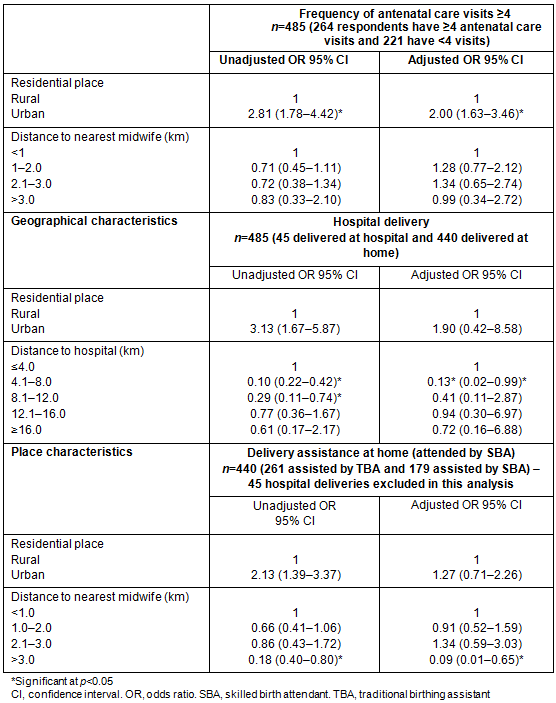
Unadjusted odds ratio indicated that women in urban areas were three times as likely to have at least four antenatal care visits (Table 4). Controlling individual characteristics (age, education, household access, initial antenatal care visits and distance to the nearest midwife) lowered the odds ratio by 80%, but the association was still significant (confidence interval (CI) 1.63-3.64). Distance to the nearest midwife, however, was not associated with the likelihood of a pregnant woman having at least four antenatal care visits.
The unadjusted OR indicated that women in urban areas were three times more likely to deliver at hospital (CI 1.67-5.87) than women who lived in rural areas (Table 4). However, while women who lived 4-8 km from the hospital were less likely to deliver at hospital, women who lived >12 km from hospital were as likely to deliver at hospital as women residing <4 km from hospital. Further, after controlling for other variables, the likelihood of an urban resident to deliver at hospital reduced to 1.90, not significantly different from women living in rural areas. The likelihood to deliver at hospital decreased by 87% among women who resided 4-8 km compared those who lived <4 km from hospital. However, those who lived >8 km from hospital were no different from those living <4 km from hospital. Rural or urban area of residence was not associated with delivery with an SBA at home. Women living >3 km from the nearest midwife, however, were less likely to be assisted by an SBA at home (demonstrated by both adjusted and unadjusted odds ratio). Therefore, residing >3 km from the midwife influenced women's decision to be assisted (or not) by a midwife at home.
Table 4: Multivariate analysis between geographical characteristics and birthing decision
Spatial cluster detection
Women's behaviour regarding antenatal care and birthing decisions was spatially clustered (Table 5). This included a cluster of women who never presented for antenatal care, those who received late antenatal care, and/or those who received less than four antenatal care visits.
While there was no geographic cluster of women who made their initial antenatal care visits in the last trimester of pregnancy, in the northern part of the district there were two clusters, each with six respondents who never presented for antenatal care (Fig2). Each cluster contained 26.1% of the total respondents who never presented for antenatal care, and these women were located in isolated rural areas where the terrain was relatively steep. Women who had fewer than four antenatal visits were also geographically clustered in the north-west of the district (Fig3).
Women who delivered their babies at hospital or delivered with an SBA at home were clustered in two distinct zones within the urban area (Fig4). The hospital delivery cluster represented 31.1% of total hospital deliveries in the study period. The ratio of the number of observed and expected hospital deliveries in this area was 4.43. Similarly, SBA at home was clustered in urban areas, with the ratio of observed and expected SBA at home being 2.00. In contrast, the cluster of rural women who delivered at home with TBA geographically coincided with the cluster of women who had fewer than four antenatal care visits (Fig5).
Table 5: Cluster identification of women's behaviours on antenatal care and birthing decision
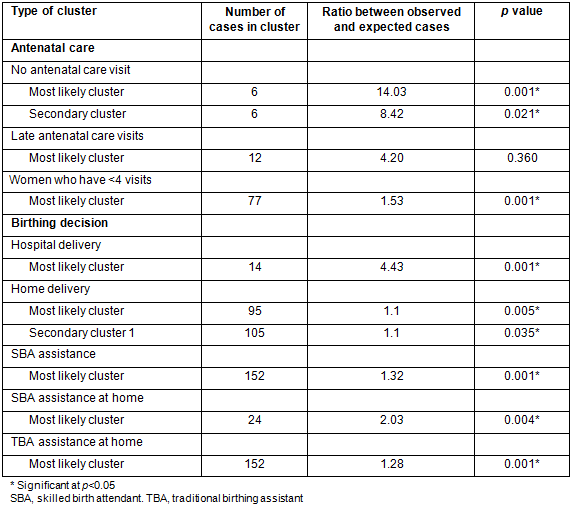
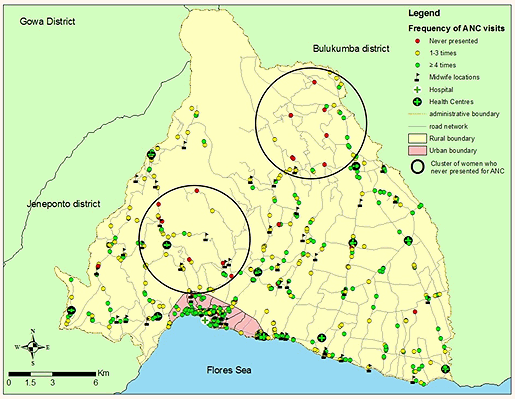
Figure 2: Location of clusters of women who did not present for antenatal care.
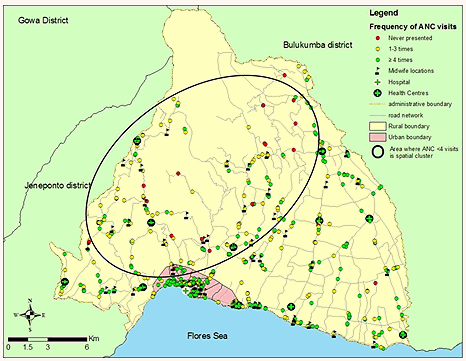
Figure 3: Location of cluster of women who had fewer than four antenatal care visits.
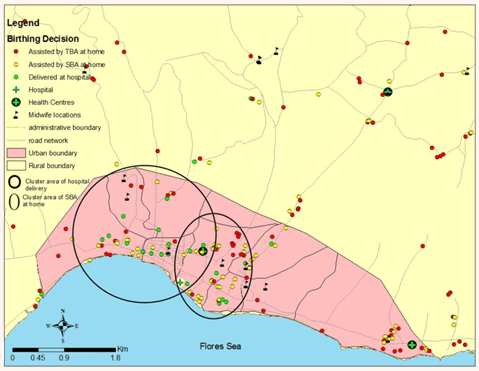
Figure 4: Clusters of hospital deliveries and skilled birth attendant assistance at home.
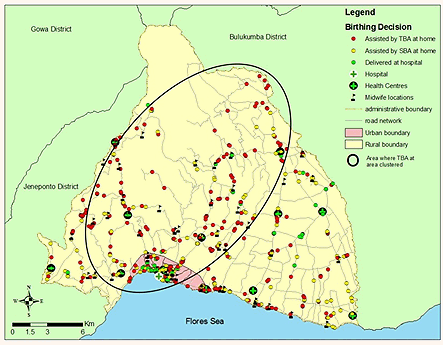
Figure 5: Location of clusters of traditional birthing assistance at home.
Discussion
In this study, the authors found a low percentage of hospital deliveries (<10%). Further, only 40.7% of women delivered at home with SBAs, which was lower than provincial and national levels (77%). Area of residence influenced the likelihood of women having at least four antenatal care visits, and these were clustered in the same locations as women assisted by TBAs. Area did not influence whether women delivered at hospital or at home with SBAs, although hospital deliveries and deliveries attended by SBAs at home were clustered in urban areas. Further, while living a certain distance to midwives (>3 km) reduced the likelihood of assistance by SBAs at home, there was no difference in birth assistance between women who lived >8 km from or <4 km from hospital.
Women in urban areas had more antenatal care visits than did their rural counterparts, consistent with other studies including in Indonesia16,47-49. In contrast, in a study in Colombia50, the urban-rural dichotomy did not appear to influence women's antenatal care behaviour, and the author hypothesised that in this case, access was determined by the whole region rather than by the specific location.
Area of residence influenced the odds of having at least four visits irrespective of distance to midwife. This result may be due to the availability of a community-operated health service where a cadre and nurse or midwife provides maternal and child health services such as immunization and weight gain monitoring. Midwives also offer antenatal care for pregnant women at neighbourhood-based health posts. As a component of Indonesia's efforts to reduce maternal mortality rates since 1990, the village-based midwives program was intended to reduce urban-rural disparities of antenatal care visits. However, this may only be a local instance in the reduction of urban-rural differences in antenatal care. Further study would be required to determine if this observation holds true elsewhere in the archipelago.
The authors in the present study did not find differences in the likelihood of delivering at hospital or with SBAs at home due to different areas of residence, in contrast with other studies16,47-49,51. Again, this finding may be atypical, given that publications that have used data from the national Demographic and Health Survey (DHS) in Indonesia[23, 48} have reported that residential area determines whether women deliver at hospital or at home with SBAs. Another explanation is that in this district, people from rural areas might prefer to deliver at a hospital when referred by a village midwife in the context of the development of delivery complications. This would explain the lack of association between area of residence and hospital delivery. The difference in results between the present study and previous studies that used Indonesia DHS data may be because the data were collected in this study 1 year after the Civil Health Insurance (jamkesmas) was introduced, while the DHS study was conducted before the insurance scheme had been implemented.
The location of the hospital was a distinct and obvious advantage to women living in its proximity in the urban area. Similarly, the superior availability of multi-modal transportation in urban areas, when compared to rural areas, could contribute to disparities in antenatal care. For instance, rickshaws - small vehicles that can carry one or two passengers - were relatively inexpensive, and could be used by women to go to the hospital, but they were available only in urban areas. In rural areas, public transportation was infrequent - three to four times a day and rarely at night - and generally women needed cars, which were more expensive, to access care. Women who went into labour during the night especially had difficulty accessing the hospital because of lack of transport and lack of cash to pay for a private car.
Our study did not include travel time. One of the limitations of using a straight-line (Euclidian) method is that it does not take into account topographic and other factors, such as road surface, road condition and availability of transportation, all of which influence travel time. Longer distances and longer travel times directly influence access to health services although this is less so for acute or emergency conditions52,53.
Lack of association between distance to hospital and delivery at hospital may occur if women had an obstetric emergency at home and were referred to a hospital by a midwife; these were women who were informed during antenatal care visits that they had a higher risk of complications due to conditions such as transverse location of the baby. However, it is not clear whether more women from urban areas close to the hospital or people far from the hospital presented because they had obstetric complications and were referred by TBAs or SBAs.
According to Thind and Banerjee48, differences in birthing decisions between areas can also be influenced by the different distribution of traditional birth attendants. In Bantaeng, according to the District Health Office, at the time of the study there were 220 TBAs and 50 midwives across the district. However, the individual addresses of the TBA were not available, leading to difficulty in examining the relationship between clusters of TBA at home delivery and the spatial distribution of TBAs in the district. Another explanation is that the cost of SBAs is much higher than the cost of TBAs. From field observations, SBA attendance at home cost around 300 000-500 000 rupiah (US$40-70) and therefore, only those women who came from the highest socioeconomic background could afford this. A TBA, on the other hand, is paid around 50 000-250 000 rupiah (US$6-30), depending on negotiations between the family and the TBA.
In addition to looking at urban and rural differences, the authors investigated any geographical clusters within urban and rural areas. This approach explored heterogeneity within these residential settings. Although there was no significant difference between urban and rural areas in regard to hospital delivery, delivery at hospital and SBA at home were both clustered within urban areas. Those who delivered at hospital or were attended by SBAs at home tended to be clustered geographically, while women in rural areas with similar birthing decisions to those in urban areas tended to be distributed equally in rural areas.
As this study included all women who delivered during the data collection period, the cluster of TBAs in the north-west and north of the district suggests that these areas should be the focus for any interventions. Although there may be recall bias on the number of antenatal care visits during pregnancy, this is unlikely to have occurred with regard to types of birth assistance and place of birth. In this study, the authors did not explore the characteristics of the midwives or hospital, and SBA characteristics such as locality, age, marital status and working experiences may have affected women's willingness to have them at delivery54,55. In addition, midwives would have personal characteristics that influenced women's choices and explain the clustering.
This study only included women who delivered their babies during a 4-month period. Selection bias may occur if the numbers of women who deliver at hospital or delivered at home with SBA or TBA were higher at a particular time. However, the distribution of pregnant women on a monthly basis is not available from the District Health Office, making it difficult to assess possible selection bias in this study.
A spatial approach provides useful information on women's use of maternal health services, with point data enabling the examination of individual antenatal care and birthing decisions. This approach can assist policy makers to identify areas with low accessibility to maternal health resources and to identify the prevalence of factors that contribute to poor maternal health outcomes. Deliveries at home with SBAs and at hospital are spatially clustered at different locations within urban areas, while poor antenatal care attendance and TBAs are clustered in rural areas.
Residence has a strong influence on frequency of antenatal care visits, but not on birthing decisions. Within rural areas, lack of prenatal care and the reliance on TBAs are not distributed randomly. Similarly, in urban areas, clusters of hospital or at-home SBA deliveries appear to reflect underlying geographical concentrations of wealth and income. Taken together, these findings highlight the importance of the locational analysis of behaviours and decision making when developing specific interventions to address social exclusion and poor health outcomes.
Acknowledgement
The research on which this article is based was a part of Ansariadi's PhD project in Monash University. The School of Psychology and Psychiatry, Faculty of Medicine, Nursing and Health Sciences, Monash University and the Australian Agency for International Development, through an Australian Development Scholarship, provided financial assistance for data collection. The authors thank the Director of Bantaeng District Health Office for facilitating in the field and village midwives and research assistants for assisting in the collection of data. They especially thank the research participants for providing relevant information.
References
1. Bappenas. Indonesian MDGs report. Jakarta: Indonesian National Planning Bureau (Bappenas), 2012.
2. Adegoke AA, Hofman JJ, Kongnyuy EJ, van den Broek N. Monitoring and evaluation of skilled birth attendance: a proposed new framework. Midwifery 2011; 27(3): 350-359.
3. Campbell OMR, Graham WJ. Strategies for reducing maternal mortality: getting on with what works. Lancet 2006; 368(9543): 1284-1299.
4. Koblinsky M, Matthews Z, Hussein J, Mavalankar D, Mridha MK, Anwar I, et al. Going to scale with professional skilled care. Lancet 2006; 368(9544): 1377-1386.
5. Cummins S, Curtis S, Diez-Roux AV, Macintyre S. Understanding and representing 'place' in health research: a relational approach. Social Science & Medicine 2007; 65(9): 1825-1838.
6. Marmot M. Social determinants of health inequalities. Lancet 2005; 365: 1099-1104.
7. Rajaratnam JK, Burke JG, O'Campo P. Maternal and child health and neighborhood context: the selection and construction of area-level variables. Health & Place 2006; 12(4): 547-556.
8. Webster PC. Indonesia makes maternal health a national priority. Lancet 2012; 380(9858): 1981-1982.
9. Arcury TA, Gesler WM, Preisser JS, Sherman J, Spencer J, Perin J. The effects of geography and spatial behavior on health care utilization among the residents of a rural region. Health Services Research 2005; 40(1): 135-155.
10. Alvarez PLL, Guerra-Yi ME, Faes C, Alvare YG, Molenberghs G. Spatial analysis of breast and cervical cancer incidence in small geographical areas in Cuba, 1999-2003. European Journal of Cancer Prevention 2009; 18(5): 395-403.
11. Grady SC, Enander H. Geographic analysis of low birthweight and infant mortality in Michigan using automated zoning methodology. International Journal of Health Geographics 2009; 8: 10.
12. Lebel A, Pampalon R, Hamel D, Theriault M. The geography of overweight in Quebec: a multilevel perspective. Canadian Journal of Public Health-Revue Canadienne De Sante Publique. 2009; 100(1): 18-23.
13. Meliker JR, Jacquez GM, Goovaerts P, Copeland G, Yassine M. Spatial cluster analysis of early stage breast cancer: a method for public health practice using cancer registry data. Cancer Causes & Control 2009; 20(7): 1061-1069.
14. Zhang WY, Wang LP, Fang LQ, Ma JQ, Xu YF, Jiang JF, et al. Spatial analysis of malaria in Anhui province, China. Malaria Journal 2008; 7: 206.
15. Anwar, Sami M, Akhtar N, Chowdhury ME, Salma U, Rahman M, et al. Inequity in maternal health-care services: evidence from home-based skilled-birth-attendant programmes in Bangladesh. Bulletin of the World Health Organization 2008; 86(4): 252-259.
16. Fan L, Habibov NN. Determinants of maternity health care utilization in Tajikistan: learning from a national living standards survey. Health & Place 2009; 15(4): 952-960.
17. Mishra V, Retherford RD. The effect of antenatal care on professional assistance at delivery in rural India. Population Research and Policy Review 2008; 27(3): 307-320.
18. Gabrysch S, Cousens S, Cox J, Campbell OMR. The influence of distance and level of care on delivery place in rural Zambia: a study of linked national data in a geographic information system. PLOS Medicine 2011; 25 January, 8(1).
19. Kyei NNA, Campbell OMR, Gabrysch S. The influence of distance and level of service provision on antenatal care use in rural Zambia. PLOS One 2012 4 October, 7(10).
20. Lohela TJ, Campbell OMR, Gabrysch S. Distance to care, facility delivery and early neonatal mortality in Malawi and Zambia. PLOS One 2012; 7(12): e52110.
21. Kitui J, Lewis S, Davey G. Factors influencing place of delivery for women in Kenya: an analysis of the Kenya demographic and health survey, 2008/2009. BMC Pregnancy and Childbirth 2013; Feb 17: 13.
22. Masters SH, Burstein R, Amofah G, Abaogye P, Kumar S, Hanlon M. Travel time to maternity care and its effect on utilization in rural Ghana: a multilevel analysis. Social Science &Medicine 2013; 93: 147-154.
23. Titaley CR, Dibley MJ, Roberts CL. Utilization of village midwives and other trained delivery attendants for home deliveries in Indonesia: results of Indonesia Demographic and Health Survey 2002/2003 and 2007. Maternal and Child Health Journal 2011; 15(8): 1400-1415.
24. Ronsmans C, Scott S, Adisasmita A, Deviany P, Nandiaty F. Estimation of population-based incidence of pregnancy-related illness and mortality (PRIAM) in two districts in West Java, Indonesia. BJOG - an International Journal of Obstetrics and Gynaecology 2009; 116(1): 82-90.
25. Kulldorff M. Spatial disease clusters: detection and inference. Statistics in Medicine 1995; 14: 799-810.
26. Lawson AB. Disease cluster detection: a critique and a Bayesian proposal. Statistics in Medicine 2006; 25(5): 897-916.
27. Lawson AB, Simeon S, Kulldorff M, Biggeri A, Magnani C. Line and point cluster models for spatial health data. Computational Statistics & Data Analysis 2007; 51(12): 6027-6043.
28. Wartenberg D. Investigating disease clusters: why, when and how? Journal of the Royal Statistical Society Series A - Statistics in Society. 2001; 164: 13-22.
29. Elliott P, Wartenberg D. Spatial epidemiology: current approaches and future challenges. Environmental Health Perspectives 2004; 112(9): 998-1006.
30. United Nations Development Programme. A social determinants approach to maternal health. (Online) 2011. Available: http://www.undp.org/content/dam/undp/library/Democratic%20Governance/Discussion%20Paper%20MaternalHealth.pdf. (Accessed 12 December 2012).
31. Westercamp N, Moses S, Agot K, Ndinya-Achola JO, Parker C, Amolloh KO, et al. Spatial distribution and cluster analysis of sexual risk behaviors reported by young men in Kisumu, Kenya. International Journal of Health Geographics 2010; 9: 24.
32. Gayawan E. A Poisson regression model to examine spatial patterns in antenatal care utilisation in Nigeria. Population Space Place 2013; 20(6): 485-497.
33. Charreire H, Combier E. Poor prenatal care in an urban area: a geographic analysis. Health & Place. 2009; 15(2): 412-419.
34. Johnson FA, Padmadas SS, Brown JJ. On the spatial inequalities of institutional versus home births in Ghana: a multilevel analysis. Journal of Community Health 2009; 34(1): 64-72.
35. Atkinson R, Kintrea K. Disentangling area effects: evidence from deprived and non-deprived neighbourhoods. Urban Studies 2001; 38(12): 2277-2298.
36. Smith LK, Draper ES, Manktelow BN, Dorling JS, Field DJ. Socioeconomic inequalities in very preterm birth rates. Archives of Disease in Childhood: Fetal and Neonatal 2007; 92(1): F11-F14.
37. Provincial Health Office. South Sulawesi province health profile. Makassar: PHO, 2008.
38. Hermiyanti S. The challenge of making safe motherhood a reality of community midwives in Indonesia. (Online) 2008. Available: http://www.searo.who.int/LinkFiles/FCH_d3-7challenges-msm-ino.pdf (Accessed 10 September 2010).
39. Koohsari MJ, Kaczynski AT, Giles-Corti B, Karakiewicz JA. Effects of access to public open spaces on walking: is proximity enough? Landscape and Urban Planning 2013; 117: 92-99.
40. Lovasi GS, Moudon AV, Pearson AL, Hurvitz PM, Larson EB, Siscovick DS, et al. Using built environment characteristics to predict walking for exercise. International Journal of Health Geographics 2008; 7(10): doi: 10.1186/1476-072X-7-10
41. Moudon AV, Lee C, Cheadle AD, Garvin C, Johnson D, Schmid TL, et al. Operational definitions of walkable neighborhood: theoretical and empirical insights. Journal of Physical Activity and Health 2006; 1(S1): S99-S117.
42. Kulldorff M, Feuer EJ, Miller BA, Freedman LS. Breast cancer clusters in the northeast United States: a geographic analysis. American Journal of Epidemiology 1997; 146(2): 161-170.
43. Yiannakoulias N, Rowe BH, Svenson LW, Schopflocher DP, Kelly K, Voaklander DC. Zones of prevention: the geography of fall injuries in the elderly. Social Science & Medicine 2003; 57(11): 2065-2073.
44. Kulldorff M, Heffernan R, Hartman J, Assuncao R, Mostashari F. A space-time permutation scan statistic for disease outbreak detection. PLOS Medicine 2005; 2(3): 216-224.
45. Moore GE, Ward MP, Kulldorff M, Caldanaro RJ, Guptill LF, Lewis HB, et al. A space-time cluster of adverse events associated with canine rabies vaccine. Vaccine 2005; 23(48-49): 5557-5562.
46. Kulldorff M, Huang L, Konty K. A scan statistic for continuous data based on the normal probability model. International Journal of Health Geographics 2009, 8: 58.
47. Ronsmans C, Scott S, Qomariyah SN, Achadi E, Braunholtz D, Marshall T, et al. Professional assistance during birth and maternal mortality in two Indonesian districts. Bulletin of the World Health Organization 2009; 87(6): 416-423.
48. Thind A, Banerjee K. Home deliveries in Indonesia: who provides assistance? Journal of Community Health 2004; 29(4): 285-303.
49. Titaley CR, Dibley MJ, Roberts CL. Factors associated with non-utilisation of postnatal care services in Indonesia. Journal of Epidemiology and Community Health 2009; 63(10): 827-831.
50. Veciono-Ortiz AI. Determinants of demand for antenatal care in Colombia. Health Policy 2008; 86: 363-372.
51. Thind A, Mohani A, Banerjee K, Hagigi F. Where to deliver? Analysis of choice of delivery location from a national survey in India. BMC Public Health 2008; 8: 29.
52. Cromley EK, McLafferty SL. GIS and public health. New York: The Guilford Press, 2002.
53. Arcury TA, Gesler WM, Preisser JS, Sherman J, Spencer J, Perin J. The effects of geography and spatial behavior on health care utilization among the residents of a rural region. Health Services Research 2005; 40(1): 135-155.
54. Galotti KM, Pierce B, Reimer RL, Luckner AE. Midwife or doctor: a study of pregnant women making delivery decisions. Journal of Midwifery & Women's Health 2000; 45(4): 320-329.
55. Titaley CR, Hunter CL, Heywood P, Dibley MJ. Why don't some women attend antenatal and postnatal care services? A qualitative study of community members' perspectives in Garut, Sukabumi and Ciamis districts of West Java Province, Indonesia. BMC Pregnancy and Childbirth 2010; 10: 61.

