Available evidence shows that rural Australians bear an unequal burden when it comes to their health and suffer from the double disadvantage of poorer health and poorer access to health services1,2. Rural Australians are often stereotyped as stoical3. Certainly they consistently use fewer Medicare services and see their general practitioner (GP) fewer times per annum than their urban counterparts2,3. However, this may relate more to lack of opportunity than to inherent stoicism4.
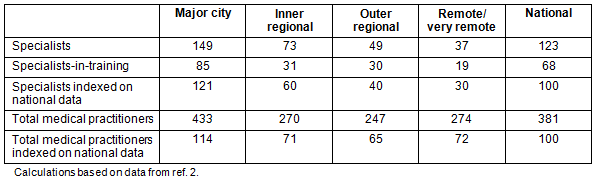
Rural health care and service delivery is recognised as a problem all over the world, not just in Australia5. However, the vast geographical expanse of the country makes it even more difficult to attract the requisite health workforce to rural and remote regions. Consequently there is a chronic shortage of health professionals in rural and remote Australia6-10. While nurses are the group best represented in rural areas, there is still a severe mal-distribution of health professionals in Australia. The need for additional healthcare services in the bush is well recognised. According to data from the Australian Institute of Health and Welfare Medical Labour Force Survey 20112, there are very low rates of medical specialists by population in remote and very remote Australia compared to the national average (Table 1).
Various strategies have been used in order to recruit and retain the rural health workforce. These strategies have been described as 'selection, education, coercion, incentives, and support'5. The current evidence supports the use of careful and well-defined selection and educational policies, and incentives and support schemes may also have value5. Despite compulsory programs being implemented in as many as 70 countries worldwide, there is no strong evidence to date that they succeed11.
Compulsory programs vary in scope and duration and can be classified into three main types: (1) state or government employment programs (or condition of service contracts) with a requirement to work for the government with little or no provision for working in private practice, (2) compulsory programs with incentives and (3) compulsory programs without incentives. Examples of the first type of compulsory program in Australia include the requirement for international medical graduates to work within the Australian healthcare system in a district of workforce shortage, as part of their immigration and relocation. Compulsory programs with incentives can offer options for future educational and/or employment opportunities, the provision of financial support such as house rental or other family benefits or a program offering one or more of the above incentives. Compulsory programs without incentives are less common compared with the first two categories11.
A systematic review by Bärnighausen and Bloom of 43 studies (of which 34 were US-based and none Australian) found that programs offering financial incentives do lead to increased numbers of health workers in under-served regions. Nonetheless the evidence was limited in generalisability and no evidence was found that could conclusively attribute increased workforce redistribution to such financial incentives12. In their review, Frehywot et al. suggest that compulsory programs may not provide a permanent answer to capacity development or guarantee that remote communities will receive a permanent workforce11. Dwyer argued that Commonwealth-funded rural clinical schools, especially those within metropolitan-based universities, have had limited impact in terms of attracting doctors to work in rural areas13. In a counter-argument, Walker claimed that the main issue was not rural clinical placements but the lack of postgraduate medical training places14.
Wakerman et al15 described the need for different service delivery models for differing levels of remoteness. They also emphasised the need to ensure that a comprehensive range of primary healthcare services were available locally wherever possible, and defined the critical minimum population base as about 5000 inhabitants in order to sustain such services. In remote areas, there is a need to provide services that are culturally appropriate for Aboriginal and Torres Strait Islander people16.
The inclusion of flying-in and flying-out (FIFO) and drive-in drive-out (DIDO) models of service delivery in the definition of remote medicine formulated by an experienced working group of doctors and academics17 indicated the importance and need for such models of care. According to Bourke et al. there are a number of recognised fit-for-purpose models of care operating in rural and remote Australia including FIFO and DIDO services18. Wakerman et al. pointed out there are various ways of defining FIFO or DIDO services that are currently used19:
1. Specialist outreach services.
2. Hub-and-spoke or outreach arrangements for various allied health and specialist programs.
3. 'Orbiting staff' who spend significant periods of time (12 months or more) in one or two specific communities.
4. Long-term shared positions, such as month on/month-off, where the same practitioners service the same communities.
5. Short-term locum or agency staff who move from place to place or as a one off19.
In February 2013, the House of Representatives released the report of a comprehensive inquiry on FIFO health services20, which is discussed in a later section.
In this article we review the recent literature relating to FIFO and DIDO healthcare services and discuss their benefits and potential disadvantages for rural Australia, and for health practitioners. We question whether or not FIFO and DIDO are a form of expediency or efficiency in relation to healthcare service delivery.
Table 1: Specialists, specialists-in-training and total medical practitioners:
full-time equivalent per 100 000 population by remoteness area 2011
FIFO and DIDO service provision relies heavily on the existence of a well-functioning primary healthcare system to operate efficiently. It also relies on the altruism of the clinicians involved, who offer many forms of support to local staff through 'education, mentorship, shared care and supervision to name a few'9, thereby strengthening local service delivery.
The main advantages of FIFO and DIDO healthcare services are that they provide much-needed care to people who would otherwise need to travel large distances, often at their own cost. Provided that there are adequate and well-resourced primary care services in place, visiting specialists can add significantly to the quality of care being offered19 and are often greatly appreciated by locals. Clearly, such services offer health care that could otherwise not be provided in small rural or remote communities, with the resultant benefits to both patients and to resident clinicians.
The recent report from the House of Representatives inquiry conducted by the Standing Committee on Regional Australia20 urged the Australian Government to see FIFO and DIDO workforces as the exception rather than the rule, due to concerns that the practice 'could lead to a hollowing out of established regional towns, particularly those inland'. Although the report focused mainly on the resources industry, it also made recommendations about the need to develop 'strategies and targets for achieving fair access to health services for people living in regional and remote areas recognizing the use of fly-in, fly-out/drive-in, drive-out health services, providing for appropriate funding and infrastructure support [our emphasis]'20.
The report acknowledges the reluctance of medical staff to live and work in rural and remote communities, because of barriers such as poor or inadequate accommodation, security concerns, poor rosters leading to a poor life-work balance, inadequate orientation, poor access to professional development and training, and the relatively high cost of some services and essentials such as food20. It recommends developing policy that acknowledges the infrastructure needs of FIFO medical professionals including accommodation, the need to have residential staff with capacity, the administrative burdens placed on residential staff by FIFO medical professionals, the role that technology can play in future, and the need for funding models that reflect the true cost of service provision through FIFO delivery.
Many health professionals have expressed concern over the dismantling of community care, as demonstrated within the mental health sector. This has occurred despite a consensus among experts that 'community centred health services should be placed in the centre of communities'21. There is a danger that FIFO and DIDO services will 'have a deleterious effect on the community. Both communities and the level of service delivery are eroded by FIFO' especially in communities that are large enough to support residential health workers20.
FIFO and DIDO services are complicated to administer, particularly in remote communities where the provision of culturally appropriate services is so critical. Personnel tend to change frequently and women working in remote communities often have to deal with gender issues17. The main difficulties experienced by female FIFO and DIDO service providers are feeling lonely, finding it difficult to fit in (both at work and socially), and feeling undervalued. Nurses and female doctors, especially those working part-time or who are new to practice, feel excluded from decision-making at work, which leads them to feel undervalued, frustrated, excluded and lonely.
Rural clinicians work long hours and often have few colleagues that they can turn to for peer support22, which can lead them to feel deskilled over time. It is known that 'specialists that deliver services to rural and remote areas often do this at considerable personal cost of time and effort'7. Many FIFO health practitioners work long hours, including after hours, have a poor life-work balance, and are consequently at risk of burnout3. The Department of Health and Ageing workforce audit (2008) noted that medical specialists in rural Australia struggle with professional isolation, lack of support and lack of infrastructure. Nonetheless, it is important to acknowledge that various models of FIFO/DIDO services have different impacts on underlying health services infrastructure (see Wakerman's list above). The adverse impact of 'short-term locum-tenant' (model 5) or 'orbiting staff' (model 3) arrangements are greater as compared to 'long-term shared positions' (model 4) as these options are expensive and do not create an environment in which there is a critical mass of health providers who are able to sustain peer networks and/or offer mentoring to clinical teams.
A detailed analysis of FIFO and DIDO health services in remote Indigenous communities identified the positives and negatives attached to current service provision and made some suggestions for improvements in relation to convenience and cost of services, social diversity of the service personnel, quality of service personnel, quality of service provision for the providers, quality of service provision for the community and the nature of social relationships4. For example, the cost and convenience was seen as an advantage to community members but it was recognised that service providers sometimes have to waste their time travelling for up to 2 days before even providing a service. We suggest that a cultural broker could help to improve planning for such visits.
Perkins questions whether or not 'all this travelling' by visiting health professionals is sustainable and deducts from the 'development of a robust local workforce with impacts for the sustainability, productivity and quality of services'9. Wakerman et al. question whether or not FIFO health services are part of the problem or a panacea and are concerned about adding to the deficit view of working in rural and remote health care19, and Hanley expresses concern that such services do not contribute to social capital or social cohesion23.
The concept of social capital has been increasingly used in relation to individual health and in health systems research. Putnam considers social capital to be a form of reciprocal communal interest that binds individuals through common interests, cooperation and collaboration24,25. When social capital is limited, there is no strong sense of community or reciprocity, as is the case in areas with large numbers of FIFO workers. This is likely to undermine social cohesion, largely because of the transient nature of the FIFO healthcare workforce. They place disproportionate demands on local services and infrastructure, but offer limited returns for the permanent health professionals in the community in terms of building professional and communal relationships.
FIFO and DIDO service models already play an important role in the bush, and could be used in future to deliver innovative methods of practice, higher levels of clinical acumen among health professionals, cross-cultural understanding and resourcefulness17. The current literature suggests that FIFO and DIDO healthcare services operate best where local primary healthcare services are adequately resourced and staffed. The advantages of FIFO and DIDO services are that they offer services that would otherwise be unavailable, avoiding the need for patients to travel large distances to receive health care. In most instances, it is not just the patient who is greatly inconvenienced but also their families, since a designated carer has to accompany the patient, causing considerable disruption to family caring arrangements. The issue of equity is a core issue. However, FIFO and DIDO services 'should be seen not as a replacement for local health care, but as a necessary compromise between the tyranny of distance and equity of access to health services'23.
It is of concern that, by continuing to use FIFO and DIDO services, especially to fill generalist positions, local services and infrastructure may be eroded over time. This is particularly true where certain localities are so dependent on the ever-increasing locum-tenant system of service provision that they have undeservedly gained a reputation as places to which no clinician wants to move. These services are often eventually downgraded and full-time positions are, at times, withdrawn.
Whilst FIFO and DIDO services create opportunities for clinicians, they also create challenges, including travelling long distances, working long hours, a lack of collegial support and supervision, and a lack of local infrastructure. In order to make FIFO and DIDO services work well, continued support for local primary healthcare services is essential and a new funding model is necessary. One option would require greater flexibility on the part of employers to sustain a team of FIFO health professionals in rural regions on a longer term job-share basis, so that they and their colleagues feel part of the local healthcare system and communities26. Another longer term option would be to create a robust rural generalist pathway for clinical practice, with appropriate remuneration benefits.
Acknowledgements
The authors acknowledge the contribution made by the Collaborative Research Network for Mental Health and Well-being in Rural and Regional Communities, supported by the Department of Industry, Innovation, Science, Research and Tertiary Education, Commonwealth Government of Australia.
References
1. Schofield DJ, Shrestha RN, Callander EJ. Access to general practitioner services amongst underserved Australians: a microsimulation study. Human Resources for Health 2012; 10(1): 1-6.
2. Australian Institute of Health and Welfare. Medical workforce 2011. National health workforce series no. 3. Cat no. HWL 49. Canberra, ACT: AIHW, 2013.
3. Chater AB. Looking after health care in the bush. Australian Health Review 2008; 32(2): 313-318.
4. Guerin P, Guerin B. Social effects of fly-in fly-out and drive-in drive-out services for remote Indigenous communities. Australian Community Psychologist 2009; 21(2): 7-22.
5. Wilson NW, Couper ID, De Vries E, Reid S, Fish T, Marais BJ. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural and Remote Health 2009; 9(1060): 1-21.
6. National Health and Hospitals Network. A national health and hospitals network for Australia's future. Canberra, ACT: Commonwealth of Australia, 2010.
7. Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia, April 2008. Canberra, ACT: Commonwealth of Australia, 2008.
8. Bayley S, Magin PJ, Sweatman JM, Regan CM. Effects of compulsory rural vocational training for Australian general practitioners: a qualitative study. Australian Health Review 2011; 35: 81-85.
9. Perkins D. Editorial: Fly in fly out and drive in drive out - useful contribution or worrying trend? [Editorial] Australian Journal of Rural Health 2012; 20(5): 239-240.
10. Zhao Y, Malyon R. Cost drivers of remote clinics: remoteness and population size. Australian Health Review 2010; 34: 101-105.
11. Frehywot S, Mullan F, Payne PW, Ross H. Compulsory services programmes for recruiting health workers in remote and rural areas: do they work? Bulletin of the World Health Organization 2010; 88(5): 364-370.
12. Bärnighausen T, Bloom DE. Financial incentive for return of service in underserved areas: a systematic review. BMC Health Services Research 2009; 9: 86.
13. Dwyer J. Rural clinical schools have little to show for a decade's work. Charles Sturt University News. Wagga Wagga: Charles Sturt University, 2013.
14. Walker J. No place to go for rural medical graduates. News from the School of Rural Health. Melbourne, VIC: Monash University, 2013.
15. Wakerman J, Humphreys JS, Wells R, Kuipers P, Entwistle P, Jones J. Primary health care delivery models in rural and remote Australia - a systematic review. BMC Health Services Research 2008; 8(276): 1-10.
16. Birks M, Mills J, Francis K, Coyle M, Davis J, Jones J. Models of health service delivery in remote or isolated areas of Queensland: a multiple case study. Australian Journal of Advanced Nursing 2010; 28(1): 25-34.
17. Smith JD, Margolis SA, Ayton J, Ross V, Chalmers E, Giddings P, et al. Defining remote medical practice: a consensus viewpoint of medical practitioners working and teaching in remote practice. Medical Journal of Australia 2008; 188(3): 159-161.
18. Bourke L, Humphreys JS, Wakerman J, Taylor J. Understanding rural and remote health: a framework for analysis in Australia. Health & Place 2012; 18: 496-503.
19. Wakerman J, Curry R, McEldowney R. Fly in/fly out health services: the panacea or the problem? Rural and Remote Health 12(2268): 1-4. (Online) 2012. Available: www.rrh.org.au (Accessed 10 March 2015).
20. House of Representatives Standing Committee on Regional Australia. Cancer of the bush or salvation for our cities? Fly-in, fly-out and drive-in, drive-out workforce practices in regional Australia. Submission to Inquiry into the use of 'fly-in, fly-out' and 'drive-in, drive-out' workforce practices in regional Australia. Canberra, ACT: Commonwealth of Australia, 2013.
21. Rosen A, Gurr R, Fanning P. The future of community-centred health services in Australia: lessons from the mental health sector. Australian Health Review 2010; 34: 106-115.
22. Veitch C, Lincoln M, Bundy A, Gallego G, Dew A, Bulkeley K, et al. Integrating evidence into policy and sustainable disability services delivery in western New South Wales, Australia: The 'wobbly hub and double spokes' project. BMC Health Services Research 2012; 12(70): 1-8.
23. Hanley P. The FIFO conundrum. Australian Journal of Rural Health. 2012; 20: 48.
24. Putnam RD. The prosperous community: social capital and public life. The American Prospect 1993; 13: 35-42.
25. Putnam RD. 'Health by association': some comments. [Commentary] International Journal of Epidemiology 2004; 33(4): 667-671.
26. Margolis SA. Is Fly in/Fly out (FIFO) a viable interim solution to address remote medical workforce shortages? Rural and Remote Health 12: 2261. (Online) 2012. Available: www.rrh.org.au (Accessed 10 March 2015).



