Health professionals and communities have often been concerned about the capacity of their urgent care or emergency medical services to cope with unplanned or unexpected health events1. This has been of particular concern in the rural context, which may lack basic health and emergency services taken for granted in urban settings. When combined with the problems of geography, such a paucity of services has become a major challenge for those expected to respond to medical emergencies.
Rural emergency medical services have formed part of the overall health and emergency response system, and because of their contexts and environments these services have needed to use a range of strategies to achieve the best outcomes for their communities2. To maintain a balance between the services delivered and the needs of the community, a mutual valuing between the community and local health practitioners has needed to be brokered.
This article was written with an aim to relate the experiences of one small remote community in improving urgent care arrangements, in order to assist other communities facing similar issues.
The data cited in this article came from project documentation, direct observation and in-depth discussions with participants in the project. The article presents the issues that were of concern to the Mallacoota community, describes the project structure and developmental processes used, along with the medical and ambulance service perspectives of the issues and outcomes. Lessons learned are highlighted for the benefit of other communities concerned about the adequacy of their emergency health systems.
Issues
Mallacoota in south-eastern Australia is a small, isolated community that has had a long-standing concern about the adequacy of their emergency medical systems. Mallacoota is 520 km east of Melbourne, the capital of Victoria, Australia, and close to the New South Wales state border, 85 km south of Eden and 147 km east of Orbost (Fig 1). At the time of writing, Mallacoota was one of the few isolated communities in Victoria defined as 'remote'. Australian Bureau of Statistics 2001 data estimated that Mallacoota's population was 1041 in the town area, with an additional 341 in the surrounding area. During the summer holiday season, the population of Mallacoota rises to between 3000 and 5000 people.
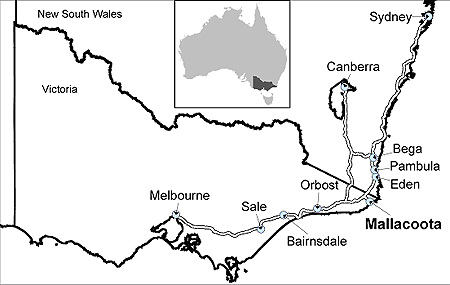
Figure 1: Location of Mallacoota in south eastern Australia.
In common with many small towns in rural Australia, Mallacoota had no hospital, the local medical practitioners reported being under stress and there were limited ambulance services. The Mallacoota Medical Centre was staffed by two medical practitioners working on a rotational basis together with on-call responsibilities covering 24 h per day. Four Ambulance Community Officers (volunteers) operated locally, while full-time paramedics were posted to the town during the 6 week peak of the tourist season. The nearest hospitals of any size were at Orbost (16 acute beds) and Pambula (30 acute beds). The nearest hospitals with fully staffed emergency departments were at Bairnsdale, Victoria, 242 km away, and Bega, New South Wales, 144 km away3. The nearest critical care facilities were further away at Central Gippsland Health Service in Sale, Victoria, or Canberra Hospital, Australian Capital Territory. The Mallacoota aerodrome was an important part of emergency service management and air ambulance services used the airport for critical care patients. Crucially, a night landing required the groundsman to ensure that kangaroos were removed from the enclosed fenced area before the plane landed.
Early consultations with the community and providers revealed a lack of balance between community expectations and the ability and willingness of health service providers to meet these expectations in Mallacoota. Medical practitioners were keen to do less out-of-hours work and to be better supported in their care of patients needing emergency medical care. The local volunteer ambulance officers had limited training and support, resulting in an inability to provide the necessary level of care for critically-ill patients being transferred to distant hospitals. This, in turn, placed even more pressure on the local medical practitioners.
The situation came to a crisis point when the medical practitioners indicated that they may leave the area if the situation remained unchanged. One of the medical practitioners wrote to the State Minister of Health on 24 July 2002, seeking help to address the situation.
The East Gippsland Division of General Practice offered to help the local medical practice improve the situation. They approached Monash University School of Rural Health for assistance through the implementation of a facilitation package that had been developed from a research project in 1999, examining urgent care in small Victorian rural towns4,5. The Victorian Department of Human Services funded the project to develop and trial an integrated approach to assist rural communities that wished to improve their urgent care services. The process, called Transforming Rural Urgent Care Systems (TrUCs), provided a framework and resource material to assist communities to improve the delivery of urgent care services. It helped develop practical and effective urgent-care response strategies, designed to respond specifically to local needs.
The anticipated outcomes of the process in Mallacoota were:
- Establishment of an effective and sustainable urgent care system that met local needs and expectations in the event of incidents that required an urgent medical response.
- Development of long-term community ownership of the urgent care system, with the operation and maintenance of the system being managed from within the local community.
Issues explored
During 2002, key members of the community identified that the state of their emergency care services was an issue of concern to them; they made a commitment to improve the situation. On 22 August 2002, a meeting of key stakeholders was held to determine a way forward. As a result, a representative Steering Committee was formed to develop a proposal to improve the emergency and critical care services for Mallacoota and district. Shortly afterwards, Monash University appointed two local people with extensive experience in research and submission writing to provide assistance and support to the Steering Committee6. While the School of Rural Health facilitator provided resources and support, the Steering Committee oversaw the local management of the project.
The Steering Committee committed itself to implementing a series of steps to develop a sustainable emergency and critical care system that would meet the community's needs and expectations. The basic steps were to:
- Commit to implementing TrUCs.
- Carry out a feasibility study to determine the current state of readiness for urgent care demands and to identify the feasible changes required that could improve the situation.
- Develop action plans through a community consultation and decision-making process.
- Ensure that the project would be independently sustainable.
- Develop an evaluation process as a means of measuring success.
Structure of the program
The program structure (Fig 2), consisted of the Steering Committee, project officers and the university facilitator, along with links to other stakeholders. The establishment of a Community Steering Committee marked the beginning of the TrUCs program. They oversaw the establishment stages of the program. This included having the power to decide whether the program proceeded past the preliminary planning meeting. The preparation of a locally tailored urgent care vision for presentation to the community at a public forum was a starting point for local discussion and debate.
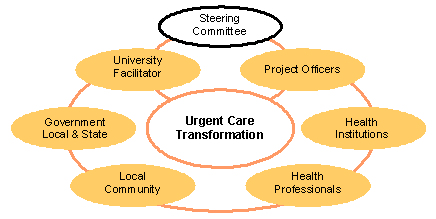
Figure 2: The TrUCs program structure.
The composition and aims of the Steering Committee, as well as its specific responsibilities and reporting arrangements, were decided locally following discussions with the university facilitator. The Steering Committee publicised its operation through a combination of direct mail, articles in the local newsletter (The Mallacoota Mouth) and a well-attended public meeting.
The Steering Committee had representation from all the main interest groups in the district. Members were drawn from the following groups:
- Local health and welfare service
- Community ambulance officers
- Ambulance auxiliary
- Victoria Police
- Rural Ambulance Victoria
- Medical practitioners
- Surf lifesaving club
- Country Fire Authority
- Community Association
- State Emergency Service
The Developmental Process
The formal TrUCs process proceeded from the initial meeting in August 2002, and ended with a major meeting with Rural Ambulance Victoria in June 2003. Running parallel to these meetings was the research process that produced a proposal and presentation to the Minister of Health to improve the emergency medical and critical care services in Mallacoota and District. These activities are summarised (Table 1).
Table 1: Mallacoota project summary
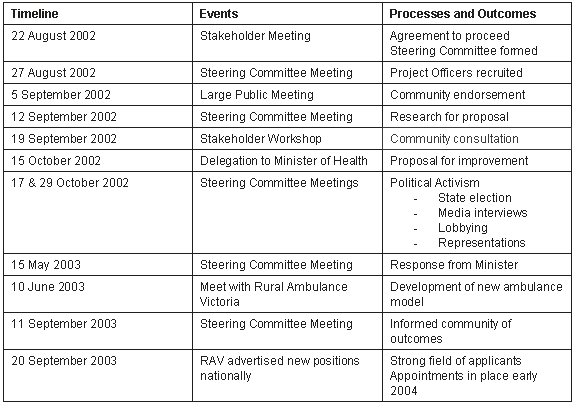
The project officers played a major role in community development and in drafting the proposal to the Minister of Health. One of the project officers also acted as the secretary to the Steering Committee and facilitated a workshop of local stakeholders.
Negotiating the challenges
The highlights of the policy development work at Mallacoota included:
- A successful public meeting to endorse the work of the Steering Committee.
- A workshop of Steering Committee members and stakeholders to develop a conceptual framework and recommendations for improvement.
- Development and presentation of an emergency and critical care model for Mallacoota to the State Minister of Health.
- Adoption of and funding of a new ambulance paramedic model for Mallacoota and another small, isolated community in the same region.
On the 5 September 2002, a public meeting was held in Mallacoota to share with the community the progress made and to seek community support for the work. A total of 240 local residents attended this meeting, with 63 apologies, making it the largest public meeting ever held in Mallacoota. The meeting unanimously adopted a vision that the Steering Committee had drafted and also a motion authorising the Steering Committee to progress the issue on behalf of the community6.
Following this show of community unity and support, the Steering Committee and project officers completed a submission to the Minister of Health. This was developed through an extensive research process and the conduct of a five-hour workshop with the members of the Steering Committee and three invited resource people from the East Gippsland Division of General Practice, Bairnsdale Regional Health Service and Monash University.
With the assistance of the local Independent Member of Parliament, who at the time jointly held the balance of Parliamentary power in Victoria, a meeting with the Minister was arranged. The presentation and submission to the Minister highlighted the critical problems with the existing situation in Mallacoota. Principally these were:
- Local medical practitioners were working under an intolerable burden of being constantly available for emergencies.
- Community ambulance officer numbers had fallen to four, with those remaining finding it difficult to cope.
- Communications were inadequate for transporting critically ill patients.
- Air ambulance services to transport critically ill patients were limited in availability.
- Mallacoota did not have a hospital or a critical care facility.
Recommendations to Minister of Health
The proposal made seven recommendations to improve the Mallacoota emergency and critical care system6:
- Mallacoota and district be supplied with an adequate standard, back-up and interstate communication system.
- Mallacoota and District be supplied with full-time 24 h/7 day advanced life support and/or MICA (intensive care) paramedic service.
- Contractual service provision for urgent services be provided for doctors in remote rural areas without public medical facilities.
- Emergency medical and ambulance consumables be provided and controlled by Rural Ambulance Victoria.
- Mallacoota and district be provided with an emergency critical care facility for the maintenance of patients.
- Air ambulance services be prioritised to cater for the needs and remoteness of the Mallacoota and district community.
- Adequacy of the Mallacoota Airport lighting to be assessed for emergency services.
These recommendations broadly fell into two groups: (i) those related to ambulance services; and (ii) those more concerned with medical services. In reality, the integrated nature of urgent care systems means that they were inevitably intertwined and inter-related5. Recommendations 1, 2, 6 and 7 directly related to ambulance service provision, while recommendations 3, 4 and 5 were the province of medical service provision.
Ambulance perspective
Communications issues (Recommendation 1) were of particular concern to the local ambulance staff who were distant from hospital facilities and who routinely travelled between Victoria and New South Wales. Their inability to adequately request help from their communications centre in Victoria or from the New South Wales Ambulance Service was of major concern to the ambulance volunteers who had limited training and experience. Rural Ambulance Victoria has addressed the majority of these concerns and are continuing to improve their communications system in the Mallacoota area.
The need to improve the responsiveness of air ambulance service (Recommendation 6) and to ensure the lighting at Mallacoota airport (Recommendation 7) were crucial elements if acutely ill or injured patients were to be evacuated promptly and safely to higher level services. Some six to eight ambulance night flights left Mallacoota each year. Using road transport offered no advantages when adequate hospitals were so far away and medical escorts were required to support the ambulance volunteers when critically ill patients were transferred. Related to this issue was the need for patient stabilisation and holding facilities while air ambulance/retrieval services made their way to Mallacoota. The local medical centre consulting rooms and the ambulance vehicle were both unsuitable for this task.
The ambulance service staffing profile of the Mallacoota area was highlighted as a major concern, with a high reliance on a diminishing pool of volunteers and full-time staff for only 6 weeks during the peak of the holiday season. The submission recommended that staffing be upgraded to full-time, professionally trained staff (Recommendation 2).
In Mallacoota, Ambulance Community Officers (ACO) were casual, on-call officers who provided emergency response and transport. They provided basic life support skills (including shock advisory defibrillation) and administered a range of baseline medications under strict protocols. Over the previous 3 years, the number of ACOs in Mallacoota had dropped from seven to four. Ensuring an adequate supply of trained and motivated staff to volunteer-based systems was an ongoing challenge that was shared with other emergency services, competing for a diminishing pool of potential members. Positive factors that were identified in this regard included the provision of good management, training, recognition, organizational support and activity, and internal communication networks7-9.
A related personnel issue was the maintenance of competency among volunteer staff, who may have small individual caseloads and limited opportunity to maintain their skills or to develop satisfactory clinical judgement. When operating from Mallacoota during the holiday season, full-time ambulance paramedics provided additional training opportunities for volunteers on an ad hoc basis.
Medical perspective
For the local medical practitioners' perspective, the major issues were the provision of resources to support emergency and after-hours care. For instance, Australia's universal health insurance scheme (Medicare) did not provide item numbers for emergency care that meet the requirements for rural medical practitioners in areas without a hospital (Recommendation 3). Current Medicare item numbers related to a regular medical practice, or institutions such as a hospital, as distinct from offering medical services in an emergency context. The role of the medical practitioner in providing urgent and emergency services in conjunction with ambulance services in towns without a hospital needed to be acknowledged.
Another issue for the local medical practice was the need for extra medical supplies to replace those used when medical practitioners were called to emergency incidents and administered resources from the medical centre supplies (Recommendation 4). A mechanism was needed for the medical practitioner to be reimbursed for consumables used in such a situation.
One of the continuing issues for the medical practitioners in Mallacoota was the need for a critical care facility in which to stabilise and hold patients until they could be transferred to definitive care. While not ignoring the aim of minimizing the period of time from injury to definitive treatment, guidelines advising that patients should be transported to tertiary care within 30 min are impracticable in remote areas like Mallacoota. Emergency and critical care services should be:
- Accessible and available to patients at all times.
- Have provision for emergency transport services including road, fixed wing and rotary wing where appropriate.
- Committed to establishing two-way communications that allow field-to-hospital communication between ambulance and hospital.
- Committed to maintaining and communicating information about the status of the service to other providers10.
It was acknowledged that rural areas with limited medical facilities required special consideration within a retrieval system, because '...it needs to be emphasised that where a rural hospital or medical practitioner requests retrieval, the service should err on the side of over-responsiveness to ensure that practitioners are not left to manage cases with which they are not comfortable'11.
The political and policy process
The process of considering the submission to the Minister of Health took considerably longer than expected due to the calling of a State election and a change of Minister following the re-election of the Labor government in its own right. During this time, staff of the Department of Human Services, Rural Ambulance Victoria and the local stakeholders worked together to determine policy initiatives that would meet the needs of the Mallacoota community.
There was a degree of political action involved in the process, such as radio interviews and contact with all political parties. Some public servants and health service providers had difficulty accepting this political process, despite their acceptance of the idea in principle. Overall though, all parties made an effort to remain non-party political in their actions, on the understanding that they would need to work together during the implementation phase.
The most significant proposal considered during this time was Rural Ambulance Victoria's development of a new community-based paramedic model, Paramedic Community Support Coordinator, which drew on developments in Australia12, the UK13-15 and the USA16-24. Internationally, the most influential document was the US National Highway Traffic Safety Administrator's Agenda for the Future, which saw emergency medical services of the future undertaking a community-based health management role, fully integrated into the overall health system25. In the UK, the report of the Joint Royal Colleges and Ambulance Liaison Committee on the future role and education of paramedics set the agenda26.
The proposal from Rural Ambulance Victoria sought to expand the role of ambulance paramedics to encompass broader community development; a larger role in public health, health promotion and education; and improved support for ambulance volunteers. On paper, this proposal was different from Recommendation 2 that suggested a conventional full-time ambulance staffing profile. However, Rural Ambulance Victoria shared with the community a firm commitment to improve the accessibility and quality of emergency medical services to the community. (The remaining recommendations were pursued by the community liaison sub-committee of the TrUCs Steering Committee, after the new ambulance paramedic was appointed.)
Success and its policy implications
In the first post-election budget, the Victorian State Government allocated funding to implement the community paramedic model in Mallacoota and another isolated rural community in the same region. In total AU$400 000 was allocated in the State budget to provide a new service delivery model for ambulance services in these two remote areas, with the same amount made available for establishment costs.
Lessons
At the time of writing, Rural Ambulance Victoria was working with the local Steering Committee to fully develop and implement the new ambulance model, who they involved in the recruitment and selection processes, through the supply of information about the community and input into the position description. A local community representative was involved in the selection process.
One of the other major benefits of the process was an evident improvement in community cohesiveness. At least within the area of emergency medical services, the community demonstrated shared values, aspirations and goals. The program has seen a partnership formed among agencies, community groups and commercial enterprises. An important aspect of the exercise was community engagement in the political and policy processes. This forced government departments and service providers to accept a community-driven process, rather than acting out the rhetoric or apparently listening to the community while implementing centrally-driven policy initiatives.
To some extent, the case was unproven because it was possible that the interests of the major stakeholders and the local community matched through serendipity, rather than through a process of negotiation. The test of the relationships formed and nurtured would be when the community began to ask for policy changes that did not match those of the external stakeholders. A good start was made in this regard through Rural Ambulance Victoria including members of the community in the process of refining their new ambulance paramedic model. This promising start needed to be made more permanent through the establishment of permanent community links to facilitate the exchange of information, as well as the sharing of resources and the commitment of skills, time and effort to planning and preparedness.
The TrUCs process developed at Monash University with the financial assistance of the Victorian Department of Human Services, proved to be a successful approach because it encouraged members of the local community to be part of the political and policy process. It was also important to have local project officers with high-level skills who could work with the local Steering Committee, and a university facilitator who was able to work behind the scenes. Keeping 'out of the way' and not seeking to control the process was central to this facilitation role.
This small isolated community appeared to have met its needs and expectations through the adoption of this policy development process, their own commitment and unity of purpose. While policy development and implementation took longer than the community activists would have liked, the longer timeframe had the advantage of encouraging a more positive and sustainable engagement with State Government authorities and service providers.
The community development approach developed and trialled in Mallacoota had the potential to be applied in other rural and remote places that face challenges in the delivery of essential emergency medical services. To do this effectively, government authorities should consider providing the financial resources to adopt the policy development processes described, and to employ suitably skilled and independent facilitators and project officers to assist with implementation.
Specific lessons include:
- Crucial to the success of the program were the community consultation and decision-making processes that aimed to positively engage community members.
- The establishment of a community Steering Committee was a vital component of the community development effort.
- A key role was the preparation of a locally tailored urgent care vision for presentation to the community at a public forum because insufficient community support for the urgent care vision would have indicated that the process should not proceed further.
- One of the important roles of the Steering Committee was to publicise the operation of the committee in order to minimise confusion and maximise transparency of the change process for everyone involved.
- The appointment of the project officers was crucial because they played a major role in community development and in drafting the proposal to the Minister of Health. One of the project officers also acted as the secretary to the Steering Committee and facilitated a workshop of local stakeholders. Monash University provided administrative and research support for the project officers and the facilitator acted as a 'sounding board' in the background.
- In order for full-time ambulance paramedics to provide ad hoc training for volunteers, the role of ambulance paramedics needed to be broadened to include responsibilities for community and volunteer development.
Acknowledgements
We would like to thank the people of Mallacoota and the members of the Project Steering Committee for their enthusiasm and unity of purpose. Without them this project would not have been successful. The Department of Human Services, Victoria, provided funding to Monash University School of Rural Health for the development of the community development processes and the accompanying manual. For further information, contact Dr Peter O'Meara at the School of Public Health, Charles Sturt University, Panorama Avenue, Bathurst, New South Wales 2795, Australia. Telephone +612 63384090. email pomeara@csu.edu.au
References
1. Turner J, Judge TP, Ward ME et al. New worldwide systems model for emergency medical services: statement from the Cape Town EMS summit, South Africa, January 1998. Journal of Pre-hospital Immediate Care 2000; 4: 183-188.
2. Williams JM, Ehrlich PF, Prescott JE. Emergency medical care in rural America. Annals of Emergency Medicine 2001; 38: 323-327.
3. Department of Human Services, Gippsland Region. Emergency and Critical Care Services Plan for the Gippsland Region. Traralgon: Department of Human Services Victoria, Gippsland Region, August 2001.
4. Kelly H, O'Meara P, Burley M. Urgent care in Victorian rural towns: final Report. Traralgon: Monash University Centre for Rural Health, 1999.
5. O'Meara P, Burley M, Kelly H. Rural urgent care models: what are they made of? Australian Journal of Rural Health 2002; 10: 45-50.
6. Steering Committee for Mallacoota Emergency and Critical Services. 2002. Mallacoota emergency critical care services: a model for transforming rural urgent care. Submission to Minister of Health. Mallacoota: Steering Committee for Mallacoota Emergency and Critical Services, October 2002.
7. Duffield C, Macneil F, Bullock C, Franks H. The role of the Advanced Casualty Management Team in St John Ambulance Australia (New South Wales District). Australian Health Review 2000; 23: 90-99.
8. Howard BW. Managing volunteers. Australian Journal of Emergency Management 1999; Spring: 37-38.
9. Reinholtd S, Smith P. Directions in volunteer development in Australian emergency services. Melbourne: Country Fire Authority Victoria, 1998.
10. Ministerial Taskforce on Trauma and Emergency Services and Department of Human Services Working Party on Emergency and Trauma Services. Review of Trauma and Emergency Services. Melbourne: Department of Human Services, 1998.
11. KPMG Consultants. Services Specification for Medical Retrieval Services in Victoria, Final Report. Melbourne: Department of Human Services, March, 2001.
12. O'Meara P. Would a pre-hospital practitioner model improve patient care in rural Australia? Emergency Medicine Journal 2003; 20: 199-203.
13. Lendrum K, Wilson S, Cooke MW. Does the training of ambulance personnel match the workload seen? Pre-hospital Immediate Care 2000; 4: 7-10.
14. Roberts G. Paramedics: should we be creating a new profession? Ambulance UK 1998; 13: 7-8.
15. Nicholl J, Turner J, Martin D. The future of ambulance services in the United Kingdom 2000-2010. Sheffield: Ambulance Service Association, 2001.
16. Garza MA. Rethinking EMS after Sand Key, things will never be the same. Journal of Emergency Medical Services 1994; 19: 103-107.
17. Martinez R. New vision for the role of emergency medical services. Annals of Emergency Medicine 1998; 32: 594-599.
18. Meade DM. Expanded-scope practice: EMS at the crossroads of care. Emergency Medical Services 1998; 27(5): 39-40.
19. Spaite DW, Criss EA, Valenzuel TD, Meislin HW. Developing a foundation for the evaluation of expanded-scope EMS: a window of opportunity that cannot be ignored. Annals of Emergency Medicine 1997; 30: 791-796.
20. Neely KW, Drake MER, Moorhead JC, Schmidt TA, Skeen DT, Wilson EA. Multiple options and unique pathways: a new direction for EMS? Annals of Emergency Medicine 1997; 30: 797-799.
21. Delbridge TR, Baily B, Chew JL et al. EMS agenda for the future: where we are ... where we want to be. Annals of Emergency Medicine, 1998; 31: 251-263.
22. O'Connor RE, Cone DC, De Lorenzo RA et al. EMS systems: foundations for the future. Academic Emergency Medicine 1999; 6: 46-53.
23. Hunt JD, Gratton MC, Campbell JP. Prospective determination of medical necessity for ambulance transport by on-scene paramedics. Academic Emergency Medicine 1999; 6: 447.
24. Schmidt T, Atcheson R, Federiuk C, Mann NC, Pinney T, Fuller D. Evaluation of protocols allowing emergency medical technicians to determine need for treatment and transport. Academic Emergency Medicine 2000; 7: 663-669.
25. National Highway Traffic Safety Administrator. Emergency Medical Services Agenda for the Future. (Online) 1996. Available: http://www.nhtsa.dot.gov/people/injury/ems/agenda/emsman.html (Accessed 15 September 2003).
26. Joint Royal Colleges Ambulance Liaison Committee. 2000. The future role and education of paramedic ambulance service personnel (emerging concepts). (Online) 2000. Available: http://www.jrcalc.org.uk/ (Accessed 15 September 2003).

